Abstract
Oral administration of some probiotic bacteria (e.g. Lactobacillus rhamnosus) attenuates various types of experimental arthritis, including collagen-induced arthritis (CIA) and inhibits arthritogenic autoantibodies. Much less is known about the possible anti-arthritogenic properties of exopolysaccharide (EPS), the major component of lactic bacteria biofilm. In this study, we asked the question whether systemic administration of EPS derived from L. rhamnosus KL37 depresses the production of anti-collagen IgG and affects the development of CIA in DBA/1 mice. Arthritis was induced employing two models of active CIA, in which mice were immunized with type II collagen (CII) either in the presence of lipopolysaccharide (LPS; mild arthritis with moderate CII-specific IgG production) or with Complete Freund’s Adjuvant and LPS (severe arthritis with massive CII-specific IgG production). Passive CIA was induced by intravenous injection of CII-specific monoclonal antibodies and LPS. Disease progression, the incidence and severity of arthritis, were determined. Serum concentration of CII-specific IgG was measured by enzyme-linked immunosorbent assay. Systemic administration of EPS markedly reduced CII-specific antibody production. Moreover, EPS significantly ameliorated arthritis in the active models of CIA, especially, when LPS alone was used as an adjuvant. In contrast, when arthritogenic antibodies were injected to mice in high amounts, the effect of EPS on the development of passive CIA was negligible and transient. These results show that EPS can suppress active CIA by the inhibition of arthritogenic antibodies production. Therefore, we suggest that EPS or EPS-producing probiotics may be promising agents for the supporting therapy of patients with rheumatoid arthritis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It has been commonly accepted that infectious agents play a role in pathogenesis of chronic inflammatory and autoimmune disorders, such as rheumatoid arthritis (RA) (Aoki et al. 1996; Navarra 2007; Yoshino and Ohsawa 2000). The best documented is a pathogenic role of Porphyromonas gingivalis, a periodontal bacteria, responsible for the association between chronic periodontitis and RA (Detert et al. 2010). Interestingly, components from various closely related species of both Gram-negative and Gram-positive intestinal bacteria may be either arthritogenic or non-arthritogenic (Simelyte et al. 2001, 2003). However, the specific factors contributing to the arthritogenecity of bacterial cell wall components (e.g. peptidoglycans, β-glucan, lipopolysaccharide: LPS) have not yet been fully determined (Hida et al. 2006). Some bacterial components (for example, LPS or mycobacterial components) are commonly used as adjuvants to induce or exacerbate joint inflammation in experimental models of RA, including collagen-induced arthritis (CIA) in mice and rats (Courtenay et al. 1980; Yoshino et al. 2000; Williams 2004). A rapid onset of arthritis can be induced by a passive transfer of monoclonal antibodies specific to arthritogenic epitopes of collagen type II (CII) and LPS (Nandakumar et al. 2003; Oestergaard et al. 2008). Importantly, the severity of arthritis depends on the amount of antibodies injected. Our previous studies confirmed that anti-CII antibodies play a critical arthritogenic role. We have shown that CIA-induced mice with high serum level of IgG anti-CII antibodies developed severe arthritis, while mice with low level of these antibodies developed mild arthritis with significantly lower incidence (Marcinkiewicz et al. 2007b).
Bacteria may also play a protective role in the development of autoimmune diseases (Stephani et al. 2011). Several studies have shown the beneficial/suppressive effects of some probiotic bacteria on the development of various types of arthritis, including CIA in mice (Kano et al. 2002; Sheil et al. 2004). Lactobacillus casei and L. rhamnosus, closely related lactic bacterial species, have been commonly used for these studies (Baharav et al. 2004; So et al. 2008a, b). However, much less is known, about the possible anti-arthritogenic properties of lactic bacteria exopolysaccharide (EPS), the major component of lactobacilli biofilm (Ciszek-Lenda 2011; Flemming et al. 2007; Vu et al. 2009). EPS has been tested successfully in other models of chronic inflammation. For example, EPS-producing probiotic strains significantly attenuate experimental colitis, and the degree of attenuation was dependent on the amount of EPS released (Şengül et al. 2006). The use of EPS instead of whole bacteria is in agreement with new alternative bacteriotherapy. As the biological properties of probiotic bacteria are strain specific, one of the current strategies to improve the reproducibility of probiotic therapies is to replace the use of live bacteria with bacterial components (peptidoglycan, lipoteichoic acid, EPS) of known immunoregulatory properties (Myhre et al. 2006; Seo et al. 2008; Vinderola et al. 2006).
Recently, we have shown that EPS derived from L. rhamnosus KL37 (Lipiński et al. 2003) alters the production of inflammatory mediators by macrophages in vitro (Ciszek-Lenda et al. 2011). Moreover, L. rhamnosus KL37-derived EPS inhibits the production of ovalbumin (OVA)-specific antibodies in mice immunized with OVA adjuvantized with LPS (unpublished data; the patent application no. P387319).
As EPS is able to inhibit humoral response and it is known that high levels of arthritogenic CII-specific IgG are crucial for the development of CIA, therefore, it was reasonable to address the issue whether EPS can inhibit the production of collagen-specific antibodies and ameliorate arthritis. In this study, we used two models of CIA, with the induction of either high or low levels of anti-collagen antibodies and a third model of arthritis induced by a passive transfer of anti-collagen antibodies together with LPS.
Materials and Methods
EPS Isolation
Exopolysaccharide was obtained from L. rhamnosus KL37C strain isolated from the feces of the human newborns as previously described (Lipiński et al. 2003). In brief, bacteria stored at −70 °C in MRS broth supplemented with 10 % glycerol were cultivated for 48 h in supplemented MRS liquid broth (Biocorp Polska, Warszawa, Poland) at 37 °C under anaerobic conditions. After centrifugation at 8,000 rpm (4 °C, 30 min), bacteria were washed twice with PBS, suspended in water (10 ml) and sonicated three times for 5 min, in an ice bath. Supernatant collected after the centrifugation at 6,000 rpm (30 min, 4 °C) was centrifuged twice at 12,000 rpm at 4 °C for 1 h and then precipitated with five volumes of cold ethanol (−20 °C, overnight). The precipitated material was recovered by centrifugation at 12,000 rpm, 4 °C for 20 min and freeze-dried. Finally, the material (polysaccharide) was passed through the gel filtration column in TSK HW-50 (1.6 × 100 cm) in 0.05 M aqueous pyridine acetate buffer (pH 5.6). The eluted fractions were monitored with a Knauer differential refractometer. The first fraction, which eluted in the void volume, contained polysaccharide (crude EPS) used in the present investigation.
Mice
Inbred DBA/1 male mice and CBA mice were bred in the Animal Breeding Unit, Department of Immunology of Jagiellonian University College of Medicine, Kraków. Mice were housed 4–5 per cage and maintained under clean conventional conditions with free access to standard rodent diet and water. Mice were used at 8–10 weeks of age. The authors were granted permission for this study by the Local Bioethical Committee. Experiments were conducted according to the ethical guidance of the Local Bioethical Committee.
Mice Immunization with OVA
Protocol 1 Mice were injected intraperitoneally with 200 μg OVA alone (n = 6) or with LPS (E. coli 011:B4; 1 μg/mouse; n = 6; both Sigma-Aldrich, Germany) or EPS (50 μg/mouse; n = 6). Thirty days after first immunization mice were boosted either with OVA (200 μg/mouse) alone or with OVA (200 μg/mouse) in the presence of LPS (1 μg/mouse) or EPS (50 μg/mouse). Seven days after second immunization, mice were bled and serum was prepared. Experiment was repeated three times.
Protocol 2 Mice were given an intraperitoneal injection of OVA (200 μg/mouse) in the presence of LPS (1 μg/mouse; n = 6) or/and EPS (50 μg/mouse; n = 6 each) twice on day 0 and 14. Seven days after the second immunization mice were bled and serum was prepared. Experiment was repeated at least four times.
Induction and Evaluation of CIA
Model 1 To induce CIA, DBA/1 mice were injected intraperitoneally with CII from chicken sternal cartilage (Sigma-Aldrich) (100 μg/mouse) in the presence of LPS (5 μg/mouse; n = 10–15) and/or EPS (200 μg/mouse; n = 10–15 and n = 4–6, respectively) on day 0, 14, 28, 42 and 56 (Fig. 1). The experiment was repeated three times.
CIA induction protocol: Model 1. DBA/1 mice were injected intraperitoneally (ip) with CII (100 μg/mouse) in the presence of LPS (5 μg/mouse) without (saline; n = 13) or with EPS (200 μg/mouse; n = 15) on day 0, 14, 28, 42 and 56. Mice were examined for the clinical symptoms of arthritis by visual observation and measurement of paw thickness to estimate the incidence and severity of CIA. At the end of the experiment (day 63), blood was collected and anti-CII antibodies (IgG, IgG1) were measured in individual mouse sera by ELISA
Model 2 DBA/1 mice were immunized subcutaneously with CII (200 μg/mouse) emulsified in Complete Freund’s Adjuvant (CFA; Sigma-Aldrich). Three weeks later (on day 21), mice received boost intraperitoneal injection of CII (100 μg/mouse) in the presence of LPS (5 μg/mouse). Starting from the day of boost immunization mice were given intraperitoneal injections of EPS (200 μg/mouse; n = 8–12) or saline (n = 8–12), three times a week till the end of the experiment. Last injection of EPS was done on day 41, 2 days before final evaluation of arthritis (Fig. 2). The experiment was repeated three times.
CIA induction protocol: Model 2. DBA/1 mice were immunized subcutaneously (sc) with CII (200 μg/mouse) in the presence of Complete Freund’s Adjuvant (CFA). Three weeks later, mice were given intraperitoneal (ip) boost injection of CII (100 μg/mouse) in the presence of LPS (5 μg/mouse; n = 8). Starting on the day of boost immunization (day 21) EPS (200 μg/mouse; n = 8) or saline (n = 8) was administered intraperitoneally three times a week till the end of the experiment (last injection of EPS was on day 41). Mice were examined for the symptoms of arthritis (CIA incidence) and severity of joint inflammation by visual observation and hind paws thickness measurement. At the end of the experiment (day 43), blood was collected and anti-CII antibodies (IgG, IgG1, IgG2a) were measured in individual mouse sera by ELISA
Model 3 DBA/1 mice were given intravenous injection of ArthritoMAB™ Arthritis Inducing Antibody Cocktail (MD Biosciences, Switzerland; 4 mg/mouse) followed with LPS (25 μg/mouse) administered 2 days later intraperitoneally (Nandakumar and Holmdahl 2005). EPS (300 μg/mouse; n = 6) or saline (n = 6) was injected intraperitoneally 2 days before, 2 days after and on the day of ArthritoMAB™ injection (day −2, 0, 2; Fig. 3). The experiment was repeated twice.
CIA induction protocol: Model 3. Arthritogenic monoclonal antibody cocktail (ArthritoMAB™; 4 mg/mouse) was injected intravenously (iv) to DBA/1 mice (day 0). Two days later, mice received intraperitoneal (ip) injection of LPS (25 μg/mouse). Saline (n = 6) or EPS (300 μg/mouse; n = 6) was injected intraperitoneally three times in total, on day −2 (two days before ArthritoMAB™ injection), 0 and 2. Mice were examined for the symptoms of arthritis (CIA incidence) and severity of joint inflammation by visual observation and hind paws thickness measurement
To evaluate CIA development, mice were examined visually every other day for the incidence and severity of arthritis (joint swelling and redness). According to the extent of erythema and edema of the periarticular tissues, the lesions of the four paws were each graded from 0 to 4 as follows: 0 = no swelling/normal, 1 = slight swelling of the limb or the single digits, 2 = moderate swelling/erythema of the limb and/or multiple digits, 3 = pronounced swelling and erythema, of the limb and multiple digits, 4 = severe swelling and erythema of the limb/digits and joint rigidity/deformity. The scores of all four paws were summed to yield arthritis (CIA) index (maximum 16 for each animal). Paw thickness (swelling of paws) was measured using Mitutoyo micrometer. To evaluate the level of anti-CII antibodies, the blood was collected from CIA-induced mice at the end of the experiments (day 63: model 1; day 43: model 2). Serum was prepared and stored at −20 °C until used.
Measurement of Serum Antigen-Specific Antibody Titers
Anti-OVA or anti-CII antibodies in serum were measured by sandwich ELISA as described previously (Kwaśny-Krochin et al. 2002). In brief, plates (Costar EIA/RIA plates, Corning Incorporated, USA) were coated with OVA (5 μg/ml) or native chicken CII (5 μg/ml) overnight. Serial dilutions of mouse serum in PBS were applied to antigen-coated wells for 1 h at room temperature followed by biotin-conjugated antibodies against IgG (Sigma-Aldrich), IgG1 (MP Biomedicals, USA) or IgG2a (Southern Biotech, USA). Horseradish peroxidase-conjugated streptavidin (Vector, USA) was used as detection reagent and developed using o-phenylenediamine dihydrochloride and hydrogen peroxide (both Sigma-Aldrich). The reaction was stopped with 3 M H2SO4 (POCH, Poland). The optical density of each sample was measured at 492 nm. 0.05 % Tween 20 (Sigma-Aldrich) in phosphate buffer was used as a washing solution. The antibody levels were expressed in arbitrary ELISA units calculated from anti-OVA or anti-CII immunoglobulin titer: 1 unit = 1/100 titer of immunoglobulin specific to OVA or CII.
Statistical Analysis
Statistical significance of differences between groups was analyzed using unpaired Student’s t test. Results are expressed as mean values ± SEM. A p value <0.05 was considered statistically significant. Analysis was performed using Microsoft Excel.
Results
The Effect of EPS on OVA-Specific Humoral Responses
In preliminary studies, the effect of EPS on in vivo antigen-specific antibody production, tested by measurement of serum concentration of anti-OVA IgG, was compared with that of LPS, a well-known bacterial stimulator of B cell proliferation. LPS markedly enhanced the production of OVA-specific IgG antibodies when injected with antigen during either the primary (Fig. 4a) or the secondary immunization (Fig. 4b). Unlike LPS, EPS did not act as an adjuvant when administered together with antigen (OVA), but rather diminished the production of antibodies induced by OVA (Fig. 4). Furthermore, EPS given with antigen and LPS abolished the adjuvant effect of LPS, and resulted in lower concentrations of OVA-specific IgG (Fig. 5). Similar suppressor effects of EPS on antigen-specific antibody production were observed when EPS and LPS were administered by different routes (data not shown).
The effect of EPS on the generation (a) and the stimulation (b) of OVA-specific memory cells. a CBA mice were immunized with 200 μg of OVA (white n = 6) together with LPS (1 μg/mouse; black n = 6) or EPS (50 μg/mouse; gray n = 6) administered intraperitoneally. Thirty days later, mice in all groups were boosted with OVA alone. b All mice were immunized with 200 μg of OVA alone and after 30 days mice received 200 μg of OVA (white n = 6) and LPS (1 μg/mouse; black n = 6) or EPS (50 μg/mouse; gray n = 6). Blood was collected 7 days after last immunization. The level of IgG specific to OVA in individual mouse sera was determined by ELISA. Data are expressed in arbitrary ELISA unit (1 U = 1/100 titer of anti-OVA IgG). Data shown are representative of two selected experiments. *p < 0.05; **p < 0.01; ***p < 0.001 (Student’s t test)
The effect of EPS on OVA-specific IgG production. CBA mice were given intraperitoneal injection of OVA (200 μg/mouse) alone (white n = 6) or in the presence of LPS (1 μg/mouse; black n = 6) or EPS (50 μg/mouse; gray n = 6) or both (hatched n = 6) twice, on day 0 and 14. Blood was collected 7 days after boost immunization. The level of IgG specific to OVA in individual mouse sera was determined by ELISA. Data from one representative experiment are expressed in arbitrary ELISA unit (1 U = 1/100 titer of anti-OVA IgG). **p < 0.01; ***p < 0.001 (Student’s t test)
The Effect of EPS on the Development of CIA and the Production of CII-Specific IgG (Model 1)
Immunization of DBA/1 mice with CII and LPS resulted in elevated concentration of serum IgG-specific to CII, especially of IgG1 subclasses (Fig. 6). As anti-CII antibodies are essential for the development of CIA (Williams et al. 1998), the serum level of IgG to CII was measured in each mouse individually and was analyzed along with the clinical symptoms of arthritis. In this experimental model of CIA, the effectiveness of induction of joint inflammation was low. The repeated administration of collagen and LPS (5 times) induced mild arthritis (mean arthritic score 4–6) with relatively low incidence (approximately 50 %) (Fig. 7), correlated with a moderate increase in titer of collagen-specific antibodies (Fig. 6). Interestingly, mice immunized with CII and EPS, without any adjuvant, showed extremely low serum levels of collagen-specific antibodies (Fig. 6) and no signs of arthritis (not shown). When mice immunized with CII and LPS were treated with EPS, the serum level of total IgG and IgG1-specific to CII was significantly reduced (Fig. 6). Reduction in antibody was associated with strong inhibition of arthritis. None of the EPS-treated mice developed clinical signs of CIA within the time frame of the experiment (up to day 55; Fig. 7).
The effect of EPS on collagen-specific antibody production (Model 1). DBA/1 were mice immunized in the presence of LPS (black bars n = 13) and/or with EPS (hatched n = 15/gray bars n = 4, respectively). Mice were bled on day 63 (the end of the experiment). Anti-CII IgG (a) and IgG1 (b) were measured in individual mouse sera by ELISA. ***p < 0.001 (Student’s t test)
The effect of EPS on the development of CIA (Model 1). DBA/1 were mice immunized in the presence of LPS without (closed triangles n = 13) or with EPS (open circles n = 15). The symptoms of arthritis (CIA incidence) (a) and severity of joint inflammation (mean arthritis score) (b) were evaluated by visual observation. Data from one representative out of three experiments are shown. *p < 0.05; **p < 0.01; ***p < 0.001 (Student’s t test)
The Effect of EPS on the Development of CIA and the Production of CII-Specific IgG (Model 2)
To examine if EPS has the ability to ameliorate severe arthritis, we immunized DBA/1 mice with CII and CFA, followed by an administration of CII with LPS 3 weeks later. In this model, the incidence (~80 %) and the severity of arthritis (mean arthritis score ~10) were close to those observed previously in a classical model of CIA (mice immunized with CII + CFA twice) (Kwaśny-Krochin et al. 2002; Marcinkiewicz et al. 2007b). As shown in Fig. 8, the serum concentration of anti-CII IgG was very high. The concentration of total anti-CII IgG was fourfold higher than that observed in the model 1. EPS inhibited the production of CII-specific IgG. The serum level of both measured subclasses of IgG, namely IgG1 and IgG2a, was strongly reduced. Nevertheless, EPS did not affect the serum level of anti-CII IgM (not shown). Moreover, in contrast to the model 1, EPS only slightly reduced incidence and severity of CIA between days 28 and 36 (Fig. 9).
The effect of EPS on collagen-specific antibody production (Model 2). Saline (black bars n = 8) or EPS (hatched bars n = 8) was given to DBA/1 mice intraperitoneally. Blood was collected at the end of the experiment (day 43). Collagen-specific antibodies: IgG, IgG1, IgG2a were measured in serum by ELISA. Data from one representative (out of three) experiment are expressed in arbitrary ELISA unit (1 U = 1/100 titer of anti-CII antibodies). *p < 0.05; **p < 0.01 (Student’s t test)
The effect of EPS on the development of CIA (Model 2). Saline (closed triangles n = 8) or EPS (open circles n = 8) was given to DBA/1 mice intraperitoneally. Mice were examined for the symptoms of arthritis (CIA incidence) (a) and severity of joint inflammation (mean arthritis score) (b). Hind paws thickness was measured every 2–3 days (untreated mice: closed diamonds; n = 5) (c). *p < 0.05 (Student’s t test)
The Effect of EPS on the Development of Arthritis Induced by mAb Specific to CII and LPS (Model 3)
Finally, we examined the effect of EPS on the development of arthritis induced by intravenous administration of monoclonal antibodies specific to CII followed by administration of a high dose of LPS (25 μg/mouse; Fig. 3). In this model, onset of arthritis was observed on day two with 100 % incidence. EPS treatment did not prevent the development of arthritis. Although EPS did not affect the final incidence of CIA, the onset of symptoms of arthritis in mice treated with EPS was delayed when compared with a reference group. Moreover, the severity of joint inflammation (CIA index, paw thickness) was reduced when mice were given EPS (Fig. 10).
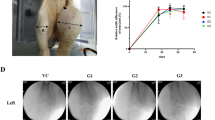
The effect of EPS on the development and severity of CAIA (collagen-antibody-induced arthritis) (Model 3). Saline (closed triangles n = 6) or EPS (300 μg/mouse; open circles n = 6) was given to CAIA-induced DBA/1 mice intraperitoneally. Mice were examined for the symptoms of arthritis (CIA incidence = 100 % on day 2) and severity of joint inflammation: mean arthritis score (a), hind paws thickness (b). *p < 0.05; ***p < 0.001 (Student’s t test)
Discussion
The studies described above document the effects of systemic administration of bacterial EPS on the development of CIA in DBA/1 mice. We have examined EPS derived from L. rhamnosus KL37, an EPS of known chemical structure (Lipiński et al. 2003). Recent experiments in our laboratory demonstrated that L. rhamnosus KL37-derived EPS affects the production of a variety of mediators by peritoneal macrophages (Ciszek-Lenda et al. 2011). We have also found that EPS strongly suppresses OVA-specific humoral response in mice (unpublished data). In addition, it has been reported that oral administration of live L. rhamnosus and L. casei strains suppresses various types of arthritis, including CIA in mice and rats (Sheil et al. 2004). These data, along with studies demonstrating amelioration of experimental colitis by EPS-producing lactobacilli (Şengül et al. 2006), suggested that EPS might have anti-arthritogenic potential.
In the present study, we have shown for the first time the ability of lactic bacteria EPS to attenuate the clinical symptoms of CIA. Interestingly, a protective effect of EPS administration was observed in mice that received an arthritogenic inoculum containing collagen (CII) and LPS, and this effect was associated with a strong reduction in titer of CII-specific IgG antibodies. Different mechanisms have been proposed to explain the lactobacilli-dependent amelioration of arthritis. These include inhibition of pro-inflammatory mediators (cytokines, prostaglandins) and modulation of collagen-specific humoral or cell-mediated immune responses (Amdekar et al. 2011; Kato et al. 1998). Little is known, however, about the immunoregulatory properties of lactobacilli EPSs, the major components of bacterial biofilm. Oral administration of EPSs resulted in enhanced production of IgA in gut-associated lymphoid tissue (GALT) (Vinderola et al. 2006). In contrast, a consistent finding of the present study is a suppressive activity of EPS on humoral responses, after systemic administration to immunized mice. EPS in two unrelated antigen systems (OVA, CII) significantly inhibited the production of immunoglobulins, as measured by serum concentrations of circulating antigen-specific antibodies. In an OVA model, EPS inhibited the production of IgG, the predominant immunoglobulin isotype of the secondary humoral response. Interestingly, co-administration of EPS and LPS abolished the adjuvant activity of the latter. Similar effects were observed when EPS and LPS were administered by different routes. Therefore, it is unlikely that EPS alters antigen processing and interferes with LPS action at the level of antigen-presenting cells. Rather, seems more likely that the observed “anti-adjuvant” effect of EPS may be caused by neutralization of the stimulatory effect of LPS on B cells. It is well documented that LPS activates B cells for enhanced production of antibodies, triggers secretion of various kinds of mediators from inflammatory cells and acts also as an adjuvant to induce autoimmune arthritis (Cavallo and Granholm 1990; Yoshino et al. 2000). Nevertheless, the precise molecular mechanism of inhibition of humoral response by the systemic administration of EPS remains unknown.
The suppressive potential of EPS on the antigen-specific humoral response demonstrated in OVA system was confirmed in experimental models of type II CIA. The effect of EPS on the production of anti-CII IgG, IgG1 and IgG2a antibodies and on the development of CIA was examined, and the results from different experimental models were compared. The EPS treatment reduced significantly the serum levels of IgG antibody to CII in both active immunization models of CIA. The reduction of the CII-specific humoral response was accompanied by a reduced development of CIA. The amelioration of arthritis by EPS was most pronounced when mice were immunized with CII and LPS (model 1). The serum level of CII-specific IgG in this experimental model was markedly lower than in the model in which strong adjuvant (CFA) was used during the primary immunization (model 2). From these findings, we hypothesize that the EPS-dependent reduction of anti-collagen antibodies could result in inhibition of the development of CIA in DBA/1 mice. Indeed, there are many studies showing a close link between humoral responses to collagen and disease severity (Marcinkiewicz et al. 2007b; Nandakumar et al. 2003; Nowak et al. 2010; Williams et al. 1998). In our experimental set-up, the protective effects of EPS in model 1 of CIA were stronger than in model 2, perhaps because of the very high serum levels of CII-specific antibodies after using CFA as an adjuvant. This interpretation is supported by the results from model 3, in which acute arthritis is induced by passive administration of massive amounts of anti-CII IgG2a monoclonal antibodies. In this model EPS only slightly and temporarily ameliorated arthritis, suggesting that EPS acts predominantly via modulation of active immunization. To explain mechanisms of EPS activities, studies on the effect of highly purified EPS on secretory properties of immune cells are being carried out in our laboratory.
In general, investigations on microbial long polysaccharide molecules (including EPS) are at the preliminary stage. Although the number of reports showing immuno-modifying activity of microbial polysaccharides is growing, the underlying mechanism remains unclear. Polysaccharide molecules of pathogenic bacteria shield other cell surface molecules and prevent them from interacting with host pattern recognition receptors (PRRs). Probiotic bacteria polysaccharides might also shield other cell surface molecules as shown for L. rhamnosus GG polysaccharide (Lebeer et al. 2009). The direct interaction of microbial polysaccharides with PRRs or co-receptors cannot be excluded. It has been shown that polysaccharide A of Bacterioides fragilis activates NF-κB signaling and cytokine production in dendritic cells by Toll-like receptor 2-dependent mechanism modulating antigen presentation and CD4+ T cell activation (Mazmanian et al. 2005). EPS used in our study refers to a crude EPS and as a component of bacterial biofilm may contain small amounts of other molecules, e.g. DNA. Therefore, it is very difficult to speculate, which receptor, if any, might be responsible for immunoregulatory activities of EPS.
In conclusion, systemic administration of EPS resulted in amelioration of active CIA that was associated with reduced production of CII-specific antibodies. The strongest effects of EPS were observed in a model of mild CIA, in which production of anti-CII antibodies was moderate. Therefore, EPS derived from L. rhamnosus KL 37 shows promising suppressive and anti-arthritogenic properties. As the beneficial effect was most pronounced when EPS neutralized the arthritogenic activity of LPS, EPS may have therapeutic potential in arthritis induced or exacerbated by Gram-negative bacterial infections. The biological effects of probiotic bacteria are strongly strain specific (Marcinkiewicz et al. 2007a), so further studies with highly purified EPSs derived from other lactobacilli strains are necessary. Our results may open new strategies for probiotic therapies in autoimmune diseases such as arthritis.
References
Amdekar S, Singh V, Singh R et al (2011) Lactobacillus casei reduces inflammatory joint damage associated with collagen-induced arthritis (CIA) by reducing the pro-inflammatory cytokines: Lactobacillus casei:COX-2 inhibitor. J Clin Immunol 31:147–154
Aoki S, Yoshikawa K, Yokoyama T et al (1996) Role of enteric bacteria in the pathogenesis of rheumatoid arthritis: evidence for antibodies to enterobacterial common antigens in rheumatoid sera and synovial fluids. Ann Rheum Dis 55:363–369
Baharav E, Mor F, Halpern M et al (2004) Lactobacillus GG bacteria ameliorate arthritis in Lewis rats. J Nutr 134:1964–1969
Cavallo T, Granholm NA (1990) Lipopolisaccharide from Gram-negative bacteria enhances polyclonal B cell activation and exacerbates nephritis in MLR/lpr mice. Clin Exp Immunol 82:515–521
Ciszek-Lenda M (2011) Biological functions of exopolysaccharides from probiotic bacteria. Centr Eur J Immunol 36:51–55
Ciszek-Lenda M, Nowak B, Śróttek M et al (2011) Immunoregulatory potential of exopolysaccharide from Lactobacillus rhamnosus KL37: effects on the production of inflammatory mediators by mouse macrophages. Int J Exp Pathol 92:382–391
Courtenay JS, Dallman MJ, Dayan AD et al (1980) Immunization against heterologous type II collagen induces arthritis in mice. Nature 283:666–668
Detert J, Pischon N, Burmester GR et al (2010) The association between rheumatoid arthritis and periodontal disease. Arthritis Res Ther 12:218–224
Flemming HC, Neu TR, Wozniak DJ (2007) The EPS matrix: “house of biofilm cells”. J Bacteriol 198:7945–7947
Hida S, Nagi-Miura N, Adachi Y et al (2006) Beta-glucan derived from zymosan acts as an adjuvant for collagen-induced arthritis. Microbiol Immunol 50:453–461
Kano H, Kaneko T, Kaminogawa S (2002) Oral intake of Lactobacillus delbrueckii subsp. bulgaricus OLL1073R-1 prevents collagen-induced arthritis in mice. J Food Prot 65:153–160
Kato I, Endo-Tanaka K, Yokokura T (1998) Suppressive effects of the oral administration of Lactobacillus casei on type II collagen-induced arthritis in DBA/1 mice. Life Sci 63:635–644
Kwaśny-Krochin B, Bobek M, Kontny E et al (2002) Effect of taurine chloramine, the product of activated neutrophils, on the development of collagen-induced arthritis in DBA/1 J mice. Amino Acids 23:419–426
Lebeer S, Verhoeven TL, Francius G et al (2009) Identification of a gene cluster for the biosynthesis of a long galactose-rich exopolysaccharide in Lactobacillus rhamnosus GG and functional analysis of the priming glycosyltransferase. Appl Environ Microbiol 75:3554–3563
Lipiński T, Jones C, Lemercinier X et al (2003) Structural analysis of the Lactobacillus rhamnosus strain KL37C exopolysaccharide. Carbohydr Res 338:605–609
Marcinkiewicz J, Ciszek M, Bobek M et al (2007a) Differential inflammatory mediator response in vitro from murine macrophages to lactobacilli and pathogenic intestinal bacteria. Int J Exp Pathol 88:155–164
Marcinkiewicz J, Głuszko P, Kontny E et al (2007b) Is Taurolidine a candidate for treatment of rheumatoid arthritis? Clin Exp Rheumatol 25:211–218
Mazmanian SK, Liu CH, Tzianabos AO et al (2005) An immunomodulatory molecule of symbiotic bacteria directs maturation of the host immune system. Cell 122:107–118
Myhre AE, Aasen AO, Thiemermann C et al (2006) Peptidoglycan—an endotoxin in its own right? Shock 25:227–235
Nandakumar KS, Holmdahl R (2005) Efficient promotion of collagen antibody induced arthritis (CAIA) using four monoclonal antibodies specific for the major epitopes recognized in both collagen induced arthritis and rheumatoid arthritis. J Immunol Methods 304:126–136
Nandakumar KS, Svensson L, Holmdahl R (2003) Collagen type II-specific monoclonal antibody-induced arthritis in mice. Am J Pathol 163:1827–1837
Navarra S (2007) Role of infectious agents in autoimmunity. Fut Rheumatol 2:321–328
Nowak B, Głuszko P, Ciszek-Lenda M et al (2010) High-dose methotrexate ameliorates collagen-induced arthritis but does not inhibit the release of proinflammatory cytokines by peritoneal macrophages in mice. Centr Eur J Immunol 35:128–137
Oestergaard S, Rasmussen KE, Doyle N et al (2008) Evaluation of cartilage and bone degradation in murine collagen antibody-induced arthritis model. Scan J Immunol 67:304–312
Şengül N, Aslím B, Uçar G et al (2006) Effects of exopolysaccharide-producing probiotic strains on experimental colitis in rats. Dis Colon Rectum 49:250–258
Seo HS, Michalek SM, Nahm MH (2008) Lipoteichoic acid is important in innate immune response to Gram-positive bacteria. Infect Immun 76:206–213
Sheil B, McCarthy J, O’Mahony L et al (2004) Is the mucosal route of administration essential for probiotic function? Subcutaneous administration is associated with attenuation of murine colitis and arthritis. Gut 53:694–700
Simelyte E, Isomäki P, Rimpiläinen M et al (2001) Cytokine production in arthritis susceptible and resistant rats: a study with arthritogenic and non-arthritogenic Lactobacillus cell walls. Scand J Immunol 53:132–138
Simelyte E, Rimpiläinen M, Zhang X et al (2003) Role of peptidoglycan subtypes in the pathogenesis of bacterial cell wall arthritis. Ann Rheum Dis 62:976–982
So JS, Kwon HK, Lee CG et al (2008a) Lactobacillus casei suppresses experimental arthritis by down-regulating T helper 1 effector functions. Mol Immunol 45:2690–2699
So JS, Lee CG, Kwon HK et al (2008b) Lactobacillus casei potentiates induction of oral tolerance in experimental arthritis. Mol Immunol 46:172–180
Stephani J, Radulivic K, Niess JH (2011) Gut microbiota, probiotics and inflammatory bowel disease. Arch Immunol Ther Exp 59:161–177
Vinderola G, Perdigón G, Duarte J et al (2006) Effects of the oral administration of the exopolysaccharide produced by Lactobacillus kefiranofaciens on the gut mucosal immunity. Cytokine 36:254–260
Vu B, Chen M, Crawford RJ et al (2009) Bacterial extracellular polysaccharides involved in biofilm. Molecules 14:2535–2554
Williams PJ, Jones RH, Rademacher TW (1998) Correlation between IgG anti-type II collagen levels and arthritic severity in murine arthritis. Autoimmunity 27:201–207
Williams RO (2004) Collagen-induced arthritis as a model for rheumatoid arthritis. Methods Mol Med 98:207–216
Yoshino S, Ohsawa M (2000) The role of lipopolysaccharide injected systematically in the reactivation of collagen-induced arthritis in mice. Br J Pharmacol 129:1309–1314
Yoshino S, Sasatomi E, Ohsawa M (2000) Bacterial lipopolysaccharide acts as an adjuvant to induce autoimmune arthritis in mice. Immunology 99:607–614
Acknowledgments
The authors thank Prof. Benjamin Chain, University College London, for general help in the preparation of this manuscript for publication. This study was supported by Jagiellonian University College of Medicine grant No. K/ZDS/000678 and the Ministry of Science and Higher Education (Poland) grant No. N N401 042438.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Nowak, B., Ciszek-Lenda, M., Śróttek, M. et al. Lactobacillus rhamnosus Exopolysaccharide Ameliorates Arthritis Induced by the Systemic Injection of Collagen and Lipopolysaccharide in DBA/1 Mice. Arch. Immunol. Ther. Exp. 60, 211–220 (2012). https://doi.org/10.1007/s00005-012-0170-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00005-012-0170-5