Abstract
Purpose
Placing patients with severe acute respiratory distress syndrome (ARDS) in the prone position has been shown to improve survival as compared to the supine position. However, a higher frequency of pressure ulcers has been reported in patients in the prone position. The objective of this study was to verify the impact of prone positioning on pressure ulcers in patients with severe ARDS.
Methods
This was an ancillary study of a prospective multicentre randomised controlled trial in patients with severe ARDS in which the early application of long prone-positioning sessions was compared to supine positioning in terms of mortality. Pressure ulcers were assessed at the time of randomisation, 7 days later and on discharge from the intensive care unit (ICU), using the four-stage Pressure Ulcers Advisory Panel system. The primary end-point was the incidence (with reference to 1,000 days of invasive mechanical ventilation or 1,000 days of ICU stay) of new patients with pressure ulcers at stage 2 or higher from randomisation to ICU discharge.
Results
At randomisation, of the 229 patients allocated to the supine position and the 237 patients allocated to the prone position, the number of patients with pressure ulcers was not significantly different between groups. The incidence of new patients with pressure ulcers from randomisation to ICU discharge was 20.80 and 14.26/1,000 days of invasive mechanical ventilation (P = 0.061) and 13.92 and 7.72/1,000 of ICU days (P = 0.002) in the prone and supine groups, respectively. Position group [odds ratio (OR) 1.5408, P = 0.0653], age >60 years (OR 1.5340, P = 0.0019), female gender (OR 0.5075, P = 0.019), body mass index of >28.4 kg/m2 (OR 1.9804, P = 0.0037), and a Simplified Acute Physiology Score II at inclusion of >46 (OR 1.2765, P = 0.3158) were the covariates independently associated to the acquisition of pressure ulcers.
Conclusion
In patients with severe ARDS, prone positioning was associated with a higher frequency of pressure ulcers than the supine position. Prone positioning improves survival in patients with severe ARDS and, therefore, survivors who received this intervention had a greater likelihood of having pressure ulcers documented as part of their follow-up. There are risk groups for the development of pressure ulcers in severe ARDS, and these patients need surveillance and active prevention.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It has recently been demonstrated in patients with severe acute respiratory distress syndrome (ARDS) that if the patient is kept in the prone position (PP) for long sessions at an early stage of treatment, mortality significantly decreases as compared to patients with severe ARDS kept in the supine position (SP) [1]. This result should encourage healthcare providers to implement this procedure in their ICUs. Indeed, one of the barriers to the routine use of PP for patients with severe ARDS was that the procedure was not associated with any proven benefit in terms of patient outcome, and hence the benefit–risk ratio was no better for the PP than for the SP. In the Proseva study [1], not only was survival higher in the PP group, but there was also no significant difference in airway-related complications between the PP and SP groups. However, it should be noted that several studies have found a higher frequency of pressure ulcers in patients kept for long sessions in the PP [2–6], a finding that was confirmed in a meta-analysis by Sud et al. [7]. Pressure ulcers are a complication of concern in the intensive care unit (ICU) because they are associated with pain, super infections, longer stays and increased costs [8]. Previous studies have only assessed the attack rate of pressure ulcers and, furthermore, they did not take into account confounding factors for pressure ulcers other than positioning, such as the duration of invasive mechanical ventilation and the length of stay in the ICU. The following risk factors for pressure ulcers in ICU patients have been reported: age [9, 10], emergency admission [11], use of norepinephrine [10, 12], cardiovascular comorbidity [10], respiratory comorbidity [11], Sequential Organ Failure Assessment Score (SOFA) [11], length of stay in the ICU, duration of invasive ventilation [9, 10, 13], winter ICU admission [11] and immobilisation [10, 11, 13].
The objective of our study reported was to compare the incidence and severity of pressure ulcers in patients with severe ARDS enrolled in the Proseva trial [1], with the aim of determining, if possible, whether the higher frequency of pressure ulcers in patients allocated to the prone position group was related to body position or to better survival.
Methods
Patients
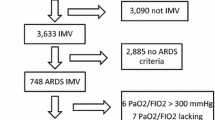
This is an ancillary study of the Proseva trial [1] that focussed on a secondary outcome measure included in the original protocol. In this ancillary trial we enrolled 474 patients with severe ARDS, of whom 466 were analysed (229 in the SP group, 237 in the PP group). Severe ARDS was defined as a PaO2/FIO2 (partial pressure oxygen in arterial blood/fraction of inspired oxygen) ratio of <150 mmHg with a FIO2 of ≥0.6, a positive end-expiratory pressure (PEEP) of ≥5 cm H2O and a tidal volume (VT) of 6 ml/kg predicted body weight. In the PP group, patients were placed in a fully horizontal prone position (180°) within 1 h after the randomisation for sessions of ≥16 consecutive hours until predetermined stopping criteria were met. The patient remained in his/her own bed with no additional support. Participating centres were provided with guidelines so that PP placement, protection using colloid dressings and other pressure ulcer prevention and follow-up measures were standardised as far as possible [14]. The protocol was approved by the ethics committee. The study was performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. Informed consent was obtained from next of kin in every instance.
Data collection
The pressure ulcers were staged according to the National Pressure Ulcer Advisory Panel’s Updated Pressure Ulcer Staging System (NPUAP) [15, 16] at the time of randomisation (day 1), 7 days after randomisation (day 7) and at the time of ICU discharge in both groups. The NPUAP scoring system includes the following four stages: (1) intact skin with non-blanchable erythema; (2) partial thickness loss of dermis; (3) full thickness skin loss; (4) full thickness tissue loss with exposed bone, tendon or muscle. The assessment of the NPUAP score was conducted in real time by the investigator responsible for the study at each centre, together with other data (see below). Furthermore, the data were checked by the research assistant in each centre in real time or 1 day later if the inclusion, day 7 or ICU discharge occurred at the weekend. For confirmation, the nurse’s notes on the chart were used.
The following confounding variables were recorded at day 1: SP or PP group, gender, age, body mass index, trauma, PaO2/FIO2, Simplified Acute Physiology Score (SAPS) II [17], sepsis [18], comorbidities (cardiac, vascular and pulmonary [19]), pneumonia as the main risk factor for ARDS and SOFA score [20]. The number of days each patient in the ICU was administered norepinephrine in a dose of at least 0.1 mg/kg/min was also recorded.
Analysis
The number of patients with at least one pressure ulcer and the number of patients according to pressure ulcer site were measured in each group and expressed as counts and percentage points per group. The pressure ulcer score was computed by taking the NPUAP stage as a continuous variable and therefore using each NPUAP stage (1–4) as a quantitative value.
Grouping variables were: (1) SP versus PP group, which was a controlled variable; (2) presence or absence of pressure ulcers at day 1; (3) presence or absence of patients with new pressure ulcers between day 1 and day 7, or ICU discharge. For grouping variables 2 and 3, we reasoned that the clinical assessment of NPUAP stage 1 was likely to be variable over time and across observers as compared to that of the other three stages. Therefore, two distinct analyses were conducted: firstly on all pressure ulcers regardless of NPUAP stage and, secondly, on pressure ulcers at stage 2 or higher.
The primary end-point was the incidence of new patients with pressure ulcers at stage 2 or higher from day 1 to ICU discharge. The secondary end-points were the incidence of new patients with pressure ulcers from day 1 to day 7, the incidence of new pressure ulcers from day 1 to day 7 and to ICU discharge, the proportion of patients with pressure ulcers both overall and according to site at day 7 and ICU discharge and mean pressure ulcer score overall and by site.
The incidence of new pressure ulcers was computed as the number of new pressure ulcers divided by 1,000 days of invasive mechanical ventilation or by 1,000 days of ICU stay in each group. The incidence of new patients with pressure ulcers was computed as the number of new patients with pressure ulcers divided by 1,000 days of invasive mechanical ventilation or by 1,000 days of ICU stay in each group.
The comparison between groups was performed using parametric and non-parametric tests as fitting. The comparison of incidence between groups was performed using the Z score. A logistic regression analysis was performed to adjust the primary end-point with the confounding factors found to be statistically significant in the univariate analysis. In order to more clearly identify the subgroups at risk when pertaining to discrete covariates, these were collapsed into two groups, i.e. equal to or greater than the median value and lower than the median value. This additional analysis was performed for the following two reasons: (1) to explore whether the higher frequency of pressure ulcer resulted from either a direct effect of the prone position or was an indirect effect of prolonged survival in the prone position group; (2) to select those patients at higher risk for pressure ulcer who should receive preventive measures once the clinician has chosen to use prone positioning. The statistical analysis was carried out using SPSS software ver. 17.0 (http://www-01.ibm.com/software/fr/analytics/spss/products/statistics/). The P value of <0.05 was taken as the statistical significant threshold.
Results
Proportion of patients with pressure ulcers
Data on pressure ulcers at the time of randomisation were missing for four patients in the SP group and for one patient in the PP group. More data were missing at day 7, as some patients had either died or been discharged. At ICU discharge, data were missing for two patients in the SP group and for three patients in the PP group.
At day 1, the number of patients with pressure ulcers, overall and by site, was not significantly different between the two groups [Electronic Supplementary Material (ESM) Table 1]. The mean overall pressure ulcer score was 0.4 ± 1.1 and 0.4 ± 1.0 in the SP and the PP groups, respectively (P = 0.980). At day 7, the rate of patients with pressure ulcers was significantly higher in the PP group than in the SP group (Table 1). As expected, the rate of pressure ulcers involving the face and the anterior part of the thorax was significantly higher in patients in the PP group than in those in the SP group (Table 1). Compared to the SP group, the pressure ulcer score in the PP group was significantly higher for the face, thorax and other sites, and the opposite was true for the score for the back sites (Table 2).
At the time of ICU discharge, the rate of patients with pressure ulcers was no longer different between groups. The rate of pressure ulcers involving the face and the anterior part of the thorax was significantly higher in patients in the PP group than in those in the SP group, and the rate of pressure ulcers on the back and the back of the head was significantly higher in the SP group than in the PP group (Table 1). The overall score was not significantly different between the two groups due to the higher scores for the face, thorax and other sites in the PP group being balanced out by lower scores for the back, sacrum, and back of the head sites also in the PP group compared to the SP group (Table 2).
Incidence of pressure ulcers
The incidence of new patients with pressure ulcers per 1,000 days of invasive ventilation from day 1 to ICU discharge was not significantly different between the two groups for the pressure ulcers at stages 1–4 or at stages >1 (Fig. 1, bar chart top left). However, the incidence of new patients with pressure ulcers at stages >1 per 1,000 days of ICU stay was significantly higher in the PP group than in the SP group (Fig. 1, bar chart top right). The incidence of new patients with pressure ulcers from day 1 to day 7 was significantly higher in the PP group than in the SP group for both stage analyses and both denominators (Fig. 1, top charts). The findings were similar for the incidence of new pressure ulcers (Fig. 1, bottom charts). In both groups, the incidence of pressure ulcers was higher from day 1 to day 7 than during the stay as a whole.
Incidence of new patients with pressure ulcers (PU) (top) and of new PUs (bottom) from randomisation (D1) to 7 days after randomisation (D7) and from day 1 to ICU discharge (discharge) in the supine position (SP; grey bars) and the prone position (PP; black bars) groups expressed per 1,000 days of mechanical ventilation (left) or per 1,000 of days in the intensive care unit (ICU) (right). *P < 0.05, **P < 0.01, † P < 0.001 as compared to the PP group. Two analyses were done: one for the four PU stages (all PU) and one restricted to PU stages 2–4 (PU >1)
Risk factors for pressure ulcers
Age and SOFA score were significantly higher at the time of randomisation in patients with pressure ulcers than in those without at all stages (ESM Table 2). For patients with pressure ulcers at stages 1–4, SAPS II was significantly higher and sepsis was significantly more frequent in patients with pressure ulcers. This difference was not observed for the ulcers at all stages.
Age was significantly higher and female gender was more frequent in patients with pressure ulcers acquired between randomisation and ICU discharge compared to those without, regardless of the stage analysis used (Table 3). Body mass index and SAPS II at inclusion were significantly higher in patients with pressure ulcers, but only for pressure ulcer stage >1.
Therefore, these confounding variables were used in the regression analysis together with the patient position group. The results of the regression analysis pertaining to the risk factors for new patients with a pressure ulcer of stage >1 at the time of ICU discharge are shown in Table 4. Male gender, age ≥60 years and body mass index ≤28.4 kg m2 were significant risk factors.
Discussion
The main findings of our study are: (1) patients in the PP group had a higher frequency of pressure ulcers acquired during their ICU stay; (2) the effect of PP group was no longer significant after controlling for confounders. Although length of stay in the ICU is a commonly accepted risk factor for pressure ulcers, the incidence of patients with pressure ulcers acquired per 1,000 days of ICU stay is not available in most studies on pressure ulcers. The incidence of pressure ulcers found in the Proseva trial [1] (15.5 per 1,000 ICU days) is higher than that measured by Manzano in 2010 [9], which amounted to 14.3 per 1,000 ICU days. This difference could be due to the fact that the Proseva trial included patients with more baseline risk factors, such as higher PaO2/FIO2 ratio or SOFA score. The strict inclusion criteria for the Proseva study prevent further comparison with the other studies. The incidence of pressure ulcers acquired per 1,000 days of ICU stay in the Proseva trial (23.1) is lower than that measured in our first trial [21]. In the latter study the incidence for pressure ulcers was as high as 33.3 per 1,000 ICU days, but it should be noted that pressure ulcers were not assessed in the same way in this study as in the other two studies. In the Proseva trial a lower incidence was found for both the PP and the SP groups than in our previous trial, but the reduction was greater in the latter than in the former. The global comparison performed on the incidence does not take into account two important points. The first is that the risk for pressure ulcer is not constant during the whole ICU stay as the first week of ICU stay is associated with a higher risk. The second is that the comparison between PP and SP groups is biased by the prolonged survival of the patients in the PP group, who are consequently exposed for a longer period to the risk for subsequent pressure ulcer.
The relative risk ratio of pressure ulcer acquisition between the SP and PP groups computed from the global incidence rate is available in a relatively large number of studies. In the Proseva trial [1] it was equal to 1.41 (38.4 % for the PP group, 27.1 % for the SP group). This risk ratio is similar to that calculated in the meta-analysis of different trials by Sud et al. [7] (1.36) and that found in Gattinoni’s study (1.31) [2], and it is slightly higher than that reported in our previous trial (1.22) [21]. The difference could be explained by longer PP sessions, inclusion of more severe patients, and, as discussed above, prolonged survival in the Proseva trial. The overall conclusion that can be drawn from these considerations is that prone positioning generates pressure ulcers at a steady rate. This has important implications in terms of preventive measures because the results of the Proseva trial are likely to change practices, and hence more patients may well be exposed to the risk of pressure ulcers. Therefore, healthcare providers working in the ICU should not only implement the prone positioning technique but also the associated preventive measures for pressure ulcers.
In the present study we found that the body mass index, male gender and age were significant covariates for the risk of pressure ulcers during the stay in the ICU. This finding is important because it helps to identify those patients who require preventive measures. Therefore, male patients aged ≥60 years and with a body mass index of at least 28.4 kg m2 should be given much more attention in terms of pressure ulcer prevention. Furthermore, the results of the present study did not confirm the impact of previously identified risk factors for pressure ulcers, such as the use of vasopressors, winter admissions, SOFA score, respiratory and cardiovascular comorbidities. We have no clear explanation for this.
The considerations discussed above have some limitations. The studies investigating PP were conducted over a long period of time, between 2000 and 2012. During this period, practices may well have changed in line with the prevention policy implemented in the ICUs, and new preventive devices have been developed. Furthermore, it is highly likely that the practice of positioning is different across the ICUs, and due to the relative small number of patients included in each ICU this factor is difficult to analyse. Prevention guidelines were distributed to ICUs participating in the Proseva trial, but compliance with the measures was not assessed during the study, and the support was not standardised [22]. However, investigators in each centre used the own support of the patient and no specific bed was employed during the trial. It should be acknowledged that the incidence of pressure ulcers was not the primary end-point of the study. A more relevant analysis would have been a Cox proportional hazard model, but the date of occurrence of pressure ulcers was not included in the protocol. Finally, the present results were obtained from a randomised controlled trial with several non-inclusion criteria. Therefore, the present results are only valid for the population enrolled, at least theoretically.
In conclusion, in patients with severe ARDS, prone positioning, partly because it markedly prolonged patients’ survival, was associated with a higher risk of pressure ulcers than the supine position. This means that preventive measures should be implemented when the decision to place the patient in the prone position is made. Further trials should be carried out to test these preventive measures.
References
Guerin C, Reignier J, Richard JC, Beuret P, Gacouin A, Boulain T, Mercier E, Badet M, Mercat A, Baudin O, Clavel M, Chatellier D, Jaber S, Rosselli S, Mancebo J, Sirodot M, Hilbert G, Bengler C, Richecoeur J, Gainnier M, Bayle F, Bourdin G, Leray V, Girard R, Baboi L, Ayzac L, Group PS (2013) Prone positioning in severe acute respiratory distress syndrome. N Engl J Med 368:2159–2168
Gattinoni L, Tognoni G, Pesenti A, Taccone P, Mascheroni D, Labarta V, Malacrida R, Di Giulio P, Fumagalli R, Pelosi P, Brazzi L, Latini R (2001) Effect of prone positioning on the survival of patients with acute respiratory failure. N Engl J Med 345:568–573
Beuret P, Carton MJ, Nourdine K, Kaaki M, Tramoni G, Ducreux JC (2002) Prone position as prevention of lung injury in comatose patients: a prospective, randomized, controlled study. Intensive Care Med 28:564–569
Curley MA, Hibberd PL, Fineman LD, Wypij D, Shih MC, Thompson JE, Grant MJ, Barr FE, Cvijanovich NZ, Sorce L, Luckett PM, Matthay MA, Arnold JH (2005) Effect of prone positioning on clinical outcomes in children with acute lung injury: a randomized controlled trial. JAMA 294:229–237
Voggenreiter G, Aufmkolk M, Stiletto RJ, Baacke MG, Waydhas C, Ose C, Bock E, Gotzen L, Obertacke U, Nast-Kolb D (2005) Prone positioning improves oxygenation in post-traumatic lung injury–a prospective randomized trial. J Trauma 59:333–341 (discussion 341–333)
Chan MC, Hsu JY, Liu HH, Lee YL, Pong SC, Chang LY, Kuo BI, Wu CL (2007) Effects of prone position on inflammatory markers in patients with ARDS due to community-acquired pneumonia. J Formos Med Assoc 106:708–716
Sud S, Sud M, Friedrich JO, Adhikari NK (2008) Effect of mechanical ventilation in the prone position on clinical outcomes in patients with acute hypoxemic respiratory failure: a systematic review and meta-analysis. CMAJ 178:1153–1161
Allman RM, Goode PS, Burst N, Bartolucci AA, Thomas DR (1999) Pressure ulcers, hospital complications, and disease severity: impact on hospital costs and length of stay. Adv Wound Care 12:22–30
Manzano F, Navarro MJ, Roldan D, Moral MA, Leyva I, Guerrero C, Sanchez MA, Colmenero M, Fernandez-Mondejar E, Granada UPPG (2010) Pressure ulcer incidence and risk factors in ventilated intensive care patients. J Crit Care 25:469–476
Cox J (2011) Predictors of pressure ulcers in adult critical care patients. Am J Crit Care 20:364–375
Kaitani T, Tokunaga K, Matsui N, Sanada H (2010) Risk factors related to the development of pressure ulcers in the critical care setting. J Clin Nurs 19:414–421
Cox J (2013) Pressure ulcer development and vasopressor agents in adult critical care patients: a literature review. Ostomy Wound Manage 59(50–54):56–60
Sayar S, Turgut S, Dogan H, Ekici A, Yurtsever S, Demirkan F, Doruk N, Tasdelen B (2009) Incidence of pressure ulcers in intensive care unit patients at risk according to the Waterlow scale and factors influencing the development of pressure ulcers. J Clin Nurs 18:765–774
Bergquist-Beringer S, Dong L, He J, Dunton N (2013) Pressure ulcers and prevention among acute care hospitals in the United States. Jt Comm J Qual Patient Saf 39:404–414
Shea JD (1975) Pressure sores: classification and management. Clin Orthop Relat Res (122):89–100
Black J, Baharestani MM, Cuddigan J, Dorner B, Edsberg L, Langemo D, Posthauer ME, Ratliff C, Taler G, (NPUAP) aTNPUAP (2007) National pressure ulcer advisory panel’s updated pressure ulcer staging system. Dermatol Nurs 19:343
Le Gall JR, Lemeshow S, Saulnier F (1993) A new simplified acute physiology score (SAPS II) based on a European/North American multicenter study. JAMA 270:2957–2963
Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, Knaus WA, Schein RM, Sibbald WJ (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 101:1644–1655
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Vincent JL, Moreno R, Takala J, Willatts S, De Mendonca A, Bruining H, Reinhart CK, Suter PM, Thijs LG (1996) The SOFA (sepsis-related organ failure assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 22:707–710
Guerin C, Gaillard S, Lemasson S, Ayzac L, Girard R, Beuret P, Palmier B, Le QV, Sirodot M, Rosselli S, Cadiergue V, Sainty JM, Barbe P, Combourieu E, Debatty D, Rouffineau J, Ezingeard E, Millet O, Guelon D, Rodriguez L, Martin O, Renault A, Sibille JP, Kaidomar M (2004) Effects of systematic prone positioning in hypoxemic acute respiratory failure: a randomized controlled trial. JAMA 292:2379–2387
McInnes E, Jammali-Blasi A, Bell-Syer SE, Dumville JC, Cullum N (2011) Support surfaces for pressure ulcer prevention. Cochrane Database Syst Rev (4):CD001735
Conflicts of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Take-home message: In patients with severe ARDS, prone positioning was associated with a higher risk of pressure ulcers than the supine position. This means preventive measures should be implemented when the decision to use prone positioning is made.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Girard, R., Baboi, L., Ayzac, L. et al. The impact of patient positioning on pressure ulcers in patients with severe ARDS: results from a multicentre randomised controlled trial on prone positioning. Intensive Care Med 40, 397–403 (2014). https://doi.org/10.1007/s00134-013-3188-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-013-3188-1