Abstract
Organic cation transporters (OCTs) of the solute carrier family (SLC) 22 and multidrug and toxin extrusion (MATE) transporters of the SLC47 family have been identified as uptake and efflux transporters, respectively, for xenobiotics including several clinically used drugs such as the antidiabetic agent metformin, the antiviral agent lamivudine, and the anticancer drug oxaliplatin. Expression of human OCT1 (SLC22A1) and OCT2 (SLC22A2) is highly restricted to the liver and kidney, respectively. By contrast, OCT3 (SLC22A3) is more widely distributed. MATEs (SLC47A1, SLC47A2) are predominantly expressed in human kidney. Data on in vitro studies reporting a large number of substrates and inhibitors of OCTs and MATEs are systematically summarized. Several genetic variants of human OCTs and in part of MATE1 have been reported, and some of them result in reduced in vitro transport activity corroborating data from studies with knockout mice. A comprehensive overview is given on currently known genotype–phenotype correlations for variants in OCTs and MATE1 related to protein expression, pharmacokinetics/-dynamics of transporter substrates, treatment outcome, and disease susceptibility.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Drug transporters
- Organic cation transport
- Excretion
- OCT1
- OCT2
- OCT3
- MATE1
- MATE2-K
- Liver
- Kidney
- tissue distribution
- Knockout mice
- Pharmacogenomics
- Genotype–phenotype correlation
- Metformin
- Single nucleotide polymorphisms
- Drug response
- Interindividual variability
- Drug–drug interaction
- Pharmacokinetics
1 Introduction
A large number of clinically used drugs are administered orally, from which approximately 40% are cations or weak bases at physiological pH (Neuhoff et al. 2003). For absorption, distribution, metabolism, and elimination (ADME), they need to be taken up into and effluxed from various cell types in the body. Several families of membrane transporters have been recognized to play a role in the transport of organic cations across the plasma membrane. These include members of the solute carrier (SLC) family 22 (organic cation transporters, OCTs) and of the SLC family 47 (multidrug and toxin extrusion, MATEs) (Koepsell et al. 2007). The human SLC22 family can be divided into several subgroups according to substrates and transport mechanisms (Koepsell and Endou 2004) (Fig. 1). One subgroup comprises OCT1, OCT2, and OCT3, which translocate organic cations and weak bases in an electrogenic manner. Human MATE transporters have only recently been identified as proton/cation antiporters participating in the excretion of organic cations in the liver and kidney (Otsuka et al. 2005; Masuda et al. 2006). Alterations in the expression and function of these transporters may significantly contribute to drug pharmacokinetics and the interindividual variability of drug response. This review summarizes current knowledge about the molecular characteristics, tissue distribution, (drug) substrates and inhibitors, drug–drug interactions, and the fast-growing field of pharmacogenomics of human OCT and MATE transporters.
Phylogenetic tree of the 23 transporters of the human SLC22 family. Protein sequences were downloaded from the NCBI gene database and aligned with the ClustalX2 program (Larkin et al. 2007). The tree was drawn with the “drawtree” program of the PHYLIP3.67 program package (http://evolution.genetics.washington.edu/phylip.html). The distance along the branches is inversely correlated to the degree of sequence identity. For example, the amino acid sequence identity of OCT1 and OCT2 is 70% and that of OCT1 and URAT1 31%. Electrogenic cation transporters are marked by black boxes, transporters for organic cations and carnitine by gray boxes, and transporters for organic anions by white boxes. Transporters whose function is as yet unknown are unmarked
2 Cloning and Molecular Characterization of OCT and MATE Transporters
A large number of physiological and biochemical studies had suggested the presence of different carrier systems mediating the transport of organic solutes in hepatocytes and renal proximal tubule cells (Giacomini et al. 1988; Boyer et al. 1992). However, molecular identification of these transporters succeeded not until molecular biology techniques became available in the late 1980s. The first member of the electrogenic OCT family was isolated from rat kidney by expression cloning (Gründemann et al. 1994). It took another 11 years until Otsuka et al. identified in 2005 human orthologs of the bacterial MATE family as proton/organic cation exchangers responsible for the electroneutral transport of organic cations into bile and urine.
2.1 OCT Transporters
The genes encoding human OCT1 (gene symbol: SLC22A1), OCT2 (SLC22A2), and OCT3 (SLC22A3) are located in a cluster on chromosome 6q26–q27 and have a common structure of 11 coding exons and 10 introns (Koehler et al. 1997; Gründemann et al. 1998; Hayer et al. 1999; Verhaagh et al. 1999; Gründemann and Schömig 2000). The amino acid sequence identity of OCT1 and OCT2 is 70%, and 50% for both OCT1/OCT3 and OCT2/OCT3. OCT orthologs have been cloned from other mammalian species as well (Koepsell et al. 2007) (Fig. 2).
OCT1 orthologs in different vertebrates. The phylogenetic tree on the left was constructed from OCT1/Oct1 protein sequences aligned using the ClustalX2 program (Larkin et al. 2007) and drawn with the “drawgram” program of the PHYLIP3.67 program package (http://evolution.genetics.washington.edu/phylip.html). The sequence comparison on the right shows the aligned sequences in the vicinity of amino acid arginine 61, which is highly conserved among species. A genetic variant was identified in human OCT1 that leads to a nonsynonymous exchange of arginine 61 to a cysteine (Kerb et al. 2002; Shu et al. 2003). OCT1-Cys61 shows a reduced in vitro transport function (Kerb et al. 2002; Shu et al. 2003, 2007), is associated with a significant decrease of hepatic OCT1 protein levels (Nies et al. 2009), and affects metformin pharmacokinetics in humans (Shu et al. 2008). For further details see Tables 4–12. The following protein sequences were used for alignments: human NP_003048; orangutan ENSPPYP00000019207; chimpanzee XP_527554; rhesus monkey ENSMMUP00000020546; dog XP_850971; mouse NP_033228; rat NP_036829; cow NP_001094568; pig NP_999154; elephant ENSLAFP00000009760; cat ENSFCAP00000002624; chicken XP_419621; rabbit ENSOCUP00000002189; bushbaby ENSOGAP00000004719; squirrel ENSSTOP00000008083; zebrafish ENSDARP00000048889. Accession numbers are either from the ENSEMBL genome server (http://www.ensembl.org; numbers starting with “ENS”) or from the “Protein” database at http://www.ncbi.nlm.nih.gov/entrez. Sequences from elephant, cat, rabbit, bushbaby, and squirrel are in part incomplete
Based on sequence and hydropathy analyses, OCTs have a predicted topology comprising 12 transmembrane helices, an intracellular amino and carboxyl terminus, and a large glycosylated extracellular loop between the first two transmembrane helices (Fig. 3a). The large intracellular loop between transmembrane helix 6 and 7 carries several putative phosphorylation sites that are used for short-term modulation of OCT activity (Koepsell et al. 2007; Ciarimboli 2008). Employing detailed mutagenesis and modeling of the tertiary structure in analogy to the crystallized structure of lactose permease from Escherichia coli (Abramson et al. 2003), several amino acids in the 4th, 10th, and 11th transmembrane helix of rat Oct1 were identified that are involved in substrate and/or inhibitor binding (Gorboulev et al. 1999, 2005; Popp et al. 2005; Sturm et al. 2007; Volk et al. 2009). These amino acids are localized within the center of a large cleft that may exist in an outward- or inward-facing conformation. The cleft contains high- and low-affinity substrate and/or inhibitor binding sites (Popp et al. 2005; Gorbunov et al. 2008; Minuesa et al. 2009; Volk et al. 2009). Whereas the affinities of the low-affinity substrate binding sites are in the same range as the respective Michaelis-Menten constant values, the high-affinity binding sites may have a 10,000-fold higher affinity. The different substrate and inhibitor binding sites overlap and may exhibit competitive or allosteric interactions. Both the low- and high-affinity sites may be inhibitory (Minuesa et al. 2009). High-affinity binding sites may be also involved in transport since for inhibition of organic cation transport different IC50 values may be obtained when the uptake measurements were performed using different substrate concentrations far below the respective K m values (see e.g. Table 2: inhibition of OCT2-mediated MPP uptake by flecainide or quinidine). The existence of various substrate and inhibitor binding sites and the complex interactions between different sites explains why largely different IC50 values were obtained for individual transporters when different substrates were used for transport measurements (see, e.g., Tables 1–2: inhibition of OCT1-mediated TEA uptake versus MPP uptake by dopamine or histamine, or inhibition of OCT1-mediated TEA uptake vs. ASP uptake by quinidine). Many naturally occurring genetic variants of human OCT1, OCT2, and OCT3 exist that encode transporters with changed functions (Sect. 6).
Predicted membrane topology models of human OCT1 (a) and human MATE1 (b). Topology prediction was performed with the TMHMM algorithm (http://www.cbs.dtu.dk/services/TMHMM-2.0) and the model was drawn with TOPO2 (http://www.sacs.ucsf.edu/TOPO-run/wtopo.pl). (a) Tree-like structures indicate the location of putative N-glycosylation sites in OCT1. OCT2 and OCT3 have similar predicted secondary structures as OCT1. (b) There are no putative N-glycosylation sites in MATE1. Thirteen transmembrane segments are also predicted for human MATE2 and for most of the orthologs from other mammalian species (Terada and Inui 2008)
2.2 MATE Transporters
The human MATE1 gene (SLC47A1) and the MATE2 gene (SLC47A2) are located in tandem on chromosome 17p11.2 and encode proteins of 570 and 602 amino acids, respectively (Otsuka et al. 2005). The amino acid sequence identity of MATE1 and MATE2 is 47.5%. Two additional human MATE2 isoforms have been cloned: MATE2-K (NM_001099646) coding for a 566-amino acid protein and MATE2-B encoding a truncated protein of 220 amino acids (Masuda et al. 2006). Of note, MATE2-K is currently the only isoform in the MATE2 subfamily, for which function has been demonstrated; MATE2-B is nonfunctional and MATE2 function has not been tested (Masuda et al. 2006; Tanihara et al. 2007). MATE orthologs have also been cloned from other mammalian species, including mouse (Otsuka et al. 2005; Kobara et al. 2008), rat (Terada et al. 2006; Ohta et al. 2006), and rabbit (Zhang et al. 2007).
The hydropathy analysis performed by Otsuka et al. (2005) suggested that MATE1 consists of 12 transmembrane helices. However, most of the current topology analysis programs predict 13 transmembrane helices with an extracellular location of the carboxyl terminus (Zhang et al. 2007; Terada and Inui 2008) (Fig. 3b). Immunocytochemical analyses using accessibility of an antibody to a carboxyl-terminal tag in nonpermeabilized cells proved the extracellular location of the carboxyl terminus of rabbit Mate1 (Zhang et al. 2007). Whether this holds true for other MATE orthologs awaits investigation. Several histidine, cysteine, and glutamate residues in different transmembrane helices of human MATE1 and MATE2-K are apparently involved in substrate binding and/or transport (Asaka et al. 2007; Matsumoto et al. 2008). As for the OCTs, naturally occurring genetic variants have been identified in human MATEs that lead to synthesis of functionally impaired transporters (Sect. 6).
3 Tissue Distribution and Subcellular Localization
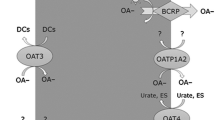
By screening the abundance of human transcript sequences (“UniGene” database at http://www.ncbi.nlm.nih.gov) one can assess the approximate gene expression pattern for each OCT and MATE transporter. Northern blot and real-time quantitative PCR analyses have revealed the different mRNA expression profiles in more detail (Koepsell et al. 2007; Okabe et al. 2008). In addition to the mRNA expression profiles, knowledge of the protein expression profiles and the subcellular localization of each transporter in distinct cell types of a given tissue are of equal importance, and they have been analyzed to some extent as well. Although each cell is equipped with a number of different transporters, it is of particular interest to identify transporters in the absorptive and secretory cells of the small intestine, liver, and kidney, because these are the major organs of drug absorption, metabolism, and excretion. The combined action of electrogenic OCT uptake and MATE efflux transporters, which function as proton/cation antiporters, results in the transcellular movement of organic cations in the small intestine, liver, and kidney (Fig. 4).
Localization of OCT and MATE transporters in human hepatocytes (a) and proximal tubule epithelial cells in the kidney (b). The basolateral localization of OCT1 and OCT3 in hepatocytes and of OCT2 in proximal tubule epithelial cells together with the apical localization of MATE transporters results in the transcellular movement and, thereby, secretion of organic cations into bile and urine. MDR1 P-glycoprotein (ABCB1) is an ATP-dependent efflux pump for organic cations. In addition, OCTN1 (SLC22A4) and OCTN2 (SLC22A5) are present in the luminal membrane of proximal tubule cells, where they may exchange luminal carnitine plus sodium or luminal cations against intracellular cations. An apical OCT1 localization in proximal tubule cells was recently reported and was suggested to be involved in reabsorption of metformin from the urine
Because OCTs and MATEs also transport cationic cytostatic drugs such as platinum drugs (see Sect. 4), transporter expression may affect intracellular levels of anticancer drugs and, thus, response to chemotherapy. Therefore, several studies have analyzed transporter expression profiles in cancer-derived cells as well as in normal tissue in comparison to cancerous tissue (Hayer-Zillgen et al. 2002; Zhang et al. 2006; Ballestero et al. 2006; Yokoo et al. 2008; Okabe et al. 2008). Only recently, OCT1 expression was identified as an important clinical determinant of the response to imatinib in chronic myeloid leukemia (Wang et al. 2008a) (see Sect. 6).
3.1 OCT1
Rat Oct1, the first cloned member of the SLC22A family, is strongly expressed in liver, kidney, and intestine (Gründemann et al. 1994). In humans, on the contrary, OCT1 mRNA is most prominently expressed in the liver (Gorboulev et al. 1997; Nishimura and Naito 2005; Jung et al. 2008; Nies et al. 2009). The OCT1 protein has been localized in the sinusoidal (basolateral) membrane of rat and human hepatocytes (Meyer-Wentrup et al. 1998; Nies et al. 2008), where it mediates the uptake of substrates from the blood and, thereby, mediates the first step in hepatic excretion of many cationic drugs (Fig. 4a). Other reported locations of human OCT1 include the lateral membrane of intestinal epithelial cells (Müller et al. 2005) and the luminal (apical) membrane of ciliated cells in the lung (Lips et al. 2005) and of tubule epithelial cells in the kidney (Tzvetkov et al. 2009).
3.2 OCT2
Human OCT2 mRNA is most strongly expressed in kidney (Gorboulev et al. 1997; Nishimura and Naito 2005; Jung et al. 2008), where the OCT2 protein has been localized in the basolateral membrane of proximal tubule epithelial cells (Motohashi et al. 2002; Nies et al. 2008). Analogous to OCT1 in hepatocytes, OCT2 plays an important role in the secretion of organic cations in the kidney by mediating the first step, that is, the uptake of organic cations across the basolateral membrane (Fig. 4b). OCT2 transcripts were also detected in several other human organs, including small intestine, lung, and different brain regions, and the inner ear (Gorboulev et al. 1997; Busch et al. 1998; Lips et al. 2005; Taubert et al. 2007; Ciarimboli et al. 2010). The human OCT2 protein has been localized in the luminal membrane of ciliated epithelial cells in the lung (Lips et al. 2005) and in pyramidal cells of the hippocampus (Busch et al. 1998).
3.3 OCT3
Human OCT3 was initially cloned from a kidney-derived cell line and termed extraneuronal monoamine transporter (EMT) because substrate specificity is similar to monoamine uptake measured in extraneuronal tissues, neuronal expression of OCT3 was not established, and it was not known that monoamines are also transported by OCT2 (Gründemann et al. 1998); for discussion see Koepsell et al. (2003). Unlike OCT1 and OCT2, OCT3 has a broad tissue distribution (Verhaagh et al. 1999; Nies et al. 2009) and transcripts have been detected, among others, in placenta, adrenal gland, liver, kidney, heart, lung, brain, and intestine (Koepsell et al. 2007). The human OCT3 protein was identified in basolateral membrane vesicles from placenta (Sata et al. 2005), in the plasma membrane of normal human astrocytes (Inazu et al. 2003), in the luminal membrane of bronchial and intestinal epithelial cells (Müller et al. 2005; Lips et al. 2005), and in the sinusoidal membrane of hepatocytes (Nies et al. 2009) (Fig. 4).
3.4 MATE1 and MATE2-K
Human MATE1 is strongly expressed in liver and kidney as well as in skeletal muscle, adrenal gland, and testis (Otsuka et al. 2005; Masuda et al. 2006). Immunolocalization analyses identified the MATE1 protein in the canalicular membrane of hepatocytes (Otsuka et al. 2005) and in the luminal membrane of tubular epithelial cells in the kidney (Otsuka et al. 2005; Masuda et al. 2006). Human MATE2-K is almost exclusively expressed in the kidney and is localized in the luminal membrane of proximal tubular epithelial cells (Masuda et al. 2006) (Fig. 4).
4 Functional Characterization of OCT and MATE Transporters
4.1 Common Functional Properties of OCTs
The functional characteristics of OCTs have been studied in detail using cRNA-injected Xenopus laevis oocytes or OCT-transfected mammalian cell lines. Several transport characteristics are shared by all OCTs irrespective of their subtype or the species. OCTs transport a broad range of organic cations with diverse molecular structures exhibiting K m values in the micro- to millimolar range (Tables 1–3). Typically, the relative molecular masses of the substrates are below 500 (Suhre et al. 2005; Schmitt and Koepsell 2005; Ahlin et al. 2008; Zolk et al. 2008). OCTs are electrogenic facilitative diffusion systems that translocate organic cations in both directions across the plasma membrane (Busch et al. 1996; Nagel et al. 1997; Kekuda et al. 1998; Budiman et al. 2000; Lips et al. 2005). Transport of organic cations by OCTs is driven by the electrochemical potential but not accelerated by gradients of sodium or protons. For rat Oct2, a nonselective cotranslocation of inorganic cations together with transported organic cation substrates has been observed under depolarized conditions (Schmitt et al. 2009). OCTs are inhibited by a large number of cations and uncharged compounds that are not transported themselves. Partial or total inhibition of transport activity may be achieved (Volk et al. 2009). Transport inhibition may be competitive, partial competitive, or noncompetitive. Importantly, the affinities of the inhibitors are also dependent on the transported substrate (Tables 1–3). For human OCTs, IC50 values between 10 pM and 24 mM have been determined. Transported substrates and inhibitors of OCTs are of endogenous origin, xenobiotics, and clinically used drugs.
4.2 Substrate and Inhibitor Specificities of Human OCTs
Human OCT1, OCT2, and OCT3 have largely overlapping but distinctly different substrate and inhibitor specificities (Tables 1–3). The substrates of human OCTs (hOCT) are typically organic cations with one positive charge or two positive charges (furamidine and paraquat) or weak bases that are positively charged at physiological pH (Tables 1–3). Noncharged compounds such as cimetidine at alkaline pH (Barendt and Wright 2002) may also be transported. Whether OCTs may be also able to transport organic anions remains to be clarified. Transport of prostaglandins by hOCT1 and hOCT2 has been reported by Kimura et al. (2002) but was not confirmed by Harlfinger et al. (2005).
Transported endogenous substrates of human OCTs include monoamine neurotransmitters, neuromodulators, and other compounds such as choline, creatinine, and guanidine. Among the >120 clinically used drugs that were shown to interact with human OCTs, about 20 were identified as transport substrates (Table 2). These include antineoplastic platinum compounds, the histamine H2 receptor antagonist cimetidine, the antiviral drugs acyclovir, ganciclovir, lamivudine, and zalcitabine, the antidiabetic drug metformin, and the antiarrhythmic drug quinidine. The neurotoxin 1-methyl-4-phenyl pyridinium (MPP), the antidiabetic drug metformin, and the antiviral drug lamivudine are transported with similar affinities by the three human OCT orthologs. The model cation TEA is transported with similar affinities by hOCT1 and hOCT2 but shows low-affinity interaction with hOCT3. At variance, epinephrine and norepinephrine are transported with similar affinity by hOCT2 and hOCT3, and only exhibit low-affinity interactions with hOCT1. Histamine is transported with higher affinity by hOCT3 compared to hOCT2 and is apparently not transported by hOCT1 (Koepsell et al. unpublished data).
Inhibitors of OCTs may have larger molecular weights compared to substrates. They may bind to the central substrate binding pockets of the OCTs or to more peripheral regions in the clefts. Two or more inhibitor molecules may bind at the same time. Transport of a specific substrate may be inhibited partially after inhibitor binding to a high-affinity site and total inhibition may be observed when the inhibitor has bound to the low-affinity site (Minuesa et al. 2009).
It may be difficult to distinguish whether a compound that inhibits an OCT transporter is translocated or not. The reasons are (1) that transport rates may be low, (2) that the expression of endogenous cation transporters may be different in transfected and nontransfected cell lines, and (3) that OCT inhibitors that inhibit control substrates may have different affinities for other substrates. It has to be kept in mind that a correlation between transporter expression and the effect of a drug that interacts with the transporter does not prove that the drug is transported because the transporter inhibition may block cellular uptake of an endogenous compound that may critically influence drug effects on cell functions.
Thomas et al. (2004) observed that compounds that inhibit OCTs decreased uptake of imatinib, a first-generation tyrosine kinase inhibitor, into a human T-cell lymphoblast-like cell line. Similarly, imatinib uptake into blood cells from patients with chronic-phase chronic myeloid leukemia (CML) was blocked by OCT inhibitors (White et al. 2006). When the CML cell line KCL22 was transfected with hOCT1, imatinib uptake was about 1.6-fold higher compared to uptake into control transfectants (Wang et al. 2008a). At variance, expression of hOCT1 in X. laevis oocytes or in human embryonic kidney cells did not lead to a significant increase of imatinib uptake (Hu et al. 2008 and Koepsell, Nies, et al. unpublished data). Independent from the conflicting transport data, it was demonstrated that OCT1 mRNA levels and OCT1 genotype are important clinical determinants of treatment response in CML patients (Wang et al. 2008a; Kim et al. 2009) (Sect. 6.3).
4.3 Drug–Drug Interactions Involving OCTs
Various clinically used drugs were identified as inhibitors of OCT-mediated transport by investigating their potency to inhibit in vitro uptake of transported cations (Table 2). When these inhibitory drugs are coprescribed with drugs that are transported by OCTs, drug pharmacokinetics may be altered. Several studies, therefore, investigated the ability of drugs to inhibit transport of the OCT drug substrates metformin or cimetidine in vitro. For example, OCT2-mediated cimetidine transport is inhibited by ranitidine (Tahara et al. 2005) and OCT2-mediated metformin transport by sodium channel blockers (Umehara et al. 2008), β-adrenergic receptor antagonists (Bachmakov et al. 2009), and cimetidine (Zolk et al. 2009). The oral antidiabetics repaglinide and rosiglitazone inhibit OCT1-mediated metformin transport (Bachmakov et al. 2008).
Clinical studies suggest that drug–drug interactions involving OCTs also occur in vivo and may mainly affect cationic drugs that are predominantly eliminated by renal secretion (Ayrton and Morgan 2008; Kindla et al. 2009). For example, cimetidine decreases the renal tubular secretion of ranitidine (van Crugten et al. 1986), procainamide (Lai et al. 1988), dofetilide (Abel et al. 2000), and varenicline (Feng et al. 2008). The inhibition of tubular secretion of metformin by cimetidine was first described more than 20 years ago (Somogyi et al. 1987), but only recently this drug–drug interaction was attributed to OCT2 (Wang et al. 2008b). Other in vivo drug–drug interactions were reported between lamivudine and trimethoprim and between cisplatin and cimetidine or imatinib. It was shown that renal lamivudine clearance was decreased after coadministration of trimethoprim (Moore et al. 1996) and that the concomitant administration of imatinib has a protective effect against cisplatin-induced nephrotoxicity and ototoxicity (Tanihara et al. 2009; Ciarimboli et al. 2010).
4.4 Common Functional Properties of MATEs
MATE transporters are electroneutral transporters that operate independently of a sodium gradient, but use an oppositely directed proton gradient as driving force; translocation of organic cations across the plasma membrane may occur in both directions (Otsuka et al. 2005; Tanihara et al. 2007). MATEs are apparently the functionally long known but searched for proton-driven cation efflux transporters of the canalicular hepatocyte membrane and the luminal membrane of proximal tubule epithelial cells, which have been functionally described for many years (Koepsell 1998; Otsuka et al. 2005).
4.5 Substrate and Inhibitor Specificities of MATEs
MATE1 and MATE2-K have similar substrate and inhibitor specificities, which overlap with those of OCTs (Tables 1–3). The OCT substrates MPP and TEA are also transported by the two MATE orthologs. Endogenous substrates include the organic cations creatinine, guanidine, thiamine, and also the organic anion estrone sulfate. About 30 clinically used drugs have been shown to interact with MATE transporters, and several were identified as transport substrates such as metformin, cimetidine, oxaliplatin, acyclovir, and fexofenadine (Table 2).
4.6 Drug–Drug Interactions Involving MATEs
Information of drug–drug interactions involving MATEs is currently limited. In vitro, cimetidine inhibits MATE1-mediated transport of fexofenadine (Matsushima et al. 2009) and metformin (Tsuda et al. 2009b). Thus, the clinical observation that metformin tubular secretion is inhibited by cimetidine (Somogyi et al. 1987) may not only be due to inhibition of OCT2-mediated metformin uptake (Wang et al. 2008b) but also to inhibition of MATE1-mediated luminal metformin efflux (Tsuda et al. 2009b).
5 Knockout Mouse Models
Knockout mouse models are valuable tools to identify the physiological and pharmacokinetic roles of transporters in vivo. For that purpose, Oct1 (Jonker et al. 2001; Shu et al. 2007), Oct2 (Jonker et al. 2003), Oct3 (Zwart et al. 2001; Wultsch et al. 2009), and Mate1 (Tsuda et al. 2009a) single-knockout mice and Oct1/Oct2 double-knockout mice (Jonker et al. 2003) have been generated. All strains are viable and fertile and show no apparent phenotypical abnormalities, indicating that none of the transporters is essential for obvious physiological functions in mice. However, the tissue distribution and disposition of endogenous or exogenous organic cations may differ significantly between wild-type mice and the knockout mouse strains. These knockout mouse models may be used for the prediction of pharmacokinetics in humans, especially in those carrying genetic variants that encode transporters with reduced function (Sect. 6).
5.1 Oct1 Knockout Mice
Intravenous injection of the model cation TEA into Oct1(−/−) mice resulted in a fourfold to sixfold reduced hepatic accumulation and in a twofold reduced direct intestinal excretion of TEA in comparison to wild-type mice (Jonker et al. 2001). On the other hand, urinary TEA excretion was increased, probably because lack of hepatic Oct1 leads to increased availability of TEA to the kidney. Similar to TEA, the levels of the anticancer drug meta-iodobenzylguanidine, the neurotoxin MPP (Jonker et al. 2001), and the antidiabetic drug metformin (Wang et al. 2002; Shu et al. 2007) were also lower in livers from Oct1(−/−) mice than in those from wild-type mice. The decreased hepatic metformin uptake resulted in a reduced effect on AMP-activated protein kinase phosphorylation and gluconeogenesis, and, in consequence, the glucose-lowering effect of metformin was completely abolished (Shu et al. 2007). Thus, mouse Oct1 – as well as human OCT1 (see Sect. 6) – is a major determinant of the pharmacodynamic responses to metformin. It is of interest that Oct1(−/−) mice do not develop metformin-induced lactic acidosis, which is a severe and rare adverse drug reaction of metformin treatment in humans (Wang et al. 2003).
5.2 Oct2 Single-Knockout and Oct1/Oct2 Double-Knockout Mice
In contrast to the absence of Oct1, the targeted disruption of the murine Oct2 gene had only little effect on the pharmacokinetics of intravenously injected TEA (Jonker et al. 2003). The hepatic and renal concentrations of TEA and the excretion of TEA in the urine and feces were similar in Oct2(−/−) and wild-type mice. Because Oct1 is expressed in mouse kidney in addition to Oct2 (Alnouti et al. 2006) and Oct1 and Oct2 have overlapping substrate specificities (Gründemann et al. 1999), renal Oct1 expression is apparently sufficient for secretion of most organic cations even in the absence of Oct2. In order to develop a mouse model for studying the renal secretion of organic cations, Oct1/Oct2 double-knockout mice have been generated (Jonker et al. 2003). Renal tubular secretion of TEA was completely abolished and TEA was only eliminated by glomerular filtration in these double-knockout mice, which resulted in significantly elevated TEA plasma levels compared to wild-type mice. Similarly, urinary excretion of cisplatin was significantly impaired in Oct1/Oct2(−/−) mice so that the animals were protected from severe cisplatin-induced renal tubular damage and from cisplatin-induced loss of hearing (Filipski et al. 2009; Ciarimboli et al. 2010).
5.3 Oct3 Knockout Mice
After cloning human OCT3 it was hypothesized that the functional defined corticosterone-sensitive extraneuronal transport activity for monoamine neurotransmitters is mainly mediated by OCT3 (Gründemann et al. 1998; Koepsell et al. 2003). Interestingly, steady-state norepinephrine and dopamine levels did not differ between several tissues from wild-type and Oct3(−/−) mice whereas differences in MPP accumulation were observed (Zwart et al. 2001). Intravenous injection of MPP into Oct3(−/−) mice resulted in significantly reduced MPP levels in heart, but not in small intestine, liver, kidney, brain, and placenta in comparison to tissues from wild-type mice. Moreover, fetuses from pregnant Oct3(−/−) mice had three times lower MPP levels. Because MPP is a substrate of murine Oct1, Oct2, and Oct3, these data suggest a prominent role of Oct3 in the heart and fetoplacental interface, whereas in other tissues the lack of Oct3 is apparently well compensated by the function of other Octs. Although Oct3(−/−) mice did not show overt phenotypical abnormalities, Oct3 is probably critically involved in central nervous function. Vialou et al. (2004) showed that Oct3 is implicated in the appropriate neural and behavioral responses to environmentally induced changes in osmolarity. Whether Oct3 also plays a role in the regulation of fear and anxiety is being discussed (Vialou et al. 2008; Wultsch et al. 2009). Of note, there is compensatory upregulation of Oct3 in the brain of mice that lack the neuronal serotonin transporter Slc6a4/Sert (Schmitt et al. 2003; Baganz et al. 2008).
5.4 Mate1 Knockout Mice
Pharmacokinetic characterization of Mate1(−/−) mice (Tsuda et al. 2009a) was carried out with metformin, a typical drug substrate of human MATE1 (Table 2). After intravenous injection, renal and hepatic metformin concentrations were markedly increased in the Mate1(−/−) mice compared to wild-type mice. In addition, plasma metformin levels were increased in Mate1(−/−) mice, whereas urinary metformin excretion was significantly decreased. These data indicate a crucial role of Mate1 in the renal clearance of metformin and probably other drugs as well.
6 Pharmacogenomics of OCT and MATE Transporters
It is well accepted that drug response to the same medication differs among individuals (Kerb 2006). Besides factors such as age, organ function, concomitant therapy, drug–drug interactions, and the nature of the disease, genetic factors have been recognized as important determinants of interindividual variability of drug response. Because OCTs and MATEs function as drug uptake and efflux transporters, respectively (Sect. 4), genetic variants in these transporters may account for interindividual variability of pharmacokinetics of many drugs (Ho and Kim 2005; Giacomini and Sugiyama 2006; Kerb 2006). At present, major research efforts are being taken to identify OCT and MATE variants, to analyze their potential functional consequences, and to determine their contribution to a patient’s response to pharmacotherapy.
6.1 Identification of Genetic Variants, Their Predicted Consequences, and Their Effects In Vitro
More than 1,100 and 450 single-nucleotide polymorphisms (SNPs) are currently listed for the OCT and MATE genes, respectively, in the NCBI-SNP database (National Center for Biotechnology Information, http://www.ncbi.nlm.nih.gov/SNP; build 130, January 2010). The Pharmacogenetics and Genomics Knowledge Base (PharmGKB, http://www.pharmgkb.org) is another public database comprising data and information related to all areas of pharmacogenetics including a large collection of DNA samples from ethnically diverse populations (Giacomini et al. 2007). Moreover, the International HapMap Consortium (http://www.hapmap.org) has generated a haplotype map of the human genome by identifying more than 3.1 million SNPs genotyped in 270 individuals from four geographically diverse populations (International HapMap Consortium et al. 2007). It is expected that the current next generation sequencing projects aiming at the complete sequencing of 1,000 human genomes (Kaiser 2008; Siva 2008) will identify more variants, especially those with low frequencies between 0.1% and 1% (Ionita-Laza et al. 2009).
Whereas most sequence variants are present in the introns, others are located in the 5′- and 3′-flanking regions and may lead to an altered expression level of the respective OCT or MATE transporter (Ogasawara et al. 2008; Nies et al. 2009; Hesselson et al. 2009; Ha Choi et al. 2009). Sequence variants within the exons (coding SNPs, cSNPs) may result in amino acid substitutions. These nonsynonymous or missense variants are of considerable interest because they may affect the transport function of the OCT and MATE transporters. A comprehensive list of the currently known cSNPs in the genes encoding human OCTs and MATEs are given in Table 4.
PolyPhen (polymorphism phenotyping, http://genetics.bwh.harvard.edu/pph2; Ramensky et al. 2002) and SIFT (Sorting Intolerant from Tolerant, http://sift.jcvi.org/; Kumar et al. 2009) are two commonly used algorithms, with which the potential functional effects of single amino acid substitutions can be predicted in silico. Based on multiple sequence alignments and in part on information from known three-dimensional protein structures, the algorithms predict the probability that an amino acid substitution has an impact on protein structure and function. However, these in silico predictions cannot substitute for the experimental analysis of each amino acid variant to proof functional changes of the respective OCT or MATE transporter. For comparison, Table 4 lists the predicted functional consequences as well as in vitro transport data for many of the known nonsynonymous OCT and MATE variants. SIFT and PolyPhen predictions are similar for most variants though they differ for some (e.g., OCT1-Ser14Phe, OCT1-Leu23Val, OCT1-Pro341Leu, OCT2-Lys432Gln, MATE1-Leu125Phe). Moreover, amino acid substitutions that are predicted to be tolerated have no transport activity in vitro (e.g., OCT1-Gly220Val, MATE1-Val480Met). This shows limitations of the in silico predictions, which did not include recent structural analysis data (Popp et al. 2005; Volk et al. 2009). The differences may partly be due to the fact that several variants are not properly incorporated into the plasma membrane but are rather retained intracellularly (Shu et al. 2007; Kajiwara et al. 2009; Chen et al. 2009b). The observations that variants alter transport function in a substrate-dependent manner (e.g., OCT1-Ser189Leu, OCT1-Met420del) illustrate the difficulty to predict complex effects of mutagenesis on functions of polyspecific transporters.
6.2 Interethnic Variability
Geographic, ethnic, and racial differences in the frequency of genetic variants are well known and several examples in the field of ADME genes have been reported as a mechanistic basis for differences in drug response and/or drug toxicity (Schaeffeler et al. 2001; Klein et al. 2005).
Significant ethnic differences exist also in the frequency of allele and genotype distributions of SLC22A1, SLC22A2, and SLC47A1 variants as listed in Tables 5–8. For instance, whereas in European-Americans and Caucasians the allele frequency of the SLC22A1-Arg61Cys polymorphism is approximately 8%, in African-Americans as well as Asian-Americans, no variant subject including 260 individuals tested were identified. In contrast, for the SLC22A1-Pro341Leu variant a significant higher allele frequency was found in African-Americans and Asian-Americans (8% and 17%) than in Caucasians (up to 2%). Finally, the Met408Val polymorphism was detected with high-frequency distributions in all ethnic groups (Caucasians, Africans, Asians). Currently it is unclear whether these differences in allele frequencies between various ethnic groups are of any clinical importance and potentially may render individuals more susceptible to certain xenobiotics and/or environmental factors. For example, aflatoxin B1 is a substrate of OCT1 and it is well recognized that the incidence of hepatocellular carcinoma is significantly more frequent in Asians compared to Caucasians. One may assume that such a difference in disease frequency may be explained by functional relevant genetic variants of the uptake transporter OCT1 that are more common in Asian populations.
6.3 Phenotype–Genotype Correlations
Currently data on tissue expression of OCTs and MATEs correlated to genetic variants are limited. The only polymorphism identified so far that affects OCT1 expression in human liver on mRNA and protein levels is Arg61Cys (Nies et al. 2009; Table 9) after correction for nongenetic factors (such as cholestasis) and additional SLC22A1 variants. Of note, a total of 36 variants in the SLC22A1 gene were tested including some SNPs, which showed reduced function in vitro (Table 4). It would be of major interest to analyze whether expression of OCT2, which is the predominant OCT uptake transporter in human kidney and involved in renal excretion of several drugs (e.g., metformin), is also influenced by genetic factors.
Several studies addressed the association of OCT genotypes with pharmacokinetic parameters of OCT substrates in humans (Tables 9–12). These investigations were based on initial observations that some variants alter OCT function in in vitro cell experiments (Table 4). A key publication in this field showed that metformin AUC and C max are significantly higher in OCT1-variant healthy subjects as compared to individuals with OCT1 reference gene sequence (Shu et al. 2008). In addition and in line with Oct1 knockout mice experiments, OCT1 variant human subjects revealed poor response to metformin measured by the oral glucose tolerance test (Shu et al. 2007). These data suggested for the first time that OCT1 may be a promising candidate gene for better prediction of the response to the antidiabetic agent metformin. Although some studies including type 2 diabetes patients were subsequently performed, unfortunately the results are inconsistent (Tables 9–12). A second clinically highly relevant agent, which was related to OCT1 expression and activity (White et al. 2007; Wang et al. 2008a), is the tyrosine kinase inhibitor imatinib, a mainstay in treatment of patients with chronic myeloid leukemia (CML). Although one study suggests a significant contribution of the OCT1-Phe160Leu variant related to loss of response to imatinib or treatment failure (Kim et al. 2009), further confirmatory studies are still missing, which are mandatory to support such an association.
Regarding OCT2 variants, the Ala270Ser polymorphism was investigated in several pharmacokinetic metformin studies with discrepant results (Table 10). The study with the most representative number of subjects included (n = 103) did not show any association (Tzvetkov et al. 2009). Interestingly, the OCT2-Ala270Ser variant was also related to a significantly reduced cisplatin-induced nephrotoxicity in patients with solid tumors, which fits to the fact that cisplatin is indeed an OCT2 substrate and OCT2 is highly expressed in human kidney (Filipski et al. 2009).
Although the physiological role of OCTs and MATEs is not fully resolved, it is conceivable that membrane transporters determine intracellular concentration of potentially efficient and/or toxic agents and metabolites. In this context it is plausible to hypothesize that genotype-dependent OCT/MATE expression may also contribute to a certain disease susceptibility. Of interest, susceptibility for diseases was repeatedly related to OCT3 (Table 11), whereas convincing data for both, OCT1 and OCT2, are lacking. The SLC22A3 gene was identified as a potential risk factor for prostate cancer as well as coronary artery disease by genomewide association studies (GWA), including thousands of index cases and confirmed by independent control groups (Eeles et al. 2008; Tregouet et al. 2009).
Taken together, compared with other transport proteins the research on the impact of OCT and MATE variants is only at the beginning. Comprehensive genotype–phenotype correlation studies including different human tissues as well as clinical response data are required in the future.
References
Abel S, Nichols DJ, Brearley CJ, Eve MD (2000) Effect of cimetidine and ranitidine on pharmacokinetics and pharmacodynamics of a single dose of dofetilide. Br J Clin Pharmacol 49:64–71
Abramson J, Smirnova I, Kasho V, Verner G, Kaback HR, Iwata S (2003) Structure and mechanism of the lactose permease of Escherichia coli. Science 301:610–615
Ahlin G, Karlsson J, Pedersen JM, Gustavsson L, Larsson R, Matsson P et al (2008) Structural requirements for drug inhibition of the liver specific human organic cation transport protein. J Med Chem 51:5932–5942
Alnouti Y, Petrick JS, Klaassen CD (2006) Tissue distribution and ontogeny of organic cation transporters in mice. Drug Metab Dispos 34:477–482
Amphoux A, Vialou V, Drescher E, Bruss M, La Mannoury CC, Rochat C et al (2006) Differential pharmacological in vitro properties of organic cation transporters and regional distribution in rat brain. Neuropharmacology 50:941–952
Aoyama N, Takahashi N, Kitaichi K, Ishihara R, Saito S, Maeno N et al (2006) Association between gene polymorphisms of SLC22A3 and methamphetamine use disorder. Alcohol Clin Exp Res 30:1644–1649
Asaka J, Terada T, Tsuda M, Katsura T, Inui K (2007) Identification of essential histidine and cysteine residues of the H+/organic cation antiporter multidrug and toxin extrusion (MATE). Mol Pharmacol 71:1487–1493
Ayrton A, Morgan P (2008) Role of transport proteins in drug discovery and development: a pharmaceutical perspective. Xenobiotica 38:676–708
Bachmakov I, Glaeser H, Fromm MF, König J (2008) Interaction of oral antidiabetic drugs with hepatic uptake transporters: focus on OATPs and OCT1. Diabetes 57:1463–1469
Bachmakov I, Glaeser H, Endress B, Morl F, König J, Fromm MF (2009) Interaction of beta-blockers with the renal uptake transporter OCT2. Diabetes Obes Metab 11:1080–1083
Baganz NL, Horton RE, Calderon AS, Owens WA, Munn JL, Watts LT et al (2008) Organic cation transporter 3: keeping the brake on extracellular serotonin in serotonin-transporter-deficient mice. Proc Natl Acad Sci U S A 105:18976–18981
Ballestero MR, Monte MJ, Briz O, Jimenez F, Gonzalez-San MF, Marin JJ (2006) Expression of transporters potentially involved in the targeting of cytostatic bile acid derivatives to colon cancer and polyps. Biochem Pharmacol 72:729–738
Barendt WM, Wright SH (2002) The human organic cation transporter (hOCT2) recognizes the degree of substrate ionization. J Biol Chem 277:22491–22496
Bayer M, Kuci Z, Schömig E, Gründemann D, Dittmann H, Handgretinger R et al (2009) Uptake of mIBG and catecholamines in noradrenaline- and organic cation transporter-expressing cells: potential use of corticosterone for a preferred uptake in neuroblastoma- and pheochromocytoma cells. Nucl Med Biol 36:287–294
Becker ML, Visser LE, van Schaik RH, Hofman A, Uitterlinden AG, Stricker BH (2009a) Genetic variation in the multidrug and toxin extrusion 1 transporter protein influences the glucose-lowering effect of metformin in patients with diabetes: a preliminary study. Diabetes 58:745–749
Becker ML, Visser LE, van Schaik RH, Hofman A, Uitterlinden AG, Stricker BH (2009b) Genetic variation in the organic cation transporter 1 is associated with metformin response in patients with diabetes mellitus. Pharmacogenomics J 9:242–247
Becker ML, Visser LE, van Schaik RH, Hofman A, Uitterlinden AG, Stricker BH (2010) Interaction between polymorphisms in the OCT1 and MATE1 transporter and metformin response. Pharmacogenet Genomics 20:38–44
Bednarczyk D, Ekins S, Wikel JH, Wright SH (2003) Influence of molecular structure on substrate binding to the human organic cation transporter, hOCT1. Mol Pharmacol 63:489–498
Biermann J, Lang D, Gorboulev V, Koepsell H, Sindic A, Schroter R et al (2006) Characterization of regulatory mechanisms and states of human organic cation transporter 2. Am J Physiol Cell Physiol 290:C1521–C1531
Bourdet DL, Pritchard JB, Thakker DR (2005) Differential substrate and inhibitory activities of ranitidine and famotidine toward human organic cation transporter 1 (hOCT1; SLC22A1), hOCT2 (SLC22A2), and hOCT3 (SLC22A3). J Pharmacol Exp Ther 315:1288–1297
Boyer JL, Graf J, Meier PJ (1992) Hepatic transport systems regulating pHi, cell volume, and bile secretion. Annu Rev Physiol 54:415–438
Budiman T, Bamberg E, Koepsell H, Nagel G (2000) Mechanism of electrogenic cation transport by the cloned organic cation transporter 2 from rat. J Biol Chem 275:29413–29420
Busch AE, Quester S, Ulzheimer JC, Waldegger S, Gorboulev V, Arndt P et al (1996) Electrogenic properties and substrate specificity of the polyspecific rat cation transporter rOCT1. J Biol Chem 271:32599–32604
Busch AE, Karbach U, Miska D, Gorboulev V, Akhoundova A, Volk C et al (1998) Human neurons express the polyspecific cation transporter hOCT2, which translocates monoamine neurotransmitters, amantadine, and memantine. Mol Pharmacol 54:342–352
Cetinkaya I, Ciarimboli G, Yalcinkaya G, Mehrens T, Velic A, Hirsch JR et al (2003) Regulation of human organic cation transporter hOCT2 by PKA, PI3K, and calmodulin-dependent kinases. Am J Physiol Renal Physiol 284:F293–F302
Chen Y, Zhang S, Sorani M, Giacomini KM (2007) Transport of paraquat by human organic cation transporters and multidrug and toxic compound extrusion family. J Pharmacol Exp Ther 332:695–700
Chen Y, Li S, Brown C, Cheatham S, Castro RA, Leabman MK et al (2009a) Effect of genetic variation in the organic cation transporter 2 on the renal elimination of metformin. Pharmacogenet Genomics 19:497–504
Chen Y, Teranishi K, Li S, Yee SW, Hesselson S, Stryke D et al (2009b) Genetic variants in multidrug and toxic compound extrusion-1, hMATE1, alter transport function. Pharmacogenomics J 9:127–136
Cheng Y, Wright SH, Hooth MJ, Sipes IG (2009) Characterization of the disposition and toxicokinetics of N-butylpyridinium chloride in male F-344 rats and female B6C3F1 mice and its transport by organic cation transporter 2. Drug Metab Dispos 37:909–916
Ciarimboli G (2008) Organic cation transporters. Xenobiotica 38:936–971
Ciarimboli G, Struwe K, Arndt P, Gorboulev V, Koepsell H, Schlatter E et al (2004) Regulation of the human organic cation transporter hOCT1. J Cell Physiol 201:420–428
Ciarimboli G, Ludwig T, Lang D, Pavenstädt H, Koepsell H, Piechota HJ et al (2005) Cisplatin nephrotoxicity is critically mediated via the human organic cation transporter 2. Am J Pathol 167:1477–1484
Ciarimboli G, Deuster D, Knief A, Sperling M, Holtkamp M, Edemir B et al (2010) Organic cation transporter 2 mediates cisplatin-induced oto- and nephrotoxicity and is target for protective interventions. Am J Pathol 176(3):1169–1180
Dresser MJ, Xiao G, Leabman MK, Gray AT, Giacomini KM (2002) Interactions of n-tetraalkylammonium compounds and biguanides with a human renal organic cation transporter (hOCT2). Pharm Res 19:1244–1247
Dudley AJ, Bleasby K, Brown CD (2000) The organic cation transporter OCT2 mediates the uptake of beta-adrenoceptor antagonists across the apical membrane of renal LLC-PK(1) cell monolayers. Br J Pharmacol 131:71–79
Eeles RA, Kote-Jarai Z, Giles GG, Olama AA, Guy M, Jugurnauth SK et al (2008) Multiple newly identified loci associated with prostate cancer susceptibility. Nat Genet 40:316–321
Feng B, Obach RS, Burstein AH, Clark DJ, de Morais SM, Faessel HM (2008) Effect of human renal cationic transporter inhibition on the pharmacokinetics of varenicline, a new therapy for smoking cessation: an in vitro–in vivo study. Clin Pharmacol Ther 83:567–576
Filipski KK, Mathijssen RH, Mikkelsen TS, Schinkel AH, Sparreboom A (2009) Contribution of organic cation transporter 2 (OCT2) to cisplatin-induced nephrotoxicity. Clin Pharmacol Ther 86:396–402
Fujita T, Urban TJ, Leabman MK, Fujita K, Giacomini KM (2006) Transport of drugs in the kidney by the human organic cation transporter, OCT2 and its genetic variants. J Pharm Sci 95:25–36
Fukushima-Uesaka H, Maekawa K, Ozawa S, Komamura K, Ueno K, Shibakawa M et al (2004) Fourteen novel single nucleotide polymorphisms in the SLC22A2 gene encoding human organic cation transporter (OCT2). Drug Metab Pharmacokinet 19:239–244
Giacomini KM, Sugiyama Y (2006) Membrane transporters and drug response. In: Brunton LL, Lazo JS, Parker RL (eds) Goodman and Gilman’s. The pharmacological basis of therapeutics, 11th edn. McGraw Hill, New York, pp 41–70
Giacomini KM, Hsyu PH, Gisclon LG (1988) Renal transport of drugs: an overview of methodology with application to cimetidine. Pharm Res 5:465–471
Giacomini KM, Brett CM, Altman RB, Benowitz NL, Dolan ME, Flockhart DA et al (2007) The pharmacogenetics research network: from SNP discovery to clinical drug response. Clin Pharmacol Ther 81:328–345
Gorboulev V, Ulzheimer JC, Akhoundova A, Ulzheimer-Teuber I, Karbach U, Quester S et al (1997) Cloning and characterization of two human polyspecific organic cation transporters. DNA Cell Biol 16:871–881
Gorboulev V, Volk C, Arndt P, Akhoundova A, Koepsell H (1999) Selectivity of the polyspecific cation transporter rOCT1 is changed by mutation of aspartate 475 to glutamate. Mol Pharmacol 56:1254–1261
Gorboulev V, Shatskaya N, Volk C, Koepsell H (2005) Subtype-specific affinity for corticosterone of rat organic cation transporters rOCT1 and rOCT2 depends on three amino acids within the substrate binding region. Mol Pharmacol 67:1612–1619
Gorbunov D, Gorboulev V, Shatskaya N, Mueller T, Bamberg E, Friedrich T et al (2008) High-affinity cation binding to organic cation transporter 1 induces movement of helix 11 and blocks transport after mutations in a modelled interaction domain between two helices. Mol Pharmacol 73:50–61
Gründemann D, Schömig E (2000) Gene structures of the human non-neuronal monoamine transporters EMT and OCT2. Hum Genet 106:627–635
Gründemann D, Gorboulev V, Gambaryan S, Veyhl M, Koepsell H (1994) Drug excretion mediated by a new prototype of polyspecific transporter. Nature 372:549–552
Gründemann D, Schechinger B, Rappold GA, Schömig E (1998) Molecular identification of the corticosterone-sensitive extraneuronal catecholamine transporter. Nat Neurosci 1:349–351
Gründemann D, Liebich G, Kiefer N, Köster S, Schömig E (1999) Selective substrates for non-neuronal monoamine transporters. Mol Pharmacol 56:1–10
Gründemann D, Hahne C, Berkels R, Schomig E (2003) Agmatine is efficiently transported by non-neuronal monoamine transporters extraneuronal monoamine transporter (EMT) and organic cation transporter 2 (OCT2). J Pharmacol Exp Ther 304:810–817
Ha Choi J, Wah Yee S, Kim MJ, Nguyen L, Ho LJ, Kang JO et al (2009) Identification and characterization of novel polymorphisms in the basal promoter of the human transporter, MATE1. Pharmacogenet Genomics 19:770–780
Hardman JG, Limbird LE, Gilman AG (eds) (2001) Goodman & Gilman's. The pharmacological basis of therapeutics, 10th edn. New York, McGraw Hill
Harlfinger S, Fork C, Lazar A, Schömig E, Gründemann D (2005) Are organic cation transporters capable of transporting prostaglandins? Naunyn Schmiedebergs Arch Pharmacol 372:125–130
Hasannejad H, Takeda M, Narikawa S, Huang XL, Enomoto A, Taki K et al (2004) Human organic cation transporter 3 mediates the transport of antiarrhythmic drugs. Eur J Pharmacol 499:45–51
Hayer M, Bönisch H, Brüss M (1999) Molecular cloning, functional characterization and genomic organization of four alternatively spliced isoforms of the human organic cation transporter 1 (hOCT1/SLC22A1). Ann Hum Genet 63:473–482
Hayer-Zillgen M, Brüss M, Bönisch H (2002) Expression and pharmacological profile of the human organic cation transporters hOCT1, hOCT2 and hOCT3. Br J Pharmacol 136:829–836
Hesselson SE, Matsson P, Shima JE, Fukushima H, Yee SW, Kobayashi Y et al (2009) Genetic variation in the proximal promoter of ABC and SLC superfamilies: liver and kidney specific expression and promoter activity predict variation. PLoS One 4:e6942
Ho RH, Kim RB (2005) Transporters and drug therapy: implications for drug disposition and disease. Clin Pharmacol Ther 78:260–277
Hu S, Franke RM, Filipski KK, Hu C, Orwick SJ, de Bruijn EA et al (2008) Interaction of imatinib with human organic ion carriers. Clin Cancer Res 14:3141–3148
Inazu M, Takeda H, Matsumiya T (2003) Expression and functional characterization of the extraneuronal monoamine transporter in normal human astrocytes. J Neurochem 84:43–52
International HapMap Consortium, Frazer KA, Ballinger DG, Cox DR, Hinds DA, Stuve LL et al (2007) A second generation human haplotype map of over 3.1 million SNPs. Nature 449:851–861
Ionita-Laza I, Lange C, Laird M (2009) Estimating the number of unseen variants in the human genome. Proc Natl Acad Sci U S A 106:5008–5013
Ito S, Kusuhara H, Kuroiwa Y, Wu C, Moriyama Y, Inoue K et al (2010) Potent and specific inhibition of mMate1-mediated efflux of type I organic cations in the liver and kidney by pyrimethamine. J Pharmacol Exp Ther 333:341–350
Itoda M, Saito Y, Maekawa K, Hichiya H, Komamura K, Kamakura S et al (2004) Seven novel single nucleotide polymorphisms in the human SLC22A1 gene encoding organic cation transporter 1 (OCT1). Drug Metab Pharmacokinet 19:308–312
Iwai M, Minematsu T, Narikawa S, Usui T, Kamimura H (2009) Involvement of human organic cation transporter 1 in the hepatic uptake of 1-(2-methoxyethyl)-2-methyl-4, 9-dioxo-3-(pyrazin-2-ylmethyl)-4, 9-dihydro-1H-napht ho[2, 3-d]imidazolium bromide (YM155 monobromide), a novel, small molecule survivin suppressant. Drug Metab Dispos 37:1856–1863
Jonker JW, Wagenaar E, Mol CA, Buitelaar M, Koepsell H, Smit JW et al (2001) Reduced hepatic uptake and intestinal excretion of organic cations in mice with a targeted disruption of the organic cation transporter 1 (Oct1 [Slc22a1]) gene. Mol Cell Biol 21:5471–5477
Jonker JW, Wagenaar E, Van ES, Schinkel AH (2003) Deficiency in the organic cation transporters 1 and 2 (Oct1/Oct2 [Slc22a1/Slc22a2]) in mice abolishes renal secretion of organic cations. Mol Cell Biol 23:7902–7908
Jung N, Lehmann C, Rubbert A, Knispel M, Hartmann P, van Lunzen J et al (2008) Relevance of the organic cation transporters 1 and 2 for antiretroviral therapy in HIV infection. Drug Metab Dispos 36:1616–1623
Kaiser J (2008) DNA sequencing. A plan to capture human diversity in 1000 genomes. Science 319:395
Kajiwara M, Terada T, Ogasawara K, Iwano J, Katsura T, Fukatsu A et al (2009) Identification of multidrug and toxin extrusion (MATE1 and MATE2-K) variants with complete loss of transport activity. J Hum Genet 54:40–46
Kang HJ, Song IS, Shin HJ, Kim WY, Lee CH, Shim JC et al (2007) Identification and functional characterization of genetic variants of human organic cation transporters in a Korean population. Drug Metab Dispos 35:667–675
Kekuda R, Prasad PD, Wu X, Wang H, Fei YJ, Leibach FH et al (1998) Cloning and functional characterization of a potential-sensitive, polyspecific organic cation transporter (OCT3) most abundantly expressed in placenta. J Biol Chem 273:15971–15979
Kerb R (2006) Implications of genetic polymorphisms in drug transporters for pharmacotherapy. Cancer Lett 234:4–33
Kerb R, Brinkmann U, Chatskaia N, Gorbunov D, Gorboulev V, Mornhinweg E et al (2002) Identification of genetic variations of the human organic cation transporter hOCT1 and their functional consequences. Pharmacogenetics 12:591–595
Khamdang S, Takeda M, Noshiro R, Narikawa S, Enomoto A, Anzai N et al (2002) Interactions of human organic anion transporters and human organic cation transporters with nonsteroidal anti-inflammatory drugs. J Pharmacol Exp Ther 303:534–539
Kim DH, Sriharsha L, Xu W, Kamel-Reid S, Liu X, Siminovitch K et al (2009) Clinical relevance of a pharmacogenetic approach using multiple candidate genes to predict response and resistance to imatinib therapy in chronic myeloid leukemia. Clin Cancer Res 15:4750–4758
Kimura H, Takeda M, Narikawa S, Enomoto A, Ichida K, Endou H (2002) Human organic anion transporters and human organic cation transporters mediate renal transport of prostaglandins. J Pharmacol Exp Ther 301:293–298
Kimura N, Masuda S, Tanihara Y, Ueo H, Okuda M, Katsura T et al (2005a) Metformin is a superior substrate for renal organic cation transporter OCT2 rather than hepatic OCT1. Drug Metab Pharmacokinet 20:379–386
Kimura N, Okuda M, Inui K (2005b) Metformin transport by renal basolateral organic cation transporter hOCT2. Pharm Res 22:255–259
Kimura N, Masuda S, Katsura T, Inui K (2009) Transport of guanidine compounds by human organic cation transporters, hOCT1 and hOCT2. Biochem Pharmacol 77:1429–1436
Kindla J, Fromm MF, König J (2009) In vitro evidence for the role of OATP and OCT uptake transporters in drug–drug interactions. Expert Opin Drug Metab Toxicol 5:489–500
Klein K, Lang T, Saussele T, Barbosa-Sicard E, Schunck WH, Eichelbaum M et al (2005) Genetic variability of CYP2B6 in populations of African and Asian origin: allele frequencies, novel functional variants, and possible implications for anti-HIV therapy with efavirenz. Pharmacogenet Genomics 15:861–873
Kobara A, Hiasa M, Matsumoto T, Otsuka M, Omote H, Moriyama Y (2008) A novel variant of mouse MATE-1 H+/organic cation antiporter with a long hydrophobic tail. Arch Biochem Biophys 469:195–199
Koehler MR, Wissinger B, Gorboulev V, Koepsell H, Schmid M (1997) The two human organic cation transporter genes SLC22A1 and SLC22A2 are located on chromosome 6q26. Cytogenet Cell Genet 79:198–200
Koepsell H (1998) Organic cation transporters in intestine, kidney, liver, and brain. Annu Rev Physiol 60:243–266
Koepsell H, Endou H (2004) The SLC22 drug transporter family. Pflugers Arch 447:666–676
Koepsell H, Schmitt BM, Gorboulev V (2003) Organic cation transporters. Rev Physiol Biochem Pharmacol 150:36–90
Koepsell H, Lips K, Volk C (2007) Polyspecific organic cation transporters: structure, function, physiological roles, and biopharmaceutical implications. Pharm Res 24:1227–1251
Kumar P, Henikoff S, Ng PC (2009) Predicting the effects of coding non-synonymous variants on protein function using the SIFT algorithm. Nat Protoc 4:1073–1081
Lai MY, Jiang FM, Chung CH, Chen HC, Chao PD (1988) Dose dependent effect of cimetidine on procainamide disposition in man. Int J Clin Pharmacol Ther Toxicol 26:118–121
Larkin MA, Blackshields G, Brown NP, Chenna R, McGettigan PA, McWilliam H et al (2007) Clustal W and Clustal X version 2.0. Bioinformatics 23:2947–2948
Lazar A, Gründemann D, Berkels R, Taubert D, Zimmermann T, Schömig E (2003) Genetic variability of the extraneuronal monoamine transporter EMT (SLC22A3). J Hum Genet 48:226–230
Lazar A, Zimmermann T, Koch W, Gründemann D, Schömig A, Kastrati A et al (2006) Lower prevalence of the OCT2 Ser270 allele in patients with essential hypertension. Clin Exp Hypertens 28:645–653
Lazar A, Walitza S, Jetter A, Gerlach M, Warnke A, Herpertz-Dahlmann B et al (2008) Novel mutations of the extraneuronal monoamine transporter gene in children and adolescents with obsessive-compulsive disorder. Int J Neuropsychopharmacol 11:35–48
Leabman MK, Huang CC, Kawamoto M, Johns SJ, Stryke D, Ferrin TE et al (2002) Polymorphisms in a human kidney xenobiotic transporter, OCT2, exhibit altered function. Pharmacogenetics 12:395–405
Lee WK, Reichold M, Edemir B, Ciarimboli G, Warth R, Koepsell H et al (2009) Organic cation transporters OCT1, 2, and 3 mediate high-affinity transport of the mutagenic vital dye ethidium in the kidney proximal tubule. Am J Physiol Renal Physiol 296:F1504–F1513
Li Q, Sai Y, Kato Y, Muraoka H, Tamai I, Tsuji A (2004) Transporter-mediated renal handling of nafamostat mesilate. J Pharm Sci 93:262–272
Lips KS, Volk C, Schmitt BM, Pfeil U, Arndt P, Miska D et al (2005) Polyspecific cation transporters mediate luminal release of acetylcholine from bronchial epithelium. Am J Respir Cell Mol Biol 33:79–88
Masuda S, Terada T, Yonezawa A, Tanihara Y, Kishimoto K, Katsura T et al (2006) Identification and functional characterization of a new human kidney-specific H+/organic cation antiporter, kidney-specific multidrug and toxin extrusion 2. J Am Soc Nephrol 17:2127–2135
Matsumoto T, Kanamoto T, Otsuka M, Omote H, Moriyama Y (2008) Role of glutamate residues in substrate recognition by human MATE1 polyspecific H+/organic cation exporter. Am J Physiol Cell Physiol 294:C1074–C1078
Matsushima S, Maeda K, Inoue K, Ohta KY, Yuasa H, Kondo T et al (2009) The inhibition of human multidrug and toxin extrusion 1 is involved in the drug–drug interaction caused by cimetidine. Drug Metab Dispos 37:555–559
Meyer-Wentrup F, Karbach U, Gorboulev V, Arndt P, Koepsell H (1998) Membrane localization of the electrogenic cation transporter rOCT1 in rat liver. Biochem Biophys Res Commun 248:673–678
Minematsu T, Iwai M, Umehara KI, Usui T, Kamimura H (2010) Characterization of human organic cation transporter 1 (OCT1/SLC22A1)-, and OCT2 (SLC22A2)-mediated transport of YM155 monobromide, a novel survivin suppressant. Drug Metab Dispos 38:1–4
Ming X, Ju W, Wu H, Tidwell RR, Hall JE, Thakker DR (2009) Transport of dicationic drugs pentamidine and furamidine by human organic cation transporters. Drug Metab Dispos 37:424–430
Minuesa G, Volk C, Molina-Arcas M, Gorboulev V, Erkizia I, Arndt P et al (2009) Transport of lamivudine (3TC) and high-affinity interaction of nucleoside reverse transcriptase inhibitors with human organic cation transporters 1, 2, and 3. J Pharmacol Exp Ther 329:252–261
Moore KH, Yuen GJ, Raasch RH, Eron JJ, Martin D, Mydlow PK et al (1996) Pharmacokinetics of lamivudine administered alone and with trimethoprim-sulfamethoxazole. Clin Pharmacol Ther 59:550–558
Motohashi H, Sakurai Y, Saito H, Masuda S, Urakami Y, Goto M et al (2002) Gene expression levels and immunolocalization of organic ion transporters in the human kidney. J Am Soc Nephrol 13:866–874
Müller J, Lips KS, Metzner L, Neubert RH, Koepsell H, Brandsch M (2005) Drug specificity and intestinal membrane localization of human organic cation transporters (OCT). Biochem Pharmacol 70:1851–1860
Nagel G, Volk C, Friedrich T, Ulzheimer JC, Bamberg E, Koepsell H (1997) A reevaluation of substrate specificity of the rat cation transporter rOCT1. J Biol Chem 272:31953–31956
Neuhoff S, Ungell AL, Zamora I, Artursson P (2003) pH-dependent bidirectional transport of weakly basic drugs across Caco-2 monolayers: implications for drug–drug interactions. Pharm Res 20:1141–1148
Nies AT, Herrmann E, Brom M, Keppler D (2008) Vectorial transport of the plant alkaloid berberine by double-transfected cells expressing the human organic cation transporter 1 (OCT1, SLC22A1) and the efflux pump MDR1 P-glycoprotein (ABCB1). Naunyn Schmiedebergs Arch Pharmacol 376:449–461
Nies AT, Koepsell H, Winter S, Burk O, Klein K, Kerb R et al (2009) Expression of organic cation transporters OCT1 (SLC22A1) and OCT3 (SLC22A3) is affected by genetic factors and cholestasis in human liver. Hepatology 50:1227–1240
Nishimura M, Naito S (2005) Tissue-specific mRNA expression profiles of human ATP-binding cassette and solute carrier transporter superfamilies. Drug Metab Pharmacokinet 20:452–477
Ogasawara K, Terada T, Motohashi H, Asaka J, Aoki M, Katsura T et al (2008) Analysis of regulatory polymorphisms in organic ion transporter genes (SLC22A) in the kidney. J Hum Genet 53:607–614
Ohta KY, Inoue K, Hayashi Y, Yuasa H (2006) Molecular identification and functional characterization of rat multidrug and toxin extrusion type transporter 1 as an organic cation/H+ antiporter in the kidney. Drug Metab Dispos 34:1868–1874
Okabe M, Szakacs G, Reimers MA, Suzuki T, Hall MD, Abe T et al (2008) Profiling SLCO and SLC22 genes in the NCI-60 cancer cell lines to identify drug uptake transporters. Mol Cancer Ther 7:3081–3091
Okuda M, Kimura N, Inui K (2006) Interactions of fluoroquinolone antibacterials, DX-619 and levofloxacin, with creatinine transport by renal organic cation transporter hOCT2. Drug Metab Pharmacokinet 21:432–436
Otsuka M, Matsumoto T, Morimoto R, Arioka S, Omote H, Moriyama Y (2005) A human transporter protein that mediates the final excretion step for toxic organic cations. Proc Natl Acad Sci U S A 102:17923–17928
Popp C, Gorboulev V, Muller TD, Gorbunov D, Shatskaya N, Koepsell H (2005) Amino acids critical for substrate affinity of rat organic cation transporter 1 line the substrate binding region in a model derived from the tertiary structure of lactose permease. Mol Pharmacol 67:1600–1611
Ramensky V, Bork P, Sunyaev S (2002) Human non-synonymous SNPs: server and survey. Nucleic Acids Res 30:3894–3900
Sakata T, Anzai N, Shin HJ, Noshiro R, Hirata T, Yokoyama H et al (2004) Novel single nucleotide polymorphisms of organic cation transporter 1 (SLC22A1) affecting transport functions. Biochem Biophys Res Commun 313:789–793
Sata R, Ohtani H, Tsujimoto M, Murakami H, Koyabu N, Nakamura T et al (2005) Functional analysis of organic cation transporter 3 expressed in human placenta. J Pharmacol Exp Ther 315:888–895
Schaeffeler E, Eichelbaum M, Brinkmann U, Penger A, Asante-Poku S, Zanger UM et al (2001) Frequency of C3435T polymorphism of MDR1 gene in African people. Lancet 358:383–384
Schmitt BM, Koepsell H (2005) Alkali cation binding and permeation in the rat organic cation transporter rOCT2. J Biol Chem 280:24481–24490
Schmitt A, Mossner R, Gossmann A, Fischer IG, Gorboulev V, Murphy DL et al (2003) Organic cation transporter capable of transporting serotonin is up-regulated in serotonin transporter-deficient mice. J Neurosci Res 71:701–709
Schmitt BM, Gorbunov D, Schlachtbauer P, Egenberger B, Gorboulev V, Wischmeyer E et al (2009) Charge-to-substrate ratio during organic cation uptake by rat OCT2 is voltage dependent and altered by exchange of glutamate 448 with glutamine. Am J Physiol Renal Physiol 296:F709–F722
Shikata E, Yamamoto R, Takane H, Shigemasa C, Ikeda T, Otsubo K et al (2007) Human organic cation transporter (OCT1 and OCT2) gene polymorphisms and therapeutic effects of metformin. J Hum Genet 52:117–122
Shnitsar V, Eckardt R, Gupta S, Grottker J, Muller GA, Koepsell H et al (2009) Expression of human organic cation transporter 3 in kidney carcinoma cell lines increases chemosensitivity to melphalan, irinotecan, and vincristine. Cancer Res 69:1494–1501
Shu Y, Leabman MK, Feng B, Mangravite LM, Huang CC, Stryke D et al (2003) Evolutionary conservation predicts function of variants of the human organic cation transporter, OCT1. Proc Natl Acad Sci U S A 100:5902–5907
Shu Y, Sheardown SA, Brown C, Owen RP, Zhang S, Castro RA et al (2007) Effect of genetic variation in the organic cation transporter 1 (OCT1) on metformin action. J Clin Invest 117:1422–1431
Shu Y, Brown C, Castro R, Shi R, Lin E, Owen R et al (2008) Effect of genetic variation in the organic cation transporter 1, OCT1, on metformin pharmacokinetics. Clin Pharmacol Ther 83:273–280
Siva N (2008) 1000 Genomes project. Nat Biotechnol 26:256
Somogyi A, Stockley C, Keal J, Rolan P, Bochner F (1987) Reduction of metformin renal tubular secretion by cimetidine in man. Br J Clin Pharmacol 23:545–551
Song I, Shin H, Shim E, Jung I, Kim W, Shon J et al (2008) Genetic variants of the organic cation transporter 2 influence the disposition of metformin. Clin Pharmacol Ther 84:559–562
Sturm A, Gorboulev V, Gorbunov D, Keller T, Volk C, Schmitt BM et al (2007) Identification of cysteines in rat organic cation transporters rOCT1 (C322, C451) and rOCT2 (C451) critical for transport activity and substrate affinity. Am J Physiol Renal Physiol 293:F767–F779
Suhre WM, Ekins S, Chang C, Swaan PW, Wright SH (2005) Molecular determinants of substrate/inhibitor binding to the human and rabbit renal organic cation transporters hOCT2 and rbOCT2. Mol Pharmacol 67:1067–1077
Tachampa K, Takeda M, Khamdang S, Noshiro-Kofuji R, Tsuda M, Jariyawat S et al (2008) Interactions of organic anion transporters and organic cation transporters with mycotoxins. J Pharmacol Sci 106:435–443
Tahara H, Kusuhara H, Endou H, Koepsell H, Imaoka T, Fuse E et al (2005) A species difference in the transport activities of H2 receptor antagonists by rat and human renal organic anion and cation transporters. J Pharmacol Exp Ther 315:337–345
Takeda M, Khamdang S, Narikawa S, Kimura H, Kobayashi Y, Yamamoto T et al (2002) Human organic anion transporters and human organic cation transporters mediate renal antiviral transport. J Pharmacol Exp Ther 300:918–924
Tanihara Y, Masuda S, Sato T, Katsura T, Ogawa O, Inui K (2007) Substrate specificity of MATE1 and MATE2-K, human multidrug and toxin extrusions/H(+)-organic cation antiporters. Biochem Pharmacol 74:359–371
Tanihara Y, Masuda S, Katsura T, Inui KI (2009) Protective effect of concomitant administration of imatinib on cisplatin-induced nephrotoxicity focusing on renal organic cation transporter OCT2. Biochem Pharmacol 78:1263–1271
Taubert D, Grimberg G, Stenzel W, Schömig E (2007) Identification of the endogenous key substrates of the human organic cation transporter OCT2 and their implication in function of dopaminergic neurons. PLoS One 2:e385
Terada T, Inui KI (2008) Physiological and pharmacokinetic roles of H(+)/organic cation antiporters (MATE/SLC47A). Biochem Pharmacol 75:1689–1696
Terada T, Masuda S, Asaka J, Tsuda M, Katsura T, Inui K (2006) Molecular cloning, functional characterization and tissue distribution of rat H+/organic cation antiporter MATE1. Pharm Res 23:1696–1701
Thomas J, Wang L, Clark RE, Pirmohamed M (2004) Active transport of imatinib into and out of cells: implications for drug resistance. Blood 104:3739–3745
Tregouet DA, Konig IR, Erdmann J, Munteanu A, Braund PS, Hall AS et al (2009) Genome-wide haplotype association study identifies the SLC22A3-LPAL2-LPA gene cluster as a risk locus for coronary artery disease. Nat Genet 41:283–285
Tsuda M, Terada T, Mizuno T, Katsura T, Shimakura J, Inui KI (2009a) Targeted disruption of the multidrug and toxin extrusion 1 (Mate1) gene in mice reduces renal secretion of metformin. Mol Pharmacol 75:1280–1286
Tsuda M, Terada T, Ueba M, Sato T, Masuda S, Katsura T et al (2009b) Involvement of human multidrug and toxin extrusion 1 in the drug interaction between cimetidine and metformin in renal epithelial cells. J Pharmacol Exp Ther 329:185–191
Tzvetkov MV, Vormfelde SV, Balen D, Meineke I, Schmidt T, Sehrt D et al (2009) The effects of genetic polymorphisms in the organic cation transporters OCT1, OCT2, and OCT3 on the renal clearance of metformin. Clin Pharmacol Ther 86:299–306
Umehara KI, Iwatsubo T, Noguchi K, Usui T, Kamimura H (2008) Effect of cationic drugs on the transporting activity of human and rat OCT/Oct 1–3 in vitro and implications for drug–drug interactions. Xenobiotica 38:1203–1218
Urakami Y, Kimura N, Okuda M, Inui K (2004) Creatinine transport by basolateral organic cation transporter hOCT2 in the human kidney. Pharm Res 21:976–981
van Crugten J, Bochner F, Keal J, Somogyi A (1986) Selectivity of the cimetidine-induced alterations in the renal handling of organic substrates in humans. Studies with anionic, cationic and zwitterionic drugs. J Pharmacol Exp Ther 236:481–487
van Montfoort JE, Muller M, Groothuis GM, Meijer DK, Koepsell H, Meier PJ (2001) Comparison of “type I” and “type II” organic cation transport by organic cation transporters and organic anion-transporting polypeptides. J Pharmacol Exp Ther 298:110–115
Verhaagh S, Schweifer N, Barlow DP, Zwart R (1999) Cloning of the mouse and human solute carrier 22a3 (Slc22a3/SLC22A3) identifies a conserved cluster of three organic cation transporters on mouse chromosome 17 and human 6q26–q27. Genomics 55:209–218
Vialou V, Amphoux A, Zwart R, Giros B, Gautron S (2004) Organic cation transporter 3 (Slc22a3) is implicated in salt-intake regulation. J Neurosci 24:2846–2851
Vialou V, Balasse L, Callebert J, Launay JM, Giros B, Gautron S (2008) Altered aminergic neurotransmission in the brain of organic cation transporter 3-deficient mice. J Neurochem 106:1471–1482
Volk C, Gorboulev V, Kotzsch A, Muller TD, Koepsell H (2009) Five amino acids in the innermost cavity of the substrate binding cleft of organic cation transporter 1 interact with extracellular and intracellular corticosterone. Mol Pharmacol 76:275–289
Wang DS, Jonker JW, Kato Y, Kusuhara H, Schinkel AH, Sugiyama Y (2002) Involvement of organic cation transporter 1 in hepatic and intestinal distribution of metformin. J Pharmacol Exp Ther 302:510–515
Wang DS, Kusuhara H, Kato Y, Jonker JW, Schinkel AH, Sugiyama Y (2003) Involvement of organic cation transporter 1 in the lactic acidosis caused by metformin. Mol Pharmacol 63:844–848
Wang L, Giannoudis A, Lane S, Williamson P, Pirmohamed M, Clark RE (2008a) Expression of the uptake drug transporter hOCT1 is an important clinical determinant of the response to imatinib in chronic myeloid leukemia. Clin Pharmacol Ther 83:258–264
Wang ZJ, Yin OQ, Tomlinson B, Chow MS (2008b) OCT2 polymorphisms and in-vivo renal functional consequence: studies with metformin and cimetidine. Pharmacogenet Genomics 18:637–645
White DL, Saunders VA, Dang P, Engler J, Zannettino AC, Cambareri AC et al (2006) OCT-1-mediated influx is a key determinant of the intracellular uptake of imatinib but not nilotinib (AMN107): reduced OCT-1 activity is the cause of low in vitro sensitivity to imatinib. Blood 108:697–704
White DL, Saunders VA, Dang P, Engler J, Venables A, Zrim S et al (2007) Most CML patients who have a suboptimal response to imatinib have low OCT-1 activity: higher doses of imatinib may overcome the negative impact of low OCT-1 activity. Blood 110:4064–4072
Wu X, Huang W, Ganapathy ME, Wang H, Kekuda R, Conway S et al (2000) Structure, function, and regional distribution of the organic cation transporter OCT3 in the kidney. Am J Physiol Renal Physiol 279:F449–F458
Wultsch T, Grimberg G, Schmitt A, Painsipp E, Wetzstein H, Breitenkamp AF et al (2009) Decreased anxiety in mice lacking the organic cation transporter 3. J Neural Transm 116:689–697
Yokoo S, Masuda S, Yonezawa A, Terada T, Katsura T, Inui KI (2008) Significance of OCT3/SLC22A3, organic cation transporter 3, expression for the cytotoxic effect of oxaliplatin in colorectal cancer. Drug Metab Dispos 36:2299–2306
Yonezawa A, Masuda S, Yokoo S, Katsura T, Inui KI (2006) Cisplatin and oxaliplatin, but not carboplatin and nedaplatin, are substrates for human organic cation transporters (SLC22A1-3 and MATE family). J Pharmacol Exp Ther 319:879–886
Zach O, Krieger O, Foedermayr M, Zellhofer B, Lutz D (2008) OCT1 (SLC22A1) R61C polymorphism and response to imatinib treatment in chronic myeloid leukemia patients. Leuk Lymphoma 49:2222–2223
Zhang L, Dresser MJ, Gray AT, Yost SC, Terashita S, Giacomini KM (1997) Cloning and functional expression of a human liver organic cation transporter. Mol Pharmacol 51:913–921
Zhang L, Schaner ME, Giacomini KM (1998) Functional characterization of an organic cation transporter (hOCT1) in a transiently transfected human cell line (HeLa). J Pharmacol Exp Ther 286:354–361
Zhang L, Gorset W, Washington CB, Blaschke TF, Kroetz DL, Giacomini KM (2000) Interactions of HIV protease inhibitors with a human organic cation transporter in a mammalian expression system. Drug Metab Dispos 28:329–334
Zhang S, Lovejoy KS, Shima JE, Lagpacan LL, Shu Y, Lapuk A et al (2006) Organic cation transporters are determinants of oxaliplatin cytotoxicity. Cancer Res 66:8847–8857
Zhang X, Cherrington NJ, Wright SH (2007) Molecular identification and functional characterization of rabbit MATE1 and MATE2-K. Am J Physiol Renal Physiol 293:F360–F370
Zhou K, Donnelly LA, Kimber CH, Donnan PT, Doney AS, Leese G et al (2009) Reduced-function SLC22A1 polymorphisms encoding organic cation transporter 1 and glycemic response to metformin: a GoDARTS study. Diabetes 58:1434–1439
Zolk O, Solbach TF, König J, Fromm MF (2008) Structural determinants of inhibitor interaction with the human organic cation transporter OCT2 (SLC22A2). Naunyn Schmiedebergs Arch Pharmacol 379:337–348
Zolk O, Solbach TF, König J, Fromm MF (2009) Functional characterization of the human organic cation transporter 2 variant p. 270Ala>Ser. Drug Metab Dispos 37:1312–1318
Zwart R, Verhaagh S, Buitelaar M, Popp-Snijders C, Barlow DP (2001) Impaired activity of the extraneuronal monoamine transporter system known as uptake-2 in Orct3/Slc22a3-deficient mice. Mol Cell Biol 21:4188–4196
Acknowledgments
The authors’ work on the importance of transporters in drug therapy is supported by the Robert-Bosch Foundation Stuttgart, the IZEPHA Grants #6-0-0/672 and #8-0-0/674, the Federal Ministry for Education and Research (BMBF, Berlin, Germany) grant 03 IS 2061C, the German Research Foundation Grant SFB487/A4, and the Deutsche Krebshilfe (grant 107150). We thank Dr. Elke Schaeffeler for helpful discussions.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2011 Springer Berlin Heidelberg
About this chapter
Cite this chapter
Nies, A.T., Koepsell, H., Damme, K., Schwab, M. (2011). Organic Cation Transporters (OCTs, MATEs), In Vitro and In Vivo Evidence for the Importance in Drug Therapy. In: Fromm, M., Kim, R. (eds) Drug Transporters. Handbook of Experimental Pharmacology, vol 201. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-14541-4_3
Download citation
DOI: https://doi.org/10.1007/978-3-642-14541-4_3
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-14540-7
Online ISBN: 978-3-642-14541-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)