Abstract
Her-2/neu is a tumor-associated antigen that has been targeted with both antibodies and cytotoxic T lymphocytes (CTL). Despite the isolation of Her-2/neu-reactive CTL in vaccinated patients, their therapeutic use has been limited by the observation that they often do not robustly recognize Her-2/neu+ tumors. We sought to determine the mechanism for this escape using Ag201P and Ag201M cells, which are murine osteosarcoma tumor lines that express a functional HLA-A2/Kb molecule. We now demonstrate that Ag201P and Ag201M express low levels of murine Her-2/neu, and that Ag201M was modestly and inconsistently recognized by an HLA-A2-restricted, Her-2/neu-reactive human CTL clone. In order to determine whether inefficient antigen processing might account for the weak recognition, COS-A2 cells were transfected with a short Her-2/neu minigene coding for the immunodominant Her-2/neu:369 epitope that did not require antigen processing or a long Her-2/neu minigene that did require antigen processing. Her-2/neu-reactive CTL clones only recognized COS-A2 cells transfected with the short minigene, indicating that lack of proper antigen processing could be responsible for the poor recognition of target cells. To confirm these results, it was demonstrated that following treatment with interferon-γ, both Ag201P and Ag201M robustly and consistently stimulated the CTL clones. Furthermore, CTL clone recognition was enhanced following interferon-γ treatment using another murine tumor line that expressed low levels of Her-2/neu (B16-A2/Kb). The enhanced recognition of Ag201P and Ag201M in the presence of interferon-γ was not due to an upregulation of Her-2/neu protein expression. Collectively, these results suggest that inefficient antigen processing of Her-2/neu can contribute to the lack of tumor recognition by CTL. These results also suggest that even tissues that express low levels of Her-2/neu might become CTL targets under conditions in which antigen processing is enhanced.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Her-2/neu is a 185-kDa transmembrane receptor protein that is part of the epidermal growth factor (EGF) family of receptors. Although there is no known ligand identified for Her-2/neu, it serves as the preferred binding partner for the other members of the EGF receptor family [1]. It has been described as a tumor-associated antigen that is frequently overexpressed in various types of cancers, including breast, ovarian, gastric and renal cell carcinomas [2–6]. The mechanism of action for this overexpression of Her-2/neu in human carcinomas has often been attributed to gene amplification, although other mechanisms also exist (reviewed in [1]).
Expression of Her-2/neu in breast tumors correlates with poor prognosis [7, 8], therefore, a need to develop new therapeutic strategies that target Her-2-positive tumors exists. Clinically, this has been achieved primarily through the use of trastuzumab (Herceptin), a humanized murine monoclonal antibody directed against the extracellular domain of Her-2/neu [9]. For patients with Her-2/neu+ breast cancer, the use of trastuzumab, often in combination with traditional chemotherapeutic drugs, resulted in longer time to disease progression, higher rate of objective response, longer survival and reduction in death risk (reviewed in [10]).
In addition to antibody responses to Her-2/neu, CTL directed against Her-2/neu have been isolated both from vaccinated patients and from preexisting effectors in untreated patients [11–14]. CTL specific for Her-2/neu epitopes often fail to recognize Her-2/neu-expressing tumors [15] and Her-2/neu has been described to downregulate antigen processing [16–18]. Therefore, levels of Her-2/neu expression on tumor targets and sensitivity to CTL may not always correlate. To investigate this further, a CTL clone specific for the immunodominant Her-2/neu:369-377 epitope [12] was tested against human and murine Her-2/neu-expressing tumor targets, focusing on our recently described novel murine osteosarcoma cell lines, Ag201P and Ag201M. We demonstrate that there was no correlation between Her-2/neu expression levels and recognition by this CTL clone. We hypothesize that the reason for this lack of correlation was the result of inefficient processing of Her-2/neu and demonstrate that under conditions where antigen processing was enhanced, or unnecessary, CTL recognition was enhanced as well. These studies suggest that tissues in which Her-2/neu is expressed at low levels might become CTL targets, assuming efficient antigen processing is occurring.
Materials and methods
Cell lines
Ag201P and Ag201M are murine osteosarcoma cell lines that are HLA-A2/Kb -positive [19]. Both cell lines were maintained in DMEM medium (Mediatech, Herndon, VA, USA) supplemented with 20% fetal bovine serum (Invitrogen, Carlsbad, CA, USA), 100 U/ml penicillin (Invitrogen), 100 μg/ml streptomycin (Invitrogen), 2 mM L-glutamine (Invitrogen), 0.1 mM non-essential amino acids (Invitrogen), and 1 mM sodium pyruvate (Invitrogen). B16, B16-A2/Kb, and COS-A2 cells were maintained in DMEM medium supplemented with 10% fetal bovine serum, 100 U/ml penicillin, 100 μg/ml streptomycin, and 2 mM L-glutamine. T2, C1RA2, and C1RA2-Her-2 cells were maintained in RPMI medium (Mediatech, Herndon, VA, USA) supplemented with 10% fetal bovine serum, 100 U/ml penicillin, 100 μg/ml streptomycin, and 2 mM L-glutamine. C1RA2 and C1RA2-Her-2 cells are human MHC class I-defective lymphoblastoid cell lines that overexpress HLA-A2.1 and HLA-A2.1, and Her-2, respectively [20]. Her-2/neu-reactive human CTL, which recognize the HLA-A2-restricted Her-2/neu:369-377 peptide, KIFGSLAFL, were raised from a healthy donor by stimulation of the non-adherent fraction of PBMC with irradiated peptide pulsed autologous dendritic cells and the adherent fraction of PBMC. Her-2 CTL clones were maintained in RPMI medium supplemented with 10% pooled human AB serum (Valley Biomedical Inc., Winchester, VA, USA), 100 U/ml penicillin, 100 μg/ml streptomycin, 2 mM L-glutamine, and recombinant human IL-2 (Chiron, Emeryville, CA, USA; 50 CU/ml).
Immunofluorescence analysis
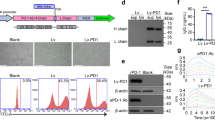
COS-A2 cells were plated at 2.5×105 cells in 6-well plates overnight followed by a 48 h incubation in the presence or absence of recombinant human interferon-γ (100 U/ml; Biosource, Camarillo, CA, USA). 5×105 cells were washed with buffer (Hanks’ balanced salt solution containing 5% FBS and 0.05% sodium azide). Cells were then analyzed for green-fluorescent protein 24 h after transfection in order to confirm the presence of a Her-2 minigene-GFP fusion protein. Following two washes in buffer, the cells were resuspended in 0.5 ml buffer for immunofluorescence analysis using a FACScan (Becton Dickinson, Franklin Lakes, NJ, USA). Each histogram represents the log fluorescence of 104 cells.
Reverse transcriptase polymerase chain reaction
Total RNA was extracted from 1×106 Ag201P or Ag201M cells using 1 ml Trizol reagent (Sigma, St. Louis, MO, USA). Samples were treated with RNase-free DNase (Invitrogen) to prevent genomic DNA contamination during PCR amplification. First strand cDNA was prepared from 1 μg of total cellular RNA using first strand cDNA synthesis Kits with oligo dT as the primer (Invitrogen). All PCR reactions were carried out in a 50 μl total volume containing 1x PCR buffer, 1.5 μM MgCl2, 200 μM dNTP, 400 nM each of forward and reverse primers (Invitrogen and IDT, Coralville, IA, USA), and 1 U of Taq Polymerase (CLP, San Diego, CA, USA) in a Peltier Thermal Cycler (MJ Research, Waltham, MA, USA). Reaction conditions were as follows: after an initial 92°C incubation for 2 min, reactions were amplified for 35 cycles at 92°C for 30 s, 58°C for 30 s, and 72°C for 60 s. The reactions were then incubated at 72° for 8 min. PCR amplification products were separated on a 1% agarose gel and visualized by ethidium bromide staining. The primers used to amplify the murine Her-2/neu gene were based on the work of Nagata et al. [21] and are as follows: mHer-2 forward, 5′-GGTCTGGGCATGGAGCA; mHer-2 reverse, 5′-GTTCCCACTGTGGAGTA.
Real time PCR
Total RNA was extracted and cDNA was prepared from 5 μg RNA as described above. All real time PCR reactions were carried out in a 25 μl total volume using Platinum qPCR Supermix-UDG (Invitrogen). Reactions were analyzed using a Perkin-Elmer 5700 thermocycler and the reaction conditions were as follows: after an initial 50°C incubation for 2 min, followed by a 95°C incubation for 10 min, reactions were amplified for 50 cycles at 95°C for 15 s, and 58°C for 1 min. PCR amplification products were analyzed using TET-BHQ probes and primer pairs. The primers and probe sequences for murine Her-2/neu were as follows: Taqman mHer-2/neu forward, 5′-TTCACCGCAACACCCATCT; Taqman mHer-2/neu reverse, 5′-GGTGCGGGTTCCGGAA; Taqman mHer-2/neu probe, 5′-TGCTTTGTAAACACTGTACCTTGGGACCAGC. The primers and probes for murine β-actin were purchased from Biosource (Camarillo, CA, USA). Standard curves were generated using plasmid DNA. Briefly, 300–400 bp fragments of both murine Her-2/neu and murine β-actin were amplified from murine cDNA. The murine Her-2/neu PCR fragment was inserted in TOPO TA (Invitrogen) according to the manufacturer’s instructions. The murine β-actin PCR fragment was amplified using primers that contained an XhoI restriction site and the XhoI-β-actin fragment was ligated into the plasmid that already contained the murine Her-2/neu fragment. Therefore, standard curves were generated for both genes from one plasmid. Plasmid DNA was isolated using a QIAprep Spin Miniprep Kit (Qiagen, Valencia, CA, USA). The DNA was quantified using a spectrophotometer and converted to concentration (nanomolar).
Western blotting
Whole cell protein lysates were prepared from 1×106 C1RA2, C1RA2-Her-2, B16, B16-A2/Kb, Ag201P or Ag201M cells. For studies in which murine interferon-γ was utilized, cells were treated for 48 h with 100 U/ml recombinant mouse interferon-γ (Biosource). Cells were lysed in buffer (phosphate-buffered saline containing 1% Igepal CA-630, 0.5% sodium deoxycholate and 0.1% sodium dodecyl sulfate, and 1:100 dilution of protease inhibitor cocktail; Sigma), incubated on ice for 30 min and centrifuged at 10,000 g for 20 min, after which the supernatant containing the protein was retained. Total protein was quantified with the BCA Protein Assay (Sigma). For electrophoresis, protein was prepared in the buffer described above, incubated with Tris–glycine SDS Sample Buffer (Invitrogen) and Sample Reducing Agent (Invitrogen), and heated at 85°C for 5 min. The samples were then resolved on a 4–12% Tris–glycine Gel (Invitrogen), transferred to nitrocellulose and incubated with primary antibody. The primary antibodies used were anti-c-ErbB2/c-Neu Ab-3 (Oncogene Research Products, San Diego, CA, USA), anti-actin Ab-1 (Oncogene Research Products), or anti-proteasome 20S LMP-2 (Affinity Bioreagents, Golden, CO, USA). Antibody binding was detected by staining the blots with a goat anti-mouse horseradish peroxidase conjugate (Novagen, San Diego, CA, USA), peroxidase goat anti-mouse IgM (Oncogene Research Products) or goat anti-rabbit IgG horseradish peroxidase (Cayman Chemical, Ann Arbor, MI, USA), respectively. Blots were then exposed to enhanced chemiluminescence (ECL) Western blotting detection reagents (Amersham, Piscataway, NJ, USA).
Transient transfections
Her-2/neu minigenes were prepared by PCR. The short Her-2/neu minigene encodes the Her-2/neu:369 peptide (KIFGSLAFL) and therefore, does not require processing. The long Her-2/neu minigene encodes a longer peptide fragment (EFAGCKKIFGSLAFLPESFDG) from which the Her-2/neu:369 peptide must be processed and presented. Both peptides encode fragments of Her-2/neu that are shared between mouse and human [21]. The short-minigene was ligated into pCDNAIII and the long-minigene was ligated into CT-GFP Fusion TOPO TA (Invitrogen). COS-A2 cells were plated at subconfluent densities one day prior to transfection. Transfections were performed utilizing Lipofectamine 2000 (Invitrogen) according to manufacturer’s instructions. Twenty-four hours after transfection, cells were harvested, washed and enumerated for either immunofluorescence analysis or cytokine release assays.
Cytokine release assays
B16, B16-A2/Kb, Ag201P, and Ag201M cells were plated at 2×105 cells in 100×20 mm tissue culture dishes. The following day, cells were either untreated or treated with 100 U/ml recombinant murine interferon-γ (Biosource) for 48 h. Subsequently, cells were harvested, washed, enumerated, and the cell densities adjusted to 2.5×105 cells/ml. 100-μl aliquots were distributed to wells of a 96-well round-bottom plate, resulting in 2.5×104 cells/well. Alternatively, transfected COS-A2 cells were distributed to 96-well round-bottom plates at 2×104 cells/well. Human CTL were harvested, washed, enumerated and distributed to the 96-well plates as above, resulting in a responder to stimulator ratio of 1:1. As a positive control, peptide-pulsed T2 cells were used as stimulators. T2 cells (1×106 cells) were loaded with 5 μg/ml Her-2/neu:369–377 or irrelevant peptide for 2 h at 37°C. Cells were then harvested, washed, and the cell density was adjusted to yield the number of cells required for a responder to stimulator ratio of 1:1. Cultures were incubated for 18–24 h at 37°C after which the supernatants were collected and human interferon-γ was measured by ELISA. Statistical analyses were performed within each tumor cell group.
Statistical analysis
The mean ± SD was determined for each treatment group in the individual experiments. For the cytokine release assays, homogenous data were evaluated by parametric analysis of variance and the Student–Neuman–Keull’s test to compare treatment groups when significant differences were observed.
Results
Ag201P and Ag201M express murine Her-2/neu
Ag201P and Ag201M are novel murine osteosarcoma tumor lines that express a functional HLA-A2/Kb molecule [19]. Putative tumor-associated antigens in osteosarcomas include, but are not limited to, Her-2/neu, SART, and p53 [22–33]. However, there are conflicting reports as to whether Her-2/neu is overexpressed in osteosarcomas and associated lung metastases [22–24]. Since Ag201P and Ag201M represent a primary and metastatic osteosarcoma, respectively [19], Her-2/neu expression in these lines was characterized. As seen in Fig. 1, murine Her-2 was found in Ag201P and Ag201M as assessed by reverse transcriptase PCR. Expression of murine Her-2/neu was confirmed using quantitative real-time PCR and it was demonstrated that the expression level of murine Her-2/neu mRNA was extremely low (more than 1,000-fold lower than murine β-actin). Specifically, the ratio of expression of murine Her-2/neu to murine β-actin was 2.8×10−3 for Ag201P and 3.6×10−4 for Ag201M (calculated as micromolar cDNA based on standard curves for Her-2/neu and β-actin). Nevertheless, the primers amplified a 465 bp fragment, which contained the BglII restriction element, confirming the presence of murine Her-2/neu [21]. Since it has been shown previously that murine and human Her-2/neu share 85% nucleotide sequence identity, which includes the 369-377 peptide KIFGSLAFL [21], we determined whether Ag201P and Ag201M could be recognized by an HLA-A2-restricted, Her-2/neu-reactive human CTL clone (Table 1). The specificity for the Her-2/neu:369-377 epitope and the cytotoxic activity of this CTL clone was confirmed by HLA-A2 tetramer staining and 51Cr-release assays (unpublished observation). In three separate experiments, there was low and inconsistent production of interferon-γ in response to Ag201M. In only one experiment did Ag201P stimulate the CTL clone. As a comparative control, C1RA2-Her-2 cells, which overexpress HLA-A2 and the human form of Her-2/neu ([20] and Fig. 5), also stimulated the CTL clone in a similar manner as Ag201M. This low interferon-γ production was not due to defective T cell function as T2 cells loaded with Her-2/neu:369-377 peptide robustly stimulated the CTL clone (Table 1). Collectively, these results demonstrate that Ag201P and Ag201M express murine Her-2/neu, and that these murine tumors were weakly recognized by a human Her-2/neu-reactive CTL clone.
Murine Her-2/neu mRNA was expressed at low levels in Ag201P and Ag201M cells. Total RNA was isolated and cDNA was synthesized as described in Materials and methods. Primers amplified a 445 bp fragment that was sensitive to digestion by BglII. Following PCR amplification of cDNA, a 10-μl aliquot of PCR product was incubated with BglII for 1 h at 37°C, confirming the presence of murine Her-2/neu. Bands were separated on a 1% agarose gel and visualized by ethidium bromide staining
Recognition of cells expressing Her-2/neu:369 minigenes
In order to determine whether inefficient antigen processing of Her-2/neu might account for the weak recognition of Ag201P and Ag201M by the Her-2/neu-reactive CTL clone, two different Her-2/neu minigenes were constructed that encode the Her-2/neu 9-mer peptide fragment KIFGSLAFL (369–377). The short Her-2/neu:369 minigene encodes only the nine-mer peptide and therefore does not require processing. The long Her-2/neu:369 minigene encodes a peptide fragment that includes the nine-mer peptide flanked on either side by the six adjacent native amino acids (which are shared between human and mouse), and therefore requires processing prior to the presentation by MHC class I. Furthermore, the long Her-2/neu:369 minigene was fused to the N-terminal end of green fluorescent protein (GFP) so that expression of GFP confirms expression of the minigene. As seen in Fig. 2, COS-A2 cells transiently transfected with the short Her-2/neu:369 minigene were recognized by the Her-2 CTL clone, whereas the long Her-2/neu:369 minigene was not recognized despite modest GFP expression. These results provide evidence that inefficient processing of the Her-2/neu tumor antigen might contribute to the lack of recognition by CTL.
CTL recognized COS-A2 transfected with a Her-2/neu minigene that did not require antigen processing. a Subconfluent COS-A2 cells were transfected with either a short- or long-Her-2/neu minigene. Twenty-four hours following transfection, cells were harvested, enumerated, and cultured in a 1:1 ratio with human HLA-A2-restricted, Her-2/neu-reactive CTL overnight at 37°C (2×105 cells per cell type). Interferon-γ production was measured by ELISA. CTL produced <26 pg/ml interferon-γ in response to T2 cells loaded with irrelevant peptide (CMV pp65:495–503) and 2,492±58 pg/ml interferon-γ in response to T2 cells loaded with 5 μg/ml exogenous Her-2/neu peptide. *P<0.001 versus COS-A2 alone. Results are representative of three independent experiments. b COS-A2 cells were transfected with a long Her-2/neu minigene fused with green fluorescent protein. Transfected and untransfected COS-A2 cells were analyzed by immunofluorescence analysis for green-fluorescent protein 24 h after transfection. Each histogram represents the log fluorescence of 104 cells
Weak recognition of Ag201P and Ag201M was enhanced by murine interferon-γ
Since the stimulation of the CTL clone by Ag201M was modest and might be due to inefficient antigen processing of Her-2/neu, Ag201P and Ag201M were pretreated with interferon-γ to enhance expression of various components of the antigen processing machinery [34–37]. As shown in Fig. 3, treatment of Ag201P and Ag201M for 48 h with murine interferon-γ robustly enhanced tumor recognition by the CTL clone. Interestingly, Ag201P, which previously did not significantly stimulate the CTL clone in the absence of murine interferon-γ, now robustly and consistently stimulated the CTL clone to produce human interferon-γ. The ability of the tumors to stimulate CTL was specific for the Her-2/neu reactive clone as murine interferon-γ treated Ag201P and Ag201M cells were not recognized by HLA-A2-restricted, irrelevant CTL (data not shown). Furthermore, interferon-γ treated Ag201P and Ag201M were not universally recognized by Her-2/neu:369-377 specific CTL clones, as only two of the four tested clones recognized murine interferon-γ treated Ag201P and Ag201M (unpublished observation). These two clones that recognized the interferon-γ treated Ag201P and Ag201M possessed high avidity and were determined to be sister clones based on sequence analysis of their T cell receptor α and β CDR3 regions (unpublished observation). Collectively, these results demonstrate that in the presence of murine interferon-γ, both Ag201P and Ag201M stimulated a CTL clone in a Her-2/neu-specific manner and that even in this setting CTL clones must possess sufficient avidity for tumor recognition.
Interferon-γ enhanced the ability of CTL to recognize Ag201P and Ag201M cells. C1RA2, C1RA2-Her-2, Ag201P, and Ag201M were untreated or treated with 100 U of human (C1RA2 and C1RA2-Her-2) or murine (Ag201P and Ag201M) interferon-γ for 48 h. Cells were then harvested, washed, enumerated and cultured in a 1:1 ratio with human HLA-A2-restricted, Her-2/neu-reactive CTL overnight at 37°C (2.5×105 cells per cell type). Interferon-γ production was measured by ELISA. CTL produced <26 pg/ml interferon-γ in response to T2 cells loaded with irrelevant peptide (MART-1:27-35) and 14,518±2470 pg/ml interferon-γ in response to T2 cells loaded with 5 μg/ml exogenous Her-2/neu peptide. *P<0.001 versus Ag201P alone; **P<0.01 versus Ag201M alone. Results are representative of three independent experiments
Recognition of B16-A2/Kb by CTL clones was enhanced by murine interferon-γ treatment
Human melanoma lines have been shown to express significant levels of Her-2/neu and to be lysed by HLA-A2-restricted Her-2/neu specific CTL [38]. Therefore, the murine melanoma lines B16 and the transfectant B16-A2/Kb were also utilized. Very low but significant protein expression of murine Her-2/neu in B16 and B16-A2/Kb was detected (Fig. 4a). Despite the low protein expression levels of murine Her-2/neu in B16 and B16-A2/Kb, B16-A2/Kb cells were also targets for the CTL clone following murine interferon-γ treatment, but were not recognized when untreated (Fig. 4b). Interestingly, the amount of human interferon-γ produced in response to murine interferon-γ treated B16-A2/Kb was higher than that of either Ag201P or Ag201M under similar experimental conditions. The specificity for B16-A2/Kb as compared to B16 demonstrated the requirement for HLA-A2/Kb in this interaction. Again, this response was specific for Her-2/neu as murine interferon-γ treated B16 and B16-A2/Kb were unable to stimulate HLA-A2-restricted, irrelevant CTL (data not shown). These results suggest that murine tumor lines that express low levels of murine Her-2/neu might also be CTL clone targets following interferon-γ treatment.
Interferon-γ enhanced the ability of CTL to recognize B16-A2/Kb cells. a Whole-cell protein was prepared from B16 and B16-A2/Kb cells as described in Materials and methods. Her-2/neu and β-actin expression were analyzed by Western blot analysis. Results are representative of three independent experiments. b B16, B16-A2/Kb, Ag201P and Ag201M cells were untreated or treated with 100 U of murine interferon-γ for 48 h. Cells were then harvested, washed, enumerated and cultured in a 1:1 ratio with human HLA-A2-restricted, Her-2/neu-reactive CTL overnight at 37°C (2×105 cells per cell type). Interferon-γ production was measured by ELISA. CTL produced <26 pg/ml interferon-γ in response to T2 cells loaded with irrelevant peptide (gp100:209-217) and 18,917±1949 pg/ml interferon-γ in response to T2 cells loaded with 5 μg/ml exogenous Her-2/neu peptide. ‡P<0.001 versus B16-A2/Kb alone; *P<0.001 versus Ag201P alone; **P<0.01 versus Ag201M alone. Results are representative of four independent experiments
Effect of murine interferon-γ on Her-2/neu expression
The enhanced human interferon-γ production by a CTL clone in response to Ag201P and Ag201M treated with murine interferon-γ could be due, in part, to upregulation of MHC class I antigen presentation. Indeed, cell surface expression of HLA-A2/Kb, H-2Kb, and H-2Db were all (at least modestly) enhanced following incubation with murine interferon-γ in Ag201P and Ag201M cells [19]. However, it was also determined whether murine interferon-γ treatment influenced the expression of murine Her-2/neu in Ag201P and Ag201M cells. Using Western blot analysis, it was demonstrated that the protein levels of Her-2/neu in Ag201P and Ag201M were extremely low, which was consistent with the low level of expression of murine Her-2/neu mRNA. Furthermore, Her-2/neu expression was not enhanced by murine interferon-γ treatment, and even appeared to be modestly inhibited (Fig. 5). The modest effect of murine interferon-γ was not due to the lack of activity as murine interferon-γ treatment enhanced expression of LMP-2, one component of the antigen processing machinery that is well-known to be interferon-γ-responsive (reviewed in [39]). Interestingly, C1RA2-Her-2 cells that express high levels of Her-2/neu were only poorly recognized by the CTL clone even after treatment with human interferon-γ (compare Figs. 3, 5).
The effect of interferon-γ on murine Her-2/neu expression in Ag201P and Ag201M cells. Ag201P and Ag201M were untreated or treated with 100 U of murine interferon-γ for 48 h. Whole-cell protein was prepared from C1RA2, C1RA2–Her-2, Ag201P and Ag201M (cultured in the presence and absence of interferon-γ, respectively) cells as described in Materials and methods. Her-2/neu, β-actin and LMP-2 expression were analyzed by Western blot analysis. Results are representative of three independent experiments
Discussion
We have previously described Ag201P and Ag201M, which are two novel osteosarcoma murine cell lines that express a functional HLA-A2/Kb molecule [19]. The studies herein provide further characterization of these tumor lines, including the fact that they both expressed low levels of murine Her-2/neu. This suggested that Her-2/neu might be a putative tumor antigen for Ag201P and Ag201M, and indeed, Ag201M stimulated a human HLA-A2-restricted, Her-2/neu-reactive CTL clone to produce modest amounts of human interferon-γ.
The production of human interferon-γ by the CTL clone in response to Ag201M, however, was low and inconsistent over several replicates of the experiment. In addition, Ag201P, which also expressed low levels of murine Her-2/neu, was essentially unable to stimulate the CTL clone. With the demonstration that the CTL were high-avidity clones as assessed by their ability to recognize T2 cells loaded with Her-2/neu:369-377 peptide (Table 1, Figs. 2a, 3, 4b and unpublished observation), these results initially suggested that the lack of CTL clone reactivity was the result of either low cross-species Her-2/neu identity, or low-level Her-2/neu expression. However, as previously stated, murine and human Her-2/neu share 85% nucleotide sequence identity, including the 369-377 peptide [21]. Furthermore, C1RA2–Her-2 cells, which overexpress human Her-2/neu, were also unable to robustly stimulate the CTL clone. We therefore hypothesized that the lack of CTL stimulation by Her-2/neu-expressing tumors was the result of inefficient antigen processing of the Her-2/neu molecule. There were several lines of evidence to support this hypothesis. First, pretreatment of Ag201P and Ag201M with murine interferon-γ resulted in robust and consistent CTL clone stimulation. These results correlated with the observation that interferon-γ pretreatment enhanced cell surface expression of HLA-A2/Kb, H-2Kb, and H-2Db [19], and as shown here, the immunoproteasome subunit LMP-2. In contrast, interferon-γ treatment did not enhance the weak CTL recognition observed against C1RA2–Her-2, although this could be due to the fact that C1RA2 and C1RA2–Her-2 cells are MHC class I-defective, which would be consistent with our observations that lack of recognition might be due to inefficient antigen processing [20]. Second, another distinct murine tumor line, B16-A2/Kb, which also possessed very low Her-2/neu expression, stimulated the CTL clone following murine interferon-γ treatment. Third, COS-A2 cells that had been transfected with either a short or long Her-2/neu:369 minigene stimulated the Her-2/neu CTL clone only under conditions in which antigen processing was not required. Although the extent to which the Her-2/neu:369-377 epitope from the GFP fusion was processed and presented was not assessed in the transfected cells, these studies demonstrate that overexpression of the antigenic epitope alone provided CTL recognition, whereas the necessity of antigen processing and presentation of the antigenic epitope from a protein prevented CTL recognition.
Several studies in experimental mouse models and human T cells have demonstrated that CTL recognize Her-2/neu+ tumors in vitro and in vivo [12, 14, 40–44]. Complicating this picture, however, and in line with our findings here, is evidence that antigen processing and MHC class I expression in Her-2/neu tumor transfectants, mammary carcinomas from Her-2/neu transgenic mice, and human Her-2/neu+ carcinomas, are impaired [17, 18, 45], potentially providing a mechanism by which Her-2/neu+ tumors escape CTL recognition. These studies are also consistent with the findings that CTL lysis of SKOV3.A2 cells was enhanced in the presence of geldanamycin, an antibiotic that specifically targets Her-2/neu degradation [46–48]. One interpretation of these results is that enhancement of Her-2/neu degradation provides more opportunities for antigenic epitopes to be presented on the surface of tumor cells. Also, it has been demonstrated that CTL raised against the Her-2/neu:369 epitope failed to recognize HLA-A2+, Her-2/neu+ tumors, despite the ability of CTL to recognize exogenously loaded peptide [11]. Collectively, these studies support the hypothesis that CTL recognition of certain Her-2/neu+ tumors is impaired due to suboptimal antigen processing and could therefore be enhanced under conditions that promote more efficient processing and presentation of Her-2/neu.
It was unlikely that the enhanced recognition of Ag201P and Ag201M by the CTL clone was due to interferon-γ-mediated enhancement of Her-2/neu expression in these cells. There was no evidence by Western blot analysis that murine Her-2/neu expression was enhanced by murine interferon-γ treatment. These results were consistent with similar studies conducted in cell lines and Her-2/neu transgenic mice demonstrating that interferon-γ treatment has little effect on Her-2/neu expression, and if anything, slightly inhibits it [18, 45, 49–51]. In fact, several studies have demonstrated a reciprocal relationship between expression of components of the antigen processing machinery and expression of Her-2/neu [17, 18, 45, 46]. Therefore, following interferon-γ treatment, which upregulated MHC class I molecules [19] and LMP-2 in both Ag201P and Ag201M, one might expect a slight inhibition of Her-2/neu expression. Although the mechanism for this inhibition is not fully understood, the enhanced expression of components of the antigen processing machinery might lead to increased Her-2/neu degradation.
Upon careful examination of Her-2/neu protein expression, it was also interesting to note that the molecular weight of murine Her-2/neu was slightly lower than that of human Her-2/neu. It was unlikely due simply to differences between human and mouse protein identity since they are 87% identical at the amino acid level and estimates of the respective molecular weights are similar [21]. However, there have been reports of slightly different molecular weights for Her-2/neu, depending on phosphorylation state, glycosylation state and expression of a precursor form (170 kDa) versus a mature form (175–185 kDa) of the Her-2/neu protein [52, 53]. These various forms regulate both the amount of tyrosine kinase activity Her-2/neu exhibits and the interaction potential of Her-2/neu with other intracellular signaling proteins [52]. Although speculative, it is tempting to hypothesize that whatever the cause for the molecular weight difference between Her-2/neu in C1RA2–Her-2 versus Ag201P and Ag201M might account for the ability (or lack thereof) of CTL to recognize the tumor. Assuming the higher molecular weight form of Her-2/neu seen in C1RA2–Her-2 was due to enhanced phosphorylation, the low capacity of C1RA2–Her-2 to stimulate CTL was unlikely due to changes in tyrosine phosphorylation because a correlation was established between the ability of tumor cells to stimulate Her-2/neu-reactive CTL and increased tyrosine phosphorylation state of Her-2/neu [54]. However, this does not exclude the possibility that the enhanced phosphorylation was due to serine and threonine residues and perhaps these phosphorylation events mask ubiquitin binding sites rendering Her-2/neu resistant to degradation and subsequently, antigen processing and presentation. Alternatively, enhanced phosphorylation of Her-2/neu promotes the interaction of other intracellular proteins such as SHC, PLC-γ and PI3 kinase (reviewed in [55]), which also might have prevented degradation through steric hindrance of ubiquitin enzymes. Finally, it is possible that one difference between the precursor and mature forms of Her-2/neu is its susceptibility to degradation. Perhaps the higher molecular weight form seen in C1RA2-Her-2 cells represents a Her-2 molecule that is resistant to degradation. None of these possibilities can be ruled out at this time.
Collectively, these results suggest that the strength of Her-2/neu as a tumor antigen depends partially on its ability to be processed and presented on the surface of tumor cells. Several lines of evidence, including the data presented here, suggest that degradation and/or processing and presentation of Her-2/neu is often inefficient. The corollary to this is that even tissues (tumor or normal) that do not express high levels of Her-2/neu might become CTL targets under conditions in which antigen processing and presentation are enhanced. Based on these studies, Her-2/neu should be more widely described as a target for tumors even when it is not overexpressed (such as osteosarcoma and melanoma as shown here). Furthermore, expression levels of Her-2/neu on tumors should not be a deciding factor for potential therapeutic use of Her-2/neu-reactive CTL; one should also consider the expression levels and/or activity of various components of the antigen processing machinery prior to CTL therapy. Finally, these results suggest that there is potential for autoimmunity to develop in normal tissues that express low levels of Her-2/neu and possess sufficient antigen processing activity. Overall, these data suggest that there is no correlation between Her-2/neu expression level and tumor recognition by CTL, and that caution should be exercised when Her-2/neu-reactive CTL therapy is administered to patients with normal antigen processing activity.
Abbreviations
- HLA:
-
Human leukocyte antigen
- MHC:
-
Major histocompatibility complex
- IFN:
-
Interferon
- CTL:
-
cytotoxic T lymphocytes
References
Holbro T, Civenni G, Hynes NE (2003) The ErbB receptors and their role in cancer progression. Exp Cell Res 284:99–110
Hellstrom I, Goodman G, Pullman J, Yang Y, Hellstrom KE (2001) Overexpression of HER-2 in ovarian carcinomas. Cancer Res 61:2420–2423
Liu E, Thor A, He M, Barcos M, Ljung BM, Benz C (1992) The HER2 (c-erbB-2) oncogene is frequently amplified in in situ carcinomas of the breast. Oncogene 7:1027–1032
Press MF, Jones LA, Godolphin W, Edwards CL, Slamon DJ (1990) HER-2/neu oncogene amplification and expression in breast and ovarian cancers. Prog Clin Biol Res 209–221
Seliger B, Rongcun Y, Atkins D, Hammers S, Huber C, Storkel S, Kiessling R (2000) HER-2/neu is expressed in human renal cell carcinoma at heterogeneous levels independently of tumor grading and staging and can be recognized by HLA-A2.1-restricted cytotoxic T lymphocytes. Int J Cancer 87:349–359
Tsugawa K, Fushida S, Yonemura Y (1993) Amplification of the c-erbB-2 gene in gastric carcinoma:correlation with survival. Oncology 50:418–425
Seshadri R, Firgaira FA, Horsfall DJ, McCaul K, Setlur V, Kitchen P (1993) Clinical significance of HER-2/neu oncogene amplification in primary breast cancer. The South Australian Breast Cancer Study Group. J Clin Oncol 11:1936–1942
Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A, McGuire WL (1987) Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 235:177–182
Carter P, Presta L, Gorman CM, Ridgway JB, Henner D, Wong WL, Rowland AM, Kotts C, Carver ME, Shepard HM (1992) Humanization of an anti-p185HER2 antibody for human cancer therapy. Proc Natl Acad Sci USA 89:4285–4289
Ross JS, Fletcher JA, Linette GP, Stec J, Clark E, Ayers M, Symmans WF, Pusztai L, Bloom KJ (2003) The Her-2/neu gene and protein in breast cancer 2003: biomarker and target of therapy. Oncologist 8:307–325
Zaks TZ, Rosenberg SA (1998) Immunization with a peptide epitope (p369-377) from HER-2/neu leads to peptide-specific cytotoxic T lymphocytes that fail to recognize HER-2/neu+ tumors. Cancer Res 58:4902–4908
Fisk B, Blevins TL, Wharton JT, Ioannides CG (1995) Identification of an immunodominant peptide of HER-2/neu protooncogene recognized by ovarian tumor-specific cytotoxic T lymphocyte lines. J Exp Med 181:2109–2117
Disis ML, Smith JW, Murphy AE, Chen W, Cheever MA (1994) In vitro generation of human cytolytic T-cells specific for peptides derived from the HER-2/neu protooncogene protein. Cancer Res 54:1071–1076
Sotiropoulou PA, Perez SA, Voelter V, Echner H, Missitzis I, Tsavaris NB, Papamichail M, Baxevanis CN (2003) Natural CD8+ T-cell responses against MHC class I epitopes of the HER-2/neu oncoprotein in patients with epithelial tumors. Cancer Immunol Immunother 52:771–779
Kono K, Halapi E, Hising C, Petersson M, Gerdin E, Vanky F, Kiessling R (1997) Mechanisms of escape from CD8+ T-cell clones specific for the HER-2/neu proto-oncogene expressed in ovarian carcinomas: related and unrelated to decreased MHC class 1 expression. Int J Cancer 70:112–119
Lollini PL, Colombo MP, De Giovanni C, Nicoletti G, Parmiani G, Prodi G, Nanni P (1985) In vivo reexpression of H-2 antigens in B16 melanoma cells. Exp Clin Immunogenet 2:14–23
Choudhury A, Charo J, Parapuram SK, Hunt RC, Hunt DM, Seliger B, Kiessling R (2004) Small interfering RNA (siRNA) inhibits the expression of the Her2/neu gene, upregulates HLA class I and induces apoptosis of Her2/neu positive tumor cell lines. Int J Cancer 108:71–77
Herrmann F, Lehr HA, Drexler I, Sutter G, Hengstler J, Wollscheid U, Seliger B (2004) HER-2/neu-mediated regulation of components of the MHC class I antigen processing pathway. Cancer Res 64:215–220
Kaplan BLF, Moore TV, Schreiber K, Callender GG, Schreiber H, Nishimura MI (2004) A new murine model for studying HLA-A2-restricted anti-tumor immunity. Cancer Lett 224:153–166
Kono K, Rongcun Y, Charo J, Ichihara F, Celis E, Sette A, Appella E, Sekikawa T, Matsumoto Y, Kiessling R (1998) Identification of HER2/neu-derived peptide epitopes recognized by gastric cancer-specific cytotoxic T lymphocytes. Int J Cancer 78:202–208
Nagata Y, Furugen R, Hiasa A, Ikeda H, Ohta N, Furukawa K, Nakamura H, Kanematsu T, Shiku H (1997) Peptides derived from a wild-type murine proto-oncogene c-erbB-2/HER2/neu can induce CTL and tumor suppression in syngeneic hosts. J Immunol 159:1336–1343
Zhou H, Randall RL, Brothman AR, Maxwell T, Coffin CM, Goldsby RE (2003) Her-2/neu expression in osteosarcoma increases risk of lung metastasis and can be associated with gene amplification. J Pediatr Hematol Oncol 25:27–32
Akatsuka T, Wada T, Kokai Y, Sawada N, Yamawaki S, Ishii S (2001) Loss of ErbB2 expression in pulmonary metastatic lesions in osteosarcoma. Oncology 60:361–366
Thomas DG, Giordano TJ, Sanders D, Biermann JS, Baker L (2002) Absence of HER2/neu gene expression in osteosarcoma and skeletal Ewing’s sarcoma. Clin Cancer Res 8:788–793
Harada K, Yamada A, Mine T, Kawagoe N, Takasu H, Itoh K (2000) Mouse homologue of the human SART3 gene encoding tumor-rejection antigen. Jpn J Cancer Res 91:239–247
Ishida H, Komiya S, Inoue Y, Yutani S, Inoue A, Itoh K (2000) Expression of the SART1 tumor-rejection antigen in human osteosarcomas. Int J Oncol 17:29–32
Tsuda N, Murayama K, Ishida H, Matsunaga K, Komiya S, Itoh K, Yamada A (2001) Expression of a newly defined tumor-rejection antigen SART3 in musculoskeletal tumors and induction of HLA class I-restricted cytotoxic T lymphocytes by SART3-derived peptides. J Orthop Res 19:346–351
Houbiers JG, Nijman HW, van der Burg SH, Drijfhout JW, Kenemans P, van de Velde CJ, Brand A, Momburg F, Kast WM, Melief CJ (1993) In vitro induction of human cytotoxic T lymphocyte responses against peptides of mutant and wild-type p53. Eur J Immunol 23:2072–2077
Gnjatic S, Bressac-de Paillerets B, Guillet JG, Choppin J (1995) Mapping and ranking of potential cytotoxic T epitopes in the p53 protei: effect of mutations and polymorphism on peptide binding to purified and refolded HLA molecules. Eur J Immunol 25:1638–1642
Hoffmann TK, Nakano K, Elder EM, Dworacki G, Finkelstein SD, Appella E, Whiteside TL, DeLeo AB (2000) Generation of T cells specific for the wild-type sequence p53(264-272) peptide in cancer patients: implications for immunoselection of epitope loss variants. J Immunol 165:5938–5944
Hoffmann TK, Loftus DJ, Nakano K, Maeurer MJ, Chikamatsu K, Appella E, Whiteside TL, DeLeo AB (2002) The ability of variant peptides to reverse the nonresponsiveness of T lymphocytes to the wild-type sequence p53(264-272) epitope. J Immunol 168:1338–1347
Wurtzen PA, Claesson MH (2002) A HLA-A2 restricted human CTL line recognizes a novel tumor cell expressed p53 epitope. Int J Cancer 99:568–572
Vierboom MP, Nijman HW, Offringa R, van der Voort EI, van Hall T, van den Broek L, Fleuren GJ, Kenemans P, Kast WM, Melief CJ (1997) Tumor eradication by wild-type p53-specific cytotoxic T lymphocytes. J Exp Med 186:695–704
Brooks P, Murray RZ, Mason GG, Hendil KB, Rivett AJ (2000) Association of immunoproteasomes with the endoplasmic reticulum. Biochem J 352(Pt 3):611–615
Brooks P, Fuertes G, Murray RZ, Bose S, Knecht E, Rechsteiner MC, Hendil KB, Tanaka K, Dyson J, Rivett J (2000) Subcellular localization of proteasomes and their regulatory complexes in mammalian cells. Biochem J 346(Pt 1):155–161
Fruh K, Yang Y (1999) Antigen presentation by MHC class I and its regulation by interferon gamma. Curr Opin Immunol 11:76–81
Tanaka K, Tanahashi N, Tsurumi C, Yokota KY, Shimbara N (1997) Proteasomes and antigen processing. Adv Immunol 64:1–38
Rongcun Y, Salazar-Onfray F, Charo J, Malmberg KJ, Evrin K, Maes H, Kono K, Hising C, Petersson M, Larsson O, Lan L, Appella E, Sette A, Celis E, Kiessling R (1999) Identification of new HER2/neu-derived peptide epitopes that can elicit specific CTL against autologous and allogeneic carcinomas and melanomas. J Immunol 163:1037–1044
Van den Eynde BJ, Morel S (2001) Differential processing of class-I-restricted epitopes by the standard proteasome and the immunoproteasome. Curr Opin Immunol 13:147–153
Lindencrona JA, Preiss S, Kammertoens T, Schuler T, Piechocki M, Wei WZ, Seliger B, Blankenstein T, Kiessling R (2004) CD4+ T cell-mediated HER-2/neu-specific tumor rejection in the absence of B cells. Int J Cancer 109:259–264
Reilly RT, Machiels JP, Emens LA, Ercolini AM, Okoye FI, Lei RY, Weintraub D, Jaffee EM (2001) The collaboration of both humoral and cellular HER-2/neu-targeted immune responses is required for the complete eradication of HER-2/neu-expressing tumors. Cancer Res 61:880–883
Gallo P, Dharmapuri S, Nuzzo M, Maldini D, Iezzi M, Cavallo F, Musiani P, Forni G, Monaci P (2005) Xenogeneic immunization in mice using HER2 DNA delivered by an adenoviral vector. Int J Cancer 113:67–77
Knutson KL, Schiffman K, Disis ML (2001) Immunization with a HER-2/neu helper peptide vaccine generates HER-2/neu CD8 T-cell immunity in cancer patients. J Clin Invest 107:477–484
Knutson KL, Disis ML (2002) Clonal diversity of the T-cell population responding to a dominant HLA-A2 epitope of HER-2/neu after active immunization in an ovarian cancer patient. Hum Immunol 63:547–557
Lollini PL, Nicoletti G, Landuzzi L, De Giovanni C, Rossi I, Di Carlo E, Musiani P, Muller WJ, Nanni P (1998) Down regulation of major histocompatibility complex class I expression in mammary carcinoma of HER-2/neu transgenic mice. Int J Cancer 77:937–941
Castilleja A, Ward NE, O’Brian CA, Swearingen B II, Swan E, Gillogly MA, Murray JL, Kudelka AP, Gershenson DM, Ioannides CG (2001) Accelerated HER-2 degradation enhances ovarian tumor recognition by CTL. Implications for tumor immunogenicity. Mol Cell Biochem 217:21–33
Hartmann F, Horak EM, Cho C, Lupu R, Bolen JB, Stetler-Stevenson MA, Pfreundschuh M, Waldmann TA, Horak ID (1997) Effects of the tyrosine-kinase inhibitor geldanamycin on ligand-induced Her-2/neu activation, receptor expression and proliferation of Her-2-positive malignant cell lines. Int J Cancer 70:221–229
Tikhomirov O, Carpenter G (2000) Geldanamycin induces ErbB-2 degradation by proteolytic fragmentation. J Biol Chem 275:26625–26631
Kominsky SL, Hobeika AC, Lake FA, Torres BA, Johnson HM (2000) Down-regulation of neu/HER-2 by interferon-gamma in prostate cancer cells. Cancer Res 60:3904–398
Marth C, Muller-Holzner E, Greiter E, Cronauer MV, Zeimet AG, Doppler W, Eibl B, Hynes NE, Daxenbichler G (1990) Gamma-interferon reduces expression of the protooncogene c-erbB-2 in human ovarian carcinoma cells. Cancer Res 50:7037–7041
Mishra S, Hamburger AW (1994) Interferon gamma-induced reduction in erbB-2 tyrosyl phosphorylation in human ovarian carcinoma cells. Int J Cancer 58:538–542
Epstein RJ, Druker BJ, Roberts TM, Stiles CD (1990) Modulation of a Mr 175,000 c-neu receptor isoform in G8/DHFR cells by serum starvation. J Biol Chem 265:10746–10751
Huang SS, Koh HA, Konish Y, Bullock LD, Huang JS (1990) Differential processing and turnover of the oncogenically activated neu/erb B2 gene product and its normal cellular counterpart. J Biol Chem 265:3340–3346
Castilleja A, Ward NE, Epstein RB, Kudelka AP, Gershenson DM, Efferson CL, O’Brian CA, Ioannides CG (2002) Treatment with HER-2 phosphorylation agonists enhance tumor ability to stimulate epitope specific CTL in vitro. Oncol Rep 9:929–935
Reese DM, Slamon DJ (1997) HER-2/neu signal transduction in human breast and ovarian cancer. Stem Cells 15:1–8
Acknowledgments
This research was supported by National Institutes of Health Grants CA90873 and CA10228, and American Cancer Society, Illinois Division Grant 01-21 (to M.I.N.), and grants from the Swedish Cancer Society, the Swedish Research Medical Council, and the Cancer Society of Stockholm (to R.K.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaplan, B.L.F., Norell, H., Callender, G.G. et al. Interferon-γ renders tumors that express low levels of Her-2/neu sensitive to cytotoxic T cells. Cancer Immunol Immunother 55, 653–662 (2006). https://doi.org/10.1007/s00262-005-0050-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-005-0050-5