Abstract
Background
A number of plastic surgeons have advocated using hypotonic solution in ultrasound lipoplasty, theorizing that induced adipocyte swelling increases membrane susceptibility to ultrasonic disruption. Additionally, it has been theorized that potassium increases membrane permeability. This study aimed to determine the effect of solution osmolality on adipocyte diameter, the time course of hypotonic solution action, and the effect of potassium addition on adipocyte diameter.
Methods
Base solutions with three different osmolalities were prepared: normal saline (NS) (154 mOsm/l), 1/2NS (77 mOsm/l), and 1/4NS (38.5 mOsm/l). Each solution was modified to contain 0, 5, and 10 mEq/l of potassium and adjusted to starting osmolality. Adipocytes of six patients were suspended in the nine solutions, and diameters were determined at 0, 15, 30, and 45 min. Diameters were measured using imaging software (Kodak ID 3.6).
Results
At time 0, the average adipocyte diameter was 79 ± 8 μm, and no difference was seen in any of the solutions. Cells in the NS group showed no significant increase in diameter over 45 min. The 1/2NS group achieved an 8% ± 1.9% increase in diameter at 45 min (p < 0.05). The 1/4NS group showed an increase by 14% ± 2.4% (p < 0.01) at 15 min, and 15% ± 2.3% (p < 0.01) at 45 min. Potassium had no independent effect on cell diameter.
Conclusions
Hypotonic solution can significantly increase human adipocyte diameter. The findings showed that 1/2NS had a significant effect within 15 min. Tumescent solutions with an osmolality of 1/4NS may be useful in facilitating ultrasonic lipoplasty.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Since its inception in 1976, liposuction has undergone a series of modifications including injection of tumescent fluid and application of ultrasound energy [13,17–22,24,25,34]. As the demand for minimally invasive plastic surgery escalates, there is a growing emphasis on attaining superior aesthetic outcome in a time- and labor-efficient manner. Altering tumescent fluid to maximize the efficiency of ultrasound may represent a further advancement in lipoplasty.
Injection of tumescent fluid before suction is a widely accepted practice. The standard tumescent fluid contains dilute epinephrine, which provides hemostasis through vasoconstriction, and lidocaine, which provides some degree of postoperative anesthesia [25,30]. Surgeons report that tumescent fluid eases the mechanical strain felt during a nontumescent liposuction [28]. The additional ease felt during tumescent liposuction is likely attributable to the additional space created by the fluid. The physiologic impact of tumescent injection on adipocytes is at best an educated guess.
The advocates of hypotonic tumescent solution have touted the view that the resulting osmosis isolates, swells, and sensitizes the adipocyte to ultrasound energy [15,16,26,27]. Hoefflin [15,16] asserted that the combination of his hypotonic solution and external ultrasound application results in chemophysical dissolution of moderately sized pockets of adipose tissue. He hypothesized that ultrasonography acts to further emulsify and “vectorize” fat already partially emulsified by the hypotonic solution, and that the ruptured membranes, triglycerides, and intracellular contents are reabsorbed by the body. However, these effects have not been demonstrated scientifically. Hoefflin bases these theories on anecdotal clinical experience. Palmieri et al. [26] suggested that hypotonic solutions improve ultrasound efficiency in an ex vivo model, but this lacked convincing evidence.
The theoretical advantage of hypotonic solution is that induced adipocyte swelling increases stress on the cell membrane, making it more susceptible to disruption by ultrasound energy [15,16]. However, the optimal tonicity of injectable fluids for increasing adipocyte cell size is currently unknown. Additionally, it is theorized that the presence of potassium in a tumescent solution increases cell membrane permeability by increasing the osmotic gradient [15]. No study to date has examined the impact of hypotonic solution on adipocyte size, or the time course of the effect. No existing studies have examined the effect of potassium in a tumescent solution on adipocyte size.
One prior study attempted to demonstrate the physiologic impact of hypotonic solution. Adamo et al. [1] studied the effect of ultrasound-assisted versus traditional lipectomy on adipocytes after injection with hypotonic solution. The lipoaspirates were processed and assessed microscopically. The lipoaspirate from the ultrasound-assisted lipectomy consisted of “empty cells,” with concomitant destruction of intercellular junctions and extravasation of intracellular lipid. However, the lipoaspirate from traditional suction-assisted lipectomy, which underwent the same preoperative injection with hypotonic solution, displayed largely intact adipocytes. The study of Adamo et al. [1] did not include a normotonic control group. Although it was evident that more lipodissolution occurred with ultrasonic energy, there was no evidence to show that the hypotonic solution injection had induced a physiologic transformation in the adipocytes.
We aimed to prove that hypotonic tumescent fluid has a well-timed physiologic impact on adipocytes. The current practice in liposuction is to inject the tumescent fluid 10 to 20 min before suction for maximal exploitation of its anesthetic and vasoconstrictor properties [29]. Ideally, a useful physiologic effect on adipocytes would occur within this time frame.
The specific aims of our study were to determine the effect of the tumescent solution osmolality on the diameter of adipocytes isolated from fresh human abdominal subcutaneous tissue, the time course of change in adipocyte size during exposure to hypotonic solution, and the differential effect of potassium added to the solutions.
Methods
Human Subjects
Discarded abdominal subcutaneous tissue samples were obtained from body contouring surgeries performed by one surgeon (J.P.R.). Tissue was collected from five women and one man with a mean age of 46 years (range, 30–55 years). Before processing, 10 g of adipose tissue were placed in a sterile container and stored at room temperature for less than 24 h. Tissue collection was performed according to a protocol approved by the University of Pittsburgh Institutional Review Board.
Preparation of Solutions
Base solutions with three different osmolalities were prepared for the study: normal saline (NS) (154 mOsm/l), 1/2NS (77 mOsm/l), and 1/4NS (38.5 mOsm/l). Each base solution was further modified to contain 0, 5, and 10 mEq/l of potassium by the addition of dry potassium chloride. Free water was added to adjust the solutions to starting osmolality. This resulted in a total of nine different solutions (Table 1). The solutions were filter purified and stored in heat-sterilized bottles at room temperature.
Adipocyte Isolation and Suspension
Adipocytes from abdominal subcutaneous tissue of the six patients were isolated by collagenase digestion. From each sample, 5 g were excised and placed in a 15-mg collagenase/3.5% bovine serum albumin mixture, then minced with sterile scissors. The minced samples underwent collagenase digestion for 20 to 30 min in a 37°C shaker water bath set at 115 rotations per minute, then were centrifuged at 1,000 rpm for 10 min. The fatty supernatant underwent a second centrifugation. Aliquots of 100 μl were extracted from the middle adipocyte layer and stabilized in isotonic solution before experimentation. Adipocytes from each of the six patients were suspended in each of the nine solutions in a Petri dish, and immobilized under a light microscope.
Adipocyte Sizing
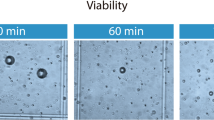
Adipocyte sizing was performed using previously described methods [2,5,32]. Cell sizing was performed using a light microscope at a ×200 setting. Digital photographs of fields containing 50 to 100 adipocytes were taken at a standardized focal length (Fig. 1). The diameters of the individual cells in the digitized images were measured using imaging software (Kodak ID 3.6). From each sample, 50 adipocyte diameters were measured. Adipocyte diameters were determined 0, 15, 30, and 45 min after immersion in their respective fluids.
Statistical Analysis
Statistics were performed using one-way analysis of variance (ANOVA) and post hoc tests (GraphPad Quickcalcs). Results were confirmed with additional post hoc paired t tests (Microsoft Excel for Windows 2000).
Results
The average adipocyte diameter was 79 ± 8 μm at time 0 (immediately after resuspension in solution). No significant difference in cell diameter was seen at time 0 in any of the solutions tested. Cells suspended in NS showed no significant increase in cell diameter over a period of 45 min.
Cells suspended in 1/2NS achieved an 8% increase in diameter at 45 min (p < 0.05). Adipocytes in 1/2NS displayed an upward trend in mean diameter at 15 and 30 min. However, the difference was not statistically significant (Fig. 2).
Adipocyte diameter in solution over 45 min. The x-axis represents the amount of time adipocytes are suspended in solution. The y-axis denotes adipocyte diameter. There was no significant increase in adipocyte diameter for cells suspended in normal saline (NS). Adipocytes suspended in both 1/2NS and 1/4NS had an increased mean diameter within 45 min (n = 6; p < 0.05).
The 1/4NS solution had the most profound and early impact on cell diameter. Mean adipocyte diameter had increased by 14% ± 2.4% (p < 0.01) at 15 minutes and 15% ± 2.3% at 45 min (p < 0.01). The increase in adipocyte diameter was statistically significant at all three time points (Table 2).
Potassium, as an independent variable, had no effect on cell diameter. The addition of potassium neither significantly decreased nor increased the impact of the various solutions on mean adipocyte diameter. This held true for all time points.
Discussion
Ultrasound requires a conversion and amplification of electrical energy into ultrasound energy [35]. The most common view of the ultrasound mechanism is that it destroys adipocytes by cavitation, a process of formation and implosion of microcavities containing gas vapors within the adipocytes [4,8,9,14,33]. Cavitation theoretically leads to selective destruction of adipocytes and relative sparing of neurovasculature [14]. In addition to cavitation, other forces such as shearing stress and direct “jackhammer” mechanical stress may contribute to adipocyte rupture [1,4].
The physiologic basis for our study was the theory of the thin shell [6,7,9]. When a spherical object encased in a shell undergoes expansion, the expanded shell will be measurably thinner than in its original state. Theoretically, a thinner shell should also be more fragile and susceptible to disruption. In addition, a thinner shell presents a shorter distance between external energy and intracellular content. When external ultrasound energy is applied, the affect is thus twofold. The membrane not only is more susceptible to disintegration, but the intracellular contents also can undergo cavitation.
Another study demonstrated with biocompatible dye particles that inertial cavitation by ultrasound depends on the property of the shell [6]. When multiple ultrasound cycles were needed to cause fragmentation, thinner shells needed fewer acoustic cycles to reach the fragmentation threshold than thicker shells.
If hypotonicity increases adipocyte diameter, it should theoretically also make the membrane stretch to a thinner state. The resulting thinned membrane or “shell” should enhance ultrasound-induced cell lysis. One study immersed a leukemic cell line in hypotonic solution [10]. Enhancement of ultrasound-induced cell lysis was observed at all intensities. The authors concluded that hypotonia was responsible for the increased cell membrane susceptibility to mechanical damage. Cellular ion scanning images also suggested that hypotonia had a damaging effect on the membrane damage and repair mechanism of the cells [10]. It is reasonable to guess that hypotonic solution could, in addition to increasing cell diameter, generate physiologic damage to adipocyte membrane function.
In our study, adipocytes immersed in hypotonic solution underwent a significant increase in size. Although the change in adipocyte diameter was statistically significant, the data do not prove that the change is biologically profound. We do not know the amount of cell volume expansion that would be conducive to ultrasound receptivity and sensitivity. We know that a 15% increase in cell diameter results in more than a 50% increase in intracellular volume and a 15% increase in surface tension. Although these numbers certainly sound impressive, we do not know whether they are of physiologic consequence. A useful analogy would be that of a water balloon. If a deflated balloon is half filled with water, the concomitant increases in surface tension and volume still are not sufficient to cause the water balloon to rupture with a low-energy impact. It is possible that even a 50% increase in volume is not sufficiently profound to increase susceptibility to ultrasound energy significantly. Additional studies are needed to correlate the increase in adipocyte diameter to likeliness of dissolution with ultrasound application.
Potassium is added because its presence is thought to make the cell membrane more osmotically active. In theory, active and passive transmembrane transport of potassium could result in additional unidirectional fluid shift, so that there would be a greater increase in cell size [16]. We determined that potassium did not play a significant role in our case, considering that sodium, not potassium, played the major role in determining fluid balance between the solution and intracellular space. Although potassium did not have an independent impact on adipocyte size, we cannot conclusively determine the influence of potassium in the context of tumescent injection. If hypotonic fluid also causes membrane damage in addition to osmotic swelling, potassium may or may not play a biologically significant role [10].
In several studies, ultrasound liposuction has been demonstrated to cause less tissue damage. Kenkel et al. [23] compared traditional and ultrasound lipectomies after tumescent injection and found, through radiographic assessments, less tissue damage with ultrasonic liposuction. In a study of 75 patients undergoing ultrasound versus traditional liposuction, the dopplered skin perfusion of suction-assisted lipectomy patients remained lower than that of ultrasound-assisted lipectomy patients at 1 week postoperatively [14]. Blondeel et al. [3] found that liposuction resulted in tissue damage, and that isotonic fluid injection alone produced significant tissue damage. If tumescent fluid could preferentially sensitize adipocytes to ultrasound energy, there is a potential for a further decrease in tissue damage. Subcutaneous injection of hypotonic fluid has had long-standing application outside plastic surgery, as hypodermoclysis, or subcutaneous infusion. Studies have determined it to be a safe and efficacious alternative to intravenous rehydration in the elderly [11,31]. With 1/2NS or 1/3NS infusions, local reactions were minor and systemic complications were rare. The most hypotonic solution used in our study, 1/4NS, has a consistent track record for safe clinical use in the pediatric population [12]. We can deduce that 1/4NS is most likely safe as a subcutaneous infusion.
There are limitations to our data. First, the conditions of our study do not accurately reflect the clinical scenario. Cell sizing cannot be performed effectively in whole-tissue specimens. Although isolation of adipocytes allows us to measure adipocyte size precisely, we must extrapolate this effect to intact tissue. We also must make the assumption that a majority of the injected fluid will come in contact with the majority of adipocytes in the treated region.
A second limitation is that the adipocytes floating in solution were subject to some degree of drift although the culture dish was immobilized under the microscope. Therefore, there were subtle variations in the sample population measured at different time points. Experimental variation attributable to cell drift is minimized by the fact that we observed a small standard deviation in our measurement of cell diameter (i.e., big cells and small cells manifested a similar increase in diameter when exposed to hypotonic solution). Moreover, we assumed an even distribution of adipocyte cell size throughout the culture dish that would compensate for any cell drift variations occurring between timed measurements.
Third, these data provide a theoretical framework for an increase in adipocyte sensitivity to ultrasonic dissolution. In further experiments, the authors are pursuing actual correlation of adipocyte diameter and cell lysis in response to ultrasound energy.
Conclusions
This study confirms that hypotonic solution can significantly increase human adipocyte cell diameter. The use of 1/4NS, a standard, commercially available fluid, has a significant effect on cell diameter within 15 min. Therefore, a tumescent solution with an osmolality of 1/4NS may facilitate ultrasonic lipoplasty.
References
Adamo C, Mazzocchi M, Rossi A, Suderi N: Ultrasonic liposcupturing: Extrapolations from the analysis of in vivo sonicated adipose tissue. Plast Reconstr Surg 100:220, 1997
Bjornheden T, Jakubowicz B, Levin M, Oden B, Eden S, Sjostrom L, Lonn M: Computerized determination of adipocyte size. Obes Res 12:95, 2004
Blondeel PN, Derks D, Roche N, Van Lanuyt KH, Monstrey SJ: The effects of ultrasound-assisted liposuction and conventional liposuction on the perforator vessels in the lower abdominal wall. Br J Plast Surg 56:266, 2003
Bond LJ, Cimino WW: Physics of ultrasonic surgery using tissue fragmentation: Part II. Ultrasound Med Biol 22:101, 1996
Bray: GA: Measurement of subcutaneous fat cells from obese patients. Ann Int Med 73:565, 1970
Chen WS, Matula TJ, Brayman AA, Crum LA: A comparison of the fragmentation thresholds and inertial cavitation doses of different ultrasound contrast agents. J Acoust Soc Am 113:643, 2003
Cimino WW. Personal communications, 2004
Cimino WW: The physics of soft tissue fragmentation using ultrasound frequency vibration of metal probes. Clin Plast Surg 26:447, 1999
Cimino WW, Bond LJ: Physics of ultrasonic surgery using tissue fragmentation: Part I. Ultrasound Med Biol 22:89, 1996
Feril LB Jr, Kondo T, Takaya K, Riesz P: Enhanced ultrasound-induced apoptosis and cell lysis by a hypotonic medium. Int J Radioat Biol 80:165, 2004
Ferry M, Dardaine V, Constans T: Subcutaneous infusion or hypodermoclysis: A practical approach. J Am Geriatr Soc 47:93, 1999
Filston HC: Fluid and electrolyte management in the pediatric surgical patient. Surg Clin North Am 72:1189, 1992
Fisher A, Fisher G: First surgical treatment for molding body’s cellulite with three 5-mm incisions. Bull Int Acad Cosmet Surg 3:35, 1976
Gupta SC, Khiabani KT, Stephenson LL, Zamboni WA: Effect of liposuction on skin perfusion. Plast Reconstr Surg 110:1748, 2002
Hoefflin SM: Lipoplasty with hypotonic pharmacologic lipodissolution. Aesthetic Surg J 22:573, 2002
Hoefflin SM: The future of liposuction and fat. Plast Reconstr Surg 104:1585, 1999
Illouz YG: Body contouring by lipolysis: A 5-year experience with over 3,000 cases. Plast Reconstr Surg 72:591, 1983
Illouz YG: Illouz’s technique of body contouring by lipolysis. Clin Plast Surg 11:409, 1984
Illouz YG: Refinement in lipoplasty technique. Clin Plast Surg 16:217, 1989
Illouz YG: Surgical remodeling of the silhouette by aspiration lipolysis or selective lipectommy. Aesth Plast Surg 9:7, 1985
Illouz YG: Surgical remodeling of the silhouette by lipolysis–aspiration or selective lipectomy. Ann Chir Plast Esthet 29:162, 1984
Illouz YG, Pfulg ME: Selective lipectomy and lipolysis after Illuoz. Handchir Mikrochir Plast Chir 18:118, 1986
Kenkel JM, Robinson JB Jr, Beran SJ, Tan J, Howard B, Zocchi ML, Rohrich RJ: The tissue effects of ultrasound-assisted lipoplasty. Plast Reconstr Surg 102:213, 1998
Kesselring UK, Meyer R: A suction curette for removal of excessive local deposits of subcutaneous fat. Plast Reconstr Surg 62:305, 1978
Klein JA: The tumescent technique for liposuction surgery. Am J Cosmetic Surg 4:263, 1987
Palmieri B, Criscuolo M, Gozzi G: Ultrasonic lipo-emulsification: A working definition and ex vivo study on human adipose tissue. Minerva Chir 49:71, 1994
Palmieri B, Gozzi G, Perrone V, Palmieri B: Ultrasonic liquid medium for lipo-emulsification: An experimental study. Minerva Chir 49:199, 1994
Perez JA, Tetering JPB: Ultrasound-assisted lipoplasty: A review of over 350 cases using a two-stage technique. Aesth Plast Surg 27:68, 2003
Rohrich RJ, Beran SJ, Fodor PB: The role of subcutaneous infiltration in suction-assisted lipoplasty: A review. Plast Reconstr Surg 99:514–519, 1997
Rohrich RJ, Kenkel JM, Janis JE, Beran SJ, Fodor PB: An update on the role of subcutaneous infiltration in suction-assisted lipoplasty. Plast Reconstr Surg 111:926, 2002
Slesak G, Schnürle JW, Kinzel E, Jakob J, Dietz K: Comparison of subcutaneous and intravenous rehydration in geriatric patients: A randomized trial. J Am Geriatr Soc 51:155, 2003
Tchoukalova YD, Harteneck DA, Karwoski RA, Tarara J, Jensen MD: A quick, reliable, and automated method for fat cell sizing. J Lipid Res 44:1795, 2003
Weninger K, Camara C, Putterman S: Physical acoustics of ultrasound-assisted lipoplasaty. Clin Plast Surg 26:463, 1999
Zocchi M: New perspective in lipoplasty: The ultrasonic-assisted lipectomy (UAL). Proceedings from the Congress of the French Society of Aesthetic Surgery. Paris, France, May, 1988
Zocchi ML: Basic physics for ultrasound-assisted lipoplasty. Clin Plast Surg 26:209, 1999
Acknowledgments
The authors thank Julio Clavijo, MD, PhD, Jeremy Breitinger, BS, and Aurele Taieb, MD, for their technical assistance in this project. Financial support for this project came from the Division of Plastic Surgery, University of Pittsburgh.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Song, A., Bennett, J.M., Marra, K.G. et al. Scientific Basis for the Use of Hypotonic Solutions with Ultrasonic Liposuction. Aesth Plast Surg 30, 233–238 (2006). https://doi.org/10.1007/s00266-005-0087-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-005-0087-z