Abstract
We evaluated the relationship between regional cerebral oxygen saturation (rSO2) measured by near-infrared spectroscopy (NIRS) cerebral oximeter with superior vena cava (SVC), inferior vena cava (IVC), right atrium (RA), and pulmonary artery (PA) saturation measured on room air and 100% inspired oxygen administered via a non-rebreather mask (NRB) in children. Twenty nine pediatric post-orthotopic heart transplant patients undergoing an annual myocardial biopsy were studied. We found a statistically significant correlation between rSO2 and SVC saturations at room air and 100% inspired oxygen concentration via NRB (r = 0.67, p = 0.0002 on room air; r = 0.44, p = 0.02 on NRB), RA saturation (r = 0.56, p = 0.002; r = 0.56, p = 0.002), and PA saturation (r = 0.67, p < 0.001; r = 0.4, p = 0.03). A significant correlation also existed between rSO2 and measured cardiac index (r = 0.45, p = 0.01) and hemoglobin levels (r = 0.41, p = 0.02). The concordance correlations were fair to moderate. Bias and precision of rSO2 compared to PA saturations on room air were −0.8 and 13.9%, and they were 2.1 and 15.6% on NRB. A stepwise linear regression analysis showed that rSO2 saturations were the best predictor of PA saturations on both room air (p = 0.0001) and NRB (p = 0.012). In children with biventricular anatomy, rSO2 readings do correlate with mixed venous saturation.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Jobsis [15] was the first to describe the use of near-infrared spectroscopy (NIRS) technology in humans when he detected transmission of photons through the brain tissue. Since then, the NIRS-based technology has found diverse applications in monitoring of deltoid muscle oxygen supply to guide resuscitation [30], monitoring of splanchnic circulation in neonates with acute abdomen [10, 43, 47], and in measuring regional blood supply in skeletal muscles to assess the effects of exercise [5, 8].
However, the most common application of this technology has been in assessing regional cerebral saturation. This application stems from multiple studies that have shown a positive correlation between cerebral oxygenation as measured by NIRS and jugular venous saturation (SjVO2) [1, 2, 12, 19, 28, 29, 35, 36, 38]. Clinical studies in adults have suggested that a decline in regional cerebral oxygen saturation (rSO2) values of >20% from baseline or absolute values of less than 50 are associated with decreased cognitive function and prolonged intensive care unit (ICU) stay [6, 31]. Such a sharp decline from a baseline measurement or a low absolute value may affect long-term neurological outcome.
As many as 50% of neonatal patients undergoing cardiac surgery on cardiopulmonary bypass (CPB) are at risk for developing mild ischemic lesions, primarily in the form of Periventricular Leukomatacia (PVL), postoperatively [26]. Therefore, a monitor that allows clinicians to follow trends in cerebral oxygenation could identify critical periods associated with inadequate oxygenation [1, 2, 33], which in turn could lead to early interventions to minimize such periods. After initially being utilized in operating rooms [3], it is now increasingly being used as a non-invasive method to monitor regional oxygen saturation during the postoperative period after cardiac surgery [32, 46], and some authors have suggested that rSO2 should be routinely used to guide therapy to minimize periods of low oxygen delivery [13].
However, previously published studies show a correlation between rSO2 and mixed venous saturation (SmVO2) in patients with a variety of congenital heart diseases with different anatomy and physiology, surgical course, postoperative respiratory and hemodynamic support, and measurement sites for mixed venous saturations. Thus, the results from these studies cannot be generalized to other clinical settings.
In order to minimize some of this variability, we designed a prospective study to examine the relationship between rSO2 and saturations measured in the superior vena cava (SVC) and right atrium (RA) (also known as central venous saturations or ScVO2) and pulmonary artery (PA) (SmVO2), both on room air and on 100% inspired oxygen administered via a non-rebreather mask. Our study population included patients with biventricular anatomy who were undergoing routine cardiac catheterization for annual biopsies after orthotopic heart transplant.
Materials and Methods
Study Population
Twenty-nine pediatric patients who had previously undergone an orthotopic heart transplant and were undergoing cardiac catheterization for a routine annual myocardial biopsy or for hemodynamic measurement were recruited for this study prospectively. The institutional review board of the University of Arkansas for Medical Sciences approved this study. The study was performed in the cardiac catheterization laboratory at Arkansas Children’s Hospital. Informed consent was obtained from the patients’ legal guardians and patient assent from children older than 7 years.
Cerebral Oximeter
The continuous, non-invasive cerebral oximeter uses NIRS technology to measure regional changes in oxygenated and deoxygenated hemoglobin in the brain. It does this by emitting light of two different wavelengths (730 and 810 nm), which corresponds to the spectral absorption of oxygenated and deoxygenated hemoglobin. Light in the visible spectrum (400–700 nm) is highly absorbed and can penetrate only go a few millimeters into tissue [8]. Light in the near infrared spectrum (700–1100 nm) undergoes the least amount of absorption and scattering and can thus travel for long distances through biological materials [15]. Deoxygenated hemoglobin absorbs light in the range of 760 nm or lower, whereas both deoxygenated and oxygenated hemoglobin absorb light at 800 nm [27]. Thus, the passage of light of two different wavelengths can allow the opportunity to assess the quantitative changes in the concentrations of these molecules.
The INVOS 5100B cerebral oximeter (Somanetics, Troy, MI, USA) was purchased for use in this study through an intramural grant. The sensors were placed on each side of the patient’s forehead, with the lower edge above the patient’s eyebrows and the medial edge of the sensor in the midline as per the manufacturer’s specifications. No data obtained by this device were used for making clinical decisions.
Data Collection
During these routine cardiac catheterizations, blood samples were collected in capillary tubes from the SVC, inferior vena cava (IVC), RA, and PA to measure oxygen saturations and hemoglobin while the patient was breathing room air using the GEM OPL oximeter (Instrumentation Laboratory, Lexington, MA, USA). In addition, thermodilution measurements to assess the cardiac index (CI) were performed. We also obtained the saturation measurements from sites previously mentioned on 100% fractional inspired oxygen (FiO2) administered through a non-rebreather mask (NRB). Measurements were taken after patients had been on oxygen for 5 minutes. This was done to assess whether the NIRS monitor continues to have a good correlation under hyperoxic conditions. The blood samples for measurements of oxygen saturations were obtained from the same anatomical site in each of the patients when sampling the IVC, SVC, RA, and PA.
Data were collected by the primary investigator (PI) or a co-investigator. Data collected included baseline rSO2 values and rSO2 values every 2 minutes on room air and 100% FiO2 via NRB mask. In addition, simultaneous rSO2 values and oxygen saturation from the sites mentioned previously were collected. The CI was determined by thermodilution method. We collected other information, including patient’ age, sex, weight, height, medical diagnoses, baseline vital signs, and vital signs every 2 minutes during the procedure (heart rate, respiratory rate, blood pressure, and systemic oxygen saturations).
Data were entered in a Microsoft Excel spreadsheet designed for this study. This spreadsheet was only accessible to the PI or the co-investigators.
Statistical Analysis
Descriptive statistics were performed on the demographic data. We calculated the Pearson’s correlation between the rSO2 values and the measured saturations at the same time points. Statistical significance was set at p values of <0.05. We also calculated Pearson’s correlation, which tests whether the line of fit has a slope different from zero, and Lin’s concordance correlation, which tests whether the line of fit has a slope different from identity (line of perfect agreement). Bland–Altman plots, which illustrate the difference versus the average of the two methods [4], were used to estimate the precision and bias of the study variables.
In addition, a linear regression analysis with stepwise variable selection was performed. Dependent variables included the SVC, IVC, RA, and PA saturations, whereas the independent variables included age, sex, systolic blood pressure percentile (adjusted for height), hemoglobin, pulse oximeter values, rSO2 and cardiac index. A p value of 0.2 was used to enter the model, and a 0.1 cut off was used to be removed from the model.
Data were analyzed using SAS version 8.2.
Results
Of 29 patients, 13 (45%) were female and 16 (55%) were male. Twenty-two patients (76%) were Caucasian and 7 non-Caucasian. The mean age was 8 years, 7 months, with a range of 15 months to 17 years, 6 months. The mean weight was 28 kg (range, 8.2–70 kg).
Using Pearson’s correlation, we found a statistically significant correlation between rSO2 and the SVC saturation (r = 0.65, p = 0.0003 on room air; r = 0.44, p = 0.02 on NRB mask), RA (r = 0.56, p = 0.002; RA r = 0.57, p = 0.002), and PA (r = 0.67, p < 0.001, r = 0.4, p = 0.03) at room air and NRB mask, respectively. A significant correlation also existed between rSO2 and measured cardiac index (CI) (r = 0.45, p = 0.01) and hemoglobin (r = 0.41, p = 0.02). No statistically significant correlation was found between rSO2 and IVC saturation (r = 0.32, p = 0.13 on room air; r = −0.32, p = 0.14 on NRB mask). The Pearson’s and Lin’s correlations between PA and SVC, RA, and IVC on room air and NRB are shown in Table 1.
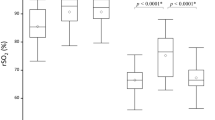
The Lin’s concordance correlation coefficients for SVC, IVC, RA, and PA saturation measurements with rSO2 on room air and oxygen are shown in Fig. 1. Using the scale proposed by Landis and Koch [24], the strength of agreement ranges between fair to moderate. The Bland–Altman plots showing the bias and precision are shown in Fig. 2.
(A) Lin’s concordance correlation calculated on room air for superior vena cava (SVC) saturation compared to rSO2 was 0.55 (95% CI 0.28–0.74); the concordance correlation for right atrium (RA) saturation was 0.49 (95% CI 0.2–0.7) that for interior vena cava (IVC) saturation was 0.31 (95% CI 0.09–0.63), and that for pulmonary artery (PA) saturation was 0.53 (95% CI 0.31–0.69). (B) Lin’s concordance correlation calculated on 100% oxygen administered via a non-rebreather mask for SVC saturation compared to rSO2 was 0.38 (95% CI 0.05–0.64); the concordance correlation RA saturation was 0.42 (95% CI 0.15–0.64); IVC saturation was −0.3 (95 % CI −0.6–0.09), and that for PA saturation was 0.36 (95% CI 0.03–0.61)
(A) The bias and precision (twice the standard deviation of the error) of rSO2 when compared on room air with superior vena cava (SVC) saturation were 1.9 and and 14.4%; the bias and precision in comparison with right atrium (RA) saturation were 0.48 and 14.7% those in comparison with interior vena cava (IVC) saturation −0.9 and 22%, and those in comparison with pulmonary artery (PA) saturation were −0.8 and 13.9%. (B) The bias and precision (twice the standard deviation of the error) of rSO2 when compared on 100% oxygen administered via a non -rebreather mask with SVC saturation were 3.9 and 15.7%; the bias and precision in comparison with RA saturation were 3.5 and 13.9%, those in comparison with IVC saturation were 1.6 and 32%, and those in comparison with PA saturation were 2.1 and 15.6%
The stepwise linear regression analysis was performed to examine the variables that best predict PA saturations. Age, sex, systolic blood pressure percentile (adjusted for height), hemoglobin, pulse oximeter values, rSO2, and cardiac index were used in the model. The best predictor of PA saturation was rSO2 on both room air (p = 0.001) and NRB (p = 0.012). The only other statistically significant predictor of PA saturation on room air was pulse oximeter value (p = 0.03), whereas hemoglobin level was the only other significant predictor on NRB (p = 0.04).
Discussion
Our study shows that the NIRS cerebral oximeter readings do correlate with SmVO2 both on room air and on 100% inspired oxygen administered via NRB mask. Although the absolute rSO2 values are different from SmVO2 because of the regional nature of monitoring, the mix of arterial and venous blood being monitored, and the physical properties of near infrared light, they trend in the same direction as the ScVO2 and SmVO2. We show a fair to moderate agreement of rSO2 values with ScVO2 and SmVO2 on both room air and 100% inspired oxygen delivered via NRB mask in postcardiac transplant patients with no intracardiac shunting. However, the correlation between rSO2 and SmVO2 is better on room air than on NRB, and variance in mixed venous saturation accounted for the largest source of variance in rSO2. Furthermore, the bias and precision of rSO2 values compared to SmVO2 and ScVO2 in our study (see Fig. 2) were similar to the measurements obtained in other studies [19, 46]. The bias between rSO2 and SmVO2 in our study is small, signifying that the difference between the averages of rSO2 values and the measured values was small, whereas the large precision signifies the variability between the rSO2 readings, which can result from changes in physiological states or changes in the measuring instrument.
The results of our study confirm findings of other published studies on postoperative patients. Tortoriello et al. [46] reported a Spearman’s correlation of 0.67 between rSO2 and SmVO2 measured in the SVC or PA. They published a study of 20 patients with a variety of congenital cardiac lesions who underwent biventricular repair or single ventricle palliation. Nagdyman et al. [32] compared rSO2 values with saturations measured in the RA in children who underwent repair of noncyanotic congenital heart lesions and found a significant correlation (r = 0.52) between rSO2 and SvO2. However, these investigators did not measure saturations at any other site or under varying conditions of inspired oxygen.
SmVO2 reflects a global balance between oxygen delivery and tissue oxygen demands. A decrease in SmVO2 reflects either a decrease in oxygen delivery or an increase in tissue oxygen demands. Current continuous SmVO2 monitors use infrared oximetery to detect oxygenated hemoglobin. However, these monitors are placed invasively in the pulmonary artery, which limits their clinical application in children. As an alternative, central venous oxygen saturation measured via catheters placed in the SVC or RA is often used. This technique, although invasive, is more easily achieved due to routine placement of central venous catheters in ICU patients. Rivers et al. [40] have summarized the numerous studies done to evaluate the correlation between ScVO2 and SmVO2 and concluded that ScVO2 is a satisfactory substitute for SmVO2. Although the absolute values of ScVO2 and SmVO2 may differ, they track each other closely under both physiologic and pathologic conditions [25, 39]. When SmVO2 remains persistently low, tissue hypoxia and lactic acidosis develop [17, 40]. SmVO2 monitoring is used extensively in a multitude of clinical scenarios in both adults and children to monitor the relationship between oxygen delivery and tissue oxygen demand [7, 14, 18, 20–22, 34, 37, 41, 42].
Multiple studies have shown that SmVO2 values do not correlate well with IVC saturations in children [9, 44, 45]. Our study results also confirm the findings from these prior investigations.
The limitations of NIRS technology include absorption of 10–15% of the emitted light by extralcranial tissue and skull [11, 15, 27]. However, the degree of absorption of emitted light by the extracranial tissue and skull may vary with patient age. In infants and younger children, this light absorption may be smaller because the light can penetrate into deeper tissues compared to older children. Photons get absorbed in larger blood vessels, whereas light passing through small vessels is absorbed to a very small degree. Therefore, NIRS predominantly detects changes in tissue oxygenation at the level of capillaries, venules, arterioles, and the intracellular compartment [27]. The biologic variations in transcranial optical path length and cerebral hemoglobin concentration between subjects may also introduce potential sources of error and variability [23].
The validity of comparing rSO2 and SjVO2 has been questioned by some investigators [38] because SjVO2 measures saturation in the venous compartment, whereas rSO2 measures saturation in arteries, capillaries, and veins. The rSO2 values displayed are based on the assumption that cerebral tissue contains arterial and venous blood distributed in a 1:3 ratio. Watzman et al. [48] have shown that the contribution of arterial and venous blood may vary between 40:60 and 0:100, respectively. However, blood in the venous compartment does account for the majority of the hemoglobin measured by NIRS technology. rSO2 values do change appropriately with changes in inspired oxygen concentration. A decrease in arterial and venous saturations was seen in studies on healthy volunteers who were administered a hypoxic gas mixture [28, 35].
Our investigation is limited to studying only two different clinical conditions (room air and NRB mask). We did not perform our study over a range of varying FiO2 concentrations. We found that the correlation and agreement between rSO2 and PA were higher on room air and worsened on NRB mask. This was true for the relationship between the PA and ScVO2 as well. Hemoglobin concentration becomes more significant as a predictor of rSO2 when breathing inspired oxygen. It is possible that the increased FiO2 delivered via NRB mask may have altered the distribution ratio of blood between the venous and arterial compartments in the cerebral circulation. This may have led to a decrease in correlation and agreement between rSO2 and SmVO2 in our study [48]. Another limitation of our study is that we did not measure PaCO2 levels, which can significantly alter cerebral blood flow [16, 36], or investigate the effects of hyper or hypo ventilation on rSO2 and the effects on correlation with various measured saturation values in our study subjects. We assumed that for the duration of the procedure, the PaCO2 values would remain unchanged. Our study population did not include neonates and infants.
Conclusions
In children with no intracardiac shunts, who have no obvious cerebral injury or evidence of inadequate systemic oxygen delivery, continuous rSO2 measured using the noninvasive NIRS monitor shows correlation and agreement with mixed venous saturations. This agreement is stronger on room air than on 100% inspired oxygen. Therefore, rSO2 measurements can be used as a monitor for trends in mixed venous saturations. However, this should be used keeping in mind the limitations of this technique.
References
Abdul-Khaliq H, Schubert S, Troitzsch D, et al. (2001) Dynamic changes in cerebral oxygenation related to deep hypothermia and circulatory arrest evaluated by near-infrared spectroscopy. Acta Anaesth Scand 45:696–701
Abdul-Khaliq H, Troitzsch D, Schubert S, et al. (2002) Cerebral oxygen monitoring during neonatal cardiopulmonary bypass and deep hypothermic circulatory arrest. Thorac Cardiovasc Surg 50:77–81
Andropoulos DB, Stayer SA, Diaz LK, Ramamoorthy C (2004) Neurological monitoring for congenital heart surgery. Anesth Analg 99:1365–1375
Bland JM, Altman DG (1999) Measuring agreement in method comparison studies. Stat Methods Med Res 8:135–160
Boushel R, Langberg H, Olesen J, et al. (2000) Regional blood flow during exercise in humans measured by near-infrared spectroscopy and indocyanine green. J Appl Physiol 89:1869–1878
Casati A, Fenelli G, Pietropaoli P, Proeittu R (2004) Paper presented at the American Society of Anesthesiologists annual meeting, Las Vegas, NV
de la Rocha AG, Edmonds JF, Williams WG, Poirier C, Trusler RN (1978) Importance of mixed venous oxygen saturation in the care of critically ill patients. Can J Surg 21:227–229
Edwards AD, Richardson C, Van der Zee P, et al. (1993) Measurement of hemoglobin flow and blood flow by near-infrared spectroscopy. J Appl Physiol 75:1884–1889
Fernandez EG, Green TP, Sweeney M (2004) Low inferior vena caval catheters for hemodynamic and pulmonary function monitoring in pediatric critical care patients. Pediatr Crit Care Med 5:14–18
Fortune PM, Wagstaff M, Petros AJ (2004) Cerebro-splanchnic oxygenation ratio (CSOR) using near infrared spectroscopy may be able to predict splanchnic ischaemia in neonates. Intensive Care Med 27:1401–1407
Hampson NB, Piantadosi CA (1998) Near infrared monitoring of human skeletal muscle oxygenation during forearm ischemia. J Appl Physiol 64:2449–2457
Henson LC, Calalang C, Temp JA, Ward DS (1998) Accuracy of a cerebral oxmieter in healthy volunteers under conditions of isocapnic hypoxia. Anesthesiology 88:58–65
Hoffman GM, Mussatto KA, Brosig CL, et al. (2005) Systemic venous oxygen saturation after the Norwood procedure and childhood neurodevelopmental outcome. J Thorac Cardiovasc Surg 130:1094–1100
Inomata S, Nishikawa T, Taguchi M (1994) Continuous monitoring of mixed venous oxygen saturation for detecting alterations in cardiac output after discontinuation of cardiopulmonary bypass. Br J Anaesth 72:11–16
Jobsis FF (1977) Non-invasive, infra-red monitoring of cerebral O2 sufficiency, blood volume HbO2-Hb shifts and blood flow. Acta Neurol Scand Suppl 64:452–453
Kaiser JR, Gauss CH, Williams DK (2004) Surfactant administration acutely affects cerebral and systemic hemodynamics and gas exchange in very-low-birth-weight infants. J Pediatr 144:809–814
Kasnitz P, Druger GL, Yorra F, Simmons DH (1976) Mixed venous oxygen tension and hyperlactatemia. Survival in severe cardiopulmonary disease. J Am Med Assoc 236:570–574
Kazarian KK, Del Guercio LR (1980) The use of mixed venous blood gas determinations in traumatic shock. Ann Emerg Med 9:179–182
Kim MB, Ward DS, Cartwright CR, et al. (2000) Estimation of jugular venous O2 saturation from cerebral oximetry or arterial O2 saturation during isocapnic hypoxia. J Clin Monit Comput 16:191–199
Krauss XH, Verdouw PD, Hughenholtz PG, Nauta J (1975) Online monitoring of mixed venous oxygen saturation after cardiothoracic surgery. Thorax 30:636–643
Kremzar B, Spéac-Marn A, Kompan L, Cerovic O (1997) Normal values of SvO2 as therapeutic goal in patients with multiple injuries. Intensive Care Med 23:65–70
Krivec B, Vogá G, Podbregar M (2004) Monitoring mixed venous oxygen saturation in patients with obstructive stock after massive pulmonary embolism. Wiener Klin Wochenschrift 116:326–331
Kurth CD, Steven JL, Montenegro LM, et al. (2001) Cerebral oxygen saturation before congenital heart surgery. Ann Thorac Surg 72:187–192
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Lee J, Wright F, Barber R, Stanley L (1972) Central venous oxygen saturation shock: a study in man. Anesthesiology 36:472–478
Mahle WT, Tavani F, Zimmerman RA, et al. (2002) An MRI study of neurological injury before and after congenital heart surgery. Circulation 106:I109–I114
Mancini DM, Bolinger L, Li H, et al. (1994) Validation of near-infrared spectroscopy in humans. J Appl Physiol 77:2740–2747
McCormick PW, Stewart M, Goetting MG, Balakrishnan G (1991) Regional cerebrovascular oxygen saturation measured by optical spectroscopy in humans. Stroke 22:596–602
McCormick PW, Stewart M, Goetting MG, et al. (1991) Noninvasive cerebral optical spectroscopy for monitoring cerebral oxygen delivery and hemodynamics. Crit Care Med 19:89–97
McKinley BA, Marvin RG, Cocanour CS, Moore FA (2000) Tissue hemoglobin O2 saturation during resuscitation of traumatic shock monitored using near infrared spectrometry. J Trauma-Injury Infect Crit Care 48:637–642
Monk T, Weldon J, Van der Aa M (2002) Paper presented at the American Society of Anesthesiologists annual meeting, Orlando, Fl
Nagdyman N, Fleck T, Barth S, et al. (2004) Relation of cerebral tissue oxygenation index to central venous oxygen saturation in children. Intensive Care Med 30:468–471
Nollert G, Jonas RA, Reichart B (2000) Optimizing cerebral oxygenation during cardiac surgery: a review of experimental and clinical investigations with near infrared spectrophotometry. Thorac Cardiovasc Sur 48:247–253
O’Connor TA, Hall RT (1994) Mixed venous oxygenation in critically ill neonates. Crit Care Med 22:343–346
Pollard V, Prough DS, DeMelo AE, et al. (1996) Validation in volunteers of a near-infrared spectroscope for monitoring brain oxygenation in vivo. Anesth Analg 82:269–277
Pollard V, Prough DS, DeMeIo AE, et al. (1996) The influence of carbon dioxide and body position on near infrared spectroscopic assessment of cerebral hemoglobin oxygen saturation. Anesth Analg 82:278–287
Powelson J, Maini BS, Bishop RL, Sottile FD (1992) Continuous monitoring of mixed venous oxygen saturation during aortic operations. Crit Care Med 20:332–336
Prough DS, Pollard V (1995) Cerebral near-infrared spectroscopy: ready for prime time? Crit Care Med 23:1624–1626
Reinhart K, Rudolph T, Bredle DL, Hannemann L, Cain SM (1989) Comparison of central-Venous to mixed-venous oxygen saturation during changes in oxygen supply/demand. Chest 95:1216–1221
Rivers EP, Ander DS, Powell D (2001) Central venous oxygen saturation monitoring in the critically ill patient. Curr Opin Crit Care 7:204–211
Schranz D, Schmitt S, Oelert H, et al. (1989) Continuous monitoring of mixed venous oxygen saturation in infants after cardiac surgery. Intensive Care Med 15:228:232
Sumimoto T, Takayama Y, Iwasaka T, et al. (1991) Mixed venous oxygen saturation as a guide to tissue oxygenation and prognosis in patients with acute myocardial infarction. Am Heart J 122:27–33
Teller J, Wolf M, Keel M, et al. (2000) Can near infrared spectroscopy of the liver monitor tissue oxygenation? Eur J Pediatr 159:549
Thayssen P, Klarholt E (1980) Relation between caval and pulmonary artery oxygen saturation in children. Br Heart J 43:574–578
Thomsen A (1978) Calculation of oxygen saturation of mixed venous blood in infants. Scand J Clin Lab Invest 38:389–392
Tortoriello T, Stayer SA, Mott AR, et al. (2005) A noninvasive estimation of mixed venous oxygen saturation using near-infrared spectroscopy by cerebral oximetry in pediatric cardiac surgery patients. Pediatr Anaesth 15:495–503
Varela JE, Cohn SM, Giannotti GD, et al. (2001) Near-infrared spectroscopy reflects changes in mesenteric and systemic perfusion during abdominal compartment syndrome. Sur 129:363–370
Watzmam HM, Kurth CD, Montenegro LM (2000) Arterial and venous contributions to near-infrared cerebral oximetry. Anesthesiology 93:947–953
Acknowledgment
This work was supported by the University of Arkansas for Medical Sciences College of Medicine Dean’s CUMG/Research Development Fund Grant Program.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bhutta, A.T., Ford, J.W., Parker, J.G. et al. Noninvasive Cerebral Oximeter as a Surrogate for Mixed Venous Saturation in Children. Pediatr Cardiol 28, 34–41 (2007). https://doi.org/10.1007/s00246-006-1379-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-006-1379-z