Abstract
Purpose
The aim of this study was to report the complication rate after a medial patellofemoral ligament (MPFL) reconstruction using transverse patellar tunnels in a retrospective case series performed in a single institution.
Methods
Case series of 179 patients (192 knees) that had an MPFL reconstruction, with or without additional bony realignment procedures, between January 2009 and March 2015. Data were obtained from available patient charts.
Results
Thirty-nine complications (20.3 %) were registered. Twenty-seven of these (14.7 %) were minor. Seven patients (3.6 %) sustained a patellar fracture without adequate trauma. Male gender was a risk factor for patellar fracture (p < 0.001). Sixteen (8.1 %) reported recurrence of instability, of whom 10 (5.1 %) were defined as objective instability (reported dislocation and positive apprehension test).
Conclusion
This is largest patient series to date in which the complications after a two tunnel MPFL reconstruction are described. The use of transverse patellar tunnels increases the risk of sustaining a patellar fracture.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The medial patellofemoral ligament (MPFL) is a soft tissue restraint to lateral dislocation of the patella [1, 23]. It is nearly always disrupted after an initial dislocation [9, 22]. After sustaining a primary dislocation, the risk of recurrence is relatively high. Reported percentages differ greatly, but approximately half of all patients have recurrent dislocations [8, 17, 29]. In case of persistent instability, surgical management is the best option [29]. There are several anatomical factors associated with instability [30]. Surgery is aimed at addressing these abnormalities. Soft tissue repairs were introduced two decades ago. These soft tissue approaches seem to be safer than the osseous techniques, which were the keystone of patellar stabilization in the previous decades.
Since the introduction of MPFL reconstruction, numerous techniques have been described. All techniques employ fixation of a graft to the femur and the patella with sutures, bone tunnels or anchors. Overall results have been favourable so far in terms of functional outcome and recurrence of instability [19, 28, 31]. As with all new techniques, the early success of the procedure has outshone the potential risks of the procedure. Post-operative complications are rarely reported, and the use of different definitions of complications, heterogeneity in surgical techniques and small sample sizes make it practically impossible to give a realistic comparison between studies and techniques. The incidence of reported complication is highly variable and ranges from 3 to 85 % [7, 12, 25, 27], ranging from wound infections to patellar fractures. A large systematic review on complications of MPFL reconstructions by Shah et al. [27] reported a mean complication rate of 26 ± 21 % among included studies. Overall recurrence of dislocations and subluxations was 3.7 %; there was significant post-operative pain in 5.4 % and patellar fractures occurred in studies using tunnel fixation in 0.9 %. However, these numbers are mere averages and do not represent the complication rates of specific surgical techniques. Large studies reporting complication rates of specific surgical techniques are needed to give a clearer view on this. These studies can help determine what the safest technique is.
This retrospective study reports the complications and recurrence rates of patellofemoral instability in a large group of patients after an MPFL reconstruction using two transverse patellar tunnels performed in a single institution. The aim of this study was to give a clear view on the complication rates of this technique.
Materials and methods
Data collection
All patients who were operated between January 2009 and March 2015 for recurrent patellar dislocations using a double-bundle dynamic MPFL reconstruction were included. Patient charts were reviewed for data collection. If the procedure was not complicated, patients were asked to visit the outpatient clinic at 6 weeks and 6 months post-operatively.
Patients
One hundred and ninety-two knees in 171 patients with persistent patellar instability were included. Patellar instability was defined as a history of multiple patellar dislocations as reported by the patient and the presence of a hypermobile patella with a positive apprehension test on physical examination. The indications for MPFL surgery were recurrence (2 or more episodes) of patellar instability after failure of conservative management or a first-time patellar dislocation with a concurrent osteochondral fracture. All procedures were performed by one of the two authors (ST, SK) using a similar surgical technique. If needed, the MPFL reconstruction was combined with other procedures such as a tibial tubercle transfer or a trochlear osteotomy.
The median age at operation was 19 years (range 10–57 years), and 129 of the knees were female (67.2 %). Twenty patients had a history of previous unsuccessful surgery to stabilize the patella. Sixteen of these knees previously had a distal realignment procedure and four knees a soft tissue procedure, such as medial reefing or a lateral release. Preoperatively, patellar height, the degree of trochlear dysplasia, lateralization of the tibial tubercle and patellar tilt were assessed using lateral X-rays and CT or MRI scans. In case of the presence of a patella alta (Caton—Deschamps index >1.2) or a lateralized tubercle (TT-TG distance >15 mm), a tibial tubercle osteotomy (TTO) was performed concurrent with the MPFL reconstruction. In patients with severe trochlear dysplasia, the need for a trochleoplasty (TP) was assessed intraoperatively, based on the presence of a bump and the degree of instability. An overview of which specific procedures each patient had and their surgical history is listed in Table 1. One hundred and fifty-six out of the 197 knees (81.3 %) had at least one additional procedure to the MPFL reconstruction. In 134 knees (69.8 %), an additional TTO was performed; 2 knees (1.0 %) underwent an additional TP and in 21 knees (10.9 %), both procedures were performed. Nine patients had open epiphyseal plates and did not have any additional procedures, despite the presence of a patella alta or lateralized tibial tubercle in six of these patients. In one patient with a previous open lateral release, the lateral retinaculum was closed in addition to the MPFL reconstruction and TTO.
Surgical technique
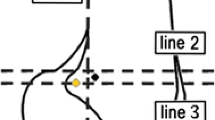
The MPFL was reconstructed using a hamstring autograft, preferably the gracilis. The graft was harvested from the ipsilateral knee using an incision over the tibial tubercle. For fixation to the patella and the femur, two small separate incisions were used, one at the medial border of the patella and one at the medial femoral epicondyle. First, the adductor tubercle was located on the femoral condyle. The graft was looped around the tendon, and the two free ends were passed under the superficial retinaculum. The graft was passed between layer 2 (medial retinaculum) and layer 3 (capsule) on the medial side of the knee. Using a 4.5-mm endobutton drill, two transverse tunnels were drilled from the medial border of the patella to the anterior patellar cortex. The free ends of the graft were passed through the tunnels and attached to the patella using absorbable sutures. The isometry of the graft was determined through a complete range of motion. After temporary fixation, a maximum of 5 mm of length change with flexion–extension of the knee was achieved (see Fig. 1). In patients with a lateralized tubercle or a patella alta, a TTO was performed prior to the MPFL reconstruction, using the same incision that was used for harvesting the graft. The osteotomy was fixed using two small fragment compression screws. The technique and results for this procedure have been described previously [15, 32]. In patients with severe trochlear dysplasia, where an MPFL reconstruction and TTO would be insufficient, a TP was performed. A midline incision was used at the patella instead of the medial incision. The lateral retinaculum was opened with a z-shaped incision, and the shape of the trochlea was assessed. In case of a trochlear bump without significant cartilage damage, the proximal cartilage was liberated from the subchondral bone and a bur was used to deepen the trochlea. The cartilage was reattached to the trochlea using absorbable sutures at the proximal edge. If the lateral side of the trochlea was insufficient, an anterior lateral open wedge osteotomy was performed. The opening was filled with a small bone block that was harvested from either the tibial tubercle or the iliac crest. This technique and its results have also been described previously [16]. All patients followed the same rehabilitation protocol: full weight bearing in a removable Velcro splint or plaster cast with a restricted knee flexion to 90 degrees for six weeks (Fig. 2).
Data analysis
Both objectives as subjective instability were included in the results, with objective instability defined as a reported episode of instability and the presence of a hypermobile patella and/or a positive apprehension test on physical examination. The complications were stratified into patients undergoing an isolated MPFL reconstruction and patients undergoing an MPFL reconstruction with additional procedures. All complications were categorized as either minor or major. Minor complications include events that are unlikely to have influenced the functional outcome or caused no permanent harm to the patient. Complications were classified as major if they affected outcome or required re-operation. Complications that were specific for the TTO (such as irritation of the screws used for fixation of the osteotomy) were not included in the results.
Statistical analysis
An independent sample t test was used to compare the average age of the group with and the group without complications. A Fisher’s exact test was used to detect significant differences in prevalence of complications between the following subgroups: male versus female, isolated MPFL versus combined procedures and skeletally mature versus skeletally immature patients. This test was repeated for every individual complication as well. For all datasets, differences with p values <0.05 were considered statistically significant.
Results
Patients were routinely followed up at 6 weeks and at 6 months post-operatively. Thirty-three patients did not come to the clinic at 6 months and had a shorter follow-up. One hundred and thirty-three patients had a follow-up of more than 6 months. Median follow-up was 9 months (range 1–67 months). Most common reasons for longer follow-up were: recurrent instability, post-operative complications, consultation for contralateral knee issues and request for TTO hardware removal. Out of the 192 operated knees, 39 knees had a registered complication (20.3 %) (Table 2). Of these complications, 12 were considered minor (6.3 %) and 27 major (14.1 %). Two patients had complications in both knees.
The patients in the complication group were younger on average than the patients without a complication (2.4 years, 95 % confidence interval (CI) −4.52 to −0.24, p = 0.029). There were no significant differences in age for the separate complications. There was no difference in recurrence of instability between male and female patients.
Major complications
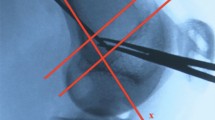
Twenty-six major complications were reported. Six patients sustained a patellar fracture, one of them in both knees. Figure 2 shows the x-ray and an image from the CT scan of one of the patients. All patients were male; mean age was 20 years (range 15–27). Mean time of occurrence after surgery was 5.8 months (SD 4.3). There was no significant difference in occurrence between the isolated and combined procedure group. Male patients had a significant higher risk of sustaining a patellar fracture (p < 0.001).
Ten patients (5.2 %) had objective recurrence of instability, of whom 6 in the isolated MPFL group (17.1 %). In patients with open epiphyseal plates, the recurrence was 33.3 % (3 out of 9), which was significantly higher than the recurrence in patients with skeletal maturity (33.3 vs. 3.8 %, p < 0.01). There was no significant difference in recurrence between the isolated MPFL and combined group.
Six patients (3.1 %) had subjective recurrence of instability. There was no difference in subjective recurrence between the isolated and combined group.
Other major complications were reported only once: a medial dislocation after failure of a repair of the lateral retinaculum concurrent with the MPFL reconstruction, a locally painful graft in both knees, laxity of the graft without instability and a post-operative flexion deficit of 60°.
Minor complications
There were 12 complications related to the surgical wound: 11 wound infections and 1 dehiscence. All these complications occurred in the group with combined procedures.
Discussion
The most important finding of the present study was the high prevalence of post-operative patellar fractures, which occurred in 3.6 % of patients, usually within 1 year after surgery. All fractures occurred in male patients (7.5 % of all male patients). The results in terms of stability were good, with a recurrence of objective instability in only 5.1 %. Recurrence rate in patients with open epiphyseal plates was high (3 out of 9, 33 %). Patients in the complication group were younger on average, but although this difference is statistically significant, it is small and probably not clinically relevant.
A patellar fracture is a major complication. This complication has been frequently reported [2–6, 10, 11, 13, 14, 18, 20, 21, 24, 25]. The available studies are too heterogeneous and small to determine a reliable prevalence of patellar fractures. An association with tunnels placed too anteriorly, and thus weakening the anterior cortex of the patella, has been mentioned [4, 11, 25]. The use of two transverse tunnels gives a higher risk, but fractures have also been reported in studies using only one tunnel or sockets [2, 5, 11, 18, 20]. A study on the complications of a similar technique to the one used in this study, employing two transverse patellar tunnels, in patients under 21 years (N = 179) reported 6 patellar fractures, only two of whom were male [25]. This contradicts this study’s finding of male gender being a risk factor for patellar fractures. Other studies were too small to determine the influence of gender. The time between the MPFL reconstruction and patellar fractures was similar in other studies, mostly occurring within 1 year [3, 5, 14, 18, 21, 24, 25].
Most MPFL techniques employ a static fixation with an interference screw at the femur; the technique in this study reports the results of the adductor sling technique. A cadaver study by Rood et al. [26] on patellofemoral pressures in different MPFL reconstructions shows that there is no increased contact pressure after the adductor sling technique, as was used in this study, while the pressure increases 3–5 times in the static technique from 60 to 110 degrees of flexion. This implies that the femoral fixation method used in this study has no negative influence on the risk of patellar fractures, i.e. by overloading the patellar attachment.
Recurrence of instability in this group was similar to other studies [19, 27]. It should be noted that the recurrence in this group cannot be solely attributed to the MPFL reconstruction, since more than 80 % of patients had a combined procedure, and it was impossible to determine the exact reason of failure retrospectively.
The major strength of this study is the large sample size. Patellofemoral instability is a relatively uncommon disorder, and most other single centre studies have a much smaller population than the one that was reported here, with an average sample size of about 30 [19, 27].
The main limitation of this study is its retrospective nature, using only available patient charts, and the spread in follow-up. Recurrent instability occurred on average after 17 months, so it is possible that the recurrence instability is underreported in this study. The majority of patients (81.3 %) required additional procedures to the MPFL reconstruction, and complication rates of an isolated MPFL reconstruction can be different.
It is possible that (minor) complications are underreported.
Conclusion
This is largest patient series to date in which the complications after a two tunnel MPFL reconstruction are described. The surgical technique that was used in this study gives an unacceptable high risk of patellar fractures due to the use of transverse patellar tunnels. Alternative patellar fixation methods should be considered. More comparative research is needed to determine which fixation method gives the best functional results and the lowest complication rates.
References
Amis AA, Firer P, Mountney J, Senavongse W, Thomas NP (2003) Anatomy and biomechanics of the medial patellofemoral ligament. Knee 10(3):215–220
Astur DC, Gouveia GB, Borges JH, Astur N, Arliani GG, Kaleka CC, Cohen M (2015) Medial patellofemoral ligament reconstruction: a longitudinal study comparison of 2 techniques with 2 and 5-years follow-up. Open Orthop J 9:198–203
Calvo Rodriguez R, Figueroa Poblete D, Anastasiadis Le Roy Z, Etchegaray Bascur F, Vaisman Burucker A, Calvo Mena R (2015) Reconstruction of the medial patellofemoral ligament: evaluation of the clinical results of autografts versus allografts. Rev Esp Cir Ortop Traumatol 59(5):348–353
Christiansen SE, Jacobsen BW, Lund B, Lind M (2008) Reconstruction of the medial patellofemoral ligament with gracilis tendon autograft in transverse patellar drill holes. Arthroscopy 24(1):82–87
Dhinsa BS, Bhamra JS, James C, Dunnet W, Zahn H (2013) Patella fracture after medial patellofemoral ligament reconstruction using suture anchors. Knee 20(6):605–608
Ellera Gomes JL (1992) Medial patellofemoral ligament reconstruction for recurrent dislocation of the patella: a preliminary report. Arthroscopy 8(3):335–340
Enderlein D, Nielsen T, Christiansen SE, Fauno P, Lind M (2014) Clinical outcome after reconstruction of the medial patellofemoral ligament in patients with recurrent patella instability. Knee Surg Sports Traumatol Arthrosc 22(10):2458–2464
Fithian DC, Paxton EW, Stone ML, Silva P, Davis DK, Elias DA, White LM (2004) Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 32(5):1114–1121
Guerrero P, Li X, Patel K, Brown M, Busconi B (2009) Medial patellofemoral ligament injury patterns and associated pathology in lateral patella dislocation: an MRI study. Sports Med Arthrosc Rehabil Ther Technol 1(1):17
Hinterwimmer S, Imhoff AB, Minzlaff P, Saier T, Rosenstiel N, Hawe W, Feucht MJ (2013) Anatomical two-bundle medial patellofemoral ligament reconstruction with hardware-free patellar graft fixation: technical note and preliminary results. Knee Surg Sports Traumatol Arthrosc 21(9):2147–2154
Hopper GP, Leach WJ, Rooney BP, Walker CR, Blyth MJ (2014) Does degree of trochlear dysplasia and position of femoral tunnel influence outcome after medial patellofemoral ligament reconstruction? Am J Sports Med 42(3):716–722
Howells NR, Barnett AJ, Ahearn N, Ansari A, Eldridge JD (2012) Medial patellofemoral ligament reconstruction: a prospective outcome assessment of a large single centre series. J Bone Joint Surg Br 94(9):1202–1208
Howells NR, Eldridge JD (2012) Medial patellofemoral ligament reconstruction for patellar instability in patients with hypermobility: a case control study. J Bone Joint Surg Br 94(12):1655–1659
Kita K, Horibe S, Toritsuka Y, Nakamura N, Tanaka Y, Yonetani Y, Mae T, Nakata K, Yoshikawa H, Shino K (2012) Effects of medial patellofemoral ligament reconstruction on patellar tracking. Knee Surg Sports Traumatol Arthrosc 20(5):829–837
Koeter S, Diks MJ, Anderson PG, Wymenga AB (2007) A modified tibial tubercle osteotomy for patellar maltracking: results at two years. J Bone Joint Surg Br 89(2):180–185
Koeter S, Pakvis D, van Loon CJ, van Kampen A (2007) Trochlear osteotomy for patellar instability: satisfactory minimum 2-year results in patients with dysplasia of the trochlea. Knee Surg Sports Traumatol Arthrosc 15(3):228–232
Lewallen L, McIntosh A, Dahm D (2015) First-time patellofemoral dislocation: risk factors for recurrent instability. J Knee Surg 28(4):303–309
Lippacher S, Reichel H, Nelitz M (2010) Patellar fracture after patellar stabilization. Orthopade 39(5):516–518
Mackay ND, Smith NA, Parsons N, Spalding T, Thompson P, Sprowson AP (2014) Medial patellofemoral ligament reconstruction for patellar dislocation: a systematic review. Orthop J Sports Med 2(8):2325967114544021
Mikashima Y, Kimura M, Kobayashi Y, Miyawaki M, Tomatsu T (2006) Clinical results of isolated reconstruction of the medial patellofemoral ligament for recurrent dislocation and subluxation of the patella. Acta Orthop Belg 72(1):65–71
Mulliez A, Lambrecht D, Verbruggen D, Van Der Straeten C, Verdonk P, Victor J (2015) Clinical outcome in MPFL reconstruction with and without tuberositas transposition. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-015-3654-0
Nomura E, Horiuchi Y, Inoue M (2002) Correlation of MR imaging findings and open exploration of medial patellofemoral ligament injuries in acute patellar dislocations. Knee 9(2):139–143
Nomura E, Horiuchi Y, Kihara M (2000) Medial patellofemoral ligament restraint in lateral patellar translation and reconstruction. Knee 7(2):121–127
Panni AS, Alam M, Cerciello S, Vasso M, Maffulli N (2011) Medial patellofemoral ligament reconstruction with a divergent patellar transverse 2-tunnel technique. Am J Sports Med 39(12):2647–2655
Parikh SN, Nathan ST, Wall EJ, Eismann EA (2013) Complications of medial patellofemoral ligament reconstruction in young patients. Am J Sports Med 41(5):1030–1038
Rood A, Hannink G, Lenting A, Groenen K, Koeter S, Verdonschot N, van Kampen A (2015) Patellofemoral pressure changes after static and dynamic medial patellofemoral ligament reconstructions. Am J Sports Med 43(10):2538–2544
Shah JN, Howard JS, Flanigan DC, Brophy RH, Carey JL, Lattermann C (2012) A systematic review of complications and failures associated with medial patellofemoral ligament reconstruction for recurrent patellar dislocation. Am J Sports Med 40(8):1916–1923
Singhal R, Rogers S, Charalambous CP (2013) Double-bundle medial patellofemoral ligament reconstruction with hamstring tendon autograft and mediolateral patellar tunnel fixation: a meta-analysis of outcomes and complications. Bone Joint J 95-b(7):900–905
Smith TO, Song F, Donell ST, Hing CB (2011) Operative versus non-operative management of patellar dislocation. A meta-analysis. Knee Surg Sports Traumatol Arthrosc 19(6):988–998
Steensen RN, Bentley JC, Trinh TQ, Backes JR, Wiltfong RE (2015) The prevalence and combined prevalences of anatomic factors associated with recurrent patellar dislocation: a magnetic resonance imaging study. Am J Sports Med 43(4):921–927
Stupay KL, Swart E, Shubin Stein BE (2015) Widespread implementation of medial patellofemoral ligament reconstruction for recurrent patellar instability maintains functional outcomes at midterm to long-term follow-up while decreasing complication rates: a systematic review. Arthroscopy 31(7):1372–1380
Tigchelaar S, van Essen P, Benard M, Koeter S, Wymenga A (2015) A self-centring osteotomy of the tibial tubercle for patellar maltracking or instability: results with ten-years’ follow-up. Bone Joint J 97-b(3):329–336
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schiphouwer, L., Rood, A., Tigchelaar, S. et al. Complications of medial patellofemoral ligament reconstruction using two transverse patellar tunnels. Knee Surg Sports Traumatol Arthrosc 25, 245–250 (2017). https://doi.org/10.1007/s00167-016-4245-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4245-4