Abstract
Background and Purpose
Spreader grafts and spreader flaps are one of the most common techniques utilized in rhinoplasty surgeries. The aim of this study was to determine the complications, satisfaction, and revision rates associated with spreader grafts and spreader flaps and to compare these two modalities.
Materials and Methods
PRISMA guidelines were followed for conducting this systematic review. The authors searched the literature systematically for pertinent materials in PubMed/Medline and Google Scholar. Inclusion criteria of this search included: randomized and non-randomized clinical trials, cohorts, and case series with more than 5 participants on rhinoplasty using spreader grafts or spreader flaps with detailed report either on complications, revision, and satisfaction rates. Furthermore, exclusion criteria included: any cadaveric or non-human study, case reports, technical notes, and review articles.
Results
The initial literature search yielded a total of 193 studies. Following screening each paper and implementing the inclusion and exclusion criteria, 40 articles were chosen. In the spreader graft group, from 21 studies reporting complications, 6 of them reported no complication. The most common complications were nasal obstruction, inverted V deformity and open roof deformity, deviation, and infection. In the spreader flap group, from 6 studies reporting any existing complications, 1 reported no complications. Five other studies reported some degree of complications. In terms of revision rate, 10 patients (0.62%) underwent revision surgery after spreader graft placement, while only 2 patients (0.35%) revised surgically in the spreader flap group.
Conclusion
These two methods seem to have no significant difference in terms of complication rates, and both are recommended as a choice in middle vault reconstruction when each of their clinical use is indicated.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Despite several challenges and complications, rhinoplasty had been one of the most common plastic surgeries through past decades. Complications such as inverted V deformity, internal nasal valve impairment, and nasal obstruction are among important issues that may lead one to an undesirable revisional surgery [1,2,3]. During a rhinoplastic procedure, the surgeon should consider midvault preservation, particularly in patients with a narrow roof, thin skin, and weak tissues who are more susceptible to nasal valve collapse [4]. Over the years, several techniques have been described and performed to maintain a stable nasal midvault such as spreader grafts [5], upper lateral cartilage (ULC) suspension[6], butterfly graft [7], upper lateral splay graft [8], and bending the ULC [9].
In the 1980s, spreader grafts were introduced by Sheen et al. [5] for treating patients with short nose syndrome. Later, their usage expanded to a variety of rhinoplastic procedures including nasal tip support or straightening a deviated septum. Placement of a spreader graft between the ULCs and the septum increases the cross-sectional area of the internal nasal valve which is the narrowest part of the airway, but harvesting a cartilaginous graft is a necessity in this method, and inaccuracy in suturing may cause graft displacements. Furthermore, widening of the nasal dorsum might be another unwanted consequence of this technique. In order to overcome the shortcomings, some changes such as pedestal spreader grafts [10], triangular spreader grafts [11], and diced inverted Y-shaped spreader grafts [12] have been made.
Seyhan et al. [9] described an alternative that was simpler and eliminated the need for harvesting (later in 1998 named as spreader flap technique). In this maneuver, the excess height of ULC is bent inwardly and then sutured, so decreasing the valve area would be avoided. Multiple modifications have been described for this method, such as flaring-type spreader flaps, support-type spreader flaps, and partial spreader flaps in order to adjust the width and shape of the middle nasal vault according to patients’ individual requirements [10].
Considering the shortcomings and differences in surgeons’ opinions, we aimed to assess the complication, satisfaction, and revision rates of the two techniques in a systemic review. Some subjective measurements (NOSE and VAS questionnaire) noted in papers pre- and postoperatively were the secondary purposes.
Materials and Methods
PRISMA Registration
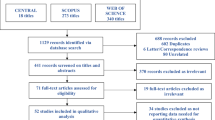
We followed the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines for conducting this systematic review (Fig. 1). Our search protocol was specified and registered at PROSPERO (international prospective register of systematic reviews) no. CRD42021239732.
PICO Question
Patient: Patients undergoing reconstructive or cosmetic rhinoplasty using spreader grafts and spreader flaps
Intervention: reconstructive or cosmetic rhinoplasty of nasal dorsum using spreader grafts and spreader flaps
Comparison: the results for spreader grafts were compared with the results for spreader flaps
Outcome: complication rate, satisfaction rate, revision rate, and graft harvesting site comorbidities of the two techniques
Search Strategy
The literature was searched systematically for pertinent materials in PubMed/Medline and Google Scholar up to and including March 2021 with no time and language restrictions. The reference list of included studies was searched manually for potential materials. The following search strategies were used for each database:
-
1. PubMed/Medline: (107 papers)
("spreader graft"[Title] OR "spreader flap"[Title] OR "cartilage grafts"[Title] OR "cartilaginous graft"[Title] OR "cartilage graft"[Title]) AND ("Rhinoplasty"[Title] OR "Rhinosurgery"[Title] OR "nasal vault"[Title] OR (("nasalance"[All Fields] OR "nasality"[All Fields] OR "nasalization"[All Fields] OR "nasalized"[All Fields] OR "nasally"[All Fields] OR "nose"[MeSH Terms] OR "nose"[All Fields] OR "Nasal"[All Fields] OR "nasals"[All Fields]) AND "vault collapse"[Title]) OR "crooked nose"[Title] OR ("Humpy"[All Fields] AND "nose"[Title]))
-
2. Google Scholar: (32, 17 papers)
Concept 1: allintitle: allintitle: Rhinoplasty OR Rhinosurgery OR Rhinosurgeries OR "Nasal vault" OR "Nasal vault collapse" OR "Crooked nose" OR "Humpy nose" "Spreader graft"
Concept 2: allintitle: Rhinoplasty OR Rhinosurgery OR Rhinosurgeries OR "Nasal vault" OR "Nasal vault collapse" OR "Crooked nose" OR "Humpy nose" "Spreader flap"
Inclusion and Exclusion Criteria
The inclusion criteria of the current review were as follows:
Randomized and non-randomized clinical trials, cohorts, and case series with more than 5 participants on rhinoplasty using spreader grafts or spreader flaps with detailed report either on complications, revision, and satisfaction rates were included. There was no time limitation for papers, and materials written in English up to April 2021 were included.
The exclusion criteria of the current review were as follows:
Any cadaveric or non-human study, case reports, technical notes as well as review papers were excluded.
Study Selection Process
Two reviewers conducted a duplicate searching process independently in order to determine suitable studies using the inclusion and exclusion criteria. Instances of divergence were resolved by consulting a third investigator. The full-text version of studies was obtained for all titles that appeared to meet the inclusion criteria. After that each paper was studied at least twice by two independent reviewers.
Data Extraction
Whenever applicable, the following data were retrieved from the finally included studies by an author based on a predefined checklist worksheet and supervised by two other authors for accuracy. In case of missing data or any hesitancy, the corresponding author of the study was contacted via emails, up to two emails, as the poorly reported outcomes of included materials could thread the validity of our work. The following data were extracted: first author, year of publication, study type, mean age, sex, number of cases, mean follow-up (range), primary/secondary or tertiary rhinoplasty, open or closed technique, main outcomes, satisfaction rate (percent), reported complications.
Risk of Bias Assessment
Quality assessment of our included studies was done independently by two reviewers, and instances of divergence were resolved by consulting a third investigator. We used Newcastle Ottawa scale [13] for grading cohort studies and Cochrane ROB2 tool [14] for clinical trials whether they were randomized or not [15] (Tables 6 and 7).
Result
Study Selection
The initial literature search yielded a total of 193 studies. Following screening title and abstract and eliminating duplicates, 131 papers excluded and 62 papers left for full-text screening. Three full text did not retrieve, and among 59 remained studies, we excluded 19 papers due to low number of cases, not to be an original article, different technique, combination therapy, or cadaveric study. Finally, 40 studies were included, as reported in the PRISMA flow diagram.
Study Characteristics
Spreader grafts were used in 28, and spreader flaps were used in 8 studies. Four papers discussed both spreader grafts and spreader flaps.
In the spreader graft group, a total of 1596 patients were enrolled in this review that 406 (25.4%) of them were treated through an endonasal approach, while the rest of the surgeries were performed open. Except for 92 patients who were treated with synthetic material (porous polyethylene), the other patients' spreader grafts were made from their cartilaginous tissues (mostly septal cartilage). In total, 52% of them were females, with a mean age of 31.9 years. The mean follow-up period after surgery was 13.3 months (3 months to 5 years range). Also in the spreader flap group, a total of 570 patients were enrolled that all were treated through an open approach except 39 (6.84%) who were treated endonasal. In total, 66% of them were females (2 studies did not mention the sexuality of their patients [16, 17]), with a mean age of 27.04 years old (4 papers did not mention the mean age). The mean follow-up period after surgery was 13.5 months. Table 2 shows brief details of our included papers' characteristics.
In the case of primary or revision rhinoplasty, in the spreader graft group, 5 studies did not mention their patients' characteristics [12, 17,18,19,20]. Of 1410 remained patients, 233 had undergone revision surgery and the rest were primary. In the spreader flap group, from 9 studies reporting surgical phase, only 2 studies included revision cases (13 patients). Tables 1 and 2 present a summary of our included papers' characteristics.
Patient Satisfaction
In the spreader graft group, 20 studies noted nothing about their patients' satisfaction after surgery. Among 12 other studies, the mean satisfaction rate was 93.7%. Also in the spreader flap group, 6 studies did not notice anything about their patients' satisfaction, while in the other 6 papers, the mean satisfaction rate was 94% which was not different from the spreader graft group significantly.
Complications
From all included papers, 13 studies did not mention anything about complications [12, 19, 21,22,23,24,25,26,27,28,29,30,31] in the spreader graft group. From 22 studies reporting complications, 6 of them reported no complications [11, 32,33,34,35,36], and in other studies, reported complications are as mentioned in Table 3. The most common complications were nasal obstruction (in 9 patients), different kinds of deformity such as inverted V deformity and open roof deformity (in 9 patients), deviation (in 7 patients), and infection (in 7 patients). Other noticeable complications mentioned were irregularity, extrusion, overcorrection, hematoma, columella scar, nasal tip rotation, erythema at the auricular donor site, and epistaxis.
In the spreader flap group, from 6 studies reporting any existing complications, 1 reported no complications [37]. Other studies' postsurgical complications are noticed in Table 3.
In a study [38], 1 aesthetically narrow midvault was reported, while dorsum fullness (in 3 patients) and deviation (in 1 patient) were seen in another record [16]. One paper mentioned nasal breathing problems in 12 of their included patients due to rhinitis and pinch nose [39]. Ozmen et al. [40] reported synechiae in 8 of their patients postoperatively. The other study compared respiratory complications in both spreader graft and spreader flap groups [17].
Revision Rate
Ten patients (0.62%) underwent revision surgery after spreader graft placement, while only 2 patients (0.35%) revised surgically in the spreader flap group.
Subjective Measurements
In the spreader graft group, 9 studies measured their patients' nasal obstruction symptom evaluation (NOSE) scores pre- and postoperatively [11, 19, 21, 29, 30, 33, 36, 41, 42]. All of them reported an improvement in postoperative evaluations (Table 4). In the spreader flap group, 4 papers reported NOSE scores pre- and postoperatively [19, 21, 24, 27]. They also noted an improvement in the postoperative scores compared with the preoperative ones (Table 5).
In the spreader graft group, 8 studies used visual analog scale (VAS) questionnaire to assess their patients' opinions about the result of surgery [11, 21, 23, 25, 28, 42,43,44]. Six papers reported an improvement in mean postoperative VAS scores. One of them reported no significant difference before and after rhinoplasty [44]. One remained study reported overall improvement though there were unsatisfied patients [23] (Table 4). In the spreader flap group, 4 papers reported VAS scores pre- and postoperatively [21, 23, 27, 37]. Three studies reported an improvement in the mean postoperative scores, while one study [23] noted unsatisfaction in some of their patients and satisfaction in most of them (Table 5).
Discussion
This article is the first systematic review that sought to compare complication and satisfaction rates and subjective measurements between spreader grafts and spreader flaps in patients undergoing rhinoplasty. Our systematic review revealed that there is not a significant difference among the abovementioned factors when comparing spreader grafts and spreader flaps (Tables 6 and 7).
Numerous reasons justify the need for rhinoplasty, among which may be found septal deviation or deformation most commonly. Such abnormalities are frequently associated with functional complications that necessitate a combination of cosmetic and functional rhinoplasty [23]. However, functional and cosmetic features of the nose seem to be closely intertwined; hence, utilizing the correct surgical approach will technically achieve the desired functional and cosmetic outcomes simultaneously [5].
Spreader grafts are one of the long-established techniques utilized in rhinoplasty surgeries. This technique incorporates moving the upper lateral cartilages away from the nasal septum with grafts, therefore increasing the angle between the upper lateral cartilages and septum. The use of grafts improves the function of the nasal cavity and renders aesthetically pleasing contours to the middle nasal vault [45]. Despite its routine use in rhinoplasty procedures, this technique may lead to few complications, one of which includes falling of the graft tissue into the mucoperichondrial pocket and therefore resulting in the movement of the grafts away from their original desired position [26].
In the spreader flap technique, a specific length of perichondrium of the upper lateral cartilages is spread over the whole length of nasal cartilages and the conjunction of the lateral cartilages to the nasal bones is locally released. Nevertheless, this technique also comes with few complications including excessively wide middle nasal vault, an asymmetry in nasal cartilages, the collapse of lateral walls, and reduction of internal nasal valve angle which results in nasal obstruction [46].
While both spreader grafts and flaps can achieve the same results, each has its advantages and disadvantages. Spreader grafts can provide distinct designs and shapes in order to achieve the desired objective. Furthermore, they can be placed into pockets created on either side of the dorsal septum. However, adequate grafting material is required in order to design such grafts. Conversely, spreader flaps provide more limited volumes, which are determined by the thickness of the dorsal edges of the upper lateral cartilages. Moreover, sufficient upper lateral cartilage excess must remain following cartilaginous hump removal in order to provide the adequate inward fold of the cephalic edge of the upper lateral cartilage for flap construction. The supporting literature suggests that 2 mm of residual excess upper lateral cartilage after septal cartilage reduction is considered sufficient for performing spreader flap [38, 47,48,49]. Furthermore, spreader flaps need to be fixed in place using sutures, while spreader grafts can be exempted from this necessity. Furthermore, their use spares the excess cartilage that is otherwise trimmed [50, 51]. Numerous researches have described the indications for these two techniques, including widening of the internal nasal valve, correction of deviated dorsal septum, correction of unilateral asymmetry due to inward curvature of one upper lateral cartilage, preventing delayed contracture deformity of the upper lateral cartilage, and serving as a cantilever to lengthen an overly rotated lobule [5, 52,53,54].
In 2020, a panel of internationally recognized rhinoplasty surgeons participated in a two-part organized communication method summit. The summit transcription was analyzed by thematic content analysis in order to develop a survey encompassing clinical scenarios for primary rhinoplasty. The following key anatomical features were utilized as selection criteria for preferred approach to midvault reconstruction: size of the dorsal hump reduction, width of the midvault relative to the upper vault, presence of dorsal angulation, and presence of nasal obstructive symptoms. In cosmetic scenarios with large dorsal hump reduction in patients with a straight dorsal septum undergoing dorsal hump reduction of greater than 2 mm, the consensus of panel of experts was to use spreader flaps for midvault reconstruction. Conversely, for patients who have dorsal septal angulation, there was a split preference in the method of midvault reconstruction depending on the middle vault width. Preferred methods for these scenarios were asymmetric spreader flaps or asymmetric spreader grafts. In cosmetic scenarios with small dorsal hump reduction in patients with a straight dorsal septum undergoing dorsal hump reduction less than 2 mm, the panel majority preference was the use of spreader grafts. For patients with small dorsal hump reduction with dorsal septal angulation, the general consensus was to use asymmetric spreader grafts for equal and narrow middle vault widths. Furthermore, in cases with a wide midvault, there was still majority preference for the use of asymmetric spreader grafts. In functional scenarios with both small and large dorsal hump reduction with either static or dynamic valvular stenosis, the dominant preference among specialists was the use of spreader grafts [47].
Another issue related to spreader grafts is that weak upper lateral cartilages may not be supportive enough to provide structural stability equivalent to spreader grafts. To our knowledge, no study has specifically investigated the strength/stiffness of ULC's when used in functional cases.
We sought to review and compare the cardinal indicators of complications among these two approaches including extrusion, irregularity, hematoma, overcorrection, deviation (graft displacement), infection, and revision rates. As can be concluded from the results section, in the case of appropriately selected patients, there is not any significant difference between spreader graft and spreader flap techniques in terms of complications.
Comparing the patients’ satisfaction rates following the surgery, the majority of the articles stated very high satisfaction rates among both spreader flap and spreader graft techniques; however, the number of articles comparing these two was limited. ElBestar et al. [21] analyzed the improvement in postoperative patients’ satisfaction using the visual analog scale (VAS), and the difference was found to be statistically insignificant. Furthermore, Hassanpour et al. [23] compared the satisfaction rates, in which the differences were found to be statistically insignificant.
In terms of comparing subjective measurements using the NOSE scores pre- and postoperatively, again the majority of articles in both approaches showed improvements in this score postoperatively. Two papers [19, 21] compared the pre- and postoperative NOSE score in spreader flaps and spreader grafts in which both groups showed a significant improvement; however, the inter-group comparison depicted no significant difference.
Very few studies have compared the complication rates between these two techniques. Shafaeei et al. [17] reported that only in the incidence of obstructive sleep apnea there is a significant difference between the two groups in terms of respiratory complications, with the patients treated with spreader graft technique showing a lower incidence than those treated with spreader flap technique. However, concerning other respiratory complications, no significant difference was observed between these two groups.
A considerable limitation of this review is the paucity of the studies which report any complications or solely compare the complications among these two modalities. The results of our study reflect what has been reported and may not reflect what exactly happens in clinical practice. Also, the risk of bias cannot be completely overlooked due to multiple reasons including the fact that only English literature has been reviewed in this article. Besides, the short follow-up period in some of the articles can lead to a neglect of a significant portion of valuable data regarding long-term complications. We are also aware of the fact that some of the included studies slightly vary from the original intended methods; however, these modifications do not seem to play an important role in the final results; therefore, the decision was made to include these studies as well. To the best of our knowledge, this study is the most comprehensive study to date that has assessed the complication rates of these two techniques based on different indicating factors with reliable statistical tools. Finally, it should be noted that to improve statistical efficiency, further high-quality studies employing larger subject pools, longer follow-ups, and more comprehensive assessments should be conducted in the future.
Conclusion
Based on our systematic review of the complications as reported in the literature, spreader flaps and spreader grafts seem to have no significant difference in terms of complication and revision rates. Of course, overall reporting of complications is relatively deficient, but both techniques can restore the integrity of the middle vault in properly selected cases with no expectation for greater or lesser incidence of complication.
References
Sykes JM, Tapias V, Kim J-E (2011) Management of the nasal dorsum. Facial Plast Surg 27(02):192–202
Keyhan SO, Ramezanzade S, Bohluli B, Fallahi HR, Mirzahoseini S, Nahai F (eds) (2021) Autologous fat injection for augmentation rhinoplasty: a systematic review. Aesthetic Surgery Journal Open Forum. Oxford University Press US
Keyhan SO, Ramezanzade S, Bohluli B, Fallahi HR, Shakiba M, Yates J (2021) A Systematic review and meta-analysis of complications associated with autogenous diced cartilage wrapped in fascia used in nasal dorsum augmentation. Aesthet Surg J 41(9):NP1152–NP1165
Byrd HS, Meade RA, Gonyon DL Jr (2007) Using the autospreader flap in primary rhinoplasty. Plast Reconstr Surg 119(6):1897–1902
Sheen JH (1984) Spreader graft: a method of reconstructing the roof of the middle nasal vault following rhinoplasty. Plast Reconstr Surg 73(2):230–239
Paniello RC (1996) Nasal valve suspension: an effective treatment for nasal valve collapse. Arch Otolaryngol Head Neck Surg 122(12):1342–1346
Clark JM, Cook TA (2002) The ‘butterfly’ graft in functional secondary rhinoplasty. Laryngoscope 112(11):1917–1925
Guyuron B, Michelow BJ, Englebardt C (1998) Upper lateral splay graft. Plast Reconstr Surg 102(6):2169–2177
Seyhan A (1997) Method for middle vault reconstruction in primary rhinoplasty: upper lateral cartilage bending. Plast Reconstr Surg 100(7):1941–1943
Kovacevic M, Riedel F, Göksel A, Wurm J (2016) Options for middle vault and dorsum restoration after hump removal in primary rhinoplasty. Facial Plast Surg 32(04):374–383
Sahin MS, Ozmen OA (2016) Early results and description of a new modification of spreader graft to enlarge nasal valve area: modified triangular spreader graft. J Craniofac Surg 27(4):839–842
El Sherif AF, Kamel IH (2019) The role of a diced inverted Y shaped spreader graft to enhance function in open rhinoplasty. A novel technique. Egypt J Plast Reconstruct Surg 43(2):313–318
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, et al (2000) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Oxford
Higgins JP, Savović J, Page MJ, Elbers RG, Sterne JA (2019) Assessing risk of bias in a randomized trial. In: Cochrane handbook for systematic reviews of interventions, pp 205–228.
Farrah K, Young K, Tunis MC, Zhao L (2019) Risk of bias tools in systematic reviews of health interventions: an analysis of PROSPERO-registered protocols. Syst Rev 8(1):1–9
Elnaggar A, Ashraf M (2020) The aesthetic and functional roles of spreader flap in primary rhinoplasty. Am J Cosmet Surg 37(3):148–153
Shafaeei Y, Zare NJ (2019) A comparison of the aesthetics outcomes and respiratory side effects of the use of spreader flap and spreader graft techniques in open rhinoplasty. J Craniofac Surg 30(8):2546–2548
Atighechi S, Sarafraz Z, Baradaranfar M, Dadgarnia M, Zand V, Meybodian M et al (2018) The effect of spreader graft and mattress suture technique on rhinoplasty in patients with nasal hump smaller than 3 mm. J Craniofac Surg 29(8):2110–2113
Sowder JC, Thomas AJ, Gonzalez CD, Limaye NS, Ward PD (2020) Use of spreader flaps without dorsal hump reduction and the effect on nasal function. JAMA Facial Plast Surg 19(4):287–292. https://doi.org/10.1001/jamafacial.2016.2057
Stacey DH, Cook TA, Marcus BC (2009) Correction of internal nasal valve stenosis: a single surgeon comparison of butterfly versus traditional spreader grafts. Ann Plast Surg 63(3):280–284
ElBestar M, Abou-Zeid MA, Lasheen H, Farahat A, ElFouly M, Sabaa M et al (2020) Spreader flap versus spreader graft in dorsal reconstruction following hump resection in primary closed rhinoplasty. Egypt J Ear Nose Throat Allied Sci 21(3):192–201
Görgülü T, Özer CM, Kargi E (2015) The accordion suture technique: a modified rhinoplasty spreader flap. J Cranio Maxillofac Surg 43(6):796–802
Hassanpour SE, Heidari A, Moosavizadeh SM, Tarahomi MR, Goljanian A, Tavakoli S (2016) Comparison of aesthetic and functional outcomes of spreader graft and autospreader flap in rhinoplasty. World J Plast Surg 5(2):133
Hussein WK, Elwany S, Montaser M (2015) Modified autospreader flap for nasal valve support: utilizing the spring effect of the upper lateral cartilage. Eur Arch Otorhinol 272(2):497–504
Ingels KJ, Orhan KS, van Heerbeek N (2008) The effect of spreader grafts on nasal dorsal width in patients with nasal valve insufficiency. Arch Facial Plast Surg 10(5):354–356. https://doi.org/10.1001/archfaci.10.5.354
Jang YJ, Sinha V (2007) Spreader graft in septo-rhinoplasty. Indian J Otolaryngol Head Neck Surg 59(2):100–102
Kocak OF, Düzenli U (2018) Assessment of vertical triangular spreader graft technique for reconstruction of middle vault and internal nasal valve angle. J Craniofac Surg 29(8):2096–2100
Mamanov M, Batioglu-Karaaltin A, Inci E, Erdur ZB (2017) Effect of spreader graft on nasal functions in septorhinoplasty surgery. J Craniofac Surg 28(7):e618–e621
Standlee AG, Hohman MH (2017) Evaluating the effect of spreader grafting on nasal obstruction using the NOSE Scale. Ann Otol Rhinol Laryngol 126(3):219–223
Talmadge J, High R, Heckman WW (2018) Comparative outcomes in functional rhinoplasty with open vs endonasal spreader graft placement. Ann Plast Surg 80(5):468–471
Yoo DB, Jen A (2012) Endonasal placement of spreader grafts: experience in 41 consecutive patients. Arch Facial Plast Surg 14(5):318–322
André RF, Paun SH, Vuyk HD (2004) Endonasal spreader graft placement as treatment for internal nasal valve insufficiency. Arch Facial Plast Surg 6(1):36–40. https://doi.org/10.1001/archfaci.6.1.36
Erickson B, Hurowitz R, Jeffery C, Ansari K, El Hakim H, Wright ED et al (2016) Acoustic rhinometry and video endoscopic scoring to evaluate postoperative outcomes in endonasal spreader graft surgery with septoplasty and turbinoplasty for nasal valve collapse. J Otolaryngol Head Neck Surg 45(1):1–6
Gürlek A, Celik M, Fariz A, Ersöz-Öztürk A, Eren AT, Tenekeci G (2006) The use of high-density porous polyethylene as a custom-made nasal spreader graft. Aesthet Plast Surg 30(1):34–41
Palacín JM, Bravo FG, Zeky R, Schwarze H (2007) Controlling nasal length with extended spreader grafts: a reliable technique in primary rhinoplasty. Aesthet Plast Surg 31(6):645–650
Scattolin A, Orlando N, D’Ascanio L (2013) Spreader graft in closed rhinoplasty: the “rail spreader.” Facial Plast Surg 29(06):515–519
Saedi B, Amaly A, Gharavis V, Yekta BG, Most SP (2014) Spreader flaps do not change early functional outcomes in reduction rhinoplasty: a randomized control trial. Am J Rhinol Allergy 28(1):70–74
Gruber RP, Park E, Newman J, Berkowitz L, Oneal R (2007) The spreader flap in primary rhinoplasty. Plast Reconstr Surg 119(6):1903–1910
Manavbaşı Yİ, Başaran İ (2011) The role of upper lateral cartilage in dorsal reconstruction after hump excision: section 1. Spreader flap modification with asymmetric mattress suture and extension of the spreading effect by cartilage graft. Aesthet Plast Surg 35(4):487–493
Ozmen S, Ayhan S, Findikcioglu K, Kandal S, Atabay K (2008) Upper lateral cartilage fold-in flap: a combined spreader and/or splay graft effect without cartilage grafts. Ann Plast Surg 61(5):527–532
Paul MA, Kamali P, Chen AD, Ibrahim AM, Wu W, Becherer BE et al (2018) Assessment of functional rhinoplasty with spreader grafting using acoustic rhinomanometry and validated outcome measurements. Plast Reconstruct Surg Global Open 6(3):e1615
Taş BM, Erden B (2021) Comparison of nasal functional outcomes of let down rhinoplasty and open technical rhinoplasty using spreader graft. Eur Arch Otorhinolaryngol 278(2):371–377
Kim YH, Kim BJ, Jang TY (2011) Use of porous high-density polyethylene (Medpor) for spreader or extended septal graft in rhinoplasty: aesthetics, functional outcomes, and long-term complications. Ann Plast Surg 67(5):464–468
Omranifard M, Abdali H, Ardakani MR, Ahmadnia A (2013) Comparison of the effects of spreader graft and overlapping lateral crural technique on rhinoplasty by rhinomanometry. World J Plast Surg 2(2):99
Jalali MM (2015) Comparison of effects of spreader grafts and flaring sutures on nasal airway resistance in rhinoplasty. Eur Arch Otorhinolaryngol 272(9):2299–2303
Teymoortash A, Fasunla J, Sazgar A (2012) The value of spreader grafts in rhinoplasty: a critical review. Eur Arch Otorhinolaryngol 269(5):1411–1416
Avashia YJ, Marshall AP, Allori AC, Rohrich RJ, Marcus JR (2020) Decision-making in middle vault reconstruction following dorsal hump reduction in primary rhinoplasty. Plast Reconstr Surg 145(6):1389–1401
Boccieri A, Macro C, Pascali M (2005) The use of spreader grafts in primary rhinoplasty. Ann Plast Surg 55(2):127–131
Moubayed SP, Most SP (2016) The autospreader flap for midvault reconstruction following dorsal hump resection. Facial Plast Surg 32(01):036–041
Apaydin F (2016) Rebuilding the middle vault in rhinoplasty: a new classification of spreader flaps/grafts. Facial Plast Surg 32(06):638–645
Alrubaiee A, Alkamil K (2016) The effect of spreader flap in reconstruction of the middle vault of the nose after humpectomy. Bas J Surg 2016:60–65
Gerecci D, Perkins SW (2019) The use of spreader grafts or spreader flaps—or not—in hump reduction rhinoplasty. Facial Plast Surg 35(05):467–475
Rohrich RJ, Hollier LH (1996) Use of spreader grafts in the external approach to rhinoplasty. Clin Plast Surg 23(2):255–262
Flint PW, Haughey BH, Robbins KT, Thomas JR, Niparko JK, Lund VJ et al (2014) Cummings otolaryngology-head and neck surgery e-book. Elsevier Health Sciences
Samaha M, Rassouli A (2015) Spreader graft placement in endonasal rhinoplasty: technique and a review of 100 cases. Plastic Surg 23(4):252–254
Uebel CO, Matta R (2017) Alar cartilage—an alternative for spreader graft in primary rhinoplasty. Eur J Plast Surg 40(5):417–426
Mendelsohn M (2005) Straightening the crooked middle third of the nose. Arch Facial Plast Surg 7:74–80
Reiffel AJ, Cross KJ, Spinelli HM (2011) Nasal spreader grafts: a comparison of Medpor to autologous tissue reconstruction. Ann Plast Surg 66(1):24–28
de Pochat VD, Alonso N, Mendes RR, Cunha MS, Menezes JV (2012) Nasal patency after open rhinoplasty with spreader grafts. J Plast Reconstr Aesthet Surg 65(6):732–738
Demir UL (2019) A novel approach to crooked nose in rhinoplasty: asymmetric level osteotomy combined with unilateral spreader graft. J Craniofac Surg 30(5):1512–1515
Goffart Y, Karelle S, Daele J (2015) Free spreader grafts in rhinoplasty. Eur J Plast Surg 38(5):355–362
Acknowledgement
None.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fallahi, H., Keyhan, S.O., Dastgir, R. et al. Complications Associated with Spreader Grafts and Spreader Flaps: A Systematic Review. Aesth Plast Surg 46, 1831–1847 (2022). https://doi.org/10.1007/s00266-022-02790-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-022-02790-1