Abstract
This study investigated the anatomy of the structures that form the extensor mechanism of the knee joint using microsurgical techniques. Ten fresh-frozen human adult cadaveric knees were used. The quadriceps components, the infrapatellar tendon, the patellofemoral ligaments, and their relations to the neighboring anatomical structures were measured. The angles of the vastus lateralis and the vastus medialis muscle fibers to the rectus tendon were 26.6 and 41.1°, respectively. The medial patellofemoral ligament connecting the femoral medial epicondyle to the medial edge of the patella was approximately 54.2 mm long, and its width ranged from 9 to 30 mm. The medial patellomeniscal ligament had a wide attachment to the meniscus whereas the attachment to the patella was narrow. The patellar tendon was 31.9 mm broad at its attachment to the apex of the patella and 27.4 mm wide at its attachment to the tibial tubercle. It was 38–49 mm long. Using the surgical microscope we were able to dissect and identify a trilaminar arrangement of prepatellar fibrous soft tissues. Also, we were able to identify the vessels and nerves around the patella. Details of clinical relevance and the possible pathological implications of the material presented are discussed. Emphasis is placed on the stability of the patellofemoral joint and the complex interaction between a range of factors providing it.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The extensor mechanism of the knee joint has received a great deal of academic and clinical attention. It consists of a complex arrangement of various muscles, tendons, ligaments, and soft-tissue structures. These structures include the quadriceps muscle and its common tendon, the patellar tendon, the retinaculum, the pre-patellar structures, the Hoffa’s fat pad, and the quadriceps pouch.
Knowledge of the anatomy of the extensor mechanism is essential for an understanding of patellofemoral stability. The stability of the patellofemoral joint is provided by both dynamic and static stabilizers, in addition to the bony architecture [15]. Passive laxity of the patella is prevented by the peripatellar retinaculum. Medially, the restraints include a capsular condensation in addition to the patellofemoral and patellotibial ligaments [14]. Thus, the patellar tendon is a primary restraint in the coronal plane and limits patellar excursion to 10 mm proximally [11]. The “balance” of the static restraints is maintained by the dynamic restraints [26]. These are mainly the quadriceps muscle with its four components and secondarily the iliotibial band [16].
Various studies have described the possible role of anatomic variations in the quadriceps mechanism in relation to abnormal conditions [4, 9, 26]. Subluxation of the patella has been associated with multiple anatomic findings, including dystrophy of the vastus medialis (VM) muscle, external tibial torsion, lateral insertion of the patellar tendon, genu valgum, and patella alta [17].
Based on the deductions of two previous studies, in which we used microsurgical techniques [7, 21], we assumed that a microanatomical dissection of this region could answer some of the questions about the complex anatomy of the extensor mechanism.
Materials and methods
Ten fresh-frozen human adult cadaveric knees were used for the study. They were maintained at −20°C and prior to the dissection were thawed at room temperature for 18 h. There were six right and four left knees, seven male and three female, with a mean age of 55 years. There was no evidence of marked bony abnormality or degenerative disease. Ligamentous integrity was also ensured. All specimens included at least 12 cm of bone and soft tissue on each side of the knee joint.
The dissections were begun by first separating the skin and subcutaneous tissue over the anterior aspect of the knee from the superficial fascia. The dissection was then extended laterally and medially. Once the patella had been reached, each layer was sequentially incised longitudinally in the midsagittal plane. The dissection of each layer was then extended proximally, distally, medially, and laterally. When a separate aponeurotic layer was identified deep in the superficial transverse fascia, it was incised longitudinally. The separation of the layer was extended proximally, distally, medially, and laterally. The presence and character of the remaining soft tissues anterior to the patella, such as the continuation of the rectus femoris fibers, were also documented.
The procedure was performed using magnifying loupes (magnification 3.5×). After the trilaminar arrangement of prepatellar fibrous soft tissues, we continued the dissection proximally to identify the four main muscular elements of the quadriceps. We measured the superficial length of the quadriceps tendon from the patellar base to the myotendinous junction of the rectus femoris (Table 1). We also measured its width at the superior aspect of the patella as well as at its half-length with the millimetric scale of a ruler. The rectus femoris and vasti were dissected apart and reflected distally while the details of their tendinous insertions were noted carefully.
A careful dissection of all ligamentous structures of the anterior aspect of the knee joint was then performed using an operative microscope (magnification 6× and 10×) and microsurgical instruments (microsurgical scissors and forceps).
Dissecting the area, care was taken to identify the vascular anastomosis and nerves around the patella.
All the anatomic components were photographed and dimensions were recorded using a micrometer. The anatomical variations, ligament shapes, separated bundles of the ligaments, and topography of ligament attachments were also described and recorded.
Results
The extensor mechanism consisted of four distinct muscle bellies (quadriceps muscle) that shared a common tendon of insertion (Fig. 1). The quadriceps tendon was trilaminar, with the anterior layer formed by the rectus femoris, the intermediate layer formed by the VM and vastus lateralis (VL), and the deep layer by the tendon of the vastus intermedius (Fig. 1).
The quadriceps tendon (QT) is trilaminar, with the anterior layer formed by the rectus femoris (RF), the intermediate layer formed by the vastus medialis (VM) and vastus lateralis (VL) and the deep layer (not visible) by the tendon of the vastus intrmedius and patella (P). The pins are sited at the proximal and distal ends of the superficial quadriceps tendon
The rectus femoris narrowed to a tendon which inserted into the superior pole of the patella. With the knee flexed the mean distance of the most superficial layer of the quadriceps tendon from the anterosuperior part of the patella to the myofascial junction of the rectus femoris was 68 mm (SD 11.01) (Fig. 1).
The VL extended halfway down, giving off a fibrous expansion. It blended with the lateral patellar retinaculum, through which there was a direct attachment to the tibia.
The VM was a muscle which formed the intermediate layer having the most distal fibers passing almost horizontally and anteriorly toward their insertion into the common tendon and the medial border of the patella. This part of the muscle was sometimes described as the vastus medialis obliquus (VMO) (Fig. 2). Like the VL, the VM had a distal fibrous expansion that blended with the medial patellar retinaculum.
The vastus medialis (VM) has a distal fibrous expansion that blends with the medial patellar retinaculum. The most distal fibers of the VM are almost horizontal as they pass anteriorly to the insertion into the common tendon and the medial border of the patella (P). This part of the muscle is sometimes described as the vastus medialis obliquus (VMO)
The vastus intermedius partly blended with the VM medially. The fibers of the rectus femoris and vastus intermedius inserted almost perpendicularly into the superior pole of the patella, whereas the fibers of the VM and VL inserted obliquely.
A goniometer was used to measure the angles of the muscle fibers to the rectus tendon, which was 26.6° (SD 6.18) for the VL and 45.5° (SD 8.39) for the medialis (Table 1).
The width of the quadriceps tendon at mid-length and at the superior aspect of the patella was 22.7 mm (SD 4.16) and 41.1 mm (SD 6.99), respectively (Table 1). The common tendon inserted into the patella.
Medial and lateral portions of the quadriceps tendon passed down on either side of the patella and inserted into the proximal tibia on either side of the tuberosity. These expansions merged into the capsule, forming the medial and lateral retinacula.
On the medial side of the knee a band of retinacular tissue connected the femoral medial epicondyle to the proximal two-thirds of the medial edge of the patella forming the medial patellofemoral ligament (MPFL) (Fig. 3). The MPFL was approximately 54.2 mm (SD 6.08) long, and its width ranged from 9 to 30 mm (Table 1). It was overlaid by the distal part of VMO to a variable extent, and fibers of MPFL merged into the deep aspect of the muscle (Figs. 4, 5).
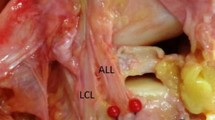
From the inferior border of the medial patellar edge the medial patellomeniscal ligament (MPML) connected the patella to the anterior horn of the medial meniscus (Fig. 6). The MPML had a wide attachment to the meniscus where the fibers fanned out making it difficult to define the posterior margin of the ligament.
The medial patellomeniscal ligament (MPML) connects the inferior border of the medial patellar edge (P) and the anterior horn of the medial meniscus (MM). The MPML had a wide attachment to the meniscus where the fibers fanned out making it difficult to define the posterior margin of the ligament; medial epicondyle (ME); medial collateral ligament (MCL); tibial plateau (TP), and patella tendon (PT)
On the lateral side of the knees, we identified the superficial oblique retinaculum. Posteriorly, the deep transverse retinaculum was found to consist of three major components: the transverse patellofemoral ligament or epicondylopatellar band, which coursed superolaterally, the transverse retinaculum, which coursed directly from the ITB to the midpatella and the patellotibial band, which ran between the patella and the tibia inferiorly.
A trilaminar arrangement of prepatellar fibrous soft tissues was observed in all knees dissected, similar to the findings of Dye et al. [8] (Fig. 7). All knees demonstrated a superficial fascial layer with orientation of the fibers transverse to the long axis of the patella (Fig. 8). One knee did not demonstrate an intermediate oblique aponeurotic layer. The fibers of this layer in the other knees had a more oblique orientation and were contributed to by expansions of the VL and VM tendons as well as the more superficial fibers of the rectus femoris. An incision of this intermediate aponeurotic layer revealed the deep longitudinally oriented fibers of the rectus femoris anterior to the patella (Fig. 9). All knees had a continuation of the rectus femoris fibers, which were always inserted directly into the anterior patellar bone.
The trilaminar arrangement of prepatellar fibrous soft tissues. The superficial fascial layer (layer 1) with orientation of the fibers transverse to the long axis of the patella, the intermediate oblique aponeurotic layer (layer 2) and the deep longitudinally oriented fibers of the rectus femoris anterior to the patella (layer 3)
The fibers of the intermediate layer (layer 2) have a more oblique orientation and were contributed to by the expansions of the vastus lateralis and vastus medialis tendons as well as the more superficial fibers of the rectus femoris. An incision of this intermediate aponeurotic layer revealed the deep longitudinally oriented fibers of the rectus femoris anterior and adherent to the patella (layer 3); retracted superficial fascial layer (layer 1)
The patellar tendon was a flat structure derived primarily from the central fibers of the rectus femoris that extended distally over the anterior surface of the patella. It inserted on the tibial tubercle, usually beginning just distal to the tubercle’s most superior extreme. It continued past the tubercle to blend with the fascial expansions of the iliotibial tract on the anterior surface of the tibia. It was 31.9 mm (SD 3.6) broad at its insertion into the apex of the patella and 27.4 mm (SD 3.5) wide at its insertion into the tibial tubercle. It was 38–49 mm long (Table 1).
The infrapatellar fat pad covered the extra-articular portion of the posterior patellar surface. The fat pad extended superiorly to merge with the peripatellar fold on both sides of the patella. It was pierced by numerous blood vessels derived from the genicular arteries.
Dissecting the anterior aspect of the knee, care was taken to identify the infrapatellar branch of the saphenous nerve (Fig. 10). It traversed the sartorius muscle and joined the patellar plexus, providing innervation to the anteromedial capsule, patellar tendon, and skin anteromedially.
The infrapatellar branch of the saphenous nerve (IBSN) traversed the sartorius muscle and joined the patellar plexus, providing innervation to the anteromedial capsule, patellar tendon (PT), and skin anteromedially; patella (P), inferior pole of the patella (IPP), vastus medialis (VM), and medial epicondyle (ME)
A vascular circle was identified around the patella, which according to Scapinelli [29], supplied the patella by nutrient arteries that entered predominantly at the inferior pole.
Discussion
An accurate and ever-improving knowledge of musculoskeletal structure and the associated relationships should be a fundamental goal for all orthopedic surgeons. For those with an interest in the knee joint, the anatomy and biomechanics of the extensor apparatus present a substantial challenge [19].
Despite the prevalence of literature describing the morphology and function of the VMO as an individual muscle, limited bibliography actually substantiates the existence of the VMO as a separate, distinct muscle from the vastus medialis longus (VML) [14].
The VMO muscle is reported to be the primary stabilizer of the patella during knee extension. Many articles have been published describing the fiber alignment, nerve innervation, function, sequela from injury to and/or atrophy of the VMO and its rehabilitation [1, 4, 9, 15, 20, 26]. However, it remains controversial if the VMO appears to be an anatomically and functionally separate structure from the VML [14]. The average fiber angle measurements seen in this study of 45.5° for the distal fibers of the VM are in agreement with previously published VM fiber angle measurements. Koskinen and Kujala, however, have noted more proximal insertion of the VM in patients with patellar dislocation [18]. Understanding the relationship between the VMO morphology and patellar tracking [19] will be useful in diagnosis, treatment, and prevention of patellar subluxation and dislocation.
The MPFL, although varying in thickness and quality [2, 10, 31], was found to be the major medial soft-tissue restraint to patellar lateral displacement [2, 5, 13]. Its stabilizing role in the normal knee and its injury as an essential lesion of patellar instability has been appreciated only recently [2, 31]. There is a 97% incidence of traumatic tears of the MPFL in acute patellar dislocation. Lateral patellar displacement tests in vitro showed that the patella subluxed most easily at 20° knee flexion [9, 28]. Isolated release resulted in a 50% increase in lateral displacement. We found, in agreement with Tuxoe et al. [38], that the distal edge of the MPFL was very often difficult to define. Therefore, we may find difficulties in surgical exploration of this ligament.
In addition, the patellotibial and patellomeniscal ligament complex have been found to play an important secondary role in restraining lateral patellar displacement. Isolated repair of these ligaments restored balance to near normal levels [13]. In our study, similar to the findings of Feller et al. [10] and Tuxoe et al. [38], we found that the patellar insertion of the PML is very narrow and the meniscal insertion very wide. This could explain why many patients with acute lateral patellar dislocation have a tear from the inferior medial part of the patella at the attachment of the PML. Management should, therefore, be directed both at correcting anatomic abnormalities when indicated, and at reconstruction of medial restraints of patellar tracking [3, 9, 11].
The arterial supply of the human patellar ligament has been systematized on 20 knees by Soldado et al. [32]. We observed three arterial pedicles: superior, middle, and inferior placed on each side of the patellar ligament. Medial pedicles had their origin from the descending and the inferior medial genicular arteries. The lateral pedicles took their origin from the lateral genicular arteries and the recurrent tibial anterior artery. Two main vascular arches anastomosed with these pedicles: the retropatellar and the supratubercular.
A goal of this study was to define carefully the anatomic distribution of the infrapatellar branch of the saphenous nerve. Tifford et al. [37] with an anatomic study provide the surgeon with reliable parameters as to where the nerve is most commonly encountered and specific surgical recommendations to minimize the risk of nerve injury.
In conclusion, the findings of this study should help in understanding the complex function of the extensor mechanism, which demands knowledge of not only its anatomic structures but of their balanced relationships as well. An awareness of a layer concept of tissue orientation is helpful in understanding surgical access as well as the normal function of the decelerator mechanism. This awareness is a prerequisite to the evaluation and treatment of musculoskeletal disorders [36].
Such a disorder is the recurrent dislocation or subluxation of the patellofemoral joint, which is always a challenge to the orthopedic surgeon. Once a correct diagnosis is established, appropriate treatment plans, including both non-operative and operative methods, may yield consistent results.
References
Adler N, Perry B, Kent B, Robertson K (1983) Electromyography of the vastus medialis oblique and vasti in normal subjects during gait. Electromyogr Clin Neurophysiol 233:643–649
Amis AA, Firer P, Mountney J, Senavongse W, Thomas NP (2003) Anatomy and biomechanics of the medial patellofemoral ligament. Knee 10(3):215–220
Beasley LS, Vidal AF (2004) Traumatic patellar dislocation in children and adolescents: treatment update and literature review. Curr Opin Pediatr 16(1):29–36
Bose K, Kanagasuntheram R, Osman MBH (1980) Vastus medialis oblique: an anatomic and physiologic study. Orthopaedics 3:880–883
Conlan T, Garth WP Jr, Lemons JE (1993) Evaluation of the medial soft-tissue restraints of the extensor mechanism of the knee. J Bone Joint Surg Am 75(5):682–693
Desio SM, Burks RT, Bachus KN (1998) Soft tissue restraints to lateral patellar translation in the human knee. Am J Sports Med 26(1):59–65
Diamantopoulos A, Tokis A, Tzurbakis M, Patsopoulos I, Georgoulis A (in press) The posterolateral corner of the knee: evaluation under microsurgical dissection. Arthroscopy (in press)
Dye SF, Campagna-Pinto D, Dye CC, Shifflett S, Eiman T (2003) Soft-tissue anatomy anterior to the human patella. J Bone Joint Surg Am 85A(6):1012–1017
Farahmand F, Tahmasbi NM, Amis AA (2004) The contribution of the medial retinaculum and quadriceps muscles to patellar lateral stability—an in-vitro study. Knee (11):89–94
Feller JA, Feagin JA Jr, Garrett WE Jr (1993) The medial patellofemoral ligament revisited: an anatomical study. Knee Surg Sports Traumatol Arthrosc 1(3–4):184–186
Fithian DC, Paxton EW, Cohen AB (2004) Indications in the treatment of patellar instability. J Knee Surg 1(1):47–56
Fulkerson JP, Hungerford DS (1990) Disorders of the patellofemoral joint, 2nd edn. Williams & Wilkins, Baltimore
Hautamaa PV, Fithian DC, Kaufman KR, Daniel DM, Pohlmeyer AM (1998) Medial soft tissue restraints in lateral patellar instability and repair. Clin Orthop 349:174–182
Hubbard KJ, Sampson HW, Elledge JR (1997) Prevalence and morphology of the vastus medialis oblique muscle in human cadavers. Anat Rec 249:135–142
Hughston JC (1968) Subluxation of the patella. J Bone Joint Surg Am 50:1003–1026
Jeffreys TE (1963) Recurrent dislocation of the patella due to abnormal attachment of the ilio-tibial tract. J Bone Joint Surg Br 45:740–743
Kaplan EB (1962) Some aspects of functional anatomy of the human knee joint. Clin Orthop 23:18–29
Koskinen SK, Kujala UM (1992) Patellofemoral relationships and distal insertion of the vastus medialis muscle: a magnetic resonance imaging study in nonsymptomatic subjects and in patients with patellar dislocation. Arthroscopy 8(4):465–468
Lieb FJ, Perry J (1968) Quadriceps function. an anatomical and mechanical study using amputated limbs. J Bone Joint Surg 50:1535–1548
MacNab I (1952) Recurrent dislocation of the patella. J Bone Joint Surg Am 34:957–967
Makris CA, Georgoulis AD, Papageorgiou CD, Moebius UG, Soucacos PN (2000) Posterior cruciate ligament architecture: evaluation under microsurgical dissection. Arthroscopy 16(6):627–632
Merchant AO (1988) Classification of patellofemoral disorders. Arthroscopy 4(4):235–240
Mont MA, Rajadhyaksha AD, Low K, LaPorte DM, Hungerford DS (2001) Anatomy of the knee extensor mechanism: correlation with patellofemoral arthrosis. J South Orthop Assoc 10(1):24–31
Ober FR (1939) Recurrent dislocation of the patella. Am J Surg 43:497
Reider B, Marshall J, Koslin B, Ring B, Girgis F (1981) The anterior aspect of the knee joint. J Bone Joint Surg 63A:351–356
Sakai N, Luo Z, Rand J, An K (2000) The influence of weakness in the vastus medialis oblique muscle on the patellofemoral joint: an in vitro biomechanical study. Clin Biomechanics 15:335–339
Salzman A, Torburn L, Perry J (1993) Contribution of rectus femoris and vasti to knee extension. An electromyographic study. Clin Orthop 290:236–243
Senavongse W, Farahmand F, Jones J, Andersen H, Bull AM, Amis AA (2003) Quantitative measurement of patellofemoral joint stability: force-displacement behavior of the human patella in vitro. J Orthop Res 21(5):780–786
Scapinelli R (1967) Blood supply of the human patella. Its relation to ischaemic necrosis after fracture. J Bone Joint Surg Br 49(3):563–570
Smillie IS (1951) Injuries of the knee joint.2nd edn. E & S Livingstone, Edinburgh, p 249
Smirk C, Morris H (2003) The anatomy and reconstruction of the medial patellofemoral ligament. Knee 10(3):221–227
Soldado F, Reina F, Yuguero M, Rodriquez-Baeza A (2002) Clinical anatomy of the arterial supply of the human patellar ligament. Surg Radiol Anat 24(3–4):177–182
Speakman HG, Weisberg J (1977) The vastus medialis controversy. Physiotherapy 63:249–254
Suzuki S (1987) The role of the quadriceps muscle for the patellofemoral malalignment syndrome. J Jpn Orthop Assoc 61:905–916
Tanner SM, Garth Jr WP, Soileau R, Lemons JE (2003) A modified test for patellar instability: the biomechanical basis. Clin J Sport Med 13(6):327–338
Terry GC (1989) The anatomy of the extensor mechanism. Clin Sport Med 8(2):163–177
Tifford CD, Spero L, Luke T, Plancher KD (2000) The relationship of the infrapatellar branches of the saphenous nerve to arthroscopy portals and incisions for anterior cruciate ligament surgery. An anatomic study. Am J Sports Med 28(4):562–567
Tuxoe IJ, Teir M, Winge S, Nielsen LP (2002) The medial patellofemoral ligament: a dissection study. Knee Surg Sports Traumatol Arthrosc 10(2):96–101
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Andrikoula, S., Tokis, A., Vasiliadis, H.S. et al. The extensor mechanism of the knee joint: an anatomical study. Knee Surg Sports Traumatol Arthrosc 14, 214–220 (2006). https://doi.org/10.1007/s00167-005-0680-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-005-0680-3