Abstract
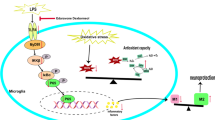
Abnormal neuroinflammation ignited by overproduction of chemokines and cytokines via microglial cells can induce the occurrence and development of neurodegenerative disorders. The aim of this study is to investigate the effects of dexamethasone sodium phosphate (Dex-SP) on chemokine and cytokine secretion in lipopolysaccharide (LPS)-activated microglial cells. LPS markedly enhanced the secretion of pro-inflammatory factors such as regulated on activation, normal T cell expressed and secreted (RANTES), transforming growth factor beta-β1 (TGF-β1) and nitric oxide (NO), but decreased the production of macrophage inflammatory protein-1α (MIP-1α) and interleukin 10 (IL-10) in BV-2 microglial cells. Furthermore, LPS increased BV-2 microglial cell migration. However, Dex-SP treatment had the opposite effect, dampening the secretion of RANTES, TGF-β1, and NO, while increasing the production of MIP-1α and IL-10 and blocking migration of LPS-stimulated BV-2 microglial cells. Furthermore, Dex-SP markedly suppressed the LPS-induced degradation of IRAK-1 and IRAK-4, and blocked the activation in TRAF6, p-TAK1, and p-JNK in BV-2 microglial cells. These results showed that Dex-SP inhibited the neuroinflammatory response and migration in LPS-activated BV-2 microglia by inhibiting the secretion of RANTES, TGF-β1, and NO and increasing the production of MIP-1α and IL-10. The molecular mechanism of Dex-SP may be associated with inhibition of TRAF6/TAK-1/JNK signaling pathways mediated by IRAK-1 and IRAK-4.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuroinflammation is a complex, specialized immune response to pathological processes or injury in the brain. Controlled neuroinflammation can be beneficial, while exaggerated neuroinflammation plays a fundamental role in the pathogenesis of neuronal dysfunction. The hallmark of neuroinflammation is the activation of microglia (Walker and Lue 2005; Kim and Joh 2006; Lopes 2016). Hyperactivation of microglia results in deleterious and progressive neuronal dysfunction by abnormal expression of inflammatory mediators such as NO, IL-10, RANTES, MIP-1α, and TGF-β (Kreutzberg 1996).
The improper regulation of TLR4 signaling has the potential to induce massive neuroinflammation (Hausmann et al. 1998; Rahimifard et al. 2017). It is also known that LPS, the principal component of the outer membrane of gram-negative bacteria, evokes the inflammatory process by the transmembrane receptor Toll-like receptor 4 (TLR4) (Rahimifard et al. 2017). After recognition of LPS by TLR4, numerous intracellular signaling cascades such as IRAK-4, IRAK-1, TGF-β-activated kinase 1 (TAK-1), and JNK are activated, leading to the activation of nuclear factor-activating protein (AP)-1 and (NF)-κB translocation to the nucleus (Flannery and Bowie 2010). Thus, blocking the above signaling molecules may be an important therapeutic intervention to curtail neuroinflammation and restore homeostasis in the diseased brain.
Dexamethasone (Dex), a synthetic glucocorticoid, is a most extensively employed prescribed drug. Dex is well-known to possess anti-inflammatory and immunosuppressive effects in peripheral organs via modulating the production of inflammatory mediators by binding and activating glucocorticoid receptors, which results in cross-talk with other inflammatory pathways (Schoneveld et al. 2004; Schweingruber et al. 2012). However, recent studies have shown that the effect of glucocorticoid in the inflammatory response to the brain is complex (Duque Ede and Munhoz 2016). It is also known that Dex has low water solubility. The available solution of Dex for administration is dexamethasone sodium phosphate (Dex-SP), a water-soluble ester prodrug. Dex-SP is hydrolyzed rapidly by phosphatases to transfer highly lipophilic dexamethasone (Rohdewald et al. 1987). Although the effects of Dex-SP on inflammation outside the CNS are well documented, there is growing evidence that the effects of the two drugs differ in the brain (Siegal et al. 1988). Until now, the direct effect of Dex-SP on microglia is still poorly understood. Therefore, the purpose of the present study was to explore the anti-neuroinflammatory effects of Dex-SP on LPS-induced BV-2 microglia cell.
Materials and methods
Chemicals
The following chemicals were used in this study: LPS, 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT), Dulbecco’s Modified Eagle’s Medium (DMEM), Dex-SP (Sigma Aldrich). Also used in this study are as follows: fetal bovine serum (Zhejiang Tianhang Biotechnology Co., Ltd., Hangzhou, China); penicillin and streptomycin (Sangon Biotech, Shanghai Co., Ltd., Shanghai, China); enzyme-linked immunosorbent assay (ELISA) kits for TGF-β1, IL-10, MIP-1α, and RANTES (Boster Bio-engineering Co., Ltd., Wuhan, China); antibodies for IRAK-1, IRAK-4, TRAF6, TAK-1, and JNK (Cell Signaling Technology, Inc). Dex-SP was dissolved with aseptic technology in deionized water. The concentrations of Dex-SP (0, 1, 2, or 4 μM) were chosen based on our own preliminary experiments and literatures (Papoff et al. 1998). All other chemicals were reagent-grade or better.
Cell line and cell culture
Microglia BV-2 cells were obtained from the Institute of Basic Medical Sciences of the Chinese Academy of Medical Sciences (Beijing, China). BV-2 microglia cells were cultured in DMEM containing 10% fetal bovine serum, penicillin 100 U/mL, and streptomycin 100 mg/mL at 37 °C in a humidified atmosphere of 5% CO2. Cells were cultured in serum-free DMEM for at least 4 h before treatments.
MTT assay
BV-2 cell viability was assayed by MTT reduction assay (Sargent and Taylor 1989). The cells (1 × 104 cells/well) were incubated in 96-well plates. Twenty-four hours post-seeding, the cells were incubated with Dex-SP (0, 1, 2, or 4 μmol/L) for 23 h. Then, 20 μL of the MTT (5 mg/mL) solution was added to each well and were incubated for 4 h. Next, 100 mL of 10% SDS in HCl was added. The absorbance of each well was recorded at 570 nm in a Bio-Rad Model 630 microplate reader (Bio-Rad Laboratories, Richmond, CA, USA).
NO, cytokines, and chemokines assays
BV-2 cells (3 × 105 cells/well) were incubated in a 24-well plate overnight, Dex-SP (0, 1, 2, or 4 μM) was pre-added to culture medium for 3 h, then LPS (1 μg/mL) was added to each well and stimulated for 24 h. The culture media was collected, centrifuged to remove residual cells, aliquoted, and stored at − 80 °C before use. The production of NO was determined by measuring the content of nitrite—a major product of NO—accumulated in the cell supernatants using the Griess reagent according to the manufacturer’s instruction (Nanjing Jiancheng Bioengineering Institute, Nanjing, China).
Cytokines TGF-β1 and IL-10, and chemokines MIP-1α and RANTES secreted into the culture media were determined by ELISA kits. The absorbance at 450 nm was determined using a microplate reader (Model 550; Bio-Rad).
In vitro Transwell migration assay
Microglia BV-2 cells were seeded in the upper chambers with a cell density of 3 × 105 cells/well. Cells were allowed to adhere to the polycarbonate filters (8 μm pore) overnight at 37 °C in a humidified atmosphere of 5% CO2. Dex-SP (4 μM) was pre-added into the lower chambers for 3 h and then LPS was added into the lower chambers and cells were allowed to transmigrate into the lower chamber for 18 h. Cells that did not migrate and remained on the upper chamber surface were removed. Cells that had migrated to the lower surface were fixed with ice-cold methanol for 15 min and stained with 2% crystal violet for 30 min. Cells were viewed using an Olympus Imaging microscope equipped with a digital camera.
Western blot assay
Microglia BV-2 cells were seeded in 6-well plate with cell density of 3 × 105 cells/well. After pretreatment with Dex-SP (0, 1, 2, or 4 μM) for 3 h, LPS (1 μg/mL) was added and stimulated for 30 min. Cells were washed with ice-cold PBS, and lysed with a protein extraction kit (Beyotine Biotechnology, China) following the manufacturer’s instructions. Equal amounts of protein (20 μg) from each sample were subjected to 10% SDS-PAGE and transferred on nitrocellulose membranes. Primary antibodies against total or phosphorylated forms of TRAF 6 (1:1000), TAK-1 (1:1000), JNK (1:2000), actin-β (1:1000), and horseradish peroxidase-conjugated secondary antibody were added to the membranes according to the manufacturer’s recommendations. The immunoblots were developed using the Amersham enhanced chemiluminescence (ECL) system. The optical density of the bands was measured using the IPP software.
Statistical analysis
Assay data are expressed as the mean ± standard error (S.D.) obtained from at least three independent experiments. Statistical analysis was conducted using Kruskal-Wallis test (GraphPad Prism 7.0). The differences between the groups were considered to be statistically significant at a p value of less than 0.05.
Results
Dex-SP did not induce cytotoxicity in BV2 cells
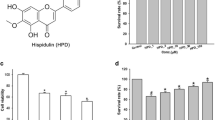
Prior to studying the effects of Dex-SP on BV2 cells, the MTT assay was applied to detect the cytotoxicity of Dex-SP to BV2 cells. After 27 h of incubation with different concentrations of Dex-SP, cell viability of BV2 cells was not markedly affected by Dex-SP treatment from 1 μM up to 4 μM (Fig. 1). These results indicated that the dosage of Dex-SP used in this study did not incite BV2 cytotoxicity.
Effect of Dex-SP on BV-2 cell viability. BV-2 cells were treated with different concentrations of Dex-SP (1, 2, or 4 μM) or equal volume of sterile deionized water (control group). An MTT assay was used to measure the cell viability. Viability of untreated cells was referred to as 100% viability. Results are expressed as the mean ± S.D. (calculated as a percentage of control, n = 4 per group) from three independent experiments. (*p value ≤ 0.05, **p value ≤ 0.01)
Dex-SP dampened LPS-induced RANTES, TGF-β1, and NO production in BV-2 microglia cells
In order to study whether Dex-SP could regulate the production of RANTES, TGF-β1, and NO in LPS-induced microglia BV2 cells, the cells were stimulated with or without LPS (1 μg/mL) for 24 h after 3-h pre-exposure to Dex-SP (0, 1, 2, and 4 μM, respectively). As shown in Fig. 2, LPS (1 μg/mL) increased the expression of RANTES (by 183.3 ± 27.5%, p < 0.01), TGF-β1 (by 14.1 ± 7.4%, p < 0.05), and NO (by 354.8 ± 12.8%, p < 0.01) as compared with control group, respectively. However, Dex-SP at 1, 2, and 4 μM significantly reduced the secretion of RANTES by 34.5 ± 5.3% (p < 0.05), 41.5 ± 14.3% (p < 0.05), and 45.6 ± 5.6% (p < 0.05), respectively (Fig. 2a). As shown in Fig. 2 b and Fig. 2 c, Dex-SP at 1, 2, and 4 μM lowered the secretion of TGF-β1 by 18.2 ± 5.2%, 19.4 ± 2.8% (p < 0.05), 17.6 ± 6.2% and NO by 43.7 ± 18.7%, 49.1 ± 22.8% (p < 0.01), 31.4 ± 10.1% (p < 0.05) as compared with LPS stimulation, respectively (Fig. 2). Furthermore, Dex-SP (4 μM) alone showed no inhibition on the production of the above inflammatory mediators.
Dex-SP inhibited RANTES, TGF-β1 and NO production in LPS-stimulated BV-2 cells. BV-2 cells were pretreated with various concentrations of Dex-SP (1, 2, or 4 μM) for 3 h or equal volume of sterile deionized water (control group) followed by incubation with LPS (1 μg/mL) for 24 h. The production of RANTES and TGF-β1 in the supernatant was analyzed by ELISA. NO production in the medium was detected by the Griess reagent. Results were normalized to basal cytokine levels or NO of untreated cells. Results are showed as mean ± S.D. (n = 4 per group) from three independent experiments. #p < 0.05, ##p < 0.01, ###p < 0.001 vs. control group. *p < 0.05, **p < 0.01, ***p < 0.001 vs. LPS group
Dex-SP increased LPS-reduced MIP-1α and IL-10 in BV-2 microglia cells
The effect of Dex-SP on the production of MIP-1α and IL-10 in BV-2 microglial cells was next analyzed. As show in Fig. 3, LPS reduced production of IL-10 by 41.3 ± 14.4% (p < 0.01) and MIP-1α by 11.3 ± 4.46% (p < 0.05) as compared with control group, respectively (Fig. 3a, b). However, Dex-SP only at 4 μM upregulated IL-10 (by 34.1 ± 7.7%, p < 0.05) and MIP-1α (by 8.4 ± 0.79%, p < 0.05) as compared with LPS group. Interestingly, Dex-SP (4 μM) alone reduced production of IL-10 by 37.3 ± 9.7% as compared with control group (p < 0.05, Fig. 3a), but it had no effect on MIP-1α production (p > 0.05) (Fig. 3b).
Dex-SP increased IL-10 and MIP-1α in LPS-induced BV-2 microglia cells. BV-2 cells were pretreated with various concentrations of Dex-SP (1, 2, or 4 μM) or equal volume of sterile deionized water (control group) for 3 h followed by incubation with LPS (1 μg/mL) for 24 h. The production of IL-10 and MIP-1α in the supernatant was analyzed by ELISA. Results were normalized to basal IL-10 and MIP-1α levels of untreated cells. Results are showed as mean ± S.D. (n = 4 per group) from three independent experiments. #p < 0.05, ##p < 0.01, ###p < 0.001 vs. control group. *p < 0.05, **p < 0.01, ***p < 0.001 vs. LPS group
Dex-SP mitigated LPS-induced BV-2 cell migration
Transwell assay was used to measure the effect of Dex-SP on the LPS-induced BV-2 cell migration. As shown in Fig. 4, LPS increased migration of BV-2 cell by 3.2 ± 0.7 times as compared to the control group (p < 0.001). However, pretreatment of BV-2 microglia cells with high dosage of Dex-SP (4 μM) was effective in inhibiting LPS-induced migration (p < 0.01, Fig. 4a, b). As shown in Fig. 4, Dex-SP alone did not alter BV-2 cell migration as compared with the control. This result suggests that Dex-SP can inhibit LPS-induced migration of BV-2 microglia.
Dex-SP inhibited migration of BV-2 microglia cell in vitro. The migration of BV-2 cells was detected by Transwell migration assay. a The quantitative analysis showed a decrease in the migration of BV-2 microglia with Dex-SP (4 μM) treatment. b Light microscopy images of BV-2 cells treated with equal volume of sterile deionized water (control group), LPS (1 μg/mL), Dex-SP (4 μM), or Dex-SP (4 μM) + LPS (1 μg/mL) were shown (scale bar, 50 μm). Data are shown as mean ± S.D. (n = 4 per group), #p < 0.05, ##p < 0.01, ###p < 0.001 vs. control group. *p < 0.05, **p < 0.01, ***p < 0.001 vs. LPS group
Dex-SP ameliorates LPS-induced degradation of IRAK-1 and IRAK-4, and the activation of TRAF6, TAK-1, and JNK
To further investigate the anti-neuroinflammation and migration mechanism of Dex-SP, the effect of Dex-SP on the expression of proteins in the IRAK-1,4/TRAF6/TAK-1/JNK signaling pathway in LPS-stimulated BV-2 cells was assayed by western blotting analysis. As compared with the control group, LPS significantly decreased the expression of IRAK-1 (by 94.2 ± 1.6%, p < 0.001, Fig. 5a), IRAK-4 (by 49.9 ± 7.7%, p < 0.01, Fig. 5b), markedly increased the activation of TRAF6 (by 373.3 ± 4.9%, p < 0.001, Fig. 5c), p-TAK1 (by 198.6 ± 5.8%, p < 0.001, Fig. 5d), and completely reversed the expression of p-JNK (p < 0.001, Fig. 5e) in BV-2 microglial cells. However, pretreatment with Dex-SP markedly inhibit the LPS-induced degradation of IRAK-1 and IRAK-4, and blocked the LPS-induced increase in TRAF6, p-TAK1, and p-JNK expression in BV-2 microglial cells (Fig. 5).
Dex-SP inhibited LPS-induced degradation of IRAK-1 and IRAK-4, and the activation of TRAF6, TAK-1, and JNK. BV-2 microglia were treated with Dex-SP (1, 2, or 4 μM) or equal volume of sterile deionized water (control group) for 3 h followed by stimulating with LPS (1 μg/mL) for 30 min. Cell lysates were prepared and analyzed for IRAK-1 (a), IRAK-4 (b), TRAF6 (c), TAK-1 (d), and JNK (e) by western blotting. The quantification of western blot results proteins was analyzed by Image-Pro Plus (IPP) software. Data shown are typical of three independent experiments with similar results. Data are shown as mean ± S.D. (n = 3 per group). #p < 0.05, ##p < 0.01, ###p < 0.001 vs. control group; *p < 0.05, **p < 0.01, ***p < 0.001 vs. LPS group
Discussion
Abnormal neuroinflammation triggered by over-activated microglia is closely linked with several neurological diseases such as tumors, stroke, Alzheimer’s disease, multiple sclerosis, and trauma (Chao et al. 1992; Krupinski et al. 1996; Nicoletti et al. 1998; Kim and Joh 2006; Lim and Zhu 2006; Town et al. 2008). Disordered inflammatory mediator production such as the increase of RANTES, TGF-β, NO and the decrease of MIP-1α and IL-10 promotes neuroinflammation via recruiting leukocytes as well as glial cells to sites of injury of CNS (Saukkonen et al. 1990; Baggiolini et al. 1994; Qiu and Li 2015). Thus, therapeutic targeting of suppression of microglia-mediated neuroinflammation may allow for control of potentially injurious neuroinflammatory responses.
Dex, a widely used anti-inflammatory drug, also has been used in the clinic to control acute bacterial meningitis, several non-infectious, and infectious neuropathologies (Chaudhuri 2004). Dex inhibits inflammatory response by regulating the activity of transcription factors such as nuclear factor kappa B (NF-κB) and activating protein 1 (AP-1) (Chantong et al. 2012; Park et al. 2019). Moreover, high doses of Dex-SP are shown to reach detectable concentrations in the CNS (Yu et al. 2017). Although Dex and Dex-SP have similar clinical applications, there are still gaps in their mechanisms of action or biological responses (Siegal et al. 1988). For example, Dex has been shown to markedly eliminate spinal cord edema and have an inhibitory effect on PGE2 production; however, Dex-SP failed to reduce spinal cord edema and PGE2 synthesis (Siegal et al. 1988). Recently, Dex-SP has been widely used as a release agent from biomaterials to improve integration of the biomaterial with the host tissue (Morais et al. 2010; Vallejo-Heligon et al. 2014; Keeler et al. 2015). Moreover, Dex-SP has been used for brain implants to attenuate inflammation and the reactive tissue response around surgical implants (Duque Ede and Munhoz 2016; Kozai et al. 2016). Despite its widespread and long-term use, the direct effect of Dex-SP on microglial cells is still poorly understood.
Microglial cell line BV-2 is a valid substitute for primary microglia to test the efficacy of the potential of therapeutic compounds for neuroinflammatory disorders (Henn et al. 2009). In the present study, the effect of Dex-SP on the production of neuroinflammatory mediators was studied in LPS-stimulated BV-2 microglial cells. Our results showed that LPS potentiated the production of RANTES, TGF-β, and NO; however, Dex-SP significantly reduced the production of RANTES, TGF-β, and NO induced by LPS. Our results are in accordance with the previous studies (Zhou et al. 2007; Lu et al. 2008; Taka et al. 2015). The present results also showed that LPS slightly decreases IL-10 production, which is consistent with another group’s study (Zhang et al. 2017). However, Dex-SP at 4 μM markedly reversed the decrease of IL-10 induced by LPS. Surprisingly, our results showed that LPS decreased rather than increased the production of MIP-1α in BV-2 microglial cells after stimulation with LPS for 24 h (Fig. 3). In contrast to our results, Murphy et al. found that LPS (10 μg/mL) stimulation for 6 h promoted MIP-1α mRNA in BV-2 microglial (Murphy Jr. et al. 1995). The discrepancy may be related to the concentration of LPS used, the duration of stimulation, or the detected targets and methods. It is also known that microglia can be polarized, resulting in M1 (classic, inflammatory) or M2 (alternative, anti-inflammatory) phenotypes (Porta et al. 2009; Michels et al. 2017). The different ratio of M1 to M2 in the tested microglial cells may be another reason for the discrepancy. The precise mechanism of the discrepancy needs further study.
Activated microglial cells showed remarkable changes in behavior, such as migration. The present results also showed that LPS markedly augmented migration of BV-2 microglia. However, pretreatment with Dex-SP significantly blocked LPS-induced BV2 migration towards the lower layer area. Furthermore, the concentration of Dex-SP used also reversed the production of inflammatory cytokines and chemokines. The effect of Dex-SP blocking BV2 migration may be ascribed to modulating the production of cytokines and chemokines. The results are in line with others that Dex-SP retrodialysis reduces microglial response to implanted probes in vivo, blocks the production of NO, and acutely activates microglia cells (Meijer et al. 1998; Kozai et al. 2016). All of these results suggest that the Dex-SP has a potent anti-inflammatory effect on microglial cell.
IRAK-1 and IRAK-4, which possess serine/threonine kinase activity, play critical roles downstream of TLR4 signaling (Li et al. 2002; Song et al. 2009). After TLR4 stimulation, IRAK-1 and IRAK-4 combine and form myddosome complex, then IRAK-1 is phosphorylated, which leads to IRAK-1 hyperphosphorylation (Kawagoe et al. 2008; Lin et al. 2010; Gay et al. 2011). Hyperphosphorylated IRAK-1 is separated from the myddosome complex and combined with TRAF-6, followed by IRAK-1 ubiquitination and degradation, and ultimately activates TAK-1 (Cao et al. 1996a; Cao et al. 1996b; Kobayashi et al. 2002; Huang et al. 2004). The activation of TAK-1 then sensitizes JNK and leads to gene transcription of encoded inflammatory mediators (Gottipati et al. 2008; Dai et al. 2012). In this study, LPS increased the degradation of IRAK-1 and IRAK-4, followed by activation of TRAF6 and phosphorylation of TAK-1 and JNK-1 in BV-2 microglia. However, Dex-SP markedly inhibited LPS-induced degradation of IRAK-1 and IRAK-4, as well as the activation of TRAF6, TAK-1, and JNK-1.
Conclusion
Our results showed that Dex-SP inhibits the neuroinflammatory response and migration in LPS-activated BV-2 microglial by reducing the secretion of RANTES, TGF-β1, NO and increasing the production of MIP-1α as well as IL-10. The molecular mechanism of Dex-SP may be associated with inhibition of TRAF6/TAK-1/JNK signaling pathways mediated by IRAK-1 and IRAK-4. This study will help to elucidate the therapeutic effect of Dex-SP on patients with neuroinflammation and reduce its side effects in the treatment process.
References
Baggiolini M, Dewald B, Moser B (1994) Interleukin-8 and related chemotactic cytokines—CXC and CC chemokines. Adv Immunol 55:97–179
Cao Z, Henzel WJ, Gao X (1996a) IRAK: a kinase associated with the interleukin-1 receptor. Science 271:1128–1131
Cao Z, Xiong J, Takeuchi M, Kurama T, Goeddel DV (1996b) TRAF6 is a signal transducer for interleukin-1. Nature 383:443–446
Chantong B, Kratschmar DV, Nashev LG, Balazs Z, Odermatt A (2012) Mineralocorticoid and glucocorticoid receptors differentially regulate NF-kappaB activity and pro-inflammatory cytokine production in murine BV-2 microglial cells. J Neuroinflammation 9:260
Chao CC, Hu S, Molitor TW, Shaskan EG, Peterson PK (1992) Activated microglia mediate neuronal cell injury via a nitric oxide mechanism. J Immunol 149:2736–2741
Chaudhuri A (2004) Adjunctive dexamethasone treatment in acute bacterial meningitis. Lancet Neurol 3:54–62
Dai L, Aye Thu C, Liu XY, Xi J, Cheung PC (2012) TAK1, more than just innate immunity. IUBMB Life 64:825–834
Duque Ede A, Munhoz CD (2016) The pro-inflammatory effects of glucocorticoids in the brain. Front Endocrinol (Lausanne) 7:78
Flannery S, Bowie AG (2010) The interleukin-1 receptor-associated kinases: critical regulators of innate immune signalling. Biochem Pharmacol 80:1981–1991
Gay NJ, Gangloff M, O’Neill LA (2011) What the myddosome structure tells us about the initiation of innate immunity. Trends Immunol 32:104–109
Gottipati S, Rao NL, Fung-Leung WP (2008) IRAK1: a critical signaling mediator of innate immunity. Cell Signal 20:269–276
Hausmann EH, Berman NE, Wang YY, Meara JB, Wood GW, Klein RM (1998) Selective chemokine mRNA expression following brain injury. Brain Res 788:49–59
Henn A, Lund S, Hedtjarn M, Schrattenholz A, Porzgen P, Leist M (2009) The suitability of BV2 cells as alternative model system for primary microglia cultures or for animal experiments examining brain inflammation. ALTEX 26:83–94
Huang Q, Yang J, Lin Y, Walker C, Cheng J, Liu ZG, Su B (2004) Differential regulation of interleukin 1 receptor and Toll-like receptor signaling by MEKK3. Nat Immunol 5:98–103
Kawagoe T, Sato S, Matsushita K, Kato H, Matsui K, Kumagai Y, Saitoh T, Kawai T, Takeuchi O, Akira S (2008) Sequential control of Toll-like receptor-dependent responses by IRAK1 and IRAK2. Nat Immunol 9:684–691
Keeler GD, Durdik JM, Stenken JA (2015) Effects of delayed delivery of dexamethasone-21-phosphate via subcutaneous microdialysis implants on macrophage activation in rats. Acta Biomater 23:27–37
Kim YS, Joh TH (2006) Microglia, major player in the brain inflammation: their roles in the pathogenesis of Parkinson’s disease. Exp Mol Med 38:333–347
Kobayashi K, Hernandez LD, Galan JE, Janeway CA Jr, Medzhitov R, Flavell RA (2002) IRAK-M is a negative regulator of Toll-like receptor signaling. Cell 110:191–202
Kozai TDY, Jaquins-Gerstl AS, Vazquez AL, Michael AC, Cui XT (2016) Dexamethasone retrodialysis attenuates microglial response to implanted probes in vivo. Biomaterials 87:157–169
Kreutzberg GW (1996) Microglia: a sensor for pathological events in the CNS. Trends Neurosci 19:312–318
Krupinski J, Kumar P, Kumar S, Kaluza J (1996) Increased expression of TGF-beta 1 in brain tissue after ischemic stroke in humans. Stroke 27:852–857
Li S, Strelow A, Fontana EJ, Wesche H (2002) IRAK-4: a novel member of the IRAK family with the properties of an IRAK-kinase. Proc Natl Acad Sci U S A 99:5567–5572
Lim H, Zhu YZ (2006) Role of transforming growth factor-beta in the progression of heart failure. Cell Mol Life Sci 63:2584–2596
Lin SC, Lo YC, Wu H (2010) Helical assembly in the MyD88-IRAK4-IRAK2 complex in TLR/IL-1R signalling. Nature 465:885–890
Lopes PC (2016) LPS and neuroinflammation: a matter of timing. Inflammopharmacology 24:291–293
Lu YC, Yeh WC, Ohashi PS (2008) LPS/TLR4 signal transduction pathway. Cytokine 42:145–151
Meijer OC, de Lange EC, Breimer DD, de Boer AG, Workel JO, de Kloet ER (1998) Penetration of dexamethasone into brain glucocorticoid targets is enhanced in mdr1A P-glycoprotein knockout mice. Endocrinology 139:1789–1793
Michels M, Sonai B, Dal-Pizzol F (2017) Polarization of microglia and its role in bacterial sepsis. J Neuroimmunol 303:90–98
Morais JM, Papadimitrakopoulos F, Burgess DJ (2010) Biomaterials/tissue interactions: possible solutions to overcome foreign body response. AAPS J 12:188–196
Murphy GM Jr, Jia XC, Song Y, Ong E, Shrivastava R, Bocchini V, Lee YL, Eng LF (1995) Macrophage inflammatory protein 1-alpha mRNA expression in an immortalized microglial cell line and cortical astrocyte cultures. J Neurosci Res 40:755–763
Nicoletti F, Di Marco R, Patti F, Reggio E, Nicoletti A, Zaccone P, Stivala F, Meroni PL, Reggio A (1998) Blood levels of transforming growth factor-beta 1 (TGF-beta1) are elevated in both relapsing remitting and chronic progressive multiple sclerosis (MS) patients and are further augmented by treatment with interferon-beta 1b (IFN-beta1b). Clin Exp Immunol 113:96–99
Papoff P, Christensen RD, Harcum J, Li Y (1998) In vitro effect of dexamethasone phosphate on hematopoietic progenitor cells in preterm infants. Arch Dis Child Fetal Neonatal Ed 78:F67–F69
Park MJ, Park HS, You MJ, Yoo J, Kim SH, Kwon MS (2019) Dexamethasone induces a specific form of ramified dysfunctional microglia. Mol Neurobiol 56:1421–1436
Porta C, Rimoldi M, Raes G, Brys L, Ghezzi P, Di Liberto D, Dieli F, Ghisletti S, Natoli G, De Baetselier P, Mantovani A, Sica A (2009) Tolerance and M2 (alternative) macrophage polarization are related processes orchestrated by p50 nuclear factor kappaB. Proc Natl Acad Sci U S A 106:14978–14983
Qiu D, Li XN (2015) Pioglitazone inhibits the secretion of proinflammatory cytokines and chemokines in astrocytes stimulated with lipopolysaccharide. Int J Clin Pharmacol Ther 53:746–752
Rahimifard M, Maqbool F, Moeini-Nodeh S, Niaz K, Abdollahi M, Braidy N, Nabavi SM, Nabavi SF (2017) Targeting the TLR4 signaling pathway by polyphenols: a novel therapeutic strategy for neuroinflammation. Ageing Res Rev 36:11–19
Rohdewald P, Mollmann H, Barth J, Rehder J, Derendorf H (1987) Pharmacokinetics of dexamethasone and its phosphate ester. Biopharm Drug Dispos 8:205–212
Sargent JM, Taylor CG (1989) Appraisal of the MTT assay as a rapid test of chemosensitivity in acute myeloid leukaemia. Br J Cancer 60:206–210
Saukkonen K, Sande S, Cioffe C, Wolpe S, Sherry B, Cerami A, Tuomanen E (1990) The role of cytokines in the generation of inflammation and tissue damage in experimental gram-positive meningitis. J Exp Med 171:439–448
Schoneveld OJ, Gaemers IC, Lamers WH (2004) Mechanisms of glucocorticoid signalling. Biochim Biophys Acta 1680:114–128
Schweingruber N, Reichardt SD, Luhder F, Reichardt HM (2012) Mechanisms of glucocorticoids in the control of neuroinflammation. J Neuroendocrinol 24:174–182
Siegal T, Siegal T, Shohami E, Shapira Y (1988) Comparison of soluble dexamethasone sodium phosphate with free dexamethasone and indomethacin in treatment of experimental neoplastic spinal cord compression. Spine (Phila Pa 1976) 13:1171–1176
Song KW, Talamas FX, Suttmann RT, Olson PS, Barnett JW, Lee SW, Thompson KD, Jin S, Hekmat-Nejad M, Cai TZ, Manning AM, Hill RJ, Wong BR (2009) The kinase activities of interleukin-1 receptor associated kinase (IRAK)-1 and 4 are redundant in the control of inflammatory cytokine expression in human cells. Mol Immunol 46:1458–1466
Taka E, Mazzio EA, Goodman CB, Redmon N, Flores-Rozas H, Reams R, Darling-Reed S, Soliman KF (2015) Anti-inflammatory effects of thymoquinone in activated BV-2 microglial cells. J Neuroimmunol 286:5–12
Town T, Laouar Y, Pittenger C, Mori T, Szekely CA, Tan J, Duman RS, Flavell RA (2008) Blocking TGF-beta-Smad2/3 innate immune signaling mitigates Alzheimer-like pathology. Nat Med 14:681–687
Vallejo-Heligon SG, Klitzman B, Reichert WM (2014) Characterization of porous, dexamethasone-releasing polyurethane coatings for glucose sensors. Acta Biomater 10:4629–4638
Walker DG, Lue LF (2005) Investigations with cultured human microglia on pathogenic mechanisms of Alzheimer’s disease and other neurodegenerative diseases. J Neurosci Res 81:412–425
Yu AC, Neil SE, Quandt JA (2017) High yield primary microglial cultures using granulocyte macrophage-colony stimulating factor from embryonic murine cerebral cortical tissue. J Neuroimmunol 307:53–62
Zhang Q, Lu Y, Bian H, Guo L, Zhu H (2017) Activation of the alpha7 nicotinic receptor promotes lipopolysaccharide-induced conversion of M1 microglia to M2. Am J Transl Res 9:971–985
Zhou Y, Ling EA, Dheen ST (2007) Dexamethasone suppresses monocyte chemoattractant protein-1 production via mitogen activated protein kinase phosphatase-1 dependent inhibition of Jun N-terminal kinase and p38 mitogen-activated protein kinase in activated rat microglia. J Neurochem 102:667–678
Funding
This study was supported by the Foundation of Shanghai University of Medicine & Health Sciences (Talent Introduction Project 2018).
Author information
Authors and Affiliations
Contributions
Bin Hui, Liping Zhang, and Qinhua Zhou designed the experiments; Bin Hui, Xin Yao, Qinhua Zhou, and Liping Zhang performed parts of the experiments; Bin Hui, Qinhua Zhou, and Liping Zhang analyzed the data; Bin Hui, Qinhua Zhou, and Liping Zhang wrote the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing financial interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(TIFF 9.37 mb)
Rights and permissions
About this article
Cite this article
Hui, B., Yao, X., Zhang, L. et al. Dexamethasone sodium phosphate attenuates lipopolysaccharide-induced neuroinflammation in microglia BV2 cells. Naunyn-Schmiedeberg's Arch Pharmacol 393, 1761–1768 (2020). https://doi.org/10.1007/s00210-019-01775-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-019-01775-3