Abstract
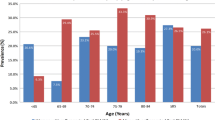
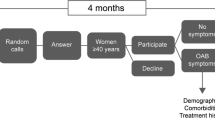
Overactive bladder (OAB)—a syndrome characterized by urinary urgency, with or without urge incontinence, urinary frequency and nocturia—is estimated to affect 10% to 20% of the US and European populations. This study was carried out to validate a patient-administered screening awareness tool to identify patients with bothersome OAB symptoms. Patients were recruited from 12 primary care and 1 gynecology practice during regularly scheduled appointments. Enrollees completed an 8-item questionnaire assessing the amount of “bother” they associated with OAB symptoms. Clinicians then asked the patients 4 questions regarding urinary frequency, urgency, nocturia, and incontinence. If the screening was positive for symptoms of OAB or if the patient provided positive responses to the urinary symptom questions, the clinician asked additional questions regarding lifestyle and coping behaviors. The clinician then diagnosed the patient, placing him or her in the “No OAB,” “Possible OAB,” or “Probable OAB” category. Multivariable logistic regressions controlling for age and sex were performed to assess the applicability of the tool for identifying patients with OAB. A total of 1299 patients were enrolled, and 1260 provided complete data. Patients were aged 51.6±17.0 years, 62% were female, most (89%) were Caucasian, 22% experienced urinary urgency, and 18% experienced urge incontinence. The prevalence of Probable OAB was 12%. The c-index of the model identifying patients with a diagnosis of Probable OAB was 0.96, with a sensitivity and specificity of 98.0 and 82.7. For OAB-V8 scores ≥8, the odds ratio for Probable OAB was 95.7 (95% Cl: 29.3; 312.4). The OAB-V8 performed well in helping clinicians identify patients with bothersome OAB symptoms in a primary care setting and will assist clinicians in identifying patients who may benefit from treatment.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Abrams P, Cardozo L, Fall M, et al. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Am J Obstet Gynecol. 2002;187:116–126.
Milsom I, Abrams P, Cardozo L, Roberts RG, Thuroff J, Wein AJ. How widespread are the symptoms of an overactive bladder and how are they managed? A population-based prevalence study. BJU Int. 2001;87:760–766.
Stewart WF, Van Rooyen JB, Cundiff GW, et al. Prevalence and burden of overactive bladder in the United States. World J Urol. 2003;20:327–336.
Burgio KL, Ives DG, Locher JL, Arena VC, Kuller LH. Treatment seeking for urinary incontinence in older adults. J Am Geriatr Soc. 1994;42:208–212.
Roberts RO, Jacobsen SJ, Rhodes T, et al. Urinary incontinence in a community-based cohort: prevalence and healthcare-seeking. J Am Geriatr Soc. 1998;46:467–472.
Wyman JF, Harkins SW, Fantl JA. Psychosocial impact of urinary incontinence in the communitydwelling population. J Am Geriatr Soc. 1990;38:282–288.
Shaw C, Tansey R, Jackson C, Hyde C, Allan R. Barriers to help seeking in people with urinary symptoms. Fam Pract. 2001;18:48–52.
Cunningham-Burley S, Allbutt H, Garraway WM, Lee AJ, Russell EB. Perceptions of urinary symptoms and health-care-seeking behaviour amongst men aged 40–79 years. Br J Gen Pract. 1996;46:349–352.
Cohen SJ, Robinson D, Dugan E, et al. Communication between older adults and their physicians about urinary incontinence. J Gerontol A Biol Sci Med Sci. 1999;54:M34-M37.
Ricci JA, Baggish JS, Hunt TL, et al. Coping strategies and health care-seeking behavior in a US national sample of adults with symptoms suggestive of overactive bladder. Clin Ther. 2001;23: 1245–1259.
Chiaffarino F, Parazzini F, Lavezzari M, Giambanco V. Impact of urinary incontinence and overactive bladder on quality of life. Eur Urol. 2003;43:535–538.
Coyne K, Revicki D, Hunt T, et al. Psychometric validation of an overactive bladder symptom and health-related quality of life questionnaire: the OAB-q. Qual Life Res. 2002;11:563–574.
Liberman JN, Hunt TL, Stewart WF, et al. Health-related quality of life among adults with symptoms of overactive bladder: results from a US community-based survey. Urology. 2001; 57:1044–1050.
Cox DR, Snell EJ. The Analysis of Binary Data. 2nd ed. New York, NY: John Wiley & Sons; 1989.
Hosmer DW, Lemeshow S. Applied Logistic Regression. 2nd ed. New York, NY: John Wiley & Sons; 2000.
Tabachnick BG, Fidell LS. Using Multivariate Statistics. 4th ed. Boston, Mass: Allyn and Bacon; 2001.
Parazzini F, Lavezzari M, Arbitani W. Prevalence of overactive bladder and urinary incontinence. J Fam Pract. 2002;51:1072–1075.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Coyne, K.S., Zyczynski, T., Margolis, M.K. et al. Validation of an overactive bladder awareness tool for use in primary care settings. Adv Therapy 22, 381–394 (2005). https://doi.org/10.1007/BF02850085
Issue Date:
DOI: https://doi.org/10.1007/BF02850085