Abstract
Purpose
The risk for re-tear following anterior cruciate ligament (ACL) reconstruction is influenced by several hormonal, neuromuscular, biomechanical and anatomic factors. One of the most important negative prognostic factors that markedly increase the risk for ACL re-tear is the presence of high knee-abduction moment (KAM), which can be measured immediately by landing on both feet after a vertical jump. We evaluated the effect in postoperative values for KAM according to the type of graft used for ACL reconstruction (hamstring vs patellar tendon) and a specific rehabilitation protocol focusing on recovery of muscular strength, proprioception and joint stabilisation.
Methods
From November 2010 to September 2012, we enrolled 40 female recreational athletes with clinical and imaging evidence of ACL tear and randomised them in two groups. One group of patients underwent reconstruction with a hamstring-tendon graft and the second with a patellar-tendon graft. A custom rehabilitation programme focusing on proprioception was adopted. Clinical outcomes [International Knee Documentation Committee (IKDC) and Lysholm scores] and performance in functional test for stability (single-leg hop, timed hop, crossover triple hop, KAM test) were assessed preoperatively at three and six months postoperatively.
Results
All patients showed statistically significant clinical improvements postoperatively when compared with preoperative values (P < 0.0001). No significant intergroup difference was observed in all clinical scores and functional tests, with the exception of the value registered for the KAM test (P < 0.0001).
Conclusions
ACL reconstruction using patellar-tendon graft followed by rehabilitation centred on strength, proprioception and stability restoration can produce satisfactory values for KAM within the physiological range. The surgical strategies should be adapted to the patient on the basis of a multidisciplinary approach.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Biomechanical, neuromuscular, psychological, hormonal and anatomical factors all impact on the risk of developing anterior cruciate ligament (ACL) tears [1–5]. In particular, epidemiological data show that women are particularly at risk for re-tear following ACL reconstruction [6, 7]. Biomechanical studies focusing on the knee-abduction moment (KAM), an index of knee stability, report that the higher the KAM value, the greater the risk of ACL re-tear [7–9]. Several factors influence KAM values; the most important are knee valgus moment, range of motion (ROM) in knee flexion, body mass, tibial length and quadriceps:flexor muscle ratio [8]. In women, KAM values are physiologically higher than in men [10], possibly (at least partially) explaining the higher incidence of re-tear in women. If using autologous semitendinosus and gracilis tendons as the graft for ACL reconstruction, the harvest can alter the ratio of strength between knee extensor and flexor muscles, resulting in even higher postoperative KAM values in these patients [11].
The definitive aim of the study was to compare the KAM values assesses in different patients to evaluate the possible different effects of the two surgical approaches (reconstruction using semitendinosus and gracilis vs patellar tendon) on knee stability restoration. Along with this primary intention, we attempted to verify the hypothesis of no difference in functional score [International Knee Documentation Committee (IKDC) and Lysholm score) in patient undergoing ACL reconstruction using either semitendinosus and gracilis or patellar tendon as graft choice in a population of female recreational athletes. We also aimedd to verify whether a rehabilitation protocol based on recovery of knee proprioception and postural control can improve postoperative KAM values compared with a historical control group in which a standard rehabilitation protocol was followed after surgery.
Materials and methods
Patients studied were recreational female athletes with a symptomatic, complete ACL tear detected on clinical (positive Lachman and pivot shift tests [12]) and imaging: lateral and anteroposterior (AP) weight-bearing radiographs to detect fractures, osteoarthritis grading and varus–valgus malalignment assessment; MRI to evaluate lesions to the ACL, cartilage, menisci and other knee ligaments.
Patients were all scheduled to undergo ACL reconstruction using a semitendinosus and gracilis or patellar tendon graft, followed by a standardised postoperative rehabilitation programme for 24 weeks. Patients requiring concomitant surgical management of meniscal lesions were also included in the study. Exclusion criteria were history of previous surgery on either knee, detection of cartilage lesions or osteoarthritic changes (joint-space narrowing >50 % in any compartment), multiligamentous involvement [posterior cruciate ligament (PCL), lateral collateral ligament (LCL), medial collateral ligament (MCL), posterolateral corner], concomitant ipsilateral leg fracture and cardiovascular disease.
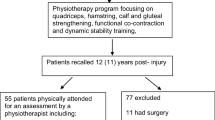
A total of 73 consecutive female recreational athletes operated at out institution between 2010 and 2012 met our inclusion criteria. However, 13 patients did not want to participate in the study, five had a grade III or IV chondral lesion, seven had multiligamentous injury and eight had positive history of surgery to the same knee; these patients were excluded. Ultimately, 40 patients were considered eligible for the study. The Consolidated Standards of Reporting Trials (CONSORT) flowchart [13] for this trial is presented in Fig. 1. Patients were then randomised into two groups using a computerised combination generator operaded by an investigator with no clinical involvement in the trial (SD). The first group consisted of patients who underwent ACL reconstruction using semitendinosus and gracilis tendon grafts (STG group); the second group consisted of patients undergoing ACL reconstruction using the middle third of the patellar tendon for reconstruction [bone–patellar tendon–bone (BPTB) group].
All patients played either football (N = 16), volleyball (N = 8) or basketball (N = 16). Although they all participated in sports before the accident, significant differences were found given the different types of training, intensity and physical load between required for the different sports. Mean follow-up was 12 months; mean interval of time from injury to surgery was 84 days [standard deviation (SD) ± 20, 95 % confidence interval (CI) 64–104] for the STG group and 89 days (SD ± 27, 95 % CI 72–100) for the BPTB group. Prior to data collection, each athlete read and signed an informed consent to participate in the study, which was approved by our Institution ethics committee. The study was conducted at the Department of Orthopaedic and Trauma Surgery of the Campus Bio-Medico University Hospital in Rome.
Operative findings and surgical technique
All patients were operated by two experienced orthopaedic surgeons (RP and FF) who performed routine ACL reconstructions using the transtibial technique [11, 14]. At diagnostic arthroscopy, all 40 patients were confirmed to have complete ACL tears. In the STG group, six underwent partial meniscectomies (three medial and three lateral) and three medial meniscus repair for a red–red zone tear. In the BPTB group, six patients underwent partial meniscectomies (three medial and three lateral) and two a meniscal repair: one for a red–red zone and one for a white–red zone tear. In the BPTB group, fixation was accomplished using metal interference screws (Arthrex, Naples, FL, USA); in the STG group, femoral fixation was accomplished using the TightRope® system (Arthrex). In the tibia, the graft was fixed using absorbable screw (Arthrex).
Rehabilitation protocol
All recruited patients followed a standard rehabilitation programme for a period of 24 weeks that consisted of five phases focusing on different recovery objectives: ROM (one to two weeks), force (three to four weeks), proprioception and stability (five to 11 weeks), run (nine to 14 weeks), power (15–24 weeks). Particular attention was paid to the third stage—fifth to 11th week—during which patients trained proprioception and postural stability. No patient withdrew from the study, and all attended at least 85 % of the rehabilitation sessions.
Postoperative clinical evaluation
Anteroposterior and rotational laxity were assessed using the Lachman [15] and the pivot shift [15] test, which were graded according to the IKDC. Pre- and postoperative clinical function was assessed according to the IKDC subjective knee assessment form [16] and Lysholm score [17]. These tests were evaluated preoperatively and at three and six months after surgery. Two weeks after the end of the rehabilitation protocol, all participants arrived at the Department of Physiotherapy to perform stability tests, which consisted in four exercises designed to evaluate both the knee stability and postural control. Tests used were single-leg hop, crossover triple hop, timed hop and KAM test.
-
Single-leg hop: with this test we calculated the maximum distance the patient could cover with a skip performed with one leg, taking off and landing on operated limb.
-
Timed hop (6 m): we calculated the time spent by the patient in covering a distance of 6 m jumping on one leg.
-
Crossover triple hop: three consecutive jumps were performed on one leg alternately from side to side of a line drawn on the floor, at the end of which the patient had to stop at the exact spot where she landed after the last jump and stay in balance.
-
KAM test: Patients were asked to jump from a box 30 cm high and, once they had touched the ground, to maintain the position of equilibrium. The exercise was repeated twice, and in the third repetition, two jumps as high as possible were performed after landing. This exercise primarily evaluated KAM and valgus attitude upon landing, an element that is particularly significant in predicting the risk of re-tear of the ACL. Upon landing, the patients’ ability to absorb the shock with their gluteus without subsequent knee failure was also evaluated. To supervise proper execution of this exercise, the instructor directed each patient to land with the weight equally divided between both lower limbs. This test was conducted under the supervision of two observers: a trained orthopaedic surgeon described the task and supervised the patient during the entire exercise to guarantee correct execution while preventing injuries. The other observer recorded the task using a series of HD video recorders located precisely in front and at both sides of the individual at a distance of 5 m from the landing surface. This individual measured knee angles in the coronal and sagittal planes by tracing the axes of interest using computer software on single frames. Knee abduction angles were the primary points of interest of these measurements, being a reliable indicator of KAM borne by the knee.
Statistical analysis
Descriptive statistics were calculated. Clinical improvement over time was assessed using analysis of variance (ANOVA) with repeated-measures analysis in clinical and functional scores. A P value of <0.05 was considered to be statistically significant. Statistical analysis was carried out using the Statistical Package for the Social Sciences (SPSS) software version 20.0 (SPSS Inc., Chicago, IL, USA).
We performed a priori power analysis to estimate the sample size: we took into account a large anticipated effect size (Cohen’s d value) of 0.9, setting statistical significance (P value) at 0.05 to reach a desired statistical power of ∼0.80, obtaining a minimum required sample size per group of 20 patients to achieve this level of significance for our comparison.
Results
The patient median age at presentation was 25.4 years (18–36) for the STG group and 24.7 years (17–30) for the BPTB group. All additional demographic data are shown in Table 1.
No statistically significant differences were found between groups in preoperative assessment (P<0.0001) (Tables 2 and 3).
Postoperative results at three and six months showed a statistically significant increase in IKDC and Lysholm scores compared with mean preoperative values in both treatment groups (Tables 4 and 5, Figs. 2 and 3). Approximately two weeks after completing rehabilitation, patients underwent knee-stability evaluation using the functional tests. While the single-leg hop, timed hop and crossover triple hop tests showed no statistically significant differences between groups, the BPTB group, the KAM test was significantly reduced compared with the STG group (P <0.0001). (Table 6)
These values were then compared with a historical control group of 40 female athletes who underwent ACL reconstruction to match the experimental groups for graft type used. However, these patients were treated with a standard postoperative rehabilitation approach. Statistically significant intergroup differences were found in this case, as shown in Tables 7 and 8.
Discussion
ACL reconstruction is undertaken to restore knee stability. An ACL lesion predisposes to a meniscal tear, and the association between the latter and an increased risk to develop knee osteoarthritis has been well established [12, 18–30]. Restoration of knee stability becomes a crucial aspect in athletes in whom articular demands are significantly higher [31–35].
Despite great advances in all aspect of ACL reconstruction surgery, such as graft type, bone-tunnel drilling technique, possible repair augmentation [36–38] and graft-fixation means [39], the rate of re-rupture remains high, particularly in women. The reasons for this are not entirely clear, but great efforts have been made to identify possible determinants [40–43].
KAM is an expression of dynamic stability of the knee, and it is a good predictor of the risk for the ACL to rupture [42]. Many factors contribute to a KAM value, amongst them being the relationship between quadriceps and flexor muscles [8]. Since STG ACL reconstruction alters this relationship, our study aimed to evaluate whether graft type can affect the KAM value and, subsequently, knee stability.
Our data confirmed that all patients who underwent ACL reconstruction, independently of graft used, demonstrated a statistically significant improvement between pre- and postoperative scores, without significant differences between groups. These data are in full agreement with the literature [44–51].
Histological studies confirmed the presence of neural structures with proprioceptive function in the ACL [12, 52, 53]. An ACL injury may lead to alterations in knee stability not only because of the altered biomechanics caused by the absence of the ligament, but also as a consequence of the alteration of proprioception from knee structures [54–59]. Therefore, full recovery of knee stability depends not only on surgical reconstruction but on a rehabilitation programme aimed at regaining proprioceptive control of the knee [60]. Our patients undertook a dedicated rehabilitation programme that provided, after the first month of standard rehabilitation training, a series of exercises intended to stimulate the recovery of neurological control of the joint. The comparison of postoperative KAM values as an indicator of knee stability between the patients in this series and a historical control group that followed standard rehabilitation demonstrates that the combination of ACL reconstruction and a custom rehabilitation programme based on recovery of postural control and proprioception could be effective in reducing the risk of graft re-rupture.
The current literature does not provide clear evidence as to whether the different surgical techniques adopted by surgeons for ACL reconstruction exert any other effect on postoperative KAM. Investigating this point was the main objective of our study. Results showed that KAM assessment through a functional test exhibited statistically significant differences between patients in whom the ACL was reconstructed using hamstring tendons compared with those in whom the patellar tendon was used. The latter showed lower KAM values, which are related to a lower risk of re-tear after surgery. From this observation, it is possible to hypothesise that surgical technique may have a primary role in attaining maximum knee stability following the intervention in female athletes, confirming previous suggestions of some authors, who demonstrated significantly greater postoperative laxity in reconstructed knees of female patients when using hamstring versus patellar tendons [61]. KAM is influenced by the relationship between quadriceps and flexor muscles of the lower limb. Using the BPTB graft does not alter this relationship, in contrast to using STG [62], and KAM may benefit from this approach. However, it is difficult to ascertain whether the greatest benefit regarding knee stability using this technique is due not only to alteration of muscle ratio or from other biomechanical and constitutional factors.
Strengths of this study are its prospective randomised design, the presence of two experienced orthopaedic surgeons, the presence of an independent operator for data collection and the use of standardised integrated tools to evaluate knee stability and, in particular, KAM. The design is pragmatic and compliant with CONSORT [13] criteria. Limitations are the relatively short follow-up and the small cohort.
Both a surgical and rehabilitation approach focusing on KAM conservation following ACL reconstruction in female athletes can improve stability of the operated knee, thus reducing the risk of postoperative re-ruptures. Results suggest considering the use of the patellar tendon as a graft combined with a dedicated rehabilitation protocol mostly focusing on recovery of postural control, proprioception and stability in female athletes with ACL deficiency.
References
Hewett TE, Lindenfeld TN, Riccobene JV, Noyes FR (1999) The effect of neuromuscular training on the incidence of knee injury in female athletes. A prospective study. Am J Sports Med 27(6):699–706
Hewett TE, Myer GD, Ford KR (2006) Anterior cruciate ligament injuries in female athletes: part 1, mechanisms and risk factors. Am J Sports Med 34(2):299–311. doi:10.1177/0363546505284183
Hewett TE, Ford KR, Myer GD (2006) Anterior cruciate ligament injuries in female athletes: Part 2, a meta-analysis of neuromuscular interventions aimed at injury prevention. Am J Sports Med 34(3):490–498. doi:10.1177/0363546505282619
Wojtys EM, Huston LJ, Lindenfeld TN, Hewett TE, Greenfield ML (1998) Association between the menstrual cycle and anterior cruciate ligament injuries in female athletes. Am J Sports Med 26(5):614–619
Ciuffreda P, Lelario M, Milillo P, Vinci R, Coppolino F, Stoppino L, Genovese E, Macarini L (2013) Mechanism of traumatic knee injuries and MRI findings. Musculoskelet Surg 97(2):127–135
Lyman S, Koulouvaris P, Sherman S, Do H, Mandl LA, Marx RG (2009) Epidemiology of anterior cruciate ligament reconstruction: trends, readmissions, and subsequent knee surgery. J Bone Joint Surg Am 91(10):2321–2328. doi:10.2106/JBJS.H.00539
Hewett TE, Myer GD, Ford KR (2005) Reducing knee and anterior cruciate ligament injuries among female athletes: a systematic review of neuromuscular training interventions. J Knee Surg 18(1):82–88
Myer GD, Ford KR, Khoury J, Hewett TE (2011) Three-dimensional motion analysis validation of a clinic-based nomogram designed to identify high ACL injury risk in female athletes. Phys Sportsmed 39(1):19–28. doi:10.3810/psm.2011.02.1858
Paterno MV, Schmitt LC, Ford KR, Rauh MJ, Myer GD, Huang B, Hewett TE (2010) Biomechanical measures during landing and postural stability predict second anterior cruciate ligament injury after anterior cruciate ligament reconstruction and return to sport. Am J Sports Med 38(10):1968–1978. doi:10.1177/0363546510376053
Webster KE, Feller JA (2012) The knee adduction moment in hamstring and patellar tendon anterior cruciate ligament reconstructed knees. Knee Surg Sports Traumatol Arthrosc: Off J ESSKA 20(11):2214–2219. doi:10.1007/s00167-011-1835-z
Pinczewski LA, Deehan DJ, Salmon LJ, Russell VJ, Clingeleffer A (2002) A five-year comparison of patellar tendon versus four-strand hamstring tendon autograft for arthroscopic reconstruction of the anterior cruciate ligament. Am J Sports Med 30(4):523–536
Papalia R, Franceschi F, Zampogna B, Tecame A, Maffulli N, Denaro V (2014) Surgical management of partial tears of the anterior cruciate ligament. Knee Surg Sports Traumatol Arthrosc : Off J ESSKA 22(1):154–165. doi:10.1007/s00167-012-2339-1
Schulz KF, Altman DG, Moher D, Group C (2010) CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. BMJ 340:c332. doi:10.1136/bmj.c332
Franceschi F, Papalia R, Rizzello G, Del Buono A, Maffulli N, Denaro V (2013) Anteromedial portal versus transtibial drilling techniques in anterior cruciate ligament reconstruction: any clinical relevance? A retrospective comparative study. Arthroscopy: J Arthrosc Relat Surg : Off Publ Arthroscopy Assoc N Am Int Arthroscopy Assoc 29(8):1330–1337. doi:10.1016/j.arthro.2013.05.020
Prins M (2006) The Lachman test is the most sensitive and the pivot shift the most specific test for the diagnosis of ACL rupture. Aust J Physiother 52(1):66
Hefti F, Muller W, Jakob RP, Staubli HU (1993) Evaluation of knee ligament injuries with the IKDC form. Knee Surg Sports Traumatol Arthrosc : Off J ESSKA 1(3–4):226–234
Briggs KK, Lysholm J, Tegner Y, Rodkey WG, Kocher MS, Steadman JR (2009) The reliability, validity, and responsiveness of the Lysholm score and Tegner activity scale for anterior cruciate ligament injuries of the knee: 25 years later. Am J Sports Med 37(5):890–897. doi:10.1177/0363546508330143
Barrios JA, Higginson JS, Royer TD, Davis IS (2009) Static and dynamic correlates of the knee adduction moment in healthy knees ranging from normal to varus-aligned. Clin Biomech 24(10):850–854. doi:10.1016/j.clinbiomech.2009.07.016
Barber FA, Click SD (1997) Meniscus repair rehabilitation with concurrent anterior cruciate reconstruction. Arthroscopy: J Arthrosc Relat Surg : Off Publ Arthroscopy Assoc of N Am Int Arthroscopy Assoc 13(4):433–437
Clatworthy M, Amendola A (1999) The anterior cruciate ligament and arthritis. Clin Sports Med 18(1):173–198, vii
Maffulli N, Osti L (2013) ACL stability, function, and arthritis: what have we been missing? Orthopedics 36(2):90–92. doi:10.3928/01477447-20130122-02
Hara K, Niga S, Ikeda H, Cho S, Muneta T (2008) Isolated anterior cruciate ligament reconstruction in patients with chronic anterior cruciate ligament insufficiency combined with grade II valgus laxity. Am J Sports Med 36(2):333–339. doi:10.1177/0363546507307501
Jacobsen K (1977) Osteoarthrosis following insufficiency of the cruciate ligaments in man. A clinical study. Acta Orthop Scand 48(5):520–526
van der Hart CP, van den Bekerom MP, Patt TW (2008) The occurrence of osteoarthritis at a minimum of ten years after reconstruction of the anterior cruciate ligament. J Orthop Surg Res 3:24
Cebesoy O (2006) What are the risk factors in the development of osteoarthritis following ACL reconstruction? Int Orthop 30(5):431–431
Krishnan SR, Randle R (2009) ACL reconstruction with unicondylar replacement in knee with functional instability and osteoarthritis. J Orthop Surg Res 4:43
Madhusudhan T, Kumar T, Bastawrous S, Sinha A (2008) Clinical examination, MRI and arthroscopy and meniscal and ligamentous knee Injuries – a prospective study. J Orthop Surg Res 3:19
Papalia R, Zampogna B, Torre G, Lanotte A, Vasta S, Albo E, Tecame A, Denaro V (2014) Sarcopenia and its relationship with osteoarthritis: risk factor or direct consequence? Musculoskeletal surgery:1–6
Maffulli N, Binfield PM, King JB (2003) Articular cartilage lesions in the symptomatic anterior cruciate ligament-deficient knee. Arthroscopy:J Arthrosc Relat Surg 19(7):685–690
Osti L, Papalia R, Del Buono A, Leonardi F, Denaro V, Maffulli N (2011) Surgery for ACL deficiency in patients over 50. Knee Surg Sports Traumatol Arthrosc 19(3):412–417
Osti L, Papalia R, Del Buono A, Leonardi F, Denaro V, Maffulli N (2011) Surgery for ACL deficiency in patients over 50. Knee Surg Sports Traumatol Arthrosc : Off J ESSKA 19(3):412–417. doi:10.1007/s00167-010-1242-x
Feller J, Webster KE (2013) Return to sport following anterior cruciate ligament reconstruction. Int Orthop 37(2):285–290
Chaves SF, Marques NP, Silva RL, Rebouças NS, de Freitas LM, de Paula Lima PO, de Oliveira RR (2012) Neuromuscular efficiency of the vastus medialis obliquus and postural balance in professional soccer athletes after anterior cruciate ligament reconstruction. MLTJ 2(2):121
Joseph C, Pathak SS, Aravinda M, Rajan D (2008) Is ACL reconstruction only for athletes? Int Orthop 32(1):57–61
Li R, Maffulli N, Hsu YC, Chan KM (1996) Isokinetic strength of the quadriceps and hamstrings and functional ability of anterior cruciate deficient knees in recreational athletes. Br J Sports Med 30(2):161–164
Yuan T, Zhang C-Q, Wang JH (2013) Augmenting tendon and ligament repair with platelet-rich plasma (PRP). MLTJ 3(3):139
Kanazawa T, Soejima T, Noguchi K, Tabuchi K, Noyama M, Nakamura K, Shiba N Tendon-to-bone healing using autologous bone marrow-derived mesenchymal stem cells in ACL reconstruction without a tibial bone tunnel-A histological study. Muscle, Ligaments and Tendons Journal 4 (2):201–206
Filomeno P, Dayan V, Touriño C (2012) Stem cell research and clinical development in tendon repair. MLTJ 2(3):204
Chambat P, Guier C, Sonnery-Cottet B, Fayard J-M, Thaunat M (2013) The evolution of ACL reconstruction over the last fifty years. Int Orthop 37(2):181–186
Samuelsson K, Andersson D, Ahlden M, Fu FH, Musahl V, Karlsson J (2013) Trends in surgeon preferences on anterior cruciate ligament reconstructive techniques. Clin Sports Med 32(1):111–126. doi:10.1016/j.csm.2012.08.011
Salmon L, Russell V, Musgrove T, Pinczewski L, Refshauge K (2005) Incidence and risk factors for graft rupture and contralateral rupture after anterior cruciate ligament reconstruction. Arthroscopy: J Arthrosc Relat Surg : Off Publ Arthroscopy Assoc of N Am Int Arthroscopy Assoc 21(8):948–957. doi:10.1016/j.arthro.2005.04.110
Myer GD, Ford KR, Khoury J, Succop P, Hewett TE (2010) Development and validation of a clinic-based prediction tool to identify female athletes at high risk for anterior cruciate ligament injury. Am J Sports Med 38(10):2025–2033. doi:10.1177/0363546510370933
Lui P, Zhang P, Chan K, Qin L (2010) Biology and augmentation of tendon-bone insertion repair. J Orthop Surg Res 5(1):1–14
Aglietti P, Buzzi R, D’Andria S, Zaccherotti G (1992) Arthroscopic anterior cruciate ligament reconstruction with patellar tendon. Arthroscopy: J Arthrosc Relat Surg : Off Publ Arthroscopy Assoc of N Am Int Arthroscopy Assoc 8(4):510–516
Aglietti P, Zaccherotti G, Menchetti PP, De Biase P (1995) A comparison of clinical and radiological parameters with two arthroscopic techniques for anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc : Off J ESSKA 3(1):2–8
Aglietti P, Buzzi R, Giron F, Simeone AJ, Zaccherotti G (1997) Arthroscopic-assisted anterior cruciate ligament reconstruction with the central third patellar tendon. A 5-8-year follow-up. Knee Surg Sports Traumatol Arthrosc : Off J ESSKA 5(3):138–144
Aglietti P, Buzzi R, Menchetti PM, Giron F (1996) Arthroscopically assisted semitendinosus and gracilis tendon graft in reconstruction for acute anterior cruciate ligament injuries in athletes. Am J Sports Med 24(6):726–731
Freedman KB, D’Amato MJ, Nedeff DD, Kaz A, Bach BR Jr (2003) Arthroscopic anterior cruciate ligament reconstruction: a metaanalysis comparing patellar tendon and hamstring tendon autografts. Am J Sports Med 31(1):2–11
Meighan AA, Keating JF, Will E (2003) Outcome after reconstruction of the anterior cruciate ligament in athletic patients. A comparison of early versus delayed surgery. J Bone Joint Surg Br Vol 85(4):521–524
Mohammadi F, Salavati M, Akhbari B, Mazaheri M, Mohsen Mir S, Etemadi Y (2013) Comparison of functional outcome measures after ACL reconstruction in competitive soccer players: a randomized trial. J Bone Joint Surg Am 95(14):1271–1277. doi:10.2106/JBJS.L.00724
Streich NA, Zimmermann D, Bode G, Schmitt H (2011) Reconstructive versus non-reconstructive treatment of anterior cruciate ligament insufficiency. A retrospective matched-pair long-term follow-up. Int Orthop 35(4):607–613
Katayama M, Higuchi H, Kimura M, Kobayashi A, Hatayama K, Terauchi M, Takagishi K (2004) Proprioception and performance after anterior cruciate ligament rupture. Int Orthop 28(5):278–281
Haus J, Halata Z (1990) Innervation of the anterior cruciate ligament. Int Orthop 14(3):293–296
Fonseca ST, Ocarino JM, Silva PL, Guimaraes RB, Oliveira MC, Lage CA (2005) Proprioception in individuals with ACL-deficient knee and good muscular and functional performance. Res Sports Med 13(1):47–61. doi:10.1080/15438620590922095
Jensen TO, Fischer-Rasmussen T, Kjaer M, Magnusson SP (2002) Proprioception in poor- and well-functioning anterior cruciate ligament deficient patients. J Rehabil Med : Off J UEMS (EBPRM) 34(3):141–149
Schultz RA, Miller DC, Kerr CS, Micheli L (1984) Mechanoreceptors in human cruciate ligaments. A histological study. J Bone Joint Surg Am 66(7):1072–1076
Woo SL-Y, Wu C, Dede O, Vercillo F, Noorani S (2006) Biomechanics and anterior cruciate ligament reconstruction. J Orthop Surg Res 1 (2)
Dhillon MS, Bali K, Prabhakar S (2012) Differences among mechanoreceptors in healthy and injured anterior cruciate ligaments and their clinical importance. MLTJ 2(1):38
Papalia R, Franceschi F, Vasta S, Di Martino A, Maffulli N, Denaro V (2012) Sparing the anterior cruciate ligament remnant: is it worth the hassle? Br Med Bull 104(1):91–111
Mohammadi F, Salavati M, Akhbari B, Mazaheri M, Khorrami M, Negahban H (2012) Static and dynamic postural control in competitive athletes after anterior cruciate ligament reconstruction and controls. Knee Surg Sports Traumatol Arthrosc : Off J ESSKA 20(8):1603–1610. doi:10.1007/s00167-011-1806-4
Gobbi A, Domzalski M, Pascual J (2004) Comparison of anterior cruciate ligament reconstruction in male and female athletes using the patellar tendon and hamstring autografts. Knee Surg Sports Traumatol Arthrosc: Off J ESSKA 12(6):534–539. doi:10.1007/s00167-003-0486-0
Barenius B, Webster WK, McClelland J, Feller J (2013) Hamstring tendon anterior cruciate ligament reconstruction: does gracilis tendon harvest matter? Int Orthop 37(2):207–212
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Papalia, R., Franceschi, F., Tecame, A. et al. Anterior cruciate ligament reconstruction and return to sport activity: postural control as the key to success. International Orthopaedics (SICOT) 39, 527–534 (2015). https://doi.org/10.1007/s00264-014-2513-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-014-2513-9