Abstract
Background
This article presents a new method using a dermis–outer orbicularis fascia–orbicularis–levator (DOOL) fixation technique for double-eyelid blepharoplasty.
Methods
Our surgical technique preserves the preorbicular venous network (POVN) and uses mattress sutures to fix the dermis, outer fascia of the orbicularis oculi muscle, and orbicularis oculi muscle with pretarsal levator aponeurosis (DOOL). Between January 2016 and July 2018, 335 patients were treated with this POVN-preserving DOOL technique (321 women and 14 men; mean age, 29.6 y). The patients were followed up for 6–30 months. The complications were documented, and the overall outcomes of the upper eyelid folds were evaluated by both surgeons and patients as good, fair, or poor.
Results
Among 335 patients, 307 (91.6%) had good results, 17 (5.1%) had fair results, and 11 (3.3%) had poor results. Postoperative complications included partial (n=4) or complete (n=3) loss of the double-eyelid line and asymmetric folds (n=4). Hypertrophic/depressed scars did not occur.
Conclusions
With less invasiveness and secure internal fixation, the DOOL fixation technique with POVN preservation can achieve a stable and natural double-eyelid appearance.
Level of evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Double-eyelid blepharoplasty is the most commonly performed aesthetic procedure in East Asia and can be divided into nonincisional (suture) and incisional techniques. The incisional method has been considered the approach with the widest indications and the most reliable results [1].
In traditional incision-based blepharoplasty, pretarsal tissue is over-resected, and sutures are used to firmly fixate the pretarsal skin to the aponeurosis or tarsus, resulting in a deep, immovable, depressed fold (static fold) [2]. In recent years, great emphasis has been placed on creating a stable, physiologic, and natural-looking double-eyelid crease (dynamic fold). However, those techniques require resection of a strip of the orbicularis oculi muscle, [2,3,4,5] elevation of the lower flap of the fold line, [3, 4] or excision of the pretarsal septal extension, [5] which prolong the recovery time due to pretarsal edema.
A recent study has shown the presence of the outer fascia of the orbicularis oculi muscle (OFOOM) under the subcutaneous layer, [6] which was also referred to as a fibroadipose layer [7]. The preorbicular venous network (POVN) is the outer venous drainage network of the upper eyelid overlaying the OFOOM [6]. There have been no clinical studies on preserving the POVN during upper blepharoplasty, which might be beneficial for the recovery of the upper eyelid.
We devised a novel technique that preserves the POVN and uses mattress sutures to fix the dermis, OFOOM, and orbicularis oculi muscle with pretarsal levator aponeurosis (DOOL). Our new technique may achieve a stable and natural double-eyelid appearance.
Patients and Methods
Between January 2016 and July 2018, 335 patients without blepharoptosis were treated with the POVN-preserving DOOL technique (321 women and 14 men; mean age, 29.6 y). A total of 212 female and 5 male patients simultaneously underwent medial epicanthoplasty. The patients were followed up for 6–30 months. This study was approved by the institutional ethical committee and adhered to the tenets of the Declaration of Helsinki. Written informed consent was obtained from all patients.
Preoperative Design and Preparation
The incision line and the extent of skin excision were determined with the patient in the supine position. The width of skin excision was no less than 3 mm for patients received this operation; otherwise, the patients could receive suture method. Local anesthesia was administered by injecting 0.8–1 mL of 1% lidocaine with 1:100,000 epinephrine using a 30-gauge needle for each upper eyelid. Local anesthetic should be injected superficially to avoid injuring the POVN. To avoid excess edema of the lower flap, the local anesthetic should be injected gently and slowly above the lower incision.
Surgical Technique
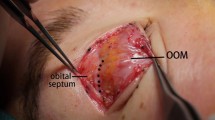
Surgery was performed under a 2.5× surgical loupe. An incision was made with a No. 11 blade, and a strip of skin was removed according to the incision line. The following dissection was mainly performed with monopolar electrical cautery. Segments of the orbicularis oculi muscle were resected, meticulously preserving the POVN (Fig. 1a-b). Three to four longitudinal veins between the upper and lower incisions were preserved. A small incision was made in the lateral side of the orbital septum, and the excessive preaponeurotic fat was removed conservatively.
Exposure and preservation of the POVN. a After skin resection, the preorbicular venous network (POVN) was exposed within the outer fascia of the orbicularis oculi muscle (OFOOM). b Segments of the orbicularis oculi muscle were resected, and the major longitudinally running preorbicular veins were preserved (black arrowhead). c Four small pretarsal holes (black arrowhead) were created in the upper margin of the lower flap, allowing the removal of loose connective tissue and enabling exposure of the surface of the pretarsal levator aponeurosis.
Three to five small pretarsal holes were created in the upper margin of the lower flap to allow the resection of adipose and loose connective tissue and enable exposure of the surface of the pretarsal levator aponeurosis (Fig. 1c). The first suture was placed at the midpupillary point, and 7-0 nylon suture was started with horizontal stitching through the pretarsal levator aponeurosis. The suture was passed through the orbicularis oculi muscle, OFOOM, and dermis twice (Fig. 2-3). Five to six knots were then tied to finish the suture fixation. Three to five sutures were required to create a stable supratarsal fold, with one suture in each small pretarsal hole.
Illustration demonstrating the dermis–outer orbicularis fascia–orbicularis–levator fixation technique with preorbicular venous network preservation for double-eyelid blepharoplasty. a 7-0 nylon suture was placed in the small pretarsal hole. b The suture was passed through the pretarsal levator aponeurosis, orbicularis oculi muscle, OFOOM, and dermis.
The skin incisions were then closed using interrupted sutures with 7-0 nylon. The stitches were made in a simple skin–skin fashion. The skin was not sutured with the pretarsal levator aponeurosis to avoid depressed scar formation. Suture removal was performed on the fifth postoperative day.
Assessment of Outcomes
All of the patients were asked to score the outcome at the last postoperative office visit 6 months to 3 years after the operation. Based on a chart review, patient satisfaction and final aesthetic results were graded by the authors and patients, as poor, fair, or good [3]. If patients could not have a clinical visit, the results were obtained through telephone calls. Postoperative complications were also recorded, such as partial or complete loss of the double-eyelid line, hypertrophic scar formation, and asymmetric folds.
Results
Of the 335 patients, 307 (91.6%) had good results, 17 (5.1%) had fair results, and 11 (3.3%) had poor results. Postoperative complications included partial (n=4) or complete (n=3) loss of the double-eyelid line and asymmetric folds (n=4). The results revealed that the double-eyelid shape was natural looking, and no patients experienced upper eyelid retraction or incomplete eye closure. Hypertrophic/depressed scars did not form. Revision procedures were performed for the patients with complications, and all the patients were satisfied with the results. Eyelid edema resolves quickly within 4 weeks. Typical cases are presented in Figs. 4 and 5. The supplementary figure showed the recovery process of a typical patient.
Discussion
The fundamental goal of double-eyelid blepharoplasty is to fix the anterior lamella of the upper eyelid to the posterior lamella. The anterior lamella is composed of skin, the orbicularis oculi muscle, and the OFOOM between them. The OFOOM exists alongside the outer venous drainage network of the upper eyelid, which is named the “preorbicular venous network (POVN)” [6]. According to the previous clinical and cadaver anatomical study, the POVN constitutes the main outer venous pathway of the upper eyelid [6]. For incisional double-eyelid blepharoplasty, a strip of redundant skin and orbicularis oculi muscle is usually resected, and the longitudinal preorbicular veins are transected during this step. There have been no publications investigating POVN preservation during incisional double-eyelid blepharoplasty.
During our procedure, local anesthetic should be injected superficially to avoid injuring the POVN. After resecting a strip of redundant skin, the orbicularis oculi was not removed as a single strip but as several small segments, preserving the POVN. In most of the patients, 3 to 4 prominent longitudinal veins were preserved. Although this preservation prolongs the operation by a few minutes, it is beneficial for preserving the venous pathway of the upper eyelid, reducing bleeding, and minimizing postoperative swelling.
In the past, the most common double-eyelid blepharoplasty involved excision of the pretarsal orbicularis oculi muscle and dermal tarsus fixation, which resulted in durable but static folds [8,9,10]. Currently, dynamic folds with preservation of the orbicularis oculi and many different structures of the posterior lamella by internal fixation methods have been advocated, including methods using the levator aponeurosis, [11] mini-flaps derived from pretarsal levator tissue, [3] septoaponeurosis junctional thickening, [2] pretarsal levator aponeurosis, [4] pretarsal septal extension,[5] white line, [12] tarsus, [13] and levator and tarsus [14]. However, those techniques require resection of a strip of the orbicularis oculi muscle, elevation of the lower flap of the fold line, or excision of the pretarsal septal extension, leading to a longer recovery time due to pretarsal edema.
To minimize the surgical trauma, our procedure does not involve elevation of a lower flap, elevation of a pretarsal levator flap, or excision of the pretarsal septal extension. For the patients with excess preaponeurotic fat, instead of opening the orbital septum completely, a small incision was made in the lateral side of the orbital septum, and part of the fat pad was removed conservatively. These technical steps, together with preservation of the POVN, minimize trauma to the upper eyelid. As a result, our patients had a quicker recovery and less swelling postoperatively. Previous study described that eyelid edema lasted for 6–8 weeks [13]. In our patients, eyelid edema resolved quickly within 4 weeks. However, as a retrospective study, there was no rigorous evaluation system with objective parameters for postoperative swelling, which is one of the limitations for this study. A prospective study with objective parameters should be conducted for postoperative swelling evaluation in future.
A recent published article described a new surgical technique with selective neurovascular preservation [15]. However, they preserved the terminal nerves and vessels below the OOM, which is different with our technique. POVN exists between the dermis and the OFOOM, which is above the OOM. Further prospective study might be conducted comparing these two surgical techniques.
Compared with the traditional dermis–tarsus procedure, orbicularis-preserving techniques are prone to the development of fold loss. Possible reasons for this problem are discussed here. First, many procedures choose the dermis [2] or orbicularis oculi [3,4,5, 11, 16] as the only anterior lamellar component for fixation, which is not sufficiently secure. Second, there are loose connective tissue and adipose tissue between the anterior and posterior lamellae, which may interfere with double-eyelid formation.
To obtain secure internal fixation, several technical points are applied. First, every suture passed through the orbicularis oculi muscle, OFOOM, and dermis twice. This maneuver involves not only more anterior lamellar structures but also more tissues for better adhesion. Second, there is often some adipose tissue and loose connective tissue between the orbicularis oculi muscle and pretarsal levator aponeurosis, which hinders adhesion between the anterior and posterior lamellae. If not treated, after the needle is passed through the pretarsal tissue, the needle might be elevated away from the tarsus because of the loose connective tissue. In our procedure, three to five small pretarsal holes were created in the upper margin of the lower flap to allow removal of the adipose tissue and loose connective tissue on the top of the pretarsal levator aponeurosis. Afterward, the needle was passed through the pretarsal levator aponeurosis within the small hole (approximately 2 mm×2 mm in size). The indicator of secure fixation of the posterior lamella is that the needle cannot be elevated away from the tarsus. Finally, the suture knots should not be too tight to avoid tissue strangulation and cutting effect.
In addition to securing internal fixation, appropriate fixation height is also very important. In previous studies, the anterior lamellar component was sutured with a higher posterior lamellar component, [2,3,4,5, 11, 16] which may lead to a high or deep fold [17, 18]. In our procedure, the anterior lamellar components (including the dermis, OFOOM, and orbicularis oculi muscle) of the lower flap were sutured with the pretarsal levator aponeurosis no more than 1 mm higher than the upper margin of the lower flap. Furthermore, local anesthetic solution was injected above the lower incision to avoid excess swelling of the lower flap. Therefore, excessive stretching of the lower flap and the formation of high/deep folds did not occur postoperatively.
For double-eyelid blepharoplasty, external fixation sutures may be placed through the skin and dermis of the superior and inferior incisions, catching a “bite” of the levator/tarsus in between [19]. However, external fixation might create too much adhesion, leading to depressed scar formation. In our procedure, the stitches were made in a simple skin–skin fashion. In our procedure, OFOOM was sutured with the pretarsal levator aponeurosis, and the skin was not sutured to the pretarsal levator aponeurosis to avoid depressed scar formation.
In our series, there were seven cases of fold loss, most of which occurred during the early phase of the application of our technique. The reason for fold loss was that we did not remove enough loose soft tissue from the small pretarsal holes. During internal fixation, there is loose connective tissue between the anterior and posterior lamellar structures, making adhesion insecure. After we modified our technique and sufficiently removed loose connective tissue in the pretarsal holes before internal fixation, the incidence of fold loss was much lower.
Conclusions
We have devised a technique that preserves the POVN and uses mattress sutures to fix the dermis, OFOOM, and orbicularis oculi muscle with pretarsal levator aponeurosis (DOOL). With less invasiveness and secure internal fixation, our technique can achieve a stable and natural double-eyelid appearance.
REFERENCES
Park KS, Park DD (2017) Objective outcome measurement after upper blepharoplasty: an analysis of different operative techniques. Aesthetic Plast Surg 41(1):64–72. https://doi.org/10.1007/s00266-016-0747-1
Kim HS, Hwang K, Kim CK, Kim KK (2013) Double-eyelid surgery using septoaponeurosis junctional thickening results in dynamic fold in asians. Plast Reconstr Surg Glob Open 1(2):1–9. https://doi.org/10.1097/GOX.0b013e318293dc69
Choi Y, Eo S (2010) A new crease fixation technique for double eyelidplasty using mini-flaps derived from pretarsal levator tissues. Plast Reconstr Surg 126(3):1048–1057. https://doi.org/10.1097/PRS.0b013e3181e3b72a
Lu L, Zhu M, Luo X, Yang Q, Wang X, Yang J, Liu F (2017) Using levator aponeurosis to create physiologically natural double eyelid: a new reconstruction technique based on three key factors in double eyelid formation. Ann Plast Surg 78(5):487–491. https://doi.org/10.1097/SAP.0000000000000951
Pan L, Sun Y, Yan S, Shi H, Jin T, Li J, Zhang L, Wu S (2019) A flexible suspension technique of blepharoplasty: clinical application and comparison with traditional technique. Aesthetic Plast Surg 43(2):404–411. https://doi.org/10.1007/s00266-019-01317-5
Choi Y, Eo S (2016) Outer fascia of orbicularis oculi muscle as an anchoring target tissue in double eyelid surgery. J Craniofac Surg 27(2):322–327. https://doi.org/10.1097/SCS.0000000000002372
Kakizaki H, Takahashi Y, Nakano T, Ikeda H, Selva D, Leibovitch I (2011) The distribution of elastic fibers in the Asian upper eyelid skin. Ophthalmic Plast Reconstr Surg 27(3):201–203. https://doi.org/10.1097/IOP.0b013e3181f9df3a
Sayoc BT (1954) Plastic construction of the superior palpebral fold. Am J Ophthalmol 38(4):556–559. https://doi.org/10.1016/0002-9394(54)90707-2
Boo-Chai K (1963) Plastic construction of the superior palpebral fold. Plast Reconstr Surg 31:74–78. https://doi.org/10.1097/00006534-196301000-00010
Fernandez LR (1960) Double eyelid operation in the Oriental in Hawaii. Plast Reconstr Surg Transplant Bull 25:257–264. https://doi.org/10.1097/00006534-196003000-00007
Park JI (1999) Orbicularis-levator fixation in double-eyelid operation. Arch Facial Plast Surg 1(2):90–95. https://doi.org/10.1001/archfaci.1.2.90
Zhou X, Wang H (2019) Orbicularis-white line fixation in asian blepharoplasty: kiss technique. Aesthetic Plast Surg 43(6):1553–1560. https://doi.org/10.1007/s00266-019-01454-x
Sun W, Wang Y, Song T, Wu D, Li H, Yin N (2018) Orbicularis-tarsus fixation approach in double-eyelid blepharoplasty: a modification of park’s technique. Aesthetic Plast Surg 42(6):1582–1590. https://doi.org/10.1007/s00266-018-1218-7
Wu LW, Ye Z, Xu Y, Yu J, Wu Y (2015) Orbicularis-levator-tarsus composite suture technique in double-eyelid operation. J Plast Reconstr Aesthet Surg 68(8):1079–1084. https://doi.org/10.1016/j.bjps.2015.04.009
Shen X (2021) Full-incision double-eyelid blepharoplasty with selective neurovascular preservation method. Aesthetic Plast Surg. https://doi.org/10.1007/s00266-021-02418-w
Li G, Ding W, Tan J, Zhang B, Chen X, He B (2018) A new method for double-eyelid blepharoplasty using orbital septum. Ann Plast Surg 81(6):633–636. https://doi.org/10.1097/SAP.0000000000001650
Kim KK, Kim WS, Oh SK, Kim HS (2017) High double eyelid fold correction using wide dual-plane dissection. Ann Plast Surg 78(4):365–370. https://doi.org/10.1097/SAP.0000000000000905
Young SM, Kim YD, Kim JH, Lang SS, Woo KI (2019) Lowering of the high eyelid crease in revision upper eyelid surgery. Aesthetic Plast Surg 43(1):139–146. https://doi.org/10.1007/s00266-018-1235-6
Kim DW, Bhatki AM (2005) Upper blepharoplasty in the Asian eyelid. Facial Plast Surg Clin North Am. https://doi.org/10.1016/j.fsc.2005.06.009
Funding
This manuscript is funded by the Key Project of the Strategic International Science and Technology Innovation Cooperation, Ministry of Science and Technology, grant No.: 2019YFE020215.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no financial or conflicts of interest to disclose.
Ethical approval
Our experiments were in accordance with the ethical standards formulated in the Declaration of Helsinki. This study was approved by the Research Ethics Board of our Hospital.
Consent to participate
Consent was obtained from the participants responding to the follow-up surveys.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

266_2021_2627_MOESM1_ESM.jpg
Supplementary Figure A patient before the operation and 6 months postoperatively, with no visible scar when the eyes are closed. A series of pictures indicated the patient opening eyes and closing eyes before operation (a1, b1), 1 day (a2, b2), 5 days (a3, b3), 2 weeks (a4, b4), 1 month (a5, b5), 2 months (a6, b6), and 6 months (a7, b7) postoperatively. Swelling resolved quickly after operation, which was minimal 2 months postoperatively. (JPG 2631 kb)
Rights and permissions
About this article
Cite this article
Huang, J., Feng, Y., Li, Z. et al. Double-Eyelid Blepharoplasty: Dermis–Outer Orbicularis Fascia–Orbicularis–Levator Fixation Technique with Preorbicular Venous Network Preservation. Aesth Plast Surg 46, 231–236 (2022). https://doi.org/10.1007/s00266-021-02627-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-021-02627-3