Abstract
Background
The aim of our study was to assess how a preoperative computed tomography (CT)-based navigation system affected the correctness and safety of transpedicular screw insertion, compared with standard techniques.
Method
Between January 2012 and February 2014, 203 patients underwent thoracic and lumbar fixation, with open and percutaneous techniques; 218 screws were implanted through an open navigated technique (1.0 Spine & Trauma 3d ver. 2.0 BrainLab, Feldkirchen Germany) in 43 patients; 220 screws were inserted with an open free-hand technique in 45 patients; 230 screws were implanted in 56 patients using percutaneous CT-based navigation; and 236 screws were inserted in 59 patients using a percutaneous fluoroscopy-guided technique. To our knowledge, this is the first work comparing these four different techniques. The position of each screw was evaluated on CT scan reconstruction and classified according to a four-point grading scale (grade 0: no breach, grade 1: breach < 2 mm, grade 2: breach between 2 and 4 mm; grade 3: breach >4 mm). Statistical analysis was assessed by two-way analysis of variance (ANOVA) t test, while the Fisher least significant difference (LSD) method was employed to determine statistical significance.
Results
Statistical analysis showed a significant difference in accuracy between the open CT-based navigation and the percutaneous CT-based navigation techniques (P= 0.0263) and between the open CT-based navigation and the percutaneous fluoroscopy-guided techniques (P=0.0258): a particular difference was observed in anterior misplacement between open CT-based navigation and the percutaneous fluoroscopy-guided technique (P= 0.0153).
Conclusions
Our results confirm the advantages of the navigation technique, which ensures greater accuracy, in open as well as percutaneous procedures.
Access provided by CONRICYT-eBooks. Download conference paper PDF
Similar content being viewed by others
Keywords
- Percutaneous pedicular screw fixation
- Free-hand pedicular screw fixation
- Fluoroscopy-guided pedicle screw fixation
- Spinal CT-based navigation system
- Pedicle screw accuracy
Introduction
Pedicle screw fixation techniques are progressively improving in terms of less invasivity and greater safety and accuracy. Advances in percutaneous techniques allow a less traumatic approach, resulting in improved short- as well as long-term results. Safety in transpedicular screw fixation especially concerns violation of the cortical bone of the pedicles and vertebral bodies that can potentially lead to the damage of neurovascular structures. Misplacement of the screws can also threaten the grip of the implant [11].
Many attempts have been made in order to improve insertion accuracy. Among these, computed tomography (CT)-based navigation seems to be the most reliable, due to visualization of the precise anatomy, as well as reduced radiation exposure.
The aim of this study was to compare the efficacy and reliability of an open free-hand technique, an open navigated technique (BrainLab® System), a percutaneous CT-based navigation technique, and a percutaneous fluoroscopy-guided technique.. To our knowledge this is the first work comparing these four different techniques applied in the same period by the same surgical team.
Materials and Methods
Between January 2012 and February 2014, 203 patients (115 females, 88 males) underwent thoracic and lumbar fusion with percutaneous (Viper 2 System, DePuy Synthes Spine, Raynham, MA) and open pedicle screw (Expedium 5.5 System, DePuy Synthes Spine, Raynham, MA) instrumentation carried out by the same neurosurgical team.
Indications for instrumentation were for degenerative pathologies (166 patients; spondylolisthesis with or without stenosis, post-laminectomy syndrome, twice-recurrent disc herniation), unstable fractures (25 patients), tumors (10 patients), aneurysmal cyst (1 patient), and inflammatory lesion (1 patient).
Two hundred and eighteen pedicle screws were implanted in 43 patients (21 females, 22 males) of average age 56.5 years (range 20–79 years) using open CT-based navigation (1.0 Spine & Trauma 3D ver. 2.0 BrainLab®) (ON group); 220 screws were implanted in 45 patients (21 females, 24 males) of average age 53.8 years (range 19–75 years) using an open free-hand technique (O group); 230 screws were implanted in 56 patients (35 female, 21 males) of average age 60.2 years (range 25–81 years) using percutaneous CT-based navigation (1.0 Spine & Trauma 3D ver. 2.0 BrainLab®) (PN group); and 236 screws were implanted in 59 patients (38 females, 21 males) of average age 59 years (range 16–78 years) using a percutaneous fluoroscopy-guided technique (P group).
Distribution of screws in all groups is shown in Table 1.
All patients were operated in the prone position on a carbon-top radiolucent table.
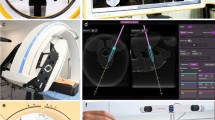
For patients in in the ON and PN groups a preoperative CT scan (CT scan 24-multislice GE Healthcare, Little Chalfont, UK) was performed in the prone position and transferred to the computer navigation platform which reconstructed data to provide real-time intraoperative three-dimensional images of the vertebra.
In the O and P groups, screws were implanted according to the Roy-Camille technique [28]. The procedure in the P group was assessed using the C-arm in a step-by-step fashion, while in the O group, we performed just a final check at the end of the procedure with the C-arm.
Postoperative CT scans with sagittal and coronal reconstruction were performed in each patient. The position of each screw was reviewed by a neurosurgeon and a radiologist uninvolved in the procedure and classified according to a four-point grading scale: grade 0 (screws fully contained in the pedicle); grade 1 (perforating screws, up to 2 mm misplacement); grade 2 (perforating screws, between 2 and 4 mm misplacement); and grade 3 (perforating screws, greater than 4 mm misplacement) [25] (Fig. 1).
Statistical relationships between various groups were assessed by two-way analysis of variance (ANOVA) t-test, while the Fisher least significant difference (LSD) method was employed for determining statistical significance. Significance was defined as P < O = 0.05.
Results
Thoracic pedicle screws were not included in the analysis, because the low number did not allow any statistical analysis.
Screw distribution, according to the Neo classification [24], is shown in Table 2.
Statistical analysis of collected data showed a significant difference in accuracy between the ON and PN groups (P: 0.0263) and between the ON and P groups (P: 0.0258): a particular difference was observed in anterior misplacement between the ON and P groups (P: 0.0153) (Table 3).
We also considered each single vertebra, but we found no significant differences (Table 4).
Complications are shown in Table 5.
Discussion
Surgical landmarks and fluoroscopy have been used routinely for pedicle screw insertion, but a number of studies reveal inaccuracies in placement using these conventional techniques (inaccuracies range from 14 to 55 %, with as many as 7 % of these misplaced screws resulting in neurological injuries) [1, 21–23, 25, 38].
Spinal navigation was introduced in 1995 in order to improve the accuracy of pedicle screw insertion and thereby minimize the risk of neurovascular injuries [25]. In a number of published studies, the use of image guidance has been reported to consistently reduce pedicle breaches to less than 5 % [14, 15, 25, 26, 31, 37].
Our accuracy rate for lumbar and sacral vertebrae with the open free-hand technique was 91.1 %, which is comparable to the literature data (range from 69 to 94 %) [10]; we found no case of grade 3 medial misplacement; only 2 cases (0.9 %) showed an anterior breach of more than 4 mm, and this was not accompanied by neurological or vascular injury.
The open CT-based navigation technique showed an accuracy of 92.5 %, which is comparable to the literature data (range from 72.03 to 95.68 %) [32, 35]. We found no case of grade 3 misplacement. In only one case we observed a transient neurological deficit.
Our accuracy rate for lumbar and sacral vertebrae with the percutaneous fluoroscopy-guided technique was 73.8 %. Accurate minimally invasive pedicle screw placement is complicated, however, by the obscuring of normal anatomical landmarks [40]. Errors in placement are therefore a primary concern, with one study reporting almost 10 % of patients needing revision surgery [27]. We reported 16 cases (7.5 %) of grade 3 misplacement, of which 8 cases (3.7 %) showed medial breach, 6 cases (2.8 %) anterior breach, 1 case (0.5 %) lateral breach, and 1 case (0.5 %) inferior breach. Only four medial screws were replaced for irritative pain in the period from the first postoperative day to 2 months after surgery. We found no permanent neurological deficit or construction failure related to screw misplacement.
The percutaneous CT-based navigation technique showed an accuracy of 85 %. Jako et al. [40] reported an accuracy rate of 64.9 % for screws placed with electromagnetic field guidance vs. 40 % for screws placed with fluoroscopy. We reported four cases (1.9 %) of grade 3 misplacement, of which two cases (0.9 %) showed medial breach and two cases (0.9 %) lateral breach. Only one medial screw was relocated for irritative pain, after 1 week. We found no permanent neurological deficit or construction failure related to screw misplacement.
The potential for neurological risk is due to the intrinsic anatomy inherent to screw placement and anatomical variability among patients. Gertzbein et al. [11] postulated a 4-mm safe zone for medial misplaced screws in the lower back region, this being without neurological complications. Even in patients with medial and lateral grade 3 misplacement no neurological deficits were observed: this may be explained in the light of the degenerative spine, which has a different threshold for nerve root irritation.
In our series, the accuracy of placement over all lumbar and sacral segments was slightly better in the open CT-based navigation group than in the conventional open free-hand group, but this difference was not statistically significant (P: 0.580).
However, we noted an advantage with statistical significance for the open CT-based navigation technique compared with the percutaneous CT-based navigation (P: 0.0263) and percutaneous fluoroscopy-guided techniques (P: 0.0258).
One important finding of our study is that screws positioned with the open CT-based navigation technique compared with the percutaneous fluoroscopy-guided technique (P: 0.0153) tended to perforate the cortex anteriorly, especially for L5 (2/4 L5screws in group ON, 12/20 L5 screws in group P), probably due to difficult evaluation of fluoroscopic bidimensional images in the lateral view and due to the shape of L5, which is similar to S1 with a reduction of the lateral diameter of the body.
Gelalis et al. [10] found that screws placed with CT navigation guidance seemed to perforate the lateral cortex more often, differently from screws placed with a free-hand technique, which tended to perforate the cortex medially. Our data did not confirm such a statistically significant difference, but we noted a more medial trajectory in the percutaneous groups than in the open groups.
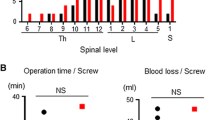
In comparison with the percutaneous technique, we found that the open technique showed five cases of wound infection, due to the significant exposure of the posterior bony elements of the spine and significant amounts of blood loss [16, 40].
These data confirm the superiority of the navigation technique, which ensures greater accuracy, above all for the percutaneous procedure, probably because of the poor quality of the fluoroscopy images (especially for obese patients); our data also reinforce the superiority of percutaneous vs. open techniques with regard to less damage to the surrounding muscles, less blood loss, less postoperative back pain, and shorter recovery time.
Although image-guided surgical techniques have resulted in lower perforation rates (ranging from 9.3 to 14.3 %), these technologies have their limitations [2–9].
Inaccuracies could also be associated with lack of correspondence between preoperative CT, acquired in the standard supine position, and the intraoperative prone position, especially in cases of severe instability and isthmic lysis. In order to reduce these inaccuracies, we started to perform preoperative CT scanning in the prone position, mimicking the position in the operation room. Although intraoperative CT scanning could be useful in screw placement, this device is not still available in every operation room, due to its high cost. Moreover, it is mandatory to consider the radiation exposure for operative staff, which is significantly higher with intraoperative CT scanning than with standard and neuronavigated techniques.
We also noted an inaccuracy in a patient with intraspinous devices from a previously implanted fixation system, due to anatomical distortion.
Intraoperative CT scanning has recently been introduced to bridge the gap between preoperative and intraoperative position-dependent changes [5, 12, 17–21, 23]. Moreover, this CT scanning offers the possibility of monitoring and visualizing pedicle screws immediately after their placement [26, 29, 30, 33–36, 39, 41]. Bydon et al. [5] maintain that the intraoperative CT scanner is much more sensitive for detecting unfavorably placed screws than conventional intraoperative fluoroscopy or radiography, and dramatically lowers the threshold for screw revision.
An advantage of a navigation system is the decreased radiation exposure for the patient, surgeon, and all the operating room staff, especially when compared with the percutaneous fluoroscopy-guided technique, where we usually perform at least five to six fluoroscopic scans for each pedicular screw. The average dose in a single scan is 0.10 mGy for patients weighing up to 75 kg and 0.21 mGy for those over 75 kg. The radiation exposure of the patient is obviously reduced with a navigation system, and also the radiation exposure of surgeons is greatly reduced, considering the addition of all such exposures during all the surgeries performed in their careers; and of course the reduced number of fluoroscopic scans is associated with a reduction in surgery time.
Another advantage of the Brainlab® system compared with fluoroscopy is that it allows simultaneous and multiplanar visualization of the spinal anatomy, which helps in virtually tracking surgical instruments in relation to the displayed anatomy in real time [13].
Conclusion
Our results confirm the superiority of the navigation technique, which ensures greater accuracy, above all for the percutaneous procedure. A significant reduction in radiation exposure was also noted in our percutaneous navigation group. The free-hand technique is safe and accurate when it is in the hands of an experienced surgeon. In our opinion the navigation system is a valuable tool for spine surgeons, especially for complex cases.
References
Amiot LP, Lang K, Putzier M, Zippel H, Labelle H (2000) Comparative results between conventional and computer-assisted pedicle screw installation in the thoracic, lumbar, and sacral spine. Spine (Phila Pa 1976) 25:606–614
Assaker R, Reyns N, Vinchon M, Demondion X, Louis E (2001) Transpedicular screw placement: image-guided versus lateral-view fluoroscopy: in vitro simulation. Spine (Phila Pa 1976) 26:2160–2164
Austin MS, Vaccaro AR, Brislin B, Nachwalter R, Hilibrand AS, Albert TJ (2002) Image-guided spine surgery: a cadaver study comparing conventional open laminoforaminotomy and two image-guided techniques for pedicle screw placement in posterolateral fusion and nonfusion models. Spine (Phila Pa 1976) 27:2503–2508
Benzel EC, Rupp FW, McCormack BM, Baldwin NG, Anson JA, Adams MS (1995) A comparison of fluoscopy and computed tomography-derived volumetric multiple exposure transmission holography for the guidance of lumbar pedicle screw insertion. Neurosurgery 37:711–716
Bydon M, Xu R, Amin AG, Macki M, Kaloostian P, Sciubba DM, Wolinsky JP, Bydon A, Gokaslan ZL, Witham TF (2014) Safety and efficacy of pedicle screw placement using intraoperative computed tomography: consecutive series of 1148 pedicle screws. J Neurosurg Spine 21:320–328
Choi WW, Green BA, Levi AD (2000) Computer-assisted fluoroscopic targeting system for pedicle screw insertion. Neurosurgery 47:872–878
Ebmeier K, Giest K, Kalff R (2003) Intraoperative computerized tomography for improved accuracy of spinal navigation in pedicle screw placement of the thoracic spine. Acta Neurochir Suppl 85:105–113
Farber GL, Place HM, Mazur RA, Jones DE, Damiano TR (1995) Accuracy of pedicle screw placement in lumbar fusions by plain radiographs and computed tomography. Spine (Phila Pa 1976) 20:1494–1499
Fu TS, Wong CB, Tsai TT, Liang YC, Chen LH, Chen WJ (2008) Pedicle screw insertion: computed tomography versus fluoroscopic image guidance. Int Orthop 32:517–521
Gelalis ID, Paschos NK, Pakos EE, Politis AN, Arnaoutoglou CM, Karageorgos AC, Ploumis A, Xenakis TA (2012) Accuracy of pedicle screw placement: a systematic review of prospective in vivo studies comparing free hand, fluoroscopy guidance and navigation techniques. Eur Spine J 21:247–255
Gertzbein SD, Robbins SE (1990) Accuracy of pedicular screw placement in vivo. Spine (Phila Pa 1976) 15:11–14
Holly LT, Foley KT (2007) Image guidance in spine surgery. Orthop Clin North Am 38:451–461
Holly LT (2006) Image-guided spinal surgery. Int J Med Robot 2:7–15
Hott JS, Deshmukh VR, Klopfenstein JD, Sonntag VKH, Dickman CA, Spetzler RF, Robert F, Papadopoulos SM (2004) Intraoperative Iso-C C-arm navigation in craniospinal surgery: the first 60 cases. Neurosurgery 54:1131–1137
Ito Y, Sugimoto Y, Tomioka M, Hasegawa Y, Nakago K, Yagata Y (2008) Clinical accuracy of 3D fluoroscopy-assisted cervical pedicle screw insertion. Clinical article. J Neurosurg Spine 9:450–453
Johnson RG, Murphy M, Miller M (1989) Fusions and trans-fusions. An analysis of blood loss and autologous replacement during lumbar fusions. Spine 14:358–362
Kamimura M, Ebara S, Itoh H, Tateiwa Y, Kinoshita T, Takaoka K (2000) Cervical pedicle screw insertion: assessment of safety and accuracy with computer-assisted image guidance. J Spinal Disord 13:218–224
Kim YJ, Lenke LG, Cheh G, Riew KD (2005) Evaluation of pedicle screw placement in the deformed spine using intraoperative plain radiographs: a comparison with computerized romography. Spine (Phila Pa 1976) 30:2084–2088
Kosmopoulos V, Schizas C (2007) Pedicle screw placement accuracy: a meta-analysis. Spine (Phila Pa 1976) 32:E111–E120
Kotani Y, Abumi K, Ito M, Takahata M, Sudo H, Ohshima S, Minami A (2007) Accuracy analysis of pedicle screw placement in posterior scoliosis surgery: comparison between conventional fluoroscopic and computer-assisted technique. Spine (Phila Pa 1976) 32:1543–1550
Laine T, Lund T, Ylikoski M, Lohikoski J, Schlenzka D (2000) Accuracy of pedicle screw insertion with and without computer assistance: a randomised controlled clinical study in 100 consecutive patients. Eur Spine J 9:235–240
Laine T, Makitalo K, Schlenzka D, Tallroth K, Poussa M, Alho A (1997) Accuracy of pedicle screw insertion: a prospective CT study in 30 low back patients. Eur Spine J 6:402–405
Laine T, Schlenzka D, Makitalo K, Tallroth K, Nolte LP, Visarius H (1997) Improved accuracy of pedicle screw insertion with computer-assisted surgery. A prospective clinical trial of 30 patients. Spine (Phila Pa 1976) 22:1254–1258
Neo M, Sakamoto T, Fujibayashi S, Nakamura T (2005) The clinical risk of vertebral artery injury from cervical pedicle screws inserted in degenerative vertebrae. Spine (Phila Pa 1976) 30:2800–2805
Quinones-Hinojosa A, Robert Kolen E, Jun P, Rosenberg WS, Weinstein PR (2006) Accuracy over space and time of computer-assisted fluoroscopic navigation in the lumbar spine in vivo. J Spinal Disord Tech 19:109–113
Richter M, Cakir B, Schmidt R (2005) Cervical pedicle screws: conventional versus computer-assisted placement of cannulated screws. Spine (Phila Pa 1976) 30:2280–2287
Ringel F, Stoffel M, Stuer C, Meyer B (2006) Minimally invasive transmuscular pedicle screw fixation of the thoracic and lumbar spine. Neurosurgery 59:ONS361–ONS367
Roy-Camille R, Saillant G, Berteaux D, Salgado V (1976) Osteosynthesis of thoraco-lumbar spine fractures with metal plates screwed through the vertebral pedicles. Reconstr Surg Traumatol 15:2–16
Sakai Y, Matsuyama Y, Nakamura H, Katayama Y, Imagama S, Ito Z, Ishiguro N (2008) Segmental pedicle screwing for idiopathic scoliosis using computer-assisted surgery. J Spinal Disord Tech 21:181–186
Sakamoto T, Neo M, Nakamura T (2004) Transpedicular screw placement evaluated by axial computed tomography of the cervical pedicle. Spine (Phila Pa 1976) 29:2510–2515
Shin BJ, James AR, Njoku IU, Hartl R (2012) Pedicle screw navigation: a systematic review and meta-analysis of perforation risk for computer-navigated versus freehand insertion. A review. J Neurosurg Spine 17:113–122
Silbermann J, Riese F, Allam Y, Reichert T, Koeppert H, Gutberlet M (2011) Computer tomography assessment of pedicle screw placement in lumbar and sacral spine: comparison between free-hand and O-arm based navigation techniques. Eur Spine J 20:875–881
Slomczykowski M, Roberto M, Schneeberger P, Ozdoba C, Vock P (1999) Radiation dose for pedicle screw insertion. Fluoscopic method versus computer-assisted surgery. Spine (Phila Pa 1976) 24:975–983
Tian NF, Huang QS, Zhou P, Zhou Y, Wu RK, Lou Y, Xu HZ (2011) Pedicle screw insertion accuracy with different assisted methods: a systematic review and meta-analysis of comparative studies. Eur Spine J 20:846–859
Tian NF, Xu HZ (2009) Image guided pedicle screw insertion accuracy: a meta-analysis. Int Orthop 33:895–903
Tjardes T, Shafizadeh S, Rixen D, Paffrath T, Bouillon B, Steinhausen ES, Bäthis H (2010) Image-guided spine surgery: state of the art and future directions. Eur Spine J 19:25–45
Tormenti MJ, Kostov DB, Gardner PA, Kanter AS, Spiro RM, Okonkwo DO (2010) Intraoperative computed tomography image-guided navigation for posterior thoracolumbar spinal instrumentation in spinal deformity surgery. Neurosurg Focus 28(3):E11
Vaccaro AR, Rizzolo SJ, Balderston RA, Allardyce TJ, Garfin SR, Dolinskas C, An HS (1995) Placement of pedicle screws in the thoracic spine Part II: an anatomical and radiographic assessment. J Bone Joint Surg Am 77:1200–1206
Verma R, Krishan S, Haendlmayer K, Mohsen A (2010) Functional outcome of computer-assisted spinal pedicle screw placement: a systematic review and meta-analysis of 23 studies including 5992 pedicle screws. Eur Spine J 19:370–375
Von Jako R, Finn MA, Yonemura KS, Araghi A, Khoo LT, Carrino JA, Perez-Cruet M (2011) Minimally invasive percutaneous transpedicular screw fixation: increased accuracy and reduced radiation exposure by means of a novel electromagnetic navigation system. Acta Neurochir 153:589–596
Xu R, Ebraheim A, Shepherd ME, Yeasting RA (1999) Thoracic pedicle screw placement guided by computed tomographic measurements. J Spinal Disord 12:222–226
Conflict of Interest Statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing Switzerland
About this paper
Cite this paper
Innocenzi, G., Bistazzoni, S., D’Ercole, M., Cardarelli, G., Ricciardi, F. (2017). Does Navigation Improve Pedicle Screw Placement Accuracy? Comparison Between Navigated and Non-navigated Percutaneous and Open Fixations. In: Visocchi, M., Mehdorn, H.M., Katayama, Y., von Wild, K.R.H. (eds) Trends in Reconstructive Neurosurgery. Acta Neurochirurgica Supplement, vol 124. Springer, Cham. https://doi.org/10.1007/978-3-319-39546-3_42
Download citation
DOI: https://doi.org/10.1007/978-3-319-39546-3_42
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-39545-6
Online ISBN: 978-3-319-39546-3
eBook Packages: MedicineMedicine (R0)