Abstract
Objective
To systematically compare the notches of the lateral femoral condyle (LFC) in patients with and without complete tears of the anterior cruciate ligament (ACL) in MR studies by (1) evaluating the dimensions of the lateral condylopatellar sulcus; (2) evaluating the presence and appearance of an extra or a double notch and its association with such tears.
Materials and methods
This retrospective study was approved by our institutional review board, and informed written patient consent was waived. In 58 cases of complete ACL tears and 37 control cases with intact ACL, the number of notches on the LFC was determined, and the depth and anteroposterior (AP) length of each notch were measured in each third of the LFC. The chi-square test, t-test, and logistic regression model were used to analyze demographic data and image findings, as appropriate.
Results
Presence of more than one notch demonstrated a sensitivity of 17.2 %, specificity of 100 %, positive predictive value of 100 %, and negative predictive value of 43.5 % for detecting a complete ACL tear. Lateral third depth measurement (p = 0.028) was a significant associated finding with a complete ACL tear.
Conclusion
A deep notch in the lateral third of the LFC is a significant associated finding with a complete ACL tear when compared with an ACL-intact control group, and the presence of more than one notch is a specific but insensitive sign of such a tear.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The condylopatellar sulcus of the lateral femoral condyle (LFC) is a shallow groove separating the patellar and tibial articular surfaces of the femur [1]. It is located lateral to the most anterior aspect of the intercondylar notch and has a triangular shape with its base lying laterally [2]. It is well seen on conventional lateral radiographs, normally dividing the articular surface of the LFC in half [3]. It is also commonly known as the terminal sulcus.
The presence of a deep lateral sulcus (or notch) has been described on conventional radiographs as an indirect sign of a tear of the anterior cruciate ligament (ACL), representing an osteochondral fracture of the LFC [2, 4] (Fig. 1). The proposed mechanism for this finding is the impaction of the posterior aspect of the lateral tibial plateau on or around the area of the lateral condylopatellar sulcus. A sulcus deeper than either 1.5 or 2.0 mm has been shown as a specific but insensitive radiographic sign of an ACL-deficient knee [2, 4].
Drawing of a sagittal slice of the lateral portion of the knee, representing the hypothetical types of notches that can be found in ACL-torn cases, owing to slightly different impaction patterns: (a) normal notch, the condylopatellar sulcus; (b) a deep notch, owing to an impaction at the site of the condylopatellar sulcus; (c) a long notch; (d) a double notch, both owing to an impaction posterior to the condylopatellar sulcus. Dotted lines indicate the original bone contour
Although MR imaging has been shown to allow detection of osteochondral fractures in the region of the lateral condylopatellar sulcus, including the finding of bone marrow edema, associated with acute trauma [5], to the best of our knowledge, there has been no study that emphasizes the dimensions of the normal or abnormal lateral sulcus, in a fashion similar to what has been done with conventional radiographs. Compared to conventional radiographs, MRI does not magnify structures and, being a multiplanar imaging method, it reduces superimposition and allows observation of the lateral notches in more than one slice, potentially altering the measurements of its dimensions and also potentially altering the previously described association between the deep notches and ACL tears.
Also present in the literature is the designation “abnormal lateral notches” in cases of ACL tears, used to describe bone irregularities or depressions that are seen at a different site or those that extend further posteriorly when compared to the contralateral uninjured knee [6]. No numeric criteria regarding the length of “long notches” exist, however. Anecdotal reports of an extra notch posterior to the lateral condylopatellar sulcus in cases of ACL tears can also be found [7] (Fig. 1).
Even though MR imaging is highly sensitive and specific in the detection of an ACL tear [8, 9], additional indirect signs of such a tear may be particularly useful in the few cases in which direct ligament visualization is not conclusive. Objective criteria for the detection of associated osteochondral fractures may also help in determining their potential role in the pathophysiology of subsequent osteoarthritis [10, 11].
Therefore, the purpose of this study was to systematically compare the notches of the lateral femoral condyle (LFC) in patients with and without complete tears of the anterior cruciate ligament (ACL) in MR studies by (1) evaluating the dimensions of the lateral condylopatellar sulcus and (2) evaluating the presence and appearance of an extra or a double notch and its association with such tears.
Materials and methods
Study population
This retrospective study was approved by our institutional review board, and informed written patient consent was waived. A review of 64 arthroscopically proven cases of complete ACL tears from one fellowship-trained orthopedic surgeon consecutively selected from 2001 to 2005 was undertaken at our own institution. The electronic medical records of all patients were reviewed. Inclusion criterion consisted of confirmation of a complete tear on arthroscopic examination. Exclusion criteria included: (1) prior ACL reconstruction and/or (2) prior history of rheumatologic or musculoskeletal disorders affecting the knee. Injuries were categorized according to the time interval between the injury and the acquisition of the MR images: acute was defined as 0–6 weeks; subacute as 6 weeks to 6 months; chronic as greater than 6 months [12]. Additionally, 37 patients with intact ACL by MR imaging criteria were consecutively selected over a 4-month period from imaging studies done in 2009 or 2010 as the control group. Reasons for imaging were pain in 34 cases, suspected meniscal tear in 7 cases, and a palpable mass in 3 cases (in some cases, more than 1 reason was given). The footprints of the ACL were thoroughly interrogated to prevent the inclusion of cases of chronic scarred ACL-torn cases in this group.
Image acquisition and analysis
All MR imaging examinations were performed with a 1.5-T superconducting magnet (Signa, General Electric Medical Systems) and a quadrature transmit-receive, four-coil phased array extremity coil (Medrad, Indianola, PA). All knees were placed in the neutral position and immobilized with foam pads. Imaging was performed in the coronal, sagittal, and transverse planes. Although several different magnets were employed with minor variations in imaging protocol, a standard MR imaging protocol was used in most cases, which included: axial proton density with fat suppression (TR/TE range 2,500–3,500/12–18), coronal proton density with fat suppression (2,500–3,000/15–19), coronal T1-weighted (400–800/12–20), sagittal T2-weighted (2,500–4,200/62–122), sagittal proton density (2,200–4,000/15–19), and sagittal STIR (3,400–5,500/20–30) sequences. Other imaging parameters included the following: number of excitations, 1; matrix range, 256 × 256 to 512 × 512; field of view range, 12–16 cm; slice thickness range, 2.5–4 mm.
MR images were reviewed by a musculoskeletal radiologist (A.G.) with 4 years of experience and a musculoskeletal radiology research fellow (H.S.) with 1 year of experience. Utilizing sagittal non-fat-suppressed proton density (PD) images, the number of notches on the LFC was determined in consensus. Then, cross-referencing with transverse images, the LFC was divided into lateral, central, and medial thirds, in consensus, and the depth of the notch(es) and its anteroposterior (AP) length were measured independently (Fig. 2). Those measurements were an adaptation of the previous methodology described for conventional radiographs [2]. When a notch was not present, its depth and AP length were recorded as 0. The presence of bone marrow edema around the area of the notches was also recorded by one reader (A.G.). The Osirix v.5.8 Picture Archiving and Communication System was used to review the images.
Statistical analysis
IBM SPSS v21.0 was used for statistical analysis. Descriptive statistics were performed on the study groups and box plots were performed. Demographics between the two groups were compared using an independent samples t-test (age) and chi-square test (gender). Sensitivity, specificity, and positive and negative predictive values were calculated based on the finding of more than one notch. Thereafter, only the measurement of the condylopatellar sulcus was included in the remainder of the analysis for those patients with more than one notch. A two-way mixed intraclass correlation coefficient (ICC) was applied to assess interobserver agreement for each measurement. The ICC ranged from 0 to 1.00, with 0.00 to 0.39 for poor, 0.40 to 0.59 for fair, 0.60 to 0.74 for good, and 0.75 to 1.00 for excellent reliability [13].
Using the average value from both readers, independent samples t-test was used to compare the two groups based on notch dimensions (depth and AP length) in the lateral, central, and medial third regions. Box plots were generated for the significantly different means. Logistic regression analysis was performed using backward model selection to determine the best associated findings with a complete ACL tear.
Results
Demographics and age of injury
Of the 64 cases of arthroscopically proven ACL tears, 6 studies were eliminated because of evidence of prior ACL surgery, resulting in 58 cases (mean age 28.9 years, SD 9.3 years; 18 females, 40 males); in the control group there were 37 cases (mean age 34.0, SD 9.9 years; 20 females, 17 males). There was no statistically significant difference in age between the two groups (p = 0.13). However, the case group had a significantly higher proportion of males (p = 0.03). Regarding age of injury, 19 cases were acute injuries, 8 were subacute, and 10 were chronic. That information was not available in 21 cases.
Presence of multiple notches
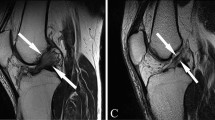
No cases in the control group had more than one notch, whereas 10 out of 58 cases (17.2 %) in the ACL tear group had more than one notch (Fig. 3). Presence of more than one notch demonstrated a sensitivity of 17.2 %, specificity of 100 %, positive predictive value of 100 %, and negative predictive value of 43.5 % for detecting a complete ACL tear.
Notches dimensions
The ICC for both readers is summarized in Table 1. Medial AP length measurement had good reliability. All other measurements had excellent reliability. AP length and depth of notches in both ACL-intact and ACL-torn groups are summarized in Table 2 and Fig. 4. Depth of notches in the lateral, central, and medial thirds was significantly greater for the ACL-torn group (p < 0.05). Differences in AP length were not significant for the lateral and central thirds, but were significant between the two groups for the medial third (p < 0.05). There were no significant differences between males and females for notch depth of the lateral, central, and mid thirds in the control group (p = 0.886, 0.460, and 0.451, respectively), ACL tear group (p = 0.476, 0.166, and 0.178, respectively), and all patients (p = 0.259, 0.236, and 0.133, respectively).
Using backward model selection, the final logistic regression analysis model showed that the lateral third depth measurement (p = 0.028) and medial third AP length (p = 0.005) were significant associated findings with a complete ACL tear. Lateral third depth measurement of 0.7 mm corresponded to a sensitivity of 66 % and specificity of 70 %. Using a measurement of 0.9 mm, specificity increased to 89 %, but sensitivity decreased to 49 %. Medial third AP length of 0.5 cm corresponded to a sensitivity of 60 % and specificity of 81 %.
Presence of bone marrow edema
Bone marrow edema was present beneath the notches in 100 % (19/19) of acute injuries, 37.5 % (3/8) of subacute injuries, 40 % (4/10) of chronic injuries, and 28.5 % (6/21) of cases in which age of injury was unknown.
Discussion
In this study, we have demonstrated that the depth of the lateral condylopatellar sulcus measured on an MR image at the level of the lateral third of the LFC is a significant associated finding with a complete ACL tear, when compared with an ACL-intact control group. We also demonstrated that the presence of more than one notch on the LFC is a very specific indirect sign of a complete ACL tear, although insensitive, when compared with an ACL-intact control group. To the best of our knowledge, this is the first time this association has been demonstrated.
We also demonstrated that the AP length of a sulcus on the medial third of the LFC is a significant associated finding with a complete ACL tear when compared with an ACL-intact control group. However, the evaluation of the articular surface in this third was limited by its oblique orientation, resulting in the occurrence of partial volume-averaging artifacts. As a consequence, there was some disagreement between the observers on the measurements taken, as expressed by the lower, but still acceptable ICC. Additionally, in only a small fraction of the cases, there was a measurable notch in this third, and there was also some disagreement on its assessment (the presence or absence of a notch). Therefore, we believe that results derived from this third of the LFC should be interpreted with caution.
Independent samples t-tests also showed that notch depth in the central and medial thirds was significantly different between ACL-torn and ACL-intact groups; however, logistic regression analysis did not demonstrate this to be a significant associated finding with an ACL tear.
MR imaging is highly sensitive and specific in the detection of an ACL tear [8, 9], but its performance is reported to be slightly worse in chronic cases [14]. One of the factors contributing to this is the scarring patterns of a torn ACL that sometimes simulate an intact ligament with MR imaging [15]. In these cases, utilizing the deep lateral notch as an indirect sign of a ligament tear might prove particularly useful. Also, in many chronic cases, the bone marrow edema that is observed during the acute phase of injury might have resolved [11], and contour abnormalities in the subchondral bone plate might be the only sign that an osteochondral fracture had occurred.
The clinical relevancy of detecting these osteochondral fractures is still debated. There is an association of prior ACL tears and the early onset of osteoarthritis [16, 17], but this association does not seem to be completely explained simply by joint instability caused by ACL insufficiency, because even in ACL-reconstructed knees, early degenerative changes have been observed [18]. Some believe that biomechanical changes in the joint due to alterations in the articular surface caused by these fractures may play a role in the pathophysiology of subsequent osteoarthritis [10, 11].
Surgical treatment for these osteochondral fractures has been proposed, including reduction of the fracture and chondroplasty [10, 19, 20], but this is usually reserved for the more severe cases. Specific criteria for deciding which patients should undergo this type of treatment are yet to be determined. Data gathered in the present study might be useful in designing future prognostic or therapeutic studies addressing these issues.
There were several limitations to this study, the first of them being its retrospective nature. Second, the observers were not blinded to the presence or absence of an ACL tear when reviewing images, which may have resulted in observation bias. It would have been very difficult to blind the observers regarding the status of the ACL, however, as portions of the ligament were clearly visible when the condylar bone surface was being analyzed. Additionally, no age or gender correction was performed when selecting control patients. No sample size calculation was performed prior to patient selection. No surgical confirmation was obtained regarding ACL integrity in the control patients; rather, only MR imaging criteria was used, although it has been shown that these criteria are highly accurate [8, 9]. Care was taken not to include chronic scarred ACL-torn cases in the control group, but it is possible that cases with a chronic ligament tear that had scarred perfectly to the native footprint might have been inadvertently included. The determination of which notch was the true lateral condylopatellar sulcus in double notch cases was done subjectively and, because there are no established criteria to make this determination, there may have been misjudgment in some cases. We did not use any correction factor to account for differences in LFC dimensions among patients, and it is conceivable that the normal lateral condylopatellar sulcus dimensions may vary in differently sized condyles. Finally, the patients included in this study had either a complete tear of the ACL or an intact ACL. Caution should be made when generalizing our results to other groups, such as patients with partial tears of the ACL.
In conclusion, using MR imaging for assessment, a deep notch in the lateral third of the LFC is a significant associated finding with a complete ACL tear, when compared with an ACL-intact control group, and the presence of more than one notch is a specific but insensitive sign of such a tear.
References
Harrison RB, Wood MB, Keats TE. The grooves of the distal articular surface of the femur—a normal variant. AJR Am J Roentgenol. 1976;126(4):751–4.
Cobby MJ, Schweitzer ME, Resnick D. The deep lateral femoral notch: an indirect sign of a torn anterior cruciate ligament. Radiology. 1992;184(3):855–8.
Danzig LA, Newell JD, Guerra Jr J, Resnick D. Osseous landmarks of the normal knee. Clin Orthop Relat Res. 1981;156:201–6.
Yu J, Bosch E, Pathria M, McAndless M, Mishra D, Daniel D, et al. Deep lateral femoral sulcus: study of 124 patients with anterior cruciate ligament tear. Emerg Radiol. 1995;2(3):6.
Kaplan PA, Walker CW, Kilcoyne RF, Brown DE, Tusek D, Dussault RG. Occult fracture patterns of the knee associated with anterior cruciate ligament tears: assessment with MR imaging. Radiology. 1992;183(3):835–8.
Nakauchi M, Kurosawa H, Kawakami A. Abnormal lateral notch in knees with anterior cruciate ligament injury. J Orthop Sci Off J Japan Orthop Assoc. 2000;5(2):92–5.
Garth Jr WP, Greco J, House MA. The lateral notch sign associated with acute anterior cruciate ligament disruption. Am J Sports Med. 2000;28(1):68–73.
Lee JK, Yao L, Phelps CT, Wirth CR, Czajka J, Lozman J. Anterior cruciate ligament tears: MR imaging compared with arthroscopy and clinical tests. Radiology. 1988;166(3):861–4.
Mink JH, Levy T, Crues 3rd JV. Tears of the anterior cruciate ligament and menisci of the knee: MR imaging evaluation. Radiology. 1988;167(3):769–74.
Sadlo PA, Nebelung W. Arthroscopically assisted reduction of a lateral femoral notch in acute tear of the anterior cruciate ligament. Arthrosc J Arthrosc Relat Surg Off Publ Arthrosc Assoc North Am Int Arthroscopy Ass. 2006;22(5):574 e571–573.
Faber KJ, Dill JR, Amendola A, Thain L, Spouge A, Fowler PJ. Occult osteochondral lesions after anterior cruciate ligament rupture. Six-year magnetic resonance imaging follow-up study. Am J Sports Med. 1999;27(4):489–94.
Flint JH, Wade AM, Giuliani J, Rue JP. Defining the terms acute and chronic in orthopaedic sports injuries: a systematic review. Am J Sports Med. 2014;42(1):235–41.
Cicchetti DV. Guidelines, criteria, and rules of thumb for evaluating normal and standardized assessment instruments in psychology. Physchological Assess. 1994;6(4):284–90.
Vahey TN, Broome DR, Kayes KJ, Shelbourne KD. Acute and chronic tears of the anterior cruciate ligament: differential features at MR imaging. Radiology. 1991;181(1):251–3.
Crain EH, Fithian DC, Paxton EW, Luetzow WF. Variation in anterior cruciate ligament scar pattern: does the scar pattern affect anterior laxity in anterior cruciate ligament-deficient knees? Arthroscopy : the journal of arthroscopic & related surgery : official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2005; 21(1):19–24
McDaniel Jr WJ, Dameron Jr TB. Untreated ruptures of the anterior cruciate ligament. a follow-up study. J Bone Joint Surg Am Vol. 1980;62(5):696–705.
McDaniel Jr WJ, Dameron Jr TB. The untreated anterior cruciate ligament rupture. Clin Orthop Relat Res. 1983;172:158–63.
Daniel DM, Stone ML, Dobson BE, Fithian DC, Rossman DJ, Kaufman KR. Fate of the ACL-injured patient. a prospective outcome study. Am J Sports Med. 1994;22(5):632–44.
Garth Jr WP, Wilson T. Open reduction of a lateral femoral notch associated with an acute anterior cruciate ligament tear. Arthrosc J Arthrosc Related Surg Off Publ Arthrosc Assoc North Am Int Arthrosc Assoc. 2001;17(8):874–7.
Tauber M, Fox M, Koller H, Klampfer H, Resch H. Arthroscopic treatment of a large lateral femoral notch in acute anterior cruciate ligament tear. Arch Orthop Trauma Surg. 2008;128(11):1313–6.
Acknowledgments
Eric Y. Chang, MD, gratefully acknowledges grant support from the VA Clinical Science Research and Development Career Development Award (IK2CX000749)
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Grimberg, A., Shirazian, H., Torshizy, H. et al. Deep lateral notch sign and double notch sign in complete tears of the anterior cruciate ligament: MR imaging evaluation. Skeletal Radiol 44, 385–391 (2015). https://doi.org/10.1007/s00256-014-2056-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-014-2056-6