Abstract
Total knee modular megaprosthesis or osteochondral allograft are used to preserve joint movement in bone tumours of the proximal tibia. The aim of this study was to compare two groups of patients with total knee modular megaprosthesis and osteochondral allograft through an objective analysis. Eighteen patients, ten treated with prosthesis (TKR group) and eight with osteochondral allografts (AL group), were included in the study. X-ray, muscular strength measurements, and studies of gait analysis including electromyography (EMG) were used to compare functional results of patients. In the TKR group a higher incidence of knee extension lag was found. While the TKR group had a prevalent knee stiff/hyperextension pattern with reduced rectus femoris activity, the AL group had a higher percentage of normal knee pattern. Knee extensor muscular strength was reduced in the TKR group. TKR functional performance during gait is in most cases abnormal, consistent with the weakness of the extensor apparatus and knee extension lag. Although a greater rate of normal walking was found in the AL group, problems related to a short patellar tendon, knee instability, and joint mismatching were considered to be responsible for abnormal knee kinematics. An allograft, when optimal reconstruction is performed, gives better functional results.
Résumé
Les prothèses totales massives et les allogreffes ostéochondrales sont utilisées pour préserver le mouvement articulaire dans les tumeurs du tibia proximal. Le but de cette étude était de comparer 2 groupes de patients ayant reçus ces traitements. 18 patients étaient inclus dans l’étude, 10 traités par prothèse (groupe TKR) et 8 par allogreffe ostéochondrale (groupe AL). Les radiographies, la mesure de la force musculaire, l’étude de la boiterie incluant l’EMG étaient utilisées pour comparer les résultats fonctionnels. Dans le groupe TKR une plus grande incidence de perte d’extension était notée. Tandis que le groupe TKR avait une réduction de l’activité du Rectus fémorus , le groupe AL avait un plus grand pourcentage de fonction normale. La force musculaire des extenseurs était réduite dans le groupe TKR. La performance fonctionnelle durant la marche des TKR étaient la plupart du temps anormal avec faiblesse de l’appareil extenseur et perte d’extension. Bien qu’un taux plus élevé de marche normale était trouvé dans le groupe AL, les problèmes dû à un tendon rotulien court, une instabilité articulaire et à une articulation mal adaptée étaient supposés responsable d’une cinématique anormale du genou. L’allogreffe, quand une reconstruction optimale était réalisée donnait un meolleur résultat fonctionnel.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteochondral allograft or total knee replacement are used to preserve joint movement in patients with bone tumours of the proximal tibia. Each of these techniques has different indications and complications [3, 19, 22]. While the incidence of infection in total knee replacement is lower, functional results seem to be poor or fair due to the residual extension lag or the stiffness of the knee [2, 15, 18]. These limitations may be attributed to difficulties in the reconstruction of the extensor mechanism [3, 5, 15]. A procedure used to overcome this problem is the medial gastrocnemius transposition to the residual patellar tendon [3, 8, 14]. In the osteochondral allograft surgical procedure, a higher incidence of infection, fractures, and loss of fixation is reported [5, 12, 17, 20, 23]. Nevertheless, it has the advantage of allowing direct suture from host to allograft, minimising bone resection and preserving the articular surface of the distal femur and patella. Better final functional results were found compared with other methods [5, 7, 14].
The aim of this study was to compare patients with total knee replacement and osteochondral allograft through an objective analysis.
Materials and methods
Eighteen patients were included in the study. Inclusion criteria were: independent gait and the absence of oncological and local severe complications. Ten patients were treated with a total knee replacement using a modular replacement prosthesis (TKR) and eight with osteochondral allografts (AL) (Table 1).
The TKR group had an average age of 22.1±2.8 years and mean follow-up of 63 months. The prosthesis used was Howmedica KMFTR noncemented hinged megaprosthesis for proximal tibia replacement. At terminal extension it may allow recurvatum of about 6° providing, if needed, stability of the knee by passive hyperextension. It has 8° of valgus alignment to reproduce the correct mechanical axis on the frontal plane. The patellar tendon was attached to the prosthesis through a polyethylene plate and a metal ring to enable stitching of the patellar tendon. In seven patients a gastrocnemius transposition was associated. At the time of gait analysis all patients had a stable implant.
The AL group had an average age of 23.1±9.2 years and mean follow-up of 37 months. The patellar tendon was directly sutured from host to recipient with nonreabsorbable stitches. One patient had a subchondral fracture of the allograft at the time of gait analysis.
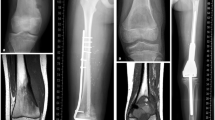
X-ray measurements consisted of the patellar tendon length in the lateral view, i.e., the distance between the inferior apex of the patella and the patellar insertion ring on the prosthesis or the allograft tibial tuberosity. Patellar tendon length difference at the time of gait analysis was expressed as a percentage of the length measured before and after surgery. The patella was considered alta for a lengthening or infera for a shortening of 10% or more in the length of the tendon [21]. Moreover, the size and position of the allograft with respect to the femoral epiphysis was measured to check joint matching. The size of the allografts was obtained by an X-ray frontal view, measuring the width of the tibial plate and femoral intercondylar distance. The anterior-posterior displacement of the allograft relative to the femur was obtained from a lateral view, measuring the distance between the longitudinal tibial axis and the anterior and posterior condylar borders.
Gait analysis was performed by means of the ELITE stereophotogrammetric system for kinematic variables and two Kistler force plates for ground reaction forces. The protocol used for kinematic and kinetic evaluation was the Calibrated Anatomical System Technique [6]. Patients performed three gait trials. Clinically relevant kinematic and kinetic parameters were selected during the gait cycle (Table 2).
The eight-channel TELEMG electromyograph was used to record the surface electromyographic signal during gait. Eight muscles were examined: homolateral and contralateral longissimus dorsi, gluteus medius, rectus femoris, gastrocnemius, tibialis anterior, and medial and lateral hamstrings. The myoelectric signals were acquired simultaneously with the kinematic and kinetic data, then processed off-line by means of a statistical detection algorithm to obtain muscle on-off timing [4], normalised to the duration of the stride. Patients were compared to ten control subjects with a mean age of 27.5±4 years [1].
Muscular strength at the knee was measured by voluntary maximal contraction isometric tests using the REV 9000 dynamometer. The test consisted of measuring the maximum extension and flexion moment with the knee joint at 90, 70, 45, and 20° of flexion (Table 3). The test was performed on both limbs (treated and healthy), and the percentage difference between the two limbs in the residual peak torque was calculated. Two patients in the allograft group did not perform the isometric test.
Knee performance was evaluated by means of a scoring system (IKS, International Knee Society) for pain, function during gait, knee range of motion, muscular strength, knee flexion deformity, and knee instability.
Statistical analysis for comparison of clinical and gait parameters of the TKR group, AL group, and control group was performed by means of one-way analysis of variance (ANOVA) (P<0.01), if the Levene test (P<0.05) for uniformity of variances was not significant. Otherwise the Kruskal-Wallis nonparametric test was used, and the Mann-Whitney test (P<0.05) was used for pairwise multiple comparison among groups. Pearson’s chi-square test by exact method was used for the frequency analysis of data (P<0.05). The SPSS statistics package was used for all statistical analysis methods.
Results
Clinical assessment
AL group
The functional mean score was 88.1, excellent in all cases but the patient with allograft fracture claimed mild pain during prolonged walking (Table 1). Active extension was complete in seven patients while one patient had an extension lag of 10°. The mean maximum knee flexion was 100±12.2°. Slight varus-valgus instability (0–5°) was present in two cases, and one of them also presented modest posterior instability. One patient had a partial detachment of the patellar tendon, not treated at the time of gait analysis. Three patients had a lower limb length difference of 2 cm, compensated for by shoes with supports.
TKR group
Functional and clinical examinations were performed at a mean follow-up of 62.8±27.5 months after surgery, significantly longer (P=0.002) than the follow-up of patients with allograft (mean: 28±13.6 months). The functional mean score was 87.1, rated good to excellent. In two patients mild occasional pain was present at the knee. Active extension was full in three patients while seven had an extension lag of 5–20° (P=0.025). The mean maximum knee flexion was 106±12.4°. Three patients had a lower limb length difference of 1 cm, not compensated for by shoes.
X-ray measurements
AL group
At the time of gait analysis three patients had patella infera as a consequence of soft tissue tight suture. In two patients an allograft oversize mismatch was observed in the frontal view (tibia/femur >1.1). The lateral view showed an anteposition of the tibial axis with respect to the femoral condyles in four patients (anterior/posterior <0.5).
TKR group
At the time of gait analysis only one patient had a patellar tendon that was shorter than before surgery (Table 1). Patella infera in the AL group was significant with the Mann-Whitney test (P=0.02).
Gait analysis
When compared to the control group, patients with TKR and AL had similar stance duration on the treated side and significantly prolonged on the contralateral side (P<0.0001). Walking speed decreased in both groups.
In both groups the biomechanics of the knee during gait was characterised by a kinematic extensor knee pattern during the stance phase (Table 2). However, while the AL group seemed to keep in contact with the ground with a slightly more extended knee, TKR patients had an increase in knee flexion at toe off and during swing (P<0.0001).
Looking at frequency of different knee patterns in each group some differences became evident. In the TKR group only one patient had a regular gait pattern; in the AL group three patients did not have any knee abnormality during the loading response phase (P=0.04).
In the TKR group, five patients had a knee hyperextension pattern (recurvatum of knee during loading response), while in the AL group there was only one hyperextension knee pattern, in the patient with patellar tendon detachment. Moreover, in the TKR group two patients had a stiff knee pattern (knee extended throughout the stance phase), and two patients a flexion pattern (continuous flexion of the knee by a few degrees throughout the stance phase).
In the AL group three patients had a stiff knee pattern and one patient an atypical pattern, characterised by marked hyperextension at heel strike followed by continuous progressive knee flexion (Fig. 1). While modest posterior instability was clinically present in the latter case, in the three patients with stiff knee, there was an associated patella infera and/or joint mismatching. The initial external flexor moment and extensor moment were reduced in both groups.
On EMG, the activity of the rectus femoris was strictly related to knee kinematics as it was reduced or absent in patients with a stiff or hyperextended knee pattern and normal or prolonged in a normal knee pattern (Fig. 2). With regards to other muscles, only the gluteus medius had a regular “on-off” phase. Instead there was a prolonged action of low back muscles (longissimi dorsii), particularly the homolateral during the stance phase and the contralateral during the swing phase, which was aimed at reducing the weight from the treated limb by the movement of the trunk.
Isometric test
A reduction of the knee extensor strength of the treated vs the contralateral limb was measured during isometric tests in both groups in all knee flexion positions (20, 45, 70, 95°). However, the reduction percentage of the extensor apparatus was significantly greater at 45 (P<0.01), 70 (P<0.005), and 95° (P<0.008) in the TKR group. No statistical significance was found for extension at 20° of knee flexion due to the large variance in the AL group (Table 3).
No significant difference in muscle strength was found between the two groups with regard to flexor muscles.
Discussion
Several papers have addressed the clinical and functional advantages and drawbacks [5, 7, 12, 23] of allograft reconstruction with respect to total knee replacement [9, 11, 13, 15, 16, 18, 24] in proximal tibia bone tumours, but only a few studies have documented the rate of functional recovery after surgery by means of gait analysis [10, 24].
Despite the small number of patients in this study, we consider our clinical results satisfactory in both groups. Mild pain was present with weight bearing only in two TKR patients and in the allograft patient with subchondral fracture. Passive range of motion was complete in extension and adequate for daily living activities in flexion in all of the patients evaluated (>100°). Extension lag was present only in one allograft patient whereas TKR patients had extension lag more frequently, as has been previously reported in the literature [9, 15, 13].
Time-distance parameters were altered without significant differences among groups. In agreement with previous findings [10], a slow and arrhythmic gait was found. Although when comparing the mean value of the two groups of patients no statistical differences were found in knee kinematics, when analysing the frequency of different gait patterns, a different distribution of knee loading acceptance phase pattern was found in the two groups. While a stiff/hyperextension pattern was prevalent in the TKR group, the AL group had a higher percentage of regular knee pattern among patients. The activity of the rectus femoris was strictly related to knee kinematics as it was reduced or absent in patients with a stiff or hyperextended knee pattern and normal or prolonged in a normal or flexed knee pattern. This is consistent also with the presence of a reduction in the knee extensor isometric strength in the TKR group, supporting the fact that knee stability is ensured in these patients only by the mechanical structure of the prosthesis.
Major problems were related to the soft tissue balancing in allografts: in three patients a shortening of the patellar tendon with respect to the preoperative length was measured at the time of gait analysis. In one patient there was posterior instability due to weakness of the capsule and soft tissues, and in another detachment of the patellar tendon. Patella infera is often responsible for restriction of knee movement and pain [21]: in the AL group the worst results with stiff knee were found in patients with a shortening of the patellar tendon. Hyperextension and atypical knee pattern were present in two patients, one with patellar tendon detachment and the other one with posterior instability of the knee. Moreover, some problems with knee motion in these patients could be related to oversizing of the allograft with respect to the femur, which could contribute to altering knee kinematics. The anterior displacement of the tibial axis does not seem to influence knee pattern gait. Finally, the patient with a small allograft fracture had normal gait. All the clinical findings discussed can explain knee abnormalities during gait in five allograft patients, while the other three allograft patients, in whom none of these problems were present, exhibited quite normal results.
The knee pattern in TKR patients was, in most cases, stiff or hyperextended during stance, consistent with the inadequacy of the extensor apparatus and the intrinsic mechanics of the implant. This pattern has been claimed to play a major role in knee prosthesis stress [15]. It is interesting to point out that also in this group the two patients with stiff knee pattern were the only two with patella infera. Two patients presented a very unusual pattern characterised by a few degrees of knee flexion throughout the stance phase. The only parameter we think could explain this pattern is the uncompensated difference in length of the lower limbs. In fact in these two patients the treated limb was slightly longer. Difference in lower limb length (always compensated) did not seem to influence gait in allograft patients.
In conclusion, TKR functional performance during gait is in most cases abnormal, consistent with the weakness of the extensor apparatus so that knee stability is only supported by the intrinsic prosthesis biomechanics. In the allograft group a greater rate of normal walking was found. The difficulty of balancing the soft tissue correctly during surgery resulting in the shortening of the patellar tendon, the presence of knee instability, and a partial patellar tendon detachment were considered to be responsible for abnormal knee kinematics in five patients. This is probably due to the tendency of surgeons to suture soft tissues tightly in an allograft in order to ensure greater stability of the joint. The presence of an oversize mismatch between femur and tibia size could play some role in knee performance anomalies during gait.
In view of the shorter follow-up for the allograft group with respect to the TKR group, the better extensor apparatus strength performance, and the higher number of patients with regular knee pattern during gait, it can be concluded that allografts have better functional results when optimal reconstruction is performed.
References
Benedetti MG, Catani F, Leardini A, Pignotti E, Giannini S (1998) Data management in gait analysis for clinical applications. Clin Biomech (Bristol, Avon) 13:204–213
Berkson E, Ponnappan R, Galvin J, Anderson K, Gitelis S (2005) Complications of modular oncology knee prostheses for sarcomas about the knee. J Knee Surg 18(4):298–304
Biau D, Faure F, Katsahian S, Jeanrot C, Tomeno B, Anract P (2006) Survival of total knee replacement with a megaprosthesis after bone tumor resection. J Bone Joint Surg Am 88(6):1285–1293
Bonato P, D’Alessio T, Knaflitz M (1998) A statistical method for the measurement of muscle activation intervals from surface myoelectric signal during gait. IEEE Trans Biomed Eng 45(3):287–299
Brien EW, Terek RM, Healy JH, Lane JM (1994) Allograft reconstruction after proximal tibial resection for bone tumors. Clin Orthop 303:116–127
Cappozzo A, Catani F, Della Croce U, Leardini A (1995) Position and orientation of bones during movement: anatomical frame definition and determination. Clin Biomech (Bristol, Avon) 10:171–178
Clohisy DR, Mankin HJ (1994) Osteoarticular allografts for reconstruction after resection of a musculoskeletal tumor in the proximal end of the tibia. J Bone Joint Surg Am 76:549–554
Eckardt JJ, Eilber FR, Rosen G, Mirra JM, Dorey FJ, Ward WG, Kabo JM (1991) Endoprosthetic replacement for stage IIB osteosarcoma. Clin Orthop 270:202–212
Grimer RJ, Carter SR, Tillman RM, Sneath RS, Walker PS (1999) Endoprosthetic replacement of the proximal tibia. J Bone Joint Surg Br 81:488–494
Harris IE, Leff AR, Gitelis S, Simon MA (1990) Function after amputation, arthrodesis, or arthroplasty for tumors about the knee. J Bone Joint Surg Am 72:1477–1485
Hillmann A, Hoffmann C, Gosheger G, Krakau H, Winkelmann W (1999) Malignant tumor of the distal part of the femur or the proximal part of the tibia: endoprosthetic replacement of rotationplasty. Functional outcome and quality-of-life measurements. J Bone Joint Surg Am 81:462–468
Hornicek FJ, Mnaymneh W, Lackman RD, Exner GU, Malinin TT (1998) Limb salvage with osteoarticular allografts after resection of proximal tibia bone tumors. Clin Orthop 352:179–186
Horowitz SM, Lane JM, Otis JC, Healey JH (1991) Prosthetic arthroplasty of the knee after resection of a sarcoma in the proximal end of the tibia. A report of sixteen cases. J Bone Joint Surg Am 73:286–292
Ilyas I, Younge D, Pant R, Moreau P (2000) Limb salvage for proximal tibial tumours using a modular prosthesis. Int Orthop 24(4):208–211
Jeon DG, Kaway A, Boland P, Healy JH (1999) Algorithm for the surgical treatment of malignant lesions of the proximal tibia. Clin Orthop 358:15–26
Kaway A, Healey JH, Boland PJ, Athanasian EA, Jeon DG (1999) A rotating-hinge knee replacement for malignant tumors of the femur and tibia. J Arthroplasty 14:187–196
Mnaymneh W, Malinin TI, Makley JT, Dick H (1985) Massive osteoarticular allografts in the reconstruction of extremities following resection of tumors not requiring chemotherapy and radiation. Clin Orthop 197:76–79
Sanjay BKS, Moreau PG (1999) Limb salvage surgery in bone tumour with modular endoprosthesis. Int Orthop 23:41–46
Sim FH, Beauchamp CP, Chao EYS (1987) Reconstruction of musculoskeletal defects about the knee for tumor. Clin Orthop Relat Res 221:188–201
Thompson RC, Garg A, Clohisy DR, Cheng EY (2000) Fractures in large segment allografts. Clin Orthop Relat Res 370:227–235
Weale AE, Murray DW, Newman JH, Ackroyd CE (1999) The length of the patellar tendon after unicompartmental and total knee replacement. J Bone Joint Surg Br 81:790–795
Wilkins RM, Camozzi AB, Gitelis SB (2005) Reconstruction options for pediatric bone tumors about the knee. J Knee Surg 18(4):305–309
Zatsepin ST, Burdygin VN (1994) Replacement of the distal femur and proximal tibia with frozen allografts. Clin Orthop 303:95–102
Zohman GL, Boardman DL, Eckardt JJ, Lane JM (1997) Stride analysis after proximal tibial replacement. Clin Orthop 339:180–184
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Colangeli, M., Donati, D., Benedetti, M.G. et al. Total knee replacement versus osteochondral allograft in proximal tibia bone tumours. International Orthopaedics (SICO 31, 823–829 (2007). https://doi.org/10.1007/s00264-006-0256-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-006-0256-y






 Normal/prolonged (3 TKR, 4 AL),
Normal/prolonged (3 TKR, 4 AL),  reduced (5 TKR, 2 AL),
reduced (5 TKR, 2 AL),  absent (2 TKR, 2 L),
absent (2 TKR, 2 L),  control
control