Abstract
Urotensin II (U-II) is a cyclic peptide that may be involved in cardiovascular dysfunction. In the present study, the acute effects of U-II on diastolic properties of the myocardium were investigated. Increasing concentrations of U-II (10−8 to 10−6 M) were added to rabbit papillary muscles in the absence (n = 15) or presence of: (1) damaged endocardial endothelium (EE; n = 9); (2) U-II receptor antagonist, urantide (10−5 M; n = 7); (3) nitric oxide (NO) synthase inhibitor, NG-Nitro-l-Arginine (10−5 M; n = 9); (4) cyclooxygenase inhibitor, indomethacin (10−5 M; n = 8); (5) NO synthase and cyclooxygenase inhibitors, NG-Nitro-l-Arginine (10−5 M) and indomethacin (10−5 M), respectively, (n = 8); or (6) protein kinase C (PKC) inhibitor, chelerythrine (10−5 M; n = 9). Passive length–tension relations were constructed before and after a single concentration of U-II (10−6 M; n = 3). U-II concentration dependently decreased inotropy and increased resting muscle length (RL). At 10−6 M, active tension decreased 13.8 ± 5.4%, and RL increased to 1.007 ± 0.001 L/L max. Correcting RL to its initial value resulted in an 18.1 ± 3.0% decrease in resting tension, indicating decreased muscle stiffness, which was also suggested by the down and rightward shift of the passive length–tension relation. This effect remained unaffected by EE damage and PKC inhibition. In contrast, the presence of urantide and NO inhibition abolished the effects of U-II on myocardial stiffness, while cyclooxygenase inhibition significantly attenuated them. U-II decreases myocardial stiffness, an effect that is mediated by the urotensin-II receptor, NO, and prostaglandins. This represents a novel mechanism of acute neurohumoral modulation of diastolic function, suggesting that U-II is an important regulator of cardiac filling.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Urotensin II (U-II) is a vasoactive peptide, first isolated from the urophysis of teleost fish (Bern et al. 1985), and recently cloned in several mammalian species, including humans (Conlon et al. 1996; Coulouarn et al. 1998, 1999; Douglas et al. 2000). U-II acts by binding to G-protein-coupled receptors that were first identified in the rat (GPR14; Marchese et al. 1995; Tal et al. 1995) and later in humans [urotensin-II (UT) receptor; Ames et al. 1999]. The G-protein associated with the UT receptor belongs to the Gq class (Opgaard et al. 2000), which is the same class of G-proteins that bind to AT1, ETA, and α-adrenergic receptors (Wheeler-Jones 2005).
U-II has been shown to have potent vasoactive properties depending on the vascular bed and the species tested (Bohm and Pernow 2002; Bottrill et al. 2000; Camarda et al. 2002; Douglas et al. 2000; Gardiner et al. 2001; Russell and Molenaar 2004; Stirrat et al. 2001). Additionally, U-II (Douglas et al. 2002; Matsushita et al. 2001), as well as its receptor (Ames et al. 1999), is highly expressed in the heart (cardiomyocytes) and blood vessels. Taking into consideration these facts, several experimental and clinical studies evaluated whether this peptide plays a role in cardiovascular regulation and the pathophysiology of heart failure (Douglas et al. 2002; Dschietzig et al. 2002; Gong et al. 2004; Johns et al. 2004; Russell et al. 2001, 2003; Tzanidis et al. 2003). However, the role of U-II within the myocardium remains poorly understood, particularly in the setting of disease.
Furthermore, U-II was reported to affect the process of cell growth in the heart. This peptide exerted mitogenic effects on smooth muscle cells (Sauzeau et al. 2001; Watanabe et al. 2001), induced collagen and fibronectin synthesis by cardiac fibroblasts, and caused cardiac hypertrophy (Tzanidis et al. 2003), thereby contributing to ventricular remodeling and deterioration of systolic and diastolic function, similarly to what has been described for other vasoconstrictor peptides such as angiotensin II (Ang II) and endothelin-1 (ET-1; Weber et al. 1994). These chronic effects have classically been considered the main mechanisms through which neurohumoral agents may influence the diastolic properties of the myocardium. However, some of these agents have been, over recent years, shown to acutely modulate myocardial stiffness. These include nitric oxide (NO; Heymes et al. 1999; Ito et al. 1997; Shah et al. 1994), ET-1 (Leite-Moreira et al. 2003), and Ang II (Leite-Moreira et al. 2006) but not ghrelin (Soares et al. 2006). In isolated cardiomyocytes, an increase in diastolic cell length is observed after exposure to a cGMP analogue or a NO donor, and in intact hearts, NO shifts downward the diastolic pressure–volume loop during filling, both indicating increased myocardial distensibility.
To further clarify this issue, we conducted the present study in rabbit papillary muscle with the aim of characterizing the diastolic effects of U-II and some of their underlying mechanisms. A preliminary report has recently appeared (Fontes-Sousa et al. 2006).
Material and methods
Animals and tissue preparation
This investigation conforms to the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication number 85-23, Revised 1996).
Functional experiments
Experimental preparation
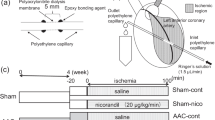
Isometric and isotonic contractions were measured in papillary muscles isolated from the right ventricle of rabbits. Male New Zealand white rabbits (Oryctolagus cuniculus; 1.4–2.7 kg; n = 53) were anesthetized with intravenous sodium pentobarbital (25 mg kg−1). A left thoracotomy was performed, and beating hearts were quickly excised and immersed in a modified Krebs–Ringer (KR) solution (composition in millimolar, 98 NaCl, 4.7 KCl, 2.4 MgSO4·7H2O, 1.2 KH2PO4, 4.5 glucose, 1.8 CaCl2·2H2O, 17 NaHCO3, 15 sodium pyruvate, 5 sodium acetate, and 0.02 atenolol) at 35°C with cardioplegic 2,3-butanedione monoxime (BDM; 3%) and 5% Newborn Calf Serum. Atenolol was used to prevent β-adrenergic mediated effects. The solutions were in equilibrium with 95% O2 and 5% CO2, to obtain a pH between 7.38 and 7.42.
The time from thoracotomy to dissection was ∼3 min. The right ventricle was opened, and papillary muscles were isolated by first dividing the chordae tendinae at the muscle tip and then freeing the muscle base and a small amount of surrounding myocardium from the ventricular wall. Only long, thin, uniformly cylindrical muscles were used.
After dissection, papillary muscles (n = 73; length, 4.3 ± 0.2 mm; weight, 3.4 ± 0.2 mg; preload, 3.4 ± 0.1 mN) were mounted vertically in a 10-ml plexiglass organ bath containing the aforementioned KR solution. The lower muscular end was fixed in a phosphorbronze clip, and the upper tendinous end was attached to an electromagnetic length–tension transducer (University of Antwerp, Belgium).
Preload was initially estimated according to muscle dimensions. After 10 min, muscles were stimulated at interstimulus interval of 1,670 ms and voltage of 10% above threshold by rectangular pulses of 5 ms duration through two platinum electrodes. Twenty minutes later, bathing solutions were replaced by corresponding KR solutions without BDM, and the muscle started to contract. One hour later, bathing solution was replaced by corresponding serum-free KR solution. During the next 2 h, the muscles were stabilized. Finally, the muscles were stretched to a muscle length at which active force development was maximal. At this point, this length (millimeter) known as maximum physiological length (L max), was measured with a microruler. During the experiment, changes in diastolic muscle length and muscle shortening were measured by the isotonic transducer. Protocols were initiated after obtaining two similar isotonic and isometric control twitches separated by a 10-min interval.
At the end of the experiment, the muscles were removed, lightly blotted, and then weighed. Muscle cross-sectional area was calculated by dividing the weight of the muscle by its length at L max. A cylindrical shape and a specific gravity of 1.0 were assumed (Leite-Moreira et al. 2006). Muscle tension was then expressed as force normalized per cross-sectional area (mN mm−2).
Experimental protocol
Effects of increasing concentrations of human U-II (hU-II; 10−8 to 10−6 M) on contraction, relaxation, and diastolic properties of the myocardium were studied in rabbit papillary muscles in control muscles with intact endocardial endothelium (EE), after selective removal of EE by a brief (1 s) immersion of the papillary muscle in a weak solution (0.5%) of the detergent Triton X-100 (Brutsaert et al. 1988, 1996), followed by abundant wash with Triton-free KR solution, and in the presence of: (1) urantide (C51H66N10O12S2; URT; 10−5 M), an antagonist of U-II receptor; (2) NG-Nitro l-Arginine (l-NNA; 10−5 M), a NO synthase inhibitor; (3) indomethacin (Indo; 10−5 M), a cyclooxygenase inhibitor; (4) NG-Nitro-l-Arginine plus Indo and (5) chelerythrine (CHE, 10−5 M), an inhibitor of protein kinase C (PKC). In a small subset of muscles (n = 5), the effects of U-II were tested in a KR solution containing nadolol (10−5 M) instead of atenolol. These substances were dissolved in the KR solution before the addition of U-II, and muscle twitches were recorded after a stable response was obtained, typically 15–20 min later. After that, U-II was added cumulatively without any washout between. Finally, in another small subset of muscles, passive length–tension relations were constructed in the absence and in the presence of the highest concentration of U-II. Of note, in each experimental protocol, all papillary muscles were obtained from different animals.
Data acquisition and analysis
Isotonic and isometric twitches were recorded and analyzed with dedicated software (University of Antwerp, Belgium). Selected parameters included: resting tension (RT; mN mm−2), active tension (AT; mN mm−2); maximal velocities of tension rise (dT/dt max; mN mm−2 s−1) and decline (dT/dt min; mN mm−2 s−1); peak isotonic shortening (PS; %L max); maximal velocities of shortening (dL/dt max; L maxs−1) and lengthening (dL/dt min; L maxs−1); time to half-relaxation (tHR, ms); and time to active tension (tAT; ms).
In the various protocols, results are given as percent change from baseline. For the parameters that are expressed as negative values (e.g. dT/dt min), such percent change refers to the absolute values. When a pharmacological inhibitor was used or the EE damaged, the term baseline refers to the performance in the presence of those inhibitors or after damage of EE, before the addition of U-II.
Drugs and materials
Drugs were obtained from the following sources: hU-II, Bachem (Bubendorf, Switzerland); urantide, Peptides International (Louisville, Kentucky, USA); all other chemicals, Sigma Chemical (St Louis, MO, USA). Stock solutions of all chemicals were dissolved in distilled water and prepared in aliquots at 100 times the final bath concentration, except for hU-II which stock concentration was 5.10−5 M. All stock solutions were stored at −20°C until use.
Statistical analysis
All values are given as mean ± standard error of mean (SE), and n represents the number of experiments. Effects of increasing concentrations of U-II alone on the different experimental parameters were analyzed by one-way repeated-measures analysis of variance (ANOVA). Effects of increasing concentrations of U-II under various experimental conditions were analyzed with a repeated-measures two-way ANOVA. Effects on the various parameters of a single concentration of the antagonists were analyzed with a paired t test. When significant differences were detected with any of the ANOVA tests, the Student–Newman–Keuls test was selected to perform pairwise multiple comparisons. A P value less than 0.05 was considered to be significant.
Results
Baseline performance of rabbit papillary muscles was similar in all experimental protocols. Mean values of the contractile parameters from the 73 papillary muscles were as follows: AT, 19.8 ± 1.3 mN mm−2; dT/dt max, 135.2 ± 8.3 mN mm−2 s−1; dT/dt min, −113.1 ± 6.7 mN mm−2 s−1; PS, 13.0 ± 0.7% of L max; dL/dt max, 1.0 ± 0.1 L maxs−1; dL/dt min, −3.3 ± 0.2 L maxs−1; tAT, 243.1 ± 5.5 ms; tHR, 382.6 ± 8.8 ms.
Effects of increasing concentrations of U-II (10−8, 10−7, and 10−6 M) on papillary muscle function are summarized and illustrated in Fig. 1, where it can be seen that U-II induced concentration-dependent negative inotropic (AT, dT/dt max) and lusitropic (dT/dt min) effects. When the papillary muscle was stimulated with the two lowest concentrations of U-II (10−8 M and 10−7 M), muscle tension gradually decreased to reach a maximal decrease within 15 min for each one (Fig. 2). When the papillary muscle was stimulated with the higher concentration of U-II (10−6 M), muscle tension reached the maximal decrease within 30 min (Fig. 2). The highest concentration (10−6 M) of U-II decreased 13.8 ± 5.4% AT (Fig. 1a), 12.0 ± 5.3% dT/dt max (Fig. 1a), 15.5 ± 4.4% dT/dt min (Fig. 1a), 11.2 ± 3.8% PS, 9.7 ± 3.3% dl/dt 2max, 13.4 ± 3.5% dl/dt min, 3.7 ± 1.3% tHR, and 3.8 ± 1.6% tAT (onset of relaxation).
Effect of increasing concentrations of urotensin II (U-II, 10−8 to 10−6 M, n = 15) on a active tension (AT), peak rates of tension rise and decline (dT/dt max and dT/dt min, respectively) and b resting muscle length (L/L max). Data are mean ± SE, expressed as percent variation from baseline. P < 0.05: α vs baseline, β vs 10−8 M U-II, γ vs 10−7 M U-II. c Representative example of isotonic twitches at baseline and in the presence of increasing concentrations of U-II
With regard to the diastolic properties of the myocardium, we observed that U-II progressively increased resting muscle length (Fig. 1b) at a constant RT. Correcting, at the end of the experiment, muscle length to its initial value resulted in an 18.1 ± 3.0% decrease in RT, without altering the other contractile parameters. This indicates an increase in muscle distensibility or, on the other hand, a decrease in muscle stiffness. Figure 3 illustrates mean length–tension relations in the absence and presence of the highest concentration of U-II, where it can be seen that the increase in muscle distensibility is observed over the entire range of muscle lengths studied.
The effect of U-II was not significantly different in the muscles in which atenolol was replaced by nadolol in the KR solution.
Effects of U-II after damaging the EE, in presence of a selective UT receptor antagonist (URT), or after inhibition of cyclooxygenase (Indo), NO synthase (l-NNA), or PKC (CHE) are illustrated in Figs. 4, 5 and 6.
Effect of increasing concentrations of urotensin II (U-II, 10−8 to 10−6 M) on a active tension and b passive muscle length (L/L max) in the absence (n = 15) or presence of selective UT receptor antagonist (urantide; URT, 10−5 M, n = 7) or PKC inhibitor chelerythrine (CHE, 10−5 M, n = 9). Data are mean ± SE, expressed as percent variation from baseline. P < 0.05: α vs baseline, β vs 10−8 M U-II, γ vs 10−7 M U-II, * vs U-II alone
Effect of increasing concentrations of urotensin II (U-II; 10−8 to 10−6 M) on a active tension and b passive muscle length (L/L max) in the absence (n = 15) or presence of NO synthase and cyclooxygenase inhibition (l-NNA, 10−5 M and Indo, 10−5 M, respectively, n = 8), NO synthase inhibition (l-NNA, 10−5 M, n = 9), cyclooxygenase inhibition (Indo, 10−5 M, n = 8) or damaged endocardial endothelium (TRX, n = 9). Data are mean ± SE, expressed as percent variation from baseline. P < 0.05: α vs baseline, β vs 10−8 M U-II, γ vs 10−7 M U-II, * vs U-II alone
Effects of urotensin II (U-II; 10−6 M) on a resting tension and b resting muscle length (L/L max) in the absence (n = 15) or presence of selective UT receptor antagonist (urantide; URT, 10−5 M, n = 7), NO synthase and cyclooxygenase inhibition (l-NNA, 10−5 M and Indo, 10−5 M, respectively, n = 8), NO synthase inhibition (l-NNA, 10−5 M, n = 9), cyclooxygenase inhibition (Indo, 10−5 M, n = 8), damaged endocardial endothelium (TRX, n = 9) or PKC inhibitor chelerythrine (CHE, 10−5 M, n = 9). Data are mean ± SE, expressed as percent variation from baseline. P < 0.05: α vs baseline, β vs U-II alone
Selective destruction of the EE or the presence of CHE resulted in a significant decrease in AT by 45.4 ± 5.7% and 44.7 ± 4.3%, respectively. The other inhibitors did not significantly modify per se any of the analyzed contractile parameters.
None of the agents significantly altered the effects of U-II on myocardial contractility (AT, dT/dt max, PS, dL/dt max), relaxation (dT/dt min, dL/dt min) or muscle twitch duration (tAT, tHR). Effects on AT, dT/dt max, and dT/dt min are illustrated in Figs. 4a and 5a. On the contrary, URT, l-NNA, and Indo significantly attenuated the effects of U-II on myocardial distensibility, although these effects were not affected by the presence of CHE or EE removal (Figs. 4b and 5b). In the presence of Indo, the effect of U-II on muscle length was markedly reduced, leading to a decrease in passive tension of only 11.6 ± 3.1% (Fig. 6). On the other hand, in presence of URT and l-NNA, the effects of U-II on passive muscle length and RT were no more statistically significant, having been totally abolished when l-NNA and Indo were simultaneously present in the bath (Fig. 6).
Discussion
This study clearly demonstrates that U-II induces a significant concentration-dependent acute increase in myocardial distensibility. This effect is attenuated by cyclooxygenase inhibition and completely abolished by U-II receptor blockade or NO synthase inhibition. This suggests that such effect is mediated by UT receptor stimulation and dependent of NO and prostaglandins release.
U-II binds to a 389-amino acid G-protein-coupled receptor termed UT (Ames et al. 1999). The UT receptor is coupled to the Gαq/11 signal transduction pathway, the same of AT1, ETA, and α-adrenoceptors, which are linked to phospholipase C activation and the consequent increase in inositol trisphosphate and diacylglycerol, with mobilization of intracellular Ca2+ (Ames et al. 1999; Opgaard et al. 2000; Tzanidis et al. 2003). In the isolated rabbit aorta, the vasoconstrictor effect of U-II is mediated by a phospholipase C-dependent increase in inositol phosphates, probably mediated by a Gq-protein-coupled receptor (Opgaard et al. 2000). On the other hand, in the rat aorta, the contraction induced by U-II is mediated by a Ca2+/calmodulin/myosin light chain (MLC) kinase system and modulated by the Ca2+ sensitization mechanisms to increase MLC phosphorylation (Tasaki et al. 2004).
In the present study, we found a mild concentration-dependent negative inotropic effect that was not altered either by EE removal or any of the used inhibitors. A similar effect was previously described in isolated canine cardiomyocytes (Morimoto et al. 2002), while a more pronounced one was reported in vivo first in nonhuman primates (Ames et al. 1999) and later in rats (Hassan et al. 2003), in response to systemic infusion of U-II, which was attributed to coronary vasoconstriction. On the contrary, in human isolated right atrial trabeculae (Russell et al. 2001) and in rat isolated left ventricular myocardium (Gong et al. 2004), a slight positive inotropic effect via a PKC-dependent mechanism (Russell and Molenaar 2004) was described. These discrepancies may be due to differences in the experimental preparation or the animal species used. Overall, however, the inotropic effects of U-II in vitro described in the literature are mild and of much smaller magnitude than those of for instance ET-1 and β-adrenergic stimulation (Russell 2004).
Myocardial stiffness is an important determinant of ventricular filling and, therefore, of diastolic function (Leite-Moreira 2006). As outlined in the introduction, classically, it was considered that neurohumoral agents only could influence the diastolic properties of the myocardium through chronic changes, as those induced by fibrosis and hypertrophy (Kass et al. 2004). More recent studies, however, have shown that diastolic stiffness may be acutely modulated by NO (Heymes et al. 1999; Shah et al. 1994), ET-1 (Leite-Moreira et al. 2003), Ang II (Leite-Moreira et al. 2006), and β-adrenoceptor stimulation or protein kinase A (PKA) activation (Borbely et al. 2005; Fukuda et al. 2005; van Heerebeek et al. 2006; Yamasaki et al. 2002), while the present study demonstrates that the same is true for U-II.
Several actions of NO on myocardial contractile function have been reported, including changes in relaxation and diastolic properties of the myocardium. NO production and release have been detected in the sequence of endothelial UT receptor stimulation and seems to modulate the U-II-induced vasoconstriction in some experimental preparations (Ishihata et al. 2006). NO has been previously shown to increase myocardial distensibility, presumably as a result of protein kinase G (PKG)-mediated phosphorylation of myofilaments (Prendergast et al. 1997; Shah et al. 1994), which could explain the effects observed in the present study of U-II on this property.
UT receptor shares some subcellular pathways and interacts with ETA and AT1 receptors (Li et al. 2005; Wang et al. 2007). With regard to diastolic function, we have recently shown, in the same animal species, that both ETA (Leite-Moreira et al. 2003) and AT1 (Leite-Moreira et al. 2006) stimulation increase myocardial distensibility through PKC and Na+/H+ exchanger-mediated effects. It is also important to underline that while the effect of ET-1 on myocardial distensibility was only observed in acutely afterloaded twitches, in the case of Ang II it was present even in isotonic contractions. With regard to U-II, the results of the present study indicate that its effects on myocardial distensibility are not mediated by PKC but instead dependent on UT receptor stimulation and NO and prostaglandins release. Interestingly, however, even if these agents are released by the endothelium, EE removal did not alter the effects of U-II on myocardial distensibility. This apparent discrepancy can be easily explained if we take into account that the microvascular coronary endothelium, another important source of NO and prostaglandins (Brutsaert 2003), remained intact even after removal of the EE. Note that NO can also be released by the cardiomyocytes themselves (Massion et al. 2003). Data related with the expression of the UT receptor in the heart support this hypothesis. In fact, expression of this receptor was shown in cardiomyocytes and vascular endothelial cells but not yet in the EE (Russell 2004).
Finally, concerning the pathophysiologic relevance of our findings, we must point out that decreases of 18% in passive tension of the isolated muscle indicate that U-II might allow the ventricle to reach the same diastolic volume with almost 20% lower filling pressures, which is undoubtedly a potentially important adaptation mechanism. As the acute effects of U-II on diastolic function were determined in an in vitro model, this excludes systemic and humoral effects of U-II; consequently, the effects of U-II in vivo, where other important adaptation mechanisms also affect diastolic filling pressures, may differ from those reported in this paper.
These acute beneficial effects of U-II on diastolic function may become deleterious on the long term due to its role in the promotion of cardiac fibrosis and hypertrophy, when its levels remain chronically elevated (Bousette et al. 2006; Yamamoto et al. 2002), and by its effects on coronary arteries by accelerating the development of atherosclerosis, thereby leading to coronary artery disease (Watanabe et al. 2006). Furthermore, we have to consider that a sustained increase in myocardial length, as the one promoted by U-II, might contribute to ventricular dilatation, which is another important feature of ventricular remodeling.
In conclusion, this study describes, for the first time, the modulation of diastolic function by U-II, which increases myocardial distensibility, an effect that requires the activation of UT receptor and is mediated by NO and prostaglandins release. This novel effect of U-II broadens our concepts with regard to the acute neurohumoral modulation of diastolic function and represents a potentially powerful regulator of cardiac filling. In addition, taking into account that U-II and its receptor exhibits increased expression in cardiac tissue and plasma in human heart failure, these results might help to better understand the pathophysiology of this syndrome.
References
Ames RS, Sarau HM, Chambers JK, Willette RN, Aiyar NV, Romanic AM, Louden CS, Foley JJ, Sauermelch CF, Coatney RW, Ao Z, Disa J, Holmes SD, Stadel JM, Martin JD, Liu WS, Glover GI, Wilson S, McNulty DE, Ellis CE, Elshourbagy NA, Shabon U, Trill JJ, Hay DW, Ohlstein EH, Bergsma DJ, Douglas SA (1999) Human urotensin-II is a potent vasoconstrictor and agonist for the orphan receptor GPR14. Nature 401:282–286
Bern HA, Pearson D, Larson BA, Nishioka RS (1985) Neurohormones from fish tails: the caudal neurosecretory system. I. “Urophysiology” and the caudal neurosecretory system of fishes. Recent Prog Horm Res 41:533–552
Bohm F, Pernow J (2002) Urotensin II evokes potent vasoconstriction in humans in vivo. Br J Pharmacol 135:25–27
Borbely A, van der Velden J, Papp Z, Bronzwaer JG, Edes I, Stienen GJ, Paulus WJ (2005) Cardiomyocyte stiffness in diastolic heart failure. Circulation 111: 774–781
Bottrill FE, Douglas SA, Hiley CR, White R (2000) Human urotensin-II is an endothelium-dependent vasodilator in rat small arteries. Br J Pharmacol 130: 1865–1870
Bousette N, Pottinger J, Ramli W, Ohlstein EH, Dhanak D, Douglas SA, Giaid A (2006) Urotensin-II receptor blockade with SB-611812 attenuates cardiac remodeling in experimental ischemic heart disease. Peptides 11:2919–2926
Brutsaert DL (2003) Cardiac endothelial-myocardial signaling: its role in cardiac growth, contractile performance, and rhythmicity. Physiol Rev 83:59–115
Brutsaert DL, Meulemans AL, Spido KR, Sys SU (1988) Effects of damaging endocardial surface on the mechanical performance of isolated cardiac muscle. Circ Res 62:358–366
Brutsaert DL, De Keulenaer GW, Fransen P, Mohan P, Kaluza GL, Andries LJ, Rouleau JL, Sys SU (1996) The cardiac endothelium: functional morphology, development, and physiology. Prog Cardiovasc Dis 39:239–262
Camarda V, Rizzi A, Calo G, Gendron G, Perron SI, Kostenis E, Zamboni P, Mascoli F, Regoli D (2002) Effects of human urotensin II in isolated vessels of various species; comparison with other vasoactive agents. Naunyn Schmiedebergs Arch Pharmacol 365:141–149
Conlon JM, Yano K, Waugh D, Hazon N (1996) Distribution and molecular forms of urotensin II and its role in cardiovascular regulation in vertebrates. J Exp Zool 275:226–238
Coulouarn Y, Lihrmann I, Jegou S, Anouar Y, Tostivint H, Beauvillain JC, Conlon JM, Bern HA, Vaudry H (1998) Cloning of the cDNA encoding the urotensin II precursor in frog and human reveals intense expression of the urotensin II gene in motoneurons of the spinal cord. Proc Natl Acad Sci USA 95:15803–15808
Coulouarn Y, Jegou S, Tostivint H, Vaudry H, Lihrmann I (1999) Cloning, sequence analysis and tissue distribution of the mouse and rat urotensin II precursors. FEBS Lett 457:28–32
Douglas SA, Sulpizio AC, Piercy V, Sarau HM, Ames RS, Aiyar NV, Ohlstein EH, Willette RN (2000) Differential vasoconstrictor activity of human urotensin-II in vascular tissue isolated from the rat, mouse, dog, pig, marmoset and cynomolgus monkey. Br J Pharmacol 131:1262–1274
Douglas SA, Tayara L, Ohlstein EH, Halawa N, Giaid A (2002) Congestive heart failure and expression of myocardial urotensin II. Lancet 359:1990–1997
Dschietzig T, Bartsch C, Pregla R, Zurbrugg HR, Armbruster FP, Richter C, Laule M, Romeyke E, Neubert C, Voelter W, Baumann G, Stangl K (2002) Plasma levels and cardiovascular gene expression of urotensin-II in human heart failure. Regul Pept 110:33–38
Fontes-Sousa AP, Brás-Silva C, Pires AP, Monteiro-Sousa D, Leite-Moreira AF (2006). Urotensin-II: a novel neurohumoral modulator of diastolic function. Circulation 114:II–315
Fukuda N, Wu Y, Nair P, Granzier HL (2005) Phosphorylation of titin modulates passive stiffness of cardiac muscle in a titin isoform-dependent manner. J Gen Physiol 125:257–271
Gardiner SM, March JE, Kemp PA, Davenport AP, Bennett T (2001) Depressor and regionally-selective vasodilator effects of human and rat urotensin II in conscious rats. Br J Pharmacol 132:1625–1629
Gong H, Wang YX, Zhu YZ, Wang WW, Yao T, Zhu YC (2004) Cellular distribution of GPR14 and the positive inotropic role of urotensin II in the myocardium in adult rat. J Appl Physiol 97:2228–2235
Hassan GS, Chouiali F, Saito T, Hu F, Douglas SA, Ao Z, Willette RN, Ohlstein EH, Giais A (2003) Effect of human urotensin-II infusion on hemodynamics and cardiac function. Can J Physiol Pharm 81:125–128
Heymes C, Vanderheyden M, Bronzwaer JG, Shah AM, Paulus WJ (1999) Endomyocardial nitric oxide synthase and left ventricular preload reserve in dilated cardiomyopathy. Circulation 99:3009–3016
Ishihata A, Sakai M, Katano Y (2006) Vascular contractile effect of urotensin II in young and aged rats: influence of aging and contribution of endothelial nitric oxide. Peptides 27:80–86
Ito N, Bartunek J, Spitzer KW, Lorell BH (1997) Effects of the nitric oxide donor sodium nitroprusside on intracellular pH and contraction in hypertrophied myocytes. Circulation 95:2303–2311
Johns DG, Ao Z, Naselsky D, Herold CL, Maniscalco K, Sarov-Blat L, Steplewski K, Aiyar N, Douglas SA (2004) Urotensin-II-mediated cardiomyocyte hypertrophy: effect of receptor antagonism and role of inflammatory mediators. Naunyn Schmiedebergs Arch Pharmacol 370:238–250
Kass DA, Bronzwaer JG, Paulus WJ (2004) What mechanisms underlie diastolic dysfunction in heart failure? Circ Res 94:1533–1542
Leite-Moreira AF (2006) Current perspectives in diastolic dysfunction and diastolic heart failure. Heart 92:712–718
Leite-Moreira AF, Bras-Silva C, Pedrosa CA, Rocha-Sousa AA (2003) ET-1 increases distensibility of acutely loaded myocardium: a novel ETA and Na+/H+ exchanger-mediated effect. Am J Physiol Heart Circ Physiol 284:H1332–1339
Leite-Moreira AF, Castro-Chaves P, Pimentel-Nunes P, Lima-Carneiro A, Guerra MS, Soares JB, Ferreira-Martins J (2006) Angiotensin II acutely decreases myocardial stiffness: a novel AT1, PKC and Na+/H+ exchanger-mediated effect. Br J Pharmacol 147:690–697
Li J, Wang J, Russell FD, Molenaar P (2005) Activation of calcineurin in human failing heart ventricle by endothelin-1, angiotensin II and urotensin II. Br J Pharmacol 145:432–440
Marchese A, Heiber M, Nguyen T, Heng HH, Saldivia VR, Cheng R, Murphy PM, Tsui LC, Shi X, Gregor P, George SR, O’Dwd BF, Docherty JM (1995) Cloning and chromosomal mapping of three novel genes, GPR9, GPR10, and GPR14, encoding receptors related to interleukin 8, neuropeptide Y, and somatostatin receptors. Genomics 29:335–344
Massion PB, Feron O, Dessy C, Balligand J-L (2003) Nitric oxide and cardiac function. Ten tears after, and continuing. Circ Res 93:388–398
Matsushita M, Shichiri M, Imai T, Iwashina M, Tanaka H, Takasu N, Hirata Y (2001) Co-expression of urotensin II and its receptor (GPR14) in human cardiovascular and renal tissues. J Hypertens 19:2185–2190
Morimoto A, Hasegawa H, Cheng H -J, Cheng C -P (2002) Urotensin II inhibits left ventricular and myocytes contractile performance and [Ca2+]i transient: normal vs CHF. Circulation 106(Suppl. II):II–26
Opgaard OS, Nothacker HP, Ehlert FJ, Krause DN (2000) Human urotensin II mediates vasoconstriction via an increase in inositol phosphates. Eur J Pharmacol 406:265–271
Prendergast BD, Sagach VF, Shah AM (1997) Basal release of nitric oxide augments the Frank-Starling response in the isolated heart. Circulation 96:1320–1329
Russell FD (2004) Emerging roles of urotensin-II in cardiovascular disease. Pharmacol Ther 103:223–243
Russell FD, Molenaar P (2004) Investigation of signalling pathways that mediate the inotropic effect of urotensin-II in human heart. Cardiovasc Res 63:673–681
Russell FD, Molenaar P, O’Brien DM (2001) Cardiostimulant effects of urotensin-II in human heart in vitro. Br J Pharmacol 132:5–9
Russell FD, Meyers D, Galbraith AJ, Bett N, Toth I, Kearns P, Molenaar P (2003) Elevated plasma levels of human urotensin-II immunoreactivity in congestive heart failure. Am J Physiol Heart Circ Physiol 285:H1576–1581
Sauzeau V, Le Mellionnec E, Bertoglio J, Scalbert E, Pacaud P, Loirand G (2001) Human urotensin II-induced contraction and arterial smooth muscle cell proliferation are mediated by RhoA and Rho-kinase. Circ Res 88:1102–1104
Shah AM, Spurgeon HA, Sollott SJ, Talo A, Lakatta EG (1994) 8-Bromo-cGMP reduces the myofilament response to Ca2+ in intact cardiac myocytes. Circ Res 74:970–978
Soares JB, Rocha-Sousa A, Castro-Chaves P, Henriques-Coelho T, Leite-Moreira AF (2006) Inotropic and lusitropic effects of ghrelin and their modulation by the endocardial endothelium, NO, prostaglandins, GHS-R1a and KCa channels. Peptides 27:1616–1623
Stirrat A, Gallagher M, Douglas SA, Ohlstein EH, Berry C, Kirk A, Richardson M, MacLean MR (2001) Potent vasodilator responses to human urotensin-II in human pulmonary and abdominal resistance arteries. Am J Physiol Heart Circ Physiol 280:925–928
Tal M, Ammar DA, Karpuj M, Krizhanovsky V, Naim M, Thompson DA (1995) A novel putative neuropeptide receptor expressed in neural tissue, including sensory epithelia. Biochem Biophys Res Commun 209:752–759
Tasaki K, Hori M, Ozaki H, Karaki H, Wakabayashi I (2004) Mechanism of human urotensin II-induced contraction in rat aorta. J Pharmacol Sci 94:376–383
Tzanidis A, Hannan RD, Thomas WG, Onan D, Autelitano DJ, See F, Kelly DJ, Gilbert RE, Krum H (2003) Direct actions of urotensin II on the heart: implications for cardiac fibrosis and hypertrophy. Circ Res 93:246–253
van Heerebeek L, Borbely A, Niessen HW, Bronzwaer JG, van der Velden J, Stienen GJ, Linke WA, Laarman GJ, Paulus WJ (2006) Myocardial structure and function differ in systolic and diastolic heart failure. Circulation 113:1966–1973
Wang YX, Ding YJ, Zhu YZ, Shi Y, Yao T, Zhu YC W (2007) Role of PKC in the novel synergistic action of urotensin II and angiotensin II and in urotensin II-induced vasoconstriction. Am J Physiol Heart Circ Physiol 292:H348–H359
Watanabe T, Pakala R, Katagiri T, Benedict CR (2001) Synergistic effect of urotensin II with mildly oxidized LDL on DNA synthesis in vascular smooth muscle cells. Circulation 104:16–18
Watanabe T, Kanome T, Miyazaki A, Katagiri T (2006) Human urotensin II as a link between hypertension and coronary artery disease. Hypertens Res 29:375–387
Weber KT, Sun Y, Guarda E (1994) Structural remodeling in hypertensive heart disease and the role of hormones. Hypertension 23:869–877
Wheeler-Jones CP (2005) Cell signalling in the cardiovascular system: an overview. Heart 91:1366–1374
Yamamoto K, Masuyama T, Sakata Y, Nishikawa N, Mano T, Yoshida J, Miwa T, Sugawara M, Yamaguchi Y, Ookawara T, Suzuki K, Hori M (2002) Myocardial stiffness is determined by ventricular fibrosis, but not by compensatory or excessive hypertrophy in hypertensive heart. Cardiovasc Res 55:76–82
Yamasaki R, Wu Y, McNabb M, Greaser M, Labeit S, Granzier H (2002) Protein kinase A phosphorylates titin’s cardiac-specific N2B domain and reduces passive tension in rat cardiac myocytes. Circ Res 90:1181–1188
Acknowledgments
The authors thank Doctor Maria José Prata for her assistance in data analysis.
This paper is supported by the Portuguese Foundation for Science and Technology (grant number POCI/SAU-FCT/60803/2004, partially funded by FEDER) through the Cardiovascular R&D Unit (FCT number 51/94). Ana Patrícia Fontes-Sousa is supported by a grant from the Portuguese Foundation for Science and Technology (number SFRH/BD/22590/2005).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fontes-Sousa, A.P., Brás-Silva, C., Pires, A.L. et al. Urotensin II acutely increases myocardial length and distensibility: potential implications for diastolic function and ventricular remodeling. Naunyn-Schmied Arch Pharmacol 376, 107–115 (2007). https://doi.org/10.1007/s00210-007-0180-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-007-0180-8