Abstract
Objective:
To describe the imaging findings in eight cases of unilateral tensor fascia lata (TFL) hypertrophy presenting as soft tissue masses.
Design:
Imaging studies and medical charts of eight patients were reviewed retrospectively. The imaging studies included five radiographs, five computed tomography (CT) and six magnetic resonance imaging (MRI) examinations.
Results:
The majority of patients (seven of eight) presented with a palpable proximal anterior thigh mass. One patient was asymptomatic and incidentally diagnosed. There were six females and two males. Ages ranged from 27 to 86 years old (mean 61). MRI and CT showed unilateral enlargement of the TFL muscle in all cases.
Conclusion:
TFL muscle hypertrophy is an uncommon clinical entity, which can simulate a soft tissue tumor. The characteristic appearance on CT or MRI allows a confident diagnosis of muscle hypertrophy to be made, avoiding unnecessary biopsy or surgical intervention.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Muscle hypertrophy presenting as a soft tissue mass has been reported in various muscle groups [1, 2, 3, 4, 5].Unilateral hypertrophy of the tensor fascia lata (TFL) muscle is an uncommon clinical entity and, to our knowledge, has not been described in the literature. We report our experience of eight patients with unilateral hypertrophy of the TFL muscle, seven of whom presented for clinical evaluation of an indeterminate soft tissue mass. Familiarity with the imaging findings of this entity may prevent unnecessary intervention.
Materials and methods
Following approval from our institutional review board, we performed a retrospective computer search for diagnosis of unilateral TFL muscle hypertrophy between April 1987 and June 2001 which revealed eight patients. Subsequently, we reviewed medical charts and imaging studies of these eight patients. Two musculoskeletal radiologists (DEW, HI) reviewed imaging studies by consensus in a non-blinded fashion. There were five radiographs, five computerized tomography (CT) and six magnetic resonance imaging (MRI) studies (Table 1). The diagnosis of TFL hypertrophy was made when there was asymmetric unilateral enlargement of the TFL muscle with at least 50% or greater difference in the transverse dimension of the muscle at the level of the ischial tuberosity. In addition to size, preservation of normal imaging features of skeletal muscle on CT or MRI was used as diagnostic criteria.
Results
Since 1987, there were eight patients (Table 1) diagnosed with unilateral TFL muscle hypertrophy (six females and two males). The ages ranged from 27 to 86 years, with a mean age of 61. The duration of symptoms ranged from 1 month to 13 years (mean 3.7 years) in seven patients. The most common symptom was a “palpable soft tissue mass” in the anterior thigh, noted in seven of eight patients. Associated pain was less common and was present in three of the patients. One patient was asymptomatic and diagnosed incidentally. There was no side predilection, with four cases on the left and four on the right.
Physical examination revealed a mobile elongated anterior thigh mass (Fig. 1A) in all patients, with tenderness in three. On the initial physical examination, muscle hypertrophy was suspected in only one patient: a 27-year-old female with a history of developmental dysplasia of the hip on the same side. Her past medical history was significant for corrective ipsilateral Salter osteotomy 13 years prior to presentation. She reported a slowly enlarging left anterior thigh mass following the surgery. An MRI was obtained to exclude the possibility of a soft tissue neoplasm. In the remaining six patients, a neoplasm was the primary clinical concern. One patient had a past history of melanoma and metastatic disease was suspected. Two patients had contralateral total hip arthroplasties (THA). One of the patients with a THA had a history of familial peripheral neuropathy (Charcot-Marie-Tooth disease).
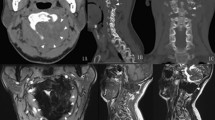
Twenty-seven-year-old female with developmental dysplasia treated with periacetabular osteotomy. Physical examination demonstrated palpable, mobile and non-tender anterior thigh mass, which had been gradually enlarging for 13 years (A). CT (B), axial (C) and coronal T1-weighted MRI (TR 400: TE:14) revealed enlargement of the left TFL muscle
Radiographs were negative in four of five cases. Minimal heterotopic ossification was observed in one patient with a history of remote trauma to the anterior thigh. Both MRI (Figs. 1B, C and 2) and CT (Fig. 3) demonstrated unilateral enlargement of the TFL muscle. The muscle was diffusely enlarged with no focal contour abnormalities. On MRI, the enlarged TFL muscle was isointense to the contralateral TFL on both T1-weighted and T2-weigted images. On axial T1-weighted images, there were small rounded foci of increased signal intensity due to fat interspersed between the muscle fibers with a resultant “marbling” appearance of normal muscle on both the affected and normal sides (Fig. 1C). There was no edema on the T2-weighted images.
Incisional biopsies were performed in the three patients with tenderness in the region of the hypertrophied TFL. The biopsy revealed hypertrophied muscle in one patient, with no evidence of an infiltrative process, confirming the diagnosis of benign hypertrophy. One of the patients presented with a tender anterior thigh mass that had been present for several weeks. The patient was concerned about the possibility of malignancy due to a family history of rhabdomyosarcoma. Biopsy showed necrotizing myopathy with muscle hypertrophy and a diagnosis of focal nodular myopathy was established. The third patient who underwent a biopsy presented with acute onset of subcutaneous masses in her right flank and anterior thigh. Her medical history was significant for being anticoagulated with coumadin. She was referred with a suspicion of a spontaneous hematoma versus neoplasm and biopsy revealed a non-inflammatory myopathic process with hypertrophy of the TFL muscle.
Discussion
A palpable soft tissue mass is a relatively common problem in clinical practice. The differential diagnosis of a focal soft tissue mass is diverse and includes a broad spectrum of tumors and tumor simulators that range from benign and malignant neoplasms to hematomas, abscesses and accessory or hypertrophied muscle. Although CT may provide helpful information, MRI is the imaging modality of choice for evaluating soft tissue lesions, due to its superior soft tissue contrast and multiplanar image capability. In our series, CT examinations were obtained because of availability or due to additional indications (e.g., evaluation of prostate cancer or urolithiasis).
Enlargement of muscles may take two forms: true hypertrophy, which is the result of an increase in size of muscle fibers, or pseudohypertrophy, which is secondary to accumulation of excess fat and connective tissue within the muscle. Pseudohypertrophy is a well-recognized phenomenon in patients with Duchenne and other muscular dystrophies [6, 7, 8, 9]. Pseudohypertrophy of the TFL muscle with fatty infiltration was described by Petersilge et al. [9] in a patient with a history of denervation. In their case, the TFL muscle showed an increase in the amount of fat between the muscle fibers compared with the normal side. On imaging studies, it is helpful to assess the amount of fatty tissue to distinguish pseudohypertrophy from true hypertrophy. Muscle hypertrophy presenting as a soft tissue mass has been reported [1, 5] with various muscle groups such as semimembranosus [2], gastrocnemius [3, 4], soleus [3, 4] and abductor hallucis muscles [10] in the lower extremities. Among these, the most frequently reported has been iliopsoas muscle hypertrophy, which can simulate several different disease processes [11, 12, 13, 14, 15]. In addition to hypertrophy, accessory muscles have also been described in the literature presenting as soft tissue masses [16]. Exercise, denervation, radiation and myopathies are frequently implicated in muscle hypertrophy [3, 17, 18, 19].
In the majority of the patients in this series (six of eight), there was a theoretical explanation for the TFL muscle hypertrophy. Three patients had prior surgical procedures with altered weight bearing mechanics possibly playing a role in the development of their TFL muscle hypertrophy. Two of these patients had a contralateral THA and one had an ipsilateral Salter innominate osteotomy for the treatment of developmental hip dysplasia. One of the patients with a THA had a familial peripheral neuropathy, Charcot-Marie-Tooth disease. Charcot-Marie-Tooth disease is an uncommon autosomal dominant demyelinating sensorimotor neuropathy that usually presents with distal muscle atrophy. Although it is uncommon, muscle hypertrophy at presentation of this disease has been reported in the literature [20]. One of our patients had diabetic peripheral neuropathy and radiculopathy. Two patients had myopathy confirmed with a biopsy.
MR imaging of hypertrophied TFL demonstrates fusiform enlargement of the muscle with a small amount of fat interposed between the muscle fibers. The presence of nodular areas of fat between muscle fibers may suggest the diagnosis of intramuscular hemangioma; the lack of associated tortuous vessels helps to differentiate these two entities. Although hypertrophied TFL can be identified in all planes, axial images provide the most accurate anatomic assessment for confirming the diagnosis.
Three of our patients, all of whom underwent biopsy, had pain in the region of hypertrophied TFL. Two biopsies showed abnormal results in addition to hypertrophied muscle that included “non-inflammatory myopathic process” and “necrotizing myopathy”. The MR imaging studies in these cases demonstrated hypertrophied muscle with no additional signal abnormalities, specifically no muscle edema was present on T2-weighted sequence. To our knowledge, there are no established MRI findings for these entities. The other biopsy revealed normal muscle. Recently, Bass and Connell reported TFL tendonopathy as a cause of anterior groin pain utilizing Ultrasound [21]. None of our patients had tendinous abnormalities on their imaging studies and their pain was confined to the muscle belly.
In conclusion, unilateral hypertrophy of the TFL muscle is an uncommon clinical entity that may simulate a soft tissue tumor. It is usually seen in older female patients. Familiarity with this entity and the characteristic imaging features of TFL hypertrophy on CT or MRI will aid in making an accurate diagnosis and avoiding unnecessary biopsy or surgical intervention.
References
Almansoor J, Boothroyd AE, Carty H. Asymmetrical muscle hypertrophy simulating a localized soft tissue mass. J Pediatr Orthop B 1998; 7:86–88.
Carroza M, Giombini A, Dragoni S, De Carolis M, Bizzari F. Localised hypertrophy of semimembranous muscle. A report of two cases in athletes. J Sports Med Phys Fitness 2001; 41:415–418.
Cooper W, Ringel S, Treihaft MM, Hall KA. Calf enlargement from S1 radiculopathy. J Neurosurg 1985; 62:442–444.
De Beuckeleer L, Vanhoenacker F, De Schepper Jr, Seynaeve P, De Schepper A. Hypertrophy and pseudohypertrophy of the lower leg following chronic radiculopathy and neuropathy: imaging findings in two patients. Skeletal Radiol 1999; 28:229–32.
Riefkohl R, Georgiade GS, Georgiade NG. Masseter muscle hypertrophy. Ann Plast Surg 1984; 12:528–532.
Heitmann C, Pelzer M, Menke H, Germann G. The free musculocutaneous tensor fascia lata flap as a backup procedure in tumor surgery. Ann Plast Surg 2000; 45:399–404.
Koshima I, Urushibara K, Inagawa K, Moriguchi T. Free tensor fascia lata flap for the reconstruction of defects in extremities. Plast Reconstr Surg 2001; 107:1759–1765.
Mettlin C, Priore R, Rao U, Gamble D, Lane W, Murphy GP. Results of the national soft-tissue sarcoma registry: analysis of survival and prognostic factors. J Surg Onc 1982; 19:224–227.
Petersilge CA, Pathria MN, Gentili A, Recht MP, Resnick D. Denervation hypertrophy of muscle: MR features. J Comput Assist Tomogr 1995; 19:596–600.
Ringelman PR, Goldberg NH. Hypertrophy of the abductor hallicus muscle: an unusual congenital foot mass. Foot Ankle 1993; 14:366–369.
Duprat G Jr, Levesque HP, Seguin R, Nemeeh J, Sylvestre J. Bowel displacement due to psoas muscle hypertrophy. J Can Assoc Radiol 1983; 34:64–65.
Haines JO, Kyaw MM. Anterolateral deviation of ureters by psoas muscle hypertrophy. J Urol 1971; 106:831–832.
McLoughlin MJ. Psoas hypertrophy mimicking retroperitoneal fibrosis. J Can Assoc Radiol 1981; 32:56–57.
Zeiss J, Smith RR, Taha AM. Iliopsoas hypertrophy mimicking acute abdomen in a bodybuilder. Gastrointest Radiol 1987; 12:340–342.
Ziter FM. Unilateral ureteral deviation due to unilateral iliopsoas muscle hypertrophy. J Can Assoc Radiol 1974; 25:327–328.
Palaniappan M, Rajesh A, Rickett A, Christopher JK. Accessory soleus muscle: a case report and review of the literature. Pediatr Radiol 2000; 29:610–612.
Korczyn AD, Kuritzky A, Sandbank U. Muscle hypertrophy with neuropathy. J Neurol Sci 1978; 38:399–408.
Serratice G, Sangla I, Pouget J, Azulay JP. Association of post-radiation focal muscular atrophy and hypertrophy. Rev Neurol (Paris) 1993; 149:812–814.
Liu GC, Jong YJ, Chiang CH, Jaw TS. Duchenne muscular dystrophy: MR grading system with functional correlation. Radiology 1993; 186:475–480.
Krampitz DE, Wolfe GI, Fleckenstein JL, Barohn RJ. Charcot-Marie-Tooth disease type 1 presenting as calf hypertrophy and muscle cramps. Neurology 1998; 51:1508–1509.
Bass CJ, Connell DA. Sonographic findings of tensor fascia lata tendinopathy: another cause of anterior groin pain. Skeletal Radiol 2002; 31:143–148.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ilaslan, H., Wenger, D.E., Shives, T.C. et al. Unilateral hypertrophy of tensor fascia lata: a soft tissue tumor simulator. Skeletal Radiol 32, 628–632 (2003). https://doi.org/10.1007/s00256-003-0687-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-003-0687-0