Abstract
Mental disorders are closely related to deficits in cognitive control. Such cognitive impairments may result in aberrations in mood, thinking, work, body functions, emotions, social engagements and general behaviour. Mental disorders may affect the phenotypic behaviour like eye movements, facial expressions and speech. Furthermore, a close association has been observed within mental disorders and physiological responses emanating from the brain, muscles, heart, eyes, skin, etc. Mental disorders disrupt higher cognitive function, social cognition, control of complex behaviours and regulation of emotion. Cognitive computation may help understand such disruptions for improved decision-making with the help of computers. This study presents a systematic literature review to promulgate state of art computational methods and technologies facilitating automated detection of mental disorders. For this survey, the relevant literature between 2010 and 2021 has been studied. Recommendations of Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) model were adopted for identification, screening, validating and inclusion of research literature. The self-diagnosis tools for detection of mental disorders like questionnaires and rating scales are inconsistent and static in nature. They cannot encompass the diversity of mental disorders, inter-individual variability and impact of emotional state of an individual. Furthermore, there are no standard baselines for mental disorders. This situation mandates a multi-faceted approach which may utilise data from physiological signals, behavioural patterns and even data obtained from various online portals like social media to efficiently and effectively detect the prevalence, type and severity of mental disorders.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Cognitive computing promulgates the development of computer systems which can model human behaviours like perception, attention and thoughts. Cognitive computing systems can collect and process individual, social and healthcare data for better disease diagnosis and patient engagement. It offers a combination of multidisciplinary technologies like artificial intelligence, deep learning, machine learning, big data analytics and natural language processing systems to identify types and symptoms of a disease. A mental disorder is a medical condition that influences the normal behaviour of a person. A mental disorder may impair the physical, emotional and social well-being of a person. Impairment to memory, attention and cognitive control is fundamental to any mental disorder. Furthermore, it may result in aberrations in mood, thinking, work, body functions, emotions, social engagements and general behaviour either once, recurrently or even permanently. Researchers have reported more than four hundred and fifty types of mental disorders with discrete symptoms. Few of the prominent mental disorders are depressive disorder, mood disorder, personality disorder, addictive disorder, sleep disorder, post-traumatic disorders, dementia, bipolar disorder and schizophrenia along with stress and anxiety disorders [1].
More than 10.7% of the world’s population is suffering from aforementioned mental disorders, most prominent being depression and anxiety which add more than 548 million to the global burden of the diseases [2, 3]. The repercussions of mental disorders are diverse, including but not limited to low employee productivity, high suicide rates, early mortality, dangerous driving, early dropping out of education, poverty, disability, physical pain and being prone to other diseases like infections and cardiovascular diseases [4,5,6,7,8,9]. The prevalence of mental disorders also leads to loss of economic growth and places a burden on the economic well-being of the patient as well as the caregivers [10]. This makes early detection of mental disorders imperative not just for health but also for development. This has led to the inclusion of mental health as one of the targets in Goal 3 of United Nations Sustainable Development Goals [11]. Subsequently, research community has laid emphasis on early detection of mental disorders in order to deploy suitable therapeutic measures.
Clinical assessment methods for detecting mental disorders rely on patients’ self-reporting and the expertise of the examiner. These methods lack precision due to social stigma, lack of knowledge, subjective bias of the examiner, time-intensive nature of the examination and lack of consistency [12]. To eliminate subjective bias and to reduce examination time, different rating scales for measuring mental disorders have been developed. These scales are used to measure the severity of the mental disorder as a function of perceived symptoms as inferred from the assessee [13,14,15]. However, the rating scales have some inherent limitations; they are inconsistent in handling the heterogeneous nature of mental disorders and results obtained from different scales are different. The rating scale cannot encompass all the symptoms associated with a particular disorder and they did not take into consideration the effects of examination environment, emotions and demographics in the rating scales [16].
This has led to exploration of novel detection techniques which could handle the heterogeneous nature of the mental disorders, eliminate subjective bias and include the effects of emotions along with demographics like age and gender on detection mechanism. As a result, mental disorder detection techniques based on machine learning and biomarkers have emerged. It is because human cognition is closely associated with the biological processes of an individual. The electrical activity of the nervous system controls almost every aspect of the human body including heart signals, sweat glands and even human cognition. Thus, any changes in human mental states like mood changes, emotional changes or mental disorders may greatly affect the activity of the brain, heart, skin, facial expressions, speech and even other biological processes like respiration and temperature. Various research studies have shown that the activity and power of different EEG bands, inter-hemispheric symmetry and statistical features like peak, variance, entropy and energy are contrasting between healthy individuals and people suffering from mental disorders. For example, depressed persons have increased beta values in their brain waves as compared to healthy persons [17,18,19,20,21,22]. Similarly, there is a difference in statistical features of heart rate variability and other ECG characteristics like peak and median frequency of healthy and non-healthy individuals [23,24,25,26,27,28]. The skin conductance response and statistical characteristics of electrodermal activity are also different for healthy and non-healthy individuals [29,30,31]. Electromyography (EMG) is a procedure to measure muscle movements and motor neuron activity. It has been observed that mental stress may result in a different EMG activity in healthy and non-healthy individuals [32,33,34]. Recent studies also investigated correlation between mental disorders and eye movements [35,36,37,38]. This has led to exploration of objective methodologies which aim to automatically decipher human cognition by machine learning with the help of biological signals of an individual. Table 1 highlights different cognitive tasks that are related to different biological processes.
Modalities like EEG, GSR, EMG, ECG, facial expressions, eye movements, online handwritten signals and speech can facilitate extraction of prominent features to be used as biomarkers. Such biomarkers could further be used for automatic detection of mental disorders using machine learning algorithms. In reference to the previously stated arguments, a systematic literature review is required to promulgate state of art research contributions in this domain. Furthermore, it may help contemporary researchers to investigate numerous multidisciplinary open research problems from the amalgamation of psychology, sociology, machine learning, computer science and behavioural sciences. The following research questions were formulated to attain the goal of this study:
-
1.
Which physiological and behavioural modalities can facilitate the detection of mental disorders using machine learning?
-
2.
Which prominent features of these modalities can be used in detection of mental disorders using machine learning?
-
3.
Which are the most suited machine learning algorithms to exploit these modalities for detecting mental disorders?
-
4.
What are the prominent challenges in detection of mental disorders using biomarker modalities?
The rest of this manuscript is organised as follows: the “Survey Methodology” section elaborates the adopted methodology and the novelty of this survey in comparison to previously published literature, the “Different Approaches of Mental Disorder Detection” section provides a discussion on different modalities used to detect mental disorders, the “Discussion” section offers a summarisation of most prominent features and most suited machine learning algorithms to detect mental disorders using these modalities and the “Research Challenges” section concludes contemporary research gaps, key findings and research challenges.
Survey Methodology
This section elaborates the adopted methodology for conducting the systematic literature survey. For this survey, the relevant literature from 2010 to 2021 has been studied based on the previously stated research questions. Recommendations of Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) model were adopted for identification, screening, validating and inclusion of research literature as shown in Fig. 1 [55]. The articles were searched using keywords like detection + mental disorders, analysis + mental disorders, prediction + mental disorders, identification + mental disorders, modalities + mental disorders, machine learning + mental disorders, physiological signals + mental disorder and verbal and non-verbal behaviour, from databases like ScienceDirect, IEEEXplore, SpringerLink, ACM Digital Library, Taylor & Francis Online and Wiley Online Library. Pre-screening exclusion was done based on duplication and article language. Articles published in English language were only considered for screening. Screening and exclusion were based on the relevance to the survey as inferred from the title, abstract and conclusion of the article. Post-screening exclusion of articles was based on user-defined inclusion criteria like articles should have a minimum of five citations per year and should be published in 2010 or later.
Mendeley was used for aggregation, filtering and removal of articles to build a consolidated library of relevant research articles.
Numerous surveys on detection of mental disorders using physiological and behavioural patterns have been published in recent past. During literature evaluation, it was observed that existing literature is primarily investigating one mental disorder based on a single modality. To the best of our knowledge, multiple physiological signals along with behavioural patterns for detection of mental disorders using machine learning techniques have not been explored to the desired extent. Table 2 offers a comparison of existing literature with this survey:
Different Approaches of Mental Disorder Detection
Physiological signals and human behaviour provide various biomarkers with respect to different mental states and disorders. These signals or behavioural aspects are called modalities. Data from these modalities can be used in the detection of mental disorders. Features from multiple modalities in collaboration with machine learning algorithms can be used to determine the prevalence, type and severity of mental disorders. A modality can be used either as unimodal or multimodal approach. Types and usage of unimodal and multimodal approaches are detailed as under:
Unimodal Approach
In unimodal approach, a single modality is used as a standalone differentiator for classification. Various modalities have been used in unimodal approach for detection and classification of mental disorders, mood changes and emotional states of an individual. The following subsections provide an overview of contemporary works which have utilised a single modality for detection or prediction of mental disorder type or severity.
Electroencephalogram (EEG)
EEG captures the brain waves corresponding to different activities happening within the central nervous system. It is acquired through electrodes placed on the scalp. Different features of EEG in time domain and frequency domain can be extracted to analyse the type of signal. Most prominent features include statistical features in time and frequency domain such as mean, median, variance, standard deviation, skewness and kurtosis along with time-domain features like peak amplitude and energy. Frequency-domain features include different frequency bands in EEG signals like delta, theta, alpha, beta and gamma. The features of EEG signals have been classified using machine learning methods to detect different mental disorders. Table 3 provides an overview of research studies which have explored the use of only EEG signals in detection of mental disorders.
Electrodermal Activity (EDA) or Galvanic Skin Response (GSR)
EDA or GSR refers to the electrical response of human skin with respect to variation in sweat secretion. It is expressed in terms of Skin Conductance Response (SCR) and Skin Conductance Level (SCL). The changes in electrodermal activity due to any mental disorder or during a mental stress task are a potential biomarker of mental disorders. Table 4 provides an overview of research studies which have explored the use of EDA or GSR signals for detection of mental disorders.
Electrocardiogram (ECG)
Electrocardiogram captures the electrical activity in the heart. It is composed of a P-Wave followed by a QRS Complex which is followed by a T-Wave. The peak of the signal is the R of the QRS complex. The time between two successive R peaks is referred to as RR interval. Since the brain modulates the electrical activity of the human body, hence the ECG of an individual also reflects the changes in mental state. Different features of ECG have been used with machine learning algorithms to discriminate between normal and aberrated ECGs and therefore can be utilised for automatic detection of mental disorders. Prominent features include statistical measures like mean, median and standard deviation as well as other features like heart rate variability (HRV), root mean sum of squares of differences between normal to normal beat intervals (RMSSD), proportion of successive normal to normal beat intervals that differ more than k ms (pNNk), standard deviation of successive differences (SDSD), low-frequency band (LF), high-frequency band (HF) and ratio of LF to HF. Table 5 provides an overview of research studies which have explored the use of ECG signals only in detection of mental disorders.
Verbal and Non-verbal Behaviour
Verbal and non-verbal behaviour is closely correlated with physical, mental and emotional state of an individual. Any mental impairment or emotional change reflects in the behaviour of an individual. The analysis of changes in facial expressions, eye movements and speech in the presence of unfavourable mental states can provide biomarkers for mental disorder detection. Table 6 provides an overview of research studies which have explored the use of human behaviour in detection of mental disorders.
Online Handwritten Signals
The exploration of novel bias-free methods for detection of mental disorders has led to research in various newer paradigms; with online handwritten signals being a prominent one. The benefits of this approach are that handwriting is a common daily task and does not need any specialised training for participants. As can be seen in Table 7, various studies have explored the use of online handwritten signals related to time, space and pressure in the field of sentiment analysis, emotion recognition and by extension mental disorder detection.
Multimodal Approach
In multimodal approaches, two or more modalities are used for detecting mental disorders. There are two prominent approaches for fusion of multiple modalities—feature level fusion and decision level fusion. In feature level fusion, the features from multiple modalities are collected to form a single feature-set. A single classifier is then run on this feature-set to make decisions. On the other hand, in decision level fusion, multiple classifiers are run independently on feature-sets of individual modalities. The results of these multiple classifiers are then studied to form a single decision. Table 8 provides an overview of research studies which have adopted a multimodal approach and used more than one biological signal in detection of mental disorders.
Discussion
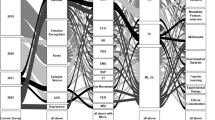
This section discusses the various findings obtained after extensive analysis of selected literature. Various findings obtained from the survey are discussed in the following subsections. As stated in the “Different Approaches of Mental Disorder Detection” section, physiological signals like EEG, GSR, ECG and EMG and behavioural patterns like handwriting, speech, eye movements and facial expressions have been extensively used for detection of mental disorders like depression, schizophrenia, bipolar disorder and mental stress. Table 9 provides a summary of different studies that have been discussed. The table shows the correlation between mental disorder studied, modalities used for detection and associated machine learning algorithms.
Different Biomarkers Used in Mental Disorder Detection
The different modalities used in mental disorder detection are EEG, ECG, EDA/GSR, EMG, eye movements, speech, online handwritten signals and facial expressions. Figure 2 illustrates the use of different modalities in detecting mental disorders using machine learning. It can be inferred that in the selected corpus of related research studies, physiological signals like EEG, ECG and GSR have been most popular amongst researchers while behaviour-based modalities such as speech, facial expressions and eye movements have been explored less often. It has been observed that almost 31% of the publications opted for EEG as a modality while ECG and GSR were preferred by 25% and 19% of researchers respectively. On the contrary, facial expressions and speech have been recommended by just 8% of the total research publications. One reason for this can be that behaviour of a person is voluntary and can be controlled by the person, thereby not revealing the true results [106,107,108]. Second reason can be that the experimental environment can change the normal behaviour of the person [109]. Another reason can be that behavioural changes vary to a great extent between individuals and can be subjective [110]. Still, research studies indicate that behavioural modalities provide important insights into mental disorder detection.
Features Used in Mental Disorder Detection
Table 10 provides an overview of the most prominent features of physiological and behavioural signals used along with detailing the type of mental disorder they have been used for.
Prominent Machine Learning Algorithms Employed in Mental Disorder Detection
The research studies included in the selected corpus have used different algorithms with various biomarkers for automatic classification and detection of mental disorders. However, the prominent ones are Support Vector Machines, k-nearest neighbour, Logistic Regression, Decision Trees, Naïve Bayes, Linear Discriminant Analysis, Random Forest, Artificial Neural Networks and CNN. As seen in Fig. 3, amongst the selected corpus of articles, SVM has been used about 24% of the times with k-nearest neighbour, Logistic Regression, Decision Trees and Naïve Bayes algorithms with around 8–10% usage. This can be due to the fact that SVM provides a fine balance between complexity and performance and therefore has been used as a baseline in most of the research studies. Also, Artificial Neural Network–based algorithms have been collectively used by about only 17% of the studies despite their high efficiency. Also, some algorithms like AdaBoost, Bayes Net, Radial Basis Function Network, Quadratic Discriminant Analysis, Partial Least Square, Gradient Boost and Gaussian Mixture Model have been used very sparsely as seen in Fig. 3 because of their high complexity when dealing with multi-feature data.
Research Challenges
The traditional methods of mental disorder detection like questionnaires rely on information provided by the individual. Besides being static in nature, these methods also cannot effectively verify the authenticity of the collected data. Hence, robust methods are required to identify or correct fabricated or tampered data. The research community has recommended the use of biomarkers related to various physiological and behavioural modalities like EEG, GSR, EMG, ECG, facial expressions, eye movements and speech for detection of mental disorders. While these approaches are objective in nature, behaviour can be faked or controlled by an individual. An individual who is conscious can easily manipulate his or her facial expressions, speech and eye movements. This mandates the requirement of methods, which can segregate genuine and controlled behaviour. Furthermore, emotional state of an individual plays a major role in the collection of data that has originated from human response, be it physiological or behavioural in nature [111]. Therefore, it becomes important to incorporate the effect of emotions on signals and further onto the analysis. Investigating this entire domain from the purview of decision intelligence may open numerous different research tracks related to mental health and diagnosis. Quantification of emotive feedback of respondents is also a major challenge for limited experimentation to diagnose mental disorders through facial expressions. Also, physiological responses vary between individuals due to human morphology and demographic factors like gender, race and age [112]. This variability needs to be managed to produce efficient and usable results. Furthermore, the experimental setups mentioned in the literature surveyed are inconsistent. For instance, different studies have mentioned different upper or lower bandwidths for frequency bands of EEG and ECG signals. Furthermore, the results obtained depend hugely on what features have been selected and which algorithm has been implemented. The selection of features-algorithms pair should be optimum to attain best results. Furthermore, collecting data from individuals suffering from mental disorders presents an ethical challenge [113]. That could be the reason for limited availability of standardised and annotated publicly available datasets pertaining to mental disorders.
Conclusion
Mental disorders are one of the leading contributors to global burden of diseases. They are one of the emerging challenges of the society. They can lead to lack of attention at work, dropping out of education, bad social behaviour and even suicide. So, there is a need for self-diagnostic methods which can automate the detection of mental disorders. The self-diagnosis tools for detection of mental disorders like questionnaires and rating scales are inconsistent and static in nature. They cannot encompass the diversity of mental disorders, inter-individual variability and impact of emotional state of an individual. Furthermore, there are no standard baselines for mental disorder datasets available. Stress of one person can be anxiety for another person and even depression for a third person. Hence, a multi-faceted approach is recommended where one can utilise data from physiological signals, behavioural patterns and even data obtained from various online portals like social media to efficiently and effectively detect the prevalence, type and severity of mental disorders.
References
Mental disorders: MedlinePlus. https://medlineplus.gov/mentaldisorders.html (accessed 07 Mar 2022).
Ritchie H, Roser M. Mental health. Our World Data. 2018; [Online]. Available: https://ourworldindata.org/mental-health.
James SL, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392(10159):1789–858. https://doi.org/10.1016/S0140-6736(18)32279-7.
Chong SA, Vaingankar JA, Abdin E, Subramaniam M. Mental disorders: employment and work productivity in Singapore. Soc Psychiatry Psychiatr Epidemiol. 2013;48(1):117–23. https://doi.org/10.1007/s00127-012-0526-5.
Too LS, Spittal MJ, Bugeja L, Reifels L, Butterworth P, Pirkis J. The association between mental disorders and suicide: a systematic review and meta-analysis of record linkage studies. J Affect Disord. 2019;259:302–13. https://doi.org/10.1016/j.jad.2019.08.054.
Lund C, et al. Poverty and mental disorders: breaking the cycle in low-income and middle-income countries. Lancet. 2011;378(9801):1502–14. https://doi.org/10.1016/S0140-6736(11)60754-X.
Liu ZH, et al. The prevalence of painful physical symptoms in major depressive disorder: a systematic review and meta-analysis of observational studies. Prog Neuro-Psychopharmacology Biol Psychiatry. 2021;111:110372. https://doi.org/10.1016/J.PNPBP.2021.110372.
Wang Q, Xu R, Volkow ND. Increased risk of COVID-19 infection and mortality in people with mental disorders: analysis from electronic health records in the United States. World Psychiatry. 2021;20(1):124–30. https://doi.org/10.1002/WPS.20806.
Scott KM, et al. Associations between DSM-IV mental disorders and subsequent heart disease onset: beyond depression. Int J Cardiol. 2013;168(6):5293–9. https://doi.org/10.1016/J.IJCARD.2013.08.012.
Razzouk D. Mental health economics: the costs and benefits of psychiatric care. Ment Heal Econ Costs Benefits Psychiatr Care. 2017;1–459. https://doi.org/10.1007/978-3-319-55266-8.
World Health Organisation. SDG indicators — SDG indicators. https://unstats.un.org/sdgs/metadata/?Text=&Goal=3&Target=3.4 (accessed 27 Aug 2021).
Moustgaard H, Bello S, Miller FG, Hróbjartsson A. Subjective and objective outcomes in randomized clinical trials: definitions differed in methods publications and were often absent from trial reports. J Clin Epidemiol. 2014;67(12):1327–34. https://doi.org/10.1016/J.JCLINEPI.2014.06.020.
Lader M. Rating scales in schizophrenia. CNS Drugs 2000. 2012;14(1):23–32. https://doi.org/10.2165/00023210-200014010-00003.
Sajatovic M, Chen P, Young RC. Rating scales in bipolar disorder. Clin Trial Des Challenges Mood Disord. 2015;105–136. https://doi.org/10.1016/B978-0-12-405170-6.00009-9.
Sheehan B. Assessment scales in dementia. Ther Adv Neurol Disord. 2012;5(6):349. https://doi.org/10.1177/1756285612455733.
Fried EI. The 52 symptoms of major depression: lack of content overlap among seven common depression scales. J Affect Disord. 2017;208:191–7. https://doi.org/10.1016/J.JAD.2016.10.019.
Yasuhara A. Correlation between EEG abnormalities and symptoms of autism spectrum disorder (ASD). Brain Dev. 2010;32(10):791–8. https://doi.org/10.1016/J.BRAINDEV.2010.08.010.
Shi T, et al. EEG characteristics and visual cognitive function of children with attention deficit hyperactivity disorder (ADHD). Brain Dev. 2012;34(10):806–11. https://doi.org/10.1016/J.BRAINDEV.2012.02.013.
Pillai V, Kalmbach DA, Ciesla JA. A meta-analysis of electroencephalographic sleep in depression: evidence for genetic biomarkers. Biol Psychiatry. 2011;70(10):912–9. https://doi.org/10.1016/J.BIOPSYCH.2011.07.016.
Narayanan B, et al. Resting state electroencephalogram oscillatory abnormalities in schizophrenia and psychotic bipolar patients and their relatives from the bipolar and schizophrenia network on intermediate phenotypes study. Biol Psychiatry. 2014;76(6):456–65. https://doi.org/10.1016/J.BIOPSYCH.2013.12.008.
Kam JWY, Bolbecker AR, O’Donnell BF, Hetrick WP, Brenner CA. Resting state EEG power and coherence abnormalities in bipolar disorder and schizophrenia. J Psychiatr Res. 2013;47(12):1893–901. https://doi.org/10.1016/J.JPSYCHIRES.2013.09.009.
Olbrich S, Arns M. EEG biomarkers in major depressive disorder: discriminative power and prediction of treatment response. 2013;25(5):604–18. https://doi.org/10.3109/09540261.2013.816269.
Blom EH, Olsson E, Serlachius E, Ericson M, Ingvar M. Heart rate variability (HRV) in adolescent females with anxiety disorders and major depressive disorder. Acta Pædiatrica. 2010;99(4):604–11. https://doi.org/10.1111/J.1651-2227.2009.01657.X.
Liang CS, Lee JF, Chen CC, Chang YC. Reactive heart rate variability in male patients with first-episode major depressive disorder. Prog Neuro-Psychopharmacology Biol Psychiatry. 2015;56:52–7. https://doi.org/10.1016/J.PNPBP.2014.08.004.
Akar SA, Kara S, Latifoğlu F, Bilgiç V. Analysis of heart rate variability during auditory stimulation periods in patients with schizophrenia. J Clin Monit Comput. 2014;29(1):153–62. https://doi.org/10.1007/S10877-014-9580-8.
Kasanuki K, et al. Impaired heart rate variability in patients with dementia with Lewy bodies: efficacy of electrocardiogram as a supporting diagnostic marker. Parkinsonism Relat Disord. 2015;21(7):749–54. https://doi.org/10.1016/J.PARKRELDIS.2015.04.024.
Faurholt-Jepsen M, Kessing LV, Munkholm K. Heart rate variability in bipolar disorder: a systematic review and meta-analysis. Neurosci Biobehav Rev. 2017;73:68–80. https://doi.org/10.1016/J.NEUBIOREV.2016.12.007.
Valenza G, et al. Predicting mood changes in bipolar disorder through heartbeat nonlinear dynamics. IEEE J Biomed Heal Informatics. 2016;20(4):1034–43. https://doi.org/10.1109/JBHI.2016.2554546.
Alam MAU, Roy N, Holmes S, Gangopadhyay A, Galik E. Automated functional and behavioral health assessment of older adults with dementia. Proc. - 2016 IEEE 1st Int. Conf. Connect. Heal. Appl. Syst. Eng. Technol. CHASE. 2016;140–149. https://doi.org/10.1109/CHASE.2016.16.
Greco A, Valenza G, Lanata A, Rota G, Scilingo EP. Electrodermal activity in bipolar patients during affective elicitation. IEEE J Biomed Heal Informatics. 2014;18(6):1865–73. https://doi.org/10.1109/JBHI.2014.2300940.
Sarchiapone M, et al. The association between electrodermal activity (EDA), depression and suicidal behaviour: a systematic review and narrative synthesis. BMC Psychiatry. 2018;18(1):1–27. https://doi.org/10.1186/S12888-017-1551-4.
Pourmohammadi S, Maleki A. Stress detection using ECG and EMG signals: a comprehensive study. Comput Methods Prog Biomed. 2020;193. https://doi.org/10.1016/j.cmpb.2020.105482.
Ghaderi A, Frounchi J, Farnam A. “Machine learning-based signal processing using physiological signals for stress detection”, 2015 22nd Iran. Conf Biomed Eng ICBME. 2016;2015:93–8. https://doi.org/10.1109/ICBME.2015.7404123.
Wijsman J, Grundlehner B, Liu H, Hermens H, Penders J. Towards mental stress detection using wearable physiological sensors. Proc Annu Int Conf IEEE Eng Med Biol Soc EMBS. 2011:1798–1801. https://doi.org/10.1109/IEMBS.2011.6090512.
Bubl E, Kern E, Ebert D, Bach M, Tebartz Van Elst L. Seeing gray when feeling blue? Depression can be measured in the eye of the diseased. Biol Psychiatry. 2010;68(2):205–8. https://doi.org/10.1016/J.BIOPSYCH.2010.02.009.
Schwitzer T, Lavoie J, Giersch A, Schwan R, Laprevote V. The emerging field of retinal electrophysiological measurements in psychiatric research: a review of the findings and the perspectives in major depressive disorder. J Psychiatr Res. 2015;70:113–20. https://doi.org/10.1016/J.JPSYCHIRES.2015.09.003.
Berman G, et al. Decreased retinal sensitivity in depressive disorder: a controlled study. Acta Psychiatr Scand. 2018;137(3):231–40. https://doi.org/10.1111/ACPS.12851.
Ma G, et al. Electrocardiographic and electrooculographic responses to external emotions and their transitions in bipolar I and II disorders. Int J Environ Res Public Heal. 2018;15:884. https://doi.org/10.3390/IJERPH15050884.
Hosseinifard B, Moradi MH, Rostami R. Classifying depression patients and normal subjects using machine learning techniques and nonlinear features from EEG signal. Comput Methods Programs Biomed. 2013;109(3):339–45. https://doi.org/10.1016/j.cmpb.2012.10.008.
Li X, Hu B, Sun S, Cai H. EEG-based mild depressive detection using feature selection methods and classifiers. Comput Methods Programs Biomed. 2016;136:151–61. https://doi.org/10.1016/j.cmpb.2016.08.010.
Kim AY, et al. Automatic detection of major depressive disorder using electrodermal activity. Sci Rep. 2018;8(1):1–9. https://doi.org/10.1038/s41598-018-35147-3.
Roh T, Hong S, Yoo HJ. Wearable depression monitoring system with heart-rate variability. 2014 36th Annu Int Conf IEEE Eng Med Biol Soc EMBC. 2014;562–565. https://doi.org/10.1109/EMBC.2014.6943653.
Williamson JR, Quatieri TF, Helfer BS, Ciccarelli G, Mehta DD. “ocal and facial biomarkers of depression based on motor incoordination and timing. AVEC 2014 - Proc 4th Int Work Audio/Visual Emot Challenge, Work MM 2014. 2014. p. 65–72. https://doi.org/10.1145/2661806.2661809.
Mashio Y, Kawaguchi H. Detecting early symptoms of mental health deterioration using handwriting duration parameters. Neuropsychopharmacol Reports. 2020;40(3):246–53. https://doi.org/10.1002/npr2.12123.
Anusha AS, et al. Electrodermal activity based pre-surgery stress detection using a wrist wearable. IEEE J Biomed Heal Informatics. 2020;24(1):92–100. https://doi.org/10.1109/JBHI.2019.2893222.
Pluntke U, Gerke S, Sridhar A, Weiss J, Michel B. Evaluation and classification of physical and psychological stress in firefighters using heart rate variability. Proc Annu Int Conf IEEE Eng Med Biol Soc EMBS. 2019;2207–2212. https://doi.org/10.1109/EMBC.2019.8856596.
Bay Ayzeren Y, Erbilek M, Celebi E. Emotional state prediction from online handwriting and signature biometrics. IEEE Access. 2019;7:164759–74. https://doi.org/10.1109/ACCESS.2019.2952313.
Khodayari-Rostamabad A, Reilly JP, Hasey G, Debruin H, MacCrimmon D. Diagnosis of psychiatric disorders using EEG data and employing a statistical decision model. 2010 Annu Int Conf IEEE Eng Med Biol Soc EMBC’10. 2010. p. 4006–4009. https://doi.org/10.1109/IEMBS.2010.5627998.
Liu Y, Du S. Psychological stress level detection based on electrodermal activity. Behav Brain Res. 2018;341:50–3. https://doi.org/10.1016/j.bbr.2017.12.021.
Na KS, Cho SE, Cho SJ. Machine learning-based discrimination of panic disorder from other anxiety disorders. J Affect Disord. 2021;278:1–4. https://doi.org/10.1016/j.jad.2020.09.027.
Cordasco G, Scibelli F, Faundez-Zanuy M, Likforman-Sulem L, Esposito A. “Handwriting and drawing features for detecting negative moods”, in Smart Innovation. Systems and Technologies. 2019;103:73–86.
Erguzel TT, Sayar GH, Tarhan N. Artificial intelligence approach to classify unipolar and bipolar depressive disorders. Neural Comput Appl. 2016;27(6):1607–16. https://doi.org/10.1007/s00521-015-1959-z.
Greco A, Lanata A, Valenza G, Rota G, Vanello N, Scilingo EP. On the deconvolution analysis of electrodermal activity in bipolar patients. Proc Annu Int Conf IEEE Eng Med Biol Soc EMBS. 2012;6691–6694. https://doi.org/10.1109/EMBC.2012.6347529.
Du Z, Huang D, Li W, Wang Y. Bipolar disorder recognition via multi-scale discriminative audio temporal representation. AVEC 2018 - Proc. 2018 Audio/Visual Emot. Chall. Work. co-located with MM 2018. 2018. p. 23–30. https://doi.org/10.1145/3266302.3268997.
PRISMA. http://www.prisma-statement.org/Default.aspx (accessed 08 Mar 2022).
Giannakakis G, Grigoriadis D, Giannakaki K, Simantiraki O, Roniotis A, Tsiknakis M. Review on psychological stress detection using biosignals. IEEE Trans Affect Comput. 2019. https://doi.org/10.1109/TAFFC.2019.2927337.
Garcia-Ceja E, Riegler M, Nordgreen T, Jakobsen P, Oedegaard KJ, Tørresen J. Mental health monitoring with multimodal sensing and machine learning: a survey. Pervasive Mob Comput. 2018;51:1–26. https://doi.org/10.1016/j.pmcj.2018.09.003.
de Aguiar Neto FS, Rosa JLG. Depression biomarkers using non-invasive EEG: a review. Neurosci Biobehav Rev. 2019;105:83–93. https://doi.org/10.1016/j.neubiorev.2019.07.021.
Mahato S, Paul S. Electroencephalogram (EEG) signal analysis for diagnosis of major depressive disorder (MDD): a review. Lect Notes Electr Eng. 2019;511:323–35. https://doi.org/10.1007/978-981-13-0776-8_30.
Vasu V, Indiramma M. A survey on bipolar disorder classification methodologies using machine learning. Proc - Int Conf Smart Electron Commun ICOSEC 2020, no. Icosec. 2020. p. 335–340. https://doi.org/10.1109/ICOSEC49089.2020.9215334.
Sabeti M, Katebi S, Boostani R. Entropy and complexity measures for EEG signal classification of schizophrenic and control participants. Artif Intell Med. 2009;47(3):263–74. https://doi.org/10.1016/j.artmed.2009.03.003.
Tekin Erguzel T, Tas C, Cebi M. A wrapper-based approach for feature selection and classification of major depressive disorder-bipolar disorders. Comput Biol Med. 2015;64:127–37. https://doi.org/10.1016/j.compbiomed.2015.06.021.
Mantri S, Patil D,. Agrawal P, Wadhai V. Non invasive EEG signal processing framework for real time depression analysis. IntelliSys 2015 - Proc. 2015 SAI Intell Syst Conf. 2015. p. 518–521. https://doi.org/10.1109/IntelliSys.2015.7361188.
Li X, Hu B, Shen J, Xu T, Retcliffe M. Mild depression detection of college students: an EEG-based solution with free viewing tasks. J Med Syst 2015;39(2). https://doi.org/10.1007/s10916-015-0345-9.
Cai H, Sha X, Han X, Wei S, Hu B. Pervasive EEG diagnosis of depression using Deep Belief Network with three-electrodes EEG collector. In 2016 IEEE International Conference on Bioinformatics and Biomedicine (BIBM). 2016. p. 1239–46. https://doi.org/10.1109/BIBM.2016.7822696.
Cai H, Qu Z, Li Z, Zhang Y, Hu X, Hu B. Feature-level fusion approaches based on multimodal EEG data for depression recognition. Inf Fusion. 2020;59:127–38. https://doi.org/10.1016/j.inffus.2020.01.008.
Mumtaz W, Xia L, Ali SSA, Yasin MAM, Hussain M, Malik AS. Electroencephalogram (EEG)-based computer-aided technique to diagnose major depressive disorder (MDD). Biomed Signal Process Control. 2017;31(2017):108–15. https://doi.org/10.1016/j.bspc.2016.07.006.
Mahato S, Paul S. Detection of major depressive disorder using linear and non-linear features from EEG signals. Microsyst Technol. 2019;25(3):1065–76. https://doi.org/10.1007/s00542-018-4075-z.
Mahato S, Paul S. Classification of depression patients and normal subjects based on electroencephalogram (EEG) signal using alpha power and theta asymmetry. J Med Syst. 2020;44(1):1–8. https://doi.org/10.1007/s10916-019-1486-z.
Bachmann M, Lass J, Hinrikus H. Single channel EEG analysis for detection of depression. Biomed Signal Process Control. 2017;31:391–7. https://doi.org/10.1016/j.bspc.2016.09.010.
Mumtaz W, Qayyum A. A deep learning framework for automatic diagnosis of unipolar depression. Int J Med Inform. 2019;132:103983. https://doi.org/10.1016/j.ijmedinf.2019.103983.
Acharya UR, Oh SL, Hagiwara Y, Tan JH, Adeli H, Subha DP. Automated EEG-based screening of depression using deep convolutional neural network. Comput Methods Programs Biomed. 2018;161:103–13. https://doi.org/10.1016/j.cmpb.2018.04.012.
A. B. et al., “Automated depression detection using deep representation and sequence learning with EEG signals,” J. Med. Syst., vol. 43, no. 7, 2019, [Online]. Available: http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L627888073%0Ahttp://dx.doi.org/10.1007/s10916-019-1345-y.
Mumtaz W, Ali SSA, Yasin MAM, Malik AS. A machine learning framework involving EEG-based functional connectivity to diagnose major depressive disorder (MDD). Med Biol Eng Comput. 2018;56(2):233–46. https://doi.org/10.1007/s11517-017-1685-z.
Ghandeharioun A, et al. Objective assessment of depressive symptoms with machine learning and wearable sensors data. 2017 7th Int Conf Affect Comput Intell Interact ACII. 2017;2018:325–32. https://doi.org/10.1109/ACII.2017.8273620.
Sánchez-Reolid R, Martínez-Rodrigo A, López MT, Fernández-Caballero A. Deep support vector machines for the identification of stress condition from electrodermal activity. Int J Neural Syst. 2020;30(7):1–16. https://doi.org/10.1142/S0129065720500318.
Aqajari SAH, Naeini EK, Mehrabadi MA, Labbaf S, Rahmani AM, Dutt N. GSR analysis for stress: development and validation of an open source tool for noisy naturalistic GSR data, no. 1, 2020 [Online]. Available: http://arxiv.org/abs/2005.01834.
Melillo P, Formisano C, Bracale U, Pecchia L. Classification tree for real-life stress detection using linear heart rate variability analysis. Case study: students under stress due to university examination. IFMBE Proc. 2013;39:477–80. https://doi.org/10.1007/978-3-642-29305-4_126.
Wang JS, Lin CW, Yang YTC. A k-nearest-neighbor classifier with heart rate variability feature-based transformation algorithm for driving stress recognition. Neurocomputing. 2013;116:136–43. https://doi.org/10.1016/j.neucom.2011.10.047.
Karthikeyan P, Murugappan M, Yaacob S. Analysis of stroop colorword test-based human stress detection using electrocardiography and heart rate variability signals. Arab J Sci Eng. 2012;39(3):1835–47. https://doi.org/10.1007/s13369-013-0786-8.
Castaldo R, Xu W, Melillo P, Pecchia L, Santamaria L, James C. Detection of mental stress due to oral academic examination via ultra-short-term HRV analysis. Proc Annu Int Conf IEEE Eng Med Biol Soc EMBS. 2016;3805–8. https://doi.org/10.1109/EMBC.2016.7591557.
Rizwan MF, Farhad R, Mashuk F, Islam F, Imam MH. Design of a biosignal based stress detection system using machine learning techniques. 1st Int Conf Robot Electr Signal Process Tech (ICREST). 2019;364–8. https://doi.org/10.1109/ICREST.2019.8644259.
Byun S, et al. Detection of major depressive disorder from linear and nonlinear heart rate variability features during mental task protocol. Comput Biol Med. 2019;112:103381. https://doi.org/10.1016/j.compbiomed.2019.103381.
Kuang D, et al. Depression recognition according to heart rate variability using Bayesian Networks. J Psychiatr Res. 2017;95:282–7. https://doi.org/10.1016/j.jpsychires.2017.09.012.
Coutts LV, Plans D, Brown AW, Collomosse J. Deep learning with wearable based heart rate variability for prediction of mental and general health. J Biomed Inform. 2020;112:103610. https://doi.org/10.1016/j.jbi.2020.103610.
Mariya LP, Kumareshan N. Depression detection using comparative analysis of QRS detection algorithms and HRV of ECG signal implemented on MATLAB and Verilog. J Phys Conf Ser. 1916;1:2021. https://doi.org/10.1088/1742-6596/1916/1/012018.
Kim EY, Lee MY, Kim SH, Ha K, Kim KP, Ahn YM. Diagnosis of major depressive disorder by combining multimodal information from heart rate dynamics and serum proteomics using machine-learning algorithm. Prog Neuro-Psychopharmacology Biol Psychiatry. 2017;76:65–71. https://doi.org/10.1016/j.pnpbp.2017.02.014.
Benson PJ, Beedie SA, Shephard E, Giegling I, Rujescu D, St D. Clair, “Simple viewing tests can detect eye movement abnormalities that distinguish schizophrenia cases from controls with exceptional accuracy.” Biol Psychiatry. 2012;72(9):716–24. https://doi.org/10.1016/J.BIOPSYCH.2012.04.019.
Meng H, Huang D, Wang H, Yang H, Al-Shuraifi M, Wang Y. Depression recognition based on dynamic facial and vocal expression features using partial least square regression. AVEC 2013 - Proc 3rd ACM Int Work Audio/Visual Emot Chall. 2013. p. 21–9. https://doi.org/10.1145/2512530.2512532.
Zhu Y, Shang Y, Shao Z, Guo G. Automated depression diagnosis based on deep networks to encode facial appearance and dynamics. IEEE Trans Affect Comput. 2018;9(4):578–84. https://doi.org/10.1109/TAFFC.2017.2650899.
Alghowinem S, et al. Multimodal depression detection: fusion analysis of paralinguistic, head pose and eye gaze behaviors. IEEE Trans Affect Comput. 2018;9(4):478–90. https://doi.org/10.1109/TAFFC.2016.2634527.
Srimadhur NS, Lalitha S. An end-to-end model for detection and assessment of depression levels using speech. Procedia Comput Sci. 2020;171:12–21. https://doi.org/10.1016/J.PROCS.2020.04.003.
Bishay M, Palasek P, Priebe S, Patras I. SchiNet: automatic estimation of symptoms of schizophrenia from facial behaviour analysis. IEEE Trans Affect Comput. 2019;12(4):949–61. https://doi.org/10.1109/taffc.2019.2907628.
Singh J, Goya G. Decoding depressive disorder using computer vision. Multimed Tools App. 2020;80(6):8189–212. https://doi.org/10.1007/S11042-020-10128-9.
Lee SC, Chen KW, Liu CC, Kuo CJ, Hsueh IP, Hsieh CL. Using machine learning to improve the discriminative power of the FERD screener in classifying patients with schizophrenia and healthy adults. J Affect Disord. 2021;292:102–7. https://doi.org/10.1016/j.jad.2021.05.032.
Rosenblum S, Werner P, Dekel T, Gurevitz I, Heinik J. Handwriting process variables among elderly people with mild Major Depressive Disorder: a preliminary study. Aging Clin Exp Res. 2010;22(2):141–7. https://doi.org/10.1007/BF03324787.
Likforman-Sulem L, Esposito A, Faundez-Zanuy M, Clemencon S, Cordasco G. EMOTHAW: a novel database for emotional state recognition from handwriting and drawing. IEEE Trans Human-Machine Syst. 2017;47(2):273–84. https://doi.org/10.1109/THMS.2016.2635441.
Nolazco-Flores JA, Faundez-Zanuy M, Velázquez-Flores OA, Del-Valle-soto C, Cordasco G, Esposito A. Mood state detection in handwritten tasks using PCA–mFCBF and automated machine learning. Sensors. 2022;22(4):1–22. https://doi.org/10.3390/s22041686.
Hindra K, Maslov AV, Pechenizkiy M. Stress detection from speech and Galvanic Skin Response signals. Proc 26th IEEE Int Symp Comput Med Syst. 2013. p. 579. https://doi.org/10.1109/cbms.2013.6627790.
Sun F, Kuo C, Cheng H, Buthpitiya S. Activity-aware mental stress detection. In International Conference on Mobile Computing, Applications, and Services. 2012. p. 282–301.
Smets E, et al. Comparison of machine learning techniques for psychophysiological stress detection. Pervasive Comput Paradig Ment Heal. 2019;604:147–56. https://doi.org/10.1007/978-3-319-32270-4.
Sandulescu V, Andrews S, Ellis D, Bellotto N, Mozos OM. Stress detection using wearable physiological sensors. Artif Comput Biol Med IWINAC 2015;9107:526–532. 2015;9107:526–32. https://doi.org/10.1007/978-3-319-18914-7.
Bobade P, Vani M. Stress detection with machine learning and deep learning using multimodal physiological data. Proc 2nd Int Conf Inven Res Comput Appl ICIRCA. 2020. p. 51–7. https://doi.org/10.1109/ICIRCA48905.2020.9183244.
Ding X, Yue X, Zheng R, Bi C, Li D, Yao G. Classifying major depression patients and healthy controls using EEG, eye tracking and galvanic skin response data. J Affect Disord. 2019;251:156–61. https://doi.org/10.1016/j.jad.2019.03.058.
Tazawa Y, et al. Evaluating depression with multimodal wristband-type wearable device: screening and assessing patient severity utilizing machine-learning. Heliyon. 2020;6(2):e03274. https://doi.org/10.1016/j.heliyon.2020.e03274.
Okubo M, Kobayashi A, Ishikawa K. A fake smile thwarts cheater detection. J Nonverbal Behav. 2012;36(3):217–25. https://doi.org/10.1007/S10919-012-0134-9.
Littlewort GC, Bartlett MS, Lee K. Automatic coding of facial expressions displayed during posed and genuine pain. Image Vis Comput. 2009;27(12):1797–803. https://doi.org/10.1016/J.IMAVIS.2008.12.010.
Gosselin P, Perron M, Beaupré M. The voluntary control of facial action units in adults. Emotion. 2010;10(2):266–71. https://doi.org/10.1037/A0017748.
Jalil NA, Yunus RM, Said NS. Environmental colour impact upon human behaviour: a review. Procedia - Soc Behav Sci. 2012;35:54–62. https://doi.org/10.1016/J.SBSPRO.2012.02.062.
Kanai R, Rees G. The structural basis of inter-individual differences in human behaviour and cognition. Nat Rev Neurosci. 2011;12(4):231–42. https://doi.org/10.1038/nrn3000.
Basu S, Bag A, Aftabuddin M, Mahadevappa M, Mukherjee J, Guha R. Effects of emotion on physiological signals. 2016 IEEE Annu. India Conf. INDICON 2016. 2017. https://doi.org/10.1109/INDICON.2016.7839091.
Kondacs A, Szabó M. Long-term intra-individual variability of the background EEG in normals. Clin Neurophysiol. 1999;110(10):1708–16. https://doi.org/10.1016/S1388-2457(99)00122-4.
Hu X, Chen J, Wang F, Zhang D. Ten challenges for EEG-based affective computing. 2019;5(1):1–20. https://doi.org/10.1177/2096595819896200.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Singh, J., Hamid, M.A. Cognitive Computing in Mental Healthcare: a Review of Methods and Technologies for Detection of Mental Disorders. Cogn Comput 14, 2169–2186 (2022). https://doi.org/10.1007/s12559-022-10042-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12559-022-10042-2