Abstract
Background
Despite improvements in prevention and rescue, mortality rates after severe blunt trauma continue to be a problem. The present study analyses mortality patterns in a representative blunt trauma population, specifically the influence of demographic, injury pattern, location and timing of death.
Methods
Patients that died between 1 January 2004 and 31 December 2005 were subjected to a standardised autopsy. Inclusion criteria: death from blunt trauma due to road traffic injuries (Injury Severity Score ≥ 16), patients from a defined geographical area and death on scene or in hospital. Exclusion criteria: suicide, homicide, penetrating trauma and monotrauma including isolated head injury. Statistical analyses included Student’s t test (parametric), Mann–Whitney U test (nonparametric) or Chi-square test.
Results
A total of 277 consecutive injured patients were included in this study (mean age 46.1 ± 23 years; 67.5% males), 40.5% of which had an ISS of 75. A unimodal distribution of mortality was observed in blunt trauma patients. The most frequently injured body regions with the highest severity were the head (38.6%), chest (26.7%), or both head and chest (11.0%). The cumulative analysis of mortality showed that several factors, such as injury pattern and regional location of collisions, also affected the pattern of mortality.
Conclusions
The majority of patients died on scene from severe head and thoracic injuries. A homogenous distribution of death was observed after an initial peak of death on scene. Moreover, several factors such as injury pattern and regional location of collisions may also affect the pattern of mortality.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Trauma continues to represent one of the leading causes of death in patients under the age of 40 years [1, 2]. The trimodal distribution of deaths related to trauma was originally described in the 1980s [3, 4]. The original description was based upon various types of trauma, including death from penetrating and blunt injuries. Haemorrhagic shock and brain injury have previously been described as the most frequent causes of death.
A recently published systematic literature review reported that studies published over the past two decades have not confirmed the trimodal distribution summarised above [5]. These studies have mainly reported unimodal and bimodal distributions of mortality, regardless of geographical location, finding differences in the proportion of early and late deaths. Moreover, great variability has been identified between studies [5].
In our opinion, more standardised studies (focused trauma entity, representative study population, etc.) in this field are required. Therefore, in this study, we have attempted to address these issues to answer the following questions:
-
1.
What is the temporal distribution of deaths resulting from road traffic injuries in a well-defined and representative population with road traffic injuries?
-
2.
What are the exact injury patterns in patients with blunt trauma based on autopsy findings?
Materials and methods
Study design and patient selection
We conducted a retrospective study of consecutive autopsy data from blunt trauma non-survivors. All patients included were subjected to an autopsy between 1 January 2004 and 31 December 2005, who had died as a result of blunt multiple trauma following a road traffic collusion (RTC) in a well-defined area [Southern Bavaria, 37,850 qkm, with 7.2 Mio. inhabitants in 2004 and 2005, on average 190 inhabitants per qkm including rural and urban areas. Munich is the biggest city with 1.3 Mio. inhabitants at that time. (https://www.regionalstatistik.de/genesis/online (06.03.2017))].
Inclusion criteria
The inclusion criteria for this study were as follows: blunt trauma due to road traffic injury, multiple trauma [Injury Severity Score (ISS) ≥ 16], collisions in a defined geographical area (representative of both urban and rural environments) and autopsy performed by a defined team of certified forensic pathologists.
Exclusion criteria
The exclusion criteria for this study were as follows: monotrauma including an isolated head injury, intentional injury (suicide or homicide), penetrating trauma, or burn injuries.
Autopsy and data collection
Standardised autopsies were conducted at the same institute (Institute of Legal Medicine) including analyses of the internal organs and brain. All autopsies were performed by certified forensic pathologists. For Munich and surroundings, the autopsy rate is higher than 90%, on average for the whole capture area the rate is around 30%.
All basic demographic data was recorded in a database. In addition, information regarding the clinical data, mechanism of injury, trauma location, injury pattern and cause of death was collected from the autopsy reports. Data relating to the site of collisions (highway, urban or rural road), traffic participation and opponent (pedestrian, bicyclist, powered two-wheeler (PTW), occupant of passenger car, etc.) was collected, and the time between the collision and death was obtained from the public prosecution files. All investigators were trained to use the Abbreviated Injury Scale © 2005 update 2008 (AAAM 2008) and how to calculate the Injury Severity Score (ISS). All coding was reassessed by physicians experienced with AIS coding.
Definitions
Clusters of mortality
Patients who had died prior to arrival of the rescue team or were declared dead after unsuccessful resuscitation or that died during transport before reaching a hospital were considered as dead “on scene”. The time of death was taken from the autopsy reports.
The time of RTC was extracted from the police reports. Patients that died during their hospital stay were grouped according to their time of death after trauma, using stratification commonly applied in previous studies: <1, 1–6, 6–24 h, 1–7, 7–30 and >30 days.
Documentation of injury patterns
For each patient, all injuries described in the chart and during the autopsy were coded according to the AIS, and the ISS was calculated [6]. The AIS is an anatomically based consensus-derived global severity scoring system which classifies each injury by body region according to is relative importance for the victim. This system differentiates between the following body regions: head, face, neck, thorax, abdomen, spine, upper extremity, lower extremity and external injuries. Moreover, this scoring system describes the type of anatomical structures affected, including the blood vessels, nerves, organs and skeleton. In addition, the maximum AIS (MAIS) was documented for each patient, representing the most severe injury severity value out of all injuries. Further, the body region in which the MAIS occurred was documented and is called “leading body region”. In cases where the MAIS was found in multiple body regions, a combination of regions was recorded as the most severely injured body regions.
Representative population
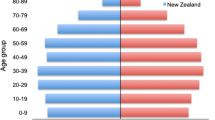
In order to demonstrate the representativeness of our study, data from the study sample were compared with the road traffic fatalities population of the same region and time (Table 1; Bavarian State Office for Statistics (Bayerisches Landesamt für Statistik 2015) for years 2004 and 2005.
Statistical analysis
All data were analysed using SPSS version 20.0 (SPSS Inc., Chicago, IL, USA). Statistical differences were determined by Chi-square test, where appropriate. Results are presented as mean and standard deviation (SD) or median and range. Frequencies are reported for nominal and ordinal data. A Chi-square test was used for the representativity calculations, using open source software available from http://www.physics.csbsju.edu/stats/ (Kirkman 1996). P < 0.05 was considered statistically significant for all analyses. In addition, a Kaplan–Meier survival chart based on the time of death of the fatalities is presented to show high share of deaths on scene.
Results
Demographic data
Of the 389 patients considered for this study, 112 were excluded according to the exclusion criteria. The majority of patients in the study population were male (n = 187, 67.5%), with a mean age of 46.1 ± 23.1 years and a median ISS of 50 (range 17–75). The patient sample (n = 277) was representative in terms of age and gender; however, the high proportion of pedestrians meant that the study was not representative of traffic participation (Table 1A–C). These patients sustained blunt trauma in the form of motor vehicle collisions (MVC; 46.9%), pedestrian run-over (27.4%), motorcycle collisions (11.6%) and bicycle collisions (10.8%).
Distribution of injuries
Figure 1 shows the frequency distribution of the most severely injured body region(s). The majority of our trauma patients sustained a severe brain injury (n = 107, 38.6%; Fig. 1), and most of these injuries were very serious and unsurvivable (AIS = 5, 20.9% of injured; AIS = 6, 26% of injured). Moreover, severe thoracic injuries were found to be the second most frequent injuries contributing to death in our population (n = 74, 26.7%), resulting from the rupture of major thoracic vessels, followed by severe cardiac injuries (AIS = 5, 27.1% of injured; AIS = 6, 17.3% of injured). We found that 11.6% (n = 32) of patients presented with both thoracic and head injuries as their most severe injuries, while a combination of thorax and extremity injuries was documented in 4.3% (n = 12) of patients (Fig. 1 and Table 2). Serious abdominal injuries as the most severe (leading) injuries were less frequently identified (n = 8, 2.9%), and extremity and pelvic injuries as the most severe (leading) injuries were only reported in 2.2% (n = 6) of patients. Not as the most severe injury, but nevertheless, abdominal injuries were present in 64% (n = 178).
Body regions (single and in combination) most severely injured (MAIS ≥ 3) in fatal road traffic collisions: Most frequent combinations were injuries of head and thorax and thoracic trauma with concomitant extremity or pelvic injuries. Severe pelvic injuries (AIS ≥ 3; unstable pelvic ring injuries and disruption of pelvic floor) were very frequently observed in patients: in up to 43% (n = 77) of patients died on scene and in up to 31% (n = 31) died with in the clinic severe pelvic injuries were present. Due to other serious injuries (e.g. head or thorax), these injuries were possibly less frequently the cause auf death
Time distribution of deaths
There was an even distribution of the timing of trauma deaths (trimodal or bimodal); therefore, we named the observed distribution “unimodal”, characterised by an initial peak of on scene fatalities followed by an even distribution thereafter (Fig. 2). The Kaplan–Meier survival curve confirmed a relationship between death and time (Fig. 2a).
When a different time interval was selected, as described previously, a trimodal distribution was confirmed (initial peak on scene of 64.3%, n = 178), second peak between 1 and 6 h (13.7%, n = 38) and a third peak between day 1 and 7 (10.8%, n = 30), as shown in Fig. 3.
Temporal interval diagram of the time point of deaths, using different timescales and intervals. The table below demonstrates the time distribution of death according to the leading body regions. Leading head, thorax and combined head and thorax injuries. Fatalities due to head trauma demonstrated the highest number of victims died “on scene” followed by deaths on “day 1–day 7”. Interestingly, fatalities with severe chest injuries also showed two major groups, with the first group “on scene” and the second groups of death died between 1 and 6 h post-injury. On other hands, fatalities with combined head and chest injuries showed a most pronounced group “on scene”. Other groups were less frequently present
Stratification of injury distribution by location of the most severe injury (head, chest and combination of chest and head trauma) showed that the injury pattern was associated with the distribution of deaths (p = 0.01, see also Fig. 3).
Type of road collision affects the mortality pattern
Cases were split for different collision locations (highway, n = 29; rural road, n = 182; and urban road, n = 66), allowing us to observe different mortality patterns (p = 0.007, Fig. 4). For all fatalities, a high percentage (up to 75%) of fatalities that sustained an injury on a highway died on scene or within the first 6 h after trauma. In comparison, a low percentage of fatalities due to urban collisions occurred on scene. Most of these patients reached the clinic and died later during the clinical course (Fig. 4). Furthermore, the highest number of trauma victims that died on scene sustained a collision on a rural road. This group of patients was also present during the clinical course, for which death occurred due to systemic complications.
Discussion
The mortality rate of multiple trauma patients has decreased from 22.8 to 18.7% over the past decades [1]. In the current autopsy study, we examined the temporal distribution and injury pattern of severely injured patients in a well-defined geographical area, which only included patients with one trauma entity. The major findings of our analysis were:
-
1.
Identification of a unimodal distribution of mortality in blunt trauma patients. The majority of these patients died on scene, followed by a consistent decrease during the post-traumatic period.
-
2.
Head and thoracic injuries were found to be the leading injuries which were most likely to be the cause of death. Abdominal and pelvic injuries were less frequently observed as the most severe (leading) injuries in our study.
-
3.
The cumulative demonstration of mortality (choosing different time intervals) revealed that several factors, such as injury pattern and the regional location of the collision, may also affect the pattern of mortality.
Within the past decades, numerous studies have analysed the temporal distribution of mortality in severely injured patients. However, several authors have pointed out that the mechanism of trauma and trauma entity are the leading factors affecting the timing of trauma mortality [6]. The causes of death and mortality patterns for patients with road traffic injuries do not appear to have been comprehensively examined, as the majority of studies also included penetrating trauma. Our analysis showed a unimodal distribution for patients with blunt trauma that had been involved in road traffic collisions. It has previously been reported that death from penetrating trauma often occurs very early, whereas death from blunt trauma occurs later during the post-traumatic course [7, 8]. According to our data, blunt trauma fatalities appear to also demonstrate a high percentage of on-scene mortality [7,8,9].
High numbers of patients included to our analysis were either pedestrians (27.4%, n = 76) or bicyclists (10.8%, n = 30). This is mainly related to high autopsy rates in the city of Munich in comparison to relatively lower autopsy frequency in rural surroundings. According to the World Health Organization (WHO), there is a disproportional involvement of pedestrians and cyclists in road traffic injuries. Especially in low- and middle-income countries, high rates of road traffic injuries have been reported. The major burden of road trauma in low- and middle-income countries is largely attributable to unsafe vehicles, lack of appropriate road infrastructure and the predominance of vulnerable road users [10,11,12]. Another important factor is the trauma system, which has a relevant effect on preclinical and clinical mortality. Moreover, the highest share in our data (47%) and all traffic fatalities in our capture area (56%) are still made from passenger car occupants.
Our analysis has shown that up to 64.3% (n = 178) of fatally injured victims do not arrive at hospital and die due to trauma prior to arrival. In a recent publication, Champion et al. reviewed a prehospital death rate in trauma patients from the year 1978–2013 including up to 55.535 early death [13]. This study revealed that the proportion of death that occurred before patient reached a hospital has increased to 56%, while the proportion of clinical death declined to 40%. Authors discussed that the reduction of the hospital death is a result of the effectiveness trauma centres. However, the high proportion of prehospital death stresses the need for strategies and improvements in primary and secondary prevention [13].
Several studies have discussed whether the initial trauma deaths (death within the first few hours) are preventable or not. Chiara and co-authors considered patients with at least one sustained injury with an AIS of 6, or a head injury with an AIS of ≥5, as being “unsalvageable” [14]. In our study, approximately 40.4% of patients had an AIS of 6, and 32.5% with an AIS of 5. According to this data, up to 20% of deaths can be considered potentially avoidable if fast and efficient support is provided. Our results are in line with previous publications. Tien et al. analysed the preventability of trauma death and calculated a potentially salvageable death rate of 16% [15]. Others reported preventable death rates in trauma patients from 21 to 27% [16, 17]. In addition, the presence of unrecognised life-threatening injuries has been described to affect 1–4% of severely injured patients [18, 19].
According to our autopsy findings, brain injury, thoracic injury and a combination of both were the leading injuries in our study. In combination with concomitant lesions, these injuries most likely contributed to the patients’ deaths. Furthermore, the relevance of brain injuries remains high. A literature review has shown that traumatic brain injury is still the leading cause of death after trauma [5]. The second frequent cause of death is exsanguination mainly due to thoracic or abdominal injuries. Isolated haemorrhage is predominant in penetrating trauma, while brain injuries in combination with severe bleeding were more frequently observed with blunt trauma. Moreover, studies indicate that there have been no considerable changes in the incidence of central nervous system (CNS) trauma over the last 30 years [20]. In contrast, the incidence of haemorrhage-related deaths appears to have decreased over the same period [20]. We observed a very low rate of severe abdominal injuries being the cause of death. Nevertheless, many patients presented abdominal injuries (n = 178, 64.3%) in our study, which may have led to additional haemorrhage and therefore can be considered a co-factor for fatalities. Moreover, the lack of penetrating injuries in our analysis may also be responsible for the lower rates of severe abdominal trauma. Previous studies have also indicated that improved haemorrhage management and implementation of Advanced Trauma Life Support (ATLS) may have had a beneficial effect on survival [21]. In addition, patients that suffered from an acute haemorrhage appeared to benefit from a damage control approach, which is widely used in trauma care [22, 23].
The grouped distribution of trauma deaths showed a trimodal pattern. When previous studies that focussed on temporal distribution were reviewed, we identified wide heterogeneity of time intervals used [5]. Moreover, we believe that the temporal distribution, as previously described, is a cumulative effect. Several authors noted that factors such as the geographical area, patient age and injury pattern may influence the time point of death, and consequently, the pattern of mortality [6]. In a large study of trauma deaths, Demetriades et al. did not find a specific universal temporal distribution of death [7, 8]. The authors pointed out that the distribution of death highly depends on mechanisms of injury, the injury patterns, injury severity and age of the patients. This study has clearly demonstrated that the temporal distribution of death in penetrating trauma is different from that in blunt trauma. Søreide et al. also questioned the trimodal distribution and postulated that the temporal distribution is an effect of selected time interval model [24, 25]. Another influencing factor may be the reduction of injury severity in traffic collisions and improvements in active and passive car safety (e.g. air bag technology, seat belt, speed limits) that has occurred in the last decades.
In our study, fatalities that sustained a collision on a highway most frequently died within the first 6 h (Fig. 4), whereas road traffic collisions within the city were associated with a higher frequency of late deaths. These data suggest that the geographical area appears to influence the mortality pattern. Patients with a road traffic collision within the city benefit from a short transportation and rescue time and survive the initial phase of treatment. Focusing on late post-traumatic deaths, Søreide and co-authors observed that patients who died due to Multiple Organ Failure (MOF) were predominantly older and less severely injured in comparison with those who died early [25]. Elderly with less severe injuries in late deaths were also found for all causes of deaths in a comparable data analysis of our capture area by Heinrich et al. [26]. Moreover, the injury pattern also influences the temporal distribution. Patients that sustained a severe head injury showed two major peaks. On the other hand, trauma patients with leading thoracic injuries showed a second peak between 1 and 6 h after the collision. Our results are consistent with previous studies, particularly a study by Bamvita et al. who showed that patients with severe thoracic injuries were more likely to die within the first 6 h, whereas patients with head trauma more frequently died later due to systemic complications [6]. The PROMMTT (Prospective Observational Multicentre Major Trauma Transfusion) study included a large number of trauma victims (n = 34.362) and reported that the median time to haemorrhagic death was 2.6 h (range, 1.7–5.4 h) [27]. Others also calculated similar values of time to death from haemorrhagic shock at approximately 2 h compared with 29 h in a cohort with traumatic brain injury [28]. This time period could be relevant in future studies focusing on treatment and strategies in patient sustained road traffic injuries.
Our results should be interpreted considering a few limitations. Firstly, this analysis is a retrospective study, with data prospectively acquired from a database. The study population includes data from the year 2004 and 2005. Therefore, changes in car safety may influence the pattern of injury and therefore the pattern of mortality. The results encourage us to proceed and analyse 2014–2015 for comparison. The patients included were from a well-defined geographical area, and the study population was representative in terms of age and sex. Secondly, the autopsy rate was not 100%; therefore, inclusion bias may have also affected the results of this study. However, we believe that one of the major strengths of our study is the use of a well-defined population with only one cause of trauma (road traffic injuries), and the exclusion of penetrating trauma, as these factors are known to affect the results.
In conclusion, we analysed 277 autopsies of trauma victims that had died due to road traffic collisions. Our study revealed that the majority of fatalities still die on scene. Brain and thoracic injuries were found to be the most severely (leading) injured body region. We also identified a unimodal distribution of mortality and showed that the time point of death is affected by the location of the collision (highway versus city, hinting towards the influence of velocities) and the injury pattern. The latter two factors were independent of treatment strategies and decision making.
Abbreviations
- ISS:
-
Injury Severity Score
- AIS:
-
Abbreviated Injury Scale
- ICU:
-
Intensive care unit
- MOD:
-
Multiple organ dysfunction
- RTC:
-
Road traffic collisions
- RTI:
-
Road traffic injuries
References
Ruchholtz S, Lefering R, Paffrath T et al (2008) Reduction in mortality of severely injured patients in Germany. Dtsch Arztebl Int 105:225–231
Bardenheuer M, Obertacke U, Waydhas C et al (2000) Epidemiology of the severely injured patient. A prospective assessment of preclinical and clinical management. AG Polytrauma of DGU. Unfallchirurg 103:355–363
Trauma Trunkey DD (1983) Accidental and intentional injuries account for more years of life lost in the US than cancer and heart disease. Among the prescribed remedies are improved preventive efforts, speedier surgery and further research. Sci Am 249:28–35
Trunkey DD, Lim RC (1974) Analysis of 425 consecutive trauma fatalities: an autopsy study. J Am Coll Emerg Phys 3:368–371
Pfeifer R, Teuben M, Andruszkow H et al (2016) Mortality patterns in patients with multiple trauma: a systematic review of autopsy studies. PLoS ONE 11:e0148844
Bamvita JM, Bergeron E, Lavoie A et al (2007) The impact of premorbid conditions on temporal pattern and location of adult blunt trauma hospital deaths. J Trauma 63:135–141
Demetriades D, Kimbrell B, Salim A et al (2005) Trauma deaths in a mature urban trauma system: is “trimodal” distribution a valid concept? J Am Coll Surg 201:343–348
Demetriades D, Murray J, Charalambides K et al (2004) Trauma fatalities: time and location of hospital deaths. J Am Coll Surg 198:20–26
MacLeod JB, Cohn SM, Johnson EW et al (2007) Trauma deaths in the first hour: are they all unsalvageable injuries? Am J Surg 193:195–199
Damsere-Derry J, Palk G, King M (2017) Road accident fatality risks for “vulnerable” versus “protected” road users in northern ghana. Traffic Inj Prev. doi:10.1080/15389588.2017.1302083
Garg N, Hyder AA (2006) Exploring the relationship between development and road traffic injuries: a case study from India. Eur J Public Health 16:487–491
Garg N, Hyder AA (2006) Road traffic injuries in India: a review of the literature. Scand J Public Health 34:100–109
Champion HR, Lombardo LV, Wade CE et al (2016) Time and place of death from automobile crashes: research endpoint implications. J Trauma Acute Care Surg 81:420–426
Chiara O, Scott JD, Cimbanassi S et al (2002) Trauma deaths in an Italian urban area: an audit of pre-hospital and in-hospital trauma care. Injury 33:553–562
Tien HC, Spencer F, Tremblay LN et al (2007) Preventable deaths from hemorrhage at a level I Canadian trauma center. J Trauma 62:142–146
Maio RF, Burney RE, Gregor MA et al (1996) A study of preventable trauma mortality in rural Michigan. J Trauma 41:83–90
Draaisma JM, de Haan AF, Goris RJ (1989) Preventable trauma deaths in The Netherlands—a prospective multicenter study. J Trauma 29:1552–1557
Pfeifer R, Pape HC (2008) Missed injuries in trauma patients: a literature review. Patient Saf Surg 2:20
Stewart RM, Myers JG, Dent DL et al (2003) Seven hundred fifty-three consecutive deaths in a level I trauma center: the argument for injury prevention. J Trauma 54:66–70 (discussion 70-61)
Pfeifer R, Tarkin IS, Rocos B et al (2009) Patterns of mortality and causes of death in polytrauma patients—has anything changed? Injury 40:907–911
van Olden GD, Meeuwis JD, Bolhuis HW et al (2004) Clinical impact of advanced trauma life support. Am J Emerg Med 22:522–525
Rotondo MF, Schwab CW, McGonigal MD et al (1993) ‘Damage control’: an approach for improved survival in exsanguinating penetrating abdominal injury. J Trauma 35:375–382 (discussion 382-373)
Pape HC, Pfeifer R (2015) Safe definitive orthopaedic surgery (SDS): repeated assessment for tapered application of Early Definitive Care and Damage Control?: an inclusive view of recent advances in polytrauma management. Injury 46:1–3
Soreide K (2010) Epidemiology of trauma deaths: location, location, location! World J Surg 34:1720–1721. doi:10.1007/s00268-010-0434-3 (author reply 1722–1723)
Soreide K, Kruger AJ, Vardal AL et al (2007) Epidemiology and contemporary patterns of trauma deaths: changing place, similar pace, older face. World J Surg 31:2092–2103. doi:10.1007/s00268-007-9226-9
Heinrich D, Holzmann C, Wagner A, Fischer A, Pfeifer R, Graw M, Schick S (2017) What are the differences in injury patterns of young and elderly traffic accident fatalities considering death on scene and death in hospital? Int J Legal Med 131(4):1023–1037. doi:10.1007/s00414-017-1531-8
Holcomb JB, Tilley BC, Baraniuk S et al (2015) Transfusion of plasma, platelets, and red blood cells in a 1:1:1 vs a 1:1:2 ratio and mortality in patients with severe trauma: the PROPPR randomized clinical trial. JAMA 313:471–482
Berbiglia L, Lopez PP, Bair L et al (2013) Patterns of early mortality after trauma in a neighborhood urban trauma center: can we improve outcomes? Am Surg 79:764–767
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Pfeifer, R., Schick, S., Holzmann, C. et al. Analysis of Injury and Mortality Patterns in Deceased Patients with Road Traffic Injuries: An Autopsy Study. World J Surg 41, 3111–3119 (2017). https://doi.org/10.1007/s00268-017-4122-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4122-4