Abstract
Introduction
While there is evidence of obstetric and neonatal outcomes from non-obstetric surgery during pregnancy, surgery during the third trimester of gestation has not been evaluated as a prognostic factor for those outcomes. The objective of this study was to determine whether appendectomies during the third trimester are associated with adverse neonatal outcomes, in comparison with appendectomies during the first two trimesters, based on national administrative data in Colombia.
Methods
A retrospective cohort study was performed using administrative health records. It included all women who had live births and who underwent an appendectomy during any stage of pregnancy, between the years 2011 and 2016, and who belonged to Colombia’s contributory health system. The main outcome was preterm birth. Birth weight and 1-min and 5-min Apgar scores were also measured, as well as outcomes used to identify neonatal near-miss cases. Propensity score matching was used in order to balance baseline characteristics (age, weeks of gestation, obstetric comorbidity index, and region and year the procedure was performed). Relative risks were estimated with Poisson regressions.
Results
This study included a total of 2507 women in Colombia’s contributory health system who underwent an appendectomy during pregnancy. Appendectomy was performed on 885 women (35.30%) in their first trimester, 1205 women (48.07%) in their second trimester, and 417 women (16.63%) in their third trimester. For the entire population, the preterm birth rate was 11.85 per 100 appendectomies. With the matched sample, this study found that women in their third trimester had a 1.65 greater risk of preterm birth [95% CI, 1.118–2.423], a 3.43 greater risk of birth at gestational ages < 33 weeks [95% CI, 1.363 to 8.625], 2.083 greater risk of weight under 1750 g [95% CI, 1.056–4.109], and a mean difference of − 0.247 [95% CI, − .382 to − .112] in the 1-min Apgar score and − .168a [95% CI, − .276 to − .060] in the 5-min Apgar. No differences were found in birth weight or Apgar scores < 7.
Conclusions
In Colombia’s contributory health system, women who undergo appendectomies in their third trimester have a greater risk of preterm birth, birth weight under 1750 g, birth at gestational ages less than 33 weeks, and decreased 1-min and 5-min Apgar scores.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Appendectomy is the most common non-obstetric surgery to be performed on pregnant women. It is estimated that 1 in 500–2000 women present acute appendicitis during pregnancy [1,2,3]. Due to physiological changes during pregnancy, reaching an early diagnosis and providing proper treatment can be challenging [4, 5]. This population is also of special interest because this surgery and its pathology pose a risk of adverse outcomes for the infant [6].
Preterm birth is an important adverse outcome in terms of neonatal morbidity and mortality. It defines the development of several complications, including neurodevelopmental, gastrointestinal, and pulmonary disorders, as well as death [7, 8]. These complications result in high socioeconomic costs for health systems and can even be an indicator of economic development [9,10,11]. It is known that the population of pregnant women who undergo appendectomies has poorer outcomes than the population that that is not operated on during pregnancy, as shown by the incidence of preterm birth, low birth weight, and low Apgar scores [12]. Nevertheless, no evidence exists that identifies the trimester of pregnancy as a prognostic factor for neonatal outcomes.
Colombia is a middle-income, developing country with an insurance-based health system that covers 97% of the population. It has two financing systems: contributory and subsidized. The contributory system serves those who have formal employment, and the subsidized system serves the lower-income population. Each of these financing systems covers roughly 50% of the population, thereby reaching a total coverage of 97% of the Colombian population [13, 14]. The set of health benefits provided by these two systems is the same for the entire population, regardless of the system to which one belongs. Although the Colombian health system has been operating since the 1990s, this is the first study to report outcomes for pregnant women who undergo appendectomies.
The aim of this study was to compare the association between birth outcomes, particularly preterm birth, and appendectomies performed during the third trimester of pregnancy versus those performed during the first two trimesters.
Methods
Type of study and source of information
This was a retrospective cohort study based on administrative claims data, using the UPC sufficiency database from Colombia’s Ministry of Health and birth certificates in Colombia. The UPC database contains information that insurers in Colombia’s health system send to the Ministry of Health in order to estimate the premiums that the system recognizes for each individual in the contributory regime. This database is highly standardized and contains detailed information about all the services used by the contributory system, including type of service provided, ICD codes, date of service, municipality, sex, age, insurer, and service provider. The birth certificate database contains information about all births in the country, including the birth itself, the mother, and the child. The databases were de-identified, and the study was approved by the ethics committee at the National University of Colombia’s School of Medicine (Acta No. 003-031-19, dated February 22, 2019).
Population
All women were included who belonged to Colombia’s contributory health system, who had live births, and had undergone an appendectomy during any stage of pregnancy between the years 2011 and 2016. The likely date of conception and whether the mother had an appendectomy during pregnancy were determined based on gestational age at birth, as registered in the birth certificate database. Two cohorts were defined: (1) women who had an appendectomy in their third trimester of pregnancy (exposed cohort) and (2) women who had an appendectomy in their first or second trimester of pregnancy (non-exposed cohort).
Variables
The main outcome was preterm birth, defined as birth at gestational ages < 37 weeks [15]. The weight of the newborn was also measured, as well as 1-min and 5-min Apgar scores. Pragmatic criteria for identifying neonatal near-miss cases were also measured based on Pileggi et al. [16], including: birth weight under 1750 g, 5-min Apgar score < 7, and birth at gestational ages < 33 weeks.
Control variables included mother’s age, comorbidities according to the recent obstetric comorbidities index [17, 18], laparoscopic appendectomy, appendectomy with peritoneal drainage, geographic region where the appendectomy was performed, and year it was performed. Obstetric comorbidities index includes the following comorbidities: alcohol abuse, asthma, cardiac valvular disease, chronic congestive heart failure, chronic ischemic heart disease, chronic renal disease, congenital heart disease, drug abuse, gestational hypertension, human immunodeficiency virus, mild / unspecified preeclampsia, multiple gestation, placenta praevia, pre-existing diabetes mellitus, pre-existing hypertension, previous cesarean delivery, pulmonary hypertension, severe pre-eclampsia, sickle cell disease, and systemic lupus erythematosus.
Statistical analysis
All of the variables mentioned were summarized descriptively for the entire population and for each cohort. Then, differences between the cohorts in the distribution of the variables that could have been confounders were evaluated based on the type of distribution of each variable and standardized differences.
In order to evaluate the association between appendectomy in the third trimester and preterm birth (as well as the other outcomes), propensity score (PS) matching was used to decrease confounding and selection bias, and to obtain unbiased estimators [19]. Each subject’s PS was calculated based on a logistic regression model, and clinical and demographic variables were included as predictors of exposure status. This model included above-mentioned confounders as well as the characteristics that presented statistical differences, according to the descriptive analysis. Subjects in the exposed cohort (appendectomy in the third trimester) were matched with subjects in the non-exposed cohort (appendectomy in the first or second trimester) using a 1:1 nearest neighbor matching without replacement.
Models with and without caliper were used to identify the most balanced model. Absolute standardized differences were used to evaluate the balance between cohorts in the matched sample, with a target value under 0.1 [20]. The association between appendectomy in the third trimester and the incidence of preterm birth (as well as the other dichotomous outcomes) was estimated with relative risks (RR) based on Poisson regressions, in accordance with Knol et al. [21]. For the continuous outcomes, linear regression was used and mean differences were estimated as a measure of effect. Confidence intervals of 95% were estimated with robust standard errors. All the analyses were performed with Stata 14 (StataCorp LP, College Station, TX).
Results
Descriptive analysis
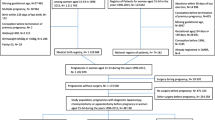
A total of 231,570 appendectomies were performed in Colombia’s contributory system between 2011 and 2016, and 115,862 (50.01%) of those were performed on women. During this same period, 3,552,093 birth certificates were issued in Colombia, 1,529,807 of which corresponded to the contributory regime. A total of 2507 women in Colombia’s contributory system underwent appendectomies during pregnancy between the years 2011 and 2016 (Fig. 1).
A total of 885 women (35.30%) underwent appendectomy during their first trimester of pregnancy, 1205 (48.07%) during their second trimester, and 417 (16.63%) during their third trimester. The average age of all the women in the sample was 26.52 ± 5.88 years, and the majority were between the ages of 18 and 35 years (2120 women, or 84.56%). The frequency was 4.51% for laparoscopic appendectomy and 19.63% for peritoneal drainage. With regard to the obstetrics index, 60.35% of the women had an index of zero and only 8.50% had an index over 3 (Table 1). Differences between regions were found. For example, more surgeries were performed in Bogota (27.6%) than in the other regions in Colombia, followed by the eastern region (24.25%). When comparing the baseline characteristics of the two cohorts with the unmatched sample, statistically significant differences were found between the proportion of laparoscopic appendectomies and appendectomies requiring peritoneal drainage (Table 1). A larger proportion of women who underwent surgery during their first or second trimester of pregnancy had laparoscopic appendectomies. And a larger proportion of women who were operated on during their third trimester had appendectomies requiring peritoneal drainages. These differences could confound the association between exposure and clinical outcomes.
Unadjusted outcomes
Table 2 shows unadjusted outcomes for the total sample and for the two cohorts, as well as average birth weight and average 1-min and 5-min Apgar scores, and rates for: preterm birth per 100 surgeries, birth at gestational ages <33 weeks, birth weight under 1750 g, and 5-min Apgar score <7. The unadjusted comparison of the two cohorts resulted in an RR over 1 against appendectomy during the third trimester, which suggests that undergoing this surgery in the third trimester is a risk factor for adverse outcomes in the newborn. Nevertheless, these results need to be adjusted due to the existence of possible confounding factors, as shown by the imbalance in the baseline characteristics presented in Table 1.
Propensity score matching
A matching analysis was performed in order to balance the baseline characteristics of the patients in the two cohorts. Two propensity score models were generated. The purpose of the first model (PSM 1) was to determine the association between appendectomy in the third trimester and the incidence of preterm birth and birth at gestational ages under 33 weeks. The variables included in the estimation of the propensity score were: age, obstetric comorbidity index, laparoscopic appendectomy, complicated appendectomy, geographic region, and year the surgery was performed. The matching algorithm with the most balanced baseline characteristics had a caliper of 0.05. As can be seen in Table 3, PSM 1 corrected the imbalance that existed in the variables related to laparoscopic appendectomy, complicated appendectomy, and surgeries in the year 2015. The final matched sample included all the exposed subjects in the total sample (417), and therefore, the quality of the matching is considered to be high [20]. With the matched sample, the Poisson model showed that surgeries in the third trimester of pregnancy had a 1.65 times greater risk of preterm birth than those performed in the other two trimesters (p < 0.001), and a 3.43 greater risk of birth at gestational ages < 33 weeks (p < 0.001) (Table 4).
Gestational age at birth is associated with birth weight and Apgar scores [22]. A second propensity score model (PSM 2) was generated in order to determine the association between appendectomy in the third trimester of pregnancy and outcomes related to birth weight and the Apgar score, independently of gestational age. This model included the same predictor variables for exposure as those in PSM 1, in addition to gestational age at birth. Thus, with the matching by PSM 2, each exposed individual had a match in the non-exposed cohort with the same gestational age at birth. In addition to the imbalance found with PSM 1, Table 3 shows that, with PSM 2, the absolute standard difference for the variable gestational age at birth was 0.22 with the sample before matching, which decreased to 0.05 when corrected with matching. With the matched sample with PSM 2, the risk of birth weight under 1750 g was 2.08 times greater for appendectomy in the third trimester than for the other two trimesters. And although no differences were found in the rate of the 5-min Apgar score < 7, the average 1-min and 5-min Apgar scores were significantly lower for the exposed cohort.
Discussion
Acute appendicitis is the most common non-obstetric surgery for pregnant women [23]. One study showed that pregnant women were less likely to be diagnosed with acute appendicitis than non-pregnant women, and it reported a lower likelihood of making that diagnosis for women in their third trimester [24]. Systematic reviews of pregnant women have been designed to compare the effectiveness and safety of open versus laparoscopic appendectomy for the fetus as well as the mother [25,26,27,28,29]. Nevertheless, to our knowledge, the present cohort study is the first in the international literature to compare the association between neonatal outcomes at birth and appendectomy during the third trimester of pregnancy versus appendectomy during the other two trimesters. Most studies have focused on the comparison of the laparoscopic with open approach, association with negative appendectomies, other risk factors, diagnostic tests performance, and several case series, but none of them have asked about the trimester in which the appendectomy is performed [24,25,26,27,28,29].
Our study was performed in Colombia with women belonging to the contributory health system. It found that 2507 of those women who had live births underwent an appendectomy during pregnancy between the years 2011 and 2016. Although the main outcome was the preterm birth rate, this study included other outcomes that have been proposed as a means to identify high-risk newborns. It also used PSM techniques to reduce the confounding effect and selection bias involved in observational studies. This study found that women undergoing appendectomy in their third trimester have a 1.6 times greater risk of preterm birth than those in their first or second trimesters, and a 3.4 times greater likelihood of birth at gestational ages < 33 weeks. This increased risk is consistent with descriptive findings reported by Sadot et al. [30], who reported that preterm birth rates were higher during the third trimester, although without significant differences.
The overall preterm birth rate in our study was 11.85%, which was higher than reports by other studies. In a systematic review that included 28 studies, Walsh et al. determined the differences between laparoscopic and open appendectomy in this population of women. They found preterm birth rates of 2.1% for laparoscopic and 8.1% for open surgery, although the studies varied greatly [25]. Our study found a mean overall birth weight of 3.048 ± 11.05, which falls within the range reported in the literature (2810–3500 g) [26]. With regard to 1-min and 5-min Apgar scores, we found means of 8.27 ± 0.89 and 9.51 ± 0.75, respectively, which also falls within reported ranges. As mentioned previously, the studies found do not describe differences in outcomes by trimester, which makes a comparison impossible. It is worth mentioning that the weight and Apgar outcomes in our study were controlled by gestational age, that is, they are independent of that variable. With the adjustment mentioned earlier, we were able to conclude that of the pregnant women who underwent appendectomy, those who were operated on in their third trimester had an increased risk of birth weight under 1750 g and decreased mean 1-min and 5-min Apgar scores.
With regard to type of appendectomy, only 4.5% was laparoscopic, with the lowest proportion performed during the third trimester. While there continues to be controversy in the current literature regarding the advantages and disadvantages of the different types of procedures for each trimester, our study found that the use of laparoscopic surgery for pregnant women is uncommon in Colombia. The literature confirms that open procedures are preferable during the third trimester and laparoscopic procedures are preferable during the first trimester. In fact, some institutions consider the third trimester to be contraindicated for laparoscopy [30,31,32]. On the other hand, the Society of American Gastrointestinal and Endoscopic Surgeons asserts that pregnant patients can safely undergo laparoscopy in any trimester, with no significant risk to the mother or fetus [33, 34]. Our study suggests that appendectomy during the third trimester increases the risk of adverse outcomes at birth, regardless of which procedure is performed.
These differences between the third trimester and the other two trimesters can be explained by the physiological and mechanical changes that occur as pregnancy progresses [35, 36]. Moreover, the accuracy of the appendicitis diagnosis is known to decrease over the time of pregnancy. Therefore, the risk of adverse outcomes found by our study suggests that pregnant women with suspected appendicitis during their third trimester need more elaborate diagnostic analyses than during other trimesters.
The main limitation of this study was that it was not possible to control the various clinical variables that could affect the association with outcomes, given the retrospective nature of the source of the data, which was obtained from administrative records. With regard to preterm birth, in some cases there may be causes other than surgical intervention that could explain the results. Nevertheless, appendectomy appears to be a sufficient stimulus for triggering preterm birth [37, 38]. Another disadvantage of our study is that it was based solely on the population belonging to the contributory health system, whose socioeconomic conditions are higher than those of the population in the subsidized system. Therefore, the population in our study may have much better access to health services than the population in the subsidized health system. Nonetheless, the sample in this study was representative of the Colombian population and the data were highly standardized, thereby making them reliable. Finally, because appendectomy is a highly standardized procedure worldwide, we believe that these results could be generalized in other populations; however, studies in different contexts should be performed for assessment reproducibility of associations.
Conclusion
In conclusion, the findings by this study suggest that in Colombia’s contributory health system, women who undergo appendectomy during their third trimester have a higher risk than women in the other trimesters of preterm birth, birth at gestational ages <33 weeks, birth weight under 1750 g, and lower 1-min and 5-min Apgar scores. This association is independent of the obstetric comorbidities evaluated, age of the mother, gestational age at the time of surgery, and the use of laparoscopic surgery.
References
Pearl J, Price R, Richardson W, Fanelli R (2011) Guidelines for diagnosis, treatment, and use of laparoscopy for surgical problems during pregnancy. Surg Endosc 25(11):3479. https://doi.org/10.1007/s00464-011-1927-3
Augustin G, Majerovic M (2007) Non-obstetrical acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol 131(1):4–12. https://doi.org/10.1016/j.ejogrb.2006.07.052
Barber-Millet S, Bueno Lledó J, Granero Castro P, Gómez Gavara I, Ballester Pla N, García Domínguez R (2016) Update on the management of non-obstetric acute abdomen in pregnant patients. Cirugía Española (English Ed) 94(5):257–265. https://doi.org/10.1016/j.cireng.2016.05.001
Chawla S, Vardhan S, Jog SS (2003) Appendicitis during pregnancy. Med J Armed Forces India 59(3):212–215. https://doi.org/10.1016/S0377-1237(03)80009-6
Lotfipour S, Jason M, Liu VJ et al (2018) Latest considerations in diagnosis and treatment of appendicitis during pregnancy. Clin Pract Cases Emerg Med. https://doi.org/10.5811/cpcem.2018.1.36218
Aggenbach L, Zeeman GG, Cantineau AEP, Gordijn SJ, Hofker HS (2015) Impact of appendicitis during pregnancy: no delay in accurate diagnosis and treatment. Int J Surg 15:84–89. https://doi.org/10.1016/j.ijsu.2015.01.025
Behrman RE, Butler AS, Outcomes I of M (US) C on UPB and AH (2007) Committee on understanding premature birth and assuring healthy outcomes. National Academies Press, New York
Saigal S, Hoult LA, Streiner DL, Stoskopf BL, Rosenbaum PL (2000) School difficulties at adolescence in a regional cohort of children who were extremely low birth weight. Pediatrics 105(2):325–331. https://doi.org/10.1542/peds.105.2.325
Behrman RE, Butler AS, Outcomes I of M (US) C on UPB and AH (2007) Societal costs of preterm birth. National Academies Press, New York
Frey HA, Klebanoff MA (2016) The epidemiology, etiology, and costs of preterm birth. Semin Fetal Neonatal Med 21(2):68–73. https://doi.org/10.1016/j.siny.2015.12.011
Vogel JP, Chawanpaiboon S, Watananrun K et al (2016) Global, regional and national levels and trends of preterm birth rates for 1990 to 2014: protocol for development of World Health Organization estimates. Reprod Health 13:76. https://doi.org/10.1186/s12978-016-0193-1
Balinskaite V, Bottle A, Sodhi V et al (2017) The risk of adverse pregnancy outcomes following nonobstetric surgery during pregnancy: estimates from a retrospective cohort study of 6.5 million pregnancies. Ann Surg 266(2):260. https://doi.org/10.1097/SLA.0000000000001976
OECD (2015) OECD reviews of health systems: Colombia 2016. OECD. https://www.oecd-ilibrary.org/social-issues-migration-health/oecd-reviews-of-health-systems-colombia-2015_9789264248908-en
Merlano-Porras CA, Gorbanev I (2013) Health system in Colombia: a systematic review of literature. Rev Gerency Políticas Salud 12(24):74–86.
Althabe F, Howson CP, Kinney M, Lawn J, World Health Organization. Born Too Soon: the Global Action Report on Preterm Birth.
Pileggi-Castro C, Camelo JS Jr, Perdoná GC et al (2014) Development of criteria for identifying neonatal near-miss cases: analysis of two WHO multicountry cross-sectional studies. BJOG An Int J Obstet Gynaecol 121(s1):110–118. https://doi.org/10.1111/1471-0528.12637
Bateman BT, Mhyre JM, Hernandez-Diaz S et al (2013) Development of a comorbidity index for use in obstetric patients. Obstet Gynecol 122(5):957–965. https://doi.org/10.1097/AOG.0b013e3182a603bb
Metcalfe A, Lix L, Johnson J-A et al (2015) Validation of an obstetric comorbidity index in an external population. BJOG An Int J Obstet Gynaecol 122(13):1748–1755. https://doi.org/10.1111/1471-0528.13254
Abadie A, Imbens GW (2016) Matching on the estimated propensity score. Econometrica 84(2):781–807. https://doi.org/10.3982/ECTA11293
Austin PC (2009) Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 28(25):3083–3107. https://doi.org/10.1002/sim.3697
Knol MJ, Le Cessie S, Algra A, Vandenbroucke JP, Groenwold RHH (2012) Overestimation of risk ratios by odds ratios in trials and cohort studies: alternatives to logistic regression. CMAJ 184(8):895–899. https://doi.org/10.1503/cmaj.101715
Behnke M, Carter R, Hardt N, Eyler F, Cruz A, Resnick M (1987) The relationship of apgar scores, gestational age, and birthweight to survival of low-birthweight infants. Am J Perinatol 4(02):121–124. https://doi.org/10.1055/s-2007-999752
Andersen B, Nielsen TF (1999) Appendicitis in pregnancy, diagnosis, management and complications. Acta Obstet Gynecol Scand 78(9):758–762. https://doi.org/10.1034/j.1600-0412.1999.780903.x
Zingone F, Sultan AA, Humes DJ, West J (2015) Risk of acute appendicitis in and around pregnancy: a population-based cohort study from England. Ann Surg 261(2):332–337. https://doi.org/10.1097/SLA.0000000000000780
Walsh CA, Tang T, Walsh SR (2008) Laparoscopic versus open appendicectomy in pregnancy: a systematic review. Int J Surg 6(4):339–344. https://doi.org/10.1016/j.ijsu.2008.01.006
Frountzas M, Nikolaou C, Stergios K, Kontzoglou K, Toutouzas K, Pergialiotis V (2019) Is the laparoscopic approach a safe choice for the management of acute appendicitis in pregnant women? A meta-analysis of observational studies. Ann R Coll Surg Engl 101(4):235–248. https://doi.org/10.1308/rcsann.2019.0011
Wilasrusmee C, Sukrat B, McEvoy M, Attia J, Thakkinstian A (2012) Systematic review and meta-analysis of safety of laparoscopic versus open appendicectomy for suspected appendicitis in pregnancy. Br J Surg 99(11):1470–1478. https://doi.org/10.1002/bjs.8889
Walker HGM, Al Samaraee A, Mills SJ, Kalbassi MR (2014) Laparoscopic appendicectomy in pregnancy: a systematic review of the published evidence. Int J Surg 12(11):1235–1241. https://doi.org/10.1016/j.ijsu.2014.08.406
Prodromidou A, Machairas N, Kostakis ID et al (2018) Outcomes after open and laparoscopic appendectomy during pregnancy: a meta-analysis. Eur J Obstet Gynecol Reprod Biol 225:40–50. https://doi.org/10.1016/j.ejogrb.2018.04.010
Sadot E, Telem DA, Arora M, Butala P, Nguyen SQ, Divino CM (2010) Laparoscopy: a safe approach to appendicitis during pregnancy. Surg Endosc 24(2):383–389. https://doi.org/10.1007/s00464-009-0571-7
Kirshtein B, Perry ZH, Avinoach E, Mizrahi S, Lantsberg L (2009) Safety of laparoscopic appendectomy during pregnancy. World J Surg 33(3):475. https://doi.org/10.1007/s00268-008-9890-4
Corneille MG, Gallup TM, Bening T et al (2010) The use of laparoscopic surgery in pregnancy: evaluation of safety and efficacy. Am J Surg 200(3):363–367. https://doi.org/10.1016/j.amjsurg.2009.09.022
Reedy MB, Galan HL, Richards WE, Preece CK, Wetter PA, Kuehl TJ (1997) Laparoscopy during pregnancy. A survey of laparoendoscopic surgeons. J Reprod Med 42(1):33–38
Oelsner G, Stockheim D, Soriano D et al (2003) Pregnancy outcome after laparoscopy or laparotomy in pregnancy. J Am Assoc Gynecol Laparosc 10(2):200–204
Pastore PA, Loomis DM, Sauret J (2006) Appendicitis in pregnancy. J Am Board Fam Med 19(6):621–626. https://doi.org/10.3122/jabfm.19.6.621
Yilmaz HG, Akgun Y, Bac B, Celik Y (2007) Acute appendicitis in pregnancy—risk factors associated with principal outcomes: a case control study. Int J Surg 5(3):192–197. https://doi.org/10.1016/j.ijsu.2006.05.005
Ibiebele I, Schnitzler M, Nippita T, Ford JB (2019) Appendicectomy during pregnancy and the risk of preterm birth: a population data linkage study. Aust N Z J Obstet Gynaecol 59(1):45–53. https://doi.org/10.1111/ajo.12807
Wei P-L, Keller JJ, Liang H-H, Lin H-C (2012) Acute appendicitis and adverse pregnancy outcomes: a nationwide population-based study. J Gastrointest Surg 16(6):1204–1211. https://doi.org/10.1007/s11605-012-1858-x
Acknowledgements
The authors thank to Oficina de Tecnología de la información y la Comunicación of Ministerio de Salud y Protección Social from Colombia, especially to Dolly Ovalle and Luz Emilse Rincon, for providing anonymized data for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Buitrago, G., Arevalo, K., Moyano, J.S. et al. Appendectomy in Third Trimester of Pregnancy and Birth Outcomes: A Propensity Score Analysis of a 6-Year Cohort Study Using Administrative Claims Data. World J Surg 44, 12–20 (2020). https://doi.org/10.1007/s00268-019-05200-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05200-x