Abstract
Objective
This study aimed to compare the spreader graft and flap techniques, which are used in nasal valve surgery, based on measurements of nasal valve angles using computed tomography.
Material and Method
In this retrospective study, all patients’ right and left internal nasal valve angles were measured from coronal computed tomography images taken preoperatively and in the third postoperative month. A paired t-test and independent t-test were used to compare continuous numerical variables.
Results
There were 52 patients with 104 valves in the spreader flap group and 54 patients with 108 valves in the spreader graft group, with a mean age of 27.76 ± 8.16 years. The angles were found to be statistically significantly higher in the postoperative period (p<0.001) in all patients. While the angles did not differ significantly between the flap and graft groups in the preoperative period, they were significantly higher in the flap group in the postoperative period (p<0.001).
Discussion
It is essential to preserve nasal valve function in rhinoplasty. The findings show that a spreader flap is superior to a spreader graft, although both techniques increase internal nasal valve function.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Rhinoplasty aims to improve the nose both functionally and esthetically. The nasal airway has two anatomical frameworks: the internal and external nasal valves. The internal nasal valve is the narrowest part of the nasal airway between the nasal septum and the upper lateral cartilage [1, 2]. It is essential to maintain 10°–15° angles in this essential anatomical structure for proper nasal airflow [3].
Spreader graft and flap techniques are the most commonly used methods to increase the internal nasal valve angle during surgery. The spreader graft technique is the gold standard method, which was first described by Sheen in 1984 [1]. It is performed by placing a cartilaginous graft between the septum and upper lateral cartilage. Meanwhile, a spreader flap involves folding upper lateral cartilages over themselves. To determine which of these two techniques is superior, this study compared the spreader graft and flap techniques used in nasal valve surgery based on angles obtained using computerized tomography.
Material and Method
This study was conducted in conformity with the World Medical Association Declaration of Helsinki and was approved by the local ethical committee (2022/034). Fifty-four patients with spreader grafts and fifty-two patients with spreader flaps who were operated on between January 2020 and July 2022 were included in the study. All patients underwent open rhinoplasty, including nasal valve surgery, and were randomly divided into two groups. The right and left nasal valves were evaluated in each patient. In this retrospective study, the internal nasal valve angle was measured and statistically compared using paranasal sinus computed tomography images, which were routinely requested before and three months after rhinoplasty. Exclusion criteria were a follow-up period of fewer than three months, smoking, allergic disease, and the absence of radiological images at the desired time. Satisfaction was evaluated based on the visual analogue scale (VAS) by the primary author. Functional assessment was performed with a Cottle maneuver and verified by two authors.
While performing the septoplasty, the upper lateral crura and septum were separated by an elevator. After the removal of the osseous and cartilaginous hump, the submucoperichondrial tunnel was undermined by an elevator under the nasal bone.
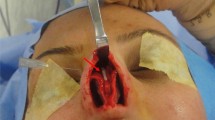
During the spreader flap technique, upper lateral cartilages were folded over themselves after scoring in the patients with thick upper lateral cartilages. Scoring was not performed if the upper lateral cartilages were not thick enough (min. 2 mm). Upper lateral cartilages and septum were sutured with 5/0 polydioxanone. Horizontal mattress sutures were placed from the caudal to the cephalic after the septum and upper lateral cartilages were fixed with a 30-gauge needle (Fig. 1).
In the spreader graft technique, cartilaginous grafts obtained from septal cartilage were placed between the septum and the upper lateral cartilages (min. 2 mm). After bilateral fixation of the grafts, horizontal mattress sutures were placed from the caudal to the cephalic with 5/0 polydioxanone (Fig. 2). Both techniques are illustrated in Fig. 3.
One hundred patients were examined based on 16-channel multislice computed tomography (CT) with a slice thickness of 0.6 mm using the bone algorithm. Axial and coronal images were obtained. Internal nasal valve angles were assessed from the coronal slices, which were taken from the anterior side of the inferior nasal concha (Fig. 4).
The Statistical Package for Social Sciences program was used for all procedures (IBM SPSS Statistics 21.0, IBM Corporation, Armonk, NY, USA). The Kolmogorov–Smirnov test was used to determine the normality distribution of the scale variables. For continuous numerical variables, descriptive statistics are presented as means and standard deviations. Categorical variables are represented by the number of cases and percent. A paired t-test and independent t-test were used to compare continuous numerical variables. Unless otherwise specified, the results were deemed statistically significant at p< 0.05.
Results
A total of 106 patients, 30 men and 76 women, with a mean age of 27.76 ± 8.16 (19–57 years), were included in the study. There were 52 patients in the spreader flap group and 54 patients in the spreader graft group.
In all patients, the angles were found to be significantly higher in the postoperative period (p<0.001). For both the graft and flap techniques, the angles were found to be significantly higher in the postoperative period (p<0.001 and p<0.001, respectively). While the angles did not differ significantly between the flap and graft groups in the preoperative period, they were significantly higher in the flap group in the post-treatment period (p<0.001) (Table 1). The average VAS score was 8.79±0.99, with no difference between the flap and graft techniques (p=0.727) (Table 2). Preoperative and postoperative images of the patients undergoing these two techniques are shown in Figs. 5 and 6. The Cottle maneuver tests were negative in all patients, and dorsal esthetic lines were acceptable. No inverted V deformities were detected in any patients.
Discussion
The internal nasal valve is an anatomical framework that was first described by Mink in the 1920s as the angle between the septum and the upper lateral cartilage [4]. Normally, the internal nasal valve angle between the septum and upper lateral cartilage should be 10°–15° [3, 5]. In rhinoplasty, after removing the bone and cartilaginous hump, it is essential to reconstruct the internal nasal valve. The use of spreader grafts and flaps is controversial in nasal valve surgery. In this study, the two techniques were compared based on the nasal valve angle, VAS score, and Cottle maneuver.
In spreader flap surgery, the perichondrium on the upper lateral cartilage is peeled 5–10 mm, and the upper lateral cartilage is folded over itself to be in line with the nasal bone after the hump is removed [6, 7]. Bercowitz used the term “spreader flap” in the 1990s for this technique, which was first described by Fomon in 1950 as an auto-spreader flap [8]. It can be performed with or without scoring in patients who require nasal hump reduction with a minimum height of 2 mm [8]. Both techniques are applied to provide nasal vault support and prevent nasal collapse in rhinoplasty [9]. The main advantage of the spreader flap is that it is faster and minimizes complications on the donor side. Further, it is simple and convenient after hump reduction due to excess cartilage tissue use. It widens the angle of the internal nasal valve due to the spring effect of folded, viable, and vascularized upper lateral cartilage. In addition, placement is easier with the spreader flap than with the spreader graft. Modifications have been developed, such as composite flaps, adding osseous tissue to provide stronger and longer support by preventing open roof deformity and insufficiency of upper lateral cartilage [10]. The dorsum can be widened, and this technique can be used to narrow lateral cartilage. In their study, Saedi et al. [9] did not detect differences between the spreader flap and control groups in the early postoperative period in terms of satisfaction and function.
In the spreader graft technique, a cartilage graft originating from the septum, auricle, or rib is placed between the bilateral upper lateral cartilage and the septum or in a pocket created submucosally. It was first described by Sheen in 1984 [1]. Currently, the spreader graft is the gold standard method for improving the nasal vault [11, 12]. It increases the angle of the nasal valve by pushing the upper lateral cartilage away from the septum [2]. Many modifications have been described in the literature related to the donor area, type, and shape. In addition to the traditional bilateral rectangular shape, it can have a unilateral or L shape [13]. Spreader grafts are used in rhinoplasty for many purposes, including improving dorsal esthetic lines, widening the dorsum and nasal vault, straightening the septum, and correcting septal deviation [5, 14]. It is the most commonly used technique for nasal mid-vault reconstruction [5, 15,16,17]. Observable complications include nasal airway problems due to graft mispositioning and a dorsal hump [17]. Additionally, saddle nose deformity has been reported after rhinoplasty using a spreader graft associated with ischemic nasal septum necrosis due to spreader graft compression [2]. In this regard, the spreader flap appears to be more advantageous because it is vascularized. In our study, while postoperative nasal valve angle measurements were higher with both techniques, better results were obtained with the spreader flap.
Both techniques provide anatomical support to the nasal vault and widen the nasal valve angle. Buba et al. did not find differences between the two methods in terms of Nasal Obstruction Symptom Evaluation (NOSE) scores [18]. In our study, there were no differences between the spreader flap and spreader graft when comparing VAS scores. In addition, anatomical support was provided with both techniques and no inverted V deformities were detected.
Rhinoscopy and Cottle’s maneuver are clinical tools for evaluating the internal nasal valve, but they are not objective. In the literature, questionnaires are frequently used to gather patients’ perceptions of the function or appearance of the nasal valve. However, the nasal valve angle can be measured objectively using computed tomography with quantitative values [3, 19]. In fact, coronal images are commonly used to assess the nasal valve angle. One of the limitations of this technique is that the position of the selected image is not standardized [3]. In this study, the images that were taken from one cut anterior to the inferior nasal concha were used for standardization [20]. Patients were evaluated for functional outcomes using the Cottle maneuver test, and the results were negative in all patients. In addition, all nasal valves were acceptable based on the images obtained by computed tomography.
While some studies have not found any differences between the two techniques, such as Shafaeei et al., Bubo et al., and Keyhan et al. [11, 18, 20,21,22], others have demonstrated the superiority of the spreader flap, such as Hussein et al. [1]. In our study, the postoperative nasal valve angles were higher compared to the preoperative values using both techniques. However, the postoperative nasal valve angles were higher in the spreader flap group, while there were no differences in preoperative measurements.
The inclusion of early postoperative period evaluations is one of the limitations of this study. We will share postoperative long-term follow-up results in future studies. In this study, CT images and internal nasal valve angles were used for objective quantitative results, but they could be combined with rhinometry and endoscopic examinations in future studies.
In conclusion, maintaining nasal valve function is essential in rhinoplasty. According to this report, while the spreader flap was superior to the spreader graft in terms of increasing the width of the angles of the internal valve (measured objectively by CT), both techniques were successful when compared with preoperative internal nasal valve angle. Also, functional outcome which was evaluated by using Cottle maneuver and patient satisfaction according to the VAS scores were achieved by both techniques. This study quantitatively compared the spreader graft and spreader flap, both of which are effective in terms of functional outcomes. So, while our quantitative data showed that spreader flap was superior to the spreader graft, it was not observed in clinical findings.
References
Hussein WK, Elwany S, Montaser M (2015) Modified autospreader flap for nasal valve support: utilizing the spring effect of the upper lateral cartilage. Eur Arch Otorhinolaryngol 272(2):497–504
Eweiss A (2023) Is there a risk of saddle nose deformity after spreader grafts and flaps? Facial Plast Surg 39(1):77–85
Poetker DM, Rhee JS, Mocan BO, Michel MA (2004) Computed tomography technique for evaluation of the nasal valve. Arch Facial Plast Surg 6(4):240–243
Weeks DM, Walker DD, Dutton JM (2012) Anatomical comparison of minimally invasive nasal valve procedures. Arch Facial Plast Surg 14(3):189–192
Uebel CO, Matta R (2017) Alar cartilage-an alternative for spreader graft in primary rhinoplasty. Eur J Plast Surg 40(5):417–426
Buba CM, Patel PN, Saltychev M, Kandathil CK, Most SP (2022) The safety and efficacy of spreader grafts and autospreaders in rhinoplasty: a systematic review and meta-analysis. Aesthetic Plast Surg 46(4):1741–1759
Pepper JP, Baker SR (2011) The autospreader flap in reduction rhinoplasty. Arch Facial Plast Surg 13(3):172
AlAwadh IH, Bogari A, Assiri H, Alabduljabbar Z, AlNassar R, Hudise J, AlArfaj A (2022) A novel technique for spreader flap by folding the dorsal hump in patients undergoing primary rhinoplasty. J Craniofac Surg 33(8):2653–2658
Saedi B, Amali A, Gharavis V, Yekta BG, Most SP (2014) Spreader flaps do not change early functional outcomes in reduction rhinoplasty: a randomized control trial. Am J Rhinol Allerg 28(1):70–74
Gerbault O (2019) Commentary on: the composite spreader flap. Aesthet Surg J 39(2):148–149
Keyhan SO, Fallahi HR, Cheshmi B, Jafari Modrek M, Ramezanzade S, Sadeghi E (2022) Spreader graft vs spreader flap in rhinoplasty: a systematic review and meta-analysis of aesthetic and functional outcomes. Aesthet Surg J 42(6):590–602
Gruber RP, Melkun ET, Woodward JF, Perkins SW (2011) Dorsal reduction and spreader flaps. Aesthet Surg J 31(4):456–464
Apaydin F (2016) Rebuilding the middle vault in rhinoplasty: a new classification of spreader flaps/grafts. Facial Plast Surg 32(6):638–645
Gerecci D, Perkins SW (2019) The use of spreader grafts or spreader flaps-or not-in hump reduction rhinoplasty. Facial Plast Surg 35(5):467–475
Grigoryants V, Baroni A (2013) The use of short spreader grafts in rhinoplasty for patients with thick nasal skin. Aesthetic Plast Surg 37(3):516–520
Sirinoglu H, Yesiloglu N, Ersoy B (2016) A new perspective for spreader graft use in severely deviated septum: is septal continuity an obligation for a stable and straight nasal septum? Facial Plast Surg 32(4):460–468
Bitik O, Kamburoglu HO, Uzun H (2019) The composite spreader flap. Aesthet Surg J 39(2):137–147
Shafaeei Y, Zare NJ (2019) A comparison of the aesthetics outcomes and respiratory side effects of the use of spreader flap and spreader graft techniques in open rhinoplasty. J Craniofac Surg 30(8):2546–2548
Karameşe M, Akdağ O, Akatekin A, Koplay TG, Koplay M, Tosun Z (2016) Extracorporeal septoplasty combined with valve surgery in rhinoplasty patients. Ann Plast Surg 76(1):7–12
Bloom JD, Sridharan S, Hagiwara M, Babb JS, White WM, Constantinides M (2012) Reformatted computed tomography to assess the internal nasal valve and association with physical examination. Arch Facial Plast Surg 14(5):331–335
Hassanpour SE, Heidari A, Moosavizadeh SM, Tarahomi MGoljanian A, Tavakoli S (2016) Comparison of aesthetic and functional outcomes of spreader graft and autospreader flap in rhinoplasty. World J Plast Surg 5(2):133–138
Zeid NG, Mohamed AS, ElSayed ElFM, Azooz KO, Aleryan MM, Abd Elmottaleb Sabaa M (2020) Objective comparison between spreader grafts and flaps for mid-nasal vault reconstruction: a randomized controlled trial. Plast Surg 28(3):137–141
Funding
None
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of ınterest
The authors declare that they have no conflicts of interest to disclose.
Human and Animal Rights
This manuscript does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
Informed consent form was obtained from the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Koplay, T.G., Inan, I. & Ozer, H. Comparison of the Effects of Spreader Graft Versus Spreader Flap on Nasal Valve Angle in Open Approach Rhinoplasty. Aesth Plast Surg 47, 2625–2631 (2023). https://doi.org/10.1007/s00266-023-03598-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03598-3