Abstract
The regulation of death pathways in neutrophils has been of long interest, but the relevance of neutrophil apoptosis to the pathogenesis and treatment of autoimmune diseases has only recently been becoming recognized. This brief review addresses the relevant pathways by which neutrophil apoptosis is regulated and summarizes the current understanding regarding the potential role of apoptotic neutrophils in the initiation and/or propagation of autoimmunity, as well as the applicability of modulation of neutrophil death in the treatment of autoimmune diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
An overview of neutrophil apoptosis
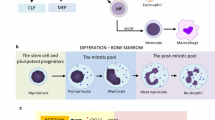
Neutrophils play critical effector and regulatory roles in a multitude of immune responses, eliminating undesired pathogens and other components of their environment by phagocytosis, the elaboration of toxic mediators, and the production of effector cytokines, which in turn recruit and modulate the activity of other cells [1]. Their activity appears to be tightly regulated, at least in part, by apoptosis, which results in a half-life of approximately 8–10 h or less in both inflammatory and noninflammatory states [2, 3]. Apoptosis appears to provide an appropriate means by which to eliminate unwanted or unnecessary neutrophils: this process eliminates cells from inflamed tissues without releasing their hazardous contents, and the uptake of apoptotic cells by surrounding phagocytic cells is associated with the release of anti-inflammatory mediators. In this way, neutrophil death via apoptosis likely makes a critical contribution to the regulation of inflammatory responses, in both pathological and nonpathological, physiological states [1].
Neutrophil apoptosis reflects a balance between both death and survival factors, some of which appear to be cell lineage specific (Fig. 1). Spontaneous neutrophil apoptosis may reflect clustering of death receptors (DRs), such as Fas (CD95), perhaps in response to reactive oxygen species (ROS) [4], leading to caspase signaling and/or mitochondrial membrane depolarization. However, this process is likely influenced by other pathways as well, particularly pro- and antiapoptotic proteins of the bcl-2 family, as well as survival factors like granulocyte-macrophage colony-stimulating factor (GM-CSF), which elicit signaling at least via phosphoinositide 3-kinase (PI3K) and mitogen-activated protein kinase (MAPK) pathways [5]. Other modulators of apoptosis and survival include the tyrosine phosphatase Src homology domain 2 (SH2)-containing tyrosine phosphatase-1 (SHP-1), which inactivates at least some Src family kinases [6], and the cystein protease calpain, which modulates Bax and caspase-3 [7], each of which is known to regulate apoptosis in primary neutrophils. Other biological pathways likely contribute as well, such as type I interferons via the phosphoinositol 3-kinase, protein kinase C-δ, and NF-κB pathways [8], or immunoglobulins and/or their immune complexes via Fc receptors such as FcγRIII [9]. Thus, a growing list of intracellular modulators regulate neutrophil apoptosis, the specific hierarchy and organization of which remain incompletely elucidated. For a more detailed discussion of neutrophil apoptosis, the reader is directed to one of several recent reviews (e.g., [10]).
A simplified view of the regulation of neutrophil death and survival. In general, neutrophil survival reflects a balance between death and survival signals. Spontaneous neutrophil apoptosis may reflect, at least in part, clustering of death receptors (DRs), such as Fas (CD95), perhaps in response to reactive oxygen species (ROS), leading to caspase signaling and/or mitochondrial membrane depolarization. This process is modulated by other pathways, especially survival factors such as cytokines (e.g., granulocyte-macrophage colony-stimulating factor, GM-CSF), which elicit signaling at least via the phosphoinositide 3-kinase (PI3K) and mitogen-activated protein kinase (MAPK) pathways, promoting survival via antiapoptotic bcl-2 family members and the inhibition of proapoptotic caspase activities
Modulation of neutrophil apoptosis as a pathogenic mechanism in autoimmunity
Perhaps the most straightforward mechanism by which modulation of apoptosis might promote inflammatory disease involves defective neutrophil apoptosis, which could allow improper neutrophil survival and thereby promote inflammation and tissue damage. Several diseases have been associated with diminished neutrophil apoptosis and increased effector neutrophil numbers: in crystal-induced arthritis, for example, this may result, at least in part, from direct antiapoptotic effects of monosodium urate or calcium pyrophosphate crystals [11, 12]. In rheumatoid arthritis, this may reflect activities in inflamed synovial fluid, perhaps adenosine [13], while in inflammatory bowel disease, this may reflect increased local concentrations mucosal G-CSF [14]. Thus, survival or other antiapoptotic factors associated with some diseased organ(s) can promote neutrophilia and inflammation (Table 1).
However, neutrophils in many autoimmune diseases are associated with an increased propensity towards apoptosis. In rheumatoid arthritis, for instance, inflamed synoival fluid often contains oligonucleosomal material consistent with apoptotic neutrophils [15]. Systemic lupus erythematosus (SLE) is characterized by an overrepresentation of apoptotic neutrophils, which may reflect a disease-specific defect in the clearance of apoptotic cells [16], the ability of autoantibodies like anti-DNA to bind to and/or penetrate cells and promote apoptosis [17], and/or abnormally elevated levels of proapoptotic factors like tumor necrosis factor (TNF)-related apoptosis-inducing ligand (TRAIL [18]). Similarly, increased neutrophil apoptosis has been observed in antineutrophil cytoplasmic antibody (ANCA)-associated vasculitides, where apoptotic neutrophils may in fact provide a source of immunologically exposed neutrophil antigens that promote the production of ANCAs [19–21]. Indeed, some studies have indicated that ANCAs preferably bind antigens in apoptotic, vs viable, neutrophils [22], either way modulating their apoptotic pathways [23]. Similar effects on neutrophils have been reported for other autoantibodies, such as anti-La in SLE [24]. In this way, neutrophil apoptosis can partake in a self-propagating cycle in autoimmunity, promoting the generation of pathogenic inflammatory mediators, such as autoantibodies, which in turn further augment neutrophil death (Table 1).
Modulation of neutrophil apoptosis as a therapeutic strategy
Modulation of neutrophil death may therefore facilitate two potential outcomes: on one hand, in diseases like ANCA vasculitis, therapeutic inhibition of apoptosis may actually help suppress the supply of apoptotic material which promotes pathogenic inflammatory mediators like autoantibodies. However, on the other hand, neutrophilic inflammation clearly remains a critical component of the inflammatory lesions in many autoimmune diseases, including arthritis, lupus, and vasculitis, such that the therapeutic induction of neutrophil death continues to appear the more therapeutically viable approach. However, few studies, if any, have addressed the relative impact of such approaches in specific disease indications; thus, current assessments must rely on studies which correlate the therapeutic effect of an intervention upon neutrophil survival.
A few widely used therapies in autoimmune diseases are though to act, at least in part, by modulating neutrophil apoptosis: sulfasalazine, for instance, promotes apoptosis in neutrophils but not in other leukocytes [25], and auranofin (gold) inhibits neutrophil apoptosis at low concentrations but induces neutrophil death at high concentrations [26]. Intravenous immunoglobulin (IVIg) preparations generally contain proapoptotic anti-Fas antibodies, which promote neutrophil apoptosis [27, 28]. Such interventions clearly also exert effects outside of apoptosis per se—e.g., the ability of IVIg to interact with Fc receptors—but their concomitant ability to affect neutrophil survival suggests that at least part of their therapeutic benefit derives from an effect on neutrophil functions.
In addition, some animal models have indirectly demonstrated the potential utility of neutrophil apoptosis modulation in autoimmune disease. For instance, in a peroxochromate-induced mouse model of arthritis, nicotinamide—an inhibitor of poly(ADP-ribose) polymerase (PARP), a nuclear enzyme which participates in the apoptotic response to oxygen- and nitrogen-radical-induced DNA strand breaks—suppressed disease severity [29]. In addition, 3-aminobenzamide and 1,5-dihydroxyisoquinoline—also PARP inhibitors—successfully ameliorated trinitrobenzene sulfonic acid-induced colitis in rats [30]. Mice deficient in the forkhead transcription factor Foxo3a were refractory to the K/BxN serum transfer model of arthritis due to an inability of their neutrophils to suppress Fas ligand-induced apoptosis [31]. Such findings interestingly suggest that, whereas the life span of inactive neutrophils might be regulated by Fas-induced apoptosis [4], inflammatory neutrophils generally may suppress apoptosis via Fas, such that alternate pathways (e.g., bcl-2 family members) regulate neutrophil life span in disease states [31]. In fact, apoptosis-inducing anti-Fas antibodies can effectively treat arthritis in several mouse models, including collagen-induced arthritis, MRL/gld mice, and human T-cell leukemia virus (HTLV)-1 Tax transgenic mice, and disease in HTLV-1 env-pX transgenic mice is exacerbated on an lpr (Fas-mutant), yet improved on a Fas-transgenic, background [32–35]. On the other hand, however, DBA/lpr mice are less susceptible to collagen-induced arthritis than their DBA/+ counterparts [36]. In all these studies, it remains unclear how much of the phenotypes reflect the specific role of Fas on neutrophils, as opposed to other cell lineages susceptible to Fas-induced apoptosis, such as T cells or synovial cells; still, the contextual importance of the Fas pathway in autoimmune-related neutrophil survival clearly remains incompletely elucidated. Nonetheless, although indirect, such accumulating evidence suggests that interventions which ameliorate autoimmune diseases like arthritis may work, at least in part, by affecting neutrophil survival and/or apoptosis.
Conclusions
The relevance of neutrophil apoptosis and death to the pathogenesis and therapy for autoimmune diseases has only relatively recently begun to become recognized. In some diseases, such as lupus or ANCA-associated vasculitis, apoptotic neutrophils may both promote and result from ongoing autoimmune processes, but in all or nearly all autoimmune diseases, neutrophils can also be considered critical effectors of inflammation. Thus, the induction of neutrophil death remains a viable desired therapeutic outcome, but the relative values of inhibiting vs promoting neutrophil death in specific disease states remain to be investigated and understood. Needed are studies which directly address the processes that regulate neutrophil death in both physiological and pathological states.
References
Burg ND, Pillinger MH (2001) The neutrophil: function and regulation in innate and humoral immunity. Clin Immunol 99:7–17
Price TH, Chatta GS, Dale DC (1996) Effect of recombinant granulocyte colony-stimulating factor on neutrophil kinetics in normal young and elderly humans. Blood 88:335–340
Dale DC, Liles WC, Llewellyn C, Price TH (1998) Effects of granulocyte-macrophage colony-stimulating factor (GM-CSF) on neutrophil kinetics and function in normal human volunteers. Am J Hematol 57:7–15
Scheel-Toellner D, Wang K, Craddock R, Webb PR, McGettrick HM, Assi LK, Parkes N, Clough LE, Gulbins E, Salmon M, Lord JM (2004) Reactive oxygen species limit neutrophil life span by activating death receptor signaling. Blood 104:2557–2564
Villunger A, O’Reilly LA, Holler N, Adams J, Strasser A (2000) Fas ligand, Bcl-2, granulocyte colony-stimulating factor, and p38 mitogen-activated protein kinase: regulators of distinct cell death and survival pathways in granulocytes. J Exp Med 192:647–658
Daigle I, Yousefi S, Colonna M, Green DR, Simon HU (2002) Death receptors bind SHP-1 and block cytokine-induced anti-apoptotic signaling in neutrophils. Nat Med 8:61–67
Altznauer F, Conus S, Cavalli A, Folkers G, Simon HU (2004) Calpain-1 regulates Bax and subsequent Smac-dependent caspase-3 activation in neutrophil apoptosis. J Biol Chem 279:5947–5957
Wang K, Scheel-Toellner D, Wong SH, Craddock R, Caamano J, Akbar AN, Salmon M, Lord JM (2003) Inhibition of neutrophil apoptosis by type 1 IFN depends on cross-talk between phosphoinositol 3-kinase, protein kinase C-δ, and NF-κB signaling pathways. J Immunol 171:1035–1041
Durand V, Renaudineau Y, Pers JO, Youinou P, Jamin C (2001) Cross-linking of human FcγRIIIb induces the production of granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor by polymorphonuclear neutrophils. J Immunol 167:3996–4007
Simon HU (2003) Neutrophil apoptosis pathways and their modifications in inflammation. Immunol Rev 193:101–110
Akahoshi T, Nagaoka T, Namai R, Sekiyama N, Kondo H (1997) Prevention of neutrophil apoptosis by monosodium urate crystals. Rheumatol Int 16:231–235
Tudan C, Fong D, Duronio V, Burt HM, Jackson JK (2000) The inhibition of spontaneous and tumor necrosis factor-alpha induced neutrophil apoptosis by crystals of calcium pyrophosphate dihydrate and monosodium urate monohydrate. J Rheumatol 27:2463–2472
Ottonello L, Cutolo M, Frumento G, Arduino N, Bertolotto M, Mancini M, Sottofattori E, Dallegri F (2002) Synovial fluid from patients with rheumatoid arthritis inhibits neutrophil apoptosis: role of adenosine and proinflammatory cytokines. Rheumatology (Oxford) 41:1249–1260
Ina K, Kusugami K, Hosokawa T, Imada A, Shimizu T, Yamaguchi T, Ohsuga M, Kyokane K, Sakai T, Nishio Y, Yokoyama Y, Ando T (1999) Increased mucosal production of granulocyte colony-stimulating factor is related to a delay in neutrophil apoptosis in inflammatory bowel disease. J Gastroenterol Hepatol 14:46–53
Yu D, Rumore PM, Liu Q, Steinman CR (1997) Soluble oligonucleosomal complexes in synovial fluid from inflamed joints. Arthritis Rheum 40:648–654
Ren Y, Tang J, Mok MY, Chan AW, Wu A, Lau CS (2003) Increased apoptotic neutrophils and macrophages and impaired macrophage phagocytic clearance of apoptotic neutrophils in systemic lupus erythematosus. Arthritis Rheum 48:2888–2897
Hsieh SC, Sun KH, Tsai CY, Tsai YY, Tsai ST, Huang DF, Han SH, Yu HS, Yu CL (2001) Monoclonal anti-double stranded DNA antibody is a leucocyte-binding protein to up-regulate interleukin-8 gene expression and elicit apoptosis of normal human polymorphonuclear neutrophils. Rheumatology (Oxford) 40:851–858
Matsuyama W, Yamamoto M, Higashimoto I, Oonakahara K, Watanabe M, Machida K, Yoshimura T, Eiraku N, Kawabata M, Osame M, Arimura K (2004) TNF-related apoptosis-inducing ligand is involved in neutropenia of systemic lupus erythematosus. Blood 104:184–191
Harper L, Cockwell P, Adu D, Savage CO (2001) Neutrophil priming and apoptosis in anti-neutrophil cytoplasmic autoantibody-associated vasculitis. Kidney Int 59:1729–1738
Patry YC, Trewick DC, Gregoire M, Audrain MA, Moreau AM, Muller JY, Meflah K, Esnault VL (2001) Rats injected with syngenic rat apoptotic neutrophils develop antineutrophil cytoplasmic antibodies. J Am Soc Nephrol 12:1764–1768
Rauova L, Gilburd B, Zurgil N, Blank M, Guegas LL, Brickman CM, Cebecauer L, Deutsch M, Wiik A, Shoenfeld Y (2002) Induction of biologically active antineutrophil cytoplasmic antibodies by immunization with human apoptotic polymorphonuclear leukocytes. Clin Immunol 103:69–78
Gilligan HM, Bredy B, Brady HR, Hebert MJ, Slayter HS, Xu Y, Rauch J, Shia MA, Koh JS, Levine JS (1996) Antineutrophil cytoplasmic autoantibodies interact with primary granule constituents on the surface of apoptotic neutrophils in the absence of neutrophil priming. J Exp Med 184:2231–2241
Deutsch M, Guejes L, Zurgil N, Shovman O, Gilburd B, Afrimzon E, Shoenfeld Y (2004) Antineutrophil cytoplasmic autoantibodies penetrate into human polymorphonuclear leukocytes and modify their apoptosis. Clin Exp Rheumatol 22:S35–S40
Hsieh SC, Yu HS, Lin WW, Sun KH, Tsai CY, Huang DF, Tsai YY, Yu CL (2003) Anti-SSB/La is one of the antineutrophil autoantibodies responsible for neutropenia and functional impairment of polymorphonuclear neutrophils in patients with systemic lupus erythematosus. Clin Exp Immunol 131:506–516
Akahoshi T, Namai R, Sekiyama N, Tanaka S, Hosaka S, Kondo H (1997) Rapid induction of neutrophil apoptosis by sulfasalazine: implications of reactive oxygen species in the apoptotic process. J Leukoc Biol 62:817–826
Liu J, Akahoshi T, Namai R, Matsui T, Kondo H (2000) Effect of auranofin, an antirheumatic drug, on neutrophil apoptosis. Inflamm Res 49:445–451
Prasad NK, Papoff G, Zeuner A, Bonnin E, Kazatchkine MD, Ruberti G, Kaveri SV (1998) Therapeutic preparations of normal polyspecific IgG (IVIg) induce apoptosis in human lymphocytes and monocytes: a novel mechanism of action of IVIg involving the Fas apoptotic pathway. J Immunol 161:3781–3790
Altznauer F, von Gunten S, Spath P, Simon HU (2003) Concurrent presence of agonistic and antagonistic anti-CD95 autoantibodies in intravenous Ig preparations. J Allergy Clin Immunol 112:1185–1190
Miesel R, Kurpisz M, Kroger H (1995) Modulation of inflammatory arthritis by inhibition of poly(ADP ribose) polymerase. Inflammation 19:379–387
Zingarelli B, O’Connor M, Hake PW (2003) Inhibitors of poly(ADP-ribose) polymerase modulate signal transduction pathways in colitis. Eur J Pharmacol 469:183–194
Jonsson H, Allen P, Peng SL (2005) Inflammatory arthritis requires Foxo3a to prevent Fas ligand-induced neutrophil apoptosis. Nat Med 11:666–671
Ogawa Y, Kuwahara H, Kimura Y, Tani Y, Yonehara S, Shiraishi A, Ohtsuki M (2001) Therapeutic effect of anti-Fas antibody on a collagen-induced arthritis model. J Rheumatol 28:950–955
Nishimura-Morita Y, Nose M, Inoue T, Yonehara S (1997) Amelioration of systemic autoimmune disease by the stimulation of apoptosis-promoting receptor Fas with anti-Fas mAb. Int Immunol 9:1793–1799
Fujisawa K, Asahara H, Okamoto K, Aono H, Hasunuma T, Kobata T, Iwakura Y, Yonehara S, Sumida T, Nishioka K (1996) Therapeutic effect of the anti-Fas antibody on arthritis in HTLV-1 tax transgenic mice. J Clin Invest 98:271–278
Iwakura Y, Itagaki K, Ishitsuka C, Yamasaki Y, Matsuzawa A, Yonehara S, Karasawa S, Ueda S, Saijo S (1998) T cell leukemia virus type-1 env-pX region is not dependent on H-2 haplotypes and modified by the expression levels of Fas antigen. J Immunol 161:6592–6598
Hoang TR, Hammermuller A, Mix E, Kreutzer HJ, Goerlich R, Kohler H, Nizze H, Thiesen HJ, Ibrahim SM (2004) A proinflammatory role for Fas in joints of mice with collagen-induced arthritis. Arthritis Res Ther 6:R404–R414
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Peng, S.L. Neutrophil apoptosis in autoimmunity. J Mol Med 84, 122–125 (2006). https://doi.org/10.1007/s00109-005-0007-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-005-0007-3