Abstract
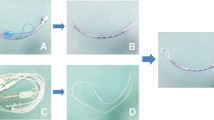
The risk of massive bleeding during liver transection and postoperative biliary leaks are due to the complex biliary and vascular anatomy of the liver. Hemorrhage was once the leading cause of death in liver resection, and the now reduced hospital mortality rate of ≤5% can be attributed to better intraoperative bleeding control. Hemorrhage and perioperative blood transfusion not only increase the risk of operative morbidity and mortality but jeopardize long-term survival after resection of liver malignancies because of the associated immunosuppression, leading to a higher risk of tumor recurrence [1]. Bleeding control is the result of the evolution of different aspects of liver surgery and anesthesia. Technological advances led to the development of specific instruments for liver transection; intraoperative ultrasound allows better delineation of the transection plane; and a better understanding of physiology and anatomy improved control of inflow and outflow. Inflow occlusion and low central venous pressure (CVP) anesthesia have been widely used to reduce bleeding from inflow vessels and backflow in the transection surface. Inflow occlusion (Pringle maneuver) has been used since the early twentieth century to prevent bleeding during transection, which is performed by crushing the liver parenchyma with the fingers or forceps (Kelly-clamp crushing), and the concomitant low CVP induced by anesthesia further minimizes blood loss by preventing retrograde bleeding from the hepatic veins. Assuming that inflow occlusion and low CVP cause significant damage due to ischemia and reperfusion, there has been a growing interest in using new devices that facilitate bloodless transection, obviating the need for inflow occlusion. In the laparoscopic setting, these factors, associated with the struggle to perform an intermittent Pringle maneuver and clamp crushing, have led to a wide diffusion of a variety of transection devices, mostly derived from those routinely used in open surgery. This chapter provides a description of the main transection device features and considerations on the Pringle maneuver associated with clamp crushing in the laparoscopic setting.
Access provided by Autonomous University of Puebla. Download to read the full chapter text
Chapter PDF
Similar content being viewed by others
Keywords
- Liver Resection
- Laparoscopic Liver Resection
- Pringle Maneuver
- Parenchymal Transection
- Laparoscopic Hepatectomy
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
References
Kooby DA, Stockman J, Ben-Porat Let al (2003) Influence of transfusions on perioperative and long-term outcome in patients following hepatic resection for colorectal metastases. Ann Surg 237(6):860–869. doi:10.1097/01.SLA.0000072371.95588.DA
Poon RT (2007) Current techniques of liver transection. HPB (Oxford) 9(3).166–173. doi:10.1080/13651820701216182
Gurusamy KS, Pamecha V, Sharma D, Davidson BR (2009) Techniques for liver parenchy-mal transection in liver resection. Cochrane Database Syst Rev (1):CD006880. doi:10.1002/14651858.CD006880.pub2
Ikeda M, Hasegawa K, Sano K et al (2009) The vessel sealing system (LigaSure) in hepatic resection: a randomized controlled trial. Ann Surg 250(2): 199–203. doi:10.1097/SLA. 0b013e3181a334f9
Nsadi B, Gilson N, Pire E et al (2011) Consequences of pneumoperitoneum on liver ischemia during laparoscopic portal triad clamping in a swine model. J Surg Res 166(1):e35–43
Takagi S (1998) Hepatic and portal vein blood flow during carbon dioxide pneumoperitoneum for laparoscopic hepatectomy. Surg Endosc 12(5):427–431
Aldrighetti L, Pulitano C, Arru M et al (2008) Ultrasonic-mediated laparoscopic liver transection. Am J Surg 195(2):270–272. doi:10.1016/j.amjsurg.2007.02.022
Troisi RI, Van Huysse J, Berrevoet F et al (2011) Evolution of laparoscopic left lateral sec-tionectomy without the Pringle maneuver: through resection of benign and malignant tumors to living liver donation. Surg Endosc 25(1):79–87. doi:10.1007/s00464-010-1133-8
Kaneko H, Otsuka Y, Tsuchiya M et al (2008) Application of devices for safe laparoscopic hepatectomy. HPB (Oxford) 10(4):219–224. doi:10.1080/13651820802166831
Slakey DP (2008) Laparoscopic liver resection using a bipolar vessel-sealing device: LigaSure. HPB (Oxford) 10(4):253–255. doi:10.1080/13651820802166880
Kim FJ, Chammas MF Jr, Gewehr E et al (2008) Temperature safety profile of laparoscopic devices: Harmonic ACE (ACE), LigaSure V (LV), and plasma trisector (PT). Surg Endosc 22(6):1464–1469.doi:10.1007/s00464-007-9650-9
Pai M, Navarra G, Ayav A et al (2008) Laparoscopic Habib 4X: a bipolar radiofrequency device for bloodless laparoscopic liver resection. HPB (Oxford) 10(4):261–264. doi:10.1080/13651820802167862
McGahan JP, Khatri VP (2008) Imaging findings after liver resection by using radiofrequency parenchymal coagulation devices: initial experiences. Radiology 247(3):896–902. doi:10.1148/radiol.2473070949
Vollmer CM, Dixon E, Sahajpal A et al (2006) Water-jet dissection for parenchymal division during hepatectomy. HPB (Oxford) 8(5):377–385. doi:10.1080/13651820600839449
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2,804 patients. Ann Surg 250(5):831–841. doi:10.1097/SLA.0b013e3181b0c4df
Cuschieri A (2005) Laparoscopic liver resections. J Minim Access Surg 1(3):99–109. doi:10.4103/0972-9941.18993
Patriti A, Ceccarelli G, Bartoli A, Casciola L (2011) Extracorporeal Pringle maneuver in robot-assisted liver surgery. Surg Laparosc Endosc Percutan Tech 21(5):e242–244. doi: 10.1097/SLE.0b01 3e31822d7fb4
Saif R, Jacob M, Robinson S et al (2011) Laparoscopic Pringle’ manoeuvre for liver resection?: how I do it. Minim Invasive Ther Allied Technol 20(6):365–368
Rotellar F, Pardo F, Bueno A et al (2011) Extracorporeal tourniquet method for intermittent hepatic pedicle clamping during laparoscopic liver surgery: an easy, cheap, and effective technique. Langenbecks Arch Surg. doi:10.1007/s00423-011-0887-3
Casciola L, Patriti A, Ceccarelli G et al (2011) Robot-assisted parenchymal-sparing liver surgery including lesions located in the posterosuperior segments. Surg Endosc 25(12):3815–3824. doi:10.1007/s00464-011-1796-9
Lee MR, Kim YH, Roh YH et al (2011) Lessons learned from 100 initial cases of laparoscopic liver surgery. J Korean Surg Soc 80:334–341. Epub 2011, May 6
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer-Verlag Italia
About this chapter
Cite this chapter
Patriti, A. (2013). Transection Devices. In: Calise, F., Casciola, L. (eds) Minimally Invasive Surgery of the Liver. Updates in Surgery. Springer, Milano. https://doi.org/10.1007/978-88-470-2664-3_9
Download citation
DOI: https://doi.org/10.1007/978-88-470-2664-3_9
Publisher Name: Springer, Milano
Print ISBN: 978-88-470-2663-6
Online ISBN: 978-88-470-2664-3
eBook Packages: MedicineMedicine (R0)