Abstract
Introduction
An important pathological feature of idiopathic normal pressure hydrocephalus (iNPH) is a dysfunction of cerebrospinal fluid dynamics. Considering the delicate olfactory structures it appears possible that the olfactory bulb (OB) is compromised by this disease. Reports on the anatomy of the olfactory bulb and smell function in patients with idiopathic normal pressure hydrocephalus are absent in the literature. The main purpose of the present study was to evaluate the olfactory bulb (OB) volume and smell function in iNPH.
Methods
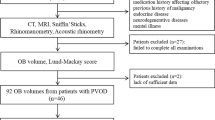
The study comprised 17 patients with iNPH (seven women and ten men, mean age = 66 years); they were compared to a group of 24 healthy people (11 women and 13 men, mean age = 62 years). Comprehensive assessment of olfactory function was conducted with the "Sniffin’ Sticks" test kit. In an additional pilot study, in a small subgroup of eight patients, measurements were performed before and approximately 7 months after surgical treatment of the hydrocephalus.
Results
The OB volume in patients with iNPH was significantly smaller compared to healthy controls. In our small postoperative patient population (n = 8), there was no significant change of the OB volume.
Conclusion
In conclusion our results suggest that iNPH significantly affects OB volumes.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Hydrocephalus is characterized by an increased accumulation of cerebrospinal fluid within ventricles and subarachnoid space. The triad of gait disturbance, incontinence, and dementia is known as the Hakim triad [1, 2] and represents the cardinal symptoms of idiopathic normal pressure hydrocephalus (iNPH). The average age at the diagnosis of iNPH is above 60 years with male predominance. The clinical presentation, the enlargement of the cerebral ventricles in contrast to the narrow supratentorial pericerebral space, plus the flattened cortical sulci is central to the diagnosis of iNPH. The magnetic resonance imaging (MRI) of iNPH patients often demonstrates deep white matter hyperintensity and subcortical lacunar infarctions. Intrusion of the CSF into the periventricular white matter and periventricular gliosis are one of the neuroimaging and histologic characteristics of iNPH [3]. Recently, the temporal changes in apparent diffusion coefficient of the frontal white matter during cardiac cycle were detected as a potential marker for the diagnosis of iNPH [4].
On average, there is intermittent increase of intracranial pressure. Acute hydrocephalus can lead to papilledema, and the chronic disruption of cerebrospinal fluid dynamics may not only damage the brain parenchyma but can also contribute to the structural changes of the olfactory bulb [5]. The absorption of cerebrospinal fluid occurs at the level of the arachnoid villi/granulations in the cranial venous sinuses. However, there may be additional mechanisms of CSF absorption with the olfactory pathway representing a route for CSF drainage. In this case, CSF leaks into the perineural sheet of the olfactory bulb (OB) to the subarachnoid space, passing the cribriform plate. The CSF would then be absorbed by lymphatic vessels in the olfactory submucosa [6]. The OB is able to change in volume due to the influx of progenitor cells and their differentiation into neurons [7]. Buschhüter et al. [8] investigated a large cohort of healthy volunteers and defined normative values for minimal–normal OB volume as 58 mm3 in people <45 years and as 46 mm3 in people >45 years. Mean values of the left and right OB volume of all investigated subjects were 48 mm3 [8].
There is an ongoing turnover of neurons in the OB [9], possibly due to local neuroregeneration. Gudziol et al. showed in 19 patients with chronic rhinitis and olfactory loss that the decreased OB volume increased in relation to recovery of the sense of smell [10].
We hypothesized that iNPH patients will exhibit morphologic alterations in the OB, accompanied by impaired smell function. In an additional pilot study in a small group of patients we investigated OB volume and olfactory function pre- and postoperatively.
Subjects and methods
Patients
The study was performed according to the Declaration of Helsinki for studies on human subjects. It was approved by the ethics committee of the Faculty of Medicine Carl Gustav Carus of the Technische Universität Dresden, Germany (EK 360112010). Written consent was obtained by each participant.
The prospective study comprised 17 patients with iNPH (seven women and ten men, mean age = 66 years) between April 2007 and August 2010. Those patients were all responders to tap testing in that they exhibited gait improvement. The average duration of neurological symptoms prior to surgery was 21 months. Patients with suspected Parkinson and Alzheimer's disease were excluded. In patients with iNPH, ventriculoperitoneal shunting was performed. Their results were compared to a group of 24 healthy people (11 women and 13 men, mean age = 62 years) who participated in a study on normative values for the OB [8].
Enlarged cerebral ventricles were present in all iNPH patients. The symptoms of the gait disturbance, dementia, and urinary incontinence varied in occurrence. The diagnosis of iNPH had already been established in outpatient clinics by clinical examination and lumbar puncture. All of the patients experienced improvement of their medical status as gait improvement following the “tap test”. After the clinical improvement, the indication for ventriculoperitoneal shunting was made.
Olfactory testing
Otorhinolaryngologic diseases were excluded by clinical examination and a detailed history in all patients. Smell testing was performed at the Department of Otorhinolaryngology 24 h before the initial tap test in all patients. The otorhinolaryngologists were blinded to the results of tap tests. As previously described, the psychophysical testing of olfactory function was performed with the validated “Sniffin' Sticks” test. Odors were presented in felt-tip pens to both nostrils (“Sniffin' Sticks”, Burghart GmbH, Wedel, Germany) [11, 12]. This testing implies subtests for phenylethyl-alcohol odor threshold, odor discrimination, and odor identification. The so-called “TDI score” is the sum of the results of the aforementioned subtests. Kobal et al. [12] investigated 1036 subjects and grouped olfactory function in functional anosmia (TDI score ≤16.5), hyposmia (16.75 ≤ TDI score ≤ 30.5), and normosmia (TDI score >30.75).
Assessment of OB volume
In addition to iNPH standard sequences in cMRI, all patients received extra coronal sequences covering the anterior fossa containing OB. MRI images were obtained by 1.5-Tesla magnetic resonance imaging system (Sonata Vision; Siemens, Erlangen, Germany) using the cp head coil (for an example of an OB in a patient and a healthy control see Fig. 1). T2-weighted fast spin-echo images of 2.0 mm in the coronal plane were generated covering the frontobasal skull region.
The protocol included T2-weighted 2D turbo spin echo (TSE) sequence in the coronal plane: repetition time (TR) = 4,800 ms; echo time (TE) = 152 ms; flip angle, 150°; number of averages, 4; matrix, 256 × 256; field of view, 120 × 120; slice thickness, 2.0 mm; spacing, 2.4 mm; number of slices, 30.
Left and right OB were separately evaluated by two examiners using AMIRA 3D visualization software (Visage Imaging, Carlsbad, USA). In case of an OB difference of more than 5.0 mm3 the average measurement from both observers was used. The Pearson correlation coefficient were for the right OB r = 0.94 (p < 0.001) and for the left OB r = 0.97 (p < 0.001). Yousem et al. showed that the volumetric measurements of the olfactory bulbs, tracts and the temporal lobes can be reliably and accurately reproduced from MR images.
Statistical analyses
All statistics were performed using SPSS software version 17.0 (SPSS, Inc., Chicago, IL, USA). T tests for independent (group comparisons) and paired samples (pre-/postsurgery comparisons) were used. Correlations according to Pearson were computed between volumetric measurements of the OB and functional measurements. The level of significance was set at 0.05.
Results
Descriptive and comparative statistics for olfactory parameters are listed in Table 1. The two groups were significantly different with patients exhibiting smaller OBs (p < 0.02); in addition, patients had lower olfactory function than controls as indicated by decreased scores in all three subtests, odor thresholds, odor discrimination, and odor identification (p < 0.04). With regard to the TDI score, only two iNPH patients were normosmic, while nine were hyposmic and three had functional anosmia (scores were not present from three patients).
Within the context of a pilot study in eight subjects it was possible to obtain measures also after surgery. When comparing results before and after surgery, however, no significant differences emerged (Table 2).
Discussion
In our study, we have shown that patients with iNPH symptoms and hydrocephalus characteristics in MRI have significantly smaller OB volumes than healthy controls. We examined the olfaction in those patients due to the described CSF absorption via olfactory pathway through the cribriform plate to nasal submucosa [6]. The majority of the patients with iNPH were hyposmic before the implantation of the ventriculoperitoneal shunt. Although our patients only have had minor demential symptoms, if any, the deficits in odor identification could already be an expression of a beginning dementia.
MRI volumetrics can be reliably used to assess the olfactory system [13]. The volume of OB has been evaluated and measured in several neurologic and otorhinolaryngologic diseases [10, 14]. Patients with idiopathic intracranial hypertension present at early stage with significantly smaller OB volume compared to healthy controls [5]. Regarding the missing effect of surgery in our pilot study, it may be that the observation time was too short, although Gudziol et al. have seen OB changes after 3 months of observation time in their patient group with chronic rhinitis [10]. Thus, a follow-up study will consider longer testing intervals between surgery and second measurement.
Limitations of the study
Underdiagnosis of iNPH and in many cases ambiguous distinction to other neurological diseases in elderly is one of the biggest limitations in general. One of the criteria is the clinical development of the disease. Although our study tried to narrow this with development of additional MRI parameters, it is restrainted by a small number of patients. Future studies should also incorporate patients with different clinical development of iNPH and other hydrocephalus forms.
Because of a very narrow diagnostic window and study criteria that included only patients without dementia or with minor symptoms of dementia, significantly more controls than patients were included in our study. Patients with major dementia were not compliant and did not fulfill the study criteria.
Why is the OB volume decreased in iNPH? Numerous hypotheses have been proposed for the development of iNPH [15, 16]. In the case of transiently increased intracranial pressure, it is imaginable that the consequent lowering of the cerebral blood flow and function of anatomic structures might be affected. In accordance to anatomic impairment of the optic nerve in hydrocephalus, the smaller OB could also result from local CSF pressure. Alternatively, plasticity of the OB could be slowed.
Conclusions
Preoperative OB volumes in patients with iNPH were significantly smaller compared to healthy controls. A longitudinal study in a larger group of patients might be needed to detect possible volume changes of OB after the placement of ventriculoperitoneal shunt and normalisation of the intracranial pressure.
References
Adams RD, Fisher CM, Hakim S, Ojemann RG, Sweet WH (1965) Symptomatic occult hydrocephalus with "normal" cerebrospinal-fluid pressure. A treatable syndrome. N Engl J Med 273:117–126. doi:10.1056/NEJM196507152730301
Hakim S, Venegas JG, Burton JD (1976) The physics of the cranial cavity, hydrocephalus and normal pressure hydrocephalus: mechanical interpretation and mathematical model. Surg Neurol 5(3):187–210
Pasquini U, Bronzini M, Gozzoli E, Mancini P, Menichelli F, Salvolini U (1977) Periventricular hypodensity in hydrocephalus: a clinico-radiological and mathematical analysis using computed tomography. J Comput Assist Tomogr 1(4):443–448
Ohno N, Miyati T, Mase M, Osawa T, Kan H, Kasai H, Hara M, Shibamoto Y, Hayashi N, Gabata T, Matsui O (2011) Idiopathic normal-pressure hydrocephalus: temporal changes in ADC during cardiac cycle. Radiology 261(2):560–565. doi:10.1148/radiol.11101860
Schmidt C, Wiener E, Hoffmann J, Klingebiel R, Schmidt F, Hofmann T, Harms L, Kunte H (2012) Structural olfactory nerve changes in patients suffering from idiopathic intracranial hypertension. PLoS One 7(4):e35221. doi:10.1371/journal.pone.0035221
Johnston M, Zakharov A, Papaiconomou C, Salmasi G, Armstrong D (2004) Evidence of connections between cerebrospinal fluid and nasal lymphatic vessels in humans, non-human primates and other mammalian species. Cerebrospinal Fluid Res 1(1):2. doi:10.1186/1743-8454-1-2
Altman J (1969) Autoradiographic and histological studies of postnatal neurogenesis. IV. Cell proliferation and migration in the anterior forebrain, with special reference to persisting neurogenesis in the olfactory bulb. J Comp Neurol 137(4):433–457. doi:10.1002/cne.901370404
Buschhuter D, Smitka M, Puschmann S, Gerber JC, Witt M, Abolmaali ND, Hummel T (2008) Correlation between olfactory bulb volume and olfactory function. Neuroimage 42(2):498–502. doi:10.1016/j.neuroimage.2008.05.004
Curtis MA, Monzo HJ, Faull RL (2009) The rostral migratory stream and olfactory system: smell, disease and slippery cells. Prog Brain Res 175:33–42. doi:10.1016/S0079-6123(09)17503-9
Gudziol V, Buschhuter D, Abolmaali N, Gerber J, Rombaux P, Hummel T (2009) Increasing olfactory bulb volume due to treatment of chronic rhinosinusitis—a longitudinal study. Brain 132(Pt 11):3096–3101. doi:awp243[pii]10.1093/brain/awp243
Hummel T, Sekinger B, Wolf SR, Pauli E, Kobal G (1997) 'Sniffin' sticks': olfactory performance assessed by the combined testing of odor identification, odor discrimination and olfactory threshold. Chem Senses 22(1):39–52
Kobal G, Klimek L, Wolfensberger M, Gudziol H, Temmel A, Owen CM, Seeber H, Pauli E, Hummel T (2000) Multicenter investigation of 1,036 subjects using a standardized method for the assessment of olfactory function combining tests of odor identification, odor discrimination, and olfactory thresholds. Eur Arch Otorhinolaryngol 257(4):205–211
Yousem DM, Geckle RJ, Doty RL, Bilker WB (1997) Reproducibility and reliability of volumetric measurements of olfactory eloquent structures. Acad Radiol 4(4):264–269
Mueller A, Rodewald A, Reden J, Gerber J, von Kummer R, Hummel T (2005) Reduced olfactory bulb volume in post-traumatic and post-infectious olfactory dysfunction. Neuroreport 16(5):475–478
Palm WM, Walchenbach R, Bruinsma B, Admiraal-Behloul F, Middelkoop HA, Launer LJ, van der Grond J, van Buchem MA (2006) Intracranial compartment volumes in normal pressure hydrocephalus: volumetric assessment versus outcome. AJNR Am J Neuroradiol 27(1):76–79
Vanneste J, Hyman R (1986) Non-tumoural aqueduct stenosis and normal pressure hydrocephalus in the elderly. J Neurol Neurosurg Psychiatry 49(5):529–535
Acknowledgements
This study was supported by a grant from Roland Ernst Stiftung to TH.
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Podlesek, D., Leimert, M., Schuster, B. et al. Olfactory bulb volume in patients with idiopathic normal pressure hydrocephalus. Neuroradiology 54, 1229–1233 (2012). https://doi.org/10.1007/s00234-012-1050-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-012-1050-8