Abstract
The purpose of this study was to evaluate the clinical results of arthroscopic single bundle posterior cruciate ligament (PCL) reconstruction in patients with chronic PCL instability not responding to conservative treatment. 18 patients were available for follow-up with an average elapsed time of 3 years between onset of injury and surgery and an average duration of 3.3 years between reconstruction and evaluation. The clinical results were investigated using the IKDC form, the Tegner rating system, a subjective evaluation, and the VAS for pain rating. The presence of femoral degenerative changes correlated strongly to the elapsed time between injury and operation (P<0.05). Before surgery all patients were graded D (severely abnormal) using the IKDC evaluation form. The final IKDC score at follow-up resulted in grade A (normal) in five patients (28%), grade B (nearly normal) in eight patients (44%), grade C (abnormal) in four patients (22%) and grade D (severely abnormal) in one patient (6%). The VAS score for pain rating revealed very few complaints of pain and it demonstrated a strong correlation between the subjective evaluation and the Tegner rating score (P<0.01). Evaluation of the Tegner score resulted in a significant improvement after surgery when compared to the situation prior to operation (P<0.01). Although there still is some controversy on the indication for treatment of PCL injury, we conclude on the basis of our findings that arthroscopic reconstruction of symptomatic chronic PCL instability, not responding to conservative therapy, can be greatly beneficial.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Data reported in the literature concerning the incidence of injury to the posterior cruciate ligament (PCL) vary between 3% and 37% of all knee injuries [1–3]. In comparison to injuries of the anterior cruciate ligament (ACL), PCL injury occurs not as often and is more inclined to occur in a population of younger, active patients. There still is some controversy on the indication for treatment of PCL instability. Although conservative therapy may result in reasonable functional outcome [4–7], results tend to deteriorate with time due to the development of pain, degenerative changes, and progressive instability influencing daily life activities [1, 6, 8–10]. Many authors recommend operative reconstruction in symptomatic chronic PCL lesions not responding on conservative therapy [1, 9, 11], but results on the longer term are few. The purpose of this study was to evaluate the clinical outcome following arthroscopic reconstruction of the PCL for chronic symptomatic instability on the mid-term.
Materials and methods
Subjects
Of the 24 patients who received arthroscopic single bundle reconstruction of the PCL between 1995 and 2000, 18 patients were available for follow-up. Six patients were lost to follow-up due to migration or unwillingness to further participate in the study. All patients had chronic instability of the PCL not responding well to conservative therapy. The diagnosis was made both clinically and radiologically through MRI.
Operative procedure
All patients underwent arthroscopic reconstruction of the PCL by two experienced surgeons in our clinic. The choice of the graft was based upon the availability of allograft material and the possibility of obtaining a suitable bone-patellar-tendon-bone (BPTB) autograft. Preoperative patellofemoral pain, maltracking and a thin patellar tendon were the main contra-indications for the use of a BPTB autograft. Eight patients received a BPTB autograft, two patients a BPTB allograft and eight patients an Achilles tendon allograft.
A standard ligament evaluation was performed preoperatively with the patients under spinal or general anesthesia. Exploration of the joint was performed and meniscal and cartilage lesions were reported and treated if necessary. Four patients had, according to the Outerbridge classification, femoral chondral lesions (3 grade II–III medially, 1 grade III diffuse), three patients patellar lesions (diffuse grade II), two patients had a medial meniscal tear and four patients a lateral meniscal tear.
A posteromedial portal was made in order to facilitate visualization of the posterior cortex of the tibia (over the back position). The intra condylar space was inspected and the remnants of the PCL were removed. For the tunnel placement, we used anatomic landmarks as obtained from previous studies (Fig. 1) [12].
The tibial tunnel was drilled through the original PCL origin using a K-wire, under direct arthroscopic visualization and with the help of an aiming device. For both the tibial tunnel as well as for the femoral tunnel, intra-operative fluoroscopy was used to confirm proper tunnel positioning. The femoral tunnel was placed using a K-wire through the anterior aspect of the femoral footprint. The graft was positioned in a retrograde fashion. First, the graft was fixed at the tibial tunnel after pretensioning manually with the knee in 70° flexion, using a biodegradable interference screw (outside-in). At the femoral side graft fixation was performed after pretensioning the graft with the use of a biodegradable interference screw (outside-in) as well. After fixation, the structural properties of the graft were evaluated manually by testing the anterior-posterior translation as well as the posterolateral stability. In two patients concomitant surgery was performed for additional instability of the posterolateral complex (PLC). A Clancy tenodesis was done in one patient and a modified biceps tendon plasty (Fanelli) in the other.
In one patient, a patellar fracture occurred during operation, which did not need osteosynthesis. Perioperatively no major complications occurred.
Postoperative rehabilitation
During the first week, the knee was immobilized in a knee brace (Stroble supplement) in full extension day and night. Patients were allowed to mobilize nonweight bearing with the use of two crutches. The quadriceps musculature was trained, but no activity of the hamstrings was allowed. The passive range of motion (ROM) was gradually increased to 70°. From the second to the sixth week weight bearing increased depending on pain and swelling. The brace could be removed for exercising the quadriceps and co-contractions of quadriceps and hamstrings musculature. Passive flexion could be increased to 90°. In week seven till twelve weight-bearing was increased to 100% and the use of the knee brace was reduced. Passive flexion increased to 110°, and the use of a home trainer would be started. After this, the level of activity was raised with increasing active training of the hamstrings.
Evaluation
All examinations and results were evaluated by a single independent experienced examiner (J.J.). We used the international knee documentation committee (IKDC) knee examination form to evaluate knee function. The differences between the operated knee and the non-involved knee were documented. To evaluate the influence on daily life and sport activities the Tegner rating system was assessed pre and postoperatively. For subjective evaluation, patients were asked to grade their knee function before injury and at the moment of evaluation. The visual analogue scale (VAS) for pain scoring was used pre- and postoperatively.
Statistical analysis was performed with the use of the Wilcoxon Signed Ranks Test and Pearson’s Two-tailed test for correlation. The minimal level of significance was set at P<0.05.
Results
There were no significant differences in our patient population regarding final outcome with respect to sex, age, or mechanism of injury. The study group included 13 males and 5 females with an average age of 33 year. As expected the presence of femoral degenerative changes correlated to a high extent to age (P<0.01). The mean time from injury to operative reconstruction was 3 years. The elapsed time between injury and operation correlated to degenerative femoral pathology as well (P<0.05). Injury occurred during sport activities in nine patients and in motor vehicle accidents in nine patients. Patients were evaluated at a mean follow-up time of 3.3 years (range 1–6 years).
IKDC knee evaluation
Before reconstruction all patients were graded D (severely abnormal) using the IKDC evaluation form.
At follow-up one patient had a lack of extension between 6° and 10° (grade C) compared to the non-involved knee, four patients between 3° and 5° (grade B), and the majority of the patients (72%) had less then three degrees (grade A) lack of extension. With respect to the flexion, only one patient had a lack of flexion between 6° and 15° (grade B) compared to the non-involved knee, and all other patients had less then 5° (grade A) lack of flexion.
Evaluation of ligament laxity tested with the posterior drawer test, demonstrated an average tibial posterior displacement of more then 10 mm (grade D) in one patient, between 6 and 10 mm in two knees, and less then 6 mm in 15 knees (grades A and B). The outcome of the posterior drawer test correlated to the Tegner rating score after surgery (P<0.01), subjective evaluation, as well as the presence of pain (P<0.05).
The step-off test was graded A in 12 patients, B in three patients, and C in three patients. Additional ligament laxity revealed an anterior tibial translation with the Lachman test of 6–10 mm in two patients with a matching grade C pivot shift, both due to postoperatively occurring ACL injury. Three patients demonstrated (postero) lateral laxity, of which one patient was graded B, 1 graded C and 1 graded D in the overall IKDC score. Two patients complained of some mild to moderate retropatellar pain, independent of level of activity.
In functional testing most patients had some reluctancy to perform the one leg hop test in the first attempt, but almost all (89%) showed an average distance of more then 90% compared to the non-involved knee in three attempts (Table 1).
The final IKDC score, determined by the worst group grade, resulted in a grade A (normal) in five patients (28%), grade B (nearly normal) in eight (44%) patients, grade C (abnormal) in four (22%) patients, and grade D (severely abnormal) in one patient (6%). There was no correlation found between time to surgery and final outcome.
Subjective evaluation
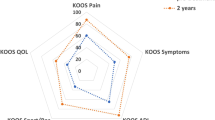
Patients graded their knees using a 1–10 scale before reconstruction and at follow-up. Before injury, the mean subjective score was 9, and at follow-up the mean score was 6.5. The subjective evaluation before injury demonstrated a correlation (P<0.01) with the existence of patellar pathology as observed during operation. The majority of patients stated their knee did not influence daily life with respect to pain or swelling and similar results were seen with respect to sport activities.
Patients evaluated their knees using the VAS for pain scoring, but pain usually only existed with very strenuous activity and presented quite variable (Fig. 2). The presence of pain correlated however strongly with the intensity of the pain (P<0.05), as well as to the subjective evaluation and the Tegner rating score (P<0.01). It was remarkable that most patients experienced pain at the femoral patellar joint when sitting on their knees for a prolonged time, but overall satisfaction after surgery was high.
Tegner rating system
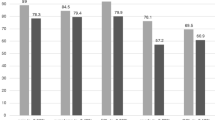
The mean Tegner score before injury was 7.8 (range 6–10). Just prior to reconstruction, none of the patients could perform sports activities at a satisfactory level, but the Tegner score restored to 6.6 at follow-up (range 4–9). Patients showed a significant improvement (P<0.01) after reconstruction when compared to the situation prior to operation. It was striking that the Tegner score at follow-up correlated to a high extent (P<0.05) to the patients’ own subjective evaluation.
Discussion
In this paper we present the results at the mid- term of arthroscopic PCL reconstruction in patients with symptomatic chronic instability of the PCL who did not respond to conservative treatment. There is still controversy concerning the best treatment for PCL injury. Although there appeared to be a consensus on conservative treatment as primary choice of treatment of isolated PCL tears and although the results of conservative treatment in this group seem to be promising [4–7], opinions vary with respect to the treatment of chronic instable knees, not responding well to conservative treatment.
The results of other studies [13–16] demonstrate reasonable effects of operative reconstruction. In a recent, retrospective study including eighty-nine patients, Richter et al. [11] compared surgical repair or reconstruction versus non-surgical treatment in traumatic knee dislocations, and on the basis of their findings suggest operational intervention in all intraligamentous ruptures.
We used a single bundle technique in our clinic for PCL reconstruction at the time surgery was being performed in the investigated patient population (1995–2000). Harner et al. demonstrated in a cadaver study [17], that the double bundle technique, restoring not only the original anterolateral bundle but also the posteromedial bundle, had superior biomechanical properties in comparison to single-bundle techniques [18, 19]. At present, reconstructions are being performed in our clinic with a double-bundle technique, and preliminary data are indeed promising. We have to keep in mind however that these results are only short-term results.
The group of patients we included in this study is comparable to other patient populations described in literature with respect to the division of age, sex, and mechanism of injury [4, 15, 16, 20, 21]. We are aware of the fact that the results of the present study may seem to be biased by having 25% of the original patient population lost to follow-up. The pre-operative characteristics with respect to the division of age, sex, mechanism of injury, and instability were nevertheless comparable with the 18 patients described in the manuscript and with the patient populations described elsewhere in literature. Hence, we are convinced that the bias is reduced to a minimum and that the data are representative. Furthermore, two of the six patients that were lost to follow-up were willing to take an interview by telephone and said to be satisfied with the results. The Tegner score before injury in our study group was average 7.8, indicating these patients participated in sports on quite a high level of activity. After falling back to unsatisfactory levels just before reconstruction, the Tegner score returned to a level of 6.6 at follow-up. A similar trend has been shown in other publications as well [7, 15]. The high correlation between patients’ own subjective evaluation and the Tegner score postoperatively was striking. These results correlated to the findings of the posterior drawer as well, although no significance was seen when compared to the final IKDC evaluation.
We used the IKDC knee examination form as a tool for examining the function of the knee. This form has been used before and has proven its usefulness for clinical application [15, 21, 22]. The most accurate test for evaluation of PCL instability has been demonstrated to be the posterior drawer test, especially in combination with tests like the step off test, the posterior sag sign and Lachman test [8, 9, 23]. Results in our study are in harmony with this finding.
We chose not to perform an instrumented evaluation with the use of an arthrometer, since its accuracy has been shown not to be optimal in evaluating PCL instability [24–26]. A possible drawback in the present study is the absence of stress radiography and the fact that objective posterior laxity has been evaluated only clinicaly. Preoperative radiologic evaluation existed of plain radiographic images and confirmation of the PCL injury with magnetic resonance imaging. Allthough clinical examination has a high accuracy for the detection of posterior cruciate ligament instability (90% sensitivity and 99% specificity), the actual detected amount of posterior translation may be biased by the examiner. We did not use additional radiographic evaluation, because during the study period the utilization of stress radiography in our clinic was not daily practice and alternative imaging (such as the Puddu view) was not validated.
We could not find any statistically significant differences between the different graft types with respect to the clinical outcome. This corresponds to other findings in the literature as well. Schultz and Carr [27] for instance conclude on the base of a comparison between clinical outcomes of several prospective randomized trials, that the results of a reconstruction with an autogenous patellar or hamstring graft do not differ much. The same results were demonstrated for PCL reconstructions [28, 29]. The two patients with additional instability did not demonstrate different results. We would like to stress the importance of addressing additional pathology when performing PCL reconstruction.
Our overall IKDC outcome showed reasonable (72% grade A/B), however not optimal results of reconstructive surgery. Although patient satisfaction and the effect of reconstruction on daily life activities was high in most of the cases, still five out of 18 patients presented with a (severely) abnormal or abnormal knee function (28% C/D), and the trend in sports activities suggested a marked decrease in level of performance. Nevertheless, although no control group is available, the 72% succesfull operation may be seen as a robust result.
As counts for all the above, it is very difficult to make conclusions based upon literature, when different patient populations and outcomes are being studied, when different techniques are being used, etc. We conclude on the basis of our findings however, that arthroscopic reconstruction of symptomatic chronic PCL instability, not responding well to conservative therapy, can be greatly beneficial.
Future directions
As is the case for ACL instability, much work still has to be done to optimize treatment of PCL injuries. Enhancement of tunnel fixation, timing of intervention, application of growth factors and the role of tissue engineering for the PCL, are just some of the many interesting topics that ask for being studied in the future.
References
Clancy WG Jr, et al (1983) Treatment of knee joint instability secondary to rupture of the posterior cruciate ligament. Report of a new procedure. J Bone Joint Surg Am 65(3):310–322
Fanelli GC, Edson CJ (1995) Posterior cruciate ligament injuries in trauma patients: Part II. Arthroscopy 11(5):526–529
Chen CH, Chen WJ, Shih CH (1999) Arthroscopic posterior cruciate ligament reconstruction with quadriceps tendon-patellar bone autograft. Arch Orthop Trauma Surg 119(1–2):86–88
Parolie JM, Bergfeld JA (1986) Long-term results of nonoperative treatment of isolated posterior cruciate ligament injuries in the athlete. Am J Sports Med 14(1):35–38
Shelbourne KD, Davis TJ, Patel DV (1999) The natural history of acute, isolated, nonoperatively treated posterior cruciate ligament injuries. A prospective study. Am J Sports Med 27(3):276–283
Keller PM, et al (1993) Nonoperatively treated isolated posterior cruciate ligament injuries. Am J Sports Med 21(1):132–136
Fowler PJ, Messieh SS (1987) Isolated posterior cruciate ligament injuries in athletes. Am J Sports Med 15(6):553–557
Covey CD, Sapega AA (1993) Injuries of the posterior cruciate ligament. J Bone Joint Surg Am 75(9):1376–1386
Harner CD, Hoher J (1998) Evaluation and treatment of posterior cruciate ligament injuries. Am J Sports Med 26(3):471–482
Geissler WB, Whipple TL (1993) Intraarticular abnormalities in association with posterior cruciate ligament injuries. Am J Sports Med 21(6):846–849
Richter M, et al (2002) Comparison of surgical repair or reconstruction of the cruciate ligaments versus nonsurgical treatment in patients with traumatic knee dislocations. Am J Sports Med 30(5):718–727
Morgan CD, Kalman VR, Grawl DM (1997) The anatomic origin of the posterior cruciate ligament: where is it? Reference landmarks for PCL reconstruction. Arthroscopy 13(3):325–331
Kim SJ, et al (2000) Comparison of 1- and 2-incision posterior cruciate ligament reconstructions. Arthroscopy 16(3):268–278
Mariani PP, et al (1997) Arthroscopic posterior cruciate ligament reconstruction with bone-tendon-bone patellar graft. Knee Surg Sports Traumatol Arthrosc 5(4):239–244
Mariani PP, Margheritini F, Camillieri G (2001) One-stage arthroscopically assisted anterior and posterior cruciate ligament reconstruction. Arthroscopy 17(7):700–707
Aglietti P, Buzzi R, Lazzara D (2002) Posterior cruciate ligament reconstruction with the quadriceps tendon in chronic injuries. Knee Surg Sports Traumatol Arthrosc 10(5):266–273
Harner CD, et al (2000) Biomechanical analysis of a double-bundle posterior cruciate ligament reconstruction. Am J Sports Med 28(2):144–151
Race A Amis AA (1998) PCL reconstruction. In vitro biomechanical comparison of ‘isometric’ versus single and double-bundled ‘anatomic’ grafts. J Bone Joint Surg Br 80(1):173–179
Giffin JR, et al (2002) Single- versus double-bundle PCL reconstruction: a biomechanical analysis. J Knee Surg 15(2):114–120
Chen CH, Chen WJ, Shih CH (2002) Arthroscopic reconstruction of the posterior cruciate ligament: a comparison of quadriceps tendon autograft and quadruple hamstring tendon graft. Arthroscopy 18(6):603–612
Nyland J, Hester P, Caborn DN (2002) Double-bundle posterior cruciate ligament reconstruction with allograft tissue: 2-year postoperative outcomes. Knee Surg Sports Traumatol Arthrosc 10(5):274–279
Hefti F, et al (1993) Evaluation of knee ligament injuries with the IKDC form. Knee Surg Sports Traumatol Arthrosc. 1(3–4):226–234
Malanga GA, et al (2003) Physical examination of the knee: A review of the original test description and scientific validity of common orthopedic tests. Arch Phys Med Rehabil 84(4):592–603
Wang CJ, et al (2002) Outcome of surgical reconstruction for posterior cruciate and posterolateral instabilities of the knee. Injury 33(9):815–821
Rubinstein RA Jr, et al (1994) The accuracy of the clinical examination in the setting of posterior cruciate ligament injuries. Am J Sports Med 22(4):550–557
Miller MD, et al (1993) Posterior cruciate ligament injuries. Orthop Rev 22(11):1201–1210
Schultz WR, Carr CF (2002) Comparison of clinical outcomes of reconstruction of the anterior cruciate ligament: autogenous patellar tendon and hamstring grafts. Am J Orthop 31(11):613–620
Wang CJ, et al (2004) Comparison of autogenous and allogenous posterior cruciate ligament reconstructions of the knee. Injury 35(12):1279–1285
Chen CH, et al (2004) Fixation strength of the different graft types used in posterior cruciate ligament reconstructions. Knee Surg Sports Traumatol Arthrosc 12(5):371–375
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jenner, J.M.G.T., van der Hart, C.P. & Willems, W.J. Mid-term results of arthroscopic reconstruction in chronic posterior cruciate ligament instability. Knee Surg Sports Traumatol Arthr 14, 848–853 (2006). https://doi.org/10.1007/s00167-006-0056-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-006-0056-3