Abstract
Health Technology (HT) is vital to health care and wellness programs. The dependence on HT services and the expectation for novel approaches has never been greater. Patients, payers, and administrators are demanding innovative HT and optimal services. Clinical Engineers (CEs) are critical members of the healthcare team and are responsible for current and emerging strategies for HT management. But is their role recognized? An IFMBE Clinical Engineering Division (CED) survey determined it was generally unrecognized and collected further data with a landmark survey of success stories. 400 stories from 125 countries qualified as evidence-based CE contributions. A subset of innovation stories were subsequently extracted to see how innovation approaches and solutions could be effectively shared with stakeholders. These stories demonstrated significant benefits from HT innovation and evidenced a compelling case for CEs to embrace innovation as brand for their work and a path to enhance recognition within the global health community.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
The clinical engineering (CE) profession has grown alongside important and visible professions like physicians and other patient caregivers. In the decade of the 1970s, the nascent patient care technology that CEs began to manage included discreet medical devices. Visibility and influence for CEs was enhanced by the unique and valuable skill set of the clinical engineer and their close relationship with physicians. The few clinical engineers available were involved in the planning, acquisition, maintenance, and use of medical devices.
A snapshot from the past illustrates the special relationship clinical engineers had with physicians. From time to time, a clinical engineer could receive requests from physicians such as coming up with a way to measure the pressure of a heart chamber to confirm a diagnosis. The CE would assemble a set of devices that included a blood pressure monitor to connect to the catheter with a transducer tip to be inserted into the patient’s heart, an EKG monitor; and a defibrillator. The procedure was conducted in a sterile room with a fluoroscope in a dynamic mode to indicate to the radiologist the catheter’s progress along the patient’s vessels. The team for this intervention included the CE who scrubbed, sat next to the large arrangement of devices, and ensured all systems were appropriately connected, calibrated, and functioning.
Moving forward just a few decades, the incredible growth and complexity of health technology along with the increased demand for patient services began changing the health delivery scene. Digital and information technology (IT) changed the health care team relationships. New players in the patient space like the health IT professionals brought another perspective to the health care team. The proliferation of user devices and networks moved health IT to center front in visibility to the policy and decision makers. Meanwhile clinical engineers were concentrating on medical devices mostly at operational levels.
Gaining visibility and enhancing the value to our organizations and stakeholders is imperative. Innovation is on the current priority list of most health care organizations. Focusing on this aspect is of high value to Clinical Engineers (CEs). This paper describes some examples of how to get visibility with our executives and grow in our careers.
2 Methodology
2.1 Background
The 1st Global CE Summit, under IFMBE/CED, was organized in 2015 to determine the common international challenges to the CE profession. At the 2nd Global CE Summit in September 2017, these concerns were reviewed and updated. At both events, attendees agreed to address the most pertinent barriers:
-
lack of professional recognition and influence, and
-
lack of sufficient education and training for entering the field and for professional development.
The Summits’ action plans included first, data collection identifying if CE contributions qualify as improvement to world health and wellness, and whether these stories can it be substantiated through evidence-based (reproducible, data-driven) records.
The results of this timely research were the base to further the quest for options to address the barriers identified in the Summits. Over four hundred stories from around the globe were collected and validated. Among the stories, there were many that displayed a high degree of innovation. Innovation is a highly valued process and outcome, and the various projects clearly validated the involvement and contribution of clinical engineers in the health care community. Following this line of thought, 78 “Success Stories” with innovation were extracted from the main body of research to start on the path of aligning with innovation to tell our stories.
2.2 Definitions
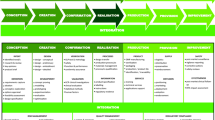
Innovation often occurs at the beginning of the HT life cycle where new ideas can offer solutions to current problems faced by healthcare providers or their patients. Clinical engineers are well positioned to understand the current problems and guide different or new approaches to resolve them. Innovation, in the CED data collection effort, means to demonstrate the team approach to solving problems all the way from a concept and building a prototype and continuing with clinical trials and demonstration of compliance with standards, regulations, and intended outcomes.
Innovation then is a pathway for clinical engineers to achieve improvement for both professional challenges outlined above. Be an innovator! We CEs already are … we just tell our stories. We need to be able to learn from all kinds of sources—both within healthcare and outside; and use ‘systems thinking’ to collaborate with others. The C-Suite in health care thrives on innovation.
Innovation for our Success Stories was defined as: “through provision of new HT solutions, adaptation of existing, or a combination to address several issues.” [1]. Summaries from CED’s 2016 and 2017 data collection of evidence-based Innovation stories are outlined below: (1) CED’s HT Resources [1] document provided to the World Health Organization (WHO’s) World Health Assembly in May 2016, WHO’s May 2017 Third Global Forum on Medical Devices [2]; (2), CED’s September 2017 Brazil II ICEHTMC [3] (S), and Others [4] from 2016–2017 IFMBE published sources (O).
2.3 Success Stories
2.3.1 2016 = 17 Total; 13 + Countries
USA | India | Ethiopia | Australia | Uruguay |
|---|---|---|---|---|
MG Hospital re test for superbugs [1] | Sharma, AMTZ—Local production of HT and MOH innov [1] | Optimal design of O2 concentrators [1] | New blood/fluid warner design [1] | Simini, CE driving facility design [1] |
Bangladesh: HT policy and HTM [1] | South Africa: Local production of HT in Africa [1] | Italy: Robotic surgery [1] | Colombia: Bus. opps in HT; Castaneda [1] | |
WHO, Tech specs O2 concentrators [1] | Malaysia: Biomechanics for Amputee [1] | Tanzania: MCH (maternal child health) rural HT [1] | Peru: Heavy metals detection [1] | Canada: Province respiratory outreach [1] |
2.3.2 2017 = 61 More; 16 + Countries
WHO/Global | India | USA | UK | Brazil | Colombia |
|---|---|---|---|---|---|
G-PATH (20) MCH [2]; G-WHO assistive HT | G-Prasant, GANDI—needs driven innov. [2] | G-Un. Oxford child Pneu. diag [2] | O-Cipro pharm model. and circuits [4] | ||
G-Priority devices, WHO HQ and EMRO [2] | G-Hypothermia alert for newborns-Bempu [2] | G-Early detection brst canc—Un WA [2] | G-Endo GI canc scrg leeds Un [2]. | G-Photometric test gestational age [2] | O-ECG signal modeling [4] |
G-UNICEF: how we drive innovations [2] | G-Prevent apnea prematurity-bempu [2] | G-Field test neo photothera. Lit Spar [2] | Norway, Denmark | O-Mechanical knee modeling [4] | |
G-Remote monitor. critical infants-Bempu [2] | G-Test pre-eclampsia Un. OSU-Geneva [2] | O-Tiss engr impr. monitoring [4] | O-Mech ventilation from pesticides [4] | ||
G-e-stethoscope child Pneu diag, Un.Gen [2]; G-Emerg. Care | G- AMTZ 2 -HT Policy impr. Svc del. [2] | Italy: G-Phototh. and transfusions [2] | S-Flow anal bld pmp [3]; O-Respiratory control with exercise [4] | ||
G-UNICEF devices for MCH, LaBarre [2], G-WHO TB diagnoses [2] | Bangladesh: G- jaundice screening-harvard [2] | IFMBE: G-BME and HTA, Pecchia [2] | S-BME aid diagnose pathologies [3], S-Hi flow nasal therapy [3] | O-Respiratory system simulation [4], O-Parkin. EEG study [4] | |
G-WHO: Dig Hlth Inv [2], G-Innov LRC 2 [2]; G-NCD kit refugees [2] | China: S-renal GRF estimation [3]; Australia: G-O2 storage [2] | G-CED Inn, david [2], G-CE-IT innovation, castaneda, judd [2] | Croatia: O-Diab Pts remote mon. [4] | Mexico: G-Hand orthosis [2] | Chile: S-Clin Sim prior to new Facility opening [3]. |
2.4 Discussion
From the validated success stories there were 78 stories that met de criteria for innovations. Additionally, they were grouped in four categories and selected ones were presented at a Special Session on CE Innovation at the 2018 Prague World BME/CE (IUPESM) World Congress: (Table 1)
A useful grouping of innovations is the simplified classification of groups into technical, administrative, product and process [5]. Further refining yields the following groups.
-
Structure of health care delivery
-
Process of care delivery
-
Outcomes of health care delivery approach
-
Individual medical device/HT system design improvement
To position the importance and need for the innovation programs presented within the four groups, it is useful to review the global healthcare needs and priorities. One of the credible sources in health care is the annual Deloitte Global Healthcare Outlook [6]. Information contained in the report is reviewed by a large number of stakeholder governments, C-suites, and industry among others.
According to the report Global health care spending is projected to increase at an annual rate of 4.1% in 2017–2021, up from just 1.3% in 2012–2016. Although the battle against communicable diseases is far from over, countries are making headway through improved sanitation, better living conditions, and wider access to health care and vaccinations. The estimated number of malaria deaths worldwide fell to 429,000 in 2015, down from nearly 1 million in 2000. The number of AIDS-related deaths dropped from 2.3 million in 2005 to an estimated 1.1 million in 2015, due largely to the successful rollout of treatment.
Rapid urbanization, sedentary lifestyles, changing diets, and rising obesity levels are fueling an increase in chronic diseases—most prominently, cancer, heart disease, and diabetes—even in developing markets. China and India have the largest number of diabetes sufferers in the world, at around 114 million and 69 million, respectively. Globally; the number is expected to rise from the current 415 million to 642 million by 2040.
3 Gaining Visibility
The highest contributors to solving the problems and issues of an organization enjoy visibility of their immediate superiors and clients. Increasing the level and value of the solutions increases the visibility and reputation of clinical engineers as problem solvers. One indication that a clinical engineer has been perceived by their employers as a valuable and innovative contributor in an organization is when the engineer gets invited to meetings of other peer departments who are seeking for solution [7]. The reputation of a CE innovator brings positive visibility.
How to be aligned with the priorities of a field and organization begins with the awareness of the current problems and priorities. With the advent of Internet information about healthcare technology is readily available. Global reports and analysis from public [8] and private organizations provided analysis and priorities that are widely read and acknowledged. For example, Deloitte points out their consensus of global health care priorities for 2018:
-
Creating a positive margin in an uncertain and changing health economy
-
Strategically moving from volume to value
-
Responding to health policy and complex regulations
-
Investing in exponential technologies to reduce costs, increase access, and improve care
-
Engaging with consumers and improving the patient experience
-
Shaping the workforce of the future
Being aware of global priorities and specifically on priorities that are of special significance to your organization and clients present an opportunity to contribute with innovative solutions. Innovation focused on immediate needs is welcomed at all level of organization. A gap analysis-oriented methodology is very useful [9]. The gap is the difference between the potential and the actual status.
Relentless thinking about solutions that add value fosters a culture of innovation. Culture encompasses many factors such as the collective consensus of what is useful and valuable, what is rewarded or punished, and what is beautiful, etc. A culture of innovation can be fostered by employers and clients. However it starts with the individual who internalizes inquiry about status quo and has the discipline of adding several perspectives to solving the issues at hand.
Embracing and internalizing innovation is a basic step. Producing outcomes that elegantly a creatively support the goals and priorities of the organization is a path to visibility. One organizing frame to evaluate the level of success of an innovative outcome is to rate the outcome in terms of uniqueness and value [10]. The desired outcome is to have a unique and valuable process or product. Any other combination of uniqueness and value provides a grade for the outcome. Not unique and not valuable process or product is therefore at the bottom of the scale.
4 Conclusions
4.1 Perspective
As a result, here are some practical observations and steps forward:
-
1.
Innovation is cool, is wanted, is admired, and everybody in health care (government, private sector, industry, and academia) has acknowledged this positive item.
-
2.
We have a survey that validates the two most pressing issues for clinical engineers: lack of recognition and influence, and lack of educational pathways to the top.
-
3.
We have this one-of-a-kind global clinical engineering (CE) project that collected and validated success stories around the world. Wow, there is some serious innovation work in these success stories.
-
4.
We will acknowledge and show this work at an Innovation Track at the IUPESM World Congress.
-
5.
As we are looking for wide (outside our peers) recognition, and innovation is a language more widely recognized, can we use these innovation success stories to communicate our work with wide audiences?
-
6.
Let us submit that CE innovation is one of our recognition tickets because it swiftly reaches beyond our peer group.
-
7.
Further, let us submit that embracing innovation as a part of our professional DNA can associate a CE with a positive brand of creativity, problem solving, and usefulness to the organization and clients.
-
8.
Let us continue to write paper and craft presentations to introduce the excellent CE innovation work around the globe and propose a CE culture adjustment that transplants innovation to all of our issue/resolution processes.
5 Summary
To transform the perception of clinical engineers by policy and decision makers, first there needs to be an alignment of values and priorities on both sides, and secondly, there needs to be meaningful communication. While the alignment of values is more natural and easier in a health care team, the priorities may be quite different.
In the current environment, the concept of innovation is understood and desired by leadership. When clinical engineers are perceived as innovators, they would be noticed and acknowledged for their culture and results. To complete the transformation the second part, meaningful communication, requires that clinical engineers also embrace a process for reporting and updating their superiors and clients of their innovation accomplishments and challenges. Professional recognition for clinical engineers will come from our peers, employers, industry, and other stakeholders when we are identified as members of a culture of innovation, and we all can speak and understand a common language—we have 78 opportunities (stories) to do it. Influence is the corollary of a valued profession.
References
IFMBE Clinical Engineering Division (CED), Health Technologies Resource, May 2016, http://cedglobal.org/global-ce-success-stories/.
World Health Organization Third Global Forum on Medical Devices, May 2017, http://www.who.int/medical_devices/global_forum/3rd_gfmd/en/.
IFMBE CED 2nd International Clinical Engineering and Health Technology Management Congress (II ICEHTMC) Proceedings, September 2017, http://cedglobal.org/icehtmc2017-proceedings/.
Other IFMBE related CE Papers, http://cedglobal.org/global-ce-stories-other/.
“Health Technology Innovation Adoption” Trugul U Daim et al., page 43 (Springer).
Deloitte 2017 and 2018 Global Health Care Sector Outlook. © 2017 and © 2018 Publications. Deloitte Touche Tohmatsu Limited.
Kaiser Permanente Clinical Technology Department Innovation teams 2010.
World Health Organization (WHO) and Pan-American Health Organization (PAHO) various HT publications.
Reverse Innovation, Vijay Govindarajan, Chris Trimble, Harvard Business Press.
Lessons from Guy Kawasaki, Forbes 1/6/2016 by Denise Lee Yohn.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Singapore Pte Ltd.
About this paper
Cite this paper
Castañeda, M., Judd, T. (2019). Global Clinical Engineering Innovation, Overview and New Perspectives. In: Lhotska, L., Sukupova, L., Lacković, I., Ibbott, G. (eds) World Congress on Medical Physics and Biomedical Engineering 2018. IFMBE Proceedings, vol 68/3. Springer, Singapore. https://doi.org/10.1007/978-981-10-9023-3_150
Download citation
DOI: https://doi.org/10.1007/978-981-10-9023-3_150
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-10-9022-6
Online ISBN: 978-981-10-9023-3
eBook Packages: EngineeringEngineering (R0)