Abstract
The dynamic interactions between leukemic cells and cells resident within the bone marrow microenvironment are vital for leukemia progression. The lack of detailed knowledge about the cellular and molecular mechanisms involved in this cross-talk restricts the design of effective treatments. Guarnerio et al. (2018) by using state-of-the-art techniques, including sophisticated Cre/loxP technologies in combination with leukemia mouse models, reveal that mesenchymal stem cells via promyelocytic leukemia protein (Pml) maintain leukemic cells in the bone marrow niche. Strikingly, genetic deletion of Pml in mesenchymal stem cells raised survival of leukemic mice under chemotherapeutic treatment. The emerging knowledge from this research provides a novel target in the bone marrow niche for therapeutic benefit in leukemia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancer is the leading cause of death worldwide [1]. The hematologic cancers, leukemias, are caused by the acquisition of malignant mutations in hematopoietic progenitor cells which confer their clonal expansion, aberrant self-renewal capacity, allowing them to proliferate indefinitely without differentiation, and prejudicing their normal functions [2]. Leukemia is characterized by the unrestrained formation of leukemic cells and defective normal hematopoiesis [3]. Despite significant improvements in the outcome of leukemic patients due to modern chemotherapeutic treatments combined with bone marrow transplants, leukemia relapse after therapy is still common.
Leukemia, similarly to other malignancies, depends not only on intrinsic genetic alterations but is supported by cooperation with bystander cells residing in the bone marrow microenvironment [4, 5]. Signals emanating from these cells are essential for leukemic clones’ maintenance, supporting survival, resistance to chemotherapy, proliferation, and migration [6]. Albeit the importance of the microenvironment for leukemic progression is well accepted, the detailed mechanisms involved in the complex interplay between the cells present in the leukemic niche and cancer cells are poorly understood. Deep understanding of the active involvement niche cells in shaping the leukemic microenvironment may offer novel clues for designing therapeutic strategies. The discovery of molecules that strengthen the niche-mediated resistance to chemotherapy challenges the eradication of residual leukemic cells hiding in the bone marrow microenvironment. Elucidating the effect of microenvironmental cues on leukemic cells will bring novel targets to achieve complete remission.
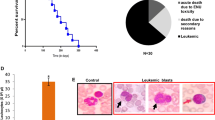
Bone marrow niches within the bones provide a sanctuary for leukemic cells to evade death. Even though it is well accepted that bone marrow stromal cells promote leukemic cells resistance to chemotherapy [7], the details of the cellular and molecular mechanisms involved in this support remain unclear. Mesenchymal stem cells are found throughout the body [8, 9]. These cells are able to self-renew and differentiate into various cell populations. In the bone marrow, they provide a niche for growth, differentiation, and survival of normal and malignant hematopoietic cells [10,11,12]. Now, in a recent article in Nature Communications, Guarnerio and colleagues reveal that the promyelocytic leukemia protein (Pml) in mesenchymal stem cells is as a therapeutic target for leukemia [13]. The authors investigated the role of mesenchymal stem cells in leukemia progression by using state-of-the-art techniques, including in vivo serial transplantation, sophisticated Cre/loxP technologies in combination with leukemia mouse models, and in vitro elegant co-culture assays. Using Prx1-Cre/Pml-floxed mice, these experiments revealed that mesenchymal stem cells expand after Pml loss in the bone marrow [13]. Interestingly, Guarnerio and colleagues showed that leukemic cell growth decreased in the bone marrow of Pml knockout mice as compared with controls, suggesting that sustainability of leukemic cells within the bone marrow depends on the expression of Pml in niche cells. Strikingly, deletion of Pml in mesenchymal stem cells increased survival of mice transplanted with leukemic cells under chemotherapeutic treatment via induction of leukemic cell cycle arrest and inhibiting leukemic reconstitution ability [13]. Moreover, Guarnerio and colleagues discovered that several pro-inflammatory molecules are downregulated post-deletion of Pml in cultured mesenchymal stem cells. Using blocking antibodies and recombinant proteins in co-cultures of leukemic cells with mesenchymal stem cells, the authors showed that chemokine (C-X-C motif) ligand 1 (CXCL1) and interleukin 6 (IL6) production depends on mesenchymal stem cells’ Pml, and this Pml is important maintenance of leukemic cells by mesenchymal stem cells. Thus, this study brings novel targets for leukemia, which is urgently needed in the clinic (Fig. 1).
Pml role in mesenchymal stem cells in the leukemia microenvironment. Bone marrow microenvironment is critical for the maintenance and expansion of leukemic cells. The study of Guarnerio and colleagues now suggests that mesenchymal stem cells’ control of leukemic cells in the bone marrow niche is dependent on Pml expression [13]. Pml expression in mesenchymal stem cells induces the production of pro-inflammatory molecules, including CXCL1 and IL6, in the leukemia microenvironment. Genetic deletion of Pml in bone marrow mesenchymal stem cells increased survival of mice under chemotherapeutic treatment after transplantation with leukemic cells. With the appearance of state-of-art technologies, future studies will reveal in detail the cellular and molecular mechanisms involved in leukemia progression in the bone marrow niche
Here, we discuss the findings from this study and evaluate recent advances in our understanding of the leukemic microenvironment in the bone marrow.
Perspectives/future directions
Specificity of the use of Prx-Cre drivers
The use of conventional knockout mouse models has been proven useful to understand the role of key genes in physiological and pathological states. Nevertheless, these technologies produce broad changes in gene function throughout the body since embryonic stages, affecting several cell populations. Thus, they are limited in that they do little to contribute with knowledge about specific roles of a gene in a precise cell type. Since the molecular functions of proteins may depend on the particular cell subset in which they are expressed, restricting gene manipulation to unique cells in the bone marrow may be useful to comprehend protein functions. Thus, conditional gene manipulation methods offer mighty alternatives [14,15,16,17,18]. The main findings from this study are based on the data obtained from Prx1-Cre/Pml-floxed mice [13]. It is known that paired-related homeobox 1 (Prx1) gene is expressed in mesenchymal stem cells [19]. Note, however, that expression of Prx1 is not restricted to mesenchymal stem cells. For instance, cells from the adipogenic lineage also may express Prx1 [20]. Additionally, Prx1 is broadly expressed early during limb bud mesoderm development [21, 22]. Consistent with this, Prx1-Cre mice may exhibit Cre recombinase activity in various cell populations during embryogenesis, in addition to mesenchymal stem cells [20]. Therefore, it is possible that the effect on leukemic cells could be due to a cell distinct from mesenchymal stem cells, in which Pml was also deleted in Prx1-Cre/Pml-floxed mice. Because of this, to avoid Cre recombinase activity in other cell types during development, a mouse model in which recombination only occur in adult Prx1-expressing cells (mesenchymal stem cells) should be used in future studies, i.e., Prx1-CreER mice [23]. In Prx1-CreER/Pml-floxed mice, it will be possible to temporally control Pml expression in mesenchymal stem cells.
According to the International Society for Cellular Therapy (ISCT), mesenchymal stem cells are defined partially based on their capacity to form colony-forming fibroblast units (CFU-F) [24,25,26]. All CFU-F activity in the bone marrow was reported to be targeted in Prx1-Cre/TdTomato mice [27]. Cells targeted in those mice are heterogeneous and reside within distinct bone marrow niches within the bone marrow [28]. Interestingly, recent work has shown that deletion of specific cytokines from mesenchymal stem cells in separate vascular beds in the bone marrow, arterioles, and sinusoids, affects differently hematopoietic stem cells in these niches [11]. It remains unknown whether the arteriolar niche cells are targeted in Prx1-Cre/Pml-floxed mice. Thus, multiple questions arise from this study. Guarnerio and colleagues indicate that in Prx1-Cre/Pml-floxed mice, normal hematopoietic stem cells are not affected [13]. If arteriolar cells are not targeted in Prx1-Cre mice, does deletion of Pml in arteriolar niche cells influence normal hematopoietic stem cells? Myh11-CreER driver could be used for this purpose [11]. On the other hand, if arteriolar cells are targeted in Prx1-Cre mice, future studies will need to explore which cell populations are important for leukemic cell maintenance via expression of Pml. Are arteriolar and sinusoid niches participating in a similar manner?
Effect of Pml deletion on mesenchymal stem cells differentiation capacity
Bone marrow mesenchymal stem cells are multipotent cells, being able to differentiate into a variety of other cell types during development, such as osteoblasts, chondrocytes, and fat cells [9, 11, 12]. Guarnerio and colleagues described that upon Pml deletion, mesenchymal stem cells do not change their differentiation capacity in vitro after exposure to special factors [13]. Nevertheless, cell culture system may cause alterations in the cultured cells, leading them to behave differently than the same cells in vivo. These artificial conditions and high concentration of mitogens can induce differentiation ability in the cultured cells that may not be shared by the corresponding endogenous mesenchymal stem cells in vivo after Pml deletion [29]. Therefore, future studies should thoroughly explore the differentiation capacity of mesenchymal stem cells in vivo in Prx1-Cre/Pml-floxed mice. Mesenchymal stem cells expand upon Pml loss in the bone marrow [13]. As those cells originate osteocytes, chondrocytes, and adipocytes during development, and if the differentiation capacity of mesenchymal stem cells is not altered, we expect that the numbers of cells derived from mesenchymal stem cells will be increased as well. Therefore, these other cell types, at a higher number, may also affect the development of leukemia seen in Prx1-Cre/Pml-floxed mice. Thus, future studies should clarify the role of Pml in mesenchymal stem cell biology in the bone marrow.
Pro-inflammatory role of Pml from mesenchymal stem cells
Inflammation is a physiological process which happens in response to tissue stressors, generating several inflammatory mediators, including chemokines and cytokines [30]. Multiple studies have reported that chronic inflammation elevates the risk for progression of certain types of cancer, and that the inflamed microenvironment facilitates cancer development via modulation of expression of growth factors and suppression of the immune response [31, 32]. Guarnerio and colleagues suggest, based on ELISA immunoassays, that Pml expression induces mesenchymal stem cells to produce various pro-inflammatory molecules [13]. Elegant co-culture systems between mesenchymal stem cells from Pml knockout mice and leukemic cells show that CXCL1 and IL6 derived from mesenchymal stem cells are important for the maintenance of leukemic cells. Nevertheless, CXCL1 and IL6 have not been conditionally deleted from bone marrow mesenchymal stem cells, so there is no direct evidence that mesenchymal stem cells are the only/main functionally important source of these factors. This may be addressed by analyzing the effect of genetic ablation of mesenchymal stem cells from leukemic bone marrow by using Prx1-Cre/iDTR mice [11]. Also, the generation of CXCL1-floxed and IL6-floxed mice to be crossed with mesenchymal stem cell-specific Cre drivers, such as Prx1-Cre mice [21], will allow to specifically delete CXCL1 and IL6 from mesenchymal stem cells. In addition to studies in genetic mouse models, transcriptomic and single bone marrow mesenchymal stem cell analysis, such as RNA sequencing upon Pml deletion, represent fundamental tools that will help to understand the roles of mesenchymal stem cells within the bone marrow leukemic microenvironment.
Bone marrow heterogeneity
The bone marrow consists of a variety of cell populations among hematopoietic and non-hematopoietic cells, including mesenchymal stem cells, osteoblasts, endothelial cells, pericytes, smooth muscle cells, fibroblasts, adipocytes, glial cells, macrophages, osteoclasts, megakaryocytes, lymphocytes, and neutrophils [8, 33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57]. Several of those cellular subtypes within the bone marrow microenvironment contribute to the complex regulation of hematopoietic stem cells function and may contribute to leukemic cells maintenance as well [58]. It will be interesting to explore in future studies what is the role of Pml expressed by other cell types, besides mesenchymal stem cells, in the regulation of normal and leukemic stem cells function. Moreover, recently, it was revealed that leukemic cells create changes in the bone marrow nerves that affect the activity of mesenchymal stem cells [59,60,61]. Since Pml may be expressed in the nervous system [62], whether Pml expression affects nerves in leukemic settings should be examined in future studies.
Clinical relevance
Leukemias are heterogeneous and are classified based on their lymphoid or myeloid origins, as well as on their acute or chronic progress into four common types: chronic myeloid leukemia, acute myeloid leukemia, chronic lymphocytic leukemia, and acute lymphocytic leukemia [63]. Guarnerio and colleagues report that not all leukemic models tested are affected by Pml ablation [13]. Future studies will reveal the molecular mechanisms induced by Pml deletion in mesenchymal stem cells, and why for some leukemias Pml expression in mesenchymal stem cells is not essential for their progression.
Arsenic trioxide (As2O3) is a small molecular inhibitor of Pml, used for acute promyelocytic leukemia therapy, approved by the Food and Drug Administration (FDA) [64]. The authors suggest that the benefic effects of AS2O3 probably come from targeting mesenchymal stem cells as well. Nonetheless, As2O3 has major limitations associated with toxic side effects, such as gastrointestinal reactions, skin damage, differentiation syndrome, cardiovascular defects, and liver and kidney dysfunctions [65,66,67,68]. Future works should develop Pml inhibitors that would block Pml function specifically in mesenchymal stem cells and leukemic cells to avoid side effects.
The role of mesenchymal stem cells Pml in other cancers
In addition to leukemia, mesenchymal stem cells have been shown to play important roles in the growth and progression of other cancers, such as lymphoma [69], breast cancer [70], prostate cancer [71], head and neck carcinoma [72], colon cancer [73], gastric cancer [74], and glioblastoma [75, 76]. Also, mesenchymal stem cells may activate the motility and invasiveness of cancer cells, inducing metastatic potential in those cells [77]. It remains completely unknown what is the role of Pml in mesenchymal stem cells in the primary as well as secondary sites of other tumors outside the bone marrow. Future studies will address this question, exploring the potential of using Pml inhibitors, utilized in leukemia clinics, for other cancers.
Conclusion
In conclusion, the study by Guarnerio and colleagues reveal that mesenchymal stem cells via Pml expression maintain leukemic cells within the bone marrow [13]. Yet, our understanding of cross-talk between different constituents of the bone marrow leukemic niche still remains limited, and the complexity of these interactions during leukemia progression should be elucidated in future studies. A big challenge that we face is how to translate animal research into humans. Improving the availability of human tissue samples may help to reach this goal.
References
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics, 2017. CA Cancer J Clin 67(1):7–30. https://doi.org/10.3322/caac.21387
Claus R, Lubbert M (2003) Epigenetic targets in hematopoietic malignancies. Oncogene 22(42):6489–6496. https://doi.org/10.1038/sj.onc.1206814
Papaemmanuil E, Gerstung M, Bullinger L, Gaidzik VI, Paschka P, Roberts ND, Potter NE, Heuser M, Thol F, Bolli N, Gundem G, Van Loo P, Martincorena I, Ganly P, Mudie L, McLaren S, O’Meara S, Raine K, Jones DR, Teague JW, Butler AP, Greaves MF, Ganser A, Dohner K, Schlenk RF, Dohner H, Campbell PJ (2016) Genomic classification and prognosis in acute myeloid leukemia. N Engl J Med 374(23):2209–2221. https://doi.org/10.1056/NEJMoa1516192
Birbrair A (2017) Stem cell microenvironments and beyond. Adv Exp Med Biol 1041:1–3. https://doi.org/10.1007/978-3-319-69194-7_1
Azevedo PO, Paiva AE, Santos GSP, Lousado L, Andreotti JP, Sena IFG, Mintz A, Birbrair A (2018) Cross-talk between lung cancer and bones results in neutrophils that promote tumor progression. Cancer Metastasis Rev
Tabe Y, Konopleva M (2017) Leukemia stem cells microenvironment. Adv Exp Med Biol 1041:19–32. https://doi.org/10.1007/978-3-319-69194-7_3
Konopleva M, Konoplev S, Hu W, Zaritskey AY, Afanasiev BV, Andreeff M (2002) Stromal cells prevent apoptosis of AML cells by up-regulation of anti-apoptotic proteins. Leukemia 16(9):1713–1724. https://doi.org/10.1038/sj.leu.2402608
Birbrair A, Almeida GG, Borges IDT, Gilson Sena IF, da Silva ML, Goncalves R, Mintz A, Delbono O (2017) How plastic are pericytes? Stem Cells Dev 26(14):1013–1019. https://doi.org/10.1089/scd.2017.0044
Frenette PS, Pinho S, Lucas D, Scheiermann C (2013) Mesenchymal stem cell: keystone of the hematopoietic stem cell niche and a stepping-stone for regenerative medicine. Annu Rev Immunol 31:285–316. https://doi.org/10.1146/annurev-immunol-032712-095919
Pinho S, Lacombe J, Hanoun M, Mizoguchi T, Bruns I, Kunisaki Y, Frenette PS (2013) PDGFRalpha and CD51 mark human nestin+ sphere-forming mesenchymal stem cells capable of hematopoietic progenitor cell expansion. J Exp Med 210(7):1351–1367. https://doi.org/10.1084/jem.20122252
Asada N, Kunisaki Y, Pierce H, Wang Z, Fernandez NF, Birbrair A, Ma'ayan A, Frenette PS (2017) Differential cytokine contributions of perivascular haematopoietic stem cell niches. Nat Cell Biol 19(3):214–223. https://doi.org/10.1038/ncb3475
Khan JA, Mendelson A, Kunisaki Y, Birbrair A, Kou Y, Arnal-Estape A, Pinho S, Ciero P, Nakahara F, Ma’ayan A, Bergman A, Merad M, Frenette PS (2016) Fetal liver hematopoietic stem cell niches associate with portal vessels. Science 351(6269):176–180. https://doi.org/10.1126/science.aad0084
Guarnerio J, Mendez LM, Asada N, Menon AV, Fung J, Berry K, Frenette PS, Ito K, Pandolfi PP (2018) A non-cell-autonomous role for Pml in the maintenance of leukemia from the niche. Nat Commun 9(1):66. https://doi.org/10.1038/s41467-017-02427-x
Almeida VM, Paiva AE, Sena IFG, Mintz A, Magno LAV, Birbrair A (2017) Pericytes make spinal cord breathless after injury. Neuroscientist:107385841773152. https://doi.org/10.1177/1073858417731522
Santos GSP, Prazeres P, Mintz A, Birbrair A (2017) Role of pericytes in the retina. Eye 32:483–486. https://doi.org/10.1038/eye.2017.220
Azevedo PO, Sena IFG, Andreotti JP, Carvalho-Tavares J, Alves-Filho JC, Cunha TM, Cunha FQ, Mintz A, Birbrair A (2017) Pericytes modulate myelination in the central nervous system. J Cell Physiol
Andreotti JP, Lousado L, Magno LAV, Birbrair A (2017) Hypothalamic neurons take center stage in the neural stem cell niche. Cell Stem Cell 21(3):293–294. https://doi.org/10.1016/j.stem.2017.08.005
Sena IFG, Paiva AE, Prazeres PHDM, Azevedo PO, Lousado L, Bhutia SK, Salmina AB, Mintz A, Birbrair A (2018) Glioblastoma-activated pericytes support tumor growth via immunosuppression. Cancer Med 7:1232–1239. https://doi.org/10.1002/cam4.1375
Greenbaum A, Hsu YM, Day RB, Schuettpelz LG, Christopher MJ, Borgerding JN, Nagasawa T, Link DC (2013) CXCL12 in early mesenchymal progenitors is required for haematopoietic stem-cell maintenance. Nature 495(7440):227–230. https://doi.org/10.1038/nature11926
Krueger KC, Costa MJ, Du H, Feldman BJ (2014) Characterization of Cre recombinase activity for in vivo targeting of adipocyte precursor cells. Stem Cell Rep 3(6):1147–1158. https://doi.org/10.1016/j.stemcr.2014.10.009
Logan M, Martin JF, Nagy A, Lobe C, Olson EN, Tabin CJ (2002) Expression of Cre recombinase in the developing mouse limb bud driven by a Prxl enhancer. Genesis 33(2):77–80. https://doi.org/10.1002/gene.10092
Martin JF, Bradley A, Olson EN (1995) The paired-like homeo box gene MHox is required for early events of skeletogenesis in multiple lineages. Genes Dev 9(10):1237–1249
Kawanami A, Matsushita T, Chan YY, Murakami S (2009) Mice expressing GFP and CreER in osteochondro progenitor cells in the periosteum. Biochem Biophys Res Commun 386(3):477–482. https://doi.org/10.1016/j.bbrc.2009.06.059
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, Deans R, Keating A, Prockop D, Horwitz E (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8(4):315–317. https://doi.org/10.1080/14653240600855905
Pereira LX, Viana CTR, Orellano LAA, Almeida SA, Vasconcelos AC, Goes AM, Birbrair A, Andrade SP, Campos PP (2017) Synthetic matrix of polyether-polyurethane as a biological platform for pancreatic regeneration. Life Sci 176:67–74. https://doi.org/10.1016/j.lfs.2017.03.015
Andreotti JP, Prazeres PHDM, Magno LAV, Romano-Silva MA, Mintz A, Birbrair A (2018) Neurogenesis in the postnatal cerebellum after injury. Int J Dev Neurosci 67:33–36
Zhou BO, Yue R, Murphy MM, Peyer JG, Morrison SJ (2014) Leptin-receptor-expressing mesenchymal stromal cells represent the main source of bone formed by adult bone marrow. Cell Stem Cell 15(2):154–168. https://doi.org/10.1016/j.stem.2014.06.008
Borges I, Sena I, Azevedo P, Andreotti J, Almeida V, Paiva A, Santos G, Guerra D, Prazeres P, Mesquita LL, Silva LSB, Leonel C, Mintz A, Birbrair A (2017) Lung as a niche for hematopoietic progenitors. Stem Cell Rev 13(5):567–574. https://doi.org/10.1007/s12015-017-9747-z
Snippert HJ, Clevers H (2011) Tracking adult stem cells. EMBO Rep 12(2):113–122. https://doi.org/10.1038/embor.2010.216
Spaeth E, Klopp A, Dembinski J, Andreeff M, Marini F (2008) Inflammation and tumor microenvironments: defining the migratory itinerary of mesenchymal stem cells. Gene Ther 15(10):730–738. https://doi.org/10.1038/gt.2008.39
Keibel A, Singh V, Sharma MC (2009) Inflammation, microenvironment, and the immune system in cancer progression. Curr Pharm Des 15(17):1949–1955
Andreotti JP, Paiva AE, Prazeres P, Guerra DAP, Silva WN, Vaz RS, Mintz A, Birbrair A (2018) The role of natural killer cells in the uterine microenvironment during pregnancy. Cell Mol Immunol. https://doi.org/10.1038/s41423-018-0023-1
Birbrair A, Frenette PS (2016) Niche heterogeneity in the bone marrow. Ann N Y Acad Sci 1370(1):82–96. https://doi.org/10.1111/nyas.13016
Sena IFG, Borges IT, Lousado L, Azevedo PO, Andreotti JP, Almeida VM, Paiva AE, Santos GSP, Guerra DAP, Prazeres P, Souto L, Mintz A, Birbrair A (2017) LepR+ cells dispute hegemony with Gli1+ cells in bone marrow fibrosis. Cell Cycle 16:1–5. https://doi.org/10.1080/15384101.2017.1367072
Azevedo PO, Lousado L, Paiva AE, Andreotti JP, Santos GSP, Sena IFG, Prazeres P, Filev R, Mintz A, Birbrair A (2017) Endothelial cells maintain neural stem cells quiescent in their niche. Neuroscience 363:62–65. https://doi.org/10.1016/j.neuroscience.2017.08.059
Paiva AE, Lousado L, Almeida VM, Andreotti JP, Santos GSP, Azevedo PO, Sena IFG, Prazeres PHDM, Borges IT, Azevedo V, Birbrair A (2017) Endothelial cells as precursors for osteoblasts in the metastatic prostate cancer bone. Neoplasia 19:928–931
Lousado L, Prazeres P, Andreotti JP, Paiva AE, Azevedo PO, Santos GSP, Filev R, Mintz A, Birbrair A (2017) Schwann cell precursors as a source for adrenal gland chromaffin cells. Cell Death Dis 8(10):e3072. https://doi.org/10.1038/cddis.2017.456
Guerra DAP, Paiva AE, Sena IFG, Azevedo PO, Batista ML Jr, Mintz A, Birbrair A (2017) Adipocytes role in the bone marrow niche. Cytometry A 93:167–171. https://doi.org/10.1002/cyto.a.23301
Dias Moura Prazeres PH, Sena IFG, Borges IDT, de Azevedo PO, Andreotti JP, de Paiva AE, de Almeida VM, de Paula Guerra DA, Pinheiro Dos Santos GS, Mintz A, Delbono O, Birbrair A (2017) Pericytes are heterogeneous in their origin within the same tissue. Dev Biol 427(1):6–11. https://doi.org/10.1016/j.ydbio.2017.05.001
Prazeres P, Almeida VM, Lousado L, Andreotti JP, Paiva AE, Santos GSP, Azevedo PO, Souto L, Almeida GG, Filev R, Mintz A, Goncalves R, Birbrair A (2017) Macrophages generate pericytes in the developing brain. Cell Mol Neurobiol 38:777–782. https://doi.org/10.1007/s10571-017-0549-2
Birbrair A, Sattiraju A, Zhu D, Zulato G, Batista I, Nguyen VT, Messi ML, Solingapuram Sai KK, Marini FC, Delbono O, Mintz A (2017) Novel peripherally derived neural-like stem cells as therapeutic carriers for treating glioblastomas. Stem Cells Transl Med 6(2):471–481. https://doi.org/10.5966/sctm.2016-0007
Birbrair A, Wang ZM, Messi ML, Enikolopov GN, Delbono O (2011) Nestin-GFP transgene reveals neural precursor cells in adult skeletal muscle. PLoS One 6(2):e16816. https://doi.org/10.1371/journal.pone.0016816
Birbrair A, Zhang T, Files DC, Mannava S, Smith T, Wang ZM, Messi ML, Mintz A, Delbono O (2014) Type-1 pericytes accumulate after tissue injury and produce collagen in an organ-dependent manner. Stem Cell Res Ther 5(6):122. https://doi.org/10.1186/scrt512
Birbrair A, Zhang T, Wang ZM, Messi ML, Enikolopov GN, Mintz A, Delbono O (2013) Skeletal muscle pericyte subtypes differ in their differentiation potential. Stem Cell Res 10(1):67–84. https://doi.org/10.1016/j.scr.2012.09.003
Birbrair A, Zhang T, Wang ZM, Messi ML, Enikolopov GN, Mintz A, Delbono O (2013) Role of pericytes in skeletal muscle regeneration and fat accumulation. Stem Cells Dev 22(16):2298–2314. https://doi.org/10.1089/scd.2012.0647
Birbrair A, Zhang T, Wang ZM, Messi ML, Enikolopov GN, Mintz A, Delbono O (2013) Skeletal muscle neural progenitor cells exhibit properties of NG2-glia. Exp Cell Res 319(1):45–63. https://doi.org/10.1016/j.yexcr.2012.09.008
Birbrair A, Zhang T, Wang ZM, Messi ML, Mintz A, Delbono O (2013) Type-1 pericytes participate in fibrous tissue deposition in aged skeletal muscle. Am J Physiol Cell Physiol 305(11):C1098–C1113. https://doi.org/10.1152/ajpcell.00171.2013
Birbrair A, Zhang T, Wang ZM, Messi ML, Mintz A, Delbono O (2014) Pericytes: multitasking cells in the regeneration of injured, diseased, and aged skeletal muscle. Front Aging Neurosci 6:245. https://doi.org/10.3389/fnagi.2014.00245
Birbrair A, Zhang T, Wang ZM, Messi ML, Mintz A, Delbono O (2015) Pericytes at the intersection between tissue regeneration and pathology. Clin Sci 128(2):81–93. https://doi.org/10.1042/CS20140278
Birbrair A, Zhang T, Wang ZM, Messi ML, Olson JD, Mintz A, Delbono O (2014) Type-2 pericytes participate in normal and tumoral angiogenesis. Am J Physiol Cell Physiol 307(1):C25–C38. https://doi.org/10.1152/ajpcell.00084.2014
Birbrair A, Delbono O (2015) Pericytes are essential for skeletal muscle formation. Stem Cell Rev 11(4):547–548. https://doi.org/10.1007/s12015-015-9588-6
Prazeres PHDM, Turquetti AOM, Azevedo PO, Barreto RSN, Miglino MA, Mintz A, Delbono O, Birbrair A (2018) Perivascular cell αv integrins as a target to treat skeletal muscle fibrosis. Int J Biochem Cell Biol 99:109–113
Paiva AE, Lousado L, Guerra DAP, Azevedo PO, Sena IFG, Andreotti JP, Santos GSP, Goncalves R, Mintz A, Birbrair A (2018) Pericytes in the premetastatic niche. Cancer Res 78:2779–2786. https://doi.org/10.1158/0008-5472.CAN-17-3883
Silva WN, Leonel C, Prazeres PHDM, Sena IFG, Guerra DAP, Diniz IMA, Fortuna V, Mintz A, Birbrair A (2018) Role of Schwann cells in cutaneous wound healing. Wound repair and regeneration: official publication of the Wound Healing Society [and] the European Tissue Repair Society
Silva WN, Prazeres P, Paiva AE, Lousado L, Turquetti AOM, Barreto RSN, de Alvarenga EC, Miglino MA, Goncalves R, Mintz A, Birbrair A (2018) Macrophage-derived GPNMB accelerates skin healing. Exp Dermatol 27:630–635. https://doi.org/10.1111/exd.13524
Costa MA, Paiva AE, Andreotti JP, Cardoso MV, Cardoso CD, Mintz A, Birbrair A (2018) Pericytes constrict blood vessels after myocardial ischemia. J Mol Cell Cardiol 116:1–4. https://doi.org/10.1016/j.yjmcc.2018.01.014
Coatti GC, Frangini M, Valadares MC, Gomes JP, Lima NO, Cavacana N, Assoni AF, Pelatti MV, Birbrair A, de Lima ACP, Singer JM, Rocha FMM, Da Silva GL, Mantovani MS, Macedo-Souza LI, Ferrari MFR, Zatz M (2017) Pericytes extend survival of ALS SOD1 mice and induce the expression of antioxidant enzymes in the murine model and in IPSCs derived neuronal cells from an ALS patient. Stem Cell Rev 13:686–698. https://doi.org/10.1007/s12015-017-9752-2
Sena IFG, Prazeres P, Santos GSP, Borges IT, Azevedo PO, Andreotti JP, Almeida VM, Paiva AE, Guerra DAP, Lousado L, Souto L, Mintz A, Birbrair A (2017) Identity of Gli1+ cells in the bone marrow. Exp Hematol 54:12–16. https://doi.org/10.1016/j.exphem.2017.06.349
Hanoun M, Maryanovich M, Arnal-Estape A, Frenette PS (2015) Neural regulation of hematopoiesis, inflammation, and cancer. Neuron 86(2):360–373. https://doi.org/10.1016/j.neuron.2015.01.026
Arranz L, Sanchez-Aguilera A, Martin-Perez D, Isern J, Langa X, Tzankov A, Lundberg P, Muntion S, Tzeng YS, Lai DM, Schwaller J, Skoda RC, Mendez-Ferrer S (2014) Neuropathy of haematopoietic stem cell niche is essential for myeloproliferative neoplasms. Nature 512(7512):78–81. https://doi.org/10.1038/nature13383
Hanoun M, Zhang D, Mizoguchi T, Pinho S, Pierce H, Kunisaki Y, Lacombe J, Armstrong SA, Duhrsen U, Frenette PS (2014) Acute myelogenous leukemia-induced sympathetic neuropathy promotes malignancy in an altered hematopoietic stem cell niche. Cell Stem Cell 15(3):365–375. https://doi.org/10.1016/j.stem.2014.06.020
Salomoni P, Betts-Henderson J (2011) The role of PML in the nervous system. Mol Neurobiol 43(2):114–123. https://doi.org/10.1007/s12035-010-8156-y
Florean C, Schnekenburger M, Grandjenette C, Dicato M, Diederich M (2011) Epigenomics of leukemia: from mechanisms to therapeutic applications. Epigenomics 3(5):581–609. https://doi.org/10.2217/epi.11.73
Lengfelder E, Hofmann WK, Nowak D (2012) Impact of arsenic trioxide in the treatment of acute promyelocytic leukemia. Leukemia 26(3):433–442. https://doi.org/10.1038/leu.2011.245
Hu J, Liu YF, Wu CF, Xu F, Shen ZX, Zhu YM, Li JM, Tang W, Zhao WL, Wu W, Sun HP, Chen QS, Chen B, Zhou GB, Zelent A, Waxman S, Wang ZY, Chen SJ, Chen Z (2009) Long-term efficacy and safety of all-trans retinoic acid/arsenic trioxide-based therapy in newly diagnosed acute promyelocytic leukemia. Proc Natl Acad Sci U S A 106(9):3342–3347. https://doi.org/10.1073/pnas.0813280106
George B, Mathews V, Poonkuzhali B, Shaji RV, Srivastava A, Chandy M (2004) Treatment of children with newly diagnosed acute promyelocytic leukemia with arsenic trioxide: a single center experience. Leukemia 18(10):1587–1590. https://doi.org/10.1038/sj.leu.2403480
Kumazaki M, Ando H, Sasaki A, Koshimizu TA, Ushijima K, Hosohata K, Oshima Y, Fujimura A (2011) Protective effect of alpha-lipoic acid against arsenic trioxide-induced acute cardiac toxicity in rats. J Pharmacol Sci 115(2):244–248
Wang M, Sun G, Wu P, Chen R, Yao F, Qin M, Luo Y, Sun H, Zhang Q, Dong X, Sun X (2013) Salvianolic acid B prevents arsenic trioxide-induced cardiotoxicity in vivo and enhances its anticancer activity in vitro. Evid Based Complement Alternat Med 2013:759483–759489. https://doi.org/10.1155/2013/759483
Ame-Thomas P, Maby-El Hajjami H, Monvoisin C, Jean R, Monnier D, Caulet-Maugendre S, Guillaudeux T, Lamy T, Fest T, Tarte K (2007) Human mesenchymal stem cells isolated from bone marrow and lymphoid organs support tumor B-cell growth: role of stromal cells in follicular lymphoma pathogenesis. Blood 109(2):693–702. https://doi.org/10.1182/blood-2006-05-020800
Karnoub AE, Dash AB, Vo AP, Sullivan A, Brooks MW, Bell GW, Richardson AL, Polyak K, Tubo R, Weinberg RA (2007) Mesenchymal stem cells within tumour stroma promote breast cancer metastasis. Nature 449(7162):557–563. https://doi.org/10.1038/nature06188
Prantl L, Muehlberg F, Navone NM, Song YH, Vykoukal J, Logothetis CJ, Alt EU (2010) Adipose tissue-derived stem cells promote prostate tumor growth. Prostate 70(15):1709–1715. https://doi.org/10.1002/pros.21206
Kansy BA, Dissmann PA, Hemeda H, Bruderek K, Westerkamp AM, Jagalski V, Schuler P, Kansy K, Lang S, Dumitru CA, Brandau S (2014) The bidirectional tumor--mesenchymal stromal cell interaction promotes the progression of head and neck cancer. Stem Cell Res Ther 5(4):95. https://doi.org/10.1186/scrt484
Zhu W, Xu W, Jiang R, Qian H, Chen M, Hu J, Cao W, Han C, Chen Y (2006) Mesenchymal stem cells derived from bone marrow favor tumor cell growth in vivo. Exp Mol Pathol 80(3):267–274. https://doi.org/10.1016/j.yexmp.2005.07.004
Li W, Zhou Y, Yang J, Zhang X, Zhang H, Zhang T, Zhao S, Zheng P, Huo J, Wu H (2015) Gastric cancer-derived mesenchymal stem cells prompt gastric cancer progression through secretion of interleukin-8. J Exp Clin Cancer Res 34:52. https://doi.org/10.1186/s13046-015-0172-3
Hossain A, Gumin J, Gao F, Figueroa J, Shinojima N, Takezaki T, Priebe W, Villarreal D, Kang SG, Joyce C, Sulman E, Wang Q, Marini FC, Andreeff M, Colman H, Lang FF (2015) Mesenchymal stem cells isolated from human gliomas increase proliferation and maintain stemness of glioma stem cells through the IL-6/gp130/STAT3 pathway. Stem Cells 33(8):2400–2415. https://doi.org/10.1002/stem.2053
Guerra DAP, Paiva AE, Sena IFG, Azevedo PO, Silva WN, Mintz A, Birbrair A (2018) Targeting glioblastoma-derived pericytes improves chemotherapeutic outcome. Angiogenesis. https://doi.org/10.1007/s10456-018-9621-x
Nabha SM, dos Santos EB, Yamamoto HA, Belizi A, Dong Z, Meng H, Saliganan A, Sabbota A, Bonfil RD, Cher ML (2008) Bone marrow stromal cells enhance prostate cancer cell invasion through type I collagen in an MMP-12 dependent manner. Int J Cancer 122(11):2482–2490. https://doi.org/10.1002/ijc.23431
Funding
Alexander Birbrair is supported by a grant from Instituto Serrapilheira/Serra-1708-15285; a grant from Pró-reitoria de Pesquisa/Universidade Federal de Minas Gerais (PRPq/UFMG) (Edital 05/2016); a grant from National Institute of Science and Technology in Theranostics and Nanobiotechnology (CNPq/CAPES/FAPEMIG, Process No. 465669/2014-0); a grant from FAPEMIG [Rede Mineira de Engenharia de Tecidos e Terapia Celular (REMETTEC, RED-00570-16)]; and a grant from FAPEMIG [Rede De Pesquisa Em Doenças Infecciosas Humanas E Animais Do Estado De Minas Gerais (RED-00313-16)]; Erika Costa de Alvarenga is supported by a grant from FAPEMIG [Rede Mineira de Pesquisa e Inovação para Bioengenharia de Nanosistemas (RED-00282-16)]; Akiva Mintz is supported by the National Institute of Health (1R01CA179072-01A1) and by the American Cancer Society Mentored Research Scholar grant (124443-MRSG-13-121-01-CDD).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
de Alvarenga, E.C., Silva, W.N., Vasconcellos, R. et al. Promyelocytic leukemia protein in mesenchymal stem cells is essential for leukemia progression. Ann Hematol 97, 1749–1755 (2018). https://doi.org/10.1007/s00277-018-3463-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-018-3463-x