Abstract
Purpose
ReO −4 has similar kinetics regarding the sodium iodide symporter (NIS) to I− and TcO −4 in NIS-expressing tissue. We investigated the therapeutic potential of 186ReO −4 in NIS-transfected neuroendocrine tumour tissue.
Methods
For experiments, the stably NIS-transfected pancreatic neuroendocrine cancer cell line Bon1C was used. NIS-mediated internalization and externalization experiments in vitro and a biodistribution study in nude mice bearing Bon1C xenografts were performed. A therapy study was also conducted consecutively in nude mice xenografted with Bon1C in which the mice were injected intravenously with Na186ReO4.
Results
In vitro studies showed exponential internalization and efflux kinetics of 186ReO −4 in the cell line. The biodistribution study showed high uptake of 186ReO −4 in NIS-expressing tumours. Tumour growth inhibition was significant after injection of 186ReO4 in two groups of animals treated with activity levels below the determined maximum tolerable activity as compared to controls.
Conclusion
These results indicate that the use of 186ReO −4 in the treatment of NIS-expressing neuroendocrine tumours is feasible and support the concept of using NIS as a therapeutic target for 186ReO −4 .
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Frequently, gastrointestinal and pancreatic neuroendocrine tumours are detected at a very advanced stage. This is due to the general absence of symptoms in the early, still localized stage when surgery alone may be curable. Most neuroendocrine tumours produce peptide hormones including serotonin, gastrin, insulin, vasoactive intestinal peptide, pancreatic polypeptide and substance P, which are catabolized mostly by a first-pass effect in the liver before they can cause systemic symptoms. In the majority of cases, the liver is the first location for metastases from intraabdominal primary tumours. Once the tumour has metastasized into the liver, the secreted endocrine active substances can reach the systemic circulation and cause symptoms. At a metastasized stage, palliative treatment including tumour debulking, liver artery embolization, cytoreductive medication and endocrine therapy with synthetic somatostatin analogues are the current options. It is known that 80–100% of neuroendocrine tumours produce chromogranin A as a specific tumour marker [1–5].
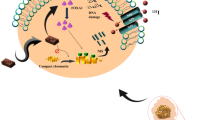
Over recent years, several studies of the structure and function of the sodium iodide symporter (NIS) and its role in the therapy of malignant diseases have been published. Such studies became possible with the cloning of the rat and human forms of this molecule in 1996 [6]. It has been shown that NIS, after transfection, is a target for radioiodide therapy [6, 7]. The transport of two Na+ cations in exchange for one I− anion by the basolateral transmembrane NIS follows the electrochemical gradient created actively by Na+/K+-ATPase [8]. NIS not only transports iodide but also negatively charged ions with a similar ionic radius, such as 99mTcO −4 and 186ReO −4 anions [9–12]. These anions are taken up by the thyroid gland but do not take part in the synthesis of thyroid hormones since they are not subject to organification.
NIS has been used for decades in the diagnosis and therapy of thyroid diseases, e.g. in the treatment of hyperthyroidism and staging and therapy of thyroid carcinoma. In differentiated thyroid tumours, radioiodide therapy is an important routinely performed treatment to eradicate thyroid remnants after surgery as well as to detect and treat metastases [13]. This procedure leads to relapse-free 5-year survival rates of more than 90%. NIS expression has also been detected in extrathyroid tissue including the stomach, salivary glands, lactating breast and potentially even breast cancer [14–16].
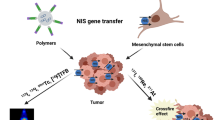
Transfection of NIS-containing vectors into non-NIS-expressing malignancies, followed by radioiodide therapy is an interesting option. The NIS gene has been transfected into various tumour tissues. Several studies have shown that the internalization of radioactive iodide in these cells is up to 225-fold higher than in control cells [17–20]. A therapeutic effect in vivo was demonstrated for the first time by Spitzweg et al. [21], and more recently by our own group [22].
In recent studies, we have demonstrated promising therapeutic results with 131I− and 99mTcO −4 [22], and with respect to the results of Dadachova et al. and Zuckier et al. [12, 23], the aim of this study was to investigate the ability of 186ReO −4 to treat NIS-transfected neuroendocrine tumours in vivo.
Materials and methods
Cell lines
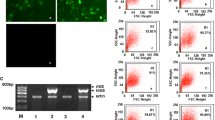
The serotonin-secreting and chromogranin A-expressing neuroendocrine pancreatic carcinoid cell line Bon1 was stably transfected with a plasmid bearing the human NIS gene and a geniticin resistance gene. Expression of the hNIS gene is controlled by the chromogranin A promoter. This transfected cell line was renamed Bon1C (pcDNA 3.1-CgA-NIS), as described previously [24]. NIS expression was proven by RT-PCR, Western blotting and repeated functional assays. The ability to take up 186ReO −4 was tested in in vitro internalization and externalization studies. Internalization and externalization kinetics of 186ReO −4 were similar to those of 131I− and 99mTcO −4 , confirming the findings of Zuckier et al. [23].
Cell culture
Bon1C cells were cultured in Dulbecco’s MEM/Nut mix F12 medium (Gibco BRL, Karlsruhe, Germany) supplemented with l-glutamine, 10% fetal calf serum (Gibco BRL), 100,000 IU/l penicillin, 100 mg/l streptomycin and 400 µg/ml geniticin. Cells were grown at 37°C in an atmosphere of 95% air/5% CO2.
Kinetics of 186ReO −4 uptake
Approximately 4x104 cells were incubated with 185 kBq/ml 186ReO −4 in 1 ml Hank’s balanced salt solution (HBSS) with and without 1 M perchlorate. After 60 min they were washed twice with ice-cold HBSS, lysed in 1 M KOH, and counted using a Cobra II auto-gamma gamma counter (Packard BioScience, Dreieich, Germany) in a 100–180 keV window (γ energy of 186ReO4 about 137 keV). For the internalization studies, 4x104 cells were incubated with 185 kBq/ml 186ReO −4 in 1 ml HBSS for 5, 10, 15, 30, 45, 60, 90 and 120 min [22]. Efflux of 186ReO −4 was investigated by incubating 4x104 cells with 185 kBq/ml 186ReO −4 in 1 ml HBSS for 60 min. Cells were washed twice with ice-cold HBSS and incubated with HBSS for 5, 10, 15, 30, 45, 60, 90 and 120 min before lysis with KOH. Experiments were performed in triplicate [22].
Animal experiments
Animal experiments were conducted in accordance with German law and were reviewed and approved by the local animal protection committee. Athymic nude (Nrc nu/nu) mice at 6–8 weeks of age were obtained from Charles River (Sulzfeld, Germany). The animals were housed under pathogen-free conditions with a 12-h light/12-h dark schedule and fed autoclaved standard food and water ad libitum. For xenografts, 6x106 tumour cells in culture medium were injected into the flanks of the mice.
In vivo biodistribution
Animals were injected with 370 kBq of 186ReO −4 in 0.1 ml 0.9% saline solution into a tail vein. For the biodistribution studies 186ReO −4 was obtained from Covidien Deutschland. Three mice were killed at 30 min, 60 min, 120 min, 360 min, 24 h and 48 h after injection. Tumour, thyroid gland, salivary glands, stomach, liver, kidneys, small intestine, spleen, pancreas, lung, heart, muscle and bone were immediately carefully removed, weighed on an analytic scale and their γ activity counted using a Cobra II auto-gamma gamma counter (Packard BioScience) in a 100–180 keV window. Uptake is expressed as percentage of injected dose per gram (%ID/g) tissue, related to a reference standard of the injected activity.
Radioisotope therapy studies
Nude mice bearing Bon1C xenografts were randomized into six groups after tumour sizes reached 260±30 mm3. Treatment groups were injected with 37 (n=5), 111 (n=5), 185 (n=5), 259 (n=8) and 370 MBq (n=8) 186ReO −4 (Covidien Deutschland) once into a tail vein. Both tumour volume, measured using a microcalliper (volume of a rotation ellipsoid was assumed as height × length × width × 0.5), and body weight were recorded weekly. Mice were killed if their weight loss was more than 30%, or if they showed cachexia and/or signs of infection or weakness, or tumour ulceration or haemorrhagia. In all cases, the study was terminated after 7 weeks.
Statistical analysis
For statistical analysis the software SigmaStat was used. The data were analysed using one-factorial ANOVA. Pair-wise post hoc comparisons were conducted when necessary using Bonferroni tests. For all statistical analyses, p values less than 0.05 were deemed significant. In the figures, values are means, and error bars indicate the standard error of the means (SE).
Results
Kinetics of 186ReO −4 uptake
The Bon1C cell line showed intense uptake of 186ReO −4 . Uptake inhibition by adding perchlorate was tested and proven in the first routine uptake experiments with a 60-min incubation time as described above. The uptake was eightfold higher than in perchlorate-inhibited control cells (data not shown). Internalization was fast, reaching a plateau after 15 min (Fig. 1a). Externalization studies showed a rapid efflux of 186ReO −4 from Bon1C cells with an approximate effective half-life of 5 min (Fig. 1b).
In vivo biodistribution
In this study we investigated the biodistribution and therapeutic value of 186ReO −4 in nude mice bearing the NIS-expressing Bon1C tumour. As expected, 186ReO −4 showed the highest uptake in the thyroid gland. The maximum was reached after 30 min (385±98.3 %ID/g; Fig. 2c). The second highest uptake was in the stomach, also reached after 30 min (18.4±4.4 %ID/g; Fig. 2a). It is remarkable that Bon1C tumour showed a maximum uptake at 120 min and showed the third-highest uptake of all measured organs (9.1±1 %ID/g; Fig. 2b) followed by the salivary glands (6.1±2.7 %ID/g), which showed the highest uptake again after 30 min. The other organs counted showed negligible uptakes due to a lower or no expression of NIS in these organs (Fig. 2a).
The characteristics of the %ID/g curves over time were very similar for each organ except the curve for the tumour. This also means that the thyroid gland did not retain 186ReO −4 , and thus externalizes in the same exponential way as the other organs (Fig. 2c). In contrast, the tumour first showed increasing uptake reaching a maximum after 2 h and subsequently showed less rapid efflux than other organs up to the 24-h time-point (Fig. 2b). After 48 h, every organ showed a %ID/g less than 0.5 except the thyroid gland, in which 5.5±3.9 %ID/g remained due to the high uptake at the beginning of the experiment.
Radioisotope therapy studies
In the therapy study with different activities of 186ReO −4 the maximum tolerable activity in nude mice was considered to be 185 MBq per animal. Tumour growth inhibition and even tumour volume reduction was observed in animals treated with 111, 185, 259 and 370 MBq (Fig. 3). In animals treated with 37 MBq 186ReO −4 , no significant difference in tumour growth compared to the control group was seen. In animals treated with 111 MBq, tumour growth inhibition was significant (p<0.05) as compared to growth in the control group on days 21 and 28. In animals treated with 185 MBq 186ReO −4 tumour volume reduction was significant (p<0.05) as compared to the volume in control group on day 21 and remained significant until day 42 of the study. The activity of 185 MBq 186ReO −4 per mouse was the most effective dose in this study concerning the duration of tumour growth inhibition with a tolerable toxicity. Tumours of animals treated with 259 MBq or 370 MBq 186ReO −4 showed the greatest volume reduction. The activities of 259 MBq and 370 Bq caused severe side effects due to radiation injury which were lethal or fulfilled the criteria for removal of the mice from the study. All animals in these groups died or had to be killed in the first 14 days of the study. These animals showed general weakness and respiratory problems. The macroscopic appearance of the explanted stomach showed signs of radiation gastritis. Weight loss of the mice increased dose dependently: 2.9±1.2%, 4±2.5%, 15.6±12.5%, 14.2±8.1% and 29.2%±11.2% in animals treated with 37, 111, 185, 259 and 370 MBq, respectively.
Discussion
The stably transfected NIS-expressing cell line Bon1C in which NIS expression is controlled by the chromogranin A promoter accumulates 186ReO −4 effectively. Chromogranin A is produced by neuroendocrine tissue as well as by 80–100% of neuroendocrine tumours and is a specific tumour marker [2–4]. The uptake of 186ReO −4 was eightfold higher than in control cells in vitro. This fits the data for 131I and 99mTcO −4 , where the uptake is 52-fold and 18-fold higher, respectively. Internalization and externalization kinetics were rapid and similar to the values found in studies performed with 131I− and 99mTcO −4 [22]. Further studies, which are already in progress, are seeking to elucidate the possibility of extending the intratumoral radioisotope half-life in the therapeutic setting, e.g. by reducing efflux through lithium administration and anion transporter inhibitors [25, 26].
In vivo the NIS-expressing neuroendocrine Bon1C tumours showed strong uptake of 186ReO −4 . As compared to 131I− and 99mTcO −4 (36.1±26.7 %ID/g; 24.6±24.0 %ID/g), the tumour accumulated 15±6 %ID/g 186ReO −4 at peak activity levels. As seen previously, and also previously described by other groups [27–29], the externalization of the radiopharmaceutical out of the tumour was fast. The peak activity was found in every tissue at 30 min with the exception of tumour tissue. In tumour tissue the maximum uptake was reached after 120 min. The prolongation of uptake compared to in vitro experiments can be explained by different geometries regarding the monolayer cell culture and the three-dimensional tumour. Externalized radioisotopes in vitro diffuse off into the incubation medium. In vivo, however, contiguous cells again take up previously externalized anions which correlates with high levels of NIS-expressing cells as well [30]. Besides the thyroid gland, the stomach and salivary glands also strongly internalize radioisotopes due to expression of NIS in these tissues [31–34]. Therefore, toxicity to these organs must be kept in mind for therapeutic studies. The thyroid gland especially is at risk because of the very high uptake and/or accumulation (iodide isotopes) of isotopes transported by NIS. Nevertheless, using isotopes which take no part in the synthesis of thyroid hormones therefore reducing the exposure time of this organ seems to be a valuable approach to reducing radiation injury [12, 35, 36].
We chose 186ReO −4 instead of 188ReO −4 because of the lower β-energy (1.1 MeV vs. 2.1 MeV) of 186ReO −4 . We expected lower toxicity because of the lower range of emitted electrons. In the therapy study with 186ReO −4 significant tumour growth inhibition and even tumour volume reduction were seen in animals treated with 111 MBq and 185 MBq compared to the control group (p<0.05). Mice treated with 37 MBq showed no significant difference in tumour growth compared to the control group. Mice treated with 259 MBq and 370 MBq showed a reduction in tumour volume but all mice in these two groups had to be killed 14 days after injection at the latest because of severe side effects fulfilling the stop criteria. Of the treated animals with NIS-expressing neuroendocrine tumours, 71% showed remission, 6.5% stable disease and 22.5% progressive disease over all groups treated with different activity levels. Of the animals treated with tolerable activities of 186ReO −4 for nude mice (37, 111 and 185 MBq), 53.3% showed regression. The maximum tolerable activity for nude mice is considered to be 185 MBq per animal. In view of the general weakness and respiratory problems of the animals and the macroscopic appearance of the explanted stomach, we consider that the toxicity of 259 MBq and 370 MBq could have been due to myelosuppressive effects of radiation and digestion problems caused by radiation gastritis.
Following our previous results regarding 99mTcO −4 and 131I− [22] showing therapeutic efficacy of these isotopes in NIS-transfected neuroendocrine Bon1C xenografts, we have now demonstrated that NIS-expressing neuroendocrine tumours can at least in principle be treated successfully and effectively using 186ReO −4 .
For clinically suitable therapy options an appropriate vector would be needed. Further studies should focus on in vivo transfections of hNIS controlled and cotransfected with a tissue-specific promoter (CgA) with, for example, adenoviruses as vectors.
References
Oberg K. The ultimate biochemical diagnosis of gastro-enteropancreatic tumours. Digestion 1996;57(Suppl 1):45–7. doi: 10.1159/000201394.
Stridsberg M. The use of chromogranin, synaptophysin and islet amyloid polypeptide as markers for neuroendocrine tumours. Ups J Med Sci 1995;100(3):169–99.
Öberg K. Carcinoid tumours: current concepts in diagnosis and treatment. Oncologist 1998;3(5):339–45.
Janson ET, Holmberg L, Stridsberg M, Eriksson B, Theodorsson E, Wilander E, et al. Carcinoid tumours: analysis of prognostic factors and survival in 301 patients from a referral center. Ann Oncol 1997;8(7):685–90. doi:10.1023/A:1008215730767.
Pucci A, Bartoloni G, Tessitore E, Carney JA, Papotti M. Cytokeratin profile and neuroendocrine cells in the glandular component of cardiac myxoma. Virchows Arch 2003;443(5):618–24. doi:10.1007/s00428-003-0882-3.
Dai G, Levy O, Carrasco N. Cloning and characterization of the thyroid iodide transporter. Nature 1996;379:458–60. doi:10.1038/379458a0.
Smanik PA, Liu Q, Furminger TL, Ryu K, Xing S, Mazzaferri EL, et al. Cloning of the human sodium iodide symporter. Biochem Biophys Res Commun 1996;226:339–45. doi:10.1006/bbrc.1996.1358.
Eskandari S, Loo DD, Dai G, Levy O, Wright EM, Carrasco N. Thyroid Na+/I- symporter mechanism, stoichiometry and specificity. J Biol Chem 1997;272:27230–8. doi:10.1074/jbc.272.43.27230.
Emamian SA, Shalaby-Rana E, Majd M. The spectrum of heterotopic gastric mucosa in children detected by Tc-99m pertechnetate scintigraphy. Clin Nucl Med 2001;26:529–35. doi:10.1097/00003072-200106000-00010.
Berquist TH, Nolan NG, Stephens DH, Carlson HC. Specificity of 99mTc-per-technetate in scintigraphic diagnosis of Meckels diverticulum: review of 100 cases. J Nucl Med 1976;17:465–9.
Meine FJ, Woloshin HJ. Radiologic diagnosis of salivary gland tumours. Radiol Clin North Am 1970;8:475–85.
Dadachova E, Bouzahzah B, Zuckier LS, Pestell RG. Rhenium-188 as an alternative to iodine-131 for treatment of breast tumours expressing the sodium/iodide symporter (NIS). Nucl Med Biol 2002;29:13–8. doi:10.1016/S0969-8051(01)00279-7.
Chow SM, Law SC, Mendenhall WM, Au SK, Chan PT, Leung TW, et al. Papillary thyroid carcinoma: prognostic factors and the role of radioiodine and external radiotherapy. Int J Radiat Oncol Biol Phys 2002;2002(52):784–95. doi:10.1016/S0360-3016(01)02686-4.
De la Vieja A, Dohan O, Levy O, Carrasco N. Molecular analysis of the sodium/iodide symporter: impact on thyroid and extrathyroid pathophysiology. Physiol Rev 2000;80:1083–105.
Tazebay UH, Wapnir IL, Levy O, Dohan O, Zuckier LS, Zhao QH, et al. The mammary gland iodide transporter is expressed during lactation and in breast cancer. Nat Med 2000;6:871–8. doi:10.1038/78630.
Kilbane MT, Ajjan RA, Weetman AP, Dwyer R, McDermott EW, O’Higgins NJ, et al. Tissue iodine content and serum-mediated 125-I uptake-blocking activity in breast cancer. J Clin Endocrinol Metab 2000;85:1245–50. doi:10.1210/jc.85.3.1245.
Cho JY, Xing S, Liu X, Buckwalter TL, Hwa L, Sferra TJ, et al. Expression and activity of human Na+/I- symporter in human glioma cells by adenovirus-mediated gene delivery. Gene Ther 2000;7:740–9. doi:10.1038/sj.gt.3301170.
Boland A, Ricard M, Opolon P, Bidart JM, Yeh P, Filetti S, et al. Adenovirus-mediated transfer of the thyroid sodium/iodide symporter gene into tumours for a targeted radiotherapy. Cancer Res 2000;60:3484–92.
Mandell RB, Mandell LZ, Link CJ Jr. Radioisotope concentrator gene therapy using the sodium/iodide symporter gene. Cancer Res 1999;59:661–8.
Spitzweg C, Zhang S, Bergert ER, Castro MR, McIver B, Heufelder AE, et al. Prostate-specific antigen (PSA) promoter-driven androgen-inducible expression of sodium iodide symporter in prostate cancer cell lines. Cancer Res 1999;59:2136–41.
Spitzweg C, O’Connor MK, Bergert ER, Tindall DJ, Young CY, Morris JC. Treatment of prostate cancer by radioiodine therapy after tissue-specific expression of the sodium iodide symporter. Cancer Res 2000;60:6526–30.
Schipper ML, Riese CG, Seitz S, Weber A, Béhé M, Schurrat T, et al. Efficacy of 99mTc pertechnetate and 131I radioisotope therapy in sodium/iodide symporter (NIS) expressing neuroendocrine tumours in vivo. Eur J Nucl Med Mol Imaging. 2007;34(5):638–50.
Zuckier LS, Dohan O, Li Y, Chang CJ, Carrasco N, Dadachova E. Kinetics of perrhenate uptake and comparative biodistribution of perrhenate, pertechnetate, and iodide by NaI symporter-expressing tissues in vivo. J Nucl Med 2004;45:500–7
Schipper ML, Weber A, Béhé M, Göke R, Joba W, Schmidt H, et al. Radioiodide treatment after sodium iodide symporter gene transfer is a highly effective therapy in neuroendocrine tumour cells. Cancer Res 2003;63(6):1333–8.
Haberkorn U, Beuter P, Kübler W, Eskerski H, Eisenhut M, Kinscherf R, et al. Iodide kinetics and dosimetry in vivo after transfer of the human sodium iodide symporter gene in rat thyroid carcinoma cells. J Nucl Med 2004;45(5):827–33.
Haberkorn U, Henze M, Altmann A, Jiang S, Morr I, Mahmut M, et al. Transfer of the human NaI symporter gene enhances iodide uptake in hepatoma cells. J Nucl Med 2001;42(2):317–25.
Min JJ, Chung JK, Lee YJ, Shin JH, Yeo JS, Jeong JM, et al. In vitro and in vivo characteristics of a human colon cancer cell line, SNU-C5N, expressing sodium-iodide symporter. Nucl Med Biol 2002;29(5):537–45. doi:10.1016/S0969-8051(02)00304-9.
Nakamoto Y, Saga T, Misaki T, Kobayashi H, Sato N, Ishimori T, et al. Establishment and characterization of a breast cancer cell line expressing Na+/I- symporters for radioiodide concentrator gene therapy. J Nucl Med 2000;41(11):1898–904.
Shimura H, Haraguchi K, Miyazaki A, Endo T, Onaya T. Iodide uptake and experimental 131I therapy in transplanted undifferentiated thyroid cancer cells expressing the Na+/I- symporter gene. Endocrinology 1997;138(10):4493–6. doi:10.1210/en.138.10.4493.
Dingli D, Bergert ER, Bajzer Z, O’Connor MK, Russell SJ, Morris JC. Dynamic iodide trapping by tumour cells expressing the thyroidal sodium iodide symporter. Biochem Biophys Res Commun 2004;325(1):157–66. doi:10.1016/j.bbrc.2004.09.219.
Jhiang SM, Cho JY, Ryu KY, De Young BR, Smanik PA, McGaughy VR, et al. An immunohistochemical study of Na+/I- symporter in human thyroid tissue and salivary gland tissues. Endocinology 1998;139:4416–9. doi:10.1210/en.139.10.4416.
Josefsson M, Grunditz T, Ohlsson T, Ekblad E. Sodium/iodide-symporter: distribution in different mammals and role of entero-thyroid circulation of iodide. Acta Physiol Scand 2002;175:129–37. doi:10.1046/j.1365-201X.2002.00968.x.
Dadachova E, Carrasco N. The Na/I symporter (NIS): imaging and therapeutic applications. Semin Nucl Med 2004;34:23–31. doi:10.1053/j.semnuclmed.2003.09.004.
Spitzweg C, Joba W, Eisenmenger W, Heufelder AE. Analysis of human sodium iodide symporter gene expression in extrathyroidal tissues and cloning of its complementary deoxyribonucleic acids from salivary gland, mammary gland, and gastric mucosa. J Clin Endocrinol Metab 1998;83:1746–51. doi:10.1210/jc.83.5.1746.
Petrich T, Helmeke HJ, Meyer GJ, Knapp WH, Pötter E. Establishment of radioactive astatine and iodine uptake in cancer cell lines expressing the human sodium/iodide symporter. Eur J Nucl Med Mol Imaging 2002;29(7):842–54. doi:10.1007/s00259-002-0784-7.
Carlin S, Akabani G, Zalutsky MR. In vitro cytotoxicity of (211)At-astatide and (131)I-iodide to glioma tumour cells expressing the sodium/iodide symporter. J Nucl Med 2003;44(11):1827–38.
Acknowledgments
This study was supported by the Stiftung P.E. Kempkes (Kempkes Foundation) and by grant no. 10-1600-Be2 (T.M.B.) from the Deutsche Krebshilfe (German Cancer Aid).
We thank Birgit Herbst (Department of Nuclear Medicine, Philipps University, Marburg) for expert technical assistance and Claudia Cyborn (Institute for Anatomy and Cell Biology, Philipps University, Marburg) for help with the animal experiments.
Author information
Authors and Affiliations
Corresponding author
Additional information
Christoph Riese and Stephan Seitz contributed equally to this study.
Rights and permissions
About this article
Cite this article
Riese, C.G.U., Seitz, S., Schipper, M.L. et al. Effective treatment of pancreatic neuroendocrine tumours transfected with the sodium iodide symporter gene by 186Re-perrhenate in mice. Eur J Nucl Med Mol Imaging 36, 1767–1773 (2009). https://doi.org/10.1007/s00259-009-1153-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-009-1153-6