Summary
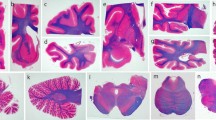
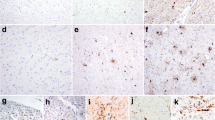
The macroscopical, histological, ultrastructural and immuno-cytochemical features of progressive supranuclear palsy (PSP) are reviewed. Recent investigations have revealed important differences in the distribution, ultrastructure and immunocytochemical profile of neurofibrillary tangles in PSP and in Alzheimer’s disease. Cortical involvement, as demonstrated by the presence of tangles and neuropil threads, has extended the neuropathological spectrum of PSP. Quantitative assessments of neuronal populations show neuronal loss, not only in various nuclei of the brainstem, diencephalon and cerebellum, but also in other areas, including the nucleus basalis of Meynert, substantia nigra and neostriatum.
A new classification, based on neuropathological criteria, is suggested in order to take into consideration the phenotypic heterogeneity of PSP. This new classification distinguishes three types: typical, atypical and combined cases. Typical (Type 1) cases conform to the original definition of PSP. Type 2, atypical cases are variants of the histological changes characteristic of PSP: either the severity or the distribution of abnormalities, or both of these deviate from the typical pattern. Cases with combined pathology belong to type 3 group: in these the typical pathology of PSP is accompanied by lesions characteristic of another neurodegenerative or vascular disease.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Preview
Unable to display preview. Download preview PDF.
Similar content being viewed by others
References
Akashi T, Arima K, Maruyama N, Ando S, Inose T (1989) Severe cerebral atrophy in progressive supranuclear palsy: a case report. Clin Neuropathol 8: 195–199.
Arai N (1989) “Grumose degeneration” of the dentate nucleus. A light and electron microscopic study in progressive supranuclear palsy and dentatorubropallidoluysial atrophy. J Neurol Sci 90: 131–145.
Bancher C, Lassmann H, Budka H, et al (1987) Neurofibrillary tangles in Alzheimer’s disease and progressive supranuclear palsy: antigenic similarities and differences. Acta Neuropathol 74: 39–46.
Barr AN (1986) Progressive supranuclear palsy. In: Vinken PJ, Bruyn GW, Klawans HJ (eds) Handbook of clinical neurology, vol 5(49). Extrapyramidal disorders. Elsevier, Amsterdam, pp 239–254.
Brown J, Lantos P, Stratton M, Roques P, Rossor M (1993) A familial dementia with progressive supranuclear palsy pathology. J Neurol Neurosurg Psychiatry 56: 473–476.
Cruz-Sanchez FF, Rossi ML, Cardozo A, Deacon P, Tolosa E (1992) Clinical and pathological study of two patients with progressive supranuclear palsy and Alzheimer’s changes. Antigenic determinants that distinguish cortical and subcortical neurofibrillary tangles. Neurosci Lett 136: 43–46.
Dubas F, Gray F, Escourolle R (1983) Maladie de Steele-Richardson-Olszewski sans ophtalmoplégie. Six cas anatomo-cliniques. Rev Neurol 139: 407–416.
Fearnley JM, Lees AJ (1991) Ageing and Parkinson’s disease: substantia nigra regional selectivity. Brain 114: 2283–2301.
Flament S, Delacourte A, Veray M, Hauw J-J, Javoy-Agid F (1991) Abnormal tau protein in progressive supranuclear palsy. Similarities and differences with the neurofibrillary degeneration of the Alzheimer type. Acta Neuropathol 81: 591–596.
Giaccone G, Tagliavini F, Street JS, Ghetti B, Bugiani O (1988) Progressive supranuclear palsy with hypertrophy of the olives. An immunocytochemical study of the cytoskeleton of argyrophilic neurons. Acta Neuropathol 77: 14–20.
Golbe LI, Davis PH, Schoenberg BS, Duvoisin RC (1988) Prevalence and natural history of progressive supranuclear palsy. Neurology 38: 1031–1034.
Hauw J-J, Verny M, Delaère P, Cervera P, He Y, Duyckaerts C (1990) Constant neurofibrillary changes in the neocortex in progressive supranuclear palsy. Basic differences with Alzheimer’s disease and aging. Neurosci Lett 119: 182–186.
Hirsch EC, Graybiel AM, Duyckaerts C, Javoy-Agid F (1987) Neuronal loss in the pedunculopontine tegmental nucleus in Parkinson disease and in progressive supra-nuclear palsy. Proc Natl Acad Sci USA 84: 5976–5980.
Hynd EW, Pirozzolo FJ, Maletta GJ (1982) Progressive supranuclear palsy. Int J Neurosci 16: 87–98.
Jackson JA, Jankovic J, Ford J (1983) Progressive supranuclear palsy: clinical features and response to treatment in 16 patients. Ann Neurol 13: 273–278.
Jellinger K, Riederer P, Tomonaga M (1980) Progressive supranuclear palsy: clinico-pathological and biochemical studies. J Neural Transm [Suppl] 16: 111–128.
Jellinger K (1971) Progressive supranuclear palsy (subcortical argyrophilic dystrophy). Acta Neuropathol 19: 347–352.
Jellinger K (1988) The pedunculopontine nucleus in Parkinson’s disease, progressive supranuclear palsy and Alzheimer’s disease. J Neurol Neurosurg Psychiatry 52: 540–543.
Kato T, Hirano A, Weinberg MN, Jacobs AK (1986) Spinal cord lesions in progressive supranuclear palsy: some new observations. Acta Neuropathol 71: 11–14.
Kleinschmidt-DeMasters BK (1989) Early progressive supranuclear palsy: pathology and clinical presentation. Clin Neuropathol 8: 79–84.
Kristensen MO (1985) Progressive supranuclear palsy—20 years later. Acta Neurol Scand 71: 177–189.
Leigh PN, Probst A, Dale GE, et al (1989) New aspects of pathology of neuro-degenerative disorders as revealed by ubiquitin antibodies. Acta Neuropathol 79: 61–72.
Lennox G, Lowe J, Morrell K, Landon M, Mayer RJ (1988) Ubiquitin is a component of neurofibrillary tangles in a variety of neurodegenerative diseases. Neurosci Lett 94: 211–217.
Love S, Saitoh T, Quijada S, Cole GM, Terry RD (1988) Alz-50, ubiquitin and tau immunoreactivity of neurofibrillary tangles, Pick bodies and Lewy bodies. J Neuropathol Exp Neurol 47: 393–405.
Maher ER, Lees AJ (1986) The clinical features and natural history of the Steele-Richardson-Olszewski syndrome (progressive supranuclear palsy). Neurology 36: 1005–1008.
Malessa S, Hirsch EC, Cervera P, et al (1991) Progressive supranuclear palsy: loss of choline acetyltransferase-like immunoreactive neurons in the pontine reticular formation. Neurology 41: 1593–1597.
Manetto V, Perry G, Tabaton M, et al (1988) Ubiquitin is associated with abnormal cytoplasmic filaments characteristic of neurodegenerative disease. Proc Natl Acad Sci USA 85: 4501–4505.
Mann DMA, Yates PO, Hawkes J (1983) The pathology of the human locus coeruleus. Clin Neuropathol 2: 1–7.
Mann DMA, Jones D (1990) Deposition of amyloid (A4) protein within the brains of persons with dementing disorders other than Alzheimer’s disease and Down’s syndrome. Neurosci Lett 109: 68–75.
Mastaglia FL, Grainger K, Kee F, Sadka M, Lefroy R (1973) Progressive supranuclear palsy (the Steele-Richardson-Olszewski syndrome): clinical and electrophysiological observations in eleven cases. Proc Aust Assoc Neurol 10: 35–44.
Milder DG, Elliott CF, Evans WA (1984) Neuropathological findings in a case of coexistent progressive supranuclear palsy and Alzheimer’s disease. Clin Exp Neurol 20: 181–187.
Mizusawa H, Yen S-H, Hirano A, Llena JF (1989) Pathology of the dentate nucleus in progressive supranuclear palsy: a histological, immunohistochemical and ultra-structural study. Acta Neuropathol 78: 419–428.
Montpetit V, Clapin DF, Guberman A (1985) Substructure of 20 nm filaments of progressive supranuclear palsy. Acta Neuropathol 68: 311–318.
Mori H, Yoshimura M, Tomonaga M, Yamanouchi H (1986) Progressive supranuclear palsy with Lewy bodies. Acta Neuropathol 71: 344–346.
Oyanagi K, Takahashi H, Wakabayashi K, Ikuta F (1988) Selective decrease of large neurons in the neostriatum in progressive supranuclear palsy. Brain Res 458: 218–223.
Probst A, Langui D, Lautenschlager C, Ulrich J, Brion JP, Anderton BH (1988) Progressive supranuclear palsy: extensive neuropil threads in addition to neuro-fibrillary tangles. Very similar antigenicity of subcortical neuronal pathology in progressive supranuclear palsy and Alzheimer’s disease. Acta Neuropathol 77: 61–68.
Pollock NJ, Mirra SS, Binder LI, Hansen LA, Wood JG (1986) Filamentous aggregates in Pick’s disease, progressive supranuclear palsy, and Alzheimer’s disease share antigenic determinants with microtubule-associated protein, tau. Lancet ii: 1211.
Posey WC (1904) Paralysis of the upward movement of the eyes. Ann Ophthal 13: 523–531.
Schmidt MK, Lee VM-Y, Hurtig H, Trojanowski JQ (1988) Properties of antigenic determinants that distinguish neurofibrillary tangles in progressive supranuclear palsy and Alzheimer’s disease. Lab Invest 59: 460–466.
Shin R-W, Kitamoto T, Tateishi J (1991) Modified tau is present in younger nondemented persons: a study of subcortical nuclei in Alzheimer’s disease and progressive supranuclear palsy. Acta Neuropathol 81: 517–523.
Spiller WG (1905) The importance in clinical diagnosis of paralysis of associated movements of the eyeballs (Blick-Lahmung), especially of upward and downward associated movements. J Nerv Ment Dis 32: 417–448 and 497-530.
Steele JC, Richardson JC, Olszewski T (1964) Progressive supranuclear palsy. Arch Neurol 10: 333–359.
Steele JC (1975) Progressive supranuclear palsy. In: Vinken PJ, Bruyn GW, deJong JMB (eds) Handbook of clinical neurology, vol 22. System disorders and atrophies, part II North Holland, Amsterdam, pp 217–229.
Takahashi H, Oyanagi K, Takedo S, Hinokuma K, Ikuta F (1989) Occurrence of 15-nm—wide straight tubules in neocortical neurons in progressive supranuclear palsy. Acta Neuropathol 79: 233–239.
Takahashi H, Takeda S, Ikuta F, Homma Y (1987) Progressive supranuclear palsy with limbic system involvement: report of a case with ultrastructural investigation of neurofibrillary tangles in various locations. Clin Neuropathol 6: 271–276.
Tagliavini F, Pilleri G, Bouras C, Constantinidis J (1984) The basal nucleus of Meynert in patients with progressive supranuclear palsy. Neurosci Lett 44: 37–42.
Tan N, Mastaglia FL, Masters CL, Beyreuther K, Kakulas BA (1988) Amyloid (A4) protein deposition in brain in progressive supranuclear palsy (PSP). Alzheimer Dis Assoc Dis 2: 264.
Tellez-Nagel I, Wisniewski HM (1973) Ultrastructure of neurofibrillary tangles in Steele-Richardson-Olszewski syndrome. Arch Neurol 29: 324–327.
Tomonaga M (1977) Ultrastructure of neurofibrillary tangles in progressive supranuclear palsy. Acta Neuropathol 37: 177–181.
Tomonaga M (1983) Neuropathology of the locus coeruleus: a semi-quantitative study. J Neurol 230: 231–240.
Will RG, Lees AJ, Gibb W, Barnard RO (1988) A case of progressive subcortical gliosis presenting clinically as Steele-Richardson-Olszewski syndrome. J Neurol Neurosurg Psychiatry 51: 1224–1227.
Yagishita S, Itoh Y, Amano N, Nakano T, Saitoh A (1979) Ultrastructure of neurofibrillary tangles in progressive supranuclear palsy. Acta Neuropathol 48: 27–30.
Yagashita S, Itoh Y, Nakano T (1986) Hypertrophy of the olivary nucleus. An ultra-sctructural study. Acta Neuropathol 69: 132–138.
Yamamoto Y, Kawamura J, Hashimoto S, Nakamura H, Kobashi Y, Ichijima K (1991) Pallido-nigro-luysian atrophy, progressive supranuclear palsy and adult onset Hallervorden-Spatz disease: a case of akinesia as a predominant feature of par-kinsonism. J Neurol Sci 101: 98–106.
Zweig RM, Whitehouse PJ, Casanova MF, Walker LC, Jankel WR, Price DL (1987) Loss of pedunculopontine neurons in progressive supranuclear palsy. Ann Neurol 22: 18–25.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 1994 Springer-Verlag Wien
About this paper
Cite this paper
Lantos, P.L. (1994). The neuropathology of progressive supranuclear palsy. In: Tolosa, E., Duvoisin, R., Cruz-Sánchez, F.F. (eds) Progressive Supranuclear Palsy: Diagnosis, Pathology, and Therapy. Journal of Neural Transmission. Supplementa, vol 42. Springer, Vienna. https://doi.org/10.1007/978-3-7091-6641-3_11
Download citation
DOI: https://doi.org/10.1007/978-3-7091-6641-3_11
Publisher Name: Springer, Vienna
Print ISBN: 978-3-211-82541-9
Online ISBN: 978-3-7091-6641-3
eBook Packages: Springer Book Archive