Abstract
Purpose
The purpose of this study was to determine the incidence of septic arthritis following arthroscopic posterior cruciate ligament (PCL) and multi-ligament reconstructions, and to evaluate a treatment regime with sequential arthroscopic irrigation and debridement procedures combined with antibiotic therapy that is focused on retention of the graft.
Methods
Between 2004 and 2016 a total of 866 PCL reconstructions and multi-ligament reconstructions were performed at our institution (408 isolated PCL reconstructions, 458 combined reconstructions). Medical charts of all cases were retrospectively reviewed with regard to the occurrence of septic complications. These cases were analysed with special focus on clinical management, number of reoperations and if the grafts were retained. Further, microbiological findings, postoperative clinical course and available clinical outcome data were evaluated.
Results
Four cases of septic arthritis (0.5%) were identified (follow-up rate 96.5%): two following isolated PCL reconstruction (0.5%), and two following multi-ligament reconstruction (0.4%), respectively. Septic arthritis was successfully treated in all cases with a mean of 2.5 ± 2.4 irrigation and debridement procedures (1–6). In one case of isolated PCL reconstruction, the graft was resected within the fifth irrigation and debridement due to septic loosing of the femoral fixation. All other grafts were retained. With regard to the outcome, all patients were subjectively satisfied with good stability (stress radiographs) in cases of retained grafts.
Conclusion
Postoperative septic arthritis after arthroscopic PCL and complex knee ligament reconstructions is a rare but serious complication. Arthroscopic graft-retaining treatment is recommended, as it is established in ACL surgery. Graft retention can be expected in the majority of the cases.
Level of evidence
Case series, Level 4.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Septic arthritis following arthroscopic knee surgery is a rare complication, but has potentially devastating consequences for the joint [7, 20]. Especially after ligament reconstruction, a standardized treatment algorithm is desirable, as the recently implanted graft is endangered. There are a number of studies on septic arthritis after anterior cruciate ligament (ACL) reconstruction; however, most of these studies report on only a few cases due to the low incidence of this complication. Incidence rates are reported between 0.14 and 2.6% [2, 8, 11, 13, 18,19,20, 27,28,29, 31, 33]. The largest study on this topic reported on 36 cases of septic arthritis in a population of more than 7000 ACL reconstructions, accordingly with an incidence rate of 0.5% [29].
Although some authors suggested early graft removal, within the last years, sequential arthroscopic irrigations and debridements combined with antibiotic therapy and focused on graft retention have become the standard treatment [2, 20, 29, 34]. Success rates of > 90% have been reported [20, 29, 34].
The number of detected injuries to the posterior cruciate ligament (PCL) is increasing, and consequently are surgical reconstructions of the posterior cruciate ligament. Often these injuries are accompanied by injuries to other structures of the knee, and combined reconstructions are common—especially PCL and posterolateral corner (PLC) reconstructions. Complication rates of these procedures in general are reported in up to 20.1% of PCL reconstructions, with surgical complications (e.g. infections) as common problems [26].
Some studies and case series on results of PCL reconstructions occasionally report on complications, but the case numbers are very low, and no systematic analysis is possible [12, 14, 35]. However, no studies systematically investigating infectious complications following PCL and multi-ligament reconstructions are available.
Therefore, the purpose of this study was first to determine the incidence of postoperative septic arthritis after PCL reconstruction and multi-ligament reconstructions in a large series from a high-volume specialized sports orthopedic centre, and second to analyse the clinical course and to evaluate a graft-retaining treatment protocol based on sequential arthroscopic irrigations and debridements plus antibiotic therapy. The hypothesis was that this is a rare complication, and that successful treatment (eradication of infection and graft retention) is possible. This is the first systematic investigation in this rare complication, and gives recommendations for standardized clinical management.
Materials and methods
Between 2004 and 2016, a total of 866 consecutive arthroscopic PCL reconstructions and multi-ligament reconstructions were performed at our institution. Medical charts of all cases were retrospectively reviewed with regard to age, sex, performed procedures (Table 1), and if postoperative septic arthritis occurred.
All patients undergoing knee ligament reconstruction at our institution were scheduled for follow-up examinations at 6 weeks, 6 months and 12 months. Postoperative septic arthritis can usually be expected within the first weeks from the index procedure [20, 29, 34]. Therefore, all cases with at least one documented follow-up examination > 3 months to the index procedure and in this regard normal findings were considered as not having suffered from postoperative septic arthritis. An infection was considered confirmed if bacterial growth was noted on cultures from joint aspiration or a biopsy specimen or if the clinical presentation together with intraoperative findings was obvious.
In cases of documented postoperative septic arthritis, medical records were retrospectively analysed with regard to surgical details of the index procedure, previous treatment, laboratory parameters [C-reactive protein (CRP)], time from index procedure to arthroscopic reoperation, number of arthroscopic reoperations, duration of in hospital treatment, duration of antibiotic administration, microbiological findings, if eradication was achieved and if the grafts were retained. Further, available data from all follow-up examinations in further course were analysed retrospectively, with special regard to documented range of motion, stability assessed with stress radiographs (Telos device) and if the patient was subjectively satisfied with the result.
Surgical technique of ligament reconstructions (index procedure)
All patients were treated with standardized surgical procedures, which have not substantially changed during the 13-year period of this study. In all cases surgery was performed with single-shot antibiotic prophylaxis (30–60 min prior to surgery) using cephalosporins (group I or II) or clindamycin (in cases of allergy or intolerance) and usually with an inflated pneumatic tourniquet (350 mmHg).
PCL reconstructions were performed arthroscopically in a transtibial technique. Concomitant ACL reconstructions were performed in anteromedial portal drilling technique for independent femoral tunnel placement. In all cases of cruciate ligament reconstruction fixation with interference screws (biodegradable or titanium) was used. In PCL reconstructions and in revision ACL reconstructions, a hybrid fixation was performed on the tibial side (interference screw plus non-absorbable suture). An intra-articular drain was placed in most cases at the end of surgery. Reconstruction of the PLC was carried out in a modified approach to Larson’s technique [25], reconstruction of the medial collateral ligament (MCL) and posteromedial structures was performed in an individual triangular technique within the first years of the study, and later in a modified approach to the technique of Lind et al. with a nearly anatomic reconstruction [16].
Autologous hamstring tendons were the first choice for cruciate ligament reconstructions, and semitendinosus tendon was preferred for collateral ligament reconstructions. Alternatively, the quadriceps tendon (ipsi- or contralateral; with or without patellar bone block) was used. In cases when more grafts were needed or autologous grafts were no more available, allografts or a combination of autografts and allografts were used.
Postoperative treatment protocol after index operation consisted of partial weight bearing (10–20 kg) for 3 weeks, and a fixed brace in full extension with posterior tibial support for 3 weeks followed by a brace with continued posterior tibial support but full range of motion for 9 weeks.
Treatment algorithm for postoperative infection
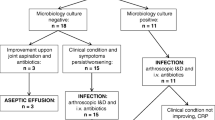
Figure 1 gives an overview over the following treatment algorithm: in cases of suspected septic arthritis, physical examination was performed with special regard to typical signs of infection, body temperature, and inspection of wound conditions. Blood tests were obtained with C-reactive protein (CRP) as the most sensitive and specific of the available parameters. Joint aspiration was not routinely performed, as in the majority of these cases indication for reoperation is clear. In unclear cases, a joint aspiration was performed, with an elevated synovial cell count being the decisive parameter [20]. After establishing the diagnosis, reoperation was performed on the day of admission. Our approach was completely arthroscopic. Two standardized anterior portals were used. The use of posterior portals is not necessary in our opinion but might be performed on individual decision. Five biopsies of the synovial membrane were taken for microbiological assessment and were cultured for 14 days. In the early years of this study only one biopsy or a swab was taken. An arthroscopic debridement of devitalized or necrotic tissue and a removal of fibrin layers and coagulated blood clots were carried out. An extensive irrigation with 10–15 l of saline fluid was performed. Synovectomy was not routinely performed, as this additional surgical trauma enhances the risk of arthrofibrosis [29]. Graft removal was only considered in loosened fixation or graft insufficiency. At the end of the procedure a drain was placed intra-articularly. Only in cases of macroscopically concomitant deep wound infections a local revision would have been performed.
An empiric antibiotic therapy was started after specimen collection. Antibiotic regimens changed over the years of the study. Within the last years, a combination of vancomycin plus ampicillin/sulbactam was administered, covering a wide spectrum of potential infection-causing bacteria. This was re-evaluated after receiving microbiological results and antibiogram. Postoperative care was based on daily physical examination and blood tests (CRP) every other day. Partial weight bearing was allowed, and after 3 weeks from the index procedure there was no limitation in range of motion. Additionally, pain-limited continuous passive motion was carefully applied to support regaining range of motion.
In cases of clinical deterioration, especially with recurrent effusion, increasing pain, increasing temperature or rise of CRP level another and sequential arthroscopic irrigations and debridements were performed. In cases of substantial and continuous improvement of clinical and lab parameters, antibiotics were switched to oral administration, depending on administered drugs and their oral bioavailability. Patients were discharged with oral antibiotics and follow-up examinations were carried out on a weekly basis. With CRP in normal range, antibiotic therapy was terminated. Patients were considered as successfully treated, when infection was eradicated and the graft was retained. Eradication was presumed when there was no recurrence of symptoms during further follow-up, and CRP remained normal. The study protocol of this retrospective case series was approved by the competent research ethics boards (Landesärztekammer Baden-Württemberg, F-2014-039).
Statistical analysis
Statistical analysis was performed using IBM SPSS Statistics for Windows (version 20, IBM Corp., Armonk, NY). The Chi-square test and Fisher’s exact test were used in evaluation of nominal data. All reported p values are two-tailed, with an alpha level < 0.05 considered as significant. Unless otherwise stated, descriptive results are presented as mean ± standard deviation (and range).
Results
From 866 reconstructions, four cases of postoperative septic arthritis were identified (0.5%). The follow-up rate of cases with follow-up data > 3 months to the index operation was 96.5% (836 of 866). There was no significant difference in the incidence of septic arthritis between isolated PCL reconstructions (0.5%) and multi-ligament reconstructions (0.4%, p = 0.908, n.s.).
On clinical presentation, all four patients had typical symptoms of joint infection with effusion and increasing pain. Three (75%) had elevated body temperature (> 38.0 °C). Mean C-reactive protein was 145 ± 72 mg/l (normal < 5 mg/l). None had immunosuppression or known chronic illness. All had unsuspicious wound conditions and no revisions of wounds were performed. The mean interval from index procedure to arthroscopic reoperation (which was carried out on the day of admission) was 18 ± 13 days (7–35). Eradication was achieved in all cases after a mean of 2.5 ± 2.4 arthroscopic irrigations and debridements (1–6). In two cases (50%) one and in one case (25%) two irrigation and debridement procedures were necessary, respectively. In all of these cases the grafts were retained. In one case with persistent signs of infection, a total of six reoperations were performed. At the time of the fifth reoperation a septic loosening of the femoral fixation with purulent fluid and cyst formation within the tunnel was seen. In this case, the graft was resected and fixation material was removed. Mean duration of inpatient treatment was 25 ± 24 days (6–59) and mean duration of antibiotic treatment was 50 ± 28 days (30–90).
In three cases (75%) infection-causing bacteria were identified: two coagulase-negative Staphylococci (Staphylococcus epidermidis and Staphylococcus hominins) and Enterococcus spp. were identified. In these three cases multiple biopsies were taken, whereas in the case without bacteria detection only a sample of synovial fluid was cultured.
All cases were seen multiple times in further follow-up from hospital discharge. Outcome data were available for all four cases in a short-term follow-up (1.4 ± 0.7 years, range 1.0–2.0). In one case (25%) arthroscopic arthrolysis was performed after 2.5 months (from the index procedure) due to a distinct flexion deficit, no other reoperations were carried out. All patients were subjectively satisfied with the result, and in cases with retention of the graft, acceptable stability results were obtained (Table 2).
Discussion
The major findings of this study are that septic arthritis is a rare complication in complex knee ligament reconstructions and can be successfully treated with arthroscopic irrigation and debridement. Graft retention is possible in the majority of the cases. Therefore, the hypotheses were confirmed.
No systematic clinical studies on infections following PCL and multi-ligament reconstructions are available in the literature. Yeranosian et al. reported on postoperative infections requiring reoperation based on patient records obtained from a large insurance company database [37]. A total of 1.217 cases of PCL repair or reconstruction were identified, with an incidence rate of 0.82% for postoperative infection. This is the largest cohort available in the literature; however, typical limitations of this type of study have to be considered. Further, the authors chose an interval of 30 days from the index procedure, which might underreport the actual incidence, e.g. one of our cases (25%) would have been missed.
Available data from clinical studies are very limited. Jung et al. reported on their prospective database of 234 PCL reconstructions over an 8-year period in a specialized sports orthopaedic centre, with two cases of postoperative infections (0.9%) that were treated by arthroscopic lavage [12]. Further, there are some more clinical studies focusing on clinical outcome following PCL and complex knee ligament reconstruction that occasionally mention septic complications [3, 9, 21]. Wang et al. reported on two cases of septic arthritis in a series of 55 PCL reconstructions (3.6%) [35]. One case with reoperation 1 week from the index procedure had an excellent result after arthroscopic debridement with graft retention. They also report on a rather uncommon case of late infection 20 months postoperatively where they resected the graft, and the patient had a poor result. However, in our experience, we have never seen a case of this kind of late infection. With regard to complex and multi-ligament reconstructions, only very small case series are available. Strobel et al. reported on 17 cases of PCL, ACL and PLC reconstruction and Denti et al. reported on 20 cases of combined PCL and ACL reconstructions, respectively [4, 30]. Fanelli and Edson reported on 41 cases of PCL reconstruction plus posterolateral procedures [6]. No infections occurred in these series, but the case numbers are simply too low for valid conclusions.
There are numerous studies focusing on postoperative infections following more commonly performed arthroscopic procedures, especially following ACL reconstructions. Incidence rates between 0.14 and 2.6% are reported [2, 8, 11, 13, 18,19,20, 27,28,29, 31, 33]. The largest series reported an incidence rate of 0.5%, with a significant higher rate in revision surgery [29]. Although the duration of an operative procedure is known as an independent risk factor for postoperative infection, the incidence found in this study seems within the same range as it is for ACL reconstructions [1]. Further, the number of necessary arthroscopic irrigation and debridement procedures seems to be within the same scale, and the spectrum of infection-causing bacteria (mainly Staphylococci) are comparable, respectively [29, 34]. It seems that reconstructive surgery per se, with the use of grafts and implants, seems to determine the rate of infections more than the duration of the procedure. Based on this assumption, prevention strategies focusing on graft contamination might be the logical consequence. Within recent years, the presoaking of tendon grafts in vancomycin has been reported to dramatically reduce the incidence of septic arthritis following ACL reconstruction [22, 24, 32]. Within this series, this technique was not yet used. Reported data are promising, but larger series are still necessary to confirm these findings.
Postoperative septic arthritis has potentially devastating consequences for the knee, and there is consensus on an urgent surgical treatment [7, 20, 29, 34]. There has been controversy over the last decades with regard to graft retention or graft resection. However, in recent years a graft-retaining treatment regimen has become prevalent, and large series have shown that graft retainment is possible in more than 90% of cases [34]. Especially in cases of complex reconstructions, the graft should be retained whenever possible, as functional insufficiency of one part of the complex reconstruction might lead to failure of the other reconstructions [15, 36]. Furthermore, after septic resection of the initial reconstruction the conditions for another complex revision reconstruction might be poor, as tunnels might be widened and autologous grafts might no longer be available.
Some authors recommend revision of all wounds in cases of septic complications following knee ligament reconstruction [23]. However, all four cases of septic arthritis in this study had unsuspicious wound conditions, and within our algorithm consequently no revision of the wounds were performed. With regard to the literature, this individual approach has been reported to be successful in the treatment of septic arthritis after ACL reconstructions [29]. Therefore, we recommend wound revision only if these appear macroscopically infected. Further, some authors suggest posterior portals for exploration and synovectomy of the posterior recessi [5]. However, irrigation and debridement of these is also possible with two anterior portals, and as synovectomy is not routinely performed in our regimen, these are not routinely necessary. There is no indication for arthrotomy as first-line therapy in these cases nowadays [29, 34]. It has been clearly shown that arthroscopic treatment was more successful, required fewer reoperations and had better long-term range of motion [10].
The short-term outcome was overall satisfying. No reinfection was noted. One patient (25%) underwent arthroscopic arthrolysis for a distinct limitation in range of motion, which is a common complication in infectious cases [17, 27]. Those with retained grafts had an acceptable posterior tibial displacement, which is comparable with the results of cases without infections [14]. However, outcome might be expected inferior compared to patients with uncomplicated postoperative course as it has been shown in studies on septic arthritis following ACL reconstructions with control groups [20, 27, 31].
There are several limitations of our study. First, this is a retrospective case series and it cannot be excluded that patients initially treated at our institution were treated for postoperative infection elsewhere. However, with a follow-up rate of 96.5% after > 3 months this bias is minimized.
Septic arthritis is a rare complication, and inherently the topic restricts high numbers. Therefore, the cohort is very heterogeneous. Consequently, general conclusions must be drawn cautiously, and serious statistical evaluation is quite limited. It is a series from a high-volume centre which assumingly reduces the rate of complications. Finally, this study is mainly focused on incidence and management and, therefore, cannot present systematic follow-up data (objectives scores), especially for mid- and long-term follow-up. It was attempted to contact the involved patients, but three were lost to follow-up, and no reasonable follow-up data are available, therefore.
The findings of this study might support surgeons in decision-making how to treat this rare but highly problematic complication, encourage them to try to retain the graft and consequently improve clinical outcome.
Conclusion
Postoperative septic arthritis after arthroscopic PCL and complex knee ligament reconstructions is a rare but serious complication. Arthroscopic graft-retaining treatment is recommended, as it is established in ACL surgery. Graft retention can be expected in the majority of the cases.
References
Armstrong RW, Bolding F, Joseph R (1992) Septic arthritis following arthroscopy: clinical syndromes and analysis of risk factors. Arthroscopy 8:213–223
Burks RT, Friederichs MG, Fink B, Luker MG, West HS, Greis PE (2003) Treatment of postoperative anterior cruciate ligament infections with graft removal and early reimplantation. Am J Sports Med 31:414–418
Chen CH, Chen WJ, Shih CH, Chou SW (2004) Arthroscopic posterior cruciate ligament reconstruction with quadriceps tendon autograft: minimal 3 years follow-up. Am J Sports Med 32:361–368
Denti M, Tornese D, Melegati G, Schonhuber H, Quaglia A, Volpi P (2015) Combined chronic anterior cruciate ligament and posterior cruciate ligament reconstruction: functional and clinical results. Knee Surg Sports Traumatol Arthrosc 23:2853–2858
Enderle E, Frosch KH (2013) Stadiengerechte Therapie des Kniegelenkinfekts nach Arthroskopie. Oper Orthop Traumatol 25:225–235
Fanelli GC, Edson CJ (2004) Combined posterior cruciate ligament-posterolateral reconstructions with Achilles tendon allograft and biceps femoris tendon tenodesis: 2- to 10-year follow-up. Arthroscopy 20:339–345
Frank M, Schmucker U, David S, Matthes G, Ekkernkamp A, Seifert J (2008) Devastating femoral osteomyelitis after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 16:71–74
Indelli PF, Dillingham M, Fanton G, Schurman DJ (2002) Septic arthritis in postoperative anterior cruciate ligament reconstruction. Clin Orthop Relat Res 182–188
Jakobsen BW, Lund B, Christiansen SE, Lind MC (2010) Anatomic reconstruction of the posterolateral corner of the knee: a case series with isolated reconstructions in 27 patients. Arthroscopy 26:918–925
Johns BP, Loewenthal MR, Dewar DC (2017) Open compared with arthroscopic treatment of acute septic arthritis of the native knee. J Bone Jt Surg Am 99:499–505
Judd D, Bottoni C, Kim D, Burke M, Hooker S (2006) Infections following arthroscopic anterior cruciate ligament reconstruction. Arthroscopy 22:375–384
Jung TM, Lubowicki A, Wienand A, Wagner M, Weiler A (2011) Knee stability after posterior cruciate ligament reconstruction in female versus male patients: a prospective matched-group analysis. Arthroscopy 27:399–403
Katz LM, Battaglia TC, Patino P, Reichmann W, Hunter DJ, Richmond JC (2008) A retrospective comparison of the incidence of bacterial infection following anterior cruciate ligament reconstruction with autograft versus allograft. Arthroscopy 24:1330–1335
Kim YM, Lee CA, Matava MJ (2011) Clinical results of arthroscopic single-bundle transtibial posterior cruciate ligament reconstruction: a systematic review. Am J Sports Med 39:425–434
LaPrade RF, Resig S, Wentorf F, Lewis JL (1999) The effects of grade III posterolateral knee complex injuries on anterior cruciate ligament graft force: a biomechanical analysis. Am J Sports Med 27:469–475
Lind M, Jakobsen BW, Lund B, Hansen MS, Abdallah O, Christiansen SE (2009) Anatomical reconstruction of the medial collateral ligament and posteromedial corner of the knee in patients with chronic medial collateral ligament instability. Am J Sports Med 37:1116–1122
Mayr HO, Stoehr A (2016) Komplikationen arthroskopischer Eingriffe am Kniegelenk. Der Orthopäde 45:4–12
McAllister DR, Parker RD, Cooper AE, Recht MP, Abate J (1999) Outcomes of postoperative septic arthritis after anterior cruciate ligament reconstruction. Am J Sports Med 27:562–570
Mei-Dan O, Mann G, Steinbacher G, Ballester SJ, Cugat RB, Alvarez PD (2008) Septic arthritis with Staphylococcus lugdunensis following arthroscopic ACL revision with BPTB allograft. Knee Surg Sports Traumatol Arthrosc 16:15–18
Mouzopoulos G, Fotopoulos VC, Tzurbakis M (2009) Septic knee arthritis following ACL reconstruction: a systematic review. Knee Surg Sports Traumatol Arthrosc 17:1033–1042
Osti M, Hierzer D, Seibert FJ, Benedetto KP (2017) The arthroscopic all-inside tibial-inlay reconstruction of the posterior cruciate ligament: medium-term functional results and complication rate. J Knee Surg 30:238–243
Perez-Prieto D, Torres-Claramunt R, Gelber PE, Shehata TM, Pelfort X, Monllau JC (2016) Autograft soaking in vancomycin reduces the risk of infection after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 24:2724–2728
Petersen W, Herbort M, Hoynck E, Zantop T, Mayr H (2014) Stage-adapted treatment of infection after reconstruction of the anterior cruciate ligament. Oper Orthop Traumatol 26:63–74
Phegan M, Grayson JE, Vertullo CJ (2016) No infections in 1300 anterior cruciate ligament reconstructions with vancomycin pre-soaking of hamstring grafts. Knee Surg Sports Traumatol Arthrosc 24:2729–2735
Richter J, Schulz-Jahrsdörfer M, Schuster P (2017) Posterolaterale Rekonstruktion in modifizierter Larson-Technik. Arthroskopie 30:49–54
Salzler MJ, Lin A, Miller CD, Herold S, Irrgang JJ, Harner CD (2014) Complications after arthroscopic knee surgery. Am J Sports Med 42:292–296
Schollin-Borg M, Michaelsson K, Rahme H (2003) Presentation, outcome, and cause of septic arthritis after anterior cruciate ligament reconstruction: a case control study. Arthroscopy 19:941–947
Schulz AP, Gotze S, Schmidt HG, Jurgens C, Faschingbauer M (2007) Septic arthritis of the knee after anterior cruciate ligament surgery: a stage-adapted treatment regimen. Am J Sports Med 35:1064–1069
Schuster P, Schulz M, Immendoerfer M, Mayer P, Schlumberger M, Richter J (2015) Septic arthritis after arthroscopic anterior cruciate ligament reconstruction: evaluation of an arthroscopic graft-retaining treatment protocol. Am J Sports Med 43:3005–3012
Strobel MJ, Schulz MS, Petersen WJ, Eichhorn HJ (2006) Combined anterior cruciate ligament, posterior cruciate ligament, and posterolateral corner reconstruction with autogenous hamstring grafts in chronic instabilities. Arthroscopy 22:182–192
Torres-Claramunt R, Pelfort X, Erquicia J, Gil-Gonzalez S, Gelber PE, Puig L et al (2013) Knee joint infection after ACL reconstruction: prevalence, management and functional outcomes. Knee Surg Sports Traumatol Arthrosc 21:2844–2849
Vertullo CJ, Quick M, Jones A, Grayson JE (2012) A surgical technique using presoaked vancomycin hamstring grafts to decrease the risk of infection after anterior cruciate ligament reconstruction. Arthroscopy 28:337–342
Wang C, Ao Y, Wang J, Hu Y, Cui G, Yu J (2009) Septic arthritis after arthroscopic anterior cruciate ligament reconstruction: a retrospective analysis of incidence, presentation, treatment, and cause. Arthroscopy 25:243–249
Wang C, Lee YH, Siebold R (2013) Recommendations for the management of septic arthritis after ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 22:2136–2144
Wang CJ, Chan YS, Weng LH, Yuan LJ, Chen HS (2004) Comparison of autogenous and allogenous posterior cruciate ligament reconstructions of the knee. Injury 35:1279–1285
Wentorf FA, LaPrade RF, Lewis JL, Resig S (2002) The influence of the integrity of posterolateral structures on tibiofemoral orientation when an anterior cruciate ligament graft is tensioned. Am J Sports Med 30:796–799
Yeranosian MG, Petrigliano FA, Terrell RD, Wang JC, McAllister DR (2013) Incidence of postoperative infections requiring reoperation after arthroscopic knee surgery. Arthroscopy 29:1355–1361
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the competent Ehtical committee.
Informed consent
No patients were contacted for this study.
Rights and permissions
About this article
Cite this article
Schuster, P., Geßlein, M., Mayer, P. et al. Septic arthritis after arthroscopic posterior cruciate ligament and multi-ligament reconstructions is rare and can be successfully treated with arthroscopic irrigation and debridement: analysis of 866 reconstructions. Knee Surg Sports Traumatol Arthrosc 26, 3029–3038 (2018). https://doi.org/10.1007/s00167-018-4902-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4902-x