Abstract
Purpose
Sudden cardiac death (SCD) is a major public health concern, but data regarding epidemiology of this disease in Western European countries are outdated. This study reports the first results from a large registry of SCD.
Methods
A population-based registry was established in May 2011 using multiple sources to collect every case of SCD in Paris and its suburbs, covering a population of 6.6 million. Utstein variables were recorded. Pre-hospital and in-hospital data were considered, and the main outcome was survival at hospital discharge. Neurologic status at discharge was established as well.
Results
Of the 6,165 cases of SCD recorded over 2 years, 3,816 had a resuscitation attempt and represent the study population. Most patients were male (69 %), the SCD occurred at home (72 %) with bystanders in 80 % of cases, and cardiopulmonary resuscitation (CPR) was performed in 45 % of cases. Initial rhythm was shockable in 26 % of cases. A total of 1,332 patients (35 %) were admitted alive to hospital. Among hospitalized patients, 58 % had a coronary angiogram, and the same proportion had therapeutic hypothermia. Finally, 279 patients (7.5 %) were discharged alive, of whom 96 % had a favorable neurological outcome. In multivariate analysis, bystander CPR (OR 2.1, 95 % CI 1.5–3.1) and initial shockable rhythm (OR 11.5, 95 % CI 7.6–17.3) were positively associated with survival at hospital discharge, whereas age (OR 0.97 per year, 95 % CI 0.96–0.98), longer response time (OR 0.93 per minute, 95 % CI 0.89–0.97), occurrence at home (OR 0.4, 95 % CI 0.3–0.6), and epinephrine dose greater than 3 mg (OR 0.05, 95 % CI 0.03–0.08) were inversely associated with survival.
Conclusion
Despite being conducted in the therapeutic hypothermia and early coronary angiogram era, hospital discharge survival rate of resuscitated SCD remains poor. The current registry suggests ways to improve pre-hospital and in-hospital care of these patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In spite of therapeutic advances, sudden cardiac death (SCD) remains a frequent and often fatal disease, with highly different survival rates between studies and countries [1]. Knowledge about the extent of this disease is crucial in order to match research themes with public health needs [2].
In a recent meta-analysis, Sasson et al. [1] reported a survival rate to hospital discharge after SCD between 6 and 8 %. However, the French emergency medical system (EMS) differs significantly from the North American EMS, with early medicalization of patients [3]. The impact of this marked specificity has been discussed [4]. To the best of our knowledge, prognosis of SCD is not documented in the French EMS system.
During hospitalization of out-of-hospital cardiac arrest (OHCA) patients, percutaneous coronary intervention (PCI) [5, 6] and therapeutic hypothermia (TH) [7–9] have been proposed to improve the prognosis of SCD. However, despite their inclusion in guidelines [10], the extent of these therapies in clinical practice is not known, and available data are derived from trials involving intensive care units highly aware of the benefits of these therapies, or from declarative surveys [11].
Considering the lack of broad epidemiological data, we developed a population-based registry with multiples sources, serving exhaustively a large population in Paris and its suburbs, representing more than 10 % of the overall French population. In this study, we reported factors from every link of the chain of survival, including both pre-hospital and hospital care, in order to perform an overview of the characteristics, management, and prognosis of SCD with resuscitation attempt.
Materials and methods
The methodology of this study is consistent with the STROBE checklist for observational studies [12].
Study setting
The Paris—Sudden Death Expertise Center (SDEC) Registry is a population-based registry concerning Paris and its suburbs (Hauts-de-Seine, Seine-Saint-Denis, Val-de-Marne), including a residential population of approximately 6.6 million and covering 762 km2 (294 square miles).
In France, the EMS is a two-tiered physician-manned system, with a basic life support tier served by firefighters of the Brigade de Sapeurs Pompiers de Paris (BSPP), who can apply automated external defibrillators (AED), and an advanced cardiac life support (ACLS) tier, provided in the field, with systematic endotracheal intubation, intravenous access line, and drug following the international guidelines if necessary [3, 13].
Study population
According to definitions from recent guidelines [14], every case of out-of-hospital SCD (defined as unexpected death without obvious extracardiac cause) occurring in the area of interest, with age over 18 years, was included in the SDEC registry, from 15 May 2011 to 15 May 2013. Exclusion criteria were patients aged under 18 years, SCD occurring outside the area of interest, prior terminal condition (such as metastatic malignancy), or obvious non-cardiac cause according to Utstein templates (trauma, submersion, respiratory, etc.) [15].
Data collection
To ensure completeness of collection, the SDEC Registry was derived from an intensive and prospective epidemiologic case-finding. Combining “passive” and “active” attitudes warranted the most extensive collection of cases of SCD, significantly superior to passive detection of cases alone. In addition, an individual review of each case ensured specificity, and avoided the overestimation often experienced in retrospective collection.
First, for every cardiac arrest supported by BSPP, a nominative case report form was sent daily (source 1). Second, an electronic query algorithm was performed in the advanced cardiac life support computer system to identify every case of SCD (source 2). Finally, retrospective controls based on diagnostic codes were conducted in selected intensive care units (control). Thus, the method of collection involved every link of the chain of survival, to ensure completeness of the registry. We performed retrospective control among a sample of three intensive care units, and combination of both sources (BSPP and ACLS) detected 99 % of cases of cardiac arrests admitted alive in this sample.
Recorded variables
Utstein templates for patient data collection were followed [15]. General data included demographics characteristics and location of arrest (street address, residential or public place). Data recorded about pre-hospital care included response time (defined by the delay between call and arrival of EMS), presence of bystander, bystander cardiopulmonary resuscitation (CPR) before EMS arrival, presence of shockable rhythm before advanced life support, defibrillation attempt during resuscitation, deliverance and dose of epinephrine (total dose delivered by EMS during advanced life support), and survival until admission.
For every hospitalized patient, the hospitalization report was recorded, including TH, coronary angiogram, death or discharge from hospital, and neurological status at discharge (according to Cerebral Performance Category (CPC) score [16], considering a CPC score of 1 or 2 as a favorable outcome; Electronic Supplementary Material no. 1). For in-hospital deaths, the cause of death was classified retrospectively as
-
Hemodynamic failure: refractory shock despite pharmacological or mechanical support, multiple organ failure, or new fatal arrhythmia
-
Neurological failure: brain death, or severe neurological prognosis leading to withdrawal of life-sustaining treatments
-
Other: acute respiratory distress, sepsis, etc.
Two investigators reviewed each record for data completion and validity.
Statistical analysis
For statistical analysis, we only included patients with a resuscitation attempt by emergency medical services. Continuous data were expressed as mean ± standard deviation (SD). Categorical data were expressed as frequencies and percentages. Variables were considered for statistical analysis if missing data did not exceed 15 %, except for epinephrine dose (23 % of missing data). We checked the linearity of quantitative variables using fractional polynomial regression. In the case of absence of linearity, continuous variables were dichotomized according to the cutoff already accepted, if possible, or according to preselected threshold otherwise. Comparisons used the χ 2 test for categorical variables and Student’s t test or Mann–Whitney–Wilcoxon test, when appropriate, for continuous variables. Patients were compared according to initial shockable rhythm and, for patients admitted alive, according to application of TH and coronary angiogram. For prognosis analysis, only pre-hospital variables were included in first multivariate analysis. Variables associated with survival at discharge (with P < 0.15) in univariate analysis were assessed in multivariate logistic regression. A second model, restricted to patients admitted alive in hospital (i.e., those likely to receive these treatments because the others died in the field), also included coronary angiography and TH as cofactors. We performed multivariate analysis with listwise deletion. Finally, variables were considered statistically significant for P < 0.05. All analyses were two-sided. Statistical analysis was performed using STATA 11.0 (Lakeway Drive, TX, USA).
Results
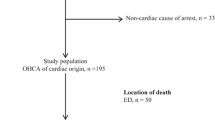
During the 2-year study period, 7,238 out-of-hospital cardiac arrests occurred in the study area. After excluding obvious extracardiac etiology, 6,165 were classified as SCD cases. Among them, 3,816 patients had a resuscitation attempt, and represent the study population (Fig. 1). Vital status at hospital discharge was available for 3,737/3,816 (98 %).
Baseline characteristics of patients with resuscitation attempt
Population characteristics are summarized in Table 1. Patients were predominantly male (69 %), with a mean age of 65.2 years. SCD occurred at home in 72 % of cases, with a bystander in 80 %. Bystander CPR was performed before EMS arrival in 45 % of SCD, and initial rhythm was shockable in 26 %. The median epinephrine dose delivered was 5 mg. A total of 2,484 patients (65 %) died on site, and 1,332 (35 %) were admitted alive to hospital. Among hospitalized patients, coronary angiography was performed only in 733/1,264 (58 %) of patients. Among them, acute myocardial infarction was ascertained in 345/733 patients (47 %). A total of 58 % of hospitalized patients had TH. Finally, 974 patients died in hospital, and 279 were discharged alive. Among in-hospital deaths, 55 % resulted from hemodynamic failure, whereas 43 % followed neurological failure. Among SCD with a resuscitation attempt, survival rate at hospital discharge was 7.5 %, 95 % CI 6.6–8.4 % (22 % of patients admitted alive). Among patients who survived until discharge, 96 % presented favorable neurological outcomes (CPC 1–2).
Baseline characteristics: according to initial rhythm
The population characteristics according to initial rhythm are presented in Table 2. Compared to patients with non-shockable initial rhythm, patients with shockable rhythm were more often male (82 vs. 66 %, P < 0.001), younger, and had more bystander-witnessed SCD (92 vs. 77 %, P < 0.001). Bystander CPR was more common among patients with initial shockable rhythm (57 vs. 41 %, P < 0.001). During in-hospital course, coronary angiography and TH were more applied among patients with shockable rhythm compared with patients with non-shockable rhythm. Finally, survival at discharge was significantly higher among patients with initial shockable rhythm (26 % of SCD with a resuscitation attempt in the shockable group vs. 2 % in the non-shockable group, P < 0.001).
Baseline characteristics: according to application of TH and coronary angiogram
Among 1,332 patients admitted alive, data regarding application of TH and coronary angiogram were available for 1,257 patients (94 %). Of these 1,257 patients, 560 (45 %) received both hypothermia and coronary angiogram, whereas 697 (55 %) received only one or none of these treatments. Characteristics of these patients are reported in Table 3 and Electronic Supplementary Material no. 4. Application of both treatments was associated in the univariate analysis with male sex, younger age, occurrence outside home, bystander CPR, and lower dose of epinephrine.
Prognostic factors
Univariate analysis of pre-hospital prognostic factors is presented in Table 4. Male sex (OR 1.4, 95 % CI 1.1–1.9), bystander CPR (OR 2.7, 95 % CI 2.0–3.6), and initial shockable rhythm (OR 14.3, 95 % CI 10.6–19.3) were positively associated with survival at discharge. By contrast, longer response time (OR 0.93 per minute, 95 % CI 0.90–0.97), ageing (OR 0.97 per year, 95 % CI 0.96–0.97), occurrence of SCD at home (OR 0.18, 95 % CI 0.1–0.2), and epinephrine dose greater than 3 mg (OR 0.06, 95 % CI 0.04–0.1) were inversely associated with survival at discharge.
In multivariate analysis (Table 4), bystander CPR (OR 2.1, 95 % CI 1.5–3.1) and initial shockable rhythm (OR 11.5, 95 % CI 7.6–17.3) remained positively associated with survival at discharge, while ageing (OR 0.97, 95 % CI 0.96–0.98), occurrence of SCD at home (OR 0.4, 95 % CI 0.3–0.6), and epinephrine dose greater than 3 mg (OR 0.05, 95 % CI 0.03–0.08) remained inversely associated with survival at discharge. In multivariate analysis, longer response time remained inversely associated with survival (OR 0.93 per minute, 95 % CI 0.89–0.97, P = 0.002).
When considering in-hospital treatments, application of hypothermia and coronary angiogram was significantly associated with survival at discharge (34 % in both treatment groups vs. 13 %, P < 0.001). Among hospitalized patients, after adjusting for other prognostic factors, coronary angiography was significantly associated with survival (OR 2.4, 95 % CI 1.4–4.0, P = 0.001) whereas TH was not associated with survival (OR 1.1, 95 % CI 0.7–1.7, P = 0.79) (Electronic Supplementary Material no. 2). Figure 2 depicts survival at hospital discharge among patients admitted alive, according to main prognostic factors.
Discussion
In this large, prospective, population-based registry conducted over 2 years in Paris and its suburbs, we reported 6,165 cases of SCD, and 3,816 had a resuscitation attempt. Out of these, 35 % of patients were admitted alive to hospital. Main therapeutics such as coronary angiogram and TH were applied in half of patients reaching hospital. Overall survival at discharge reached 7.5 %, and factors positively associated with survival at discharge were location of the arrest outside home, initial shockable rhythm, younger age, bystander CPR, and low epinephrine dose delivered during resuscitation.
The baseline characteristics of our patients were consistent with previous descriptions of SCD in whom resuscitation was attempted. Patients presenting SCD were predominantly male, in accordance with a higher prevalence of ischemic cardiopathy in men [17, 18]. Most of the cases occurred at home, with a bystander most of the time. Interestingly, we reported a rate of bystander CPR of 45 %, higher than rates previously described of 20–30 % [19–22, 23]. This unexpected higher rate could result from at least two factors. First, educational campaigns have been conducted among the public, improving the rate of bystander CPR. Second, the EMS dispatcher usually advocates for the application of CPR by the caller. In this registry, we reported a mean response time of 9 min, comparable to previous studies [20, 24, 25], which enhances the representativeness of our cohort. The first rhythm recorded was shockable in only 26 % of cases, consistent with rates observed in two previous studies ranging from 24 to 26 % [21, 26]. This rate is in line with previous results reporting decreasing rates of shockable rhythm in favor of non-shockable rhythm (especially pulseless electrical activity) [27]. This evolution could be the consequence of primary and secondary prevention strategies of coronary artery disease, which is the leading cause for SCD in shockable rhythm [28]. We confirmed strong differences in terms of population characteristics (sex, age, bystander) between shockable and non-shockable rhythm.
In this study, we reported data regarding both pre-hospital and hospital care of SCD, a significant contribution compared to available data. During hospitalization, early coronary angiography was performed in only 58 % of cases, although this intervention has been proposed to improve survival after SCD [5, 6, 29]. Several hypotheses may explain this low usage. First, many patients might present hemodynamic instability, preventing transport to the catheterization lab. Second, the benefit of early coronary angiography is not demonstrated in non-shockable rhythms, explaining why several centers do not proceed with early coronary angiogram in these patients. Third, although the proportion of coronary angiogram was high among hospitals with 24/7 interventional cardiology, only 15 of the 20 main hospitals—accounting for 93 % of overall cases of patients admitted alive—offer a 24/7 catheterization laboratory. This may contribute to the relatively low rate of coronary angiogram overall. Finally, some authors suggest that coronary angiography should be performed in selected cases according to the post-resuscitation ECG [30].
Therapeutic hypothermia has been proposed to limit anoxo-ischemic lesions consecutive to cerebral hypoperfusion, in addition to percutaneous intervention [10]. In a recent national survey in France, Orban et al. [11] reported that 92 % of French ICUs performed TH according to guidelines. The much lower rate of TH used in our study (58 %) may be explained by the fact that TH was independently assessed in our study, using medical records, whereas declarative rates were reported in other studies. In multivariate analysis, among patients admitted alive, we reported an association between coronary angiography and survival at discharge, consistent with previous reports [5, 6]. By contrast, TH was not associated with survival. Several explanations can be given for this result. First, TH has been proposed for patients with initial shockable rhythm only, and its efficiency in non-shockable rhythm remains unclear [31]. A contrario, implementing TH in only 70 % of shockable rhythm is debatable, meaning that guidelines are not fully followed. Then, modalities of hypothermia in each center are not detailed, whereas recent papers questioned the optimal timing [32] or targeted temperature [9]. Furthermore, specific modalities of TH remain unclear, and targeted temperature management could provide as much benefit as hypothermia [9]. Moreover, our study could be underpowered to study the effect of this intervention on survival at discharge.
We reported an overall survival rate of SCD of 7.5 %. This rate is consistent with reports by Giraud et al. [33] and Sasson et al. [1]. In spite of public access defibrillation programs, coronary angiography, and TH, survival after SCD remains extremely low, with high mortality in both pre-hospital and hospital settings. As expected, prognosis significantly differed according to initial rhythm, with 26 % of survival at hospital discharge in shockable rhythm, and 2 % in non-shockable rhythm. Interestingly, considering in-hospital mortality, we reported 43 % of deaths resulting from neurological injury, lower than rates previously described (68 % of deaths resulting from neurological cause, according to Laver et al. [34]). However, the population strongly differs in the two studies (in particular, initial rhythm was ventricular tachycardia or ventricular fibrillation in 73 % of cases, and application of hypothermia was not described), limiting possible comparisons. Our results reinforce the crucial nature of initial hemodynamic management, with 55 % of hospital deaths resulting from hemodynamic failure.
We must acknowledge some limitations. First, we deplore missing data; however, rates of missing data were low and acceptable in the setting of emergency care of cardiac arrest. By consequence, we performed multivariate analysis with listwise deletion. Second, determination of the mode of death and neurological status of survivors was dependent on the quality of the medical records. A more systematic autopsy investigation may be useful for patients who died on the field, and the extent to which the in-hospital view biased the overall view is unclear. Third, we acknowledge that the threshold of 3 mg is debatable for epinephrine. However, when considering epinephrine dose as linear in the model, the dose remained inversely associated with survival. Then, we evaluated the rate of bystander CPR without assessment of the quality of CPR; however, our purpose was to evaluate practices in the population as reflected by bystander CPR, whatever its quality. Also, our data are observational, and we cannot draw conclusions about causality regarding prognostic factors. Our results regarding in-hospital treatments reinforce the crucial need for prospective randomized trials, especially to evaluate the effect of TH among non-shockable rhythms [35, 36]. Moreover, we cannot provide specific data regarding the implementation of TH in each hospital, in terms of rates or modalities. Moreover, considering the differences between centers (such as catheterization laboratory availability), we cannot rule out a biased distribution of patients between centers, based on patient characteristics. However, this potential biased distribution had probably little impact on our results. Finally, vital status was not known for some patients at the time of the study; however, overall vital status knowledge reached 98 %, so the impact of missing data on survival rate is minimal. The strengths of our study are our systematic collection of every case of SCD in a given area with a large population, our systematic adjudication process, and systematic follow-up up to hospital discharge.
Conclusion
The survival after SCD remains disappointingly low, around 7 %. Although proposed by international guidelines, hypothermia and early coronary angiogram intervention are applied in only half of the patients. During the in-hospital course of treatment, causes of death are almost equally distributed between neurological and hemodynamic failure. Initial shockable rhythm, younger age, occurrence outside home, and low epinephrine dose are associated with survival at discharge. These findings suggest ways to improve patients’ care, both in the pre-hospital and in the hospital settings.
References
Sasson C, Rogers MAM, Dahl J, Kellermann AL (2010) Predictors of survival from out-of-hospital cardiac arrest: a systematic review and meta-analysis. Circ Cardiovasc Qual Outcomes 3(1):63–81
Ornato JP, Becker LB, Weisfeldt ML, Wright BA (2010) Cardiac arrest and resuscitation: an opportunity to align research prioritization and public health need. Circulation 122(18):1876–1879
Adnet F, Lapostolle F (2004) International EMS systems: France. Resuscitation 63(1):7–9
Stiell IG, Wells GA, Field B et al (2004) Advanced cardiac life support in out-of-hospital cardiac arrest. N Engl J Med 351(7):647–656
Spaulding CM, Joly LM, Rosenberg A et al (1997) Immediate coronary angiography in survivors of out-of-hospital cardiac arrest. N Engl J Med 336(23):1629–1633
Dumas F, Cariou A, Manzo-Silberman S et al (2010) Immediate percutaneous coronary intervention is associated with better survival after out-of-hospital cardiac arrest: clinical perspective insights from the PROCAT (Parisian region out of hospital cardiac arrest) registry. Circ Cardiovasc Interv 3(3):200–207
Bernard SA, Gray TW, Buist MD et al (2002) Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. N Engl J Med 346(8):557–563
Hypothermia after Cardiac Arrest Study group (2002) Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N Engl J Med 346(8):549–556
Nielsen N, Wetterslev J, Cronberg T et al (2013) Targeted temperature management at 33 versus 36 °C after cardiac arrest. N Engl J Med 369(23):2197–2206
Deakin CD, Nolan JP, Soar J et al (2010) European Resuscitation Council guidelines for resuscitation 2010 section 4. Adult advanced life support. Resuscitation 81(10):1305–1352
Orban J-C, Cattet F, Lefrant J-Y et al (2012) The practice of therapeutic hypothermia after cardiac arrest in France: a national survey. PLoS One 7(9):e45284
Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2007) Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ 335(7624):806–808
Gueugniaud P-Y, David J-S, Chanzy E et al (2008) Vasopressin and epinephrine vs. epinephrine alone in cardiopulmonary resuscitation. N Engl J Med 359(1):21–30
Fishman GI, Chugh SS, Dimarco JP et al (2010) Sudden cardiac death prediction and prevention: report from a National Heart, Lung, and Blood Institute and Heart Rhythm Society Workshop. Circulation 122(22):2335–2348
Jacobs I, Nadkarni V, Bahr J et al (2004) Cardiac arrest and cardiopulmonary resuscitation outcome reports: update and simplification of the Utstein templates for resuscitation registries: a statement for healthcare professionals from a task force of the International Liaison Committee on Resuscitation (American Heart Association, European Resuscitation Council, Australian Resuscitation Council, New Zealand Resuscitation Council, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Councils of Southern Africa). Circulation 110(21):3385–3397
Jennett B, Bond M (1975) Assessment of outcome after severe brain damage. Lancet 1(7905):480–484
Zipes DP, Camm AJ, Borggrefe M et al (2006) ACC/AHA/ESC 2006 guidelines for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: a report of the American College of Cardiology/American Heart Association Task Force and the European Society of Cardiology Committee for Practice Guidelines (writing committee to develop guidelines for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation 114(10):e385–e484
Mahapatra S, Bunch TJ, White RD, Hodge DO, Packer DL (2005) Sex differences in outcome after ventricular fibrillation in out-of-hospital cardiac arrest. Resuscitation 65(2):197–202
Jost D, Degrange H, Verret C et al (2010) DEFI 2005: a randomized controlled trial of the effect of automated external defibrillator cardiopulmonary resuscitation protocol on outcome from out-of-hospital cardiac arrest. Circulation 121(14):1614–1622
Margey R, Browne L, Murphy E et al (2011) The Dublin cardiac arrest registry: temporal improvement in survival from out-of-hospital cardiac arrest reflects improved pre-hospital emergency care. Europace 13(8):1157–1165
McNally B, Robb R, Mehta M et al (2011) Out-of-hospital cardiac arrest surveillance—cardiac arrest registry to enhance survival (CARES), United States, October 1, 2005–December 31, 2010. MMWR Surveill Summ 60(8):1–19
Morrison LJ, Visentin LM, Kiss A et al (2006) Validation of a rule for termination of resuscitation in out-of-hospital cardiac arrest. N Engl J Med 355(5):478–487
Marijon E, Bougouin W, Celermajer DS et al (2013) Major regional disparities in outcomes after sudden cardiac arrest during sports. Eur Heart J 34(47):3632–3640
Gräsner J-T, Meybohm P, Lefering R et al (2011) ROSC after cardiac arrest–the RACA score to predict outcome after out-of-hospital cardiac arrest. Eur Heart J 32(13):1649–1656
Dumas F, Rea TD, Fahrenbruch C et al (2013) Chest compression alone cardiopulmonary resuscitation is associated with better long-term survival compared with standard cardiopulmonary resuscitation. Circulation 127(4):435–441
Weisfeldt ML, Everson-Stewart S, Sitlani C et al (2011) Ventricular tachyarrhythmias after cardiac arrest in public versus at home. N Engl J Med 364(4):313–321
Cobb LA, Fahrenbruch CE, Olsufka M, Copass MK (2002) Changing incidence of out-of-hospital ventricular fibrillation, 1980-2000. J Am Med Assoc 288(23):3008–3013
Bunch TJ, White RD (2005) Trends in treated ventricular fibrillation in out-of-hospital cardiac arrest: ischemic compared to non-ischemic heart disease. Resuscitation 67(1):51–54
Larsen JM, Ravkilde J (2012) Acute coronary angiography in patients resuscitated from out-of-hospital cardiac arrest–a systematic review and meta-analysis. Resuscitation 83(12):1427–1433
Sideris G, Voicu S, Dillinger JG et al (2011) Value of post-resuscitation electrocardiogram in the diagnosis of acute myocardial infarction in out-of-hospital cardiac arrest patients. Resuscitation 82(9):1148–1153
Dumas F, Grimaldi D, Zuber B et al (2011) Is hypothermia after cardiac arrest effective in both shockable and nonshockable patients? Insights from a large registry. Circulation 123(8):877–886
Kim F, Nichol G, Maynard C et al (2014) Effect of prehospital induction of mild hypothermia on survival and neurological status among adults with cardiac arrest: a randomized clinical trial. J Am Med Assoc 311(1):45–52
Giraud F, Rascle C, Guignand M (1996) Out-of-hospital cardiac arrest. Evaluation of 1 year of activity in Saint-Etienne’s emergency medical system using the Utstein style. Resuscitation 33(1):19–27
Laver S, Farrow C, Turner D, Nolan J (2004) Mode of death after admission to an intensive care unit following cardiac arrest. Intensive Care Med 30(11):2126–2128
Vaahersalo J, Hiltunen P, Tiainen M et al (2013) Therapeutic hypothermia after out-of-hospital cardiac arrest in Finnish intensive care units: the FINNRESUSCI study. Intensive Care Med 39(5):826–837
Deye N, Arrich J, Cariou A (2013) To cool or not to cool non-shockable cardiac arrest patients: it is time for randomized controlled trials. Intensive Care Med 39(5):966–969
Conflicts of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Take-home message: Despite being conducted in the therapeutic hypothermia and early coronary angiogram era, hospital discharge survival rate of resuscitated SCD remains poor. The current registry further suggests that increasing bystander CPR, therapeutic hypothermia, and early coronary angiogram coverage may improve short-term prognosis.
On behalf of the Paris—Sudden Death Expertise Center (SDEC)
The SDEC Co-investigators are listed in the Appendix.
A. Cariou and X. Jouven contributed equally.
W. Bougouin and L. Lamhaut contributed equally.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix: SDEC Co-investigators
Appendix: SDEC Co-investigators
J.M. Agostinucci, D. Annane, F. Beganton, W. Bougouin, R. Cador, A. Cariou, P. Carli, C. Cerf, A. Chaib, G. Chironi, B. Clero, Y. Cohen, A. Combes, J.M. Coulaud, V. Das, N. Deye, J.L. Diehl, D. Dreyfuss, O. Dubourg, A. Duguet, F. Dumas, J. Duranteau, F. Fraisse, P. Henry, F. Hidden Lucet, L. Jacob, D. Jost, D. Journois, X. Jouven, L. Lamhaut, V. Lanoe, A. Leenhardt, N. Lellouche, V. Lemiale, T. Loeb, E. Marijon, A. Mekontso-Dessap, B. Misset, X. Monnet, N. Mongardon, B. Mourvillier, M.C. Perier, O. Piot, M. Raux, F. Revaux, B. Riou, F. Santoli, C. Spaulding, O. Varenne, A. Vieillard Baron.
Rights and permissions
About this article
Cite this article
Bougouin, W., Lamhaut, L., Marijon, E. et al. Characteristics and prognosis of sudden cardiac death in Greater Paris. Intensive Care Med 40, 846–854 (2014). https://doi.org/10.1007/s00134-014-3252-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-014-3252-5