Abstract
We report a case of concurrent rectus sheath and psoas hematomas in a patient undergoing anticoagulant therapy, treated by transcatheter arterial embolization (TAE) of inferior epigastric and lumbar arteries. Computed tomography (CT) demonstrated signs of active bleeding in two hematomas of the anterior and posterior abdominal walls. Transfemoral arteriogram confirmed the extravasation of contrast from the right inferior epigastric artery (RIEA). Indirect signs of bleeding were also found in a right lumbar artery (RLA). We successfully performed TAE of the feeding arteries. There have been few reports in the literature of such spontaneous hemorrhages in patients undergoing anticoagulation, successfully treated by TAE.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Spontaneous extra-peritoneal hematomas could be common and sometimes life-threatening conditions in patients undergoing anticoagulation therapy [1, 2, 3]. Commonly these hematomas originate in the context of the muscles of the anterior abdominal wall and of the psoas, and rarely these are located in both sites [4]. We present a case of concurrent spontaneous hematomas of the rectus sheath and psoas muscle in a patient undergoing anticoagulation therapy, with severe hemorrhagic shock, treated by TAE of inferior epigastric and lumbar arteries.
Case Report
A 67-year-old male presented with acute pain and palpable mass in the lower abdominal. He had a retroperitoneal bleeding 2 years ago during anticoagulation therapy that was treated conservatively. He had been admitted 7 days previously because of a suspected pulmonary thromboembolism, treated with anticoagulant therapy. The patient reported that the onset of the pain followed exertion. Physical and ultrasound (US) examination revealed a smooth mass which was present in the right lower abdomen. Laboratory findings were as follows: hemoglobin, 12.0 g/dl; hematocrit, 34.3%; red blood cell count, 4,800,000/mm3; white blood cell count, 9,800/mm3. The patient was then treated conservatively.
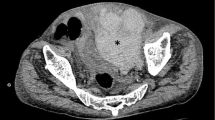
However, in the next 48 hours the symptoms worsened and the hematocrit level decreased by 20 points. Emergency enhanced CT (slice thickness of 5 mm, table speed of 7.5 mm and Pitch 1.5 after iv administration of 140 ml of contrast medium at a rate of 3 ml/sec) showed a smooth-shaped mass in the layers of the anterior abdominal wall, enlarging the normal morphology of the right rectus abdominis muscle, with signs of active bleeding (Fig. 1). The CT scan also showed another mass with the same characteristics, in the context of the right psoas muscle (Fig. 1). The patient underwent transfemoral angiography that disclosed direct signs of bleeding from the RIEA (Figs. 2,3,4). Abnormal morphology of a RLA was also detected (Fig. 5). Both arteries were embolized by using microcatheter (0.018 Fast-Tracker, Target Therapeutics, Boston Scientific, Natick, USA) and microcoils (size 3 × 30 mm Cook McReye, William Cook Denmark, Europe) (two for the epigastric and one for the lumbar artery) (Fig. 4, 6). The patient was discharged 5 days later and is still doing well after 9 month follow-up.
Discussion
The popular use of anticoagulant therapy in the pharmacological management of multiple conditions increases the rate of spontaneous hematomas [2]. The rectus sheath and the psoas muscles represent the most common sites of spontaneous bleeding in patients undergoing anticoagulation therapy [1, 3, 5]. These hematomas originate from tears in muscle fibers and are rarely bilateral [6]. Other rare sites of bleeding are the mediastinum or intramural visceral sites [1, 2, 7, 8, 9]. Small vessel arteriosclerosis [10], or related phenomenon to a thrombotic genesis involving the adrenal glands, may or may not correlate with the presence of heparin-induced immune microangiopathy [11]; they are the most accepted pathogenetic processes. Radiological evaluation, i.e., US or CT examination, in association with clinical history, symptomatology (pain, blood loss, hypotension and ecchymosis), play a basic role in the differential diagnosis and preoperative localization of rectus sheath or psoas hematomas [1, 3, 4, 12].
In hemodynamically stable conditions, the common management currently continues to be conservative (suspension of anticoagulation treatment, correction of the anticoagulation state, volume resuscitation, and supportive measures) [13, 14, 15]. In uncontrollable hemodynamic patients, surgical intervention has been considered the only option [16], although it is severely limited by the inability to localize or control the bleeding vessel(s). In case of pain related to the enlargement of psoas district, percutaneous decompression could also be indicated [17].
The role of TAE in the treatment of abdominal wall hematomas has not been stated. As reported by Sharafuddin et al. [18], this is likely because the common belief is that this entity is caused by diffuse microvascular pathology; hence, angiography is seldom requested [18]. Only 10 cases of TAE for spontaneous bleeding from abdominal wall arteries in patients undergoing anticoagulant therapy have been reported [12, 18, 19, 20, 21]. In 9 cases only an artery was embolized as the main source of bleeding (epigastric arteries n = 2, lumbar arteries n = 6, and deep circumflex iliac artery n = 1); in 1 case different arteries were embolized (inferior epigastric, deep and superficial circumflex iliac arteries). There is another report of TAE of the inferior epigastric artery supplying a rectus sheath hematoma in a patient with anticoagulant therapy, however, the hemorrhage could not be considered “spontaneous” because it was secondary to a percutaneous biopsy of an abdominal lymphoadenopathy [22]. Coils were used in 6 cases [18, 19], microcoils plus n-butyl cyanoacrylate in 1 case [21], particles in 2 [12], and in 1 reported case the used material was not indicated [20]. In our case we used microcoils agreeing with the theory of Sharafuddin et al. Thus, because a part of the standard advantages (radiopacity, accuracy, and safer deployment), coils or microcoils are able to pack the entire length of the major supplying vessel(s), preventing retrograde filling from collaterals; this is probably due to the fact that the bleeding at the rectus sheath or psoas muscle is often multifocal and involves complex collateral pathways [18]. In our case, the unstable hemodynamic conditions of the patient and the presence of active bleeding signs at CT indicated the use of angiography and the subsequent successful embolization.
References
JA Edlow P Juang S Margulies J Burstein (1999) ArticleTitleRectus sheath hematoma Ann Emerg Med 34 671–675 Occurrence Handle1:STN:280:DC%2BD3c%2FgsVGhuw%3D%3D Occurrence Handle10533018
InstitutionalAuthorNameThe Columbus investigators (1997) ArticleTitleLow-molecular-weight heparin in the treatment of patients with venous thromboembolism N Engl J Med 337 657–662
G Marquardt S Barduzal Angles F Leheta V Seifert (2002) ArticleTitleSpontaneous haematoma of the iliac psoas muscle: a case report and a review of the literature Arch Orthop Trauma Surg 122 109–111 Occurrence Handle10.1007/s004020100310 Occurrence Handle1:STN:280:DC%2BD387ks1WnsQ%3D%3D Occurrence Handle11880914
JD Berna G Guirao V Garcia Medina J Garcia Medina (1996) ArticleTitleRectus sheath hematoma: diagnostic classification by CT Abdom Imaging 21(1 62–64
CE Ray AC Wilbur (1993) ArticleTitleCT diagnosis of concurrent hematomas of the psoas muscle and rectus sheath: case reports and review of anatomy, pathogenesis and imaging Clin Imaging 17 22–26 Occurrence Handle10.1016/0899-7071(93)90007-A Occurrence Handle8439839
E Niakan JE carbone M Adams FM Schroeder (1991) ArticleTitleAnticoagulants, iliopsoas hematoma and femoral nerve compression Am Fam Physician 44(6 2100–2102
G Di Pasquale V Salpietro M Boaron (1990) ArticleTitleSpontaneous mediastinal hematoma during therapy with oral anticoagulation G Ital Cardiol 20 972–975 Occurrence Handle1:STN:280:By6B3MnktVU%3D Occurrence Handle2090537
M Marco AJ Guy (1999) ArticleTitleRetroperitoneal haematoma and small bowel intramural haematoma: a complication caused by warfarin and miconazole interaction Int J Oral Maxillofac Surg 27 485
SN Cullen RW Chapman (1999) ArticleTitleDissecting intramural haematoma of the oesophagus exacerbated by heparin therapy QJM 92 972–975 Occurrence Handle10.1093/qjmed/92.2.123
GM Torres JG Cernigliano PL Abbitt (1995) ArticleTitleIliopsoas compartment: normal anatomy and pathologic processes Radiographics 15 1285–1297 Occurrence Handle1:STN:280:BymC2Mbpslw%3D Occurrence Handle8577956
C Di Rosa S Venora N Monterosso NM La Spada S Viola (1997) ArticleTitleRetroperitoneal hematoma during heparin therapy. Comments on 3 cases Minerva Chir 52(4 493–497
SD Qanadli M El Hajjam F Mignon F Bruckert S Chagnon P Lacombe (1999) ArticleTitleLife-threatening spontaneous psoas haematoma treated by transcatheter arterial embolization Eur Radiol 9 1231–1234 Occurrence Handle10.1007/s003300050824 Occurrence Handle1:STN:280:DyaK1Mzks1egsA%3D%3D Occurrence Handle10415268
Z Sasson I Mangat KA Peckham (1996) ArticleTitleSpontaneous iliopsoas hematoma in patients with unstable coronary syndromes receiving intravenous heparin in therapeutic doses Can J Cardiol 12 490–494 Occurrence Handle1:STN:280:BymB2c%2FjvFI%3D Occurrence Handle8640595
DM Sherer AK Dayal BM Schwartz R Oren O Abulafia (1999) ArticleTitleExtensive spontaneous retroperitoneal hemorrhage: an unusual complication of heparin anticoagulation during pregnancy J Matern Fetal Med 8 196–199 Occurrence Handle10.1002/(SICI)1520-6661(199907/08)8:4<196::AID-MFM12>3.3.CO;2-P Occurrence Handle1:STN:280:DyaK1Mzjt12guw%3D%3D Occurrence Handle10406306
JD Berna I Zuazu M Madrigal V Garcia Medina C Fernandez F Guirado (2000) ArticleTitleConservative treatment of large rectus sheath hematoma in patients undergoing anticoagulant therapy Abdom Imaging 25 230–234 Occurrence Handle10.1007/s002610000007 Occurrence Handle1:STN:280:DC%2BD3czptFyhsQ%3D%3D Occurrence Handle10823439
BH Baker MS Baker (1980) ArticleTitleIndications for exploring the retroperitoneal space South Med J 73 969–970 Occurrence Handle1:STN:280:Bi%2BB2Mfnt1A%3D Occurrence Handle7403932
Rs Holscher FSS Leyten LFIJ Oudenhoven JBCM Puylaert (1997) ArticleTitlePercutaneous decompression of an iliopsoas hematoma Abdom Imaging 22 114–116 Occurrence Handle10.1007/s002619900154 Occurrence Handle1:STN:280:ByiC2MzksF0%3D Occurrence Handle9000371
MJ Sharafuddin KJ Andresen S Sun E Lang MS Stecker LA Wibbenmeyer (2001) ArticleTitleSpontaneous extraperitoneal hemorrhage with hemodynamic collapse in patients undergoing anticoagulation: management with selective arterial embolization J Vasc Interv Radiol 12 1231–1234 Occurrence Handle1:STN:280:DC%2BD3MrjvFajuw%3D%3D Occurrence Handle11585893
EA Kalinowski SO Trerotola (1998) ArticleTitlePost-catheterization retroperitoneal hematoma due to spontaneous lumbar arterial hemorrhage Cardiovasc Intervent Radiol 21 337–339
DJ Kastan TH Burke (2000) ArticleTitleImages in clinical medicine: retroperitoneal hemorrhage N Engl J Med 9 702 Occurrence Handle10.1056/NEJM200003093421005
T Katsumori T Nakajima (1998) ArticleTitleA case of spontaneous hemorrhage of the abdominal wall caused by rupture of a deep iliac circumflex artery treated by transcatheter arterial embolization Eur Radiol 8 550–552 Occurrence Handle10.1007/s003300050432 Occurrence Handle1:STN:280:DyaK1c3jslyhtw%3D%3D Occurrence Handle9569320
JR Zack H Ferral D Postoak M Wholey (2001) ArticleTitleCoil embolization of rectus sheath hemorrhage J Trauma 51(4 793–795
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Basile, A., Medina, J., Mundo, E. et al. Transcatheter Arterial Embolization of Concurrent Spontaneous Hematomas of the Rectus Sheath and Psoas Muscle in Patients Undergoing Anticoagulation. CVIR 27, 659–662 (2004). https://doi.org/10.1007/s00270-004-0192-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-004-0192-4