Abstract
Background
Although mortality after liver resection has declined, posthepatectomy liver failure (PHLF) remains a major cause of operative mortality. To date there is not consensus on a definition for PHLF. However, there have been many efforts to define PHLF causing operative mortality. In the present study we sought to identify early predictors of death from irreversible PHLF.
Materials and methods
We retrospectively analyzed the medical records of 359 patients with hepatocellular carcinoma who underwent liver resection between March 2000 and December 2010. Various biochemical parameters from postoperative days (POD) 1, 3, 5, and 7 were analyzed and compared with the “50–50” criterion.
Results
Operative mortality was 4.7 %. Prothrombin time (PT) <65 % and bilirubin ≥38 μmol/L on POD 5 showed the only significant difference as compared with “50–50” criterion. The new combination of bilirubin level and the international normalized ratio showed higher sensitivity, area under the curve, as well as similar accuracy (sensitivity 78.6 vs. 28.6 %; p = 0.002; area under the curve 0.8402 vs. 0.6396; p = 0.00176; accuracy 88.6 vs. 93.4 %; p = 0.090). Multivariate analysis revealed the combination of PT <65 % and bilirubin ≥38 μmol/L on POD 5 to be the only independent predictive factor of mortality (odds ratio, 82.29; 95 % confidence interval 8.69–779.64; p < 0.001).
Conclusions
In patients with chronic liver disease who will undergo liver resection the combination of PT <65 % and bilirubin ≥38 μmol/L on POD 5 may be a more sensitive predictor than the “50–50” criterion of mortality from PHLF. Although it needs to validated by prospective study, this measure may be applied to select patients receiving artificial liver supports or liver transplantation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Advances in preoperative evaluation, surgical techniques and equipment, and perioperative care have expanded the numbers of patients who can tolerate liver resection for hepatocellular carcinoma and dramatically reduced postoperative mortality. This mortality rate has decreased from 13 to 20 % in 1977 [1] to less than 5 % more recently [2–6].
However, because it is a major cause of postoperative mortality after liver resection, liver failure has drawn continuous attention. The incidence of posthepatectomy liver failure (PHLF) ranges from 1.2 to 32 % in the published literature [7–13]. This wide variation reflects the heterogeneous patient populations and the different definitions of PHLF between studies. Many studies have been designed to define PHLF, but an accepted standardized definition of PHLF has not yet been developed. Recently, the International Study Group of Liver Surgery (ISGLS) has defined both PHLF and severity of PHLF [14].
Although artificial liver support (ALS) has not shown short-term benefits in patients with decompensated cirrhosis [15], it has had a positive effect, relieving symptoms, extending the amount of time patients can wait for liver transplantation, and decreasing mortality [16–19]. The definition the ISGLS used included invasive procedures (i.e., ALS) as a parameter, and the prediction of mortality showed low specificity. Thus, criteria for detecting early mortality from irreversible PHLF are desperately needed.
The present study was designed to establish a new model for the early prediction of death from irreversible PHLF.
Materials and methods
Patients
Between March 2000 and December 2010, a single surgeon performed hepatectomies for 359 patients with hepatocellular carcinoma at Severance Hospital, Yonsei University Health System, Seoul, Korea. Of the 359 patients, 313 with a pure hepatocellular carcinoma component underwent liver resection were enrolled in this study to unify the diagnosis and grouping of the study population.
The indocyanine green retention rate at 15 min (ICG R15) was measured preoperatively to evaluate liver function in all patients. The surgeon determined the extent of liver resection needed according to the results of the ICG R15 test. The indication of fresh frozen plasma transfusion was prolongation of prothrombin time over 19 s. The medical records of 313 patients were analyzed retrospectively with the approval of the institutional review board.
Outcomes
Demographic and clinical characteristics, results of liver function tests, surgical findings, and results of biochemical testing on postoperative days (POD) 1, 3, 5, and 7 were investigated. The factors analyzed to suggest a possible new early predictor for mortality from PHLF were These: total bilirubin, albumin, blood urea nitrogen (BUN), aspartate transaminase (AST), alanine transaminase (ALT), cholesterol, prothrombin time (PT) to reflect synthetic function, cholestasis, and liver cell necrosis. Cut-off values for the biochemical test were calculated by using receiver operating characteristics (ROC) curve analysis and the “50–50” criterion suggested by Balzan et al. [20] (i.e., the combination of PT index <50 % and serum bilirubin >50 μmol/L) was reinvestigated. The definition of PHLF used was that suggested by ISGLS.
Statistical analysis
Among biochemical parameters, significant variables were selected with ROC curve analysis. Significant variable and combinations of significant variables were compared with the “50–50” criterion. Sensitivity, specificity, accuracy, positive predictive value (PPV) and negative predictive value (NPV) comparisons were conducted with the generalized estimating equation (post hoc Bonferroni), and ROC curve comparison was carried out by the DeLong method [21]. Univariate and multivariate analyses for operative mortality were conducted using logistic regression analysis. The results of continuous variables were presented as mean plus or minus standard deviations, and the results of categorical variables were presented as number (percentage). A p value of <0.05 was considered to be statistically significant. Statistical analysis was performed with SPSS 15.0 (SPSS Inc., Chicago, IL), and comparison of criteria was performed with SAS 9.1.3 ver (SAS Institute Inc., Cary, NC).
Results
Baseline characteristics
Demographic and clinical characteristics of 313 patients are presented in Table 1. A total of 249 (79.6 %) men and 64 (20.4 %) women underwent hepatectomy performed by a single surgeon and were included in this study. Their median age was 55 years (range: 27–76 years). Among these 313 patients, 136 (44.4 %) patients had confounding diseases; and heart disease, including hypertension, was found most frequently (18.2 %). Hepatitis B virus was the most common underlying cause of HCC (n = 261; 83.4 %). The Child-Pugh score for all patients was A. The median ICG R15 was 8.7 % (1–77.5 %).
Operative and pathologic characteristics
Of the 313 patients, 204 (65.2 %) underwent major hepatectomy (i.e., resection of three or more Couinaud segments). All liver resections were performed without the Pringle maneuver. Median operative time was 272 min (range: 91–670 min), and median estimated blood loss was 650 mL (range: 0–14,000 mL). A total of 269 patients (85.9 %) had a single tumor. Median tumor size was 3.2 cm (range: 0.7–16 cm). Pathology results revealed that most patients had chronic liver disease, such as chronic hepatitis and liver cirrhosis, which were observed in 130 (41.5 %), and 173 (55.3 %) patients, respectively (Table 2).
Operative mortality
In this series, 17 patients (4.7 %) died while hospitalized. Three patents died before POD 3 because of multiple organ failure following massive hemorrhage and transfusion during the operation; the others died at median POD 22 (range: 8–72 days) because of PHLF followed by sepsis and multiple organ failure.
Results of biochemical testing
We investigated the sensitivity and specificity of biochemical tests on each postoperative day using ROC curve analysis. Prothrombin time and bilirubin on POD 5 and 7 showed a significant area under the curve (AUC). The cutoff values for PT and bilirubin were 65 % and 38 μmol/L on POD 5 and 55 % and 32 μmol/L on POD 7, respectively.
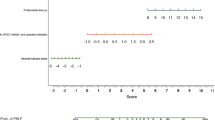
When the new cutoff values were compared with the “50–50” criterion, only the combination of PT and bilirubin on POD 5 showed significant superiority. The new combination of PT and bilirubin on POD 5 showed the higher AUC (i.e., 0.8402) compared with the AUC of the “50–50” criterion (i.e., 0.6396). This was a statistically significant difference (p = 0.0176) (Fig. 1). Though the new combination had a lower specificity (91 %) than the specificity (99.5 %) of the “50–50” criterion, it had a statistically higher sensitivity (p = 0.002; odds ratio [OR], 9.17; 78.6 %) and a similar accuracy (p = 0.090; OR, 0.55; 88.6 %) (Table 3).
Univariate and multivariate analysis for operative mortality
Univariate analysis revealed the following features associated with operative mortality: age (p = 0.035; OR 1.07), major operation (p = 0.05; OR, 4.46), operative time longer than 360 min (p = 0.009; OR, 3.75), estimated blood loss greater than 1,000 mL (p = 0.007; OR, 4.38), intraoperative transfusion (p = 0.003; OR, 5.65), and PT <65 % and bilirubin ≥38 μmol/L on POD 5 (p < 0.001; OR, 36.45). Median ICG R15 was 11.4 % (3.6–29.2 %) in the patients who died, and was not associated with operative mortality. Multivariate analysis revealed that only PT <65 % and bilirubin ≥38 μmol/L on POD 5 significantly correlated with operative mortality (p < 0.001; OR, 82.29) (Table 4).
Discussion
In liver surgery, the range of liver parenchyma disease for resection has been extended with the development of advanced surgical techniques, and the possibility of treatment via hepatectomy has increased even in patients with fibrosis, liver cirrhosis, severe fatty liver, and decreased liver function [22]. The combination of fibrosis of the liver, fatty liver, and liver cirrhosis provokes local ischemia and delays regeneration of the liver, increasing the possibility of ischemic reperfusion injury [23, 24]. This risk increases the possibility of PHLF in patients with underlying liver disease following major hepatectomy.
Therefore, a method for the early detection of mortality from irreversible PHLF has been the focus of continuous attention within the liver resection sector. To date, many studies have suggested varying definitions of liver failure [4, 13, 14, 20, 25–28], but no agreed upon definition has been developed because of the wide variations in underlying liver disease, diagnosis, and surgical methods.
Many previous studies have adapted serum bilirubin and PT as parameters for defining PHLF leading to operative mortality. Bilirubin and PT can be examined objectively and easily during the postoperative follow-up period and are seen as reasonable indicators of liver function. In the present study, results of other biochemical tests (blood urea nitrogen, creatinine, albumin, platelets, alanine aminotransferase, and aspartate aminotransferase) did not show significant predictability. However, the reported cutoff values for PT and bilirubin have been reported to be very different [14]. Most previous studies defining PHLF have been conducted in heterogeneous patient populations. When the underlying diseases of subjects were examined, the rate of chronic hepatitis or liver cirrhosis was 0–50.9 %, and diagnosis of patients was variable. However, in the present study, 96.4 % of patients had hepatitis virus infection and all patients underwent liver resection because of hepatocellular carcinoma. In addition, all liver resections were performed by a single surgeon. Therefore, our study might overcome the limitation of the heterogeneity of many previous studies.
The “50–50” criterion has been well recognized as an indicator for PHLF, and several studies have compared their results with the “50–50” criterion. When the.
“50–50” criterion was applied to our patients, it showed low sensitivity (28.6 %). However, our new combination of PT and bilirubin showed high sensitivity (78.6 %), AUC (0.8402) and similar accuracy (88.6 %). Though the positive predictive value (PPV) (39.3 %) of our criterion was lower than the PPV (80 %) of “50–50” criterion, it did not have statistical significance (p = 0.093). The negative predictive value NPV might have a more significant value than the PPV as a screening test to detect mortality early, though it might lead to overtreatment of patients who might not progress toward PHLF.
According to the definition of PHLF suggesting by ISGLS, the mortality rate associated with PHLF in our study was 4.7 %. This finding was also similar to the mortality less than 5 % cited in previous reports. None of our patients received rescue liver transplantation or ALS, although ALS has been reported to improve neurological symptoms, decrease biochemical parameters, and extend the time waiting for liver transplantation in patients with acute liver failure [18]. In addition, ALS enhances the 30-day survival rate of patients with hepatorenal syndrome [29]. In a prospective, confirmative study on the “50–50” criterion in ICU patients, Paugam-Burtz et al. [19] reported that use of the molecular adsorbents recirculating system (MARS) in five liver failure patients extended the time that two patients were able to wait for liver transplantation.
In conclusion, in this study, we found that the combination of PT <65 % and bilirubin ≥38 μmol/L on POD 5 had high sensitivity as a valuable early predictor of mortality from irreversible PHLF. Although it remains to be verified by prospective studies whether this combination of factors is a consistent and valuable predictor, intensive treatment should be initiated in patients who have the combination of PT <65 % and bilirubin ≥38 μmol/L on POD 5. However, the question of whether to perform ALS or liver transplantation should be decided by physician’s judgments based on the patient’s clinical status (ascites, encephalopathy, and multiorgan dysfunction).
References
Foster JH, Berman MM (1977) Solid liver tumors. Major Probl Clin Surg 22:1–342
Belghiti J, Hiramatsu K, Benoist S et al (2000) Seven hundred forty-seven hepatectomies in the 1990s: an update to evaluate the actual risk of liver resection. J Am Coll Surg 191:38–46
Cohnert TU, Rau HG, Buttler E et al (1997) Preoperative risk assessment of hepatic resection for malignant disease. World J Surg 21:396–400. doi:10.1007/PL00012260 discussion 401
Imamura H, Seyama Y, Kokudo N et al (2003) One thousand fifty-six hepatectomies without mortality in 8 years. Arch Surg 138:1198–1206 discussion 1206
Jarnagin WR, Gonen M, Fong Y et al (2002) Improvement in perioperative outcome after hepatic resection: analysis of 1, 803 consecutive cases over the past decade. Ann Surg 236:397–406 discussion 406–397
Sitzmann JV, Greene PS (1994) Perioperative predictors of morbidity following hepatic resection for neoplasm. A multivariate analysis of a single surgeon experience with 105 patients. Ann Surg 219:13–17
Cucchetti A, Ercolani G, Vivarelli M et al (2006) Impact of model for end-stage liver disease (MELD) score on prognosis after hepatectomy for hepatocellular carcinoma on cirrhosis. Liver Transpl 12:966–971
Dinant S, De Graaf W, Verwer BJ et al (2007) Risk assessment of posthepatectomy liver failure using hepatobiliary scintigraphy and CT volumetry. J Nucl Med 48:685–692
Farges O, Malassagne B, Flejou JF et al (1999) Risk of major liver resection in patients with underlying chronic liver disease: a reappraisal. Ann Surg 229:210–215
Karoui M, Penna C, Amin-Hashem M et al (2006) Influence of preoperative chemotherapy on the risk of major hepatectomy for colorectal liver metastases. Ann Surg 243:1–7
Kawano Y, Sasaki A, Kai S et al (2008) Short- and long-term outcomes after hepatic resection for hepatocellular carcinoma with concomitant esophageal varices in patients with cirrhosis. Ann Surg Oncol 15:1670–1676
McCormack L, Petrowsky H, Jochum W et al (2007) Hepatic steatosis is a risk factor for postoperative complications after major hepatectomy: a matched case-control study. Ann Surg 245:923–930
Mullen JT, Ribero D, Reddy SK et al (2007) Hepatic insufficiency and mortality in 1,059 noncirrhotic patients undergoing major hepatectomy. J Am Coll Surg 204:854–862
Rahbari NN, Garden OJ, Padbury R et al (2011) Posthepatectomy liver failure: a definition and grading by the International Study Group of Liver Surgery (ISGLS). Surgery 149:713–724
Banares R, Nevens F, Larsen FS et al (2010) Extracorporeal liver support with the molecular adsorbent recirculating system (MARS) in patients with acute-on-chronic liver failure (AOCLF). J Hepatol 52:S459–S460
Hassanein TI, Schade RR, Hepburn IS (2011) Acute-on-chronic liver failure: extracorporeal liver assist devices. Curr Opin Crit Care 17:195–203
Jalan R, Sen S, Williams R (2004) Prospects for extracorporeal liver support. Gut 53:890–898
Mitzner SR, Stange J, Klammt S et al (2000) Improvement of hepatorenal syndrome with extracorporeal albumin dialysis MARS: results of a prospective, randomized, controlled clinical trial. Liver Transpl 6:277–286
Paugam-Burtz C, Janny S, Delefosse D et al (2009) Prospective validation of the “fifty–fifty” criteria [sic] as an early and accurate predictor of death after liver resection in intensive care unit patients. Ann Surg 249:124–128. doi:10.1097/SLA.0b013e31819279cd
Balzan S, Belghiti J, Farges O et al (2005) The “50–50 criteria” [sic] on postoperative day 5: an accurate predictor of liver failure and death after hepatectomy. Ann Surg 242:824–828 discussion 828–829
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845
Truty MJ, Vauthey JN (2010) Surgical resection of high-risk hepatocellular carcinoma: patient selection, preoperative considerations, and operative technique. Ann Surg Oncol 17:1219–1225
Garcea G, Maddern GJ (2009) Liver failure after major hepatic resection. J Hepatobiliary Pancreat Surg 16:145–155
Min S, Kim S, Lee S et al (2011) The effect of preconditioning on liver regeneration after hepatic resection in cirrhotic rats. Clin Mol Hepatol 17:139–147
Farges O, Belghiti J, Kianmanesh R et al (2003) Portal vein embolization before right hepatectomy: prospective clinical trial. Ann Surg 237:208–217
Martin RCG, Jarnagin WR, Fong Y et al (2003) The use of fresh frozen plasma after major hepatic resection for colorectal metastasis: Is there a standard for transfusion? J Am Coll Surg 196:402–409
Schindl MJ, Redhead DN, Fearon KCH et al (2005) The value of residual liver volume as a predictor of hepatic dysfunction and infection after major liver resection. Gut 54:289–296
Vauthey JN, Pawlik TM, Abdalla EK et al (2004) Is extended hepatectomy for hepatobiliary malignancy justified? Ann Surg 239:722–730 discussion 730–722
Heemann U, Treichel U, Loock J et al (2002) Albumin dialysis in cirrhosis with superimposed acute liver injury: a prospective, controlled study. Hepatology 36:949–958
Acknowledgments
This work was supported by a grant from the Korea Healthcare Technology R&D Project, Ministry for Health, Welfare & Family Affairs, Republic of Korea (A084120).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, S.H., Kang, D.R., Lee, J.G. et al. Early Predictor of Mortality due to Irreversible Posthepatectomy Liver Failure in Patients with Hepatocellular Carcinoma. World J Surg 37, 1028–1033 (2013). https://doi.org/10.1007/s00268-013-1959-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-013-1959-z