Abstract
Purpose
The aim of study is to evaluate the accuracy of a navigation system during curved peri-acetabular osteotomy (CPO).
Methods
Forty-seven patients (53 hips) with hip dysplasia were enrolled and underwent CPO with or without navigation during surgery. Clinical and radiographical evaluations were performed and compared between the navigation group and non-navigation group, post-operatively.
Results
The clinical outcomes were not significantly different between the navigation and non-navigation groups. Furthermore, post-operative reorientation of the acetabular fragment was similar between the navigation and non-navigation groups. However, the discrepancy between the pre-operative planning line and post-operative osteotomy line was significantly improved in the navigation group compared with that in the non-navigation group (p < 0.05). Further, the complication rate was significantly improved in the navigation group (p < 0.001).
Conclusion
The accuracy of the osteotomy’s position was significantly improved by using the navigation. Therefore, the use of navigation during peri-acetabular osteotomy can avoid complications.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Developmental dysplasia of the hip (DDH) is the most common cause of osteoarthritis (OA) of the hip in Japan; more than 70% of OA of the hip is caused by DDH [1]. Many types of acetabular osteotomy have been developed to prevent OA such as rotational acetabular osteotomy (Ninomiya), peri-acetabular osteotomy (Ganz), spherical osteotomy (Wagner), and dial osteotomy (Eppright) [2,3,4,5].
The most important purpose of acetabular osteotomy is reorientation of the acetabulum into a normal position. The Bernese curved peri-acetabular osteotomy (CPO) provides good coverage of the femoral head by redirecting the acetabulum [6]. The Bernese PAO preserves the vascular supply of the transferred acetabulum and medializes the hip joint, but it has several disadvantages, including asphericity of the osteotomy surfaces due to straight cuts, leading to incongruity at the site of the osteotomy and anterior displacement of the hip joint [7]. To reduce these disadvantages, curved PAO (CPO) was developed for the treatment of DDH in Japan [6]. Exposure of the osteotomy sites and osteotomy of the ischium and pubis are performed in the same manner as that of the Bernese PAO, and iliac osteotomies are designed C-shape as previously described [4].
However, PAOs are technically demanding because of the complex anatomical structures of the pelvis and shallow visual field during surgery with potential risk for major complications and a previously reported steep learning curve [8,9,10]. The overall rate of peri-operative major complications was 6% [8], 5.9% [10], and 12% [9], respectively. The complication rate in terms of malposition cutting was 1% [8] and 3.8% [9], respectively.
The difficulty of the operation lies in determining the re-orientation of the acetabular fragment during pre-operative planning and intra-operative manipulation. One reason of the poor outcomes of peri-acetabular osteotomy is that pre-operative evaluation cannot be achieved by 2D imaging data. Because patients with dysplasia have less anterolateral acetabular coverage than those without, the distribution and degree of acetabular dysplasia have individual differences [11]. Therefore, assessment of the three-dimensional (3D) structures of the acetabulum before pre-operative planning should improve the surgical outcomes.
To compensate for these difficulties, many authors have developed 3D planning systems [12, 13], surgical navigation systems [14, 15], and custom cutting guides [16, 17]. Navigation has been developed over the last decade and potentially improves the accuracy of cutting during CPO. We have been using this navigation system for pre-operative planning and intra-operative osteotomy since 2014. In this prospective study, we aimed to evaluate the accuracy of using this navigation system during CPO.
Patients and methods
Patients and procedure
This study included 47 patients (53 hips) in six men and 41 women. The patients underwent CPO for DDH from 2014 to 2016. Pre-operatively, all patients were classified as having grade 0 or 1 OA according to the Tönnis classification [18]. The average age at surgery was 29.9 years (range 16–49 years), and the average follow-up duration was 2.1 years. We divided the patients into two groups: those in whom navigation (30 hips) or non-navigation (23 hips) was used during surgery. We used navigation during surgery from 2014 to 2015 and did not use navigation in 2016 to make a control group.
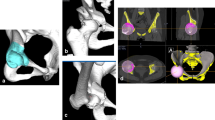
All patients underwent pre-operative 3D planning with a 100-mm radius sphere using navigation software (OrthoMap 3D Navigation System; Stryker Orthopaedics, Mahwah, NJ, USA) (Fig. 1a). The targets of pre-operative planning were as follows: (1) adequate femoral head coverage was based on the acetabular fragment (lateral CE 30°, anterior CE 60°), (2) horizontal position of the weight-bearing area of the acetabular fragment, and (3) medialization of the centre of the hip referred to the ilioischial line.
Display of the navigation system. a Pre-operative 3D planning with a 100-mm radius sphere. b The position and direction of the sphere were checked pre-operatively using a pointer with optical sensors. c The lateral edge of the acetabular fragment was checked with the navigation pointer after the fragment was rotated
The patient was placed on a radiolucent table in the supine position. Prior to incising the skin, we fixed reference markers to the contralateral iliac crest with two apex pins. A direct anterior approach with a skin incision of approximately 9 cm was used for surgical exposure. The osteotomy was performed in the same manner as that of a procedure that was previously described in detail [6]. The pelvis was registered using a surface-matched technique prior to osteotomy [19]. After registration, the position and direction of the sphere that were determined during pre-operative planning were checked using a pointer with optical sensors (Fig. 1b). A flexion chisel was introduced into the space between the distal joint capsule and the psoas tendon. When the blade contacted the surface of the ischium, the direction of the chisel toward the infracotyloid groove was confirmed with image intensifier, and osteotomy was performed. A pubic osteotomy was performed just medial to the iliopubic eminence. A C-shaped osteotomy line was marked with a power drill from the anterior inferior iliac spine to the distal part of the quadrilateral surface along the spherical position and direction.
During spherical osteotomy, the position and direction were checked with a pointer. After spherical osteotomy, the acetabular fragments were rotated laterally and anteriorly to the position and direction that were determined during pre-operative planning, checked by touching the lateral edge of the acetabular fragment with the navigation pointer (Fig. 1c), and then fixed temporarily using a Kirschner wire. Alternatively, an image intensifier was used to achieve the target position and direction when navigation was not used. Two or three poly-l-lactic acid screws or metal cancellous screws were used to finally fix the reoriented acetabular fragment (Fig. 2).
Clinical evaluation
Hip function was evaluated using the Japanese Orthopaedic Association (JOA) score, which allocates 40 points for pain, 20 points for range of motion, 20 points for walking ability, and 20 points for activities of daily living, with a maximum total score of 100 points [20]. The JOA score was evaluated pre-operatively and at the one year follow-up. The University of California, Los Angeles (UCLA) activity score was also evaluated at the one year follow-up assessment. The operation time and blood loss during osteotomy were also evaluated.
Radiographic evaluation
Pre- and post-operative computed tomography (CT) images were transferred to the navigation software and analyzed. The axis of pelvic plane was according to functional pelvic plane. The pre- and post-operative lateral and anterior 3D center-edge (CE) angles or acetabular head index (AHI) were measured on coronal and sagittal views through the center of the femoral head.
Accuracy evaluation
Pre-operative and post-operative CT images were superimposed to determine the shape of the pelvic ring using a volume registration method. The pre-operative spherical osteotomy line was superimposed on the post-operative CT images.
The accuracy of the osteotomy’s position was measured as the distance between the sphere line that was determined during pre-operative planning and the post-operative iliac bone surface.
The accuracy of the osteotomy was measured on the reconstructed coronal and axial plane through the centre of the sphere that was determined during pre-operative planning (Fig. 3a). Each measurement was performed on the external and internal surfaces of the superior pelvis at the coronal plane, and posterior pelvis at the axial plane (Fig. 3b). We defined the distance between the sphere line that was determined during pre-operative planning and the post-operative iliac bone surface as the error distance.
The measurement of the distance between the 100-mm radius sphere line that was determined during pre-operative planning and the post-operative iliac bone surface (the error distance) on the a coronal and b axial planes. a The error distance outside the pelvis on the coronal plane (50–45.5 mm = 4.5 mm). b The error of the distance inside the pelvis on the axial plane (57.8–50 mm = 7.8 mm)
Statistical analysis
All data are expressed as the mean ± standard deviation unless otherwise indicated. Between-group comparisons were evaluated using the Mann-Whitney U test. The complication rate was evaluated using a chi-square test. The database was analyzed using SPSS version 16.0 software (IBM Corp., Armonk, NY, USA). p values < 0.05 were considered to be statistically significant.
Ethics
The study protocol was approved by our institutional ethics committee on September 8, 2011 (No. 1219), and informed consent for participation in the study was obtained from all participants.
Results
Patient characteristics and clinical outcomes
The background characteristics of the patients in our study are summarized in Table 1. The mean values of the pre- and post-operative JOA and UCLA scores were not significantly different between the navigation and non-navigation groups (Table 1). Further, the operation time and blood loss were not significantly different between the navigation and non-navigation groups (Table 1).
Post-operative reorientation of the acetabular fragment was not different with navigation
The mean values of each lateral CE, anterior CE, and AHI were not significantly different between the navigation and non-navigation groups (Table 2).
The accuracy of the osteotomy position was improved with navigation
The mean error distances of the superior pelvis on the coronal plane were 1.2 mm (inside the pelvis) and 4.1 mm (outside the pelvis) with navigation, but the error distances were 5.6 mm (inside the pelvis) and 7.3 mm (outside the pelvis) without navigation (Fig. 4a). There were significant differences in the error distance between the navigation and non-navigation groups (inside the pelvis: p = 0.0004; outside the pelvis: p = 0.0478) (Fig. 4a). Furthermore, the mean error distances of the posterior pelvis on the axial plane were 3.1 mm (inside the pelvis) and 4.2 mm (outside the pelvis) with navigation, but the error distances were 6.2 mm (inside the pelvis) and 6.7 mm (outside the pelvis) without navigation (Fig. 4b). There were significant differences in the error distance between the navigation and non-navigation groups (inside the pelvis: p = 0.0192; outside the pelvis: p = 0.0179) (Fig. 4b).
Peri-operative complications
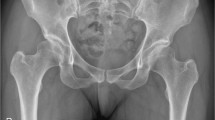
There was no peri-operative complication as pulmonary embolism, deep infection, peroneal nerve dysesthesia, and vascular injuries in this study group. In the navigation group, there were no cases of peri-operative complications of intra-articular cutting and posterior column fracture, but one patient in the non-navigation group experienced an intra-articular osteotomy (Fig. 5), and another patient experienced posterior column fracture. We compared peri-operative complications rate in terms of malposition cutting between the navigation and non-navigation groups. The complication rate was significantly improved in the navigation group compared with that in the non-navigation group (navigation group, 0%; non-navigation group, 8.7%; p < 0.001).
Discussion
The findings of our study suggested that the use of navigation during PAO did not affect clinical outcomes or reorientation of the acetabular fragment. However, the use of navigation prevented complication in terms of malposition cutting.
Computer-assisted technologies have been developed to treat bone tumours of the pelvis, with the main objective of improving the accuracy of bone cutting. Cartiaux et al. demonstrated the accuracy of cutting during navigated and non-navigated, simulated bone tumour cutting of pelvic bone [21]. The osteotomy position relative to that of the target was significantly improved by using the navigation system; the average error distance was 2.8 mm compared with 11.2 mm for the non-navigation procedure (p < 0.001) [21]. Furthermore, intralesional tumour cutting did not occur when using the navigation system [21]. Takao et al. demonstrated the clinical and radiographic outcomes of rotational acetabular osteotomy (RAO) using the same navigation system that was used in our study [19]. The average error distance between the osteotomy position and the target position was 1.3–1.5 mm inside the pelvis and 2.0–2.4 mm outside the pelvis [19]. The accuracy of the osteotomy position was more accurate than in our series. This was because they used a special chisel for navigation, which enabled them to use the chisel during bone cutting. Their study evaluated whether or not a computer navigation system combined with a pre-operative CT-based plan improved surgeons’ ability to perform RAO more accurately, regardless of their level of experience with performing osteotomies, but they did not compare the accuracy of navigation compared with that of non-navigation [19]. We demonstrated that the osteotomy’s position was improved by using navigation. The accuracy of the osteotomy position is critical to avoid disastrous complications such as posterior column fracture and intra-articular cutting. Two patients who did not undergo navigation in this series experienced an intra-articular cutting. However, among patients who underwent navigation, none experienced complications in terms of malposition cutting. Thus, the use of navigation during osteotomy should avoid the occurrence of complications in terms of malposition cutting.
Two studies compared the clinical outcomes of the radiographic reorientation angle of the acetabular fragment between patients who did and did not undergo navigation during PAO [22, 23]. There were no differences between the two groups in terms of clinical outcomes or correction of femoral head coverage and the anterior and lateral CE angles, and these studies concluded that a computer-assisted navigation system offers little additional benefit when the surgery is performed by an experienced surgeon [22, 23]. The osteotomies of these two studies were performed in a lateral decubitus position as rotational acetabular osteotomy, and the studies analyzed the reorientation angle of the acetabular fragment but did not analyze the accuracy of the osteotomy position. We compared the reorientation angle of the acetabular fragment and clinical outcomes between patients who did and did not undergo navigation. However, the average lateral CE angle, anterior CE angle, AHI, and clinical outcomes were not different between the two groups. This was because the reorientation angle of the acetabular fragment was usually controlled under C-arm imaging when navigation was not used during surgery, and adequate lateral and anterior acetabular coverage was critical to obtain excellent clinical outcomes [24]. Therefore, the reorientation angle of the acetabular fragment and clinical outcomes were not different between the navigation and non-navigation groups.
The limitation of this study is that the cohort was likely not large enough in size to enable a full evaluation of the clinical results and rare complication associations with navigation use. In conclusion, the reorientation angle of the acetabular fragment and clinical outcomes were not different between two groups, but the accuracy of the osteotomy position was significantly improved by using the navigation system. Therefore, the use of navigation during peri-acetabular osteotomy can avoid complications.
References
Nakamura S, Ninomiya S, Nakamura T (1989) Primary osteoarthritis of the hip joint in Japan. Clin Orthop Relat Res 241:191–196
Eppright RH (1975) Dial osteotomy of acetabulum in treatment of dysplasia of hip. J Bone Joint Surg Am 57:1172–1172
Ganz R, Klaue K, Vinh TS, Mast JW (1988) A new periacetabular osteotomy for the treatment of hip dysplasias. Technique and preliminary results. Clin Orthop Relat Res 232:26–36
Ninomiya S, Tagawa H (1984) Rotational acetabular osteotomy for the dysplastic hip. J Bone Joint Surg Am 66:430–436
Schramm M, Pitto RP, Rohm E, Hohmann D (1999) Long-term results of spherical acetabular osteotomy. J Bone Joint Surg Br 81:60–66
Naito M, Shiramizu K, Akiyoshi Y, Ezoe M, Nakamura Y (2005) Curved periacetabular osteotomy for treatment of dysplastic hip. Clin Orthop Relat Res 129–135
Millis MB, Murphy SB, Poss R (1996) Osteotomies about the hip for the prevention and treatment of osteoarthrosis. Instr Course Lect 45:209–226
Novais EN, Carry PM, Kestel LA, Ketterman B, Brusalis CM, Sankar WN (2017) Does surgeon experience impact the risk of complications after Bernese periacetabular osteotomy? Clin Orthop Relat Res 475:1110–1117. https://doi.org/10.1007/s11999-016-5010-1
Ito H, Tanino H, Sato T, Nishida Y, Matsuno T (2014) Early weight-bearing after periacetabular osteotomy leads to a high incidence of postoperative pelvic fractures. BMC Musculoskelet Disord 15:234. https://doi.org/10.1186/1471-2474-15-234
Zaltz I, Baca G, Kim YJ, Schoenecker P, Trousdale R, Sierra R, Sucato D, Sink E, Beaule P, Millis MB, Podeszwa D, Clohisy JC (2014) Complications associated with the periacetabular osteotomy: a prospective multicenter study. J Bone Joint Surg Am 96:1967–1974. https://doi.org/10.2106/JBJS.N.00113
Mast JW, Brunner RL, Zebrack J (2004) Recognizing acetabular version in the radiographic presentation of hip dysplasia. Clin Orthop Relat Res 418:48–53
Hipp JA, Sugano N, Millis MB, Murphy SB (1999) Planning acetabular redirection osteotomies based on joint contact pressures. Clin Orthop Relat Res 314:134–143
Liu L, Ecker TM, Schumann S, Siebenrock KA, Zheng G (2016) Evaluation of constant thickness cartilage models vs. patient specific cartilage models for an optimized computer-assisted planning of periacetabular osteotomy. PLoS One 11:e0146452. https://doi.org/10.1371/journal.pone.0146452
Pflugi S, Liu L, Ecker TM, Schumann S, Larissa Cullmann J, Siebenrock K, Zheng G (2016) A cost-effective surgical navigation solution for periacetabular osteotomy (PAO) surgery. Int J Comput Assist Radiol Surg 11:271–280. https://doi.org/10.1007/s11548-015-1267-1
Murphy RJ, Armiger RS, Lepisto J, Mears SC, Taylor RH, Armand M (2015) Development of a biomechanical guidance system for periacetabular osteotomy. Int J Comput Assist Radiol Surg 10:497–508. https://doi.org/10.1007/s11548-014-1116-7
Radermacher K, Portheine F, Anton M, Zimolong A, Kaspers G, Rau G, Staudte HW (1998) Computer assisted orthopaedic surgery with image based individual templates. Clin Orthop Relat Res 354:28–38
Otsuki B, Takemoto M, Kawanabe K, Awa Y, Akiyama H, Fujibayashi S, Nakamura T, Matsuda S (2013) Developing a novel custom cutting guide for curved peri-acetabular osteotomy. Int Orthop 37:1033–1038. https://doi.org/10.1007/s00264-013-1873-x
Tonnis D, Heinecke A (1999) Acetabular and femoral anteversion: relationship with osteoarthritis of the hip. J Bone Joint Surg Am 81:1747–1770
Takao M, Nishii T, Sakai T, Sugano N (2017) Comparison of rotational acetabular osteotomy performed with navigation by surgeons with different levels of experience of osteotomies. Int J Comput Assist Radiol Surg 12:841–853. https://doi.org/10.1007/s11548-016-1494-0
Hasegawa Y, Iwata H, Mizuno M, Genda E, Sato S, Miura T (1992) The natural course of osteoarthritis of the hip due to subluxation or acetabular dysplasia. Arch Orthop Trauma Surg 111:187–191
Cartiaux O, Banse X, Paul L, Francq BG, Aubin CE, Docquier PL (2013) Computer-assisted planning and navigation improves cutting accuracy during simulated bone tumor surgery of the pelvis. Comput Aided Surg 18:19–26. https://doi.org/10.3109/10929088.2012.744096
Hsieh PH, Chang YH, Shih CH (2006) Image-guided periacetabular osteotomy: computer-assisted navigation compared with the conventional technique: a randomized study of 36 patients followed for 2 years. Acta Orthop 77:591–597. https://doi.org/10.1080/17453670610012656
Inaba Y, Kobayashi N, Ike H, Kubota S, Saito T (2016) Computer-assisted rotational acetabular osteotomy for patients with acetabular dysplasia. Clin Orthop Surg 8:99–105. https://doi.org/10.4055/cios.2016.8.1.99
Albers CE, Steppacher SD, Ganz R, Tannast M, Siebenrock KA (2013) Impingement adversely affects 10-year survivorship after periacetabular osteotomy for DDH. Clin Orthop Relat Res 471:1602–1614. https://doi.org/10.1007/s11999-013-2799-8
Author information
Authors and Affiliations
Contributions
S. Haya designed the study. S. Haya, S. Hashi, KT, TM, KI, and NS collected the data. S. Haya and TM interpreted the data. KN performed the statistical analysis. S. Haya drafted the article. RK conducted the critical review and made the final approval.
Corresponding author
Ethics declarations
The study protocol was approved by our institutional ethics committee on September 8, 2011 (No. 1219), and informed consent for participation in the study was obtained from all participants.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Hayashi, S., Hashimoto, S., Matsumoto, T. et al. Computer-assisted surgery prevents complications during peri-acetabular osteotomy. International Orthopaedics (SICOT) 42, 2555–2561 (2018). https://doi.org/10.1007/s00264-018-3906-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-3906-y