Abstract
Pectus excavatum is a common type of congenital chest wall abnormality. The defect ranges in severity from mild to severe, and can lead to cardiopulmonary impairment caused by the caved-in chest. The case of a 27-year-old woman with mild pectus excavatum and a diagnosis of scleroderma is reported. Cosmetic correction of pectus excavatum malformation with the use of autologous fat transplantation has never been reported. The individual achievement of relief from the psychological consequences of such disfigurement and the improvement in quality of life are high. Autologous fat transfer could be a new option in the armamentarium of techniques for correction of mild pectus deformities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Pectus deformities affect about 1% of the population [1]. The hallmark of pectus excavatum is the caved-in appearance of the anterior chest. The severity of the defect and the asymmetry of the chest are quite variable. Patients may present with a very mild form of pectus excavatum or a very severe form with impairment of cardiopulmonary function because of the constricted pleural space or compromised venous return resulting from displacement of the cardiac base [2].
The use of autologous fat transplantation for the management of pectus deformity has not been previously described. We present a case of mild pectus excavatum and its correction by fat grafting.
Case Report
A 27-year-old woman presented with a mild funnel chest deformity (Fig. 1). Scleroderma had been diagnosed 10 years previously. She had been unresponsive to topical and systemic treatment with corticosteroids.
At physical examination, a mild pectus excavatum deformity and various sclerotic, atrophic, pigmented plaques all over her body were noted. Plain anteroposterior and lateral chest radiographic views were obtained. Echocardiography and a complete blood count were performed. There was no evidence of cardiopulmonary dysfunction. The choice was made to perform autologous fat transfer. The areas to be aspirated and grafted were previously marked. Appropriate perioperative sedation was administered. A solution containing 2% of xylocaine with adrenaline was infiltrated into the subcutaneous tissue of the abdominal area.
After a period of 15 min, syringe-assisted liposuction was performed with a small-bore cannula. The preparation of fat to be injected was accomplished in a manner that produced a clear, pale substance consisting mainly of viable fat cells, which is considered most adequate for grafting [3]. Fat transplantation was performed using the small-bore cannula through a stab incision placed in the anterior thorax after induction of appropriate local anesthesia (Fig. 2).
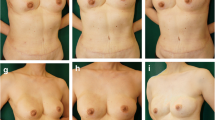
Using the same incision, different trajectories were created, and the fat was injected, starting from the deeper aspect and progressing to the surface. At the first intervention, 35 ml of fat was injected (Fig. 3). The patient was evaluated 6 months later, and a second procedure was performed because partial absorption of the injected fat had occurred (Fig. 4). Using the same incision, 18 ml of prepared fat was inserted. Figure 5 shows the final result 2 years after of the initial procedure.
The patient was able to resume her normal activities within 3 days after each intervention. She was satisfied with the final result obtained, reporting a considerable gain in her quality of life and a significant improvement in her social activities.
Discussion
Breast and chest wall disfiguration attributable to a funnel chest is an aesthetically and sometimes functionally debilitating deformity requiring correction. For severe deformities caused by pectus excavatum malformations, the standard operative procedures generally are based on either sternal elevation or turnover [4]. Although, the minimally invasive procedures, such as endoscopic correction and Erlangen repair, seem to show both optimized cosmetic results and maximized functionality, the possible secondary sequelae of these surgical approaches cannot be overlooked [5].
In an important group of pectus excavatum cases, the funnel chest is limited to the sternal plate and represents an isolated aesthetic defect. Such a defect can be corrected by insertion of a customized one-piece silicon implant, resulting in an aesthetic correction with a low complication rate [6]. Whereas the use of prefabricated silicone implants yields good cosmetic results, the safety of their use in morphea patients is highly controversial.
Morphea or scleroderma is a disorder characterized by thickening and induration of the skin and subcutaneous tissue due to excessive collagen deposition [7]. The etiology of localized scleroderma may involve genetic factors causing abnormalities in the immune system, vascular tissue, and extracellular matrix [8]. The reported trigger factors include implantation of silicon prosthesis and trauma as well as bacterial, viral, and toxic factors [9–11].
The choice of autologous fat grafting seemed to be a more appropriate and less invasive procedure for the reported specific patient. She was asymptomatic from a functional standpoint, but highly concerned about her aesthetic image. It is known that partial fat graft resorption is encountered in autologous adipose tissue transfer [12]. Overcorrection of the defect was performed because it partially compensated for fat absorption. Although the patient had to undergo a secondary intervention, she highly appreciated the cosmetic final result and the relief from the psychological consequences of such disfigurement.
No complications were observed. Although there was no further evidence of graft resorption during a 2-year follow-up period, the long-term results of fat grafting in the sternal area are yet to be determined.
Conclusion
Patient satisfaction and improved quality of life show that the described method of autologous fat transfer could be a new option in the armamentarium of techniques for correction of mild pectus deformities.
References
Williams AM, Crabbe DC (2003) Pectus deformities of the anterior chest wall. Paediatr Respir Rev 4:237–242
Fox JP, Schnell JL, Adams TA Jr, Hilton WM, Seyfer AE (2007) Pectus excavatum: Comparison of nonprosthetic repairs using multiple techniques. Plast Reconstr Surg 119:33e–39e
Pereira LH, Radwanski HN (1996) Fat grafting of the buttocks and lower limbs. Aesth Plast Surg 20:409–416
Onishi K, Maruyama Y (2001) Correction of pectus excavatum using a sternal elevator: Preliminary report. Br J Plast Surg 54:117–124
Horch RE, Stoelben E, Carbon R, Sultan AA, Bach AD, Kneser U (2006) Pectus excavatum breast and chest deformity: Indications for aesthetic plastic surgery versus thoracic surgery in a multicenter experience. Aesth Plast Surg 30:403–411
Margulis A, Sela M, Neuman R, Buller-Sharon A (2006) Reconstruction of pectus excavatum with silicone implants. J Plast Reconstr Aesthet Surg 59:1082–1086. Epub 2006 May 11
Dancey AL, Waters RA (2006) Morphea of the breast: Two case reports and discussion of the literature. J Plast Reconstr Aesthet Surg 59:1114–1117
Chen K, See A, Shumack S (2003) Epidemiology and pathogenesis of scleroderma. Australas J Dermatol 44:1–7
Granel B, Serratrice J, Gaudy C, Weiller-Merli C, Bonerandi JJ, Lepidi H, Coulomb-Marchetti B, Disdier P, Weiller PJ (2001) Localized morphea after silicone-gel-filled breast implant. Dermatology 202:143–144
Torrelo A, Suarez J, Colmenero I, Azorin D, Perera A, Zambrano A (2006) Deep morphea after vaccination in two young children. Pediatr Dermatol 23:484–487
Komocsi A, Tovari E, Kovacs J, Czirjak L (2000) Physical injury as a provoking factor in three patients with scleroderma. Clin Exp Rheumatol 18:622–624
Ghobadi F, Zangeneh M, Massoud BJ (1995) Free fat autotransplantation for the cosmetic treatment of first web space atrophy. Ann Plast Surg 35:197–200
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pereira, L.H., Sterodimas, A. Free Fat Transplantation for the Aesthetic Correction of Mild Pectus Excavatum. Aesth Plast Surg 32, 393–396 (2008). https://doi.org/10.1007/s00266-007-9110-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-007-9110-x