Abstract
This study was designed to investigate the therapeutic potential of hydroalcoholic extracts of Acorus calamus (AC) in tibial and sural nerve transection (TST)-induced neuropathic pain in rats. The hot plate, paw heat allodynia, acetone drop, and pinprick tests were performed to assess the degree of heat hyperalgesia, heat and cold allodynia, and mechanical hyperalgesia, respectively, at different time intervals, i.e., day 0, 1, 3, 6, 9, 12, 15, 18, and 21. The tissue superoxide anion and total calcium were measured as markers of oxidative stress. Tissue myeloperoxidase activity was measured as a specific marker of inflammation. Histopathological evaluation was also performed in the nervous tissue to assess the axonal degeneration. Pregabalin served as positive control in this study. TST in rats significantly induced thermal hyperalgesia and allodynia, mechanical hyperalgesia, and increased the levels of superoxide anion, total calcium, and myeloperoxidase (MPO) activity. Moreover significant histological changes were also observed. Oral administration of AC hydroalcoholic extract (100 and 200 mg/kg for 14 days) attenuated TST-induced behavioral, biochemical, and histological changes. Acorus calamus has ameliorative potential in TST-induced painful neuropathy, and this effect may be attributed to its multiple actions including anti-inflammatory, antioxidant, and neuroprotective actions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuropathic pain is characterized by continuous or intermittent pain, typically described as burning, aching, or shooting in quality, and is often associated with abnormal sensitivity of the painful site. Neuropathic pain is produced by damage to the neurons in the peripheral and central nervous systems, and involves sensitization of these systems [1]. Peripheral neuropathic pain is frequently observed in patients with cancer, AIDS, long-standing diabetes, lumbar disc syndrome, herpetic and leprotic infections, traumatic spinal cord injury, multiple sclerosis, stroke, drug-induced states such as those involving chemotherapy, HIV therapy, protein abnormalities, and toxic chemicals, nutritional deficiencies, and kidney failure. Moreover, post-thoracotomy, post-herniorrhaphy, post-mastectomy, and post-sternotomy are also associated with neuropathic pain [2, 3]. Common examples of peripheral neuropathic pain include lumbar or cervical radiculopathy, diabetic polyneuropathy (DPN), and post-herpetic neuralgia (PHN), carpal tunnel syndrome, entrapment syndromes, complex regional pain syndromes (CRPS), and phantom limb pain [4].
Many therapies have been explored for the treatment of neuropathic pain including anticonvulsants, tricyclic antidepressants, selective serotonin reuptake inhibitors, and acetaminophen/opioid combination products [5–7]. However, these therapeutic modalities provide only partial relief and there is no single treatment that works for all conditions of neuropathy. Moreover, a high incidence of side effects is also associated with these drugs [8, 9]. Therefore, there is ample scope to develop new medicine, particularly from plant origin, to treat and manage the neuropathic pain conditions. Several recent studies reported the potential of herbal drugs in peripheral neuropathy and diabetic neuropathy, e.g., Aconiti tuber, Lindera angustifolia, Teucrium polium, Phyllanthus emblica, Vochysia divergens, Cannabis sativa, Nigella sativa, and Ocimum sanctum [10–12].
Acorus calamus (AC) belongs to the family of Araceae. Traditionally, it is used as an ingredient of several drugs (including those used to treat headache, migraine, body ache, and severe inflammatory pain) of the Unani, Ayurveda, and local health care systems in Indian medicine. The plant is a perennial herb growing throughout India, Europe, Asia, and America. Acorus calamus contains glycosides, tannins, mucilage, volatile oil, and bitter principles [13, 14]. The rhizome of the AC plant has several medicinal properties, and it is used in the treatment of insomnia, melancholia, neurosis, remittent fevers, delirium, and hysteria [14]. The aqueous and hydroalcoholic extracts have hypolipidemic and neuropharmacological activities [15, 16].
Several recent studies also explored the potential usefulness of AC in treating anorexia nervosa or skin eruption and its neuroprotective action against ischemic and acrylamide-induced neuronal insult [17–19]. However, the ameliorative potential of Acorus calamus in peripheral neuropathic pain has not been explored yet. Therefore, the present study was designed to investigate the effect of hydroalcoholic extracts of Acorus calamus on tibial and sural nerve transection (TST)-induced painful neuropathy in rats. Pregabalin, a selective Cav 2.2 (α2–δ subunit) channel antagonist, served as positive control in this study.
Materials and methods
Plant materials
The fresh rhizomes of Acorus calamus were collected at Kodaikanal of Tamilnadu, India, and authenticated by staff at the Department of Botany, American College, Madurai, Tamilnadu. A voucher specimen of the plant (PUP-218/2009-2010) is kept at Punjabi University, Patiala, for future reference. After authentication, fresh rhizomes of AC were collected, cleaned thoroughly with distilled water, and dried under shade. The shade-dried rhizome was pulverized in a mechanical grinder to obtain coarse powder.
Drugs and reagents
5,5′-Dithio-bis(2-nitrobenzoic acid) (DTNB), reduced glutathione (GSH), 1,1,3,3-tetramethoxypropane, nitro blue tetrazolium (NBT) (Sigma–Aldrich, USA), bovine serum albumin (BSA) (Sisco Research Laboratories Pvt. Ltd., Mumbai, India), hexadecyltrimethylammonium bromide (HETAB), o-dianisidine hydrochloride (S.D. Fine, Mumbai India), and Folin–Ciocalteu’s phenol reagent (Merck Ltd., Mumbai, India) were procured for the present study. All the chemicals used in the present study were of analytical grade.
Preparation of extracts
The coarsely powdered plant material was subjected to extraction with mixture of ethanol/water (1:1, 50%) at room temperature. After completion of extraction, the solvent was completely removed by vacuum drying at low temperature (<50°C). The yield of hydroalcoholic extract was 26.4% (w/w). The crude extracts were evaluated for absence of β-asarone by measuring the absorbance at 253 and 303 nm. The extract was found to contain saponins, glycosides, and tannins. This hydroalcoholic extract was used to explore the potential role on TST-induced painful neuropathy in rats.
Experimental animals
Wistar rats of either sex, weighing 200–230 g (procured from Punjab Agriculture University, Ludhiana) were used in the present study. They were housed in animal cages with free access to water and standard laboratory pellet chow diet (Kisan Feeds Ltd., Mumbai, India). The rats were exposed to 12-h light and dark cycles. The experimental protocol was duly approved by the Institutional Animal Ethics Committee and the care of the animals was carried out as stated in the guidelines of the Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA), Ministry of Environment and Forest, Government of India (Reg. No. 107/1999/CPCSEA).
Acute and subchronic toxicity test
Acute and subchronic toxicity tests were performed in both male and female rats in order to evaluate the toxic effect (if any) of a single (3000, 4000, and 5000 mg/kg, p.o.) and repeated oral doses (100, 200, and 500 mg/kg for 28 consecutive days) of the AC hydroalcoholic extract in different groups. Animals were maintained and observed for 72 h for signs of acute toxicity and for 28 days for signs of subchronic toxicity (mortality and body weight changes). On the 29th day, the animals were anesthetized with chloroform and killed. Blood samples were collected by cardiac puncture for hematological and biochemical analysis. Tissue sample were collected from the liver, heart, and kidney of the rats for histopathological examinations. The LD50 was calculated according to the method of Litchfield and Wilcoxon [20]. Dose was calculated based on the LD50 value. The experimental procedure for toxicity studies was performed according to the Organization for Economic Co-operation and Development (OECD) guideline no. 401 and 425 [21–23].
Induction of painful neuropathy by TST
Peripheral neuropathic pain was induced by TST as described elsewhere [24]. Briefly, the rat was anesthetized intraperitoneally with thiopental sodium (35 mg/kg). The skin layer of the lateral surface on the left thigh was incised and a cut was made directly through the biceps femoris muscle to expose the sciatic nerve and its three terminal branches (the sural, common peroneal, and tibial nerves) were identified. Thereafter, the tibial and sural nerves were ligated, with silk suture and transection was made at 2 mm from the ligation at distal side. The common peroneal nerve was left intact and no contact was made with it. The muscle and the skin layers were closed immediately. A similar operation was performed on sham control group rats by exposing the sciatic nerve and its branches but without inducing any lesion.
Experimental protocol
Ten groups, each comprising six Wistar rats, were used in the present study.
Group I (normal control)
Rats were not subjected to any surgical procedure and were kept for 3 weeks. The behavioral tests were performed on the different days, i.e., day 0, 1, 3, 6, 9, 12, 15, 18, and 21. Thereafter, all the animals were killed and the biochemical analysis was done for estimating the total protein, superoxide anion generation, and total calcium in sciatic nerve tissue and myeloperoxidase activity in the surrounding muscular tissue sample.
Group II (sham control)
Rats were subjected to a surgical procedure (on day 0) to expose the tibial and sural nerve branches of the sciatic nerve without any transection. The behavioral tests were performed before and 24 h after surgery (i.e., day 1) on different days as described for group I. The biochemical analysis was also done as mentioned for group I.
Group III (TST)
Rats were subjected to a surgical procedure to expose and transect the tibial and sural nerve branches of the sciatic nerve. The behavioral tests and the biochemical parameters were assessed as mentioned for group I.
Group IV (vehicle in TST)
Carboxymethyl cellulose (CMC) (0.5% w/v, p.o.) was administered for 14 days (starting from day 1) in rats subjected to TST. The behavioral tests and the biochemical parameters were assessed as mentioned for group I.
Groups V and VI (low and high dose AC per se)
Hydroalcoholic extract of AC (100 and 200 mg/kg, p.o.) was administered for 14 days in normal rats, starting from day 1. The behavioral tests and the biochemical parameters were assessed as mentioned for group I.
Groups VII (pregabalin per se)
Pregabalin (10 mg/kg, p.o.) was administered for 14 days in normal rats, starting from day 1. The behavioral tests and the biochemical parameters were assessed as mentioned for group I.
Groups VIII and IX (low and high dose AC in TST)
Hydroalcoholic extract of AC (100 and 200 mg/kg, p.o.) was administered for 14 days in rats subjected to TST, starting from day 1. The behavioral tests and the biochemical parameters were assessed as mentioned for group I.
Groups X (pregabalin in TST)
Pregabalin (10 mg/kg, p.o.) was administered for 14 days in rats subjected to TST, starting from day 1. The behavioral tests and the biochemical parameters were assessed as mentioned for group I.
Behavioral examination
Hot plate test
Thermal (noxious heat) nociceptive threshold, as an index of thermal hyperalgesia, was assessed by Eddy’s hot plate method [25]. The plate was preheated and maintained at 52.5 ± 0.5°C. The rat was placed on the hot plate and nociceptive threshold, with respect to licking of the hind paw, was recorded in seconds. A cutoff time of 20 s was maintained.
Paw heat allodynia test
Thermal (non-noxious heat) nociceptive threshold, as an index of heat allodynia, was assessed by Eddy’s hot plate method [25]. The plate was preheated and maintained at 45 ± 0.5°C. The rat was placed on the hot plate and nociceptive threshold, with respect to licking of the hind paw, was recorded in seconds. A cutoff time of 30 s was maintained.
Acetone drop test
Thermal (non-noxious cold) nociceptive threshold, as an index of cold allodynia, was assessed by using the acetone drop method as described by Choi et al. [26] with slight modification according to de la Calle et al. [27] to assess the reactivity to non-noxious cold chemical stimuli. The rat was placed on the top of the wire mesh grid, allowing access to the hind paws. Acetone (100 μl) was sprayed on the plantar surface of hind paw. Cold sensitive reaction with respect to either paw licking, shaking, or rubbing the hind paw was observed and recorded as paw lifting duration the 20-s test period.
Pinprick test
Mechanical hyperalgesia was assessed by the pinprick test as described by Erichsen and Blackburn-Munro [28]. The surface of the injured hind paw was touched with the point of a bent 18-gauge needle (at 90° angle) at an intensity sufficient to produce a reflex withdrawal response in normal non-operated animals, but at an intensity which was insufficient to penetrate the skin in all other groups. The duration of the paw withdrawal was recorded in seconds. A cutoff time of 20 s was maintained.
Biochemical estimations
All the animals were killed on the 21st day after surgery with chemical euthanasia. The portions of the sciatic nerve and the tissue beneath the sciatic nerve were isolated immediately. The sciatic nerve portion, proximal to the point of transection up to its point of emergence from the spinal cord, and distal to the point of transection up to its ending, was excised. The tissue, 1 cm diameter, exactly beneath the point of the sciatic nerve transection was taken. The uniformity among the different nerve and tissue samples was maintained by taking the same weight of the respective samples. Furthermore, the samples were kept in a humidity chamber (maintained at 85% relative humidity and 37°C temperature) to remove and maintain the moisture content of the collected samples. The sciatic nerve homogenate (10%, w/v) was prepared with 0.1 M Tris–HCl buffer (pH 7.4), and deionized water for total protein and total calcium estimation, respectively. Superoxide anion measurement was carried out in sciatic nerve as described by Wang et al. [30]. Surrounding muscular tissue was homogenated with phosphate buffer (pH 7.4) and employed for myeloperoxidase (MPO) estimation.
Estimation of total protein content
The protein concentration was estimated according to the method of Lowry et al. [29] using bovine serum albumin as a standard. The absorbance was determined spectrophotometrically at 750 nm.
Estimation of superoxide anion generation
The sciatic nerve superoxide anion generation was estimated by measuring reduced nitro blue tetrazolium (NBT) as described by Wang et al. [30]. Briefly, the sciatic nerve was taken in 5 ml phosphate-buffered saline containing 100 μM of NBT and incubated at 37°C for 90 min. The NBT reduction was stopped by adding 5 ml of 0.5 M HCl. Then, the left tissue was taken out and homogenized with a mixture (5:1) of 0.1 M NaOH and 0.1% of sodium dodecyl sulfate (SDS) in water containing 40 mg/l diethylenetriaminepentaacetic acid. The mixture was centrifuged at 20,000×g for 20 min. The resultant pellet was resuspended in 1.5 ml of pyridine during heating at 80°C for 90 min to extract formazan. The mixtures were subjected to a second centrifugation at 10,000×g for 10 min. The absorbance of formazan was determined spectrophotometrically at 540 nm. The quantity of NBT reduction = A × V/(T × Wt × ε × l), where A is the absorbance of blue formazan at 540 nm, V is the volume of the solution, T is the time period (90 min) during which rings were incubated with NBT, Wt is the blotted wet weight of the sciatic nerve, ε is the extinction coefficient of blue formazan (i.e., 0.72 l/mmol/mm), and l is the length of the light path. Results are reported as picomoles per minute per milligram wet weight of sciatic nerve.
Estimation of total calcium
The total calcium levels were estimated in the sciatic nerve as described by Severinghaus and Ferrebee [31] and Muthuraman et al. [12]. Briefly, the sciatic nerve homogenate was mixed with 1 ml of trichloroacetic acid (4%) under ice-cold conditions and centrifuged at 1,500×g for 10 min. The clear supernatant was used for estimating the total calcium levels by atomic emission spectroscopy at 556 nm.
Estimation of myeloperoxidase activity
The myeloperoxidase activity was measured by a method described by Grisham et al. [32] and Patriarca et al. [33]. Inflammatory reactions are characterized by the recruitment of inflammatory cells from the blood capillaries to the connective tissue, adjacent to the point of injury. Therefore, the tissue surrounding the nerve lesion was excised as a measure of degree of inflammation. The tissue samples were homogenized in 10 volumes of ice-cold potassium phosphate buffer (pH 7.4), using a tissue homogenizer. The homogenate was centrifuged at 5,000×g for 10 min at 4°C. The supernatant was discarded and 10 ml of ice-cold 50 mM potassium phosphate buffer (pH 6.0), containing 0.5% HETAB and 10 mM EDTA was then added to the pellet. It was then subjected to one cycle of freezing and thawing and a brief period (15 s) of sonication. After sonication, the solution was centrifuged at 19,000×g for 15 min. A 100-μl aliquot of supernatant was combined with 2.9 ml of phosphate buffer (containing 0.167 mg/ml of o-dianisidine hydrochloride and 0.0005% hydrogen peroxide). The myeloperoxidase activity was measured spectrophotometrically at 460 nm. One unit of the myeloperoxidase activity is defined as that which would produce a change in absorbance of 1.0 U/min at pH 7.0 and 25°C, calculated from the initial rate of reaction with peroxide (1 μM) as the substrate. The results were expressed as myeloperoxidase activity units per milligram of protein at 1 min.
Histopathological evaluation
Samples of sciatic nerve were stored in the fixative solution (10% formalin) and cut into 4-μm-thick sections. Staining was done by using hematoxylin and eosin as described by Yukari et al. [34]. Nerve sections were analyzed qualitatively under a light microscope (450×) for axonal degeneration.
Statistical analysis
All the results were expressed as mean ± standard error of means (SEM). The data from the behavioral results were statistically analyzed by two-way analysis of variance followed by Bonferonni’s post-test by using Graph pad prism Version-5.0 software. The data from the biochemical results were statistically analyzed by one-way ANOVA followed by Tukey’s multiple range tests by using Graph pad prism Version-5.0 software. A p value less than 0.05 was considered to be statistically significant.
Results
Effect of Acorus calamus acute and subchronic toxicity test
The AC extracts given at the dose of 5000 mg/kg (for acute toxicity study) and 100, 200, and 500 mg/kg (28 consecutive days, for chronic toxicity study) did not produce any signs of behavioral, biochemical, and organ (functional/morphological) changes in rats. The body weight gain of the control and treated groups was similar (data not shown). No mortality was observed in the control and treated groups.
Effect of Acorus calamus on thermal hyperalgesia and allodynia in TST-induced neuropathic pain
TST resulted in a significant development of thermal hyperalgesia (Fig. 1) and allodynia (Fig. 2). Administration of hydroalcoholic extract of AC (100 and 200 mg/kg, p.o.) attenuated TST-induced decrease in the nociceptive threshold for thermal hyperalgesia and allodynia in a dose-dependent manner. Administration of pregabalin also produced similar effects. However, the vehicle administration did not modulate TST-induced thermal hyperalgesia and allodynia. Moreover, AC per se did not show any significant effect on above-mentioned behavior.
Effect of Acorus calamus on heat allodynia, assessed by the paw heat allodynia test using Eddy’s hot plate apparatus, in TST-induced neuropathic pain. Digits in parenthesis indicate dose in mg/kg. Values are mean ± SEM, n = 6 rats per group. α = p < 0.05 versus sham control group. β = p < 0.05 versus TST group
Effect of Acorus calamus on chemical cold allodynia in TST-induced neuropathic pain
TST resulted in a significant development of chemical cold allodynia as indicated by increase in the paw lifting duration using the acetone drop test (Fig. 3). Administration of AC (100 and 200 mg/kg) significantly attenuated TST-induced increase in paw lifting duration, i.e., cold allodynia, in a dose-dependent manner. Administration of pregabalin also produced similar effects. However, the vehicle administration did not modulate TST-induced cold allodynia. Moreover, AC per se did not show any significant effect on the above-mentioned behavior.
Effect of Acorus calamus on mechanical hyperalgesia in TST-induced neuropathic pain
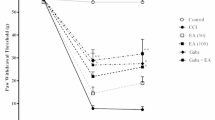
TST resulted in the development of mechanical hyperalgesia as reflected by a significant increase in the hind paw lifting duration in the pinprick test (Fig. 4). Administration of hydroalcoholic extract of AC (100 and 200 mg/kg) attenuated TST-induced increase in the hind paw lifting duration, i.e., mechanical hyperalgesia, in a dose-dependent manner. Administration of pregabalin also produced similar effects. However, the vehicle administration did not modulate TST-induced mechanical hyperalgesia. Moreover, AC per se did not show any significant effect on the above-mentioned behavior.
Effect of Acorus calamus on superoxide anion generation and total calcium level
TST resulted in a significant increase in the levels of superoxide anion generation and the total calcium in sciatic nerve tissue, as compared to sham control group. Administration of the hydroalcoholic extract of AC (100 and 200 mg/kg, p.o.) significantly attenuated TST-induced increase in the levels of superoxide anion generation and the total calcium in a dose-dependent manner. Administration of pregabalin also produced similar effects. However, the vehicle administration did not modulate TST-induced alteration in the superoxide anion generation and the total calcium levels. Moreover, AC per se did not show any significant effect on the above-mentioned biochemical levels (Table 1).
Effect of Acorus calamus on myeloperoxidase activity
TST resulted in a significant increase in the levels of myeloperoxidase activity in surrounding tissue of the tibial and sural nerve transectioned area, as compared to sham control group. Administration of the hydroalcoholic extract of AC (100 and 200 mg/kg, p.o.) significantly attenuated TST-induced increase in the activity of myeloperoxidase in a dose-dependent manner. Administration of pregabalin also produced similar effects. However, the vehicle administration did not modulate TST-induced alteration in the activity of myeloperoxidase. Moreover, AC per se did not show any significant effect on the above-mentioned biochemical levels (Table 1).
Effect of Acorus calamus on TST-induced histopathological changes
TST resulted in significant histopathological changes assessed in cross-sectional sections of the distal part of the sciatic nerve. In cross section, axonal degeneration was evident by decrease in the number of myelinated fibers along with swelling of non-myelinated and myelinated nerve fibres. Moreover, the fiber derangement and decrease in number of Schwann cells were also noted. Administration of the hydroalcoholic extract of AC (100 and 200 mg/kg, p.o.) and pregabalin significantly attenuated TST-induced axonal degeneration and histopathological alterations (Fig. 5).
Effect of Acorus calamus on TST-induced histopathological changes. Figure is the cross-sectioned sciatic nerve of normal, sham, vehicle, TST, AC (100 and 200 mg/kg), and pregabalin pretreated group (a–g), respectively. In a, arrow shows normal fiber arrangement. In c and d, thick arrows show swelling of non-myelinated nerve fiber. In c, thin arrows indicate fiber derangement and morphological alteration in Schwann cells. In d, thin arrow shows swelling of vascular bed. In e–g, arrows show attenuation of TST-induced swelling of nerve fibers by AC (100 and 200 mg/kg) and pregabalin pretreatment, respectively. Microscopic examinations under ×450 light microcopy, scale bar 35 μm
Discussion
In the present investigation, TST resulted in a significant development of heat hyperalgesia, heat allodynia, cold allodynia, mechanical hyperalgesia, and mechanical allodynia, reflecting TST-induced peripheral neuropathic pain. These behavioral alterations started on the 3rd day after the TST surgery and peaked within 8–12 days. Furthermore, TST animals also exhibited increased levels of nerve tissue superoxide anions, total calcium, and raised tissue myeloperoxidase (MPO) activity. Moreover, hematoxylin and eosin staining also showed significant histopathological changes. These observations are in line with our earlier findings [12, 35, 36] and reports from the other laboratories [24, 37].
Myeloperoxidase is an enzyme released from neutrophils and is used as a specific marker of inflammation [32]. Previous studies employing various animal models have supported that inflammation plays a critical role in the development of neuropathic pain [36, 38]. In response to an injurious insult to a nerve, initial steps of inflammatory reactions involve the release of pro-inflammatory mediators from the resident macrophages and the Schwann cells [39]. This is followed by infiltration of inflammatory cells including macrophages from the blood capillaries to an area adjacent to the nerve lesion. It has been documented that the sustained activation of peripheral nociceptors leads to the hypersensitivity of the primary afferent neurons and central sensitization of the dorsal horn neurons [40].
Neuropathic pain (including TST-induced) has been demonstrated to produce a rise in tissue total calcium levels [36, 41, 42]. Calcium ion accumulation has been documented to trigger the secondary messengers, i.e., activation of calcium binding protein (calpain, calmodulin etc.) and calcium-dependent kinase and phosphatase action, which undergo an autodestruction including long-term potentiation and neuronal hyperexcitation [17]. Calcium-induced activation of calpains has been reported to produce the axonal degeneration by degradation of the axonal cytoskeleton [43]. Furthermore, a key role of calcium accumulation has also been reported in formalin, post-traumatic, axotomy, chronic constriction injury (CCI), and vincristine-induced models of neuropathic pain [12, 35, 42].
Studies have also documented a prominent role of free radicals and oxidative stress in causing tissue injury and pain in various types of neuropathic pain viz. CCI and vincristine- and diabetes-induced neuropathic pain [35, 44, 45]. Furthermore, calcium-induced activation of calpain is associated with generation of reactive oxygen species from mitochondria, therefore indicating a prominent role of calcium in tissue oxidative stress [46]. Therefore, it looks quite evident that inflammation, increased calcium levels, and oxidative stress together play a vital role in TST-induced peripheral neuropathic pain, a conclusion which is also supported by histological studies. In the present investigation administration of hydroalcoholic extract of AC (100 and 200 mg/kg, p.o. daily for 2 weeks) attenuated TST-induced painful behavioral responses (i.e., heat hyperalgesia, heat and cold allodynia, mechanical hyperalgesia, and mechanical allodynia), biochemical changes (i.e., superoxide anion generation, total calcium, and myeloperoxidase activity), and histopathological alterations.
Traditionally, decoction of Acorus calamus rhizome has been used in treating headache, migraine, body ache, and severe inflammatory pain particularly in south India. Acorus calamus in several recent studies has been shown to exert a battery of beneficial effects in various ailments viz. epilepsy, memory deficits, dyspepsia, ulcers, rheumatic pain, neuralgia etc. [14, 15, 47]. Ethanolic extract of AC has been reported to exert anticellular and immunosuppressive properties and inhibited production of nitric oxide, interleukin-2, and tumor necrosis factor-alpha [48]. It has also been reported that antispasmodic effect of AC is mediated through calcium channel blockade [49]. Furthermore, the ethanolic extract of AC has also been demonstrated to possess potential antioxidant, anti-inflammatory, and neuroprotective actions [21, 50–53]. On the basis of data in hand and with support from the literature, therefore, it may be proposed that hydroalcoholic extract of AC rhizome produced an ameliorative effect in TST-induced painful peripheral neuropathy by virtue of its multiple effects viz. antioxidant, anti-inflammatory, and neuroprotective actions manifested in terms of alleviation of TST-induced behavioral alterations (heat hyperalgesia, heat allodynia, cold allodynia, mechanical hyperalgesia, and mechanical allodynia), biochemical changes (increased nerve tissue superoxide anions, total calcium, and tissue MPO activity), and histopathological changes. To the best of our knowledge, this is the first report indicating the ameliorative role of AC in TST-induced painful neuropathy in rats.
Pregabalin is a selective Cav 2.2 (α2–δ subunit) channel antagonist and anticonvulsant that is successfully being used to treat many neuropathic pain syndromes [54]. Various studies have demonstrated antihyperalgesic and antiallodynic effects of pregabalin in different animal models of neuropathic pain [54–56]. Therefore, pregabalin was selected as a standard control in this investigation.
Conclusion
Acorus calamus possesses a beneficial effect in TST-induced peripheral neuropathic pain. Its anti-inflammatory, antioxidant, and neuroprotective properties may be important in mediating this effect. Nevertheless further studies are needed to explore the full potential and exact mechanism of Acorus calamus in neuropathic pain.
References
Namaka M, Gramlich CR, Ruhlen D, Melanson M, Sutton I, Major J (2004) A treatment algorithm for neuropathic pain. Clin Ther 26:951–979
Alston RP, Pechon P (2005) Dysaesthesia associated with sternotomy for heart surgery. Br J Anaesth 95:153–158
Tavakoli M, Quattrini C, Abbott C, Kallinikos P, Marshall A, Finnigan J, Morgan P, Efron N, Boulton AJ, Malik RA (2010) Corneal confocal microscopy: a novel non-invasive test to diagnose and stratify the severity of human diabetic neuropathy. Diabetes Care. doi:10.1007/s00125-003-1086-8
Pramod K (2006) Chronic pain syndromes (non terminal illness). Indian J Anaesth 50:391–396
Kalita J, Vaipayee A, Misra UK (2006) Comparison of predinisolone with piroxicam in complex regional pain syndrome following stroke: a randomised controlled trial. QJM 99:89–95
Teasell RW, Mehta S, Aubut JA, Foulon B, Wolfe DL, Hsieh JT, Townson AF, Short C (2010) Spinal Cord Injury Rehabilitation Evidence Research Team. A systematic review of pharmacologic treatments of pain after spinal cord injury. Arch Phys Med Rehabil 91:816–831
Zakrzewska JM (2010) Medical management of trigeminal neuropathic pains. Exp Opin Pharmacother 11:1239–1254
Woolf CJ (2004) Pain: moving from symptom control toward mechanism-specific pharmacologic management. Ann Intern Med 140:441–451
Attal N, Cruccu G, Haanpaa M, Hansson P, Jensen TS, Nurmikko T, Sampaio C, Sindrup S, Wiffen P, Task Force EFNS (2006) EFNS guidelines on pharmacological treatment of neuropathic pain. Eur J Neurol 13:1153–1169
Comelli F, Giagnoni G, Bettoni I, Colleoni M, Costa B (2008) Antihyperalgesic effect of a Cannabis sativa extract in a rat model of neuropathic pain: mechanisms involved. Phytother Res 8:1017–1024
Kanter M (2008) Effects of Nigella sativa and its major constituent, thymoquinone on sciatic nerves in experimental diabetic neuropathy. Neurochem Res 1:87–96
Muthuraman A, Diwan V, Jaggi AS, Singh N, Singh D (2008) Ameliorative effects of Ocimum sanctum in sciatic nerve transection-induced neuropathy in rats. J Ethnopharmacol 120:56–62
Duke JA (1985) Handbook of medicinal herbs. CRC, Boca Raton
Mittal N, Ginwal HS, Varshney VK (2009) Pharmaceutical and biotechnological potential of Acorus calamus Linn: an indigenous highly valued medicinal plant species. Pharmacog Rev 3:83–93
Martis G, Rao A, Karanth KS (1991) Neuropharmacological activity of Acorus calamus. Fitoterapia 4:331–337
Parap RS, Mengi SA (2003) Evaluation of hypolipidemic activity of Acorus calamus Linn in rats. Indian Drugs 40:25–29
Young W (1992) Role of calcium in central nervous system injuries. J Neurotrauma 9:9–25
Shukla PK, Khanna VK, Ali MM, Maurya R, Khan MY, Srimal RC (2006) Neuroprotective effect of Acorus calamus against middle cerebral artery occlusion-induced ischaemia in rat. Hum Exp Toxicol 25:187–194
Hazra R, Ray K, Guha D (2007) Inhibitory role of Acorus calamus in ferric chloride-induced epileptogenesis in rat. Hum Exp Toxicol 26:947–953
Litchfield JTJR, Wilcoxon F (1949) A simplified method of evaluating dose–effect experiments. J Pharmacol Exp Ther 96:99–113
Lipnick RL, Cotruvo JA, Hill RN, Bruce RD, Stitzel KA, Walker AP, Chu I, Goddard M, Segal L, Springer JA, Myers RC (1995) Comparison of the up-and-down, conventional LD50, and fixed-dose acute toxicity procedures. Food Chem Toxicol 33:223–231
Schlede E, Mischke U, Diener W, Kayser D (1995) The international validation study of the acute toxic class method (oral). Arch Toxicol 69:659–670
Combes R, Gaunt I, Balls M (2006) A scientific and animal welfare assessment of the OECD health effects test guidelines for the safety testing of chemicals under the European Union REACH System. Altern Lab Anim 34:77–122
Lee BH, Won R, Baik EJ, Lee SH, Moon CH (2000) An animal model of neuropathic pain employing injury to the sciatic nerve branches. Neuroreport 11:657–661
Eddy NB, Touchberry CF, Lieberman JE (1950) Synthetic analgesics: I. Methadone isomers and derivatives. J Pharmacol Exp Ther 98:121–137
Choi Y, Yoon YW, Na HS, Kim SH, Chung JM (1994) Behavioral signs of ongoing pain and cold allodynia in a rat model of neuropathic pain. Pain 59:369–376
de la Calle L, Mena MA, Gonzalez-Escalada JR, Paıno CL (2002) Intrathecal transplantation of neuroblastoma cells decreases heat hyperalgesia and cold allodynia in a rat model of neuropathic pain. Brain Res Bull 59:205–211
Erichsen HK, Blackburn-Munro G (2002) Pharmacological characterization of the spared nerve injury model of neuropathic pain. Pain 98:151–161
Lowry OH, Rosenbrough NJ, Farr AL, Randall RJ (1951) Protein measurement with folin phenol reagent. J Biol Chem 193:265–275
Wang HD, Pagano PJ, Du Y, Cayatte AJ, Quinn MT, Brecher P, Cohen RA (1998) Superoxide anion from the adventitia of the rat thoracic aorta inactivates nitric oxide. Circ Res 82:810–818
Severinghaus JW, Ferrebee JW (1950) Calcium determination by flame photometry; methods for serum, urine, and other fluids. J Biol Chem 187:621–630
Grisham MB, Specian RD, Zimmerman TE (1994) Effects of nitric oxide synthase inhibition on the pathophysiology observed in a model of chronic granulomatous colitis. J Pharmacol Exp Ther 271:1114–1121
Patriarca P, Dri P, Snidero M (1977) Interference of myeloperoxidase with the estimation of superoxide dismutase activity. J Lab Clin Med 90:289–294
Yukari S, Sukumar P, Desai AE, Hadererm SS, Peter G, Douglas C, Anthony UDG, Ging KW (2004) Neurologic and histopathologic evaluation after high-volume intrathecal amitriptyline. Reg Anesth Pain Med 29:434–440
Muthuraman A, Jaggi AS, Singh N, Singh D (2008) Ameliorative effects of amiloride and pralidoxime in chronic constriction injury and vincristine-induced painful neuropathy in rats. Eur J Pharmacol 587:104–111
Jain V, Jaggi AS, Singh N (2009) Ameliorative potential of rosiglitazone in tibial and sural nerve transection-induced painful neuropathy in rats. Pharmacol Res 59:385–392
Cui JG, Holmin S, Mathiesen T, Meyerson BA, Linderoth B (2000) Possible role of inflammatory mediators in tactile hypersensitivity in rat models of mononeuropathy. Pain 88:239–248
Kuhad A, Chopra K (2009) Tocotrienol attenuates oxidative-nitrosative stress and inflammatory cascade in experimental model of diabetic neuropathy. Neuropharmacology 57:456–462
Marchand F, Perretti M, McMahon SB (2005) Role of immune system in chronic pain. Nat Rev Neurosci 6:521–532
Woolf CJ, Mannion RJ (1999) Neuropathic pain: aetiology, symptoms, mechanisms, and management. Lancet 353:1959–1964
Cecile H, Perrine I, Mohammed A, Denis G, Jean V, Frederique S (2005) Calcium dependence of axotomized sensory neurons excitability. Neurosci Lett 380:330–334
Siau C, Bennett GJ (2006) Dysregulation of neuronal calcium homeostasis in chemotherapy-evoked painful peripheral neuropathy. Anesth Analg 102:1485–1490
Glass JD, Culver DG, Levey AI, Nash NR (2002) Very early activation of m-calpain in peripheral nerve during Wallerian degeneration. J Neurol Sci 196:9–20
Zeinab K, Bereha K (2001) A role for free radicals and nitric oxide in delayed recovery in aged rats with chronic constriction nerve injury. Free Radic Biol Med 31:430–439
Siniscalco D, Fuccio C, Giordano C, Ferraraccio F, Palazzo E, Luongo L, Rossi F, Maione S, de Novellis V (2007) Role of reactive oxygen species and spinal cord apoptotic genes in the development of neuropathic pain. Pharmacol Res 55:158–166
Carriedo SG, Sensi SL, Yin HZ, Weiss JH (2000) AMPA exposures induce mitochondrial Ca(2+) overload and ROS generation in spinal motor neurons in vitro. J Neurosci 20:240–250
Rafatullah S, Tariq M, Mossa JS, Al-Yahya MA, Al-Said MS, Ageel AM (1994) Anti-secretagogue, anti-ulcer and cytoprotective properties of Acorus calamus in rats. Fitotherpia 65:19–23
Mehrotra S, Mishra KP, Maurya R, Srimal RC, Yadav VS, Pandey R, Singh VK (2003) Anticellular and immunosuppressive properties of ethanolic extract of Acorus calamus rhizome. Int Immunopharmacol 3:53–61
Gilani AU, Shah AJ, Ahmad M, Shaheen F (2006) Antispasmodic effect of Acorus calamus Linn. is mediated through calcium channel blockade. Phytother Res 20:1080–1084
Shukla PK, Khanna VK, Ali MM, Maurya RR, Handa SS, Srimal RC (2002) Protective effect of Acorus calamus against acrylamide induced neurotoxicity. Phytother Res 16:256–260
Manikandan S, Srikumar R, Jeya Parthasarathy N, Sheela Devi R (2005) Protective effect of Acorus calamus Linn on free radical scavengers and lipid peroxidation in discrete regions of brain against noise stress exposed rat. Biol Pharm Bull 28:2327–2330
Tippani R, Porika M, Rao AV, Abbagani S, Yellu NR, Tammidala C (2008) Analgesic activity of root extract of Acorus calamus Linn. Pharmacol Online 3:240–243
Yang L, Li S, Huang Y, Liang J, Wang Y (2008) Effects of Acorus gramineus and its component, alpha-asarone, on apoptosis of hippocampal neurons after seizure in immature rats. Neural Reg Res 3:19–24
Kumar K, Taylor RS, Jacques L, Eldabe S, Meglio M, Molet J, Thomson S, O’Callaghan J, Eisenberg E, Milbouw G, Buchser E, Fortini G, Richardson J, North RB (2007) Spinal cord stimulation versus conventional medical management for neuropathic pain: a multicentre randomised controlled trial in patients with failed back surgery syndrome. Pain 132:179–188
Bender G, Florian JA Jr, Bramwell S, Field MJ, Tan KK, Marshall S, DeJongh J, Bies RR, Danhof M (2010) Pharmacokinetic–pharmacodynamic analysis of the static allodynia response to pregabalin and sildenafil in a rat model of neuropathic pain. J Pharmacol Exp Ther 334:599–608
Park HJ, Joo HS, Chang HW, Lee JY, Hong SH, Lee Y, Moon DE (2010) Attenuation of neuropathy-induced allodynia following intraplantar injection of pregabalin. Can J Anaesth 57:664–671
Acknowledgments
The authors are grateful to the Department of Pharmaceutical Sciences and Drug Research, Punjabi University, Patiala, India, for supporting this study and providing technical facilities for the work. The authors also acknowledge the financial support from Council of Scientific and Industrial Research (CSIR) through senior research fellowship (SRF).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Muthuraman, A., Singh, N. & Jaggi, A.S. Effect of hydroalcoholic extract of Acorus calamus on tibial and sural nerve transection-induced painful neuropathy in rats. J Nat Med 65, 282–292 (2011). https://doi.org/10.1007/s11418-010-0486-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-010-0486-6