Abstract
Purpose
Tw o cases are presented wherein the GlideScope® videolaryngoscope (GVL) facilitated laryngeal exposure and successful endotracheal intubation, but resulted in pharyngeal injury.
Clinical features
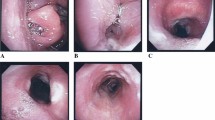
GlideScope® videolaryngoscopy was performed in two female patients, whose airways were anticipated to present difficulties for direct laryngoscopy. In the first case, following induction of anesthesia, moderate difficulty was encountered in directing the endotracheal tube (ETT) into the patient’s larynx. In the second case, minimal difficulty with the GVL was experienced, and no problems were identified with airway instrumentation until the drapes covering the patient’s face were removed. In both instances, the ETT had passed through the right palatopharyngeal arch, requiring suturing in the first patient, and electrocautery in the second patient.
Conclusion
There have been no previously published reports of injuries related to GlideScope® laryngoscopy, but perforation of the palatopharyngeal arch occurring in two patients demonstrates a rare but potentially important complication of the GVL. Strategies to minimize this complication are considered.
Résumé
Objectif
Sont présentés deux cas dans lesquels l’utilisation du vidéolaryngoscope GlideScope® (GVL) a facilité l’exposition laryngée et l’intubation endotrachéale, mais a eu pour conséquence un traumatisme pharyngé.
Eléments cliniques
La vidéolaryngoscopie avec le GlideScope® a été effectuée sur deux patientes chez qui on anticipait une laryngoscopie directe difficile. Dans le premier cas, suite à l’induction de l’anesthésie, une difficulté modérée a été rencontrée à orienter la sonde endotrachéale (SET) vers le larynx de la patiente. Dans le second cas, peu de difficultés ont été rencontrées avec le GVL, et aucun probléme n’a été identifié lors de l’instrumentation des voies aériennes jusqu’à ce que les champs qui couvraient le visage de la patiente soient enlevés. Dans les deux cas, la SET avait traversé l’arche palato-pharyngée droite, nécessitant des points de suture chez la premiére patiente et une électrocautérisation chez la seconde.
Conclusion
Il n’existe pas d’articles déjà publiés rapportant des blessures suite à une laryngoscopie avec le GlideScope®; toutefois, une perforation de l’arche palato-pharyngale, survenue chez deux patientes, illustre une complication rare du GVL, mais potentiellement importante. Nous présentons certaines stratégies pour diminuer la gravité de cette complication.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Cooper RM, Pacey JA, Bishop MJ, McCluskey SA. Early clinical experience with a new videolaryngoscope (GlideScope) in 728 patients. Can J Anesth 2005; 52: 191–8.
Doyle DJ, Ramachandran, M, Zura A, Ryckman JV, Abdelmalak B. The Glidescope video laryngoscope: clinical experience in 747 cases. Anesthesiology 2005; 103: A842 (abstract).
Rai MR, Dering A, Verghese C. The Glidescope system: a clinical assessment of performance. Anaesthesia 2005; 60: 60–4.
Sun DA, Warriner CB, Parsons DG, Klein R, Umedaly HS, Moult M. The GlideScope Video Laryngoscope: randomized clinical trial in 200 patients. Br J Anaesth 2005; 94: 381–4.
Krasser K,Missaghi-Berlini S M,Moser A,Zadrobilek E. Evaluation of the standard adult GlideScope vide-olaryngoscope: orotracheal intubation performed by novice users after formal instruction. Internet Journal of Airway Management. Available from URL; http:// www.ijam.at/volume03/clinicalinvestigation01/ default.htm (accessed May 14, 2006).
Agro F, Barzoi G, Montecchia F. Tracheal intubation using a Macintosh laryngoscope or a GlideScope in 15 patients with cervical spine immobilization (Letter). Br J Anaesth 2003; 90: 705–6.
Cooper RM. Use of a new videolaryngoscope (GlideScope) in the management of a difficult airway. Can J Anesth 2003; 50: 611–3.
Doyle DJ. Awake intubation using the GlideScope video laryngoscope: initial experience in four cases (Letter). Can J Anesth 2004; 51: 520–1.
Lim Y, Yeo SW. A comparison of the GlideScope with the Macintosh laryngoscope for tracheal intubation in patients with simulated difficult airway. Anaesth Intensive Care 2005; 33: 243–7.
Cormack RS, Lehane J. Difficult tracheal intubation in obstetrics. Anaesthesia 1984; 39: 1105–11.
Samsoon GL, Young JR. Difficult tracheal intubation: a retrospective study. Anaesthesia 1987; 42: 487–90.
Owen H, Waddell-Smith I. Dental trauma associated with anaesthesia. Anaesth Intensive Care 2000; 28: 133–45.
Warner ME, Benenfeld SM, Warner MA, Schroeder DR, Maxson PM. Perianesthetic dental injuries: frequency, outcomes, and risk factors. Anesthesiology 1999; 90: 1302–5.
Weber S. Traumatic complications of airway management. Anesthesiol Clin North America 2002; 20: 503–12.
Caplan RA, Posner KL, Ward RJ, Cheney FW. Adverse respiratory events in anesthesia: a closed claims analysis. Anesthesiology 1990; 72: 828–33.
Domino KB, Posner KL, Caplan RA, Cheney FW. Airway injury during anesthesia: a closed claims analysis. Anesthesiology 1999; 91: 1703–11.
Peterson GN, Domino KB, Caplan RA, Posner KL, Lee LA, Cheney FW. Management of the difficult airway: a closed claims analysis. Anesthesiology 2005; 103: 33–9.
Tanaka A, Isono S, Ishikawa T, Sato J, Nishino T. Laryngeal resistance before and after minor surgery: endotracheal tube versus laryngeal mask airway. Anesthesiology 2003; 99: 252–8.
Yu H, Liu B. A Comparison of hemodynamic responses to tracheal intubation with three different intubating devices: GlideScope®, Lightwand and Direct Laryngoscope in normotensive patients. Anesthesiology 2005; 103: A377 (abstract).
Stubbing JF. Anaesthetic morbidity from trauma to the uvula. Anaesthesia 1990; 45: 886–7.
Kharasch ED, Sivarajan M. Gastroesophageal perforation after intraoperative transesophageal echocardiography. Anesthesiology 1996; 85: 426–8.
Hung OR, Stewart RD. Lightwand intubation: I -A new lightwand device. Can J Anaesth 1995; 42: 820–5.
Author information
Authors and Affiliations
Corresponding author
Additional information
The author is a consultant to Saturn Biomedical Systems, the manufacturer of the GlideScope® videolaryngoscope. No financial support was received for this report.
Rights and permissions
About this article
Cite this article
Cooper, R.M. Complications associated with the use of the GlideScope® videolaryngoscope. Can J Anesth 54, 54–57 (2007). https://doi.org/10.1007/BF03021900
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03021900