Abstract
Purpose
The aim of this study was to evaluate the impact of androgen ablation therapy in different prostate cancer (PCa) cell lines—reflecting different stages of the disease—on 18F-fluorodeoxyglucose (FDG), 11C-choline and 11C-acetate uptake.
Methods
Uptake experiments were performed in androgen-sensitive (LNCaP, PC346C) and independent cell lines (22Rv1, PC346DCC, PC-3) as well as in a benign prostatic hyperplasia (BPH-1) cell line. Tracer uptake was assessed under androgen ablation. Results of the cancer cell lines were normalized to those of BPH-1. To evaluate the effect of androgen on the uptake of 18F-FDG, 11C-choline and 11C-acetate in PCa cell lines, 10−8M R1881, 10−10M R1881, the combination of 10−10M R1881 plus 10−6M Casodex or 10−6M Casodex alone were added in parallel cell cultures 1 day before uptake experiments. Uptake in androgen-supplemented cell cultures was compared to the uptake under androgen deprivation. Uptake was corrected for cell number using protein content.
Results
Compared to BPH-1, a higher 18F-FDG uptake was observed only in PC346C cells, whereas a higher 11C-choline and markedly increased 11C-acetate uptake was seen in all cancer cell lines. Androgens significantly modulated the uptake of 18F-FDG in LNCaP, PC346C and 22Rv1 cells, and of 11C-choline in the PC346C and 22Rv1 cell line. No androgenic effect on 11C-choline and 18F-FDG uptake was observed in PC-3 and PC346DCC cells. 11C-Acetate uptake was independent of androgen status in all PCa cell lines studied.
Conclusion
18F-FDG uptake in PCa cell lines showed the highest variability and strongest androgen effect, suggesting its poor potential for metabolic imaging of advanced PCa. In contrast to 18F-FDG and 11C-choline, 11C-acetate uptake was unaffected by androgens and thus 11C-acetate seems best for monitoring PCa progression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Prostate cancer (PCa) affects approximately one out of six men and is the second leading cancer-related cause of death which is generally due to progressive metastatic PCa resistant to therapy [1]. At initial diagnosis, most prostate tumours show an androgen-dependent proliferation. Therefore, therapeutic approaches interfering with androgen receptor (AR) activity are commonly used for treating advanced PCa. Unfortunately, in most patients therapy fails over a period of 2–4 years and castration-resistant prostate cancer (CRPC) with local and distant recurrences develops.
For the noninvasive detection of primary tumours as well as recurrences following therapy, anatomical and functional imaging is essential. Anatomical imaging techniques such as computed tomography (CT), ultrasound (US) and magnetic resonance imaging (MRI) show a moderate efficiency for tumour detection. On the other hand, molecular imaging with positron emission tomography (PET) offers specific biological tumour information and has a higher sensitivity for tracing tumours. This technique may also improve the detection of early therapy response since tumour metabolism can alter before morphological changes are detected. Currently 18F-fluorodeoxyglucose (FDG), a glucose analogue, is the most frequently used PET tracer in oncology. However, FDG PET has drawbacks for the detection of PCa which is mainly due to the slow growth rate of PCa cells and the renal excretion of this tracer [2, 3]. Moreover, FDG fails in differentiating PCa from benign prostatic hyperplasia and inflammation [4] which hampers the sensitive detection of local disease. Still, in patients suffering from metastatic disease the prognostic potential of FDG PET has been shown [5–7]. In the attempt to improve PCa detection other metabolic tracers such as 11C-choline (choline) and 11C-acetate (acetate) have been evaluated and show a more beneficial biodistribution and elimination compared to that of FDG [8, 9]. Currently, choline PET is preferentially used for detecting primary PCa and restaging recurrences after treatment [10]. However, until now choline uptake does not significantly correlate with tumour proliferation rate [11]. Besides this tracer, acetate is under evaluation for its application in PCa detection with PET. So far results demonstrate a good diagnostic performance comparable to that of choline [12–14].
Androgens play a key role in the evolution of PCa and evoke their cellular responses through activation of the AR. In benign as well as malignant prostate cells androgens are important regulators for cellular proliferation and control glucose and lipid metabolism [15]. However, androgen deprivation therapy given in patients with advanced disease stimulates the development of AR and AR signalling modifications [16] which makes tumour cells able to circumvent therapy-induced apoptosis. Therefore, aberrant expression of AR target genes after therapy may not only influence the proliferative character of cancer cells but may have a direct effect on metabolic processes and thus also metabolic imaging with PET. The effect of androgen deprivation on prostate tumours has been demonstrated with FDG and choline PET [17, 18]. Nevertheless, the altered uptake may not completely be due to therapeutic success, but could also result from a diminished cellular uptake of metabolic PET tracers which may be controlled by androgens under normal situations.
The ideal metabolic tracer should delineate PCa manifestations not only in hormone naïve, untreated patients, but also in men with disseminated PCa receiving androgen ablation therapy. To monitor disease progression the ideal tracer should be unaffected by androgens and independent of potential androgen-related effects on the prostate tumour cells. After all, the presence of local and/or distant recurrences could be underestimated or missed. For this purpose, we evaluated the impact of androgens on the uptake of FDG, choline and acetate in five human prostate cancer cell lines, each resembling a different state of the disease.
Materials and methods
Reagents
The synthetic androgen methyltrienolone (R1881) was purchased from PerkinElmer (Waltham, MA, USA). The antiandrogen bicalutamide (Casodex) was obtained from AstraZeneca (Brussels, Belgium). All reagents were dissolved in ethanol.
Cell lines
BPH-1 is an immortalized epithelial cell line which is derived from transurethral resected prostate tissue and negative for AR and prostate-specific antigen (PSA) expression [19]. Also, five PCa cell lines differing in AR status and androgen sensitivity (based on proliferation) were employed. The androgen-sensitive LNCaP cell line [20] originated from a lymph node metastasis of PCa, is characterized by the alanine at position 877 to threonine mutation (T877A) located in the ligand binding domain (LBD) of the AR which broadens its ligand specificity to other steroids (oestrogen, progestin, adrenal androgen) and the synthetic antiandrogen flutamide. The androgen-sensitive PC346C cell line is derived from a transrectal urethral resection of the primary tumour of a non-progressive patient and expresses a wild-type AR [21]. 22Rv1 is an androgen-independent cancer cell line and is a model for studying the progression towards CRPC [22]. The AR population of 22Rv1 is heterogeneous and characterized by the expression of a constitutive active truncated AR (AR∆LBD) and a mutated AR containing the substitution of tyrosine for histidine (H875Y) in the LBD and/or an in-frame exon 3 duplication (E3DM) in the DNA binding domain (DBD) causing decreased AR activity [23, 24]. The androgen-independent cell line PC346DCC is established from long-term culturing of PC346C in the absence of androgen and is demonstrated to have a very low expression of AR harbouring a lysine at position 311 to arginine substitution (K311R AR mutation) in the amino terminal domain (NTD) [21]. PC-3 is an androgen-independent cell line defined to be AR negative [25].
Cell culture
All cell lines were cultured at 37°C in a humidified incubator with 5% CO2/95% air atmosphere. LNCaP, 22Rv1 and BPH-1 cells were grown in RPMI 1640 medium (Invitrogen) supplemented with 10% fetal bovine serum (FBS) (Invitrogen) and 3 mM L-glutamine (Invitrogen). For routine maintenance of BPH-1 cells, 70 nmol/l testosterone (Sigma) and 1% insulin-transferrin-selenium mixture (Invitrogen) were added to this medium. PC-3 cells were cultured in Dulbecco’s modified Eagle’s medium, DMEM F12 (Invitrogen), supplemented with 10% FBS. Cells were grown in Nunclon surface treated culture flasks (NUNC, Thermo Scientific). The PC346C and -DCC cell lines were obtained from Rotterdam (Department of Urology, Erasmus University, Rotterdam, The Netherlands). Cells were grown in Primaria tissue culture flasks (BD Biosciences). PC346C cells were cultured in DMEM F12 medium adjusted with 2% FBS, 1% insulin-transferrin-selenium, 0.01% bovine serum albumin (BSA) (Invitrogen), 10 ng/ml epidermal growth factor (EGF) (Sigma-Aldrich), 0.1 μg/ml fibronectin (Sigma-Aldrich), 20 μg/ml fetuin (Sigma-Aldrich), 50 ng/ml cholera toxin (Sigma-Aldrich), 0.1 mM phosphoethanolamine (Sigma-Aldrich), 1 nM triidothyronine (T3) (Acros), 10−10 M R1881 and 1.4 μM hydrocortisone (Sigma-Aldrich). For cultivation of PC346DCC, 2% charcoal-treated FBS (CT-FBS) was supplemented instead of FBS to the above-described medium mixture and R1881 was omitted.
For examining the effect of androgens on tracer uptake, CT-FBS was used to diminish background steroid levels and addition of testosterone or R1881 was omitted. Also, supplement to the experimental medium of PC346C and -DCC cell lines was reduced to 1% insulin-transferrin-selenium, 0.01% BSA and 10 ng/ml EGF.
Radiotracer uptake experiments
Prior to the uptake experiment, BPH-1 (1×105 cells per well), PC-3 (1×105 cells per well), LNCaP (2×105 cells per well) and 22Rv1 (2.5×105 cells per well) cells were seeded in 24-well plates (NUNC, Thermo Scientific), whereas PC346C (3×105 cells per well) and -DCC (2×105 cells per well) cells were grown on Primaria surface treated 24-well plates (BD Biosciences). To compare the internalization of FDG, choline and acetate among all prostate cancer cell lines in the setting of androgen ablation, cells were grown in the absence of androgens (CT-FBS supplemented medium) 2 days preceding the uptake experiment. The BPH-1 cell line was included in every experiment as a reference to be able to compare the tracer uptake among the cell lines (uptake in cancer cells/uptake in BPH-1).
To evaluate the effect of androgen on tracer uptake, the CT-FBS supplemented medium was refreshed 1 day after seeding and cells were incubated in a volume of 0.5 ml/well containing 0.01% ethanol (native), 10−8 M R1881 or 10−6 M Casodex (complete androgen depletion). In a later stage of the experiment, also the effects of a lower androgen concentration (10−10 M R1881) and its combination with antiandrogen (10−10 M R1881 plus 10−6 M Casodex) on the uptake of metabolic tracers were examined in PC346C, 22Rv1 and PC346DCC cells. One day after supplementation, the radiotracer (4 kBq FDG, 37 kBq choline or acetate) was added to each well using a volume of 250 μl phosphate-buffered saline (PBS). Cells were incubated at 37°C for 5, 15, 30 and 60 min. Two additional incubation time points (90 and 120 min) were included for FDG uptake experiments. The radiotracer solution was removed and cells were washed twice with ice-cold PBS. Cells were finally lysed [20 mM Tris, 100 mM NaCl, 1 mM ethylenediaminetetraacetate (EDTA), 1% Triton X-100 (Merck), 0.3% sodium dodecyl sulfate (SDS)] and measured for radioactive tracer uptake in a gamma counter. A protein assay bicinchoninic acid assay (BCA) was performed for normalization of the cellular tracer uptake.
Statistical analysis
Uptake experiments were performed twice with triplicate conditions. Results are expressed as mean value ± SEM. Statistical analysis was done using one-way analysis of variance (ANOVA) and Tukey’s HSD post hoc analysis. A p value <0.05 was defined as statistically significant. Subsequently, uptake values at specific time points were compared by unpaired Student’s t test, with Bonferroni correction for the number of time points, assuming a significance at p ≤ 0.05/n (n = time points).
Results
Relative uptake of FDG, choline and acetate
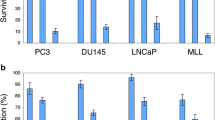
With respect to BPH-1, a significantly higher uptake of FDG was observed in the androgen-sensitive cell line PC346C (Fig. 1a) after 60, 90 and 120 min of tracer incubation. On the contrary, the relative FDG uptake was significantly lower in the androgen-sensitive LNCaP and androgen-independent 22Rv1 and PC-3 cell lines. Significant results were obtained at 60 and 120 min in LNCaP, at 5 and 15 min in PC-3 and at all time points in 22Rv1 cells. No significantly different relative FDG uptake was observed in the androgen-independent PC346DCC cell line (Fig. 1a).
Relative 18F-FDG (a), 11C-choline (b) and 11C-acetate (c) uptake in the LNCaP (○), PC346C (▲), 22Rv1 (■), PC346DCC (∆) and PC-3 (●) cell lines after 5, 15, 30, 60 (90 and 120)٭ min. Tracer uptake in the cancer cells was normalized to the uptake in BPH-1 cells (reference = 1) and is logarithmically fitted. Error bars indicate standard errors (n = 6). ٭2 additional time points included in 18F-FDG uptake experiments. Significances are indicated with *
The uptake of choline was significantly higher in every cancer cell line compared to BPH-1 (Fig. 1b). Significantly higher uptake values were seen at two time points in the PC-3 (5 and 15 min) and PC346C (30 and 60 min) cell lines, and at all time points in the other cell lines. Further, over time a slow washout of choline was observed in PC-3 and PC346DCC as opposed to the other cancer cell lines. Finally, a significantly higher relative acetate uptake was observed in all prostate cancer cell lines as compared to FDG and choline (Fig. 1c). Whereas a significantly increased tracer uptake in PC-3 cells was seen after only 5 min, acetate uptake in the other cell lines was significantly higher at the last three (LNCaP and 22Rv1) or all (PC346C and PC346DCC) time points. Unlike the other cell lines, PC-3 and PC346C showed a washout of acetate over time.
Androgen-mediated uptake of FDG, choline and acetate
To investigate whether androgens affect the uptake of FDG, choline or acetate, PCa cell lines were grown in different experimental conditions adding androgens with or without antiandrogens (see “Materials and methods” section). For every tracer, the uptake was determined at four time points (5, 15, 30 and 60 min). The tracer uptake in androgen-supplemented conditions was compared to the uptake in cells grown in the absence of androgens (native and CT-FBS plus 10−6M Casodex). For conditions showing a significant influence of androgen on tracer uptake, differences at specific time points were analysed.
Androgens did not modulate the uptake of FDG, choline or acetate in the androgen-independent, AR-negative cell lines PC-3 (Table 1) and PC346DCC (Table 2). As opposed to these cell lines, androgens (10−8 M) significantly influenced the uptake of FDG (5, 15, 60 min) and choline (15 min) in the androgen-independent, AR-expressing cell line 22Rv1 (Fig. 2a, b). Compared to control cells grown in the presence of antiandrogen (CT-FBS plus 10−6 M Casodex), the significant effect on FDG uptake was further observed at every time point in this cell line (Fig. 2a). A significant modulation of androgens (10−8 M) on the uptake of FDG and choline was observed in androgen-sensitive, AR-expressing LNCaP (5, 15, 30, 60 min) and PC346C (30 min) cells, respectively (Figs. 3a and 4b). Moreover, in the PC346C cell line a significant effect of androgens on FDG uptake was observed (Fig. 4a) compared to the uptake in a control grown in the presence of antiandrogens (CT-FBS plus 10−6 M Casodex). Androgens at a concentration of 10−10 M also significantly increased FDG uptake in the AR-expressing 22Rv1 and PC346C cell lines. This effect was reduced by the addition of the antiandrogen Casodex (10−6 M) to these cells (Figs. 2 and 4).
18F-FDG (a), 11C-choline (b) and 11C-acetate (c) uptake in the 22Rv1 cell line. Cells were grown in androgen-deprived medium (native) with or without supplemented androgens (R1881 10−8 M, R1881 10−10 M) and/or antiandrogens (Casodex 10−6 M). Tracer uptake was measured after 5, 15, 30 and 60 min. Means ± SEM are presented. The significant effect of androgens compared to native is indicated with *, compared to CT-FBS plus Casodex 10−6 M with ●
18F-FDG (a), 11C-choline (b) and 11C-acetate (c) uptake in the LNCaP cell line. Cells were grown in androgen-deprived medium (native) with or without supplemented androgens (R1881 10−8 M) or antiandrogens (Casodex 10−6 M). Tracer uptake was measured after 5, 15, 30 and 60 min. Means ± SEM are presented. The significant effect of androgens compared to native is indicated with *, compared to CT-FBS plus Casodex 10−6 M with ●
18F-FDG (a), 11C-choline (b) and 11C-acetate (c) uptake in the PC346C cell line. Cells were grown in androgen-deprived medium (native) with or without supplemented androgens (R1881 10−8 M, R1881 10−10 M) and/or antiandrogens (Casodex 10−6 M). Tracer uptake was measured after 5, 15, 30 and 60 min. Means ± SEM are presented. The significant effect of androgens compared to native is indicated with *, compared to CT-FBS plus Casodex 10−6 M with ●
Most notably, acetate uptake was unaffected by androgens and the addition of the antiandrogen Casodex in all three AR-expressing human PCa cell lines 22Rv1, LNCaP and PC346C (Figs. 2, 3 and 4).
Discussion
The present study investigated the impact of androgens on the uptake of the metabolic PET tracers FDG, choline and acetate in PCa cell lines in order to determine their potential for monitoring disease progression.
When looking at the uptake in native conditions, this study revealed a variable uptake of FDG, compared to that of choline and acetate, in PCa cell lines. With respect to the reference cell line, BPH-1, the uptake of FDG was higher in the PC346C cell line, whereas a lower uptake was observed in LNCaP, PC-3 and 22Rv1 cells. PC346DCC showed a comparable FDG uptake with respect to BPH-1. Since glucose metabolism differs between diverse stages of PCa, a variable FDG uptake comparing the cell lines could have been expected. However, in our study the uptake of FDG was compared in cells grown under androgen deprivation. Considering that androgen-sensitive cells (LNCaP, PC346C) become less metabolically active in this situation, a lower uptake than in androgen-independent PCa cell lines (22Rv1, PC-3, PC346DCC) was assumed. In a previous study LNCaP cells displayed a lower FDG uptake compared to PC-3 cells in the setting of androgen deprivation [26]. For LNCaP we could confirm these findings; however, the PC346C cell line displayed an—at the moment unclear—enhanced uptake in this condition.
In contrast to FDG, an elevated choline and acetate uptake was observed in all cancer cell lines. Compared to the other cell lines, PC-3 and PC346DCC showed a washout of choline over time. Distinct washout of acetate was observed in PC-3 and PC346C cells. Differences regarding the metabolic kinetics of choline and acetate could be a potential cause for the diverse uptake trends seen over time.
After establishing the “native” characteristics of tracer uptake in our cell lines resembling different stages of PCa, we focused on the modulation of androgen on tracer uptake. An influence of androgens on the uptake of FDG in PCa cell lines was demonstrated. Androgens affected FDG uptake in the AR-positive, androgen-sensitive cell lines LNCaP and PC346C. No effect was observed in the androgen-independent PC-3 (AR-negative) and PC346DCC cell line, whereas androgens enhanced FDG uptake in the androgen-independent, but AR-positive cell line 22Rv1. These results suggest that androgen ablation therapy may hamper accurate FDG PET imaging of androgen-sensitive PCa as well as a subset of CRPC.
Androgen-sensitive LNCaP and PC346C cells are characterized by the expression of a mutated and wild-type AR, respectively. Since androgens can activate both receptors, their influence on FDG uptake in these cell lines was conceivable. Androgen-independent PC-3 cells lack AR expression which prevented androgens from controlling FDG uptake in this cell line. However, 22Rv1 and PC346DCC, both androgen-independent cell lines, showed a diverse response to androgens concerning their FDG uptake. PC346DCC cells are known to express a mutated AR (K311R AR mutation) of which the effect on AR activation is currently unknown. Yet, previous studies suggest that these cells bypass the AR pathway for sustaining proliferation and therefore potentially also FDG uptake [21]. Unlike in the PC346DCC cell line, androgens affected the uptake of FDG in 22Rv1 cells. The 22Rv1 cell line expresses a mutated AR which is sensitive for steroids [23] and thus possibly sustains androgen to affect FDG uptake. Differences in AR can provoke a diverse response to AR activation. Depending on which AR mutation occurs following androgen ablation therapy, this can interfere with FDG PET imaging of prostate tumours. This may not only cause an overestimation of therapy response, but might underestimate the detection of dormant and a subset of androgen-independent PCa cells in which FDG uptake is reduced due to therapy. Until now FDG PET has been shown to perform reasonably in patients suffering from androgen-independent CRPC and metastatic PCa [5]. However, in the clinical setting it remains questionable whether androgen-independent proliferation develops parallel with the loss of androgen-controlled gene expression. After all, if this is not true patients may have developed clinically androgen-resistant tumours, though decreased therapy-induced tracer internalization may interfere with PET detection of these tumours.
The rationale for using FDG in oncological PET imaging is that malignant cells usually have a higher glucose metabolism to satisfy their increased energy demand compared to benign cells. The increased de novo lipogenesis is one of the energy demanding characteristics in cancer and is modulated by androgens in PCa. FDG enters the cell primarily via the glucose transporter GLUT-1 and is phosphorylated by the enzyme hexokinase. Since phosphorylated FDG is not a substrate for the further glycolysis it gets trapped in the cell and this is the basis for the detection by means of PET. In PCa increased expression levels of glucose transporters, and specifically GLUT-1, have been demonstrated [27]. Moreover, androgens were shown to induce the expression of GLUT-1 in LNCaP—but not in PC-3 cells—through activation of the hypoxia-inducible factor 1 (HIF-1) [28–30]. Besides this uptake mechanism, androgens stimulated the expression of hexokinase in LNCaP cells which mediated the increased uptake of glucose [31]. Based on these previous findings, an influence of androgens on the expression of transporters and catalysing enzymes affecting glucose utilization may be the reason for the observed increased FDG uptake seen in the cell lines studied; however, in vivo this is only of relevance in fast proliferating states of PCa.
Choline is an essential component for the lipogenesis and is taken up by a specific transporter as well as by a diffusion-like process [32]. Choline is phosphorylated by the rate-limiting enzyme choline kinase and further metabolized to phosphatidylcholine which is incorporated into the membrane of proliferating cells. In vitro choline uptake correlated well with proliferation [33]; however, in vivo this could not be observed [34]. Since micro-environmental factors such as hypoxia and surrounding tissue are obviously not mimicked in the in vitro situations, the question could arise whether choline uptake may be involved in processes besides proliferation. However, because of the small sample size and the limited number of undifferentiated cancers studied by Breeuwsma et al., a possible correlation between cellular proliferation and choline uptake could have been masked.
Since it is not completely elucidated whether choline PET imaging only reflects tumour proliferation, we investigated the influence of androgen on the uptake of this metabolic tracer in PCa. Choline uptake was affected by androgens in PCa cells. Androgens stimulated the uptake of choline in the PC346C and 22Rv1 cell lines, whereas no effect was observed in LNCaP, PC-3 and PC346DCC cells. It remains unclear why in this study androgens influenced choline uptake in one androgen-sensitive cell line (PC346C) but not in the other (LNCaP). Previously, it was shown that androgen deprivation decreases the concentration of choline metabolites in androgen-sensitive, wild-type AR-expressing LAPC-4 cells over time, whereas an increase was seen in androgen-sensitive, mutated AR-expressing LNCaP cells [35]. These results might suggest a stimulating effect of androgen deprivation on phospholipid metabolism in LNCaP cells and a reducing effect in LAPC-4 cells. As PC346C cells, like LAPC-4 cells, express a wild-type AR, a similar effect of AR signalling in both cell lines could be considered. We speculate that androgens could have stimulated choline uptake in the PC346C cell line, whereas a reverse or reduced effect could have occurred in LNCaP cells. However, in vivo androgen did not modulate choline uptake so far [36]. As a result of AR mutations and differences in AR-induced cell signalling among PCa cell lines, androgens may interfere with the uptake of choline.
In patients undergoing PET/CT for preoperative staging of PCa, a significant reduced choline uptake was observed after androgen deprivation with bicalutamide [18]. In these patients suffering from androgen-sensitive PCa, neoadjuvant therapy induces glandular atrophy and loss of choline prostate metabolites. Thus, the reduction of choline uptake following androgen deprivation in patients with newly diagnosed PCa is consistent with the known effects of this treatment on the histological and metabolic features of PCa cells. In contrast, as reported by Giovacchini et al., recurrent tumours or metastases in patients who develop biochemical failure during androgen deprivation no longer have an androgen-sensitive proliferation [37]. Results of our study are partly in line with clinical observations showing the effect of androgen on choline uptake in PCa cells. Besides in androgen-sensitive cells, androgen was also able to influence the uptake of choline in our CRPC cell line (22Rv1). Thus, although PCa recurrences can escape therapy-induced apoptosis, androgen deprivation could still affect the expression of genes involved in the uptake of choline in androgen-independent yet responsive disease. This observation, when verified in the clinical setting, could also question whether choline PET could be used for evaluating the status of androgen sensitivity of prostate tumours following antiandrogen therapy.
The initial staging of PCa is usually done by echography or MRI and 99mTc-methylene diphosphonate single photon emission computed tomography (SPECT) imaging. Although these techniques perform clinically well, the additional value of choline PET for detecting primary intraprostatic tumours as well as lymph node involvement is further being evaluated. In case of recurrence choline PET has been shown to have the greatest impact. Whether it could be helpful in therapy assessment in advanced PCa has to be further elucidated.
Besides glucose and choline, increased acetate metabolism has been observed in cancer compared to benign cells as the result of the increased fatty acid synthesis [15]. The exact cellular uptake mechanism for acetate is not yet clear. Nevertheless, the internalization is thought to be driven by monocarboxylate transporters (MCT) [38]. Although the expression of enzymes—mainly fatty acid synthase (FASN)—involved in fatty acid synthesis is regulated by androgens, androgen did not affect the uptake of acetate in PCa cells in this experiment. Therefore, our results indicate that the uptake mechanism for this tracer is not controlled by androgens which we consider the most important finding of this study. A publication of Oyama et al. also supports the lack of androgen modulation on acetate uptake in PCa cells [39]. Moreover, in patients acetate was recently indicated to be promising for the assessment of therapy response in PCa bone metastases and to be complementary to FDG PET for the detection of this disease [40]. Since our data suggest that unlike FDG acetate uptake occurs androgen independently, acetate PET may offer a more sensitive and accurate approach for post-therapeutic detection of metastatic disease. For these reasons, compared to FDG and choline, acetate holds promise for accurate PET detection of advanced prostate cancer exposed to androgen ablation therapy.
Conclusion
This study demonstrated the most variable and least efficient uptake of FDG in PCa cell lines in the setting of androgen deprivation. FDG and choline lack an androgen-independent internalization in a subset of PCa cell lines, irrespective of their androgen responsiveness, whereas the uptake of acetate appeared to be independent of androgen activation or suppression in all PCa cell lines. The fact that FDG, choline and acetate uptake responded differently to androgens suggests that androgen signalling may specifically affect their uptake mechanisms and/or biochemical pathways. Our in vitro findings conclude that acetate is the better tracer for the detection of advanced PCa and favour its use for assessing tumour response following androgen ablation therapy by PET. Nevertheless, it is necessary to investigate these results in in vivo studies in order to translate our findings to the clinical setting.
References
Jemal A, Siegel R, Xu J, Ward E. Cancer statistics, 2010. CA Cancer J Clin 2010;60:277–300.
Schöder H, Herrmann K, Gönen M, Hricak H, Eberhard S, Scardino P, et al. 2-[18F]fluoro-2-deoxyglucose positron emission tomography for the detection of disease in patients with prostate-specific antigen relapse after radical prostatectomy. Clin Cancer Res 2005;11:4761–9.
Liu IJ, Zafar MB, Lai YH, Segall GM, Terris MK. Fluorodeoxyglucose positron emission tomography studies in diagnosis and staging of clinically organ-confined prostate cancer. Urology 2001;57:108–11.
Hofer C, Laubenbacher C, Block T, Breul J, Hartung R, Schwaiger M. Fluorine-18-fluorodeoxyglucose positron emission tomography is useless for the detection of local recurrence after radical prostatectomy. Eur Urol 1999;36:31–5.
Fricke E, Machtens S, Hofmann M, van den Hoff J, Bergh S, Brunkhorst T, et al. Positron emission tomography with 11C-acetate and 18F-FDG in prostate cancer patients. Eur J Nucl Med Mol Imaging 2003;30:607–11.
Morris MJ, Akhurst T, Larson SM, Ditullio M, Chu E, Siedlecki K, et al. Fluorodeoxyglucose positron emission tomography as an outcome measure for castrate metastatic prostate cancer treated with antimicrotubule chemotherapy. Clin Cancer Res 2005;11:3210–6.
Oyama N, Akino H, Suzuki Y, Kanamaru H, Miwa Y, Tsuka H, et al. Prognostic value of 2-deoxy-2-[F-18]fluoro-D-glucose positron emission tomography imaging for patients with prostate cancer. Mol Imaging Biol 2002;4:99–104.
Sutinen E, Nurmi M, Roivainen A, Varpula M, Tolvanen T, Lehikoinen P, et al. Kinetics of [(11)C]choline uptake in prostate cancer: a PET study. Eur J Nucl Med Mol Imaging 2004;31:317–24.
Seltzer MA, Jahan SA, Sparks R, Stout DB, Satyamurthy N, Dahlbom M, et al. Radiation dose estimates in humans for (11)C-acetate whole-body PET. J Nucl Med 2004;45:1233–6.
Hara T, Kosaka N, Kishi H. PET imaging of prostate cancer using carbon-11-choline. J Nucl Med 1998;39:990–5.
Reske SN, Blumstein NM, Neumaier B, Gottfried HW, Finsterbusch F, Kocot D, et al. Imaging prostate cancer with 11C-choline PET/CT. J Nucl Med 2006;47:1249–54.
Oyama N, Akino H, Kanamaru H, Suzuki Y, Muramoto S, Yonekura Y, et al. 11C-acetate PET imaging of prostate cancer. J Nucl Med 2002;43:181–6.
Oyama N, Miller TR, Dehdashti F, Siegel BA, Fischer KC, Michalski JM, et al. 11C-acetate PET imaging of prostate cancer: detection of recurrent disease at PSA relapse. J Nucl Med 2003;44:549–55.
Kotzerke J, Volkmer BG, Glatting G, van den Hoff J, Gschwend JE, Messer P, et al. Intraindividual comparison of [11C]acetate and [11C]choline PET for detection of metastases of prostate cancer. Nuklearmedizin 2003;42:25–30.
Swinnen JV, Verhoeven G. Androgens and the control of lipid metabolism in human prostate cancer cells. J Steroid Biochem Mol Biol 1998;65:191–8.
Feldman BJ, Feldman D. The development of androgen-independent prostate cancer. Nat Rev Cancer 2001;1:34–45.
Oyama N, Akino H, Suzuki Y, Kanamaru H, Ishida H, Tanase K, et al. FDG PET for evaluating the change of glucose metabolism in prostate cancer after androgen ablation. Nucl Med Commun 2001;22:963–9.
Giovacchini G, Picchio M, Coradeschi E, Scattoni V, Bettinardi V, Cozzarini C, et al. [(11)C]choline uptake with PET/CT for the initial diagnosis of prostate cancer: relation to PSA levels, tumour stage and anti-androgenic therapy. Eur J Nucl Med Mol Imaging 2008;35:1065–73.
Hayward SW, Dahiya R, Cunha GR, Bartek J, Deshpande N, Narayan P. Establishment and characterization of an immortalized but non-transformed human prostate epithelial cell line: BPH-1. In Vitro Cell Dev Biol Anim 1995;31:14–24.
Horoszewicz JS, Leong SS, Kawinski E, Karr JP, Rosenthal H, Chu TM, et al. LNCaP model of human prostatic carcinoma. Cancer Res 1983;43:1809–18.
Marques RB, Erkens-Schulze S, de Ridder CM, Hermans KG, Waltering K, Visakorpi T, et al. Androgen receptor modifications in prostate cancer cells upon long-term androgen ablation and antiandrogen treatment. Int J Cancer 2005;117:221–9.
Sramkoski RM, Pretlow TG, Giaconia JM, Pretlow TP, Schwartz S, Sy MS, et al. A new human prostate carcinoma cell line, 22Rv1. In Vitro Cell Dev Biol Anim 1999;35:403–9.
Tepper CG, Boucher DL, Ryan PE, Ma AH, Xia L, Lee LF, et al. Characterization of a novel androgen receptor mutation in a relapsed CWR22 prostate cancer xenograft and cell line. Cancer Res 2002;62:6606–14.
van Bokhoven A, Varella-Garcia M, Korch C, Johannes WU, Smith EE, Miller HL, et al. Molecular characterization of human prostate carcinoma cell lines. Prostate 2003;57:205–25.
Kaighn ME, Narayan KS, Ohnuki Y, Lechner JF, Jones LW. Establishment and characterization of a human prostatic carcinoma cell line (PC-3). Invest Urol 1979;17:16–23.
Hara T, Bansal A, DeGrado TR. Effect of hypoxia on the uptake of [methyl-3H]choline, [1-14C] acetate and [18F]FDG in cultured prostate cancer cells. Nucl Med Biol 2006;33:977–84.
Effert P, Beniers AJ, Tamimi Y, Handt S, Jakse G. Expression of glucose transporter 1 (Glut-1) in cell lines and clinical specimens from human prostate adenocarcinoma. Anticancer Res 2004;24:3057–63.
Clavo AC, Brown RS, Wahl RL. Fluorodeoxyglucose uptake in human cancer cell lines is increased by hypoxia. J Nucl Med 1995;36:1625–32.
Mabjeesh NJ, Willard MT, Frederickson CE, Zhong H, Simons JW. Androgens stimulate hypoxia-inducible factor 1 activation via autocrine loop of tyrosine kinase receptor/phosphatidylinositol 3'-kinase/protein kinase B in prostate cancer cells. Clin Cancer Res 2003;9:2416–25.
Horii K, Suzuki Y, Kondo Y, Akimoto M, Nishimura T, Yamabe Y, et al. Androgen-dependent gene expression of prostate-specific antigen is enhanced synergistically by hypoxia in human prostate cancer cells. Mol Cancer Res 2007;5:383–91.
Moon JS, Jin WJ, Kwak JH, Kim HJ, Yun MJ, Kim JW, et al. Androgen stimulates glycolysis for de novo lipid synthesis by increasing the activities of hexokinase 2 and 6-phosphofructo-2-kinase/fructose-2,6-bisphosphatase 2 in prostate cancer cells. Biochem J 2010;433:225–33.
Müller SA, Holzapfel K, Seidl C, Treiber U, Krause BJ, Senekowitsch-Schmidtke R. Characterization of choline uptake in prostate cancer cells following bicalutamide and docetaxel treatment. Eur J Nucl Med Mol Imaging 2009;36:1434–42.
Al-Saeedi F, Welch AE, Smith TA. [methyl-3H]Choline incorporation into MCF7 tumour cells: correlation with proliferation. Eur J Nucl Med Mol Imaging 2005;32:660–7.
Breeuwsma AJ, Pruim J, Jongen MM, Suurmeijer AJ, Vaalburg W, Nijman RJ, et al. In vivo uptake of [11C]choline does not correlate with cell proliferation in human prostate cancer. Eur J Nucl Med Mol Imaging 2005;32:668–73.
Ackerstaff E, Pflug BR, Nelson JB, Bhujwalla ZM. Detection of increased choline compounds with proton nuclear magnetic resonance spectroscopy subsequent to malignant transformation of human prostatic epithelial cells. Cancer Res 2001;61:3599–603.
Jadvar H, Gurbuz A, Li X, Shahinian A, Conti PS. Choline autoradiography of human prostate cancer xenograft: effect of castration. Mol Imaging 2008;7:147–52.
Giovacchini G, Picchio M, Coradeschi E, Bettinardi V, Gianolli L, Scattoni V, et al. Predictive factors of [(11)C]choline PET/CT in patients with biochemical failure after radical prostatectomy. Eur J Nucl Med Mol Imaging 2010;37:301–9.
Halestrap AP, Price NT. The proton-linked monocarboxylate transporter (MCT) family: structure, function and regulation. Biochem J 1999;343(Pt 2):281–99.
Oyama N, Kim J, Jones LA, Mercer NM, Engelbach JA, Sharp TL, et al. MicroPET assessment of androgenic control of glucose and acetate uptake in the rat prostate and a prostate cancer tumor model. Nucl Med Biol 2002;29:783–90.
Yu EY, Muzi M, Hackenbracht JA, Rezvani BB, Link JM, Montgomery RB, et al. C11-acetate and F-18 FDG PET for men with prostate cancer bone metastases: relative findings and response to therapy. Clin Nucl Med 2011;36:192–8.
Acknowledgements
We thank Prof. Dr. Karin Haustermans and MSc. Sofie Isebaert. This study was supported by the Molecular Small Animal Imaging Center (MoSAIC) of the K.U.Leuven, Belgium and the Interuniversity Attraction Poles grant (IUAP6/38) is kindly acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Emonds, K.M., Swinnen, J.V., van Weerden, W.M. et al. Do androgens control the uptake of 18F-FDG, 11C-choline and 11C-acetate in human prostate cancer cell lines?. Eur J Nucl Med Mol Imaging 38, 1842–1853 (2011). https://doi.org/10.1007/s00259-011-1861-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-011-1861-6