Abstract
Children with sleep-disordered breathing (SDB) present alterations in posture and mobility of the stomatognathic system components. Orofacial myofunctional therapy is a modality of treatment for children with obstructive sleep apnea syndrome (OSAS) to promote changes in the orofacial musculature of the upper airways.
Orofacial myofunctional therapy helps to re-establish correct habits and functioning of orofacial muscles to avoid the residual SDB after surgical or orthodontic treatments. The treatment must be as early as possible for protecting airway health and sleep quality.
Orofacial myofunctional therapy could serve as an adjunct to other obstructive sleep apnea treatments.
Early identification and intervention during childhood development is essential to optimize normal growth of the airway and to insure a lasting impact in the treatment of SDB.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Recently there has been increasing evidence on the role of orofacial myofunctional treatment in children with sleep-disordered breathing (SDB) [1,2,3].
Obstructive SDB is an upper airway dysfunction that occurs during sleep and is characterized by snoring and/or increased respiratory effort caused by upper airway resistance and pharyngeal collapsibility [4, 5]. Obstructive SDB includes a spectrum of clinical entities from simple snoring and upper airway resistance syndrome to obstructive sleep apnea syndrome (OSAS). Adenotonsillar hypertrophy is the leading cause of OSAS; tough other risk factors include allergic rhinitis, craniofacial anomalies, neuromuscular diseases, laryngomalacia, and obesity [6,7,8].
From recent evidence in literature, we know that a stepwise therapeutic approach is needed to achieve the complete resolution of SDB. In 2010, both Bhattacharjee [9] and Ye [10] confirmed that adenotonsillectomy (AT) resolves OSAS in about 30% of children. In 2014, we also demonstrated that residual OSAS is present not only after adenotonsillectomy but even after orthodontic treatment with rapid maxillary expansion (RME) [11].
Mouth breathing and lip hypotonia are common symptoms observed in children with obstructive SDB and are related to altered nasal tone and increased nasal resistance. They are more often associated with a malposition of the tongue, thus constituting a possible interference with normal growth and development of the maxilla and mandible [12,13,14,15]. Mouth breathing could lead to deficits in orofacial muscles and directly affects the position and strength of the tongue, causing abnormal airway development and obstructive SDB [15].
The multidisciplinary therapeutic approach to children with OSAS is based on surgery, orthodontic and medical treatments, as well as weight loss in children with obesity and noninvasive ventilation when required [5, 11,12,13,14,15,16]. Different treatment modalities are often combined in a stepwise intervention to achieve the complete resolution of obstructive SDB.
Orofacial myofunctional therapy helps to re-establish correct habits and functioning of orofacial muscles to avoid the residual SDB after surgical and orthodontic treatment. The treatment must be as early as possible for protecting airway health and sleep quality. Orofacial myofunctional exercises restore a correct stomatognathic function; educate or reeducate the orofacial muscles for optimal breathing, sucking, and swallowing; eliminate wrong habits; and correct orofacial muscle problems. Therapy should be considered with integrative treatments in children with SDB [2, 3].
Craniofacial Growth and SDB
A healthy development of the jaws and upper airways is essential for good sleep and starts in the very early years. By the ninth week of fetal development, the initial cartilaginous facial skeleton is well established. By the twelfth week of fetal growth, areas of ossification appear, and bone rapidly replaces the cartilaginous template forming the early cranial base. At the same time, the bones of the cranial vault, mandible, and maxilla develop through intramembranous ossification [17,18,19].
The maximum face growth occurs between birth and 2 years of age. After birth, there is a continuous interaction between orofacial functions and the growth of anatomic features. The movement of the fetal tongue between the sixth and tenth weeks of gestational age allows the closing (i.e., vertical, horizontal, and transverse planes) of the primitive mouth (stomodeum). The tongue’s new placement below the palate changes from a previous vertical orientation to a horizontal orientation. This organization is under the control of the 39 homeobox genes (HOX). At this time in gestation, mutations involving these genes will lead to congenital orofacial syndromes such as Pierre Robin sequence. From the 20th week, the tongue grows and develops control from the brain stem, and the baby should be actively sucking and swallowing in utero from the third trimester. At birth, an infant is an obligatory nose breather. Abnormal nasal airflow also affects the palate and its maxillary alveolar dental development [20, 21]. Such changes interfere with maxillary dental arch growth which will disturb mandibular dental arch development secondarily. In particular, the changes lead to the disappearance of the diastasis (or interspace) between the deciduous incisive teeth, which in turn interferes with the placement of the permanent teeth. Nasal breathing does play a role not only in orofacial development but also in the coordination between nasal breathing and sucking which develops very early in life. Sucking and swallowing, as previously discussed, are very coordinated activities, and appropriate nasal breathing is a crucial point. Such coordinated actions (e.g., breathing and sucking) play a role in the stimulation of the structures involved in orofacial growth early in life. Mastication at close to 6 months of age is an added stimulus for such growth and must be promoted. Alterations in these functions increase the risk of abnormal development of bone structures supporting the upper airways, leading to an increased risk of collapsibility in the upper airways during sleep [12, 20]. The neurological network must be stimulated very early in life to prevent alterations in the form and function of craniofacial structures.
Orofacial Myofunctional Evaluation
Children with sleep-disordered breathing (SDB) present alterations in posture and mobility of the stomatognathic system components. Oropharyngeal muscle hypotonia is implicated in the pathogenesis of OSA, and oropharyngeal exercises may improve stomatognathic function and reduce neuromuscular impairment [2, 3].
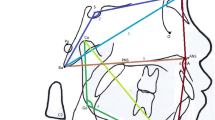
Children with SDB more often present peculiar orofacial characteristics (Fig. 40.1):
-
Long face (often asymmetric)
-
Under-eye dark circles
-
Mouth breathing
-
Lip hypotonia
-
Nasal cartilage hypotonia
Orofacial myofunctional disorders were defined as alterations/dysfunctions of the appearance, posture, and/or mobility of the lips, tongue, mandible, and cheeks and of respiration, deglutition, and mastication functions. An accurate oropharyngeal evaluation, targeted to explore the presence of mouth breathing, nasal disuse, orofacial muscle hypotonia, and an incorrect swallowing pattern, should be part in the assessment of children with SDB, in order to recognize potential improper oropharyngeal characteristics that must to be treated. In this regard, oropharyngeal exercises may help to resolve oropharyngeal muscle dysfunction that persists following the standard treatment of SDB and in this way reduce the possible contributing factors to airway collapse [22].
Validated tools that enable identifying, classifying, and grading changes in oropharyngeal muscles and function status should be used. Currently, this is possible with the Orofacial Myofunctional Evaluation with Scores (OMES)-expanded protocol validated for children [23, 24]. A standard evaluation protocol is useful for the characterization of the orofacial myofunctional conditions of children [23, 24]. Specifically, the OMES protocol is an instrument for the clinical evaluation of orofacial structures and functions of children that will permit the examiner to express numerically his perception of the characteristics and behaviors observed and that can be administered without special equipment and in a brief manner [24].
OMES-expanded permits the assessment of appearance/posture and mobility of the stomatognathic system and of functions such as breathing, swallowing, and mastication [23, 24], using observations made on an ordinal level of measurement, as defined by the psychophysical principles of measurements [23, 24]. For the orofacial myofunctional evaluation of children with SDB, it’s important to observe aspect/appearance/posture of the lips, jaws, cheeks, face, tongue, and palate; mobility of the lips, tongue, jaws, and cheeks; and functions—respiration, deglutition, and mastication [23, 24]. For respiration, the normal pattern was considered to be nasal when the subject presented labial closure without effort during rest. For deglutition, the pattern was considered normal when the subject presented the tongue contained in the oral cavity, contraction of elevator muscles, and anterior sealing of the oral cavity without effort. For mastication, the subject was instructed to chew the food (a stuffed cookie) or water in his habitual manner [23, 24].
Moreover, objective measures of muscular strength/force [25] and electromyography [26] can contribute to the oropharyngeal muscle disorder diagnosis, following the assessment of the results of the treatment.
Orofacial Myofunctional Exercises
Orofacial myofunctional exercises are designed to achieve balance of the orofacial muscles and to correct stomatognathic functions such as swallowing, breathing, speech, and chewing. Orofacial myofunctional rehabilitation consisted of isometric and isotonic exercises involving all the stomatognathic apparatus and is based on promoting proprioception, mobility, coordination, and strength of orofacial structures [23].
In our study [3], we used a set of exercises divided into three categories:
-
1.
Nasal breathing rehabilitation
-
2.
Labial seal and lip tone exercises
-
3.
Tongue posture exercises
Examples of exercises are described in Fig. 40.2.
In our study, children with residual OSAS were recruited and performed the orofacial myofunctional therapy for 3 months, exercised every day at home, at least three times a day, doing 10–20 repetitions each time. In the group treated with oropharyngeal exercises, the number of patients with a proper labial seal, increased lip tone, and re-established nasal breathing increased. In this study, oropharyngeal exercises led to a significant decrease in nasal obstruction and improved nasal patency, thereby allowing patients to regain nasal breathing; moreover, in the children with residual OSAS after adenotonsillectomy, seal lip exercises designed to strengthen the lips also allowed them to regain correct labial seal [3]. In another study conducted on subjects with primary snoring and mild to moderate OSAS, there was a significant increase in the objective measures of tongue strength, tongue peak, and endurance [25], as measured by the Iowa Oral Performance Instrument (IOPI), with the orofacial myofunctional therapy. Moreover, in the same study, the number of children with mouth breathing, abnormal tongue rest position, and lip hypotonia decreased after oropharyngeal exercises [25].
The purpose of these exercises is to increase the strength, tone, and coordination of the muscles. Added benefits include stability of treatment plans involving the upper airway. Normal muscle activity should be maintained for a lifetime; otherwise the gains in muscle strength and coordination can be lost.
The oropharyngeal reeducation involves strengthening of the tongue and orofacial muscles by teaching individuals how to assume the appropriate muscle and structure position. The tongue should be kept in a high position during sleep with its dorsal-terminal end in constant contact with the palatine striae located on the anterior aspect of the palate. Oropharyngeal reeducation may be initiated at the age of 5–6 years. The duration of treatment is variable but typically consists of 3–6 months of active therapy, followed by a maintenance period of the same duration, and it is largely related to the degree of effort parents make in reinforcing a subject to perform his or her exercises.
Usually, it is recommended that three series of exercises, with 10–20 reps for each exercise, be carried out two to three times per day at different times (at least 2 hours between sessions).
Nasal washes are most important and usually were performed two times, in the morning and evening during the entire period of treatment.
The early diagnosis and treatment of oropharyngeal muscle dysfunction in children with OSAS is mandatory to optimize the normal growth of the upper airways and to ensure a lasting impact in the treatment of obstructive SDB [2, 26].
Obstructive SDB and Orofacial Myofunctional Therapy
There are recent studies demonstrating the efficacy of orofacial myofunctional exercises as treatment for residual OSAS and as adjunct treatment in children with mild to moderate OSAS.
In a retrospective study conducted on oropharyngeal exercises in children with OSAS, Guilleminault et al. demonstrated the reduction of apnea hypopnea index (AHI) in children with residual disease [2]. The authors evaluated 24 children who were cured by the combination of adenotonsillectomy and palatal expansion (AHI 0.4 ± 0.3) [2]. Eleven children received oropharyngeal exercises (treatment group) and were compared with 13 children (control group). At the 4-year follow-up, the children who performed oropharyngeal exercises over the long term did not exhibit residual OSAS (AHI 0.5 ± 0.4 ev/h), compared to children who were never trained to perform the exercises and subsequently had a recurrence of OSAS (AHI 5.3 ± 1.5/h).
In our prospective study conducted in a small cohort of children with residual OSAS after adenotonsillectomy, we demonstrated a complete resolution of the disease [3]. Post-adeno-tonsillectomy children were randomized to either oropharyngeal exercises or control group. Fourteen patients were assigned to the treatment group, and they performed PSG before and after 2 months of oropharyngeal exercises. We observed a 62% reduction in AHI (from 4.87 ± 3.0 ev/h to 1.84 ± 3.2 ev/h, p = 0.004) in the treatment group. Minimal change in AHI (4.56 ev/h to 4.11 ev/h) was found in the control group.
In another randomized control [25] on 54 children (mean age 7.1 ± 2.5 years, 29 male) with obstructive SDB, we demonstrated the efficacy of oropharyngeal exercises on sleep respiratory parameters. Mean oxygen saturation increased (96.4 ± 0.6 vs 97.4 ± 0.7, p = 0.000), and the oxygen desaturation index decreased (5.9 ± 2.3 vs 3.6 ± 1.8, p = 0.001) only in children assigned to treatment group. Moreover, we evaluated in a randomized case-control study the effects of oropharyngeal exercises on tongue tone and symptoms in 54 children (mean age 7.1 ± 2.5 years, 29 male) with obstructive SDB [25]. Orofacial myofunctional characteristics, an assessment of tongue tone using Iowa Oral Performance Instrument (IOPI, IOPI Medical), and nocturnal pulse oximetry were performed at T0 and after 2 months (T1) in treatment and control groups. The IOPI objectively measures the tongue strength and endurance. Tongue strength is expressed as the maximum pressure in kPa exerted when an individual puts pressure with her tongue on a disposable, standard-sized tongue bulb against the roof of the mouth. The standard procedure and reference values for age have been previously validated by Potter et al. [27]. Maximum tongue pressure was measured in triplicate with each effort lasting approximately 1 second and with a rest period of 1 minute between trials. Endurance was measured by asking subjects to maintain 50% of their maximum pressure for as long as possible, and the duration of the endurance measurement was expressed in seconds.
In children who performed oropharyngeal exercises, oral breathing (83.3 vs 16.6%, p < 0.0002) and lip hypotonia (78 vs 33.3%, p < 0.003) were reduced, and normal tongue resting position (5.6 vs 33.4%, p < 0.04) was restored. Mean tongue strength (31.9 ± 10.8 vs 38.8 ± 8.3, p = 0.000), tongue peak pressure (34.2 ± 10.2 vs 38.1 ± 7.0, p = 0.000), and endurance (28.1 ± 8.9 vs 33.1 ± 8.7, p = 0.01) significantly increased in the treatment group. These data demonstrate that oropharyngeal exercises reduced respiratory symptoms during the night and mouth breathing, and increased tongue tone as measured by IOPI, in children with SDB. Moreover, subjects with SDB were found to have lower tongue strength as measured by the IOPI than healthy children, and authors have speculated that these aspects were probably due to the persistence of mouth breathing affecting tongue position and strength and possibly leading to orofacial muscle disorders and impaired growth of stomatognathic apparatus [15].
Cheng et al. [28] investigated the effects of an oropharyngeal motor training program on ten children with OSAS in Hong Kong. This reeducation training was performed to strengthen the tongue and oral-facial muscles by teaching individuals how to reposition muscles appropriately. Assessments were conducted at two time points: (a) before training and (b) 2 months post-training.
The training program consisted of ten individual mobilization exercises involving orofacial and pharyngeal area that required 45 minutes to complete. Each exercise had to be repeated ten times. Three outcome measures were chosen to study the effectiveness of the training program including tongue strength, tongue endurance level, and orofacial function. Tongue strength and tongue endurance level were assessed using the IOPI. The Nordic Orofacial Test-Screening (NOT-S) Assessment was used to assess the orofacial function. Seven out of ten participants completed the training program and attended the follow-up session after 2 months. The tongue strength (mean 38.00 vs mean 48.29 KPa, p = 0.018) and the scores of NOT-S of the seven participants were found to have significant improvement after training. Oropharyngeal motor training could improve the symptoms of children with OSAS such as oromotor function, including chewing, feeding, and reducing mouth breathing.
Mouth breathing and the resulting abnormal tongue position at rest and during sleep in children with SDB are more often associated with dento-skeletal malocclusions, as has been demonstrated by other authors [29, 30] for the consequent reduction in the modeling role of the tongue on the oral cavity [31]. The improvement in tongue function after 2 months of oropharyngeal exercises was accompanied by improved oximetry sleep parameters (mean oxygen saturation, reduced oxygen desaturation index). In children who followed the recommendations of oropharyngeal exercises with an aim to eliminate mouth breathing and recover nasal breathing, clinical and PSG improvements were achieved [32].
Other New Evidences
In a recent study, Chuang et al. [33] evaluated the short-term therapeutic effect of passive myofunctional therapy using an oral appliance during sleep in children with OSAS. The oral appliance is a one-piece, custom-made adjustable device for advancing the mandible. A bead is mounted on the lower part of the frame for the tip of the tongue to roll, which in turn places the tongue in a forward position, opening the airway [33]. The amount of mandibular advancement associated with the wearing of the device was 50%. Patients were instructed to wear their appliances and use their tongue to roll the bead (i.e., passive myofunctional therapy) during sleep every night. Twenty-nine children with OSAS were recruited and were divided into two groups: premature children and full-term children. All children wore an oral device to induce their tongue muscle activity during sleep for 6 months. Polysomnography during sleep was performed before and 1 week after the end of 6-month treatment. Both groups, full-term and premature children, had a significant decrease in the AHI. Prematurely born children had a significant decrease in the AHI during rapid eye movement sleep and in the mean heart rate during sleep [33].
Conclusions
Current literature demonstrates that orofacial myofunctional therapy plays an important role in the treatment of children with obstructive SDB and that orofacial myofunctional exercises could decrease AHI in children with residual OSAS. Oxygen saturations and SDB symptoms are improved when children perform orofacial myofunctional therapy. Treatment decreased mouth breathing, re-established nasal breathing, and improved orofacial muscle performance. Moreover, children with obstructive SDB have lower tongue strength, as measured by the IOPI, than healthy children, and oropharyngeal exercises can increase tongue tone.
Oropharyngeal exercise is repetitive muscle training, with specific gains in the coordination, tonicity, and endurance of the muscles, considering the specificity of the exercises adopted (isotonic and isometric). Oropharyngeal exercises represented a valid integrated treatment for children with mild to moderate OSAS and residual OSAS.
The objectives of orofacial myofunctional therapy are:
-
Recover and improve dyskinetic orofacial muscle function
-
Restore deficient orofacial muscle tone
-
Reacquire correct posture (tongue, jaw, lips)
-
Reeducate functions (swallowing, phonation, chewing, breathing)
-
Reduce and eliminate habits such as thumb-sucking and pacifier use
When breathing problems during sleep are present, orofacial myofunctional therapy aims to restore the function of the nose as the main upper airway route for respiration. A multidisciplinary approach with standardized orofacial myofunctional evaluation in children with obstructive SDB is mandatory.
References
Camacho M, Certal V, Abdullatif J, Zaghi S, Ruoff CM, Capasso R, Kushida CA. Myofunctional therapy to treat obstructive sleep apnea: a systematic review and meta-analysis. Sleep. 2015;38(5):669–75.
Guilleminault C, Huang YS, Monteyrol PJ, Sato R, Quo S, Lin CH. Critical role of myofascial reeducation in pediatric sleep-disordered breathing. Sleep Med. 2013;14(6):518–25.
Villa MP, Brasili L, Ferretti A, Vitelli O, Rabasco J, Mazzotta AR, Pietropaoli N, Martella S. Oropharyngeal exercises to reduce symptoms of OSA after AT. Sleep Breath. 2015;19(1):281–9.
Katz ES, D’Ambrosio CM. Pathophysiology of pediatric obstructive sleep apnea. Proc Am Thorac Soc. 2008;5:253–62.
Kaditis AG, Alonso Alvarez ML, Boudewyns A, Alexopoulos EI, Ersu R, Joosten K, Larramona H, Miano S, Narang I, Trang H, Tsaoussoglou M, Vandenbussche N, Villa MP, Van Waardenburg D, Weber S, Verhulst S. Obstructive sleep disordered breathing in 2- to 18-year-old children: diagnosis and management. Eur Respir J. 2016;47(1):69–94.
Marcus CL, Brooks LJ, Draper KA, Gozal D, Halbower AC, Jones J, Schechter MS, Sheldon SH, Spruyt K, Ward SD, Lehmann C, Shiffman RN. Clinical practice guideline. Diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics. 2012;130(3):576–84.
Kheirandish-Gozal L, Bhattacharjee R, Gozal D. Autonomic alterations and endothelial dysfunction in pediatric obstructive sleep apnea. Sleep Med. 2010;11(7):714–20.
Chang SJ, Chae KY. Obstructive sleep apnea syndrome in children: epidemiology, pathophysiology, diagnosis and sequelae. Korean J Pediatr. 2010;53(10):863–71.
Bhattacharjee R, Kheirandish-Gozal L, Spruyt K, Mitchell RB, Promchiarak J, Simakajornboon N, Kaditis AG, Splaingard D, Splaingard M, Brooks LJ, Marcus CL, Sin S, Arens R, Verhulst SL, Gozal D. Adenotonsillectomy outcomes in treatment of obstructive sleep apnea in children: a multicenter retrospective study. Am J Respir Crit Care Med. 2010;182(5):676–83.
Ye J, Liu H, Zhang GH, Li P, Yang QT, Liu X, Li Y. Outcome of adenotonsillectomy for obstructive sleep apnea syndrome in children. Ann Otol Rhinol Laryngol. 2010;119(8):506–13.
Villa MP, Castaldo R, Miano S, Paolino MC, Vitelli O, Tabarrini A, Mazzotta AR, Cecili M, Barreto M. Adenotonsillectomy and orthodontic therapy in pediatric obstructive sleep apnea. Sleep Breath. 2014;18(3):533–9.
Harvold EP, Tomer BS, Vargervik K, Chierici G. Primate experiments on oral respiration. Am J Orthod. 1981;79:359–72.
Miller AJ, Vargervik K, Chierici G. Experimentally induced neuromuscular changes during and after nasal airway obstruction. Am J Orthod. 1984;85:385–92.
Vargervik K, Miller AJ, Chierici G, Harvold E, Tomer BS. Morphologic response to changes in neuromuscular patterns experimentally induced by altered modes of respiration. Am J Orthod. 1984;85:115–24.
Huang YS, Guilleminault C. Pediatric obstructive sleep apnea and the critical role of oral-facial growth: evidences. Front Neurol. 2013;3:184.
Kaditis A, Kheirandish-Gozal L, Gozal D. Algorithm for the diagnosis and treatment of pediatric OSA: a proposal of two pediatric sleep centers. Sleep Med. 2012;13(3):217–27.
Guilleminault C, Huang YS. From oral facial dysfunction to dysmorphism and the onset of pediatric OSA. Sleep Med Rev. 2018;40:203–14.
Aknin JJ. La croissance cranio-faciale. Paris: SID Publ; 2007. p. 159–78.
Som PM, Naidich TP. Illustrated review of the embryology and development of the facial region, part 1: early face and lateral nasal cavities. Am J Neuroradiol. 2013;34:2233–40.
De Coster PJ, Marks LA, Martens LC, Huysseune A. Dental agenesis: genetic and clinical perspectives. J Oral Pathol Med. 2009;38:1–17.
Cheng MC, Enlow DH, Papsidero M, Broadbent BH Jr, Oyen O, Sabat M. Developmental effects of impaired breathing in the face of the growing child. Angle Orthod. 1988;58:309–20.
de Felício CM, da Silva Dias FV, Trawitzki LVV. Obstructive sleep apnea: focus on myofunctional therapy. Nat Sci Sleep. 2018;10:271–86. eCollection 2018. Review
de Felício CM, Folha GA, Ferreira CL, Medeiros AP. Expanded protocol of orofacial myofunctional evaluation with scores: validity and reliability. Int J Pediatr Otorhinolaryngol. 2010;74(11):1230–9.
de Felício CM, Ferreira CL. Protocol of orofacial myofunctional evaluation with scores. Int J Pediatr Otorhinolaryngol. 2008;72(3):367–75.
Villa MP, Evangelisti M, Martella S, Barreto M, Del Pozzo M. Can myofunctional therapy increase tongue tone and reduce symptoms in children with sleep-disordered breathing? Sleep Breath. 2017;21(4):1025–32. https://doi.org/10.1007/s11325-017-1489-2. Epub 2017 Mar 18.
de Felício CM, da Silva Dias FV, Folha GA, de Almeida LA, de Souza JF, Anselmo-Lima WT, Trawitzki LV, Valera FC. Orofacial motor functions in pediatric obstructive sleep apnea and implications for myofunctional therapy. Int J Pediatr Otorhinolaryngol. 2016;90:5–11.
Potter NL, Short R. Maximal tongue strength in typically developing children and adolescents. Dysphagia. 2009;24(4):391–7.
Cheng SY, Kwong SHW, Pang WM, Wan LY. Effects of an oral-pharyngeal motor training programme on children with obstructive sleep apnea syndrome in Hong Kong: a retrospective pilot study. Hong Kong J Occup Ther. 2017;30(1):1–5.
Rappai M, Collop N, Kemp S, de Shazo R. The nose and sleep-disordered breathing: what we know and what we do not know. Chest. 2003;124(6):2309–23. Review.
Van Dyck C, Dekeyser A, Vantricht E, Manders E, Goeleven A, Fieuws S, Willems G. The effect of orofacial myofunctional treatment in children with anterior open bite and tongue dysfunction: a pilot study. Eur J Orthod. 2016;38(3):227–34.
Peat JH. A cephalometric study of tongue position. Am J Orthod. 1968;54:339–51.
Lee SY, Guilleminault C, Chiu HY, Sullivan SS. Mouth breathing, “nasal disuse,” and pediatric sleep-disordered breathing. Sleep Breath. 2015;19(4):1257–64.
Chuang LC, Lian YC, Hervy-Auboiron M, Guilleminault C, Huang YS. Passive myofunctional therapy applied on children with obstructive sleep apnea: a 6-month follow-up. J Formos Med Assoc. 2017;116(7):536–41.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Villa, M.P., Evangelisti, M. (2021). Myofunctional Approaches to Pediatric Sleep Medicine. In: Gozal, D., Kheirandish-Gozal, L. (eds) Pediatric Sleep Medicine. Springer, Cham. https://doi.org/10.1007/978-3-030-65574-7_40
Download citation
DOI: https://doi.org/10.1007/978-3-030-65574-7_40
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-65573-0
Online ISBN: 978-3-030-65574-7
eBook Packages: MedicineMedicine (R0)