Abstract
Purpose
The ‘emborrhoid’ technique consists of the embolization of the hemorrhoidal arteries. The endovascular arterial occlusion is performed using coils placed in the terminal branches of the superior rectal arteries. The emborrhoid technique has been modeled after elective transanal Doppler-guided hemorrhoidal artery ligation which has been shown to be effective in hemorrhoidal disease. We report the first 14 cases of our experience with emborrhoid technique.
Materials and Methods
Fourteen patients with disabling chronic rectal bleeding were treated using the emborrhoid technique (3 women, 11 men). The stage of the hemorrhoidal disease was II (10 patients), III (3), and IV (1). This treatment was decided by a multidisciplinary team (proctologist, visceral surgeon, and radiologist). Seven patients underwent previous proctological surgery. Ten patients had coagulation disorders (anticoagulants or cirrhosis). Superior rectal arteries were embolized with pushable microcoils (0.018).
Results
Technical success of the embolization procedure was 100 %. Clinical success at 1 month was 72 % (10/14). Of the 4 patients who experienced rebleeding, two underwent additional embolization of the posterior rectal arteries with success. No pain or ischemic complications were observed in 13 patients. One patient experienced a temporary painful and edematous, perianal reaction.
Conclusion
Our case studies suggest that coil embolization of the superior rectal arteries is technically feasible, safe and well tolerated. Additional studies are needed to evaluate the efficacy of this new ‘emborrhoid’ technique in the management of hemorrhoidal disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
With a prevalence of 4–35 %, hemorrhoidal disease is the most common anorectal condition. One of the main chronic symptoms is rectal bleeding. Its recurrence can alter the quality of life and, more rarely, cause anemia. Pain is less common, only occurring in the event of a complication (congestive exacerbation, external hemorrhoidal thrombosis, fissures). The most common treatment involves hygiene and dietary measures, phlebotonics and/or non-surgical outpatient treatment (infrared photocoagulation, elastic band ligation). Surgical treatment is necessary in 10 % of cases [1]. The reference procedure is Milligan and Morgan’s open hemorrhoidectomy [2]. It consists of resecting the three hemorrhoidal cushions by ligating their arterial pedicle as high up as possible. Two less invasive techniques have been proposed. Circular-stapled anopexy (Longo procedure) consists of interrupting the terminal branches of the superior rectal arteries and resecting a ring of rectal mucosa [3]. Elective Doppler-guided hemorrhoidal artery ligation (DG-HAL) has been developed with the same objectives [4, 5].
Recently, Vidal et al. have described a new technique called “emborrhoid” for the treatment of chronic symptoms of hemorrhoid disease [6]. Emborrhoid consists of arterial occlusion of the superior rectal arteries (SRA) with coils. In the literature, few case reports have demonstrated the efficacy of embolization of the superior rectal arteries for life-threatening rectal bleeding of various origins [7–12].
Compared with DG-HAL, endovascular embolization has the enormous advantage of identifying all the hemorrhoidal arterial branches perfectly. This makes it possible to completely occlude all branches with certainty, which can noticeably improve the therapeutic results. In addition, the vascular approach avoids all anal and rectal trauma leading to a reduction in morbidity. The aim of this paper is to report the first 14 cases. We evaluate the feasibility and early morbidity of endovascular coil embolization of the SRA in the treatment of hemorrhoidal symptoms.
Materials and Methods
Fourteen patients with severe chronic rectal bleeding were treated using the emborrhoid technique (3 women, 11 men). The mean age was 57-years old (41–83). The stage of the hemorrhoidal disease was II (10 patients), III (3), and IV (1). The first 14 patients were treated after the decision of a multidisciplinary team (proctologist, visceral surgeon, and radiologist). These patients were not suitable for other medical or surgical treatments and suffered from severe rectal bleeding. The multidisciplinary team took into account the fact that in emergency situations rectal embolization with coils has been shown to be safe and effective [7–12]. The multidisciplinary team did not ask IRB approval for coil embolisation of the superior rectal artery as it was considered as “compassionate” treatment.
Seven patients previously underwent unsuccessful proctological surgery. For these 7 patients, our surgeons decided that redo surgery would be associated with a high risk of complications. Ten patients had severe coagulation disorders (six were under anticoagulants and four had cirrhosis). For these 10 fragile patients, our surgeons decided that surgery would be associated with a high risk of hemorrhage.
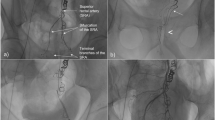
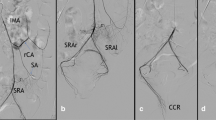
Embolizations (Figs. 1, 2, 3) were performed using a right femoral route after inserting a 5 Fr introducer sheath. The inferior mesenteric artery was catheterized using a Simmons catheter (radiofocus—Terumo). The superior rectal arteries were then catheterized with a rapid transit microcatheter (Cordis/Johnson & Johnson, Warren, NJ) or Progreat microcatheter (Radiofocus—Terumo). The coils used for the embolization were Nester 0.018″, 2 and 3 mm in diameter, and 3-cm long (Cook, Bloomington, IN).
Non-subtracted and subtracted arteriogram of the inferior mesenteric artery. A Catheterization of the inferior mesenteric artery with a Simmons catheter below the ostia of the left colic artery. B Opacification of the sigmoïdal arteries (white arrows) and of the proximal superior rectal branches (black arrows). C, D Non-subtracted and subtracted opacification of the SRAs: right, left and two posterior branches (white arrows)
The mean procedure time was 69 min (39–118 min). The average dose of contrast agent injected was 112 ml (88–143 ml). The average Dose-Area Product (DAP) was 62 Gy cm2 (22–149 Gy cm2).
Results
Technical success of the embolization procedure was 100 %. Clinical success was 72 % (10/14) with a follow-up of 2–13 months (mean 192 days). Clinical success was defined as lack of bleeding or insignificant amounts of bleeding that was well tolerated by the patients. For the first 6 patients, incomplete embolization (only right and left SRA) was performed in order to avoid ischemic complications. Due to rebleeding of 4 of these 6 patients, a complete embolization including right, left, and posterior SRA was performed for the eight following cases. No pain or ischemic complications were observed for these 8 patients.
Of the first 4 patients who experienced rebleeding, 2 patients (stage II and stage III) underwent additional embolization of the posterior rectal arteries, and 2 patients (stage II and stage III) refused additional treatment. Of the 2 patients who underwent additional embolization of the posterior rectal arteries, one had clinical success, and the other experienced rebleeding at 1 month. A third embolization was performed on two small remaining arteries leading to a complete cessation of rectal bleeding. Following this last embolization the patient had a painful, edematous, perianal reaction. This is a known benign side-effect of DG-HAL. It indicates the efficacy of the arterial occlusion, and is explained by temporary redistribution of blood flow. The patient was treated with non-steroidal anti-inflammatory drugs and symptoms disappeared after 2 weeks. With the exception of this patient, no pain or ischemic complications were observed in the 13 other patients.
Discussion
Ten percent of patients with hemorrhoidal disease undergo surgical treatment [1]. Today, the reference technique is still Milligan and Morgan’s open hemorrhoidectomy [2]. Since the 1990s, new surgical procedures have aimed to minimize pain and to ensure a rapid return to social and professional activities, as well as reduce the cost of treatment. Circular-stapled anopexy was described by Antonio Longo in 1995 for treating hemorrhoidal disease [3]. Meta-analyses have reported that circular-stapled anopexy reduces the duration of surgery and the mean length of hospitalization [13–15]. Pain is less intense and disappears more quickly than classic operating techniques. However, rates of recurrence are higher, exceeding 10 % [14–16]. Complications following Milligan and Morgan’s or Longo’s procedure are estimated at 15–20 % of cases depending on the study [17–19]. Complications are usually non-specific and benign: hemorrhagic complications (4–17 %), acute urine retention (0.3–22 %), stenosis (0.8–20 %), fecaloma, fissures, anal incontinence, exudation, delayed healing, and abscess. Rare but nevertheless severe complications have been reported following stapled circular anopexy (rectal perforation, retropneumoperitoneum, retroperitoneal sepsis, rectal stenosis, rectovaginal fistula, and peritonitis) [20]. Transanal DG-HAL, first reported in 2005, was developed to provide minimally invasive surgery [4]. This technique consists of Doppler-guided ligation of the terminal branches of the SRA in order to reduce the arterial supply to the hemorrhoids. No tissue resection is necessary, unlike with the other techniques. This method, comparable to the elastic band ligations performed blind for several decades, is effective in internal hemorrhoidal disease where there is no prolapse. Several descriptive studies [20–25] have reported a short-term efficacy rate of 90 %, and long-term efficacy of 70–92 %. Post-operative pain was present in 1–6 % of cases. It was usually relieved by non-opioid analgesics. The rate of complications was low (2–12 %), with rectal bleeding at 4.3 %, hemorrhoidal thrombosis at 1.8 %, fissures at 0.8 %, and acute urine retention at 0.7 %.
Due to the miniaturization of embolization technology, occlusion of the SRA can be performed via the endovascular route. There are many benefits of endovascular treatment including complete visualization of all the branches of SRAs and anastomoses with middle and inferior rectal arteries. With DG-HAL, it is possible that not all arteries are detected, which can lead to incomplete treatment especially if there are anastomoses (Fig. 4). Embolization eliminates the risk of direct anorectal trauma.
The embolization procedure is technically easy to perform with regular microcatheters and inexpensive coils. The possible complications are related to the femoral puncture and to a potential rectal ischemia. The risk of ischemia is limited by the use of coils which lead to a non-distal embolization. In our study, no patients experienced ischemia. In order to avoid ischemia, we completed partial embolization in the first 6 patients. Partial embolization leads to rebleeding in four of these cases. Consequently, complete embolization was performed for the following cases and no significant rebleeding or ischemia occurred. In patients who had previous rectal surgery, we found that the arterial vascular network of the rectum is more developed with more anastomoses. We can hypothesize that patients without previous rectal surgery are better candidates for “emborrhoid” treatment.
At this point, only compassionate patients have been treated. But we hypothesize that the best candidate for emborrhoid is a patient who suffers from rectal bleeding without major hemorrhoidal prolapsus (stage II). Emborrhoid could be an ideal first line treatment for younger active patient who seek a minimally invasive outpatient procedure (without direct anorectal manipulations).
We believe that rectal bleeding occurs when venous hemorrhoidal pressure reaches a certain threshold. Embolisation may decrease the arterial flow significantly leading to a decrease of the venous pressure below this threshold. This hypothesis may explain the positive clinical results observed in our study. Furthermore, the maintained flow from the anastomoses with middle and inferior rectal arteries prevents ischemic complications. Some additional studies are needed to confirm this hypothesis.
This is the first study that describes embolization of the SRA for chronic symptoms of hemorrhoidal disease. Although the sample size of the study and the follow-up are limited, results of the emborrhoid technique are promising.
Coil embolization of the SRAs is technically feasible, safe, and well tolerated. Results suggest that coil embolisation should be as complete as possible in order to avoid rebleeding. Additional studies are needed to evaluate the efficacy and safety of this new ‘emborrhoid’ technique in the management of hemorrhoidal disease as an alternative to surgical treatment.
Abbreviations
- DG-HAL:
-
Elective Doppler-guided hemorrhoidal artery ligation
- SRA:
-
Superior rectal artery
References
Madoff RD, Fleshman JW (2004) American Gastroenterological Association technical review on the diagnosis and treatment of hemorrhoids. Gastroenterology 126(5):1463–1473
Milligan ET, Morgan CN, Jones LE, Officer R (1937) Surgical anatomy of the anal canal and operative treatment of haemorrhoids. Lancet:119–24
Longo A (1998) Treatment of hemorrhoidal disease by reduction of mucosa and hemorrhoidal prolapse with circular stapling device: a new procedure. 6th world congress of endoscopic surgery. Bologna: Monduzzi Editore: 777-84
Scheyer M, Antonietti E, Rollinger G, Mall H et al (2006) Doppler-guided hemorrhoidal artery ligation. Am J Surg 191(1):89–93
Giordano P, Overton J, Madeddu F, Zaman S et al (2009) Transanal hemorrhoidal dearterialization: a systematic review. Dis Colon Rectum 52(9):1665–1671
Vidal V, Louis G, Bartoli JM, Sielezneff Y (2014) Embolization of the hemorrhoidal arteries (the emborrhoid technique): a new concept and challenge for interventional radiology. Diagn Interv Imaging 95:307–315
Berczi V, Gopalan D, Cleveland TJ (2008) Embolization of a hemorrhoid following 18 hours of life-threatening bleeding. Cardiovasc Interv Radiol 31:183–185
Baig MK, Lewis M, Stebbing JF et al (2003) Multiple microaneurysms of the superior hemorrhoidal artery: unusual recurrent massive rectal bleeding: report of a case. Dis Colon Rectum 46:978–980
Silver A, Bendick P, Wasvary H (2005) Safety and efficacy of superselective angioembolization in control of lower gastrointestinal hemorrhage. Am J Surg 189:361–363
Dobson CC, Nicholson AA (1999) Treatment of rectal hemorrhage by coil embolization. Cardiovasc Interv Radiol 22:143–146
Morar KN, Syed MI, Patel JK et al (2006) Embolization of middle hemorrhoidal artery in the management of life-threatening rectal bleeding. Cardiovasc Interv Radiol 29:128–129
Pichon N, Francois B, Pichon-Lefievre F et al (2005) Embolization of rectal arteries: an alternative treatment for hemorrhagic shock induced by traumatic intrarectal hemorrhage. Cardiovasc Interv Radiol 28:515–517
Sutherland LM, Burchard AK, Matsuda K, Sweeney JL et al (2002) A systematic review of stapled hemorrhoidectomy. Arch Surg 137(12):1395–1406
Nisar PJ, Acheson AG, Neal KR, Scholefield JH (2004) Stapled hemorrhoidopexy compared with conventional hemorrhoidectomy: systematic review of randomized, controlled trials. Dis Colon Rectum 47(11):1837–1845
Basdanis G, Papadopoulos VN, Michalopoulos A, Apostolidis S et al (2005) Randomized clinical trial of stapled hemorrhoidectomy vs open with ligasure for prolapsed piles. Surg Endosc 19:235–239
Bikhchandani J, Agarwal PN, Kant R, Malik VK (2005) Randomized controlled trial to compare the early and mid-term results of stapled versus open hemorrhoidectomy. Am J Surg 189(1):56–60
Sielezneff I, Salle E, Lécuyer J, Brunet CH et al (1997) Morbidité postopératoire précoce après hémorroïdectomie selon la technique de Milligan et Morgan. Une étude rétrospective de 1 134 cas. J Chir 134(5–6):243–247
Senagore AJ, Singer M, Abcarian H, Fleshman J et al (2004) A prospective, randomized, controlled multicenter trial comparing stapled hemorrhoidopexy and Ferguson hemorrhoidectomy: perioperative and 1-year results. Dis Colon Rectum 47(11):1824–1836
Racalbuto A, Aliotta I, Corsaro G, Lanteri R et al (2004) Hemorrhoidal stapler prolapsectomy versus Milligan-Morgan hemorrhoidectomy: a long-term randomized trial. Int J Colorectal Dis 19(3):239–244
Faucheron JL, Gangner Y (2008) Doppler-guided hemorrhoidal artery ligation for the treatment of symptomatic hemorroids: early and 3-year follow-up results in 100 consecutive patients. Dis Colon Rectum 51(6):945–949
Pol RA, van der Zwet WC, Hoornenborg D, Makkinga B et al (2010) Results of 244 consecutive patients with hemorrhoids treated with Doppler-guided artery ligation. Dig Surg 27(4):279–284
Greenberg R, Karin E, Avital S, Skornick Y et al (2006) First 100 case with Doppler-guided hemorrhoidal artery ligation. Dis Colon Rectum 49(4):485–489
Wallis de Vries BM, van der Beek ES, de Wijkerslooth LR, van der Zwet WC et al (2007) Treatment of grade 2 and 3 hemorrhoids with Doppler-Guides hemorrhoidal artery ligation. Dig Surg 24(6):436–440
Wałega P, Scheyer M, Kenig J, Herman RM et al (2008) Two-center experience in the treatment on hemorrhoidal disease using Doppler-guided hemorrhoidal artery ligation: functional results after 1-year follow-up. Surg Endosc 22(11):2379–2383
Szmulowicz UM, Gurland B, Garofalo T, Zutshi M (2011) Doppler-guided hemorrhoidal artery ligation: the experience of a single institution. J Gastrointest Surg 15(5):803–808
Conflict of Interest
Vidal V, Sapoval M, Sielezneff Y, De Parades V, Tradi F, Louis G, Bartoli JM, and Pellerin O declare that they have no conflicts of interest related to this paper.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
Statement of Human and Animal Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vidal, V., Sapoval, M., Sielezneff, Y. et al. Emborrhoid: A New Concept for the Treatment of Hemorrhoids with Arterial Embolization: The First 14 Cases. Cardiovasc Intervent Radiol 38, 72–78 (2015). https://doi.org/10.1007/s00270-014-1017-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-014-1017-8