Abstract
Aims/hypothesis
The gut hormone glucagon-like peptide-1 (GLP-1) decreases beta cell apoptosis in a protein kinase B (PKB)-dependent fashion, and increases islet cell mass and function in vivo. In contrast, cytokines induce beta cell apoptosis, leading to decreased islet mass and type 1 diabetes. In the present study we used rat INS-1E beta cells and primary rat islet cells to examine the potential role of PKB as a mediator of the effect of GLP-1 on cytokine-induced apoptosis.
Methods
Cell viability was determined by MTT assay, and apoptosis and necrosis by Hoechst 33342-propidium iodide staining. Immunoblot analysis was used to detect changes in protein expression, including active (phosphorylated) and total PKB, phosphorylated and total glycogen synthase kinase-3β, activated caspase-3 and inducible nitric oxide synthase. Reactive oxygen species were determined by 1,7-dichlorofluorescein (DCF) analysis, and mutant forms of PKB were introduced into cells using adenoviral vectors.
Results
Incubation of INS-1E cells with cytokines (IL-1β, TNF-α and interferon-γ; 10–50 ng/ml) for 18 h significantly decreased cell viability (by 44%, p<0.001), cell proliferation (by 80%, p<0.001), and activation of PKB (by 67%, p<0.001). Pre-treatment with exendin-4 (10−7 mol/l), a long-acting GLP-1 receptor agonist, partially protected the cells against cytokine-induced toxicity (p<0.01) in association with a reduction in cytokine-induced inhibition of PKB phosphorylation (p<0.05). Exendin-4 pre-treatment did not change cell proliferation. Cytokine treatment increased apoptosis (by 156%, p<0.05) and necrosis (from undetectable to 2.6% of cells). These increases were both reduced by pre-treatment with exendin-4 (p<0.05–0.01). Furthermore, cytokine-induced apoptosis and necrosis were significantly increased in cells infected with kinase-dead PKB (p<0.05), and the protective effect of exendin-4 on both parameters was fully abolished in these cells. Similar changes were observed in primary islet cells. In parallel with these changes, exendin-4 decreased the cytokine-induced activation of caspase-3 (by 46%, p<0.05), and decreased levels of inducible nitric oxide synthase (by 71%, p<0.05) and reactive oxygen species (by 27%, p<0.05).
Conclusions/interpretation
The results of our study indicate that GLP-1 plays a protective role against cytokine-induced apoptosis and necrosis in beta cells through a PKB-dependent signalling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 1 diabetes is characterised by the progressive destruction of pancreatic beta cells following lymphocytic infiltration of the islet, resulting in insulin deficiency. IL-1β, TNF-α and IFN-γ are released by T cells and macrophages during this autoimmune response and are important mediators of beta cell destruction [1]. IL-1β, especially in combination with TNF-α and IFN-γ, induces the formation of high levels of nitric oxide and reactive oxygen species (ROS), leading to the reduced generation of ATP and decreased beta cell function and viability [1, 2]. Moreover, cytokines have been shown to induce beta cell death via a mechanism that involves apoptosis and necrosis [3]. Inflammatory mediators are also increasingly implicated in the development of type 2 diabetes [4]. Consistent with this concept, lipid-laden islets isolated from obese Zucker diabetic fatty (ZDF) rats, a model of type 2 diabetes, are more susceptible to cytokine-mediated cytotoxicity than islets from lean ZDF rats [5]. Similarly, islets that are chronically exposed to high levels of fatty acids demonstrate increased apoptosis in response to cytokines compared with islets cultured in the absence of fat [6].
The incretin hormone glucagon-like peptide-1 (GLP-1) is a 30-amino acid peptide that is secreted from the intestinal L cells in response to nutrient ingestion [7, 8]. This peptide and its long-acting receptor agonist, exendin-4 [9], possess a variety of actions that are protective against diabetes and that are mediated at the level of the beta cell, as well as in peripheral tissues. These include stimulation of glucose-dependent insulin secretion [10, 11], and inhibition of glucagon release [11, 12], gastric emptying [12, 13] and food intake [14, 15]. Recent data show that the actions of GLP-1 that protect against diabetes also include the enhancement of beta cell mass in rodents, through inhibition of beta cell apoptosis, and stimulation of beta cell proliferation and islet neogenesis [16–19]. Furthermore, GLP-1 and its agonists increase the survival of immortalised rodent beta cell lines when challenged with various apoptotic stimulators, including hydrogen peroxide, fatty acids, streptozotocin and staurosporine [17, 20–22]. Importantly, exendin-4 treatment also reduces cytokine-induced apoptosis in purified rat beta cells [17]. However, the signalling pathways that mediate these anti-apoptotic actions of GLP-1 are incompletely understood.
Protein kinase B (PKB), also known as Akt, is a serine–threonine kinase that is activated by phosphatidylinositol-3-kinase (PI3-K). In mammals, three closely related isoforms of PKB are encoded by distinct genetic loci: PKBα/Akt1, PKBβ/Akt2 and PKBγ/Akt3 [23]. The pancreatic beta cell contains high levels of PKBα [24], and the targeted overexpression of PKBα in vivo enhances beta cell mass and function through effects on cell number and cell size [25, 26]. Indeed, PKB is increasingly implicated as a key player in the regulation of beta cell growth and survival [27]. Furthermore, GLP-1 has been demonstrated to increase PKB levels in beta cells, both in vivo in db/db mice and in vitro in INS-1 cells [19, 22, 28]. We have recently demonstrated that the adenovirus-mediated ablation of PKB abrogates the effect of GLP-1 in the prevention of staurosporine-induced apoptosis in INS-1 cells [22]. These findings suggest an important role for PKB as a mediator of the anti-apoptotic actions of GLP-1 in the beta cell. Using rat INS-1E beta cells and primary rat islet cells as models, the aim of the present study was to examine the role of the pro-survival signalling protein PKB as a possible mediator of the protective effects of GLP-1 against cytokine-induced apoptosis and necrosis.
Materials and methods
Cell culture
INS-1E cells (passage number 50–70; a kind gift from C. Wollheim, Department of Internal Medicine, University Medical Centre, Geneva, Switzerland) were grown in monolayer culture in RPMI-1640 medium (Gibco Invitrogen, Burlington, ON, Canada) supplemented with 10 mmol/l HEPES, 10% heat-inactivated FCS, 2 mmol/l l-glutamine, 1 mmol/l sodium pyruvate, 50 μmol/l 2-mercaptoethanol, 100 IU/ml penicillin, and 100 μg/ml streptomycin. Cells were cultured at 37°C in a humidified (5% CO2, 95% air) atmosphere [29].
Islets of Langerhans were isolated from male Wistar rats (weight 200–300 g) by collagenase digestion and dispersed into single cells with trypsin, as described previously [30]. Cells were plated on 12-well plates in RPMI medium supplemented with 11 mmol/l glucose, 0.25% HEPES, 10% FCS, 100 U/ml penicillin, 100 mg/ml streptomycin, and were cultured for 1 day prior to adenovirus infection.
Cell proliferation assay
INS-1E cells were grown to 80–85% confluence in 24-well plates, and then treated overnight with or without exendin-4 (10 nmol/l; Bachem California, Torrance, CA, USA) in the presence of 11 mmol/l glucose. DNA synthesis was measured by 3H-thymidine incorporation assay, as previously described [22].
MTT assay
Cell viability was measured by MTT [3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide] assay [31]. In brief, 50,000 cells were seeded in flat-bottomed, 96-well tissue culture dishes for 24 h; the cells were then pre-incubated with or without 10 nmol/l exendin-4 for 18 h, followed by incubation with a mixture of cytokines (10 ng/ml IL-1β, 50 ng/ml TNF-α, 50 ng/ml IFN-γ; Sigma Chemical Company, St Louis, MO, USA) in the absence or presence of 10 nmol/l exendin-4 for a further 18 h. This incubation time was based on the results of preliminary experiments (in which t=6, 12 or 18 h) showing that incubation for 18 h induced significant apoptosis under the culture conditions used (data not shown). The medium was subsequently removed, 200 μl of MTT (Sigma Chemical Company) was added to give a final concentration of 0.5 mg/ml, and the plates were incubated for 3 h at 37°C in an atmosphere of 95% O2, 5% CO2. A 150-μl aliquot was then substituted for 100 μl of 2-propanol containing 4 N HCl to solubilise the MTT formazan. The plates were placed on a mechanical shaker for 60 min at room temperature, and the optical density was read at 570 nm (n=16 wells per treatment).
Immunoblotting
Cells were grown in six-well plates to 80–85% confluence and then pre-treated with or without 10 nmol/l exendin-4 for 18 h, followed by incubation with a mixture of cytokines in the absence or presence of exendin-4 for a further 18 h. Cells were subsequently lysed in buffer containing 1% Triton X-100 and a mixture of protease and phosphatase inhibitors, as previously described [19, 22]. Protein content was measured by the Bradford assay (Bio-Rad, Hercules, CA, USA), and protein samples (50 μg) were separated on an 8 or 10% SDS-PAGE gel and electrotransferred onto polyvinylidene difluoride filters (Bio-Rad). The proteins were probed with the following specific primary antibodies: rabbit antibodies directed against phosphorylated Ser473-phosphorylated PKB, total PKB, phosphorylated GSK3β (glycogen synthase kinase 3β), total GSK3, phosphorylated and total CREB (cAMP-response-element-binding protein), cleaved caspase-3 (each at 1:1,000 dilution; New England BioLabs, Mississauga, ON, Canada), iNOS (1:500 dilution; Santa Cruz Biotechnology, Santa Cruz, CA, USA), MnSOD (manganese superoxide dismutase; 1:1,000 dilution; Santa Cruz Biotechnology), catalase (1:1,000 dilution) and β-actin (1:4,000 dilution) (both from Sigma Chemical Company). The immunoreactive bands were then visualised with horseradish peroxidase-conjugated sheep anti-rabbit IgG using an ECL detection system (Amersham Pharmacia Biotech, Baie d’Urfe, QC, Canada), as described previously [19, 22].
Adenovirus vectors and infection
Adenoviral vectors expressing enhanced green fluorescent protein (control), constitutively-active PKBα or kinase-dead PKBα; created using a K179M mutation) have been described in detail previously [32, 33]. Equivalent amounts of purified virus (0.5×107 to 2×107 plaque-forming units per ml) were added to either 80% confluent INS-1E cells or dispersed islet cells for 2–4 h. Cells were then washed and incubated for 16 h in fresh medium [22], followed by treatment with medium (plus or minus exendin-4) and then a mixture of cytokines (plus or minus exendin-4), as described above.
Apoptosis and necrosis detection
Adenovirus-infected cells were incubated overnight in the absence or presence of exendin-4 (10 nmol/l), followed by incubation with a mixture of cytokines for 18 h with or without exendin-4. At the end of the treatment period, cells were double-stained with Hoechst 33342 (10 μg/ml; Sigma Chemical Company) and propidium iodide (1 μg/μl; Sigma Chemical Company) in medium for 30 min at 37°C. Cells were then visualised by fluorescence microscopy using a Carl Zeiss Axioplan Deconvolution Microscope (Carl Zeiss Canada, Don Mills, ON, Canada). This method has been successfully used to quantitate apoptosis and necrosis in INS-1 cells, and in human, rat and mouse beta cells [34–37]. In brief, cells were defined as apoptotic if they exhibited condensed nuclear chromatin or a fragmented nuclear membrane, as visualised with Hoechst 33342. Necrotic cells were characterised by nuclear propidium iodide staining without condensed chromatic or fragmented nuclear membranes. Cells without apoptotic or necrotic features were considered viable. At least 100 cells were counted for each experimental condition.
Determination of ROS by DCF fluorescence
Production of ROS was determined using the oxidation-sensitive fluorescent probe DCFH-DA (5,6-carboxy-2′,7′-dichlorofluorescein-diacetate). DCFH-DA is a cell-permeant dye that is cleaved by intracellular esterases into DCFH, its non-fluorescent, non-permeant form, which may be oxidised by H2O2 or OH− to its fluorescent form, DCF (2′,7′-dichlorofluorescein) [38]. Cells were treated with media (plus or minus exendin-4) and cytokines (plus or minus exendin-4), as above, and washed with PBS; 10 μmol/l DCFH-DA was then added for 20 min and total fluorescence was determined (excitation at 485 nm, emission at 530 nm; n=16 wells per treatment).
Statistical analysis
All data are presented as means±SEM. Statistical analysis was performed using the Student’s t-test or ANOVA using ‘n−1’ custom hypotheses tests, as appropriate. A p value of less than 0.05 was considered significant.
Results
GLP-1 protects INS-1E cells against cytokine-induced cell toxicity and prevents cytokine-mediated suppression of PKB
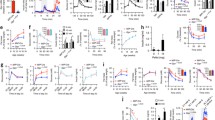
Total cell viability, as assessed by MTT assay, was decreased by 44% (p<0.001) after treatment of INS-1E cells with a mixture of cytokines for 18 h (Fig. 1a). Pre-treatment with exendin-4 reduced cytokine-induced toxicity (by 17%, p<0.01 vs cytokine-treated cells), while exendin-4 alone slightly but significantly (p<0.01) increased viability as compared with medium alone (control). Cell proliferation, as determined by 3H-thymidine incorporation assay, was significantly decreased by cytokine treatment (by 80%, p<0.001), and this decrease was not prevented by pre-incubation with exendin-4 (Fig. 1b). Incubation of INS-1E cells with a mixture of cytokines for 18 h also significantly decreased activation of PKB (by 67%, p<0.001; Fig. 1c), as assessed by immunoblot analysis of phosphorylated PKB. Consistent with the findings for total cell viability, the level of inhibition of phosphorylated PKB induced by cytokine treatment (p<0.001) was reduced by pre-incubation with exendin-4 (by 18%, p<0.05 vs cytokine-treated cells). Consistent with previous results [22], exendin-4 alone increased phosphorylation of PKB (by 36%, p<0.01). For all experiments, the normalised response to exendin-4 was not different between control and cytokine-treated cells.
Effects of exendin-4 on cytokine-induced toxicity, proliferation and PKB phosphorylation in INS-1E cells. INS-1E cells were incubated with (Ex4) or without (control) 10 nmol/l exendin-4 for 18 h, and were then treated with a mixture of cytokines in the absence (cyto) or presence (cyto+Ex4; pretreated with exendin-4) of exendin-4 for 18 h. This was followed by an MTT assay for cell viability (n=3) (a), a 3H-thymidine incorporation assay (n=12) (b), and Western blotting for Ser473-phosphorylated PKB (P-PKB) and total PKB (T-PKB) (c). The results are the means±SEM of five separate experiments. The blot shown is representative of five separate experiments (labels for treatment groups indicate both the associated histogram and the underlying immunoblot). **p<0.01 and ***p<0.001 vs control; # p<0.05 and ## p<0.01 vs cytokine-treated cells
PKB is required for the prevention of cytokine-induced apoptosis by GLP-1
To functionally ablate or overexpress PKB, INS-1E cells were infected with adenoviral vectors expressing kinase-dead PKBα (Adv-KD cells) or constitutively-active PKBα (Adv-CA cells). Cells infected with adenoviral vectors expressing enhanced green fluorescent protein (Adv-GFP cells) served as controls. As observed for uninfected cells (Fig. 1c), incubation of Adv-GFP cells with cytokines significantly decreased activation of PKB (by 31%, p<0.05; Fig. 2a), and exendin-4 treatment partially protected the cells against cytokine-induced inhibition of PKB phosphorylation (p<0.05). Levels of phosphorylated PKB were increased in cells incubated in exendin-4 as compared with cells incubated in medium alone (p<0.05). Basal levels of phosphorylated PKB were reduced by 64% (p<0.01) in Adv-KD cells as compared with Adv-GFP cells, whereas levels of phosphorylated PKB were dramatically increased in Adv-CA cells (by 115%, p<0.01). Infection of INS-1E cells with Adv-CA completely prevented the inhibitory effects of cytokines on PKB phosphorylation, and this prevention was not significantly altered by exendin-4 treatment, although levels of phosphorylated PKB were slightly higher in cells incubated in exendin-4 alone than in cells incubated in medium alone (p<0.05). Conversely, cytokines did not further decrease PKB phosphorylation in Adv-KD cells, but the protective effects of exendin-4 were completely abolished. Identical changes were observed in the levels of phosphorylated GSK3β (Fig. 2b), a downstream target of phosphorylated PKB action, whereas levels of phosphorylated CREB, a potential mediator of GLP-1 action, were not altered (data not shown).
Effects of exendin-4 on levels of phosphorylated and total PKB and phosphorylated and total GSK3β in Adv-GFP, Adv-CA and Adv-KD cells. INS-1E cells were infected with 0.5×107–2×107 plaque-forming units per ml of adenoviral vectors expressing enhanced green fluorescent protein (Adv-GFP cells), constitutively-active PKBα (Adv-CA cells) or kinase-dead PKBα (Adv-KD cells) for 2–4 h, incubated in media alone for 16 h, pre-treated with media alone or 10 nmol exendin-4 for 18 h, and then incubated with combined cytokines in the absence or presence of exendin-4 for a further 18 h. This was followed by Western blotting for Ser473-phosphorylated PKB (P-PKB) and total PKB (T-PKB) (a), and phosphorylated GSK3β (P-GSK3β) and total GSK3 (T-GSK3) (b). Representative blots and the means±SEM for the normalised optical density from five to six separate experiments are shown. The specific adenovirus used for each group is indicated below the histogram, while the respective treatments within each adenoviral group are shown above the immunoblot (open bars, control, media alone; closed bars, exendin-4 alone; hatched bars, cytokines alone; striped bars, cytokines with exendin-4 pre-treatment). *p<0.05 and **p<0.01 vs control Adv-GFP cells; # p<0.05 vs Adv-GFP cells treated with combined cytokines alone, † p<0.05 vs control Adv-CA infected cells
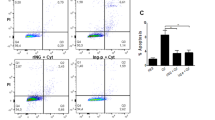
To determine the percentage of INS-1E cells comprised of apoptotic cells under the different treatment conditions, apoptosis was quantified by Hoechst 33342-propidium iodide staining. As observed for total cell viability (Fig. 1a), treatment of the Adv-GFP cells with a mixture of cytokines increased apoptosis (by 156%, p<0.05), and this was reduced by treatment with exendin-4 (by 49%, p<0.05; Fig. 3a). Basal levels of apoptosis were also reduced by exendin-4 treatment alone (by 56%, p<0.05), although this change was not as great as that seen in cytokine-treated cells (p<0.01). Adenovirus-mediated transfer of constitutively active PKB dramatically decreased basal apoptosis (by 56%, p<0.01). As expected from the cell viability study, treatment with cytokines increased apoptosis in the Adv-CA cells (by 185%, p<0.01), and this was decreased (by 37%, p<0.01) by pre-treatment of the cells with exendin-4. In contrast, basal apoptosis was increased by 85% (p<0.01) in Adv-KD cells, and cytokines induced a further increase in apoptosis (56% increase vs cytokine-treated Adv-GFP cells, p<0.05; 112% increase vs control Adv-KD cells, p<0.05). Furthermore, the anti-apoptotic effect of exendin-4 was fully abolished in Adv-KD cells treated with cytokines. Identical changes were observed in primary rat islet cells (Fig. 3b).
Effects of exendin-4 on apoptosis. INS-1E (a) and primary rat islet cells (b) were infected with 0.5×107–2×107 plaque-forming units per ml of adenoviral vectors expressing enhanced green fluorescent protein (Adv-GFP), constitutively-active PKBα (Adv-CA) or kinase-dead PKB (Adv-KD) for 2–4 h, incubated in media alone for 16 h, pre-treated with media alone or 10 nmol exendin-4 for 18 h, and then incubated with combined cytokines in the absence or presence of exendin-4 for a further 18 h. This was followed by assessment of apoptosis by Hoechst 33342 staining (n=3–5 for INS-1E cells, n=4–6 for primary islet cells). The specific adenovirus used for each group is indicated below the histogram (open bars, control, media alone; closed bars, exendin-4 alone; hatched bars, cytokines alone; striped bars, cytokines with exendin-4 pre-treatment). *p<0.05 and **p<0.01 vs control Adv-GFP cells; # p<0.05 and ## p<0.01 vs the same group of cells treated with combined cytokines alone; † p<0.05 and ‡ p<0.01 vs control cells in the same adenovirus group; ^p<0.05 vs cytokine-treated Adv-GFP cells
Activation of caspase-3 was also used as a marker of apoptosis in the INS-1E cells overexpressing constitutively active PKB and kinase-dead PKB. As shown in Fig. 4, the level of activated caspase-3 was significantly increased (by 114%, p<0.05) following the treatment of Adv-GFP cells with a mixture of cytokines for 18 h, and this increase was completely prevented by pre-treatment with exendin-4 (p<0.05). Consistent with the findings for INS-1E cell apoptosis (Fig. 3a), basal levels of activated caspase-3 were enhanced in Adv-KD cells and were decreased in Adv-CA cells, as compared with Adv-GFP controls. Furthermore, following incubation with cytokines, levels of activated caspase-3 were significantly lower (35% decrease, p<0.05) in Adv-CA cells than in Adv-GFP cells. The protective effects of exendin-4 against cytokines were abolished in Adv-KD cells. Taken together, these data suggest an important role for PKB in the prevention of the cytokine-induced apoptosis of beta cells by GLP-1.
Effects of exendin-4 on activated caspase-3 in Adv-GFP, Adv-CA and Adv-KD. INS-1E cells were infected with 0.5×107–2×107 plaque-forming units per ml of adenoviral vectors expressing enhanced green fluorescent protein (Adv-GFP cells), constitutively-active PKBα (Adv-CA cells) or kinase-dead PKBα (Adv-KD cells) for 2–4 h, incubated in media alone for 16 h, pre-treated with media alone or 10 nmol exendin-4 for 18 h, and then incubated with combined cytokines in the absence or presence of exendin-4 for a further 18 h. This was followed by Western blotting for cleaved caspase-3 and β-actin. A representative blot and the means±SEM for the optical density (normalised to β-actin) from six separate experiments are shown. The specific adenovirus used for each group is shown below the histogram, while the respective treatments within each adenoviral group are shown above the immunoblot (open bars, control, media alone; closed bars, exendin-4 alone; hatched bars, cytokines alone; striped bars, cytokines with exendin-4 pre-treatment). *p<0.05 vs control Adv-GFP cells; # p<0.05 vs Adv-GFP cells treated with cytokines alone
PKB is required for the prevention of cytokine-induced necrosis by GLP-1
In addition to apoptosis, Hoechst 34222-propidium iodide staining revealed that the treatment of INS-1E cells with a mixture of cytokines induced necrosis. As shown in Fig. 5a, under control conditions (media alone), necrosis was not detected in either Adv-GFP cells or Adv-CA cells, but was seen in Adv-KD cells. Cytokine treatment induced necrosis in 2.6±0.4% of the Adv-GFP cells; compared with the control cells, cytokine-induced necrosis was significantly decreased in Adv-CA cells (by 90%, p<0.05) and increased in Adv-KD cells (by 23%, p<0.05). Exendin-4 pre-treatment significantly decreased the effects of cytokines (by 90%, p<0.01) in Adv-GFP cells. However, the protective effect of exendin-4 was fully abolished in Adv-CA cells and Adv-KD cells. Similar changes were observed in primary rat islet cells (Fig. 5b).
Effects of exendin-4 on necrosis. INS-1E (a) and primary rat islet cells (b) were infected with 0.5×107–2×107 plaque-forming units per ml of adenoviral vectors expressing enhanced green fluorescent protein (Adv-GFP), constitutively-active PKBα (Adv-CA) or kinase-dead PKB (Adv-KD) for 2–4 h, incubated in media alone for 16 h, pre-treated with media alone or 10 nmol exendin-4 for 18 h, and then incubated with combined cytokines in the absence or presence of exendin-4 for a further 18 h. This was followed by assessment of necrosis by propidium iodide staining (n=3–5 for INS-1E cells, n=4–6 for primary islet cells). The specific adenovirus used for each group is shown below the histogram (open bars, control, media alone; closed bars, exendin-4 alone; hatched bars, cytokines alone; striped bars, cytokines with exendin-4 pre-treatment; some bars are not visible when value=0). # p<0.05 and ## p<0.01 vs Adv-GFP cells treated with cytokines alone; † p<0.05 vs control Adv-KD cells
We investigated levels of iNOS expression and ROS as markers of cell necrosis. As shown in Fig. 6, iNOS expression, which was not detectable under basal conditions, was induced by treatment of Adv-GFP cells with a mixture of cytokines, and exendin-4 pre-treatment decreased this cytokine-induced expression of iNOS (by 71%, p<0.05). The protective effects of exendin-4 were lost in Adv-CA cells and Adv-KD cells. Similarly, cytokine treatment significantly increased ROS levels in INS-1E cells (by 82%, p<0.01; Fig. 7). However, cytokine-stimulated ROS levels were significantly decreased (by 36%, p<0.05) in the presence of exendin-4. The effects of cytokines on the antioxidant enzymes MnSOD and catalase were also studied. Cytokine treatment was found to increase the expression of MnSOD, while catalase levels were decreased by the combined cytokines. Furthermore, exendin-4 pre-treatment did not significantly change the expression of either enzyme in response to cytokine treatment (data not shown).
Effects of exendin-4 on iNOS levels in Adv-GFP, Adv-CA and Adv-KD cells. INS-1E cells were infected with 0.5×107–2×107 plaque-forming units per ml of adenoviral vectors expressing enhanced green fluorescent protein (Adv-GFP cells), constitutively-active PKBα (Adv-CA cells) or kinase-dead PKBα (Adv-KD cells) for 2–4 h, incubated in media alone for 16 h, pre-treated with media alone or 10 nmol exendin-4 for 18 h, and then incubated with combined cytokines in the absence or presence of exendin-4 for a further 18 h. This was followed by Western blotting for iNOS. A representative blot and the means±SEM for the optical density (normalised to β-actin) from four separate experiments are shown. The specific adenovirus used for each group is shown below the histogram, while the respective treatments within each adenoviral group are shown above the immunoblot (open bars, control, media alone; closed bars, exendin-4 alone; hatched bars, cytokines alone; striped bars, cytokines with exendin-4 pre-treatment; some bars are not visible when value=0). # p<0.05 vs Adv-GFP cells treated with cytokines alone
Effects of exendin-4 on ROS levels in INS-1E cells. INS-1E cells were pre-treated with media alone (control) or 10 nmol/l exendin-4 for 18 h, and then treated with cytokines in the absence or presence of exendin-4 for 18 h. This was followed by determination of ROS levels by DCF fluorescence (n=3). **p<0.01 vs control cells; # p<0.05 vs cells treated with cytokines alone
Discussion
The cytotoxic effects of cytokines on beta cells have been widely demonstrated to include apoptosis and necrosis [1–3]. The results of the present study demonstrate that treatment of INS-1E beta cells with exendin-4, a long-acting GLP-1 analogue, can prevent both forms of cytokine-induced beta cell death in INS-1E cells and primary rat islet cells. Although previous studies using isolated rat islets have shown a protective effect of GLP-1 against cytokine-induced apoptosis [17], the present study is the first to demonstrate that GLP-1 has similar effects on the prevention of beta cell necrosis. Furthermore, we have extended these findings by showing that the protective effects of GLP-1 against both forms of cytokine-induced beta cell death require activation of PKB.
Treatment of INS-1E cells with a combination of IL-1β, TNF-α and IFN-γ was found to decrease levels of phosphorylated PKB in parallel with decreased cell viability and increased apoptosis and necrosis. PKB has previously been implicated in the signalling pathways of IL-1β and TNF-α [39, 40]. Consistent with such a mechanism of action, the overexpression of kinase-dead PKB enhanced cytokine-induced apoptosis and necrosis, whereas constitutively-active PKB diminished these effects. Furthermore, non-stimulated levels of apoptosis and necrosis were concomitantly altered in response to modulation of PKB levels, suggesting an important role for PKB under basal conditions and in response to cytotoxic agents.
As reported previously [22], exendin-4 treatment increased basal beta cell viability in parallel with an enhanced activation of PKB. This protective effect of GLP-1 was mediated through the inhibition of apoptosis and necrosis, particularly in the setting of cytokine-induced toxicity. These effects of exendin-4 were completely abolished by ablation of endogenous PKB levels using a kinase-dead construct of PKB; this observation is consistent with an essential role for PKB in the downstream signalling pathways that lead from the GLP-1 receptor to cell growth and survival. Furthermore, exendin-4 treatment was also able to reduce the effects of cytokines on apoptosis in cells infected with constitutively-active PKB, although the protective effects of exendin-4 were not observed in all Adv-CA cells, possibly due to the extremely high levels of activated PKB already present. Nonetheless, in agreement with the finding of an important role for PKB in GLP-1 signalling, it has been shown that inhibition of PI3-K, the upstream regulator of PKB activity [23], decreases the IGF-1-mediated protection of beta cells against cytokines [41, 42]. IGF-1 is a known regulator of PI3-K/PKB, whereas the mechanisms that link the G protein-coupled GLP-1 receptor to cell survival pathways are not well understood. It has been suggested that activation of CREB, a cAMP-dependent transcription factor, may provide a direct link between the GLP-1 receptor and the PI3-K/PKB pathway through the enhanced synthesis of the upstream effector, insulin receptor substrate-2 [43]. Furthermore, cytokines have been reported to inhibit CREB activation [44]. However, in the present study, the levels of phosphorylated and total CREB were not altered by treatment with either exendin-4 or cytokines, suggesting the existence of alternative pathways that link these agents to PKB. The possibility that exendin-4 activates pathways other than those involving PKB cannot be excluded, as the coupling of the GLP-1 receptor to multiple G proteins and to the mitogen-activated protein kinase pathway has previously been reported [45].
Somewhat unexpectedly, the exendin-4-induced changes in apoptosis (50% decrease) were greater than those in cell viability (17% increase). This difference cannot be accounted for by an effect of exendin-4 on proliferation, at least under the conditions used in the present study. Given that no necrosis could be measured in the absence of cytokines and that cell viability is a reflection of all three parameters, it is likely that, in terms of cell viability, the inhibitory effect of exendin-4 on apoptosis was balanced out by the lack of detectable necrosis. Furthermore, as the viability and proliferation studies were conducted in non-infected cells, while the apoptosis and necrosis measurements were made in adenovirus-infected cells, it is likely that the absolute changes in these parameters are not directly comparable.
Caspase-3 is an executioner enzyme that is responsible for the cellular features of apoptosis, including DNA fragmentation, nuclear condensation and plasma membrane remodelling [46]. Consistent with the results of the present study, previous studies have demonstrated that cytokines induce beta cell caspase-3 activity, whereas GLP-1 decreases cycloheximide-induced caspase-3 levels in the beta cell [17]. The effects of cytokines and exendin-4 on caspase-3 were diminished by the overexpression of constitutively active PKB, but were not significantly increased by kinase-dead PKB. Although it has been shown that the protective effects of IGF-1 on the beta cell are mediated through PKB-dependent inhibition of caspase-3 activation [33], studies in hepatocytes have demonstrated the existence of a PKB-independent effect of TNF-α on caspase-3 [47]. Thus, in INS-1E cells, the pro- and anti-apoptotic effects of the cytokines and GLP-1, respectively, may be mediated through both PKB-dependent and PKB-independent signalling pathways.
Little is known about the signalling pathways by which cytokines induce beta cell necrosis, although studies have shown that islet cell necrosis induced by IFN-γ is mediated by nitric oxide [48]. The results of the present study clearly demonstrate a role for PKB in the induction of necrosis by cytokines and in the cytoprotective effects of GLP-1 against cytokine-induced necrosis. In agreement with our results, previous studies have demonstrated that ceramide-induced necrosis is inhibited by the overexpression of PKB [49], while PKB reduces the size of the necrotic zone in ischaemic myocardium [50]. The effects of cytokines on apoptosis and necrosis may be explained by their ability to induce iNOS and, thus, production of the free radical, nitric oxide [36, 48]. The results of the present study demonstrate that cytokine treatment of INS-1E cells induces iNOS in association with increased ROS levels. Although IL-1β, TNF-α and IFN-γ signal through different receptors, the combined cytokines are known to exert synergistic effects through the induction of almost 700 target genes, including that encoding iNOS [36]. Of these genes, nearly 50% are nitric oxide-dependent, indicating an essential role for the iNOS pathway in cytokine-mediated cell toxicity.
Importantly, the stimulatory effects of cytokines on iNOS, and of nitric oxide on apoptosis and necrosis, appear to be cell specific, with pancreatic islets exhibiting a particularly high degree of sensitivity to ROS because of their low levels of antioxidants [51, 52]. Levels of MnSOD were found to be increased by cytokine treatment in the present study; this is thought to be part of a defensive response of the beta cell to oxidative stress [36], and stable expression of MnSOD confers complete protection of INS-1 cells against IL-1β-induced cytotoxicity [53]. However, it must be noted that, in the present study, the cytokine-induced changes in MnSOD appeared to be counterbalanced by a parallel decrease in catalase levels, suggesting that the INS-1E cells remained susceptible to damage by the cytokine-induced enhancement of ROS levels. Furthermore, exendin-4 did not alter the levels of either enzyme, indicating that the effects of this peptide on free radical levels are mediated indirectly, through decreased synthesis rather than through the increased removal of ROS.
Finally, the inhibitory effect of exendin-4 pre-treatment on cytokine-induced iNOS was abolished in Adv-KD cells, suggesting that this effect is PKB dependent. It was therefore somewhat unexpected that lower levels of iNOS were not observed in the Adv-CA cells, as this treatment clearly increased the levels of phosphorylated PKB. However, a trend towards a decrease was observed, and the absence of a statistical change may simply reflect the high variability of levels of this protein. Nonetheless, the changes in iNOS in response to cytokines were paralleled by decreased intracellular levels of ROS. Furthermore, similar studies have shown that the iNOS/nitric oxide-induced apoptosis of INS-1 cells can be prevented by IGF-1, through a PI3-K-dependent pathway [42]. These findings suggest that iNOS may be a target gene for the PKB signalling pathway. This possibility has previously been suggested to involve PKB-induced activation of NFκB, a known regulator of iNOS gene expression [54], although other effector pathways cannot be precluded.
In summary, the results of the present study demonstrate that the protective effects of GLP-1 against cytokine-induced apoptosis and necrosis require activation of PKB. Recent success in islet transplantation has focussed attention on cell-based insulin replacement strategies for the treatment of type 1 diabetes. However, limited tissue supply and concerns regarding the life-long administration of immunosuppressive agents may limit the applicability of this approach [55]. The finding that GLP-1 and PKB protect the beta cell against oxidative stress may lead to novel therapeutic approaches aimed at enhancing the survival of beta cells, thereby reducing or delaying cytokine-mediated beta cell destruction in the development of type 1 and/or type 2 diabetes.
Abbreviations
- CREB:
-
cAMP-response-element-binding protein
- GLP-1:
-
glucagon-like peptide-1
- GSK:
-
glycogen synthase kinase
- iNOS:
-
inducible nitric oxide synthase
- MnSOD:
-
manganese superoxide dismutase
- PI3-K:
-
phosphatidylinositol 3-kinase
- PKB:
-
protein kinase B
- ROS:
-
reactive oxygen species
References
Eizirik DL, Mandrup-Poulsen T (2001) A choice of death—the signal-transduction of immune-mediated beta-cell apoptosis. Diabetologia 44:2115–2133
Mandrup-Poulsen T (1996) The role of interleukin-1 in the pathogenesis of IDDM. Diabetologia 39:1005–1029
Saldeen J (2000) Cytokines induce both necrosis and apoptosis via a common Bcl-2-inhibitable pathway in rat insulin-producing cells. Endocrinology 141:2003–2010
Donath MY, Storling J, Maedler K, Mandrup-Poulsen T (2003) Inflammatory mediators and islet beta-cell failure: a link between type 1 and type 2 diabetes. J Mol Med 81:455–470
Shimabukuro M, Zhou YT, Lee Y, Unger RH (1998) Troglitazone lowers islet fat and restores beta cell function of Zucker diabetic fatty rats. J Biol Chem 273:3547–3550
Shimabukuro M, Koyama K, Lee Y, Unger RH (1997) Leptin- or troglitazone-induced lipopenia protects islets from interleukin 1 beta cytotoxicity. J Clin Invest 100:1750–1754
Brubaker PL, Anini Y (2003) Direct and indirect mechanisms regulating secretion of glucagon-like peptide-1 and glucagon-like peptide-2. Can J Physiol Pharm 81:1005–1012
Drucker DJ (2002) Biological actions and therapeutic potential of the glucagon-like peptides. Gastroenterology 122:531–544
Goke R, Fehmann HC, Linn T et al (1993) Exendin-4 is a high potency agonist and truncated exendin-(9–39)-amide an antagonist at the glucagon-like peptide 1-(7–36)-amide receptor of insulin-secreting beta-cells. J Biol Chem 268:19650–19655
Nauck MA, Wollschlager D, Werner J et al (1996) Effects of subcutaneous glucagon-like peptide 1 (GLP-1 [7–36 amide]) in patients with NIDDM. Diabetologia 39:1546–1553
Ritzel R, Orskov C, Holst JJ, Nauck MA (1995) Pharmacokinetic, insulinotropic, and glucagonostatic properties of GLP-1 [7–36 amide] after subcutaneous injection in healthy volunteers. Dose-response-relationships. Diabetologia 38:720–725
Willms B, Werner J, Holst JJ, Orskov C, Creutzfeldt W, Nauck MA (1996) Gastric emptying, glucose responses, and insulin secretion after a liquid test meal: effects of exogenous glucagon-like peptide-1 (GLP-1)-(7–36) amide in type 2 (noninsulin-dependent) diabetic patients. J Clin Endocrinol Metab 81:327–332
Schirra J, Kuwert P, Wank U et al (1997) Differential effects of subcutaneous GLP-1 on gastric emptying, antroduodenal motility, and pancreatic function in men. Proc Assoc Am Physicians 109:84–9797
Toft-Nielsen MB, Madsbad S, Holst JJ (1999) Continuous subcutaneous infusion of glucagon-like peptide 1 lowers plasma glucose and reduces appetite in type 2 diabetic patients. Diabetes Care 22:1137–1143
Turton MD, O’Shea D, Gunn I et al (1996) A role for glucagon-like peptide-1 in the central regulation of feeding. Nature 379:69–72
Brubaker PL, Drucker DJ (2004) Minireview: glucagon-like peptides regulate cell proliferation and apoptosis in the pancreas, gut, and central nervous system. Endocrinology 145:2653–2659
Li Y, Hansotia T, Yusta B, Ris F, Halban PA, Drucker DJ (2003) Glucagon-like peptide-1 receptor signaling modulates beta cell apoptosis. J Biol Chem 278:471–478
Stoffers DA, Kieffer TJ, Hussain MA et al (2000) Insulinotropic glucagon-like peptide 1 agonists stimulate expression of homeodomain protein IDX-1 and increase islet size in mouse pancreas. Diabetes 49:741–748
Wang Q, Brubaker PL (2002) Glucagon-like peptide-1 treatment delays the onset of diabetes in 8 week-old db/db mice. Diabetologia 45:1263–1273
Hui H, Nourparvar A, Zhao X, Perfetti R (2003) Glucagon-like peptide-1 inhibits apoptosis of insulin-secreting cells via a cyclic 5′-adenosine monophosphate-dependent protein kinase A- and a phosphatidylinositol 3-kinase-dependent pathway. Endocrinology 144:1444–1455
Kwon G, Pappan KL, Marshall CA, Schaffer JE, McDaniel ML (2004) cAMP Dose-dependently prevents palmitate-induced apoptosis by both protein kinase A- and cAMP-guanine nucleotide exchange factor-dependent pathways in beta-cells. J Biol Chem 279:8938–8945
Wang Q, Li L, Xu E, Wong V, Rhodes C, Brubaker PL (2004) Glucagon-like peptide-1 regulates proliferation and apoptosis via activation of protein kinase B in pancreatic INS-1 beta cells. Diabetologia 47:478–487
Scheid MP, Woodgett JR (2001) PKB/AKT: functional insights from genetic models. Nat Rev Mol Cell Biol 2:760–768
Holst LS, Mulder H, Manganiello V et al (1998) Protein kinase B is expressed in pancreatic beta cells and activated upon stimulation with insulin-like growth factor I. Biochem Biophys Res Commun 250:181–186
Bernal-Mizrachi E, Wen W, Stahlhut S, Welling CM, Permutt MA (2001) Islet beta cell expression of constitutively active Akt1/PKB alpha induces striking hypertrophy, hyperplasia, and hyperinsulinemia. J Clin Invest 108:1631–1638
Tuttle RL, Gill NS, Pugh W et al (2001) Regulation of pancreatic beta-cell growth and survival by the serine/threonine protein kinase Akt1/PKBalpha. Nat Med 7:1133–1137
Dickson LM, Rhodes CJ (2004) Pancreatic beta-cell growth and survival in the onset of type 2 diabetes: a role for protein kinase B in the Akt? Am J Physiol Endocrinol Metab 287:E192–E198
Trumper K, Trumper A, Trusheim H et al (2000) Integrative mitogenic role of protein kinase B/Akt in beta-cells. Ann N Y Acad Sci 921:242–250
Asfari M, Janjic D, Meda P, Li G, Halban PA, Wollheim CB (1992) Establishment of 2-mercaptoethanol-dependent differentiated insulin-secreting cell lines. Endocrinology 130:167–178
MacDonald PE, Ha XF, Wang J et al (2001) Members of the Kv1 and Kv2 voltage-dependent K(+) channel families regulate insulin secretion. Mol Endocrinol 15:1423–1435
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65:55–63
Dickson LM, Lingohr MK, McCuaig J et al (2001) Differential activation of protein kinase B and p70(S6)K by glucose and insulin-like growth factor 1 in pancreatic beta-cells (INS-1). J Biol Chem 276:21110–21120
Wrede CE, Dickson LM, Lingohr MK, Briaud I, Rhodes CJ (2002) Protein kinase B/Akt prevents fatty acid-induced apoptosis in pancreatic beta-cells (INS-1). J Biol Chem 277:49676–49684
Delaney CA, Pavlovic D, Hoorens A, Pipeleers DG, Eizirik DL (1997) Cytokines induce deoxyribonucleic acid strand breaks and apoptosis in human pancreatic islet cells. Endocrinology 138:2610–2614
Hoorens A, Van de CM, Kloppel G, Pipeleers D (1996) Glucose promotes survival of rat pancreatic beta cells by activating synthesis of proteins which suppress a constitutive apoptotic program. J Clin Invest 98:1568–1574
Kutlu B, Cardozo AK, Darville MI et al (2003) Discovery of gene networks regulating cytokine-induced dysfunction and apoptosis in insulin-producing INS-1 cells. Diabetes 52:2701–2719
Liu D, Pavlovic D, Chen MC, Flodstrom M, Sandler S, Eizirik DL (2000) Cytokines induce apoptosis in beta-cells isolated from mice lacking the inducible isoform of nitric oxide synthase (iNOS−/−). Diabetes 49:1116–1122
Tsuchiya M, Suematsu M, Suzuki H (1994) In vivo visualization of oxygen radical-dependent photoemission. Methods Enzymol 233:128–140
Kenchappa P, Yadav A, Singh G, Nandana S, Banerjee K (2004) Rescue of TNF alpha-inhibited neuronal cells by IGF-1 involves Akt and c-Jun N-terminal kinases. J Neurosci Res 76:466–474
Sizemore N, Leung S, Stark GR (1999) Activation of phosphatidylinositol 3-kinase in response to interleukin-1 leads to phosphorylation and activation of the NF-kappaB p65/RelA subunit. Mol Cell Biol 19:4798–4805
Aikin R, Rosenberg L, Maysinger D (2000) Phosphatidylinositol 3-kinase signaling to Akt mediates survival in isolated canine islets of Langerhans. Biochem Biophys Res Commun 277:455–461
Castrillo A, Bodelon OG, Bosca L (2000) Inhibitory effect of IGF-I on type 2 nitric oxide synthase expression in Ins-1 cells and protection against activation-dependent apoptosis: involvement of phosphatidylinositol 3-kinase. Diabetes 49:209–217
Jhala US, Canettieri G, Screaton RA et al (2003) cAMP promotes pancreatic beta-cell survival via CREB-mediated induction of IRS2. Genes Dev 17:1575–1580
Jambal P, Masterson S, Nesterova A et al (2003) Cytokine-mediated down-regulation of the transcription factor cAMP-response element-binding protein in pancreatic beta-cells. J Biol Chem 278:23055–23065
Montrose-Rafizadeh C, Avdonin P, Garant MJ et al (1999) Pancreatic glucagon-like peptide-1 receptor couples to multiple G proteins and activates mitogen-activated protein kinase pathways in Chinese hamster ovary cells. Endocrinology 140:1132–1140
Hengartner MO (2000) The biochemistry of apoptosis. Nature 407:770–776
Li J, Yang S, Billiar TR (2000) Cyclic nucleotides suppress tumor necrosis factor alpha-mediated apoptosis by inhibiting caspase activation and cytochrome c release in primary hepatocytes via a mechanism independent of Akt activation. J Biol Chem 275:13026–13034
Scarim AL, Arnush M, Blair LA et al (2001) Mechanisms of beta-cell death in response to double-stranded (ds) RNA and interferon-gamma: dsRNA-dependent protein kinase apoptosis and nitric oxide-dependent necrosis. Am J Pathol 159:273–283
Mochizuki T, Asai A, Saito N et al (2002) Akt protein kinase inhibits non-apoptotic programmed cell death induced by ceramide. J Biol Chem 277:2790–2797
Matsui T, Tao J, del Monte F et al (2001) Akt activation preserves cardiac function and prevents injury after transient cardiac ischemia in vivo. Circulation 104:330–335
Kroncke KD, Brenner HH, Rodriguez ML et al (1993) Pancreatic islet cells are highly susceptible towards the cytotoxic effects of chemically generated nitric oxide. Biochim Biophys Acta 1182:221–229
Lenzen S, Drinkgern J, Tiedge M (1996) Low antioxidant enzyme gene expression in pancreatic islets compared with various other mouse tissues. Free Radic Biol Med 20:463–466
Hohmeier HE, Thigpen A, Tran VV, Davis R, Newgard CB (1998) Stable expression of manganese superoxide dismutase (MnSOD) in insulinoma cells prevents IL-1 beta-induced cytotoxicity and reduces nitric oxide production. J Clin Invest 101:1811–1820
Laskin DL, Fakhrzadeh L, Heck DE, Gerecke D, Laskin JD (2002) Upregulation of phosphoinositide 3-kinase and protein kinase B in alveolar macrophages following ozone inhalation. Role of NF-kappaB and STAT-1 in ozone-induced nitric oxide production and toxicity. Mol Cell Biochem 234–235:91–98
Ruggles JA, Kelemen D, Baron A (2004) Emerging therapies: controlling glucose homeostasis, immunotherapy, islet transplantation, gene therapy, and islet cell neogenesis and regeneration. Endocrinol Metab Clin N Am 33:239–252, xii
Acknowledgements
The INS-1E cells were a kind gift from C. Wollheim (Department of Internal Medicine, University Medical Centre,Geneva, Switzerland). The authors are also grateful to D. Ahn (who was supported by a Summer Studentship from the Banting and Best Diabetes Centre [BBDC], University of Toronto) for technical assistance, and to V. Koshkin (University of Toronto) for assistance with the ROS assay. This work was supported by a grant from the Canadian Diabetes Association (CDA). L. Li was supported by post-doctoral fellowships from the CDA, the BBDC and the Department of Medicine, University of Toronto; a Timeposters Award; and a William S. Fenwick Fellowship and a Chisholm Memorial Fellowship from the Faculty of Medicine, University of Toronto. W. El-Kholy was supported by a CDA Graduate Studentship, and P. L. Brubaker was supported by the Canada Research Chairs Program.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, L., El-Kholy, W., Rhodes, C.J. et al. Glucagon-like peptide-1 protects beta cells from cytokine-induced apoptosis and necrosis: role of protein kinase B. Diabetologia 48, 1339–1349 (2005). https://doi.org/10.1007/s00125-005-1787-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-005-1787-2