Abstract
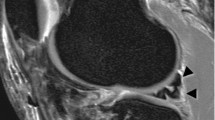
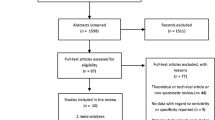
This clinical study evaluated factors affecting the decision for meniscal surgery in a patient population seen routinely at a trauma clinic. The study hypothesis was that patients who sustain a traumatic injury to the knee or have a long history of clinical symptoms are likelier to be operated on. We investigated 149 patients clinically and by magnetic resonance imaging (MRI). Group A (n = 62) underwent arthroscopic surgery and group B (n = 87) were treated conservatively. Multiple logistic regression analysis was used to examine correlations with regard to age, gender, injury pattern, period between the injury and first clinical examination, and MRI results. We found no significant difference between the two groups with regard to gender (P = 0.1), injury pattern (P = 0.44), or period between injury and first clinical examination (P = 0.5). Patients in group A were significantly older than those in group B (P = 0.044), and, as expected, MRI signal alterations were significantly higher in group A than in group B (P = 0.001). In acutely injured patients MRI helps to establish an accurate diagnosis, and in cases of positive MRI findings in a symptomatic patient, the surgeon should not wait 4–6 weeks but should immediately recommend surgery.
Article PDF
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Author information
Authors and Affiliations
Additional information
Received: 9 October 1998 Accepted: 10 May 1999
Rights and permissions
About this article
Cite this article
Muellner, T., Nikolic, A., Kubiena, H. et al. The role of magnetic resonance imaging in routine decision making for meniscal surgery. Knee Surgery 7, 278–283 (1999). https://doi.org/10.1007/s001670050164
Issue Date:
DOI: https://doi.org/10.1007/s001670050164