Abstract
Background
Blood natriuretic peptide (NP) levels have been reported to be useful for predicting postoperative atrial fibrillation (AF). We aimed to quantitatively synthesize the current evidence of the accuracy of using NP levels in predicting postoperative AF.
Methods and Results
Medline, Embase, and reference lists were searched. Studies were included if either brain natriuretic peptide (BNP) or N-terminal pro-b type natriuretic peptide (NT-proBNP) had been evaluated perioperatively to predict postoperative AF. Data were analyzed to obtain summary accuracy estimates. Data from 1,844 patients in 10 studies were analyzed. Summary estimates for the sensitivity and specificity of using NP levels for predicting postoperative AF were 75 % [95 % confidence interval (CI) 67–79 %] and 80 % (95 % CI 62–91 %), respectively. The overall diagnostic odds ratio was 3.28 (95 % CI 2.23–4.84). Subgroup analysis showed that elevated NP levels in the perioperative period were a strong independent predictor of postoperative AF. NT-proBNP appeared to have better predictive value than BNP, as did postoperative assessment over preoperative assessment. BNP had a better correlation with postoperative AF in patients undergoing thoracic surgery than in patients undergoing cardiac surgery.
Conclusions
Perioperative assessment of the natriuretic peptide level in patients undergoing major cardiothoracic surgery could be a valuable diagnostic aid for identifying patients at high risk of developing postoperative AF, and for providing critical clinical information to guide prophylactic antiarrhythmic therapy in the perioperative period.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Atrial fibrillation (AF) represents one of the most frequent postoperative cardiac complications, especially in patients undergoing cardiothoracic surgery [1, 2]. The incidence of postoperative AF varies between 10 and 40 % [1, 3]. Although AF is often benign, it has been related to increased morbidity, including hypotension, heart failure, thromboembolic complications, prolonged hospital stay, and increased hospital costs [3–7]. Several pharmacological therapies have been shown to be able to prevent the development of postoperative AF [8, 9], but there is no established method for the preoperative identification of patients at high risk of developing this arrythymia. Because use of preventive medications is not totally without risk, unselective administration of such medications is not justifiable. Several factors, including male gender, age, atrial dimension, low ejection fraction, left ventricular (LV) diastolic dysfunction, history of diabetes mellitus, hypertension, chronic obstructive pulmonary disease, and coronary artery disease, have been reported as predictors of postoperative AF following coronary artery bypass surgery (CABG) or other surgery, but only advanced age has been widely validated.
Recently, a number of observational studies have examined the predictive value of brain natriuretic peptide (BNP) or N-terminal pro-b type natriuretic peptide (NT-proBNP) for identifying patients at risk of AF after a major surgery [10–19]. B-type natriuretic peptide or its inactive cleavage product N-terminal pro-BNP is secreted mainly from the left ventricle in response to pressure and volume overload [20]. Systemic physiologic effects of natriuretic peptides (NPs) include natriuresis, diuresis, and vasodilation [21]. Although most studies have shown an association between elevated NP levels and postoperative AF, the risk estimates vary widely among studies. We therefore carried out a systematic review and meta-analysis to summarize data on the association between NP levels and postoperative AF in adult patients.
Materials and Methods
Search Strategy and Selection Criteria
We searched three electronic databases (Medline, Embase, and the Cochrane database) for studies published through January 2012 with the following MeSH terms and free text: “natriuretic peptide,” “surgery,” “arrhythmia,” and “atrial fibrillation.” We did not set any time or language restrictions for these searches. We checked the reference lists of relevant review articles. Selection was performed independently by two reviewers. Discrepancies between the selections of the reviewers were resolved by a consensus meeting with the third or fourth co-author.
The title and abstract of the studies were screened in the first round, and potentially relevant articles were retrieved for full-text review in the second round. For inclusion, the studies had to fulfil the following criteria:
-
Have a study population of consecutive patients (age >18 years) undergoing cardiac or non-cardiac surgery
-
Include results of a BNP or NT-proBNP test in the perioperative period
-
Use perioperative AF as one of the endpoints
-
Include calculations of sensitivity, specificity, or odds ratio, or have sufficient data to construct a 2 × 2 contingency table.
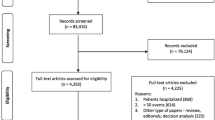
We excluded case reports, case series, review articles, editorials, and clinical guidelines. Two authors independently assessed all titles and abstracts to determine whether the inclusion criteria were satisfied. Full-text articles were retrieved if any of the reviewers considered the abstract suitable. The study inclusion and exclusion process is summarized in Fig. 1.
Quality Assessment
The methodological quality of the selected studies was evaluated independently by two reviewers with a validated tool for the quality assessment of diagnostic accuracy studies (Quality Assessment of Diagnostic Accuracy Studies, QUADAS) [22]. Discrepancies were resolved by a consensus meeting with the third and fourth co-authors.
Data Synthesis and Analysis
We calculated the pooled sensitivity, specificity, likelihood ratio, as well as the diagnostic odds ratio for the included studies. Given the inherent negative correlation between sensitivity and specificity, we estimated these parameters with the bivariate model for diagnostic meta-analyses [23]. This approach assumes a bivariate distribution for the log-transformed sensitivity and specificity. In addition to accounting for study size, the bivariate model also estimates and adjusts for the negative correlation between the sensitivity and specificity of the index test that may arise from the different thresholds used in different studies [24]. To compare diagnostic performance between two biomarkers, we calculated the area under the summary receiver operating characteristic (AUROC) curve and diagnostic odds ratio (OR) to summarize the true positive and false positive rates of different diagnostic studies, irrespective of the different cutoff points used in the various studies. To deal with zero observations in 2 × 2 contingency tables, ½ was added to each cell, reducing performance in the small studies. To formally quantify the extent of between-study variation (i.e., heterogeneity), we calculated the inconsistency index I2, which describes the variation of effect estimate that is attributable to heterogeneity across studies [25]. Summary diagnostic odds ratios were estimated by random (DerSimonian-Laird) or fixed (Mantel–Haenszel) effect models, depending on whether I 2 was greater or lower than 50 % [26]. Meta-regression was used to evaluate the amount of heterogeneity in the subgroup analysis. We defined a priori the following potential relevant covariates: biomarker, type of surgery, and the age range and underlying disease of the study patients [27]. We tested for publication bias by inspecting the symmetry of funnel plots, and we then assessed the potential for publication bias by performing Begg and Egger tests [28]. Statistical analyses were conducted using STATA 11.0 (Stata Corp, College Station, TX). All statistical tests were two-sided, and statistical significance was defined as a P value less than 0.05.
Results
A total of 10 primary studies (1 non-English-language study) met the criteria for inclusion. They included 1,844 patients undergoing major operations whose BNP or NT-proBNP levels were measured in the perioperative period (Fig. 1). Four hundred thirty-four patients (24 %) developed postoperative AF. Agreement regarding eligibility was 90 %.
Of these 10 studies, 6 included patients undergoing cardiac valve surgery or CABG, and the remaining 4 included patients undergoing thoracic surgery either for lung cancer or for esophageal cancer. The study settings included hospitalized patients (8 studies) and Intensive Care Unit (ICU) patients [2]. Details of the participants, settings, outcomes, and study quality criteria of the studies selected for meta-analyses are summarized in Table 1. The sensitivity, specificity, and diagnostic odds ratio for the BNP and NT-proBNP tests, and the timing of biomarker measurement are summarized in Table 2. The sensitivity of natriuretic peptides (NPs) in predicting postoperative AF ranged from 67 to 87 %, and the specificities ranged from 29 to 93 %. The diagnostic OR ranged from 1.00 to 27.9, with 8 studies reporting the adjusted effect estimate and 2 derived from crude calculation.
Study Characteristics
All of the included studies collected data prospectively and provided clear descriptions of patient selection criteria and index tests. All patients underwent standard electrocardiography as a reference test without differential disease ascertainment. None of the included studies provided an explanation for uninterpretable test results or participants’ withdrawal from the study. Although none of the studies specified whether they were blinded to index testing in ascertaining outcome, incorporation bias is not likely because the diagnosis of AF is not influenced by knowledge of serum levels of NPs. Figure 2 provides an overall picture of the methodological quality of studies as evaluated with the QUADAS tool.
Results of Individual Studies
Sensitivity and Specificity
We identified a total of five studies that reported estimated sensitivity and specificity of NPs in predicting postoperative AF. Overall, the pooled sensitivity was 73 % (95 % CI 67–79 %) and specificity was 80 % (95 % CI 62–91 %) (Table 3). The pooled positive likelihood ratio was 3.69 (95 % CI 1.87–7.26) and the negative likelihood ratio was 0.34 (95 % CI 0.28–0.40). Four studies evaluated NT-proBNP, while only 1 study evaluated BNP. Detailed pooled effect estimates of 5 studies reporting sensitivity and specificity are summarized in Table 3. Figure 3 shows the summary receiver operator characteristic (ROC) curve of the NP test, which revealed an area under the ROC curve of 0.78 (95 % CI 0.74–0.81).
Summary receiver operating characteristic (SROC) curve (solid line) and the bivariate summary estimate (solid square), together with the corresponding 95 % confidence ellipse (inner dashed line) and 95 % prediction ellipse (outer dotted line). The symbol size for each study is proportional to the study size
Diagnostic Odds Ratio
We identified a total of 10 studies reporting the estimated diagnostic OR for the use of perioperative NP tests in predicting postoperative AF. The overall diagnostic OR is 3.28 (95 % CI 2.22–4.84) (Fig. 4). A significant degree of heterogeneity (I 2: 95.4 %) was observed in either primary or subgroup analysis. Subgroup analysis showed an attenuated effect estimate in adjusted analysis. Comparing the two subtypes of NP, NT-proBNP was associated with a superior diagnostic OR as compared to BNP. Natriuretic peptides can predict postoperative AF more accurately in patients undergoing thoracic surgery (pooled OR 7.07, 95 % CI 1.14–44.04) than in patients undergoing cardiac surgery (pooled OR 1.90, 95 % CI 1.21–2.99). Postoperative measurement of NPs (pooled OR 5.67, 95 % CI 1.05–30.55) was associated with a higher diagnostic value than preoperative measurement (pooled OR 3.90, 95 % CI 1.86–8.19). None of the subgroup analyses were significantly different from the overall meta-regression analysis. There was evidence of publication bias. Detailed pooled effect estimates of 10 studies reporting diagnostic OR are summarized in Table 4.
Discussion
In this study, elevated plasma BNP or NT-proBNP levels obtained in the perioperative period were strong independent predictors of the occurrence of postoperative AF. NT-proBNP levels appeared to have better predictive power than BNP levels. Similarly, postoperative assessment had better predictive power than preoperative assessment. Brain NP levels showed better correlation with postoperative AF in patients undergoing thoracic surgery than in patients undergoing cardiac surgery. The overall pooled sensitivity and specificity in predicting postoperative AF were 75 % (95 % CI 67–79 %) and 80 % (95 CI 62–91 %), respectively.
Both BNP and NT-proBNP are synthesized and released by an overloaded myocardium with cyclic guanosine monophosphate-mediated natriuretic and vasodilator properties [21]. In addition to serving as indicators of heart failure, BNP and NT-proBNP levels are major biomarkers of risk for several cardiac diseases, such as coronary heart disease, sepsis, and valvular heart disease [29–31]. In major cardiac or thoracic surgery, the natriuretic peptide level reflects the magnitude of hemodynamic change and LV change. Elevated levels of NP have been linked to major adverse cardiac events in previous systematic reviews [29, 32, 33]. In major cardiothoracic surgery, there is a profound need for such a biomarker, because the identification of high-risk patients is essential, both for clinical management and to indicate patients who require close postoperative monitoring and preventive therapy for arrhythmia.
Several preventive medications have shown promise in reducing the incidence of postoperative AF, including beta-blockers, angiotensin-converting enzyme inhibitors or angiotensin receptor blockers, amiodarone, magnesium sulfate, and non-steroidal anti-inflammatory drugs [8]. However, none of these drugs are totally safe, and their unnecessary use may cause excessive iatrogenic adverse events.
Based on the high accuracy of NPs in predicting postoperative AF, an NP-guided selective preventive strategy is of high interest. To make our results more informative to clinicians, we used pooled likelihood ratio estimates to calculate the post-test probability. In a virtual population with a postoperative prevalence of 25 % (the actual pooled prevalence in this study is 24 %), a positive NP test (LR+: 3.69) would increase the post-test probability to 55 %. Likewise, in the same population, a negative NP test (LR−: 0.34) would reduce the post-test probability to 10 %. Therefore, for patients with a negative preoperative NP test result, avoiding preventive medication carries only a 10 % risk for developing postoperative AF.
In addition to the imperfect sensitivity and specificity, clinical recommendations regarding the utility of NP testing to guide prophylaxis against postoperative AF should consider several other factors. Of note, the threshold value, the timing of measurement, and the type of NP test should be clearly defined. In our analysis, measuring NT-proBNP in the operative period with a threshold level between 180 and 850 pg/mL appeared to be the most accurate combination. However, this finding needs to be confirmed, given the small number of studies and the wide range of threshold values. Moreover, the aforementioned pharmacologic prophylactic therapy was mostly administered in the preoperative setting; whether postoperative administration would be as effective remains unanswered.
One way to resolve the controversy is to enhance the predictive value of preoperative NP measurement. Further efforts to combine established risk factors for postoperative AF, such as age, gender, hypertension, echocardiographic characteristics, and cardiovascular disease, into a risk-prediction instrument may produce a robust algorithm that can further guide selective prevention with fewer false negatives in the preoperative assessment. In addition, prospective randomized controlled trials designed to evaluate both markers in the preoperative and postoperative period would be highly desirable. Results of such trials would help determine the best timing and the appropriate patient population for administration of prophylactic therapy.
The main strength of this meta-analysis is that it highlights the high predictive value of perioperative NP levels for postoperative AF. Our data suggest that use of the NT-proBNP test and measurement in the postoperative period are associated with higher predictive value. The main weaknesses of our report stem from the limitations of the identified studies. The most obvious limitation is the incomplete reporting of diagnostic accuracy parameters, especially sensitivity and specificity, in many of the included articles. The pooled sensitivity and specificity is based on half of the included articles, which may lead to biased results. A high degree of heterogeneity is another issue, where the study settings, case mix, and cutoff levels for NP tests varied greatly among the included studies, limiting the generalizability of their results. Although 7 studies reported adjusted OR that comprehensively adjusted for the comorbidities in each patient population (Table 1), there are multiple factors that may contribute to postoperative AF that may not have been controlled for in each study, and the value of NP tests may have been over-evaluated. Studies with small sample sizes also may have allowed for a type II error. We did not find significant publication bias in our analysis, but the limitation of our statistical method in detecting publication bias has been demonstrated. Therefore, we cannot disprove the inflation of accuracy estimates due to the favorable acceptance of papers reporting favorable results.
Conclusions
Preoperative natriuretic peptide levels predict postoperative AF in patients undergoing cardiothoracic surgery. BNP levels could be used to better stratify patients in this respect. In addition, BNP activation should direct the attention of clinicians toward monitoring cardiac rhythm and hemodynamic variables more closely than as might be suggested by a cursory evaluation.
References
Hogue CW Jr, Creswell LL, Gutterman DD et al (2005) Epidemiology, mechanisms, and risks: American College of Chest Physicians guidelines for the prevention and management of postoperative atrial fibrillation after cardiac surgery. Chest 128(Suppl 2):9S–16S
Mitchell LB (2011) Canadian Cardiovascular Society atrial fibrillation guidelines 2010: prevention and treatment of atrial fibrillation following cardiac surgery. Can J Cardiol 27:91–97
Rostagno C, La Meir M, Gelsomino S et al (2010) Atrial fibrillation after cardiac surgery: incidence, risk factors, and economic burden. J Cardiothorac Vasc Anesth 24:952–958
Auer J, Weber T, Berent R et al (2005) Postoperative atrial fibrillation independently predicts prolongation of hospital stay after cardiac surgery. J Cardiovasc Surg 46:583–588
Hravnak M, Hoffman LA, Saul MI et al (2002) Resource utilization related to atrial fibrillation after coronary artery bypass grafting. Am J Crit Care 11:228–238
Mathew JP, Parks R, Savino JS et al (1996) Atrial fibrillation following coronary artery bypass graft surgery: predictors, outcomes, and resource utilization. MultiCenter Study of Perioperative Ischemia Research Group. JAMA 276:300–306
Mariscalco G, Klersy C, Zanobini M et al (2008) Atrial fibrillation after isolated coronary surgery affects late survival. Circulation 118:1612–1618
Arsenault KA, Yusuf AM, Crystal E et al (2013) Interventions for preventing postoperative atrial fibrillation in patients undergoing heart surgery. Cochrane Database Syst Rev 1:CD003611
Kern LS (2004) Postoperative atrial fibrillation: new directions in prevention and treatment. J Cardiovasc Nurs 19:103–115 quiz 116–107
Tanaray MEB, Jahanzad Isa, Salehi Mehrdad et al (2010) Relationship of plasma level of NT-ProBNP with development of AF in CABG patients. Tehran Univ Med J 68:384–390
Cardinale D, Colombo A, Sandri MT et al (2007) Increased perioperative N-terminal pro-B-type natriuretic peptide levels predict atrial fibrillation after thoracic surgery for lung cancer. Circulation 115:1339–1344
Detaint D, Messika-Zeitoun D, Avierinos JF et al (2005) B-type natriuretic peptide in organic mitral regurgitation: determinants and impact on outcome. Circulation 111:2391–2397
Dogan SM, Buyukates M, Kandemir O et al (2007) Predictors of atrial fibrillation after coronary artery bypass surgery. Coron Artery Dis 18:327–331
Gibson PH, Croal BL, Cuthbertson BH et al (2009) Use of preoperative natriuretic peptides and echocardiographic parameters in predicting new-onset atrial fibrillation after coronary artery bypass grafting: a prospective comparative study. Am Heart J 158:244–251
Hou JL, Gao K, Li M et al (2008) Increased N-terminal pro-brain natriuretic peptide level predicts atrial fibrillation after surgery for esophageal carcinoma. World J Gastroenterol 14:2582–2585
Krzych LJ, Szurlej D, Kolodziej T et al (2011) Diagnostic accuracy of pre-operative NT-proBNP level in predicting short-term outcomes in coronary surgery: a pilot study. Kardiol Polska 69:1121–1127
Nojiri T, Maeda H, Takeuchi Y et al (2010) Predictive value of B-type natriuretic peptide for postoperative atrial fibrillation following pulmonary resection for lung cancer. Eur J Cardiothorac Surg 37:787–791
Salvatici M, Cardinale D, Spaggiari L et al (2010) Atrial fibrillation after thoracic surgery for lung cancer: use of a single cut-off value of N-terminal pro-B type natriuretic peptide to identify patients at risk. Biomarkers 15:259–265
Wazni OM, Martin DO, Marrouche NF et al (2004) Plasma B-type natriuretic peptide levels predict postoperative atrial fibrillation in patients undergoing cardiac surgery. Circulation 110:124–127
Gopal DJ, Iqbal MN, Maisel A (2011) Updating the role of natriuretic peptide levels in cardiovascular disease. Postgrad Med 123:102–113
Martinez-Rumayor A, Richards AM, Burnett JC et al (2008) Biology of the natriuretic peptides. Am J Cardiol 101(3A):3–8
Whiting PF, Weswood ME, Rutjes AW et al (2006) Evaluation of QUADAS, a tool for the quality assessment of diagnostic accuracy studies. BMC Med Res Methodol 6:9
Reitsma JB, Glas AS, Rutjes AW et al (2005) Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews. J Clin Epidemiol 58:982–990
Arends LR, Hamza TH, van Houwelingen JC et al (2008) Bivariate random effects meta-analysis of ROC curves. Med Decis Mak 28:621–638
Higgins JP, Thompson SG, Deeks JJ et al (2003) Measuring inconsistency in meta-analyses. BMJ (Clin Res Edition) 327(7414):557–560
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Controlled Clin Trials 7:177–188
Lijmer JG, Bossuyt PM, Heisterkamp SH (2002) Exploring sources of heterogeneity in systematic reviews of diagnostic tests. Stat Med 21:1525–1537
Song F, Khan KS, Dinnes J et al (2002) Asymmetric funnel plots and publication bias in meta-analyses of diagnostic accuracy. Int J Epidemiol 31:88–95
Rodseth RN, Padayachee L, Biccard BM (2008) A meta-analysis of the utility of pre-operative brain natriuretic peptide in predicting early and intermediate-term mortality and major adverse cardiac events in vascular surgical patients. Anaesthesia 63:1226–1233
Wang F, Wu Y, Tang L et al (2012) Brain natriuretic peptide for prediction of mortality in patients with sepsis: a systematic review and meta-analysis. Crit Care (Lond) 16:R74
Hwang IC, Kim YJ, Kim KH et al (2013) Prognostic value of B-type natriuretic peptide in patients with chronic mitral regurgitation undergoing surgery: mid-term follow-up results. Eur J Cardiothorac Surg 43:e1–e6
Ryding AD, Kumar S, Worthington AM et al (2009) Prognostic value of brain natriuretic peptide in noncardiac surgery: a meta-analysis. Anesthesiology 111:311–319
Karthikeyan G, Moncur RA, Levine O et al (2009) Is a pre-operative brain natriuretic peptide or N-terminal pro-B-type natriuretic peptide measurement an independent predictor of adverse cardiovascular outcomes within 30 days of noncardiac surgery? A systematic review and meta-analysis of observational studies. J Am Coll Cardiol 54:1599–1606
Acknowledgments
The authors are grateful to Medical Wisdom Inc. for their help in statistical analysis. This work was funded by the Zhejiang Provincial Program for the Cultivation of High-level Innovative Health talents, the Provincial and Bureau co-construction project (wkj2012-2-020), the Hygiene Bureau project (201202011), and the Zhejiang Traditional Chinese Medicine Science and Technology Project (2009za011). No commercial sponsorship or other external financial support was used in the conduct of this work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cai, GL., Chen, J., Hu, CB. et al. Value of Plasma Brain Natriuretic Peptide Levels for Predicting Postoperative Atrial Fibrillation: A Systemic Review and Meta-analysis. World J Surg 38, 51–59 (2014). https://doi.org/10.1007/s00268-013-2284-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-013-2284-2