Abstract
Background
Role of cytokines as well as matrix metalloproteinases (MMPs) is well defined in various central nervous system inflammatory diseases. However, the role of these cytokines and MMPs in acute transverse myelitis is inadequately studied.
Materials and methods
Patients with acute transverse myelitis, fulfilling the inclusion and exclusion criteria defined by Transverse Myelitis Consortium Working Group, were enrolled along with age and sex matched controls. A detailed clinical evaluation and magnetic resonance imaging of patients was done. Cerebrospinal fluid (CSF) samples both from patients and controls were collected. CSF samples were analyzed for cytokines [interleukin (IL)-6, IL-8, IL-10 and IL-17)] and matrix metalloproteinases (MMP-2, MMP-9). Patients were followed up for 3 months. Disability was assessed using modified Barthel index (MBI).
Results
CSF levels of all cytokines IL-6, IL-8, IL-10, MMP-2 and MMP-9, except IL-17, were significantly higher in patients with acute transverse myelitis (p < 0.001). CSF IL-6 and IL-8 were significantly associated with severity of the disease (MBI ≤ 12). After 3 months, quadriparesis (p = 0.001, odd’s ratio 19.5, 95 % CI 2.34–62.39) and long-segment myelitis (p = 0.035, odd’s ratio 4.37, 95 % CI 1.17–5.95) were significantly associated with poor outcome. Among cytokines and MMPs, IL-6 levels at baseline correlated significantly with the MBI at 3 months (Spearmen’s ρ = −0.335, p = 0.01).
Conclusion
In conclusion, both anti-inflammatory and pro-inflammatory cytokines, MMP-2, and MMP-9 are elevated in the acute phase of transverse myelitis. Possibly, IL-6 plays a role in determining the disability.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Transverse myelitis is an inflammatory disorder of the spinal cord characterized by an acute or subacute development of motor weakness, sensory impairment and autonomic dysfunction. Pathologically, transverse myelitis is characterized by spinal parenchymal infiltration of lymphocytes and monocytes, with varying degrees of inflammation, demyelination and axonal injury [1–3].
Transverse myelitis, as an inflammatory disorder, might as well be a part of a spectrum of autoimmune demyelinating disorders comprising of multiple sclerosis, neuromyelitis optica, and acute disseminated encephalomyelitis. The clinical and radiological characteristics, including temporal course, of these disorders help in determining the basic etiological spectrum in which they fall. This may range from regional-genetic variations in multiple sclerosis, to site-specific antibody damage in neuromyelitis optica, to post-infectious and post-vaccination-triggered antibody and host-based factor destruction in acute disseminated encephalomyelitis. The commonality in these disorders is more likely in the final common inflammatory pathways, but may be differentiated on the basis of site of lesion (with or without optic nerve; various combinations within the neuraxis), magnitude of neuronal loss (reversible or irreversible or partially reversible), and the temporal course (monophasic or multiphasic) [4, 5].
Cytokines are the key mediators of inflammation and have crucial role in determining the extent of spinal cord injury. Essentially, two types of responses are observed, a type-1 response (pro-inflammatory) and a type-2 response (anti-inflammatory). The type-1 response is mediated by Th1 and Th17 cells which secrete interleukin-1 (IL-1), IL-2, IL-17, interferon-γ (IFN-γ), and tumor necrosis factor-alpha (TNF-α), and modulate the cellular immunity.
The type-2 response is mediated by Th2, T-regulator and natural killer T cells which secrete IL-4, IL-5, IL-10, IL-14 and transforming growth factor-β (TGF-β), and modulate the humoral immunity.
Several studies have noted a distinct serum cytokine profiles in neuromyelitis optica and multiple sclerosis. For example, IL-6 could play important roles in neuromyelitis optica pathogenesis, as it is involved in the survival of plasmablasts that produce anti-AQP4 antibody in peripheral circulation and in the enhancement of inflammation in the central nervous system [6]. Cerebrospinal fluid (CSF) IL-6 has been shown to be elevated in transverse myelitis and predict disability [7].
Matrix metalloproteinases (MMP) are zinc-dependant endopeptidases responsible for degradation of extracellular matrix. MMP-2 and MMP-9 belong to gelatinase group of enzymes and have role in degradation of basement membrane leading to blood–brain barrier (BBB) disruption and recruitment of inflammatory cells. In neuromyelitis optica, the destruction of the BBB has been considered to be the first step of the disease process. Tasaki et al. in their study found that the autocrine secretion of MMP-2/9 by brain microvascular endothelial cells from neuromyelitis optica spectrum disorder patients potentially increases BBB permeability thereby facilitating the entry of inflammatory cells into the central nervous system [8–10].
Although there have been ample studies documenting the immune aberrations in multiple sclerosis and neuromyelitis optica, such cytokine profile has been eluded for acute transverse myelitis patients. Aberrations in immune system also contribute to the disease pathway in acute transverse myelitis; however, exact role of cytokines and MMPs in immunopathogenesis of acute transverse myelitis is unclear. Our aim of this study was to evaluate CSF cytokines and MMP-2 and MMP-9 in patients with transverse myelitis. We also correlated these values with disease severity and outcome.
Materials and methods
This case–control study was carried out in Department of Neurology at King George’s Medical University Uttar Pradesh, Lucknow, India. Prior ethical approval was obtained from the Institutional Ethics Committee. The written informed consent was taken from all the cases and controls.
Selection of cases
Consecutive patients presenting with acute paraplegia or quadriplegia, fulfilling the diagnostic criteria of transverse myelitis proposed by Transverse Myelitis Consortium Working Group, were included. Patients were excluded if they had any feature mentioned in the exclusion criteria of Transverse Myelitis Consortium Working Group definition of transverse myelitis [1] (Table 1). Patients who were being administered steroids (oral or parenteral) were not enrolled in the study.
Selection of controls
Control cerebrospinal fluid was obtained from 32 age- and sex-matched otherwise healthy persons undergoing spinal anesthesia in various surgical departments of our institution.
Patient evaluation
All patients underwent detailed clinical evaluation and disability assessment as per modified Barthel index (MBI). MBI is a measure of disability or dependence of a patient for his activities of daily living. The patient is scored on ten items of daily life viz. bowel, bladder, grooming, toilet use, feeding, transfer, mobility, dressing, stairs and bathing, with higher scores (maximum 20) denoting more independence. In our evaluation, patients with MBI ≤ 12 were considered to have severe neurological disability.
Routine hematological and biochemical evaluation was done in all cases; additionally, anti-nuclear antibody and aquaporin 4 antibodies were done to diagnose the respective entities.
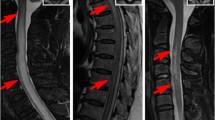
All patients were subjected to contrast-enhanced spinal magnetic resonance imaging (MRI). Patients were divided into two categories as (1) < 3 vertebral segments which we called as short segment transverse myelitis and (2) ≥ 3 vertebral segments as longitudinally extensive transverse myelitis. Visual-evoked potential was done to look for any latency prolongation suggestive of optic neuritis. CSF was obtained from all cases and controls. CSF samples were subjected to biochemical, microscopic, virological, IgG index and oligoclonal band examinations.
Estimation of cytokines and MMPs
CSF was performed within 2 weeks of onset, in the crescendo phase of the disease, before the institution of intravenous methylprednisolone. CSF samples were stored at −80 °C.
The tests were done using commercially available human ELISA kits as per manufacturer’s instructions (Bio Legend Max™, San Diego, CA, USA for IL-6, IL-8, IL-10, IL-17 and MMP-9 and Abcam plc., Cambridge, UK for MMP-2). The cytokine selection (IL 6, IL-8, IL-10, IL-17) was done to indicate both type 1 (IL 6, IL-8, IL-17) and type 2 (IL-10) responses. Thus, the acute phase response (IL-6), neutrophil-chemotaxis (IL-8) and monocyte/macrophage and lymphocyte-associated responses (IL-17) could be represented. MMPs on the other hand were shortlisted to assess the breakdown of extracellular matrix (MMP-2) and neutrophil migration across the basement membrane (MMP-9).
ELISA tests were performed in duplicate, independently for each sample, and the results were expressed as picogram/ml (pg/ml) for all cytokines and MMP-9. The results of MMP-2 were expressed in nanogram/ml (ng/ml). The median, and not the mean, values were used for statistical analyses.
Treatment and follow-up
Patients were treated with intravenous methylprednisolone for 5 days [11]. Patients were followed up for 3 months. Outcome was assessed using MBI.
Statistical analysis
Statistical analysis was done using statistical software SPSS (version 16.0, Chicago, LA, USA). All categorical variables were expressed as percentages and all continuous variables were expressed as mean ± SD. Shapiro–Wilk test was used to test whether the data were normally distributed or not. Mann–Whitney U test was applied to compare median of data that were not normally distributed. Categorical variables were compared using Chi-square or Fisher exact test which ever was applicable. Means were compared using independent sample t test. Correlation between two variables was calculated using bivariate correlation. Odd’s ratios and 95 % confidence intervals were calculated as required. All p values < 0.05 were taken as significant. Multivariate analysis using binary logistic regression was done to look for variables independently associated with poor outcome.
Results
During study period, 66 consecutive patients with transverse myelitis were considered for inclusion. Seven patients were excluded. One patient was positive for Herpes simplex virus-1, while 2 were positive for Varicella zoster virus. Two patients had NMO antibody positive. One patient denied consent. Finally, 59 patients (39 males and 20 females) were enrolled in this study (Fig. 1).
Baseline characteristics
Baseline characteristics of 59 patients with acute transverse myelitis are shown in Table 2. Majority of patients 45 (76.3 %) had paraparesis. Quadriparesis was the presenting feature in 14 (23.7 %) cases. Neuroimaging changes were common in cervico-thoracic region 30 (50.85 %). Long-segment myelitis was seen in 44 (74.6 %) cases.
Comparison of cytokines and MMPs levels between cases and controls
We observed that levels of cytokines IL-6, IL-8, IL-10, MMP-2 and MMP-9 were significantly higher in patients with transverse myelitis as compared to the controls (p < 0.001). No significant difference in the levels of IL-17 was noted (Table 3).
Correlations of cytokines and MMPs with disease severity
No significant correlation was found between baseline MBI and most of the cytokines and MMPs we estimated; however, CSF IL6 and IL8 were significantly associated with more severe disease (MBI ≤ 12) (Table 4). No significant difference was found in the levels of cytokines and MMPs in patients with short- and long-segment myelitis.
Follow-up
After 3 months, 31 cases had MBI ≤ 12 (including 4 deaths). Univariate analysis revealed that quadriparesis (p = 0.001, odd’s ratio 19.500; 95 % confidence interval 2.342–162.390) and long-segment myelitis (p = 0.035, odd’s ratio 4.37; 95 % confidence interval 1.196–15.951) were significantly associated with poor outcome (Table 5). Quadriparesis (p = 0.007) was the lone significant factor associated with poor outcome on binary logistic regression. Out of the estimated cytokines and MMPs, only CSF IL-6 levels significantly correlated with MBI at 3 months (Spearmen’s ρ = −0.335, p = 0.01) (Fig. 2).
Discussion
We found that majority of our patients with acute transverse myelitis had longitudinally extensive disease. CSF levels of IL-6, IL-8 and IL-10 and MMP-2 and MMP-9 were significantly elevated in patients with acute transverse myelitis. IL-6 and IL-8 levels correlated significantly with the level of disability at baseline. IL-6 levels showed a significant (negative, inverse) correlation with MBI at 3 months.
Historically, acute transverse myelitis is said to involve the adolescents and those between 30 and 39 years without any gender predilection [1]. Our cohort was relatively younger (mean age 28 years) with a ratio of 2:1 in favor of males. Observations from a study of 40 patients with acute transverse myelitis also suggest a male predominance with a ratio of 1.5. However, the mean age in this group was 40.7 years [11].
We observed that in patients with acute transverse myelitis both pro-inflammatory and anti-inflammatory cytokines are altered. It may be suggested that the dysregulated production of cytokines contributes in the pathogenesis of acute transverse myelitis. Review of literature suggests that changes in cytokines have consistently been observed in neuromyelitis optica and multiple sclerosis, but information related to acute transverse myelitis is limited. A varied pattern of immunological changes has been noted in neuromyelitis optica and multiple sclerosis [7, 12]. In a study to investigate the role of cytokines/chemokines in neuromyelitis optica, multiple sclerosis, and other non-inflammatory neurological disorders, the CSF levels of IL-1 receptor antagonist, IL-6, IL-8, IL-13 and granulocyte colony-stimulating factor were found to be elevated in neuromyelitis optica, while IL-9, fibroblast growth factor-basic, granulocyte macrophage colony-stimulating factor, macrophage inflammatory protein-1-beta and TNF-α were increased in multiple sclerosis. IL-10 and interferon-gamma-inducible protein-10 were elevated both in neuromyelitis optica and multiple sclerosis. IL-6 levels were found to be elevated only in patients with neuromyelitis optica [6].
We also observed that IL-6 was significantly correlated with disability at enrollment and poor outcome. IL-6 is an IL that acts as both a pro-inflammatory and anti-inflammatory cytokine. It is secreted by T cells and macrophages to stimulate immune response to trauma, especially burns, or other tissue damage leading to inflammation. CSF IL-6 plays important roles in neuromyelitis optica pathogenesis, such as CNS inflammation, astrocytic damage and BBB disruption. In addition, it might be a useful biomarker for differentiating neuromyelitis optica from multiple sclerosis, and a helpful early diagnostic marker of neuromyelitis optica. Estimation in patients with neuromyelitis optica has suggested that IL-6 by polyclonally activated CD4 + T cells directly correlated to neurological disability [13]. Our findings suggest that IL-6 is a key cytokine in patients with transverse myelitis and second the earlier elucidated pathway and role of IL-6 in such patients. As suggested by Kaplin et al., these findings may have an important bearing in terms of treatment as well as prognosis [14]. It is worth mentioning that therapeutic blockade of IL-6 by the neutralizing anti-IL-6 receptor monoclonal antibody tocilizumab has recently been approved for the treatment of many inflammatory diseases, including neuromyelitis optica [15]. Likewise, most patients enrolled in our study had long-segment myelitis that might be amenable to similar treatment protocols.
We observed that in acute phase the matrix metalloproteinase-9 (MMP-9) was significantly elevated in patients with acute transverse myelitis. MMP-9 plays an important role in some inflammatory diseases of central nervous system through the BBB disruption. Central nervous system immunological profile differs between neuromyelitis optica and multiple sclerosis. In a study, serum MMP-9 concentrations were significantly higher in neuromyelitis optica than multiple sclerosis in comparison to that of controls. Possibly, inhibition of MMPs may be of some therapeutic value to these patients [16].
These findings are contrary to the earlier observations derived from 23 patients of multiple sclerosis and 7 patients of neuromyelitis optica, where MMP-9 levels were found to be higher in patients with multiple sclerosis [17].
IL-10 levels were found to be elevated in patients with acute transverse myelitis in our study. Although study in a similar subset of patients is not available, the role of IL-10 in 120 patients with various inflammatory and non-inflammatory diseases of the central nervous system has been studied which suggests that CSF IL-10 levels are elevated in patients with CNS inflammatory diseases. Amongst notable disorders, the study included patients with multiple sclerosis [18].
Instead of going ahead with a multitude of marker of inflammation, a handpicked logical segregation of cytokines and MMPs to represent type 1 and type 2 responses along with the assessment of the BBB breach, respectively, is possibly a strength of our study. Our findings may help in the selection and evaluation of potential therapeutic agents in patients with acute transverse myelitis.
The major limitation of our study was the lack of estimation of cytokines and MMPs on follow-up. Thus, for how long the inflammatory activity continued in these patients remains unknown? Even though IL-6 was elevated in our patients, IL-17 levels were equivocal. Since IL-17 is known to regulate the production of IL-6, its levels may be reviewed in a subsequent study. We did not include patients of neuromyelitis optica and multiple sclerosis which might have served as a comparator. TNF-α could have been studied in the study subjects as anti-TNF drugs have recently been shown to be effective in acute myelopathies.
In conclusion, both anti-inflammatory and pro-inflammatory cytokines, MMP-2 and MMP-9 are elevated in acute phase of transverse myelitis. IL-6 may play a role in predicting the disability.
References
Transverse Myelitis Consortium Working Group. Proposed diagnostic criteria and nosology of acute transverse myelitis. Neurology. 2002;59:499–505.
Kaplin AI, Krishnan C, Deshpande DM, Pardo CA, Kerr DA. Diagnosis and management of acute myelopathies. Neurologist. 2005;11:2–18.
Krishnan C, Kaplin AI, Deshpande DM, Pardo CA, Kerr DA. Transverse myelitis: pathogenesis, diagnosis and treatment. Front Biosci. 2004;9:1483–99.
Pandit L. Transverse myelitis spectrum disorders. Neurol India. 2009;57:126–33.
Cree BAC. Acute inflammatory myelopathies. Handb Clin Neurol. 2014;122:613–67.
Uzawa A, Mori M, Arai K, Sato Y, Hayakawa S, Masuda S, Taniguchi J, Kuwabara S. Cytokine and chemokine profiles in neuromyelitis optica: significance of interleukin-6. Mult Scler. 2010;16:1443–52.
Wullschleger A, Kapina V, Molnarfi N, Courvoisier DS, Seebach JD, Santiago-Raber ML, Hochstrasser DF, Lalive PH. Cerebrospinal fluid interleukin-6 in central nervous system inflammatory diseases. PLoS ONE. 2013;8:e72399.
Romanic AM, Madri JA. Extracellular matrix-degrading proteinases in the nervous system. Brain Pathol. 1994;4:145–56.
Rosenberg GA. Matrix metalloproteinases in neuroinflammation. Glia. 2002;39:279–91.
Tasaki A, Shimizu F, Sano Y, Fujisawa M, Takahashi T, Haruki H, Abe M, Koga M, Kanda T. Autocrine MMP-2/9 secretion increases the BBB permeability in neuromyelitis optica. J Neurol Neurosurg Psychiatry. 2014;85:419–30.
Bruna J, Martínez-Yélamos S, Martínez-Yélamos A, Rubio F, Arbizu T. Idiopathic acute transverse myelitis: a clinical study and prognostic markers in 45 cases. Mult Scler. 2006;12:169–73.
Hofer MJ, Campbell IL. Immunoinflammatory diseases of the central nervous system—the tale of two cytokines. Br J Pharmacol. 2015. doi:10.1111/bph.13175.
Linhares UC, Schiavoni PB, Barros PO, Kasahara TM, Teixeira B, Ferreira TB, Alvarenga R, Hygino J, Vieira MM, Bittencourt VC, Andrade RM, Andrade AF, Bento CA. The ex vivo production of IL-6 and IL-21 by CD4 + T cells is directly associated with neurological disability in neuromyelitis optica patients. J Clin Immunol. 2013;33:179–89.
Kaplin AI, Deshpande DM, Scott E, Krishnan C, Carmen JS, Shats I, et al. IL-6 induces regionally selective spinal cord injury in patients with the neuroinflammatory disorder transverse myelitis. J Clin Investig. 2005;115:2731–41.
Araki M, Matsuoka T, Miyamoto K, Kusunoki S, Okamoto T, Murata M, Miyake S, Aranami T, Yamamura T. Efficacy of the anti-IL-6 receptor antibody tocilizumab in neuromyelitis optica: a pilot study. Neurology. 2014;82:1302–6.
Hosokawa T, Nakajima H, Doi Y, Sugino M, Kimura F, Hanafusa T, Takahashi T. Increased serum matrix metalloproteinase-9 in neuromyelitis optica: implication of disruption of blood–brain barrier. J Neuroimmunol. 2011;236:81–6.
Mandler RN, Dencoff JD, Midani F, Ford CC, Ahmed W, Rosenberg GA. Matrix metalloproteinases and tissue inhibitors of metalloproteinases in cerebrospinal fluid differ in multiple sclerosis and Devic’s neuromyelitis optica. Brain. 2001;124:493–8.
Graber JJ, Allie SR, Mullen KM, Jones MV, Wang T, Krishnan C, et al. Interleukin-17 in transverse myelitis and multiple sclerosis. J Neuroimmunol. 2008;196:124–32.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: Ji Zhang.
Rights and permissions
About this article
Cite this article
Dixit, P., Garg, R.K., Malhotra, H.S. et al. Cytokines and matrix metalloproteinases in the cerebrospinal fluid of patients with acute transverse myelitis: an outcome analysis. Inflamm. Res. 65, 125–132 (2016). https://doi.org/10.1007/s00011-015-0896-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-015-0896-8