Abstract
Osteoprotegerin (OPG) is a novel secreted member of the tumor necrosis factor receptor family which plays a crucial role in negative regulation of osteoclastic bone resorption. OPG-deficient (OPG–/–) mice develop severe osteoporosis caused by significant enhancement of bone resorption by osteoclasts. We investigated the effect of administering bisphosphonate on mandibular growth and development in OPG–/– mice. Eight-week-old male OPG–/– mice and wild-type (WT) mice were administered bisphosphonate (1.25 mg/kg body weight) intraperitoneally once every 3 days for 30 days. All bone formation-related parameters and bone resorption-related parameters were significantly lower in OPG–/– mice with bisphosphonate than in those without bisphosphonate. The volume of the whole condyle and the mandibular length in OPG–/– mice without bisphosphonate were significantly smaller than in WT mice without bisphosphonate. Bisphosphonate treatment of the OPG–/– mice resulted in an increase in the volume of the mandibular condyle and mandibular ramus length. In fact, the mandibular ramus length in OPG–/– mice with bisphosphonate was similar to the length in WT mice without bisphosphonate. Histologically, the surface irregularity of the mandibular condyle that was observed in the OPG–/– mice without bisphosphonate tended to be less marked in the OPG–/– mice with bisphosphonate, and the proportion of the area of the cartilage layer relative to the whole condyle was significantly larger in OPG–/– mice with bisphosphonate than in those without bisphosphonate. In conclusion, bisphosphonate treatment results in an increase in mandibular condylar dimensions and normalization of mandibular ramus growth.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
In bone tissues, the processes of bone resorption by osteoclasts and bone formation by osteoblasts are continually repeated. In rapidly growing bone tissues, modeling mainly takes place, while in bone tissues that have stopped growing, remodeling takes place. Osteoclasts are hematopoietic cells of the macrophage lineage, and they are the only cells that destroy and resorb mineralized bone tissues [1]. It has become clear that the differentiation, maturation, and functioning of osteoclasts are strictly regulated by the receptor activator of NF-κB ligand (RANKL) expressed on the cell membranes of osteoblasts or bone marrow stromal cells [1]. Osteoclasts and their precursor cells express the receptor activator of NF-κB (RANK) and recognize RANKL through cell-cell contact, resulting in differentiation into osteoclasts and further maturation [2–4]. Osteoblasts produce osteoprotegerin (OPG), which is a member of the TNF receptor superfamily and is a decoy receptor of RANKL. Since the binding affinity of OPG to RANKL is 10-fold higher than the binding affinity of RANKL to RANK, OPG suppresses the differentiation and functional expression of osteoclasts by strongly inhibiting the interaction between RANKL and RANK. In vivo, OPG overexpression in mice inhibits bone resorption and results in severe osteopetrosis [5]. In contrast, OPG-deficient (OPG–/–) mice develop severe osteoporosis caused by significant enhancement of bone resorption by osteoclasts [6–8]. In addition to enhanced bone resorption, interestingly, OPG–/– mice have been found to have high serum activity levels of alkaline phosphatase(ALP), a marker of bone formation, and histological enhancement of bone formation has been observed in these mice [6, 9].
In humans, juvenile Paget’s disease (Idiopathic hyperphosphatasia) has been recently reported to be associated with deletion or mutation of the gene encoding OPG (TNFRSF11B) [10, 11]. Histologically, patients with this disease have markedly activated osteoblasts and osteoclasts, and vigorous bone resorption and formation, and as a result, patients develop severe systemic high-turnover osteoporosis [12]. Patients with Paget’s disease also have high serum levels of ALP activity [11]. The fact that the findings in juvenile Paget’s disease are similar to those in OPG–/– mice is very interesting when considering bone metabolism.
In some parts of the mandible, particularly the mandibular condyle, growth occurs by endochondral ossification, which is said to influence the longitudinal growth of the mandibular condyle [13]. Antoniades et al. [14] reported that they observed a short mandibular ramus in a patient with juvenile Paget’s disease. Therefore, it is surmised that some changes in endochondral growth of the mandibular condyle may also be observed in OPG–/– mice. In this study, we used OPG–/– mice as a useful model for juvenile Paget’s disease and investigated the differences between these mice and wild-type (WT) mice with respect to mandibular growth and development. In addition, we studied responses after the administration of bisphosphonate, a drug that inhibits the activation of osteoclasts and is used for treatment of osteoporosis, to OPG–/– mice.
Materials and Methods
Animals and Reagents
Eight-week-old male OPG–/– mice and, as controls, C57BL/6J WT mice were used. These mice were purchased from CLEA Japan and were maintained at the Animal Experiment Laboratory,Faculty of Dentistry, Aichi-Gakuin University. They were maintained at a constant temperature (22 ± 2°C) and humidity (50% ± 10%), under a 12-h light/dark cycle. Mice were provided with laboratory chow (CE-2; CLEA Japan) and tap water ad libitum. Animals were cared for and experiments were conducted in accordance with the guidelines for animal experimentation established by the Faculty of Dentistry at Aichi-Gakuin University. We used alendronate (Teiroc, Teijin Pharma Ltd.) as a bisphosphonate.
Administration of Bisphosphonate
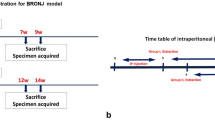
Eight-week-old male OPG–/– mice (n = 8) and WT mice (n = 8) were administered bisphosphonate (1.25 mg/kg body weight) intraperitoneally once every 3 days for 30 days. For comparison, 0 mg/kg body weight alendronate (saline solution alone) was intraperitoneally injected into OPG–/– (n = 8) and WT (n = 8) mice for the same period.
The duration and interval of administration were determined with reference to a report by Azuma (Teijin Pharma, Tokyo) [15]; in particular, as the decrease in plasma calcium level due to the action of alendronate reaches a peak on day 3 after administration, we decided to administer alendronate once every 3 days for 30 days so that its effect was maintained.
Soft X-Ray Imaging
The mice were killed with diethyl ether, and skin and muscle were removed from the head and legs as thoroughly as possible in order to obtain mandible and femur specimens. Soft x-ray images of the bones were taken using a soft x-ray generator (OMC-403; Ohmic) at 23 kV, 3 mA, for 20 sec. The mandible specimens were mounted on soft x-ray films (FR type, cabinet size [12 × 16.5 cm]; Fujifilm) so that images of the lateral sagittal sections could be obtained. Films were developed with Rendol (Fujifilm Corp.) and fixed with Renfix (Fujifilm Corp.). The soft x-ray images were scanned and transmitted with an image scanner, then morphometric analysis was performed using image analysis software (NIH Image).
Reference points and straight-line distances for measurement are shown in Fig. 1. The straight-line distances between the infradentale and the gonion (Id-Go), the condylion and the gonion (Cd-Go), the infradentale and the most posterior part of the lower third molar (Id-M3), the most posterior part of the lower third molar and the most posterior point of the mandibular foramen (M3-MF), and the most posterior point of mandibular foramen and the condylion (MF-Cd) were measured. In addition, the lengths of the femurs were also measured.
Reference points and distances measured. a Reference points: Id, infradentale; M3, most posterior part of the lower third molar; MF, most posterior point of the mandibular foramen; Cd, condylion; Go, gonion. b Distances measured: Id-M3 (infradentale–most posterior part of the lower third molar); Id-Go (infradentale–gonion); M3-MF (most posterior part of the lower third molar–most posterior point of the mandibular foramen); MF-Cd (most posterior point of the mandibular foramen–condylion); Cd-Go (condylion–gonion)
Microcomputed Tomography
Mandibles were analyzed with SMX-225CT-SV2 (Shimadzu, Kyoto, Japan). Mandibular rami were scanned perpendicular to their longitudinal axis by a fixed x-ray fan beam (40 μA, 60 kV) while the holder rotated along its axis.
Histopathological Observations
The mandibles were removed and fixed in 10% neutral buffered formalin, then decalcified in 10% EDTA at pH 7.2 for approximately 4 weeks at 4°C. The tissues were then routinely embedded in paraffin and 5-μm serial coronal sections were cut. Hematoxylin and eosin staining, tartrate-resistant acid phosphatase (TRAP) staining, and type II collagen immunostaining were performed and the specimens were observed under an optical microscope. Condylar cartilage layers were classified using the zonation scheme of Beresford [16]. The fibrous layer, the proliferative layer, and the cartilage layer (the maturative layer + the hypertrophic layer) were assessed morphologically (Fig. 2a). Histomorphometric analysis was performed using the method of Kimmel and Jee [17], using a grid and the point-hit method (Fig. 2b).
TRAP staining with an acid phosphatase, leukocyte kit (Sigma Diagnostics, St. Louis, MO) was applied as a marker for osteoclasts. TRAP-positive cells containing two or more nuclei were identified as osteoclasts. Histomorphometric analysis was done in the region of the chondro-osseous junction in mandibular condyle of OPG–/– and WT mice.
A bone resorption-related parameter (osteoclast number/bone surface) and a bone formation-related parameter (osteoblast surface/bone surface) were measured.
Measurement of Serum Bone Metabolism Markers
Blood samples from OPG–/– and WT mice were obtained by cardiocentesis under diethyl ether anesthesia at 30 days after bisphosphonate was first administered. Serum alkaline phosphatase activity was measured using a Liquitech ALP kit (Roche Diagnostic K.K., Tokyo). The osteocalcin level was measured using an ELISA kit (Nordic Bioscience). The serum TRAP level was measured using a TRAP activity assay kit (SBA Sciences).
Statistical Analysis
The experimental data are presented as mean ± standard deviation, and Student’s t-test was used to evaluate statistical significance.
Results
Comparison of OPG–/– and WT Mice
Morphological analysis of the mandible
The results of morphometric analysis of the mandible are reported in Table 1. No significant differences were found between OPG–/– and WT mice for Id-M3, Id-Go, or M3-MF. However, MF-Cd and Cd-Go, both indications of the mandibular ramus length, were significantly smaller in the OPG–/– mice than in the WT mice.
We performed micro-CT scans of the mandible. The mandible in OPG –/– mice was osteoporotic compared to that in WT mice (Fig. 3).
Histological Analysis
Histological features of the mandibular condyle
The surface profile of the mandibular condyle was more irregular in OPG–/– mice than in WT mice (Fig. 4a). In addition, in OPG–/– mice the total number of chondrocytes was smaller, their cytoarchitecture was disarrayed, and the cartilage matrix occupied a larger area of the whole condyle relative to WT mice (Fig. 4b). The volume of the whole condyle was significantly smaller in OPG–/– mice than in WT mice (Fig. 5a). The area of the cartilage layer relative to the whole condyle was significantly smaller in OPG–/– mice than in WT mice (Fig. 5b).
Osteoclast counts
A larger number of osteoclasts were observed around the osteochondral junction in OPG–/– mice than in WT mice (Fig. 6a). The number of osteoclasts in spongy bone just under the cartilage layer was significantly larger in OPG–/– mice than in WT mice (Fig. 6b).
Osteoblast surface/bone surface measurement
Bone formation-related parameters were significantly higher in trabecular sites of the mandibular condyle in untreated OPG–/– mice than in WT mice (Fig. 7).
Changes in serum bone metabolism markers
Serum alkaline phosphatase activity and osteocalcin level (both bone formation-related parameters) and TRAP level (a bone resorption-related parameter) were significantly higher in OPG–/– mice than in WT mice (Figs. 8 and 9).
Influence of Bisphosphonate on the Mandibular Condyle
Morphological analysis of the mandible and femur
No significant differences were found between OPG–/– mice that did and OPG–/– did not receive bisphosphonate for Id-M3, Id-Go, or M3-MF. Similarly, for the same parameters, no significant differences were found between WT mice that did and WT mice that did not receive bisphosphonate (Table 1).
MF-Cd and Cd-Go (measures of the mandibular ramus length) were significantly larger in OPG–/– mice that received bisphosphonate than in those that did not. In fact, in OPG–/– mice that received bisphosphonate, MF-Cd and Cd-Go values were similar to those of WT mice that did not receive bisphosphonate. MF-Cd and Cd-Go were significantly larger in WT mice that received bisphosphonate than in those that did not (Table 1).
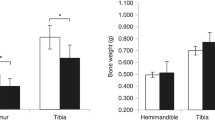
The femurs of the OPG–/– mice were shorter than those of the WT mice, but no difference in femur length was found between OPG–/– mice that received bisphosphonate and those that did not (Fig. 10).
Histological Analysis
Histological findings for the mandibular condyle
The surface irregularity of the mandibular condyle that was observed in the OPG–/– mice that did not receive bisphosphonate tended to be less marked than in the OPG–/– mice that did (Fig. 4a). The cytoarchitectural disarray was also less marked in these mice (Fig. 4b). The volume of the whole condyle was significantly larger in the OPG–/– mice that received bisphosphonate than in those that did not. The volume of the whole condyle in OPG–/– mice that received bisphosphonate was similar to the volume in WT mice that did not receive bisphosphonate. The volume of the whole condyle was significantly larger in the WT mice that received bisphosphonate than in those that did not (Fig. 5a).
The proportion of the area of the cartilage layer relative to the whole condyle was significantly larger in OPG–/– mice that received bisphosphonate than in those that did not, and thickening of the cartilage layer was observed in those that received bisphosphonate. WT mice that received bisphosphonate had a significantly larger value than WT mice that did not, and thickening of the cartilage layer was observed in WT mice that received bisphosphonate (Fig. 5b).
Osteoclast counts
The number of osteoclasts present was significantly smaller in OPG–/– mice that received bisphosphonate than in those that did not. In fact, the number present in OPG–/– mice that received bisphosphonate was similar to that in WT mice that did not receive bisphosphonate. There was no significant difference between WT mice that did and those that did not receive bisphosphonate (Fig. 6).
Osteoblast surface/bone surface measurement
Alendronate treatment decreased the elevated bone formation-related parameters to levels lower than those in WT mice (Fig. 7).
Changes in serum bone metabolism markers
The alkaline phosphatase activity, osteocalcin level, and TRAP level in OPG–/– mice that received bisphosphonate were similar to the levels in the groups of WT mice (Figs. 8 and 9).
Discussion
OPG–/– mice have been shown to develop high-turnover osteoporosis [6–8]. Although serum OPG is almost undetectable in OPG–/– mice, the serum level of soluble RANKL is high [18].
Juvenile Paget’s disease usually develops during infancy or childhood. Symptoms are systemic and their clinical severity is variable. Patients with juvenile Paget’s disease develop severe high-turnover osteoporosis [12]. Mutation of the OPG gene plus undetectable OPG levels and high concentrations of RANKL are reportedly observed in patients with juvenile Paget’s disease [10, 11, 19]. Therefore, Whyte et al. [10] noted that the findings of juvenile Paget’s disease are very similar to those of OPG–/– mice and, thus, concluded that OPG–/– mice present with the clinical features of juvenile Paget’s disease [10]. Antoniades et al. [14] reported that they observed a short mandibular ramus in a patient with juvenile Paget’s disease, and it is speculated that this abnormality may lead to large facial and jaw deformities in the future. We therefore investigated whether similar abnormalities are found in OPG–/– mice.
In the endochondral bone growth of the mandibular condyle, which influences the length of the mandibular ramus, the proliferative layer, located just under the fibrous layer covering the temporomandibular joint, provides chondrocytes and is a basis of the mandibular condyle growth. The chondrocytes provided by the proliferative layer differentiate into mature and hypertrophic chondrocytes. Then the replacement of cartilage by bone takes place at the osteochondral junction in the hypertrophic layer. Sasaki et al. [20] reported that cartilage-bone replacement consists of the following processes: (i) removal of uncalcified septal cartilage and the opening of chondrocyte lacunae via the phagocytosis of cartilage fragments by perivascular mononuclear cells (vascular invasion), (ii) bone deposition over the remaining septa by osteoblasts, and (iii) absorption of bone and calcified cartilage by osteoclasts. These mononuclear cells are considered to be fibroblast-like chondroclasts, which were reported by Cole et al. [21]. Although the mandibular condyle thus has no growth plate, there have been no studies comparing the mandibular condyle with long bones in OPG–/– mice.
In this study, we showed for the first time that OPG–/– mice have shorter mandibular rami, a smaller area of mandibular condyles, and thinner cartilage layers. The cause of these abnormalities is speculated to be as follows: under conditions in which osteoclasts are activated due to OPG deficiency, chondroclast activity is also high and cartilage-bone replacement is accelerated at the osteochondral junction; therefore, in OPG–/– mice, phagocytosis of the cartilage matrix is more active than normal, resulting in thinning of the hypertrophic layer. Sakai et al. locally administered cyclophosphamide, a drug used as an anticancer or immunosuppressive agent, to the mandibular condyle of rats. They observed suppressed growth of the mandibular condyle and considered that thinning of mandibular condyle cartilage would be one of the factors for this growth suppression [22]. We thus speculate that in the OPG–/– mice in our study, thinning of the hypertrophic cartilage layer resulted in the growth suppression of the mandibular condyle. Histological analysis showed that the mandibular condyle in the OPG–/– mice without bisphosphonate had an irregular surface, but the surface of the mandibular condyle was smoothed by bisphosphonate administration. Although it cannot be concluded from our experiment that this improvement was due to osteoclast activation, this activity is considered to somehow influence the surface morphology of the mandibular condyle.
Although Antoniades et al. [14] did not report any histological data for their patients with juvenile Paget’s disease, we think it is likely that patients with juvenile Paget’s disease have histological features similar to those observed in OPG–/– mice. Further clinical studies are necessary to clarify whether this is the case.
In the present study, we found that administering bisphosphonate to OPG–/– mice resulted in normalization of the mandibular ramus length. Increased volume of the mandibular condyle and thickening of the cartilage layer were also observed. Nakamura et al. [18] reported that bone loss was observed in the femoral trabeculae of OPG–/– mice and that the mass of the trabecular bones of OPG–/– mice increased after administration of bisphosphonate (risedronate). However, they did not mention the femur length. Bone loss was also observed in the mandibular condyle of the OPG–/– mice used in our study. However, examination of the effect of bisphosphonate on femur length in OPG–/– mice showed no changes due to administration, indicating a difference in effect between the femur and the mandibular condyle. Although, as described above, the mandibular condyle grows by endochondral bone formation, it differs from the femur in that it does not have a growth plate. This structural difference is considered to be the cause of the specific form of growth of the mandibular condyle. Tabuchi et al. [23] reported that the mass of new bone after the implantation of bone morphogenic proteins (BMPs) was less in OPG–/– mice than in WT mice. Histologically, they found that cartilage was replaced by trabecular bone and other tissues, and the percentage of cartilage in the new bone was low in OPG–/– mice. In addition, their OPG–/– mice that received bisphosphonate had a larger mass of new bone and, histologically, more remaining cartilage tissue than those that did not receive bisphosphonate. We consider that these findings by Tabuchi et al. support our results in that their experiments were performed under the same conditions, namely, using OPG–/– mice, and the size of the new bone and turnover were normalized by bisphosphonate administration.
Bisphosphonates are now used for treating patients with significantly enhanced bone resorption, including those with osteoporosis and Paget’s disease [24, 25]. Bisphosphonates are synthetic analogues of pyrophosphate, acting directly on osteoclasts to strongly inhibit bone resorption [26–28]. Other reported effects include the inhibition of vascular invasion, the prevention of apoptosis in the hypertrophic layer, a decrease in cartilage degradation, and an increase in the amount of cartilage matrix [29–31]. They reportedly have therapeutic effects with respect to the inhibition of osteoclast activity, reduction of serum ALP activity, normalization of bone metabolic turnover, and improvement of bone density in patients with juvenile Paget’s disease [12]. Regarding the growth-promoting effect of bisphosphonate on OPG–/– mice observed in our study, it is speculated that turnover at the osteochondral junction was normalized by the effects described above, and as a result, the growth of the mandibular condyle was improved. In detail, the process is considered as follows: at the osteochondral junction of the mandibular condyle, chondroclasts underwent apoptosis, vascular invasion was inhibited, and the phagocytosis of cartilage matrix was prevented; new chondrocytes and cartilage matrix were accumulated on the cartilage matrix that had avoided phagocytosis, leading to thickening of the hypertrophic layer; and as a result, the area of the mandibular condyle increased. Although it cannot be ascertained from our study whether bisphosphonate acts directly or indirectly on the cartilage of the mandibular condyle, we consider that the changes in the cartilage layer observed in our study were indirect ones that can be attributed to the inhibitions of chondroclast activity and vascular invasion at the osteochondral junction. However, this point remains unclear and requires further investigation.
There currently is no information in the literature concerning the effect of bisphosphonate on bone growth and development in patients with juvenile Paget’s disease. Our results suggest that treatment of mandibular hypoplasia with bisphosphonate in patients with juvenile Paget’s disease may be highly effective. However, osteonecrosis of the jaw (ONJ) has recently been found to develop in the jawbones of some patients who have undergone long-term treatment with bisphosphonate [32–34]. Although this ONJ reportedly occurs after tooth extraction, its etiology remains unclear. Further study is necessary to identify the cause of this ONJ, but the efficacy of bisphosphonate is undeniable, so we suggest the clinical use of bisphosphonate, with consideration given to the potential development of ONJ.
In conclusion, we found that the mandibular ramus length was shorter in OPG–/– mice than in their WT counterparts. The clinical and histological features of OPG–/– mice are similar to those of humans with juvenile Paget’s disease. We also found that the growth of the mandibular ramus in OPG–/– mice was normalized by administering bisphosphonate. These data suggest that OPG–/– mice are suitable model for juvenile Paget’s disease and can be utilized for preclinical studies of the long-term effects of bisphosphonates on the progression of the disease, the growth of the animal, and, in particular, the status of the jaw following such long-term treatment.
References
Suda T, Takahasi N, Udagawa N, Jimi E, Gillespie MT, Martin TJ (1999) Modulation of osteoclast differentiation and function by the new members of the tumor necrosis factor receptor and ligand familes. Endocr Rev 20:345–357
Kong YY, Yashida H, Sarosi I, Tan HL, Timms E, Capparelli C, Morony S, Oliveira-dos-Santos AJ, Van G, Itie A, Khoo W, Wakeham A, Dunstan CR, Lacey DL, Mak TW, Boyle WJ, Penninger JM (1999) OPGL is a key regulator of osteoclastgenesis, lymphocyte development and lymph-node organogenesis. Nature 397:315–323
Dougall WC, Glaccum M, Charrier K, Rohrbach K, Brasel K, De Smedt T, Daro E, Smith J, Tometsko ME, Maliszewski CR, Armstrong A, Shen V, Bain S, Cosman D, Anderson D, Morrissey PJ, Peschon JJ, Schuh J (1999) RANK is essential for osteoclast and lymph node development. Genes Dev 13:2412–2424
Li J, Sarosi I, Yan XQ, Morony S, Capparelli C, Tan HL, McCabe S, Elliott R, Scully S, Van G, Kaufman S, Juan SC, Sun Y, Tarpley J, Martin L, Christensen K, McCabe J, Kostenuik P, Hsu H, Fletcher F, Dunstan CR, Lacey DL, Boyle WJ (2000) RANK is the intrinsic hematopoietic cell surface receptor that controls osteoclastgenesis and regulation of bone mass and calcium metabolism. Proc Natl Acad Sci USA 97:1566–1571
Simonet WS, Lacey DL, Dunstan CR, Kelley M, Chan MS, Luthy R, Nguyen HQ, Wooden S, Bennett L, Boone T, Shimamoto G, DeRose M, Elliott R, Colombero A, Tan HL, Trail G, Sullivan J, Davy E, Bucay N, Renshaw-Gegg L, Hughes TM, Hill D, Pattison W, Campbell P, Sander S, Van G, Tarpley J, Derby P, Lee R, Boyle WJ (1997) Osteoprotegerin: a novel secreted protein involved in the regulation of bone density. Cell 89:309–319
Bucay N, Sarosi I, Dunstan CR, Morony S, Tarpley J, Capparelli C, Scully S, Tan HL, Xu W, Lacey DL, Boyle WJ, Simonet WS (1998) Osteoprotegerin-deficient mice develop early onset osteoporosis and arterial calcification. Genes Dev 12:1260–1268
Mizuno A, Amizuka N, Irie K, Murakami A, Fujise N, Kanno T, Sato Y, Nakagawa N, Yasuda H, Mochizuki S, Gomibuchi T, Yano K, Shima N, Washida N, Tsuda E, Morinaga T, Higashino K, Ozawa H (1998) Severe osteoporosis in mice lacking osteoclastgenesis inhibitory factor/osteoprotegerin. Biochem Biophys Res Commun 247:610–615
Kawata F. Sasaki T (2003) Osteoclast differentiation and characteristic trabecular bone formation during growth plate destruction in osteoprotegerin-deficiency mice. J Electron Microsc 52:515–525
Amizuka N, Shimomura J, Li M, Seki Y, Oda K, Henderson JE, Mizuno A, Ozawa H, Maeda T (2003) Defective bone remodeling in osteoprotegerin-deficiency mice. J Electron Microsc 52:503–513
Whyte MP, Obrecht SE, Finnegan PM, Jones JL, Podgornik MN, McAlister WH, Mumm S (2002) Osteoprotegerin deficiency and juvenile Paget’s disease. N Engl J Med 347:175–184
Cundy T, Hegde M, Naot D, Chong B, King A, Wallace R, Mulley J, Love DR, Seidel J, Fawkner M, Banovic T, Callon KE, Grey AB, Reid IR, Middleton-Hardie CA, Comish J (2002) A mutation in the gene TNFRSF11B encoding osteoprotegerin causes an idiopathic hyperphosphatasia phenotype. Hum Mol Genet 11:2119–2127
Cundy T, Wheadon L, King A (2004) Treatmant of idiopathic hyperphosphatasia with intensive bisphosphonate therapy. J Bone Miner Res 19:703–711
Enlow DH (1982) Handbook of facial growth. 2nd ed. W. B. Saunders, Philadelphia
Antoniades K, Karakasis D, Kapetanos G, Lasaridis N, Tzarou V (1993) Chronic idiopathic hyperphosphatasemia. Oral Surg Oral Med Oral Pathol 76:200–204
Azuma Y, Sato H, Oue Y, Okabe K, Ohta T, Tsuchimoto M, Kiyoki M (1995) Alendronate distributed on bone surfaces inhibits osteoclastic bone resorption in vitro and in experimental hypercalcemia models. Bone 16:235–245
Beresford WA (1975) Schemes of zonation in the mandibular condyle. Am J Ortho 68:189–195
Kimmel DB, Jee WSS (1983) Measurements of area, perimeter and distance: details of data collection in bone histomorphometry. In: Recker RR (eds) Bone histomorphometry. Techniques and interpretation. CRC Press, Boca Raton, FL, pp 89–108
Nakamura M, Udagawa N, Matsuura S, Mogi M, Nakamura H, Horiuchi H, Saito N, Hiraoka BY, Kobayashi Y, Takaoka K, Ozawa H, Miyazawa H, Takahashi N (2003) Osteoprotegerin regulates bone formation through a coupling mechanism with bone resorption. Endocrinology 144:5441–5446
Golob DB, McAlister WH, Mills BG, Fedde KN, Reinus WR, Teitelbaum SL, Beeki S. Whyte MP (1996) Juvenile paget disease: Life-long feature of a mildly affected young woman. J Bone Miner Res 11:132–142
Sasaki T, Kim TW, Debari K, Nagamine H (1996) The replacement processes of growth plate cartilage to bone in endochondral ossification of mandibular condyle. Kaibou-shi 71:106–114
Cole AA, Wezeman FH (1985) Perivascular cell in cartilage canals of the developing mouse epiphysis. Am J Anat 174:119–129
Sakai S (2005) Effect of local administration of cyclophosphamide on mandibular condylar growth in growing rats. Koukubyo Gakkaizassi 72:147–158
Tabuchi M, Miyazawa K, Kimura M, Maeda H, Kawai T, Kameyama Y, Goto S (2005) Enhancement of crude morphogenetic protein-induce new bone formation and normalization of endochondral ossification by bisphosphonate treatment in osteoprotegerin-deficient mice. Calcif Tissue Int 77:239–249
Gennari C, Nuti R, Agnusdei D, Camporeale A, Martini G (1994) Management of oeteoporosis and Paget’s disease. An appraisal of the risks and benefits of drug treatment. Drug Saf 11:176–195
MacGowan JR, Pringle J, Morris VH, Stamp TC (2000) Gross vertebral collapse associated with long-term disodium etidronate treatment for pelvic Paget’s disease. Skeletal Radiol 29:279–282
Schenk R, Eggli P, Fleisch H, Rosini S (1986) Quantitative morphometric evaluation of the inhibitory activity of new aminobisphosphonates on bone resorption in the rat. Calcif Tissue Int 38:342–349
Hughes DE, Wright KR, Uy HL, Sasaki A, Yoneda T, Roodman GD, Mundy GR, Boyce BF (1995) Bisphosphonates promote apotosis in murine osteoclasts in vitro and vivo. J Bone Miner Res 10:1478–1487
Freisch H (1998) Bisphosphonates: mechanisms of action. Endocr Rev 19:80–100
Smith EJ, McEvoy A, Little DG, Baldock PA, Eisman JA, Gardiner EM (2004) Transient retention of endochondral cartilaginous matrix with bisphosphonate treatment in a long-term rabbit model of distraction osteogenesis. J Bone Miner Res 19:1698–1705
Lehmann HJ, Mouritzen U, Christgau S, Cloos PAC, Christiansen C (2002) Effect of bisphosphonates on cartilage turnover assessed with a newly developed assay for collagen type ? degradation products. Ann Rheum Dis 61:530–533
Evans KD, Lau ST, Oberbauer AM, Martin RB (2003) Alendronate affects long bone length and growth plate morphology in the oim mouse model for Osteogenesis Imperfecta. Bone 32:268–274
Marx RE (2003) Pamidronate (Aredia) and zoledronate (Zometa) induced avascular necrosis of the jaws: a growing epidemic. J Oral Maxillofac Surg 61:1115–1117
Marx RE, Sawatani Y, Fortin M, Broumand V (2005) Bisphosphonate-induced exposed bone (osteonecrosis/osteopetrosis) of the jaws: risk factors, recognition, prevention, and treatment. J Oral Maxillofac Surg 63:1567–1575
Migliorati CA, Schubert MM, Peterson DE, Seneda LM (2005) Bisphosphonate-associated osteonecrosis of mandibular and maxillary bone: an emerging oral complication of supportive cancer therapy. Cancer 104:83–93
Acknowledgments
This study was partially supported by the High-Tech Research Center Project for Aichi Gakuin University, with matching fund subsidy from the Ministry of Education, Culture, Sports, Science and Technology (Japan, 2002-2007).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kimura, M., Miyazawa, K., Tabuchi, M. et al. Bisphosphonate Treatment Increases the Size of the Mandibular Condyle and Normalizes Growth of the Mandibular Ramus in Osteoprotegerin-Deficient Mice. Calcif Tissue Int 82, 137–147 (2008). https://doi.org/10.1007/s00223-007-9097-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-007-9097-y