Abstract
Purpose
The aim of the present study was to evaluate the clinical and radiological results of lesser tuberosity transfer in acute locked posterior shoulder dislocation with a humeral head defect between 25 and 45 %.
Methods
Clinical and radiological results of seven patients with locked posterior shoulder dislocation with a humeral head defect between 25 and 45 % which were managed with a modification of the McLaughlin procedure within 14 days after injury were evaluated retrospectively after a mean follow-up of 41 months.
Results
All shoulders remained stable. The results were good in one and excellent in six patients with a median absolute Constant score of 92 (range 80–98). Mean active pain-free abduction was 171.4° (SD 6.4), mean flexion was 175.7° (SD 4.9), and mean external rotation was 54.3° (SD 17.6). Internal rotation was restricted in all patients. There were no radiological signs of osteoarthritis.
Conclusions
Lesser tuberosity transfer shows excellent clinical and radiographic mid-term results in acute cases of locked posterior shoulder dislocation with a reverse Hill-Sachs lesion between 25 and 45 %.
Level of evidence
Case series with no comparison group, Level IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Posterior dislocation of the shoulder is a rare injury that can be missed initially when typical clinical and radiological indications remain unrecognized. Treatment depends aside from the age of the dislocation mainly on the size of the reverse Hill-Sachs lesion. While lesions with a defect of the humeral head of <20–25 % can be treated conservatively after reduction, arthroplasty is the procedure of choice for defects >40–50 % [12]. Different options are described for defects between 25 and 45 % depending on the age of the injury. McLaughlin in 1952 [16] proposed the transfer of the subscapularis tendon into the defect for chronic dislocations. Later, the procedure was modified by Hawkins et al. [12] with transfer of the lesser tuberosity in four chronic cases. Alternatively, a rotational osteotomy of the humerus [14, 19] or allograft reconstruction of the defect [8, 11] is successfully performed in chronic dislocations.
Good results for conservative treatment after closed reduction in acute posterior dislocations with a Hill-Sachs lesion of up to 32 % were reported [9]. However, the patients in that study were older and/or had relevant comorbidities. Thus, surgical treatment is preferred for patients with defects between 25 and 45 % [3, 12]. Anatomical procedures reconstructing the humeral head [1, 15] compete with non-anatomical lesser tuberosity transfer [10]. However, the literature concerning treatment of the acute dislocation is limited due to the fact that the injury is rare and often remains unnoticed initially.
The purpose of the present study was to evaluate clinical and radiographic results of lesser tuberosity transfer at mid-term follow-up in locked posterior shoulder dislocation with a reversed Hill-Sachs lesion between 25 and 45 % treated surgically acute, that means within 3 weeks after dislocation. The hypothesis was that it has satisfactory clinical and radiological results.
Materials and methods
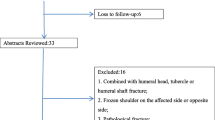
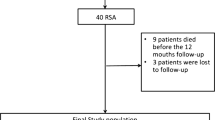
Between 2005 and 2009, thirteen patients (twelve men and one woman) with fourteen locked posterior shoulder dislocations were treated at our institution. Patients with additional proximal humeral fractures other than greater or lesser tuberosity fracture were excluded. Of these, seven male patients with a median age of 39 years (range 22–60 years) fulfilled inclusion criteria for our study (locked posterior shoulder dislocation with a reverse Hill-Sachs lesion between 25 and 45 % treated by a lesser tuberosity transfer within 3 weeks after injury). Their mean reverse Hill-Sachs lesion was 32 % (SD 6.4). Diagnosis was made after a median of 0 days (range 0–5). Surgery was performed within 14 days after injury in these patients. The dominant arm was involved in five patients. Dislocation was caused by epileptic seizure in one patient. The other dislocations were caused by trauma (skiing accident, bike and motorcycle accident, fall from stairs and fall after drug abuse). Six patients initially presented in other hospitals and were referred to our institution for further treatment; two of these had persistent locked dislocation.
One patient was admitted to our department as a multiple injured patient after a motorcycle accident. After initial reduction, lesser tuberosity transfer was done 3 days later after stabilization due to associated injuries (severe lung contusion and rupture of the posterior cruciate ligament). The other six patients had isolated posterior shoulder dislocations with no concomitant injuries.
Patients gave their written consent and permission to participate in the study, and institutional approval for the study was granted by the Medical Review Board of our institute (trial number 27/2011).
Clinical presentation and radiographic evaluation
Clinically, the three patients with dislocated shoulder at first presentation in our department showed a painfully limited range of motion, especially a limited external rotation of the shoulder. All patients had radiographs (true anteroposterior and if applicable lateral scapular view) and a computed tomography scan of the shoulder. The size of the reverse Hill-Sachs lesion was determined in the CT as proposed by Cicak as the percentage of involved humeral head [3]. The slice showing the greatest head loss was used.
Surgical technique
Stability testing under anaesthesia showed redislocation during internal rotation in all patients because the reverse Hill-Sachs lesion engaged into the posterior glenoid rim. A deltopectoral approach was used. After incision of the rotator interval, the size of the defect was determined and the indication to a lesser tuberosity transfer was confirmed. In the two patients with persistent dislocation, open reduction was performed after incision of the rotator interval with the surgeons forearm placed in the axilla and adduction of the arm with combined traction and internal rotation supported by an anteriorly directed pressure on the posterior humeral head.
The lesser tuberosity was detached with a chisel and transferred into the defect. The joint was evaluated for concomitant lesions; however, no additional lesions to the rotator cuff or cartilage were detected. The amount of lesser tuberosity along with the subscapularis tendon which was transferred varied with the size of the defect and involved either the upper two-thirds or the complete lesser tuberosity. It was fixed with one or two bicortical partially threaded cannulated self-tapering screws (3.5 mm, DePuy, Warsaw, Indiana) depending on the size of the fragment. In two patients, washers were used. One patient had an additional screw fixation of a concomitant greater tuberosity fracture. Surgery was performed by five different surgeons.
Postoperative management
The shoulders were immobilized in a splint in neutral rotation for 6 weeks. Passive range of motion exercises up to 90° of abduction and forward flexion were started after surgery with full range of motion allowed after 6 weeks.
Outcome evaluation
Patients were examined clinically, and radiographs of the shoulder were taken at a median follow-up period of 41 months (range 27–54 months). Range of motion, strength and stability were tested. The Constant–Murley shoulder score [6] and the American Shoulder and Elbow Surgeons questionnaire [20] were evaluated. Strength was tested with a calibrated digital spring balance fixed on the ground. A strap was fixed on the wrist with the forearm in pronation and the shoulder in 90° of abduction in the scapular plane. The maximum value of three repetitions was used for the Constant score. Furthermore, AP radiographs and axillary views were obtained. In one patient with a Hill-Sachs lesion of 45 %, a postoperative CT scan was available (see Fig. 1).
Results
All patients regained a stable shoulder with no redislocation or subluxation. They were all able to return to their former job without any restrictions. With respect to the age- and gender-adjusted relative Constant score, the results were excellent in six patients and good in one patient [6, 13, 24]. Five patients were free of pain, and no patient complained pain at night. No patient had to take pain medication due to shoulder pain. The median pain subscore was 15. Most patients had a decreased strength of the operated shoulder (median 21). The median absolute Constant score was 92, the median relative Constant score was 100, and the median American Shoulder and Elbow Surgeon was 98.
The mean active elevation was 175.7° (SD 4.9), contralateral side mean 175.7° (SD 4.9), the mean abduction was 171.4° (SD 6.4), contralateral side mean 175.7° (SD 4.9), the mean external rotation at side was 54.3° (SD 17.6), contralateral side mean 68.6° (SD 11.4), and the mean external rotation in 90° abduction was 83.6° (SD 8.7), contralateral side mean 86.4° (SD 4.4). All patients showed a decreased internal rotation between the waist and the 12th thoracic vertebra. In contrast, all patients reached the interscapular level on the contralateral side.
The size of reverse Hill-Sachs lesion was measured on the preoperative axial CT cuts as described by Cicak [3] and ranged between 25 and 45 %. At the time of latest follow-up, there were no signs of osteoarthritis according to Samilson and Prieto [22]. Osseous integration of the lesser tuberosity into the defect was seen on axial radiographs (see Figs. 2, 3) in all cases. One patient who was very satisfied with his result complained of mild pain in the operated shoulder. A radiograph had revealed migration of the screw. His active abduction was 170°, the flexion 180° and external rotation 70°. His internal rotation was restricted to the waist. It is unknown whether the migrated screw was responsible for his pain, nevertheless screw removal was advised.
Discussion
The most important finding of the present study was that despite being a non-anatomical procedure, the modified Mc Laughlin procedure showed an excellent clinical outcome at mid-term for acute locked posterior shoulder dislocation with a humeral head defect of between 25 and 45 %. Despite the potentially modified joint kinematics, there were no signs of osteoarthritis. This may be due to the short follow-up period. On the other hand, in contrast to anatomical procedures, the complete articulating humeral head cartilage remains intact after lesser tuberosity transfer.
While there are many studies reporting on surgical treatment of chronic dislocations [7, 8, 11, 14, 19, 21], only few reported on treatment of acute posterior shoulder dislocations [2, 5, 10]. Dislocation has been considered acute when the duration is <3 weeks [3, 21]. For humeral head defects between 20 and 45 % in acute dislocations, conservative treatment and non-anatomical or anatomical surgical procedures have been described.
Duralde and Fogle [9] reported an excellent clinical outcome with only one recurrent dislocation in seven patients with locked posterior shoulder dislocations with humeral head defects of between 18 and 32 % which were managed with closed reduction under general anaesthesia within 2 weeks. However, three of the seven patients were between 69 and 73 years old, and all seven had relevant comorbidities. A complete filling of the humeral head defect was reported in only 1 patient, and there is no information regarding the development of signs of osteoarthritis. In contrast, our patients with head defects of <32 % were young or middle-aged and healthy. Thus, we decided for operative treatment in these cases.
The McLaughlin procedure as well as the modified McLaughlin procedure was first described for the treatment of chronic missed posterior dislocations [12, 16]. Only few studies reported on lesser tuberosity transfer for acute locked posterior shoulder dislocation [4, 10].
Finkelstein et al. [10] reported about seven patients with a bony defect between 25 and 40 % managed with a modification of the McLaughlin procedure within 10 days post-injury. After a mean follow-up of 5 years, there was no recurrent dislocation. Neither radiological nor clinical results like range of motion, pain or Constant and ASES score were reported.
Checchia et al. [4] evaluated their subgroup of patients with acute (<4 weeks) management of locked posterior shoulder dislocation treated with lesser tuberosity transfer. After a mean of 35.6 month, those five out of eight patients that were available for follow-up had excellent or good results with an average elevation of 145°, an external rotation of 66° and an internal rotation up to the tenth thoracic vertebra. The elevation is less than in our study; however, the elevation of the uninvolved contralateral side was only 150°. So these patients also regained near normal elevation when compared to the contralateral side.
A painless free active range of motion with no restrictions of activity but mild pain after physical strain was reported in a patient with bilateral locked posterior shoulder dislocation managed with early bilateral lesser tuberosity transfer [18].
In another two studies, a subgroup of patients had a modified McLaughlin procedure [12, 23]. However, the authors did not report whether acute or chronic dislocations were treated.
One potential disadvantage of lesser tuberosity transfer is the alteration of the anatomy of the humeral head. Thus, different techniques reconstructing the anatomy have been described for acute dislocations in case reports or studies with small sample sizes [1, 2, 5, 15, 17].
In the largest series of Bock et al. [2] including five patients with acute management of a reverse Hill-Sachs lesion by elevation of the cartilage and filling of the bone defect with either spongiotic allograft, autograft or both, there was no recurrence at a mean follow-up of 62.7 month. The mean Constant score was 87.8, the average anteversion 158.3° and the abduction 146.7°. Internal rotation ranged from lumbar spine segment III to thoracal VII. An excellent functional outcome with no restrictions in internal rotation after raising the depressed chondral surface was reported by Assom et al. [1]; however, neither abduction nor elevation was reported.
Excellent results after autologous bone grafting either from the iliac crest or from the contralateral side after bilateral dislocation were reported in two case reports [5, 15].
These results of anatomical procedures are comparable to the results of the present study. The modified McLaughlin procedure was reliable in preventing redislocation. Except for strength and internal rotation, normal shoulder function was restored. So we regard our hypothesis is confirmed. Moreover, there is no donor site morbidity for bone grafting.
One problem of our as well as other studies is the accuracy of measurement of the Hill-Sachs lesion as this is not standardized. We feel that the method by Cicak is well practicable in daily clinical setting and that it is able to detect lesions of between 20–25 % and 45–50 %. In future, efforts should be made to improve measurement accuracy.
To our knowledge, this is the first study reporting on the modified McLaughlin’s procedure for acute locked posterior shoulder dislocation including assessment of range of motion, two commonly used shoulder scores and a radiographic evaluation.
The present study has some limitations. First, it is a retrospective study. Secondly due to the fact that it is a rare injury, the number of patients included is small. However, this is in line with the other studies. Furthermore, the follow-up period is short. Thus, the results should be interpreted carefully.
Conclusion
With respect to functional outcome, modified McLaughlin procedure is a reliable option for the treatment of acute locked posterior shoulder dislocation with a head defect of 25–45 %.
References
Assom M, Castoldi F, Rossi R, Blonna D, Rossi P (2006) Humeral head impression fracture in acute posterior shoulder dislocation: new surgical technique. Knee Surg Sports Traumatol Arthrosc 14:668–672
Bock P, Kluger R, Hintermann B (2007) Anatomical reconstruction for reverse Hill-Sachs lesions after posterior locked dislocation fracture: a case series of six patients. Arch Orthop Trauma Surg 127:543–548
Cicak N (2004) Posterior dislocation of the shoulder. J Bone Joint Surg-Br 86:324–332
Checchia SL, Santos PD, Miyazaki AN (1998) Surgical treatment of acute and chronic posterior fracture-dislocation of the shoulder. J Shoulder Elbow Surg 7:53–65
Connor PM, Boatright JR, D’Alessandro DF (1997) Posterior fracture-dislocation of the shoulder: treatment with acute osteochondral grafting. J Shoulder Elbow Surg 6:480–485
Constant CR, Gerber C, Emery RJ, Sojbjerg JO, Gohlke F, Boileau P (2008) A review of the constant score: modifications and guidelines for its use. J Shoulder Elbow Surg 17:355–361
Delcogliano A, Caporaso A, Chiossi S, Menghi A, Cillo M, Delcogliano M (2005) Surgical management of chronic, unreduced posterior dislocation of the shoulder. Knee Surg Sports Traumatol Arthrosc 13:151–155
Diklic ID, Ganic ZD, Blagojevic ZD, Nho SJ, Romeo AA (2010) Treatment of locked chronic posterior dislocation of the shoulder by reconstruction of the defect in the humeral head with an allograft. J Bone Joint Surg-Br 92:71–76
Duralde XA, Fogle E (2006) The success of closed reduction in acute locked posterior fracture-dislocations of the shoulder. J Shoulder Elbow Surg 15:701–706
Finkelstein JA, Waddell JP, O’Driscoll SW, Vincent G (1995) Acute posterior fracture dislocations of the shoulder treated with the Neer modification of the McLaughlin procedure. J Orthop Trauma 9:190–193
Gerber C, Lambert SM (1996) Allograft reconstruction of segmental defects of the humeral head for the treatment of chronic locked posterior dislocation of the shoulder. J Bone Joint Surg-A 78:376–382
Hawkins RJ, Neer CS, Pianta RM, Mendoza FX (1987) Locked posterior dislocation of the shoulder. J Bone Joint Surg-A 69:9–18
Ianotti JP, Bernot MP, Kuhlmann JR, Kelley MJ, Williams GR (1996) Postoperative assessment of shoulder function: a prospective study of full-thickness rotator cuff tears. J Shoulder Elbow Surg 5:449–457
Keppler P, Holz U, Thielemann FW, Meinig R (1994) Locked posterior dislocation of the shoulder: treatment using rotational osteotomy of the humerus. J Orthop Trauma 8:286–292
Khayal T, Wild M, Windolf J (2009) Reconstruction of the articular surface of the humeral head after locked posterior shoulder dislocation: a case report. Arch Orthop Trauma Surg 129:515–519
McLaughlin HL (1952) Posterior dislocation of the shoulder. J Bone Joint Surg-A 34:584–590
Modi CS, Wicks L, Srinivasan K (2009) Reconstruction of humeral head defect for locked posterior shoulder dislocation. Orthopedics 32:111–114
Nicola FG, Ellman H, Eckardt J, Finerman G (1981) Bilateral posterior fracture-dislocation of the shoulder treated with a modification of the McLaughlin procedure. A case report. J Bone Joint Surg-A 63:1175–1177
Porteous MJ, Miller AJ (1990) Humeral rotation osteotomy for chronic posterior dislocation of the shoulder. J Bone Joint Surg-Br 72:468–469
Richards RR, An KN, Bigliani LU, Friedman RJ, Gartsman GM, Gristina AG et al (1994) A standardized method for the assessment of shoulder function. J Shoulder Elbow Surg 3:347–352
Rowe C, Zarins B (1982) Chronic unreduced dislocation of the shoulder. J Bone Joint Surg-A 64:494–505
Samilson RL, Prieto V (1983) Dislocation arthropathy of the shoulder. J Bone Joint Surg-A 65:456–460
Schliemann B, Muder D, Geßmann J, Schildhauer TA, Seybold D (2011) Locked posterior shoulder dislocation: treatment options and clinical outcomes. Arch Orthop Trauma Surg 131:1127–1134
Yian EH, Ramappa AJ, Arneberg O, Gerber C (2005) The constant score in normal shoulders. J Shoulder Elbow Surg 14:128–133
Conflict of interest
No author declares conflict of interest regarding this publication.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Banerjee, M., Balke, M., Bouillon, B. et al. Excellent results of lesser tuberosity transfer in acute locked posterior shoulder dislocation. Knee Surg Sports Traumatol Arthrosc 21, 2884–2888 (2013). https://doi.org/10.1007/s00167-012-2217-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-012-2217-x