Abstract
Background
The aim of this prospective, randomised and single blinded study was to evaluate the efficiency and safety of a new cryotherapy device in patients undergoing unilateral, primary total knee arthroplasty (TKA). Our hypothesis was that patients administered to the new cryotherapy device would perform better than patients receiving a conventional standard cold therapy regimen.
Methods
Ninety-seven patients were randomised into two groups receiving either the cTreatment® (new cryotherapy device) or the standard cold therapy protocol (including cold pack application for six days after the surgical intervention). We evaluated the following endpoints consisting of range of motion (ROM), pain intensity, and knee girth on admission day and the second, fourth, and sixth post-operative day (POD).
Results
A statistically significant benefit of the new cryotherapy device was detected regarding the ROM on the sixth POD with an average gain of 7 degrees (p = 0.021). Pain in the numeric rating scale (NRS) score in motion was significantly lower in the cTreatment® group on the second POD (p = 0.034). There were no statistically significant differences between groups regarding the NRS in rest, patient controlled analgesia (PCA) consumption, and girth measurements. No adverse effects were observed in both study groups.
Conclusion
The new computer-controlled cooling therapy device provides benefits in terms of early post-operative remobilisation with respect to ROM and pain, which might be attributed to a reduced inflammatory response, as well as reduced secretion and bleeding. The cTreatment® system appears to be a safe and efficient procedure.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Total knee arthroplasty (TKA) is a standard approach to improve quality of life for patients with end stage osteoarthritis of their knee joint, limited range of motion (ROM), and increasing knee pain [1,2,3]. In order to enhance the recovery and outcome after TKA in recent years, more and more attention is drawn to the improvement of post-operative soft tissue treatment. It is therefore a mandatory aim of fast-track arthroplasty to enable patients to leave the hospital earlier, which might lead to less nosocomial infections and overall lower socioeconomic burdens.
External application of cold therapy in the proximity of joints can be performed with various mediums such as ice [4,5,6], cooled fluids [4, 6,7,8,9,10,11], cooled air, or cooled gas [4]. The benefit of local cooling is its universal access and the low costs. Following surgical intervention of the knee joint the cooling process aids to minimise the intra-operatively induced soft tissue damage of all affected anatomical structures. It was proven that externally and superficially applied cooling outreaches transdermal structures, which consecutively implies that not only the skin temperature is strikingly decreased but also the intra-articular measured temperature [12]. All effects triggered by local cooling, such as moderating symptoms related to inflammation, pain, and swelling [13], are superficial as well as profoundly equally active. It has been shown that locally applied cold could induce analgesia [14, 15], anti-inflammatory effects in terms of diminishing local mediators [16, 17], and reduction in peripheral blood flow due to vasoconstriction [13, 15, 16].
Systematic reviews could already detect significant enhancements favouring cryotherapy in post-operative pain, which were particularly manifest around the second post-operative day (POD) [18, 19]. Literature has demonstrated the potential of a cold-based reduction of post-operatively required analgesia after reconstruction of the anterior cruciate ligament (ACL) [20], and Su et al. [6] and Morsi et al. [11] were able to observe significantly declined post-operative administrations of analgesics in patients undergoing TKA. Whereas several studies were not able to find between-group differences regarding the post-operative swelling and knee girth [4, 6], Kullenberg et al. [8] and Morsi et al. [11] found distinct cold-induced improvements to the knee’s ROM, particularly several days after the surgical intervention and after discharge. In terms of the post-operative blood loss after TKA, which appears to be a serious clinical problem with confirmed losses reaching up to 1500 ml [21], it was evident to record significantly lower losses by use of a haemovac, which was removed after 48 hours post-operatively [10, 11]. In addition, Kullenberg et al. stated a significantly slighter haemoglobin drop after surgery in patients receiving adequate cryotherapy [8]. Recent large-scale systemic reviews performed by Adie et al. in 2010 and 2012 resulted in small reductions in post-operative blood loss after TKA based on cryotherapy [18, 19]. The same authors summarised that cryotherapy was a safe procedure, with the most common cause for withdrawal and termination of the cold therapy being subjectively experienced discomfort [18]. Concerning the length of hospital stay, two reviewed studies verified a statistically significant shortened hospitalisation to the exact same extent of 1.4 days in study groups using post-operative cryotherapy [8, 9], although Scarcella et al. could only observe this difference in patients undergoing total hip arthroplasty, as the group of patients after TKA might have been underpowered [9].
However, until today, there has not been any consensus on the optimal application method of cryotherapy after TKA and therefore the presented study is of clinical importance and highly relevant [18, 19, 22].
The purpose of this prospective, randomised, single-blind, and controlled clinical study was therefore to compare a new cryotherapy device with a standard cooling protocol, consisting of cold packs only in patients undergoing primary and unilateral TKA in terms of pain reduction, mobilisation, analgesic consumption, and knee girth circumference.
Our study hypothesis was that patients receiving the new cryotherapy device would benefit with respect to early post-operative rehabilitation, mobilisation (range of motion), analgesic consumption, and knee girth and that the device represents a safe and efficient option.
Patients and methods
This study was conducted as a prospective, randomised and single-blind, comparative controlled clinical trial between December 2011 and April 2013 at the Department of Orthopaedic Surgery of the Medical University of Graz, Austria in line with the CONSORT checklist [23]. In addition, this study was approved by the local ethics committee with the trial number: 24-214 ex 11/12.
Patients between 55 and 90 years of age suffering from severe degenerative end-stage osteoarthritis of the knee joint who were scheduled for implantation of TKA were eligible for enrolment in this study after providing informed consent. Exclusion criteria were severe pre-existing local and systemic conditions others than gonarthritis and foregone surgical interventions others than arthroscopy of the knee joint. Rheumatoid arthritis was also an exclusion criteria. We did not exclude patients who had undergone contralateral TKA or THA on one or both sides. There were no changes after trial commencement with respect to eligibility criteria.
After giving their written consent with help of a study nurse the patients were randomised to a cryotherapy group, receiving the cTreatment® system (new cryotherapy device with a continuous cold flow), or the standard group, receiving conventional cold pack application. Randomization was performed in a 1:1 ratio, using the web-based programme “Randomizer” [24]. Permuted block randomization was performed with block size 6 and stratified for sex and scheduled design type of endoprostheses to be implanted, which was either the PFC® or the LCS® system (both from DePuy®, Warsaw, IN, USA).
After being randomised to the therapy group, patients were assigned to the locally applied cryotherapy treatment by use of the new cryotherapy device until the end of the clinical study, which was set for the sixth POD. That implied the first cooling session for one hour already pre-operatively on the pre-operative day (PreOD). Furthermore, the subjects received cryotherapy immediately after TKA in the postanaesthesia care unit for six hours in total. During the in-patient setting until the sixth POD, the new cryotherapy device was applied each day for four hours in total, namely, two hours in the morning and two hours in the afternoon. In addition, there was the option to use the new cryotherapy device in terms of additional analgesia in the evening for up to four hours on each POD.
According to the manufacturer, the new cryotherapy device is a class IIa medical device, which thermodynamically exchanges heat, which is controlled by a built-in computer. It is able to regulate both the flow rate and the fluid’s temperature reaching a special pad. The new cryotherapy device is operated by use of a touch screen, which allows to start, pause, resume, and stop a cooling session. According to the instruction manual, the pad, which is connected to the server with flexible tubes using an anti-reflux design, is made of flexible polyurethane, latex free, and hypoallergenic. Using hook and loop fasteners it is easy to wrap around the knee ensuring maximum contact surface (Fig. 1a, b). The device was applied on the post-operative dressing, which was performed in a standardised way in each single case.
a, b Pictures of the new cryotherapy device, operated by use of a touch screen, which allows to start, pause, resume, and stop a cooling session. The pad, which is connected to the server with flexible tubes using anti-reflux design, is made of flexible polyurethane, latex free, and hypoallergenic. Using hook and loop fasteners it is easy to wrap around the knee ensuring maximum contact surface
The control group (standard therapy [ST] group) was treated abiding by the standard cryotherapy regimen at our department including the use of common cold packs (cold/hot pack, Dahlhausen®, Cologne, Germany). They did not receive any cryotherapy before the surgical intervention corresponding to the standard regimen. After TKA, cold packs were applied three times per day for 20 minutes each throughout the whole trial. In the context of blinding, the cold packs were placed beneath the applied pads of the cryotherapy device in subjects randomised to the standard group, in order to account for a subjectively experienced cold as the CTS was turned off. The coolpacks were put beneath the applied pads, which were switched on or off according to randomization. From an ethical and scientific standpoint, this was the correct way, as it would not have been ethically correct to test the new device against no cooling method, which is our hospital standard. It was the most appropriate methodology, to put the coolpacks beneath the device, in order to achieve appropriate blinding.
Besides that, the study setting was identical in both groups.
For the purpose of a better comparability all participating patients received general anaesthesia and a post-operative analgesic therapy based on patient controlled analgesia (PCA), which was filled with diluted hydromorphone, accounting for 0.2 mg hydromorphone per single dose. In addition to that, Novalgin® (4 times, 1 g) was exclusively administered as a non-opiate analgesic. The PCA was removed after 72 hours post-operatively.
The performed physical measurements consisted of the quantification of the knee girth and the ROM of the treated knee joint as the primary endpoints. The measurements concerning the knee girth were performed at three different levels, at the middle of the patella, 7 cm proximal of the patellar base, and 7 cm distal of the apex patellae. The ROM was evaluated by use of a hand-held goniometer with the patient in a supine position. Extension lag was considered significant with a value greater than 5 degrees. In order to avoid potential bias of these measurements, inter- and intra-class correlations were calculated by two blinded observers. Among the non-physical evaluations (secondary endpoints) was verbally assessing the subjectively experienced pain intensity by use of the 11-point numeric rating scale (NRS) pain score, with zero corresponding to “no pain at all” and ten corresponding to “strongest pain imaginable”. The NRS was always evaluated for the state of absolute rest and the state of motion. In this relation the more objectively evaluable analgesics consumption was recorded. Therefore, the total hydromorphone usage administered by use of PCA after 72 hours was noted. The physical examinations of the knee joint’s ROM and girth and the NRS score evaluation were performed on admission day and the second, fourth, and sixth POD. In the course of the regular change of dressings during the medical rounds the surgical area was exactly examined for potential cold-induced local alterations. In this context, it was particularly searched for signs of frostbite, nerve palsy, inhibited wound healing, deep vein thrombosis and infection. In case of occurrence, the patients had also been told to immediately call attention to eventual adverse effects related to the cold therapy, which they were preliminarily informed about.
IBM® SPSS® Statistics software version 20 was used in order to perform the statistical analyses. In this regard descriptive statistics were conducted using basic calculations of means, standard deviations, medians, and minima and maxima. For the comparisons between the two study groups on admission day, the second, fourth, and sixth POD we first checked the data for normal distribution using Shapiro-Wilk and Kolmogorov-Smirnov tests. In case of normal distribution, the independent-samples t-test as a parametric test was performed. Otherwise, the Wilcoxon-Mann-Whitney test as non-parametric test was performed in order to obtain values of significance regarding between-group distinctions. An a priori power analysis according to the relevant literature evaluating similar endpoints (range of motion with a clinical significant difference greater than 5 degrees) revealed a group size of n = 45 patients each to be sufficient [25]. All p-values are regarded in an explorative sense. A p-value ≤0.05 was considered to be significant (Table 1).
Results
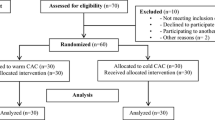
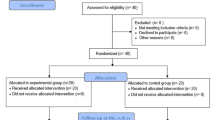
Ninety-seven patients met the inclusion criteria, gave written informed consent and were enrolled in the study. Baseline demographic and clinical characteristics are illustrated in Table 2. Eight of these patients were excluded from final statistical evaluation due to the following reasons: Two of these eight revoked their informed consent before the study proceedings started; in two cases it was intra-operatively decided to implant a constrained TKA; one patient received spinal anaesthesia although discussed otherwise when informing about the study’s requirements and proceedings; one patient suffered from an allergic reaction on the scheduled day of TKA surgery and was not able to adhere to the study protocol; one patient was discharged, because the surgical intervention was cancelled due to non-medical issues; and one final patient did not observe the cryotherapeutical protocol and showed incompliance in the first place. A flow chart of the inclusion of patients is further illustrated in Fig. 2. The trial stopped after the last follow-up of the last patient who was enrolled.
From these 97 patients, consisting of 53 females and 44 males, 46 were randomised into the cryotherapy (CT) group, receiving the new cryotherapy device, and 51 patients were randomised the standard treatment (ST) group, receiving conventional cold packs. All implanted TKAs were manufactured by the company Depuy®Synthes (Warsaw, IN), as we used 66 PFC® and 31 LCS® designs. There was no statistically significant difference between the study groups regarding the distribution of age, sex, pre-operative range of motion (ROM), and the implanted prostheses (Table 3).
Regarding the measured knee girth, we observed no statistically significant differences between both groups at any time point on any of the three measured levels (mid-patellar, 7-cm proximal to the patellar base, 7-cm distal to the apex patellae) with p-values of 0.659, 0.645, and 0.482 on the sixth POD as shown in Fig. 3.
Regarding the measured knee girth, we observed no statistically significant differences between both groups (new cryotherapy device [CT] versus standard group [Stand]) at any time point on any of the three measured levels (mid-patellar, 7-cm proximal of the patellar base, 7-cm distal of the apex patellae) with p-values of 0.659, 0.645, and 0.482, respectively on the sixth POD
Regarding the measured ROM we found high inter- and intra-class correlations with a value greater than 0.8 for each and we found that no knee joint revealed any significant extension lag. We found a statistically significant benefit of the new cryotherapy device regarding the measured flexion as the intervention group displayed greater ROM with 86 degrees ±7 SD, whereas the standard group achieved only 80 degrees ±14 SD (p = 0.021). The study groups featured approximately identical starting points on admission day, before the CT group showed more improvement on the second POD with 56 degrees ±11 SD compared to the ST group with 51 degrees ±16 SD, respectively, without statistical significance (p = 0.089) as shown in Fig. 4.
Measurements of flexion after total knee arthroplasty (TKA) in the course of the study in the new cryotherapy device (CT) group (n=46) versus the standard (Stand) cold packs (ST) group (n=51). Post-operatively, the new cryotherapy device group showed a slighter drop of flexion extent on the second post-operative day (POD) and regained flexion significantly faster and more steadily than the standard group on the sixth POD (86 versus 80 degrees, p=0.021)
We observed a statistically significant pain reduction in the NRS in motion on the second POD within the CT group displaying 3.7 points ± 2.1, whereas the ST group showed 4.6 points ± 2.1 (p = 0.034). In addition, in the ST group 12.11 mg ± 7.97 hydromorphone was required versus only 10.23 mg ± 5.05 in the CT group, but this difference was not statistically significant. The evaluated NRS score at rest did not indicate any statistically significant differences between the study groups throughout the trial. Values for NRS in motion are further illustrated in Fig. 5.
We recorded no adverse effects, such as frostbite, nerve palsy, inhibited wound healing, deep vein thrombosis, or soft tissue infection in neither the CT nor the ST group.
Discussion
The purpose of this prospective, randomised, single-blind, comparative and controlled clinical study was to evaluate a new cryotherapy device in comparison to the standard cooling protocol, consisting of cold packs only in patients undergoing primary and unilateral TKA.
Our study hypothesis was that patients receiving the new cryotherapy device would benefit with respect to early post-operative rehabilitation, mobilisation, analgesic consumption, and knee girth and that the device represents a safe and efficient option.
We found that both groups improved their ROM and had less pain but the new cryotherapy device provided substantial benefits in terms of post-operative remobilisation with respect to ROM and pain, which might be attributed to a reduced inflammatory response, as well as secretion and bleeding. The new cryotherapy device appears to be a safe and efficient procedure and might be of use for fast-track total joint arthroplasty.
Benefits of improved range of motion (ROM) as outlined in our investigation are in line with results from Kullenberg et al. proving a cold-related benefit of 11 degrees at three weeks post-operatively [8], and Morsi et al. who observed a benefit six weeks after the surgical intervention [11].
With respect to the monitored parameter of pain evaluated by use of NRS, a benefit for the CT group on the second POD was observed, which is consistent with systematic reviews handling similar investigations [18, 19]. Morsi et al. found significant benefits in the visual analogue scale (VAS) comparing cryotherapy to no cold therapy at all on the second POD [11]. A distinctly significant difference between the study groups had not been expected within the first 72 h after the surgical intervention, because of the possibility of individual pain modulation using the PCA system. Based on the controllable administration of hydromorphone, each patient was able to directly influence the subjectively perceived pain, which was quantified with the NRS score.
In this context, the objectively measured pain by use of the statistical analysis of the total PCA consumption after 72 h showed no statistical difference between the study groups (p = 0.409). This is in conformity with several other investigations [8,9,10, 29]. The absent possibility to show statistical significance might result from intensely varying data regarding the individual hydromorphone consumption by use of the PCA in patients assigned to both the new cryotherapy device group (intervention) and the standard group.
Over the course of the assessments, the mean girth of the knee joint strikingly increased after the TKA surgery in both groups, as already described by previous study groups [12, 14]. This is probably attributable to the variable intra-operative soft tissue trauma with consecutive secretion, bleeding, and oedema as well as to individual post-operative reaction. Generally, there were slight tendencies noticeably favouring the new cryotherapy device, particularly with respect to the fourth and sixth POD, but all of these results did not reach statistical significance (p > 0.05). This is in line with findings by Demoulin et al. and Su et al. [4, 6].
We could positively evaluate the safety of the new cryotherapy device in our prospective study. Although some previous studies reported on deep vein thrombosis [8] and further adverse effects within the control group [9], there was no occurrence of any adverse event recorded throughout our clinical trial. This is in conformity with the majority of the literature research [7, 10, 11, 29] revealing no significant complications after the use of cryotherapy. However, we want to record, that some of the patients noted suffering from subjective discomfort due to the cryotherapy, which was however not evaluated as a complication. The subjectively experienced discomfort in our patients might also be closely related to the high frequency of the application sessions, which was at least twice a day, and their single durations of at least two hours each.
Currently, there is still a standardised length of hospital stay for patients having undergone TKA surgery. Based on the present study’s statistical results of the knees’ ROM, which exhibited significant benefits for the new cryotherapy device on the sixth POD, and the not significantly diverging results concerning the pain evaluated in NRS and hydromorphone, it was preliminarily assumed that patients assigned to the new cryotherapy device group (intervention group) could be discharged sooner than patients in the standard group. This could however not be confirmed by the conducted study. A possible shortening of hospitalisation in patients treated with the new cryotherapy device could be shown in the future as two studies were already able to find a cryotherapy-related reduction of the length of hospitalisation to an extent of 1.4 days on average in patients undergoing TKA [8] and THA surgery [9], which was possibly due to an earlier start of independent ambulation within the cryotherapy group of both studies [8, 9]. A summary of outcomes of the recent literature using continuous cold flow cryotherapy is presented in Table 2.
We want to underline the following potential limitations: First, the used protocols between the new cryotherapy device and the standard cold pack treatment differed significantly with respect to the applied time. We decided not to change this because we wanted to compare these two treatment options in their original setting. Next, we want to outline the short follow-up period of our study. In addition, we want to underline that our main endpoint was range of motion, measured by goniometer with potential observer bias. However, we could eliminate this using intra- and inter-class observer correlations. Next, our study protocol allowed the patients a self indicated use of the device. However, this option was not chosen by any patient of this investigation. Finally, the new device was used over the postoperative dressing, which might have had an insulating effect. However, the dressing was applied in a standardised way in every single case and we used the same dressing in all patients of both groups.
Conclusion
Computer-controlled cooling therapy provides significant benefits in terms of early post-operative remobilisation with respect to early range of motion (ROM), which might be attributed to a reduced inflammatory response, as well as reduced secretion and bleeding. The new cryotherapy device appears to be a safe and efficient procedure in clinical practice.
References
Bourne RB, McCalden RW, MacDonald SJ, Mokete L, Guerin J (2007) Influence of patient factors on TKA outcomes at 5 to 11 years followup. Clin Orthop Relat Res 464:27–31
Sorrells RB, Voorhorst PE, Murphy JA, Bauschka MP, Greenwald AS (2004) Uncemented rotating-platform total knee replacement: a five to twelve-year follow-up study. J Bone Joint Surg Am 86-A(10):2156–2162
Hawker G, Wright J, Coyte P, Paul J, Dittus R, Croxford R et al (1998) Health-related quality of life after knee replacement. J Bone Joint Surg Am 80(2):163–173
Demoulin C, Brouwers M, Darot S, Gillet P, Crielaard JM, Vanderthommen M (2012) Comparison of gaseous cryotherapy with more traditional forms of cryotherapy following total knee arthroplasty. Ann Phys Rehabil Med 55(4):229–240
Holm B, Husted H, Kehlet H, Bandholm T (2012) Effect of knee joint icing on knee extension strength and knee pain early after total knee arthroplasty: a randomized cross-over study. Clin Rehabil 26(8):716–723
Su EP, Perna M, Boettner F, Mayman DJ, Gerlinger T, Barsoum W et al (2012) A prospective, multi-center, randomised trial to evaluate the efficacy of a cryopneumatic device on total knee arthroplasty recovery. J Bone Joint Surg Br 94(11 Suppl A):153–156
Radkowski CA, Pietrobon R, Vail TP, Nunley JA 2nd, Jain NB, Easley ME (2007) Cryotherapy temperature differences after total knee arthroplasty: a prospective randomized trial. J Surg Orthop Adv 16(2):67–72
Kullenberg B, Ylipaa S, Soderlund K, Resch S (2006) Postoperative cryotherapy after total knee arthroplasty: a prospective study of 86 patients. J Arthroplast 21(8):1175–1179
Scarcella JB, Cohn BT (1995) The effect of cold therapy on the postoperative course of total hip and knee arthroplasty patients. Am J Orthop (Belle Mead NJ) 24(11):847–852
Leutz DW, Harris H (1995) Continuous cold therapy in total knee arthroplasty. Am J Knee Surg 8(4):121–123
Morsi E (2002) Continuous-flow cold therapy after total knee arthroplasty. J Arthroplast 17(6):718–722
Martin SS, Spindler KP, Tarter JW, Detwiler KB (2002) Does cryotherapy affect intraarticular temperature after knee arthroscopy? Clin Orthop Relat Res (400):184–189
Demoulin C, Vanderthommen M (2012) Cryotherapy in rheumatic diseases. Joint Bone Spine 79(2):117–118
Abramson DI, Chu LS, Tuck S Jr, Lee SW, Richardson G, Levin M (1966) Effect of tissue temperatures and blood flow on motor nerve conduction velocity. JAMA 198(10):1082–1088
Ciolek JJ (1985) Cryotherapy. Review of physiological effects and clinical application. Cleve Clin Q 52(2):193–201
Stalman A, Berglund L, Dungnerc E, Arner P, Felländer-Tsai L (2011) Temperature-sensitive release of prostaglandin E2 and diminished energy requirements in synovial tissue with postoperative cryotherapy: a prospective randomized study after knee arthroscopy. J Bone Joint Surg Am 93(21):1961–1968
Jastrzabek R, Straburzynska-Lupa A, Rutkowski R, Romanowski W (2013) Effects of different local cryotherapies on systemic levels of TNF-alpha, IL-6, and clinical parameters in active rheumatoid arthritis. Rheumatol Int 33(8):2053–2060
Adie S, Kwan A, Naylor JM, Harris IA, Mittal R (2012) Cryotherapy following total knee replacement. Cochrane Database Syst Rev 9:CD007911
Adie S, Naylor JM, Harris IA (2010) Cryotherapy after total knee arthroplasty a systematic review and meta-analysis of randomized controlled trials. J Arthroplast 25(5):709–715
Raynor MC, Pietrobon R, Guller U, Higgins LD (2005) Cryotherapy after ACL reconstruction: a meta-analysis. J Knee Surg 18(2):123–129
Sehat KR, Evans RL, Newman JH (2004) Hidden blood loss following hip and knee arthroplasty. Correct management of blood loss should take hidden loss into account. J Bone Joint Surg Br 86(4):561–565
Barry S, Wallace L, Lamb S (2003) Cryotherapy after total knee replacement: a survey of current practice. Physiother Res Int 8(3):111–120
Consort checklist. www.consort-statement.org. Accessed 18 November 2017
Randomizer. Web-based patient randomization service for multi-center clinical trials. www.randomizer.at Accessed 31 December 2016
Ruffilli A, Castagnini F, Traina F, Corneti I, Fenga D, Giannini S, Faldini C (2017) Temperature-controlled continuous cold flow device after total knee arthroplasty: a randomized controlled trial study. J Knee Surg 30(7):675–681
Thienpont E (2014) Does advanced cryotherapy reduce pain and narcotic consumption after knee arthroplasty? Clin Orthop Relat Res 472:3417e23. https://doi.org/10.1007/s11999-014-3810-8
Bech M, Moorhen J, Cho M, Lavergne MR, Stothers K, Hoens AM (2015) Device or ice: the effect of consistent cooling using a device compared with intermittent cooling using an ice bag after total knee arthroplasty. Physiother Can 67:48e55
Schinsky MF, McCune C, Bonomi J (2016) Multifaceted comparison of two cryotherapy devices used after total knee arthroplasty: cryotherapy device comparison. Orthop Nurs 35:309e16
Smith J, Stevens J, Taylor M, Tibbey J (2002) A randomized, controlled trial comparing compression bandaging and cold therapy in postoperative total knee replacement surgery. Orthop Nurs 21(2):61–66
Funding
The company Waegener provided funds to finance the study nurse who acquired data for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
MG and RWP have received funding by Waegener®, Belgium and financed study nurses to obtain the data. The remaining authors report no potential conflict of interest.
Electronic supplementary material
ESM 1
(PDF 1456 kb)
Rights and permissions
About this article
Cite this article
Sadoghi, P., Hasenhütl, S., Gruber, G. et al. Impact of a new cryotherapy device on early rehabilitation after primary total knee arthroplasty (TKA): a prospective randomised controlled trial. International Orthopaedics (SICOT) 42, 1265–1273 (2018). https://doi.org/10.1007/s00264-018-3766-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-3766-5