Abstract
This chapter focuses on the relatively narrow definition of radiovirotherapy as “the use of viral vectors engineered to express genes that drive uptake of radioisotopes into cancer cells for both detection and antitumor efficacy”. Having said that, it also addresses issues relating to combinations of virotherapy and standard anticancer modalities (such as external beam radiotherapy and cytotoxic chemotherapy) and novel agents (such as molecular radiosensitisers). However, within the context of radiovirotherapy, those discussions are limited solely to approaches that aim to improve the efficacy of the radioisotopic treatment.
The introductory sections describe the biology of the sodium–iodide symporter (NIS)—the gene therapy approach that has been most widely exploited for radioisotope uptake. In subsequent sections, progress from initial work with replication-defective vectors onto replication-competent oncolytic vectors is described, and this recognises the increasing acceptance of replicating viruses as the vectors of choice for cytotoxic gene therapy strategies. The section on oncolytic NIS-expressing viruses deals mainly with vectors based on adenovirus and measles virus. The final sections describe the use of NIS-expressing vectors in multi-agent regimens and highlight the potential benefits of combinatorial therapeutic regimens. The limited number of clinical translational studies that have been performed to date are also reviewed, and opportunities for future development of NIS-based therapeutic strategies are discussed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Single Photon Emission Compute Tomography Imaging
- Oncolytic Virus
- Pituitary Tumour Transforming Gene
- Oncolytic Adenovirus
- Iodide Uptake
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Introduction
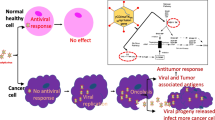
Radiovirotherapy is a term that is used to describe virally directed radioisotope therapy (Hingorani et al. 2010a). Essentially, this approach involves the use of a virus, which may be either replication defective or replication competent, as a means of delivering an exogenous gene that encodes a protein that is capable of mediating selective uptake of a specific radioisotope into a cancer cell. Most of the published literature on radiovirotherapy deals with the use of the sodium–iodide symporter (NIS) to mediate radioisotope uptake by virally infected cells [reviewed in Hingorani et al. (2010a)]. Indeed, this approach has a very strong basis in the extensive use of iodide-131 radioisotope therapy in patients with thyroid cancer. In this setting, iodide-131 has established a role as an adjuvant (radioablative) therapy post-thyroidectomy or as a definitive anticancer treatment in patients with metastatic differentiated (papillary and follicular) thyroid cancers. Therefore, in this chapter, we will focus on the use of NIS-mediated radiovirotherapy. Although this approach was initially conceived to be used with replication-defective viral vectors, in its most recent incarnation, the concept of radiovirotherapy has been modified to exploit the twin benefits of oncolytic cell killing by the virus and “bystander” killing of uninfected neighbouring cells by the emission of beta (or alpha) particles from accumulated radioisotopes.
2 Sodium–Iodide Symporter
NIS is a member of the sodium/solute symporter family (SSF) that includes more than 60 members of both prokaryotic and eukaryotic origin, many of which exhibit a high similarity of sequence and function. SSF members actively transport anions into cells by using a Na+/K+ electrochemical gradient that is generated by Na+/K+ ATPase (Jung 2002). NIS is expressed mainly on the basolateral membrane of thyroid follicular cells and cotransports sodium and iodide into cells (Fig. 9.1). Following uptake into thyroid cells, iodide is then transported to the follicular lumen and oxidised by the thyroid peroxidase in a reaction that promotes the iodination of tyrosyl residues of the thyroid hormones tri- and tetra-iodothyronine (T3 and T4) (Massart and Corbineau 2006). NIS is also expressed in a number of extrathyroidal tissues including gastric mucosa, salivary glands, digestive tract and lactating mammary glands. The expression of messenger RNA for NIS has also been documented in other tissues (e.g. pituitary gland, pancreas, thymus, lungs, prostate, testis, ovaries, kidneys, adrenal gland) by reverse-transcriptase polymerase chain reaction RT-PCR, although the functional significance of this observation is, as yet, unclear (Kogai et al. 2006; Vayre et al. 1999; Spitzweg et al. 1998, 2001a).
Diagrammatic representation of the function of NIS in iodide transport in normal thyroid follicular cells. Thyroid stimulating hormone (TSH) binding to TSH receptor (TSH-R) activates adenylate cyclase (AC) which generates cyclic AMP (cAMP) from AMP. This drives NIS-mediated co-transport of two Na+ ions along with one I− ion, with the transmembrane sodium gradient serving as the driving force for iodide uptake. Thiocyanate (CNS−) and perchlorate (ClO4−) are competitive inhibitors of thyroidal iodide accumulation. The efflux of iodide from the apical membrane to the follicular lumen is driven by pendrin (Pendred syndrome gene product). Iodide organification within the thyroid follicular lumen [mediated by thyroperoxidase (TPO) and dual oxidase 2 (Duox2)] generates iodinated tyrosine residues within the thyroglobulin (Tg) backbone. These are ultimately released as active thyroid hormone (T3 and T4) (Modified from Spitzweg et al. J. Clin. Endocrinol. Metab. 2001, 86, 3327–35)
Human NIS (hNIS) was cloned in 1996. The human NIS gene is located on chromosome 19p12–13.2, with an open reading frame of 1929 nucleotides comprising of 15 exons and 14 introns that encodes a 643-amino acid protein. Human NIS exhibits 84 % identity and 93 % similarity to rat NIS (rNIS), with the main differences accounted for by a 5-amino acid insertion between the last two hydrophobic domains and a 20-amino acid insertion in the C-terminus (Smanik et al. 1996). The protein has 13 putative transmembrane domains, an intracellular C-terminus and an extracellular N-terminus. Membrane localisation of NIS is a prerequisite for its function. NIS gene transcription in thyroid tissue is mainly regulated by thyroid-stimulating hormone (TSH), via the stimulation of the human NIS upstream enhancer (hNUE) (Taki et al. 2002). Interestingly, TSH can also modulate NIS phosphorylation and, thus, act as a post-transcriptional regulator of NIS (Riedel et al. 2001; Kogai et al. 2000). In the absence of TSH, NIS is redistributed to intracellular compartments and, therefore, functionally inactive (Riedel et al. 2001).
Other factors are also implicated in the regulation of NIS. The pituitary tumour transforming gene (PTGG), a proto-oncogene overexpressed in follicular thyroid cancers, and the PTGG-binding factor (PBF) inhibit NIS gene transcription through the inactivation of hNUE (Boelaert et al. 2007). Overexpression of these factors in thyroid cancers may have a negative impact on prognosis by reducing the potential efficacy of radioiodide therapy (Boelaert et al. 2007; Saez et al. 2006). TSH-induced NIS stimulation is also inhibited by a number of cytokines, including interleukin-1, TNF-α, interferon-α, interferon-β and interferon-γ in thyroid cells (Caraccio et al. 2005; Ajjan et al. 1998). In contrast, all-trans retinoic acid (atRA), dexamethasone and carbamazepine have each been shown to have a positive effect on NIS-mediated iodide uptake (Spitzweg et al. 2003; Willhauck et al. 2008a, 2011; Unterholzner et al. 2006), although that has not yet translated to clinical use or benefit.
Radioiodide has been used for decades to treat hyperthyroidism (Ross 2011) and differentiated thyroid cancers. Currently, it is recommended as an adjuvant treatment following total thyroidectomy in patients with unifocal or multifocal primary tumours measuring more than 1 cm in greatest dimension (pT1b, pT2, pT3), with nodal extension (N1a and N1b) or with extrathyroidal extension (pT3). It is also a standard of care in patients with disseminated metastatic well-differentiated cancers, where its use can be curative (Cooper et al. 2009). The successful treatment of thyroid tumours by NIS-mediated radioiodide therapy has sparked significant interest in virus-mediated NIS delivery as a therapeutic option in a wide range of tumour types.
3 Preclinical Studies of NIS Gene Transfer by Replication-Defective Viruses
A schematic representation of NIS-mediated radiovirotherapy is shown in Fig. 9.2. Shimura et al. (1997) successfully transfected rNIS cDNA into malignant rat thyroid cells (FRTL-Tc) by electroporation, restoring iodide transport activity in the process. In vitro, FRTL-Tc cells stably expressing rNIS accumulated 125I 60-fold and in vivo xenografts trapped up to 27.3 % of the total 125I dose with an effective half-life of approximately 6 h. However, a therapeutic dose of 37 megabecquerels (MBq) of 131I did not cause statistically significant tumour shrinkage (Shimura et al. 1997). Subsequently, several studies have confirmed the feasibility of inducing functional NIS expression in non-thyroidal tumours (Riesco-Eizaguirre and Santisteban 2006). Cho et al. (2000) showed that the delivery of exogenous hNIS by recombinant replication-defective adenovirus (Ad-CMV-hNIS) resulted in more than a 120-fold increase in iodide uptake in U1240 cells in vitro. Intratumoral injection of Ad-CMV-hNIS into subcutaneous U251 human glioma xenografts caused a 25-fold increase in 125I accumulation compared to spleen or saline-injected tumours (Cho et al. 2000). Mandell et al. (1999) demonstrated in vitro and in vivo iodide accumulation in melanoma, liver, colon and ovarian carcinoma cells after retrovirus-mediated transfection with rNIS. NIS-transduced melanoma xenografts accumulated significantly more 123I (6.9-fold increase) than non-transduced tumours (Mandell et al. 1999). Similarly Boland et al. (2000) used adenoviral-mediated NIS (CMV promoter) gene delivery to demonstrate functional levels of NIS expression in several tumour cell lines. Fold increases in iodide uptake of 125–225 times were observed in vitro, and 11 % of the total 125I dose could be recovered per gram of adenovirus-infected tumour tissue. Although an in vitro cytotoxic effect was observed, the study failed to show in vivo therapy (Boland et al. 2000). Spitzweg et al. (1999) were the first to demonstrate tissue-specific expression of hNIS cDNA in androgen-sensitive human prostate adenocarcinoma (LNCaP) following transfection with a eukaryotic expression vector in which the full-length hNIS cDNA was coupled to a prostate-specific antigen (PSA) promoter. Prostate cells transfected with PSA-NIS showed perchlorate-sensitive, androgen-dependent iodide uptake (Spitzweg et al. 1999). The same groups were also the first to demonstrate the feasibility and effectiveness of NIS-mediated cytotoxicity in vivo and, in doing, assuaged concerns that NIS-mediated therapy was unlikely to succeed due to lack of iodide-organification in non-thyroidal tumour tissues. LNCaP cell lines stably transfected with hNIS cDNA (NP-1) under the control of a PSA promoter (NP-1 cells) showed perchlorate-sensitive, androgen-dependent iodide uptake and killing in clonogenic assays in vitro. Xenograft NP-1 tumours in athymic nude mice accumulated 25–30 % of the total 123I administered with a biological half-life of 45 h. In addition, NIS protein expression in LNCaP xenografts was confirmed by Western analysis and immunohistochemistry. Critically, a single therapeutic dose of 111 MBq 131I yielded a dramatic therapeutic response in NIS-transfected LNCaP xenografts (Spitzweg et al. 2000). The same group subsequently developed a replication-deficient human adenovirus incorporating the hNIS gene driven by a CMV promoter (Ad5-CMV-NIS) for in vivo NIS gene transfer into LNCaP tumours. Following intraperitoneal injection of a single therapeutic dose of 111 MBq 131I 4 days after adenovirus-mediated intratumoral NIS gene delivery, LNCaP xenografts showed an average volume reduction of >80 % (Spitzweg et al. 2001b).
Diagrammatic representation of NIS-mediated radiovirotherapy by replication-defective adenovirus: (1) Ad-NIS is injected by the intratumoural, locoregional or systemic route. (2) Ad-NIS infects target cells through the cognate coxsackie and adenovirus receptor (CAR). (3) Ad-NIS drives NIS gene expression and protein is displayed on the cell membrane in infected cells. (4) Radioiodide is administered systemically and is taken up in NIS-expressing tumour cells. (5) β-particulate radiation mediates both direct and bystander killing of cells
Kakinuma et al. (2003) evaluated adenoviral-mediated NIS expression regulated by the tissue-specific probasin promoter in prostate and various other tumour cell lines. Interestingly, androgen-dependent and perchlorate-sensitive iodide uptake was demonstrated in LNCaP cells that was 3.2-fold higher than an Ad-CMV/hNIS vector. Furthermore, iodide uptake in a panel of non-prostate tumour cell lines infected with Ad-ARR(2)PB/hNIS was significantly lower, confirming tissue specificity with this construct (Kakinuma et al. 2003). Sieger et al. (2003) investigated radioiodide uptake in a hepatoma cell line in vitro and in vivo following the transfer of hNIS under the control of a tumour-specific regulatory element, the promoter of the glucose transporter 1 (GT1) gene. NIS-expressing stable cell lines [rat hepatoma (MH3924A)] demonstrated perchlorate-sensitive increased iodide uptake (30-fold increase in vitro and 22-fold increase in vivo) compared to the wild-type cell line. Similarly, the mean radiation dose delivered to MH3924A xenografts was 10-fold higher after the administration of 18.5 MBq of 131I (Sieger et al. 2003). Faivre et al. (2004) reported on an in vivo kinetic study of NIS-related iodide uptake in an aggressive chemically induced model of hepatocarcinoma in immunocompetent Wistar rats. An adenoviral vector expressing rNIS controlled by the CMV promoter (Ad-CMV-rNIS) was injected into the portal vein of 5 healthy and 25 hepatocarcinoma-bearing rats. This resulted in impressive (from 20 % to 30 % of the injected dose) and durable (>11 days) iodide uptake that contrasted with the rapid iodide efflux observed in vitro. Prolonged retention of iodide observed in vivo was not attributed to an active retention mechanism but to permanent recycling of the effluent radioiodide via the high hepatic blood flow. Radioiodide therapy in these circumstances was associated with strong inhibition of tumour growth, complete regression of small nodules and prolonged survival of hepatocarcinoma-bearing rats (Faivre et al. 2004).
Other preclinical studies have evaluated NIS-mediated radioiodide therapy in head and neck (FaDu, SCC-1, SCC-5) (Gaut et al. 2004), pancreatic neuroendocrine (Bon1, QGP) (Schipper et al. 2003), medullary thyroid (Cengic et al. 2005), colorectal (HCT116) (Scholz et al. 2005), breast (Dwyer et al. 2005a), ovarian (Dwyer et al. 2006a) and hepatocellular (HepG2) (Willhauck et al. 2008b) cancer models. Most of these studies confirmed that replication-defective viral vectors expressing NIS from a tissue-specific promoter were capable of mediating tumour-selective iodide uptake that translated into in vitro and in vivo therapeutic efficacy.
In addition to the rodent-based in vivo studies discussed above, a preclinical dosimetric study of NIS-mediated radioisotope therapy was performed in adult male beagle dogs. This was a safety and feasibility study in preparation for a phase I clinical trial in patients with locally recurrent prostate cancer. Animals received direct intraprostatic injections of 1 × 1012 viral particles of NIS-expressing replication-defective adenoviral vectors regulated by the CMV promoter. This was followed by intravenous injection of 111 MBq 123I and serial image acquisition using single photon emission computed tomography. Clear images of the prostate were obtained in all dogs that received Ad5-CMV-NIS, but none in the group that was injected with control virus. The average absorbed radiation dose to the prostate was estimated to be 23 ± 42 cGy/37 MBq 131I. This indicated that a 3.15 GBq dose of 131I would deliver a target dose of 20 Gy to the prostate. Following a therapeutic dose of 131I (4.3 GBq/m2), preceded by T3 supplementation for 8 days, the estimated mean doses delivered to the prostate, thyroid, stomach and liver were 12.5 ± 0.28, 0.12 ± 0.01, 0.23 ± 0.02 and 0.009 ± 0.006 Gy/37 MBq of 131I. No major toxicities or changes in blood biochemistries were noted (Dwyer et al. 2005b).
4 Preclinical Studies and Clinical Translation of NIS Gene Transfer by Replication-Competent Viruses
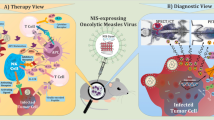
As reviewed above, the initial development of virus-mediated NIS delivery was based on the notion that the virus would act purely as a vehicle for delivering the therapeutic gene. However, within the last decade, there has been a fundamental re-evaluation of strategy such that much greater emphasis is now placed on the use of replication-competent or oncolytic virus vectors (Fig. 9.3). There are a number of potential advantages to using oncolytic viruses, including their greater potency due to their intrinsic cytotoxicity and ability to self-amplify and, thus, increase levels of transgene expression and their impressive safety record. Initial concerns regarding the possible toxic consequences of using replication-competent viruses in immunocompromised cancer patients and the threat of environmental release and contamination have been largely assuaged by data from a series of phase I and II clinical trials (see Harrington et al. (2010) for an account of this process).
Diagrammatic representation of NIS-mediated radiovirotherapy by replication-competent oncolytic measles virus: (1) MV-NIS is injected by the intratumoural, locoregional or systemic route. (2) MV-NIS infects target cells through the cognate CD46 receptor. (3) MV-NIS drives NIS gene expression and protein is displayed on the cell membrane in infected cells. (4) Radioiodide is administered systemically and is taken up in NIS-expressing tumour cells. (5) β-particulate radiation mediates both direct and bystander killing of cells. (6) Viral replication leads to death of tumour cell that was initially infected. (7) Viral oncolysis of primarily infected cell leads to release of progeny virions and second-wave infection of adjacent tumour cells
A number of NIS-expressing oncolytic agents have been assessed. We recently reported in vivo SPECT imaging of the time course of gene expression from two oncolytic adenoviruses expressing NIS in tumour-bearing mice (Merron et al. 2007). In these viruses, the hNIS cDNA was positioned in the E3 region either in a wild-type adenovirus type 5 (AdIP1) or one in which a promoter from the human telomerase gene (RNA component) was driving E1 expression (AdAM6). Viruses showed functional hNIS expression and replication in vitro, and the kinetics of spread of the two viruses in tumour xenografts were visualised in vivo using a small animal nano-SPECT/CT camera. The time required to reach maximal spread was 48 h for AdIP1 and 72 h for AdAM6 suggesting that genetic engineering of adenoviruses can affect the kinetics of their dissemination in tumours. More recently, we have shown that a Wnt-targeted oncolytic adenovirus expressing NIS can mediate a specific oncolytic effect that is augmented by the additional delivery of 131I (Peerlinck et al. 2009). Importantly, SPECT imaging studies allowed careful evaluation of the optimal therapeutic schedule for virus administration and subsequent radioisotope delivery. Thus, a single radioisotope dose delivered 48 h after virus administration resulted in very significant antitumor efficacy.
This same approach has been taken in to the clinic in a phase I study of a replication-competent Ad5 adenovirus armed with two suicide genes (yeast cytosine deaminase, mutant thymidine kinase) and the human NIS gene (Ad5-yCD/TK-hNIS) (Barton et al. 2008). Men with clinically localised prostate cancer received an intraprostatic injection of Ad5-yCD/TK-hNIS, armed with two suicide genes and the NIS gene. Expression of the NIS gene was monitored non-invasively using single photon emission computed tomography (SPECT) after injection of 99mTcO4 −. Ad5-yCD/TK-hNIS was well tolerated and 98 % of the adverse events were grade 1 or 2. Importantly, NIS gene expression was detected in the prostate of seven of the nine patients who received a dose of 1 × 1012 virus particles (vp), but not at 1 × 1011 vp. The authors reported on the time course and the geographical extent of NIS gene expression within and without the prostate following injection of 1 × 1012 vp in 1 cm3. NIS gene expression peaked at 24–48 h after injection, but was still detectable in the prostate for up to 7 days. The volume of prostate in which gene expression was seen averaged 6.6 cm3, representing 18 % of the total prostate volume. There was no evidence of extraprostatic dissemination of the adenovirus by SPECT imaging (Barton et al. 2008).
The same group conducted further studies in which they attempted to define the dose of radiotherapy that might be delivered to the entire prostate gland if 131I-based Ad5-yCD/TK-hNIS radiovirotherapy were used as a definitive therapy (Barton et al. 2011). They recruited six patients with clinically localised prostate adenocarcinoma (5 T1c, 1 T2; Gleason range from 3 + 4 to 4 + 5) that was restricted to one sextant in four patients and bilateral in the other two patients. A standard injection protocol was used to optimise Ad5-yCD/TK-hNIS delivery across the entire prostate gland, such that a total of 5 × 1012 viral particles were injected in 12 separate deposits in a volume of 5 mL. The patients then underwent serial SPECT imaging following administration of 99mTcO4 −. NIS gene expression was detected in the prostate of all six patients, and as with the previous study (Barton et al. 2008), there was no evidence of extraprostatic gene expression. The mean gene expression volume was 14.6 cm3 with a range of 6.6–28.9 cm3, and this represented 18–83 % (mean 45 %) of the total prostate volume. The authors then went on to estimate the radiation doses that would have been achieved had the patients received a dose of radioactive 131I equivalent to 7.4 GBq (200 mCi). These data revealed that the mean absorbed dose to the prostate would have been 7.2 ± 4.8 Gy (based on a gene expression volume of 45 %) and 15.4 ± 3.3 Gy (had the entire prostate been transduced to the same extent). It is important to realise that, in order to make these estimates, a number of assumptions were necessary and that their general effect would have resulted in an overestimation of radiation dose delivery. First, the deposition of 99mTcO4 − within the prostate was calculated by relating the mean image pixel intensity to that in the iliac artery. Standard values for 99mTcO4 − blood clearance and estimation of tissue attenuation of the signals detected by SPECT were then applied to yield the radioisotope activity in the volume of the prostate gland transduced with Ad5-yCD/TK-hNIS. Thereafter, the dose in Gy that would be delivered following the administration of 7.4 GBq of radioiodide was calculated by assuming that the expression of hNIS remained constant and maximal throughout the entire in vivo life of the administered 131I. The data revealed that neither of these assumptions held true (i.e. hNIS expression was not constant and maximal, but rather peaked at 2 days and declined rapidly). These findings are extremely important since they give a clear indication that, at least in the context of prostate cancer, current state-of-the-art radiovirotherapy will fail to achieve complete tumour responses because it does not deliver sufficient radiation dose (a curative course of external beam radiotherapy for prostate cancer involves the delivery of 70–84 Gy). Nonetheless, if this relatively modest virally delivered radiation dose (7–15 Gy) were to be used as a therapeutic boost in the context of a highly active oncolytic virus delivered during standard external beam irradiation with radiosensitising drug therapy, it might make a significant contribution to the overall treatment effect. This approach is discussed in greater detail in the section on combining radiovirotherapy with conventional therapeutics (see below).
In a follow-up publication, Rajecki et al. treated a single patient with chemotherapy refractory cervical cancer with direct intralesional injection of oncolytic Ad5/3-Δ24-hNIS adenovirus (Rajecki et al. 2011). Despite attempting to image with 123I and 99mTcO4 −, the authors were unable to detect gene expression and hypothesised that this might have been due to differences in vector design between Ad5-yCD/TK-hNIS and Ad5/3-Δ24-hNIS. They suggested that NIS gene expression might be optimised by using viruses of relatively low oncolytic potency with slower replication kinetics in which the NIS transgene is under the control of a ubiquitous exogenous promoter (e.g. CMV promoter) rather than an endogenous adenoviral promoter.
A recombinant NIS-expressing Edmonston strain measles virus (MV-NIS) has also been shown to have significant potential both as an in vivo imaging tool and as a therapeutic agent in combination with 131I (Dingli et al. 2004). An initial preclinical model of multiple myeloma demonstrated that MV-NIS was capable of mediating concentration of 123I such that intratumoral spread of the virus could be imaged by serial gamma camera imaging. In therapy experiments, when MV-NIS was combined with 131I, it was able to cause complete regressions of MM1 xenografts (which were resistant to virus therapy in the absence of radioisotope) (Dingli et al. 2004). Subsequent studies demonstrated that MV-NIS was active in mice bearing intraperitoneal SKOV3 ovarian cancer (Hasegawa et al. 2006) and subcutaneous BxPC-3 pancreatic cancer xenograft tumours (Carlson et al. 2006, 2009). In the first of these studies, the authors engineered measles virus to express carcinoembryonic antigen (CEA) and were able to use CEA levels in the blood as a surrogate marker of viral propagation. Further studies in prostate cancer models confirmed the ability of MV-NIS to mediate gene expression and therapeutic activity both in vitro and in vivo. MV-NIS showed single-agent activity which was enhanced by the addition of therapeutic radioisotope (131I). Importantly, systemically administered virus showed activity in these models (Msaouel et al. 2009). Additional studies have shown that MV-NIS may also be a candidate for development in the context of malignant glioma, medulloblastoma, anaplastic thyroid cancer and head and neck cancer (Allen et al. 2013; Hutzen et al. 2012; Reddi et al. 2012; Li et al. 2012). The promising nature of these studies has led to instigation of phase I clinical trials of MV-NIS in patients with a range of tumour types (Penheiter et al. 2010).
5 Choice of Radioisotope for Radiovirotherapy
Adenoviruses, MV, vesicular stomatitis viruses (VSV), vaccinia viruses and baculoviruses have all been engineered to encode the NIS gene. Different research teams have evaluated therapies combining viral and iodide-131 injections. Most studies have confirmed that combinations of NIS-expressing virotherapy and radioisotope delivery yield better antitumoral effects than viral injections alone in a range of models (Faivre et al. 2004; Peerlinck et al. 2009; Penheiter et al. 2010; Chen et al. 2007; Dwyer et al. 2006b; Herve et al. 2008; Hakkarainen et al. 2009).
Iodine-131 is the most commonly used radioisotope in preclinical studies, but other isotopes have also been investigated. Rhenium-188 is a high-energy β emitter with a 4 mm path length. Its half-life of 17 h, compared with 8 days for iodide-131, allows the delivery of high doses of radiation in relatively short periods of time. In a model of glioblastoma encoding NIS, rhenium-188 had a better effect on survival than iodide-131 therapy. In an in vivo model of prostatic cancer (LNCaP cells expressing NIS), rhenium-188 and iodide-131 therapies had similar therapeutic effects on small tumours, but rhenium-188 was superior in large tumours measuring more than 200 mm3 (Willhauck et al. 2007). Astatine-211 is an α-particle emitter that delivers high-energy α-particles (6.8 MeV) over a very short distance (less than 70 mm) (Supiot et al. 2007). Astatine-211 may, therefore, be particularly advantageous for the treatment of small tumours. In a subcutaneous model of K1-NIS tumours (thyroid cells expressing NIS), intraperitoneal injections of astatine-211 led to a complete tumour regressions (Petrich et al. 2006). An antitumoral effect has also been demonstrated in NIS-expressing prostate cancer models (Willhauck et al. 2008c). However, the use of astatine-211 is currently limited by its low availability for clinical use.
6 Combining Radiovirotherapy with Conventional Therapeutics
Conventional cancer treatments may improve the efficacy of radiovirotherapy (and vice versa). Combinations of viral therapies and external beam radiotherapy have been tested in several clinical trials (Touchefeu et al. 2011). Many studies have reported that radiotherapy and viruses can exert synergistic antitumoral effects through a variety of different mechanisms. Viral therapies can enhance the cytotoxic effects of radiation and, in effect, act as radiosensitising agents. On the other hand, tumour irradiation can change the biological effects of virotherapy. Thus, depending on the specific virus and tumour models selected, radiotherapy can increase viral infection/uptake, replication, gene expression and cytotoxicity (Touchefeu et al. 2011). In the specific case of NIS gene therapy, radiotherapy was shown to increase gene expression in a range of cell lines infected with a replication-deficient adenovirus encoding NIS (Hingorani et al. 2008a). For tumours that are treated by radiotherapy with curative intent, radiovirotherapy could represent a means of selectively increasing the total radiation dose that can be delivered. The radiobiological relationship between radiation dose and tumour control is well established for many solid cancers (Harrington and Nutting 2002), but attempts to improve clinical outcomes by escalating the doses of radiotherapy delivered by conventional means have been limited by the occurrence of radiation-induced toxicity in normal tissues. As an example, in the treatment of prostate cancer, a dose escalation from 64 Gy to 74 Gy significantly increased the biochemical progression-free survival, but was associated with increased toxicity (Dearnaley et al. 2007; Syndikus et al. 2010). In the studies reported by Barton et al. (2008, 2011) in which patients with prostate cancer received intraprostatic injections of NIS-expressing replication-competent oncolytic adenovirus, had the patients been treated with iodide-131, the estimated additional radiation dose that would have been delivered would have been 7.2 ± 4.8 Gy. Although this dose would be insufficient to exert single-agent efficacy, if delivered in the context of standard external beam radiotherapy, it might result in significant improvements in tumour control.
An alternative approach could involve the integration of existing or novel radiosensitising agents, such as DNA repair inhibitors, into combination regimens (Hingorani et al. 2008b, 2010b). Combinations of viral therapies with chemotherapy agents have also been investigated in vitro and in vivo and in a number of clinical trials. Alkylating agents (cyclophosphamide, cisplatin, temozolomide), microtubule stabilisers (paclitaxel and docetaxel), intercalating agents (doxorubicin) and mitomycin C have all shown synergistic antitumoral effects in different tumour models (Ottolino-Perry et al. 2010). More recently, the role of DNA repair inhibitors in the context of both replication-defective NIS-expressing adenovirus and oncolytic MV-NIS has been tested. In the latter study, the effect of combining a checkpoint kinase 1 inhibitor (SAR-020106) with MV-NIS, 131I and external beam radiotherapy was assessed (Touchefeu et al. 2013). Combining MV-NIS-driven radioiodide therapy with external beam radiotherapy and targeted inhibition of the DNA damage response was shown to be a promising therapeutic approach in models of head and neck and colorectal cancer. By adopting a stepwise, iterative approach to preclinical in vitro testing, it was shown that single-agent MV-NIS therapy mediated a potent antitumoral effect, especially at relatively high MOIs or later time points. Combining MV-NIS with EBRT achieved an additive or synergistic effect in short-term cytotoxicity and longer-term clonogenic assays. Other doublet combinations also exerted synergistic (or statistically significant) activities. Thus, the combination of MV-NIS and Chk1 inhibition was superior to MV-NIS or Chk1 inhibition alone in head and neck (HN5) and colorectal (HCT116) cells. As expected, combined Chk1 inhibition and external beam radiotherapy were synergistic or additive at all radiation dose levels in all cell lines. Similarly, combined MV-NIS and 131I were active in all cancer cell lines. It was subsequently shown that the triplet combination of MV-NIS, radioiodide and Chk1 inhibition was active in HCT116 cells. However, detailed analysis of the effects of the entire combination regimen—MV-NIS, 131I, EBRT and Chk1 inhibition—required in vivo analyses due to very high levels of cytotoxicity in in vitro analyses. Initially, studies confirmed the in vivo activity of the triplet combination of virus, Chk1 inhibition and EBRT in HN5 xenografts—indeed, the level of activity precluded using this model to test the quadruplet combination. In contrast, in HCT116 xenografts, the triplet combination was active, but with scope for improvement by adding radioiodide. Subsequently, it was confirmed that the addition of 131I to the combination regimen significantly increased its efficacy such that survival rates at study termination exceeded 80 %. Therefore, it would appear that this might represent a promising approach for clinical translation.
An alternative, or potentially complementary, approach may involve the use of targeted agents that exert direct anticancer effects and which also have the potential to modulate the expression and biological activity of hNIS. This approach has been assessed in the context of thyroid cancer that has become refractory to radioiodide therapy (through downregulation of NIS expression/activity) and has largely focused on the use of lithium or retinoic acid derivatives (Coelho et al. 2004; Handkiewicz-Junak et al. 2009; Simon et al. 2002; Liu et al. 2006). In general, these attempts to restore radioiodide uptake to potentially therapeutic levels have been unsuccessful and have not, thus far, yielded therapeutic benefits for patients with thyroid cancer. However, a recent report using a targeted agent that inhibits signalling in the mitogen-activated protein kinase (MAPK) pathway has provided clear evidence that this approach may be worth pursuing (Ho et al. 2013). The scientific rationale of using MAPK inhibition to increase NIS expression/activity is based on data showing that MAPK signalling exerts an inhibitory effect on NIS expression. In that study, a selective, allosteric MEK1 and MEK2 inhibitor selumetinib (AZD6244, ARRY-142886) was given to patients with radioiodide-refractory differentiated thyroid cancer, and the effect on NIS activity was measured by repeated 124I positron-emission tomography. A total of 20 patients were evaluable, and selumetinib was shown to increase 124I radioiodide uptake in 12 patients. Importantly, a link to the MAPK pathway was confirmed by the fact that selumetinib was effective in four of nine patients with BRAF mutations and five of five patients with NRAS mutations. As yet, this approach has not been tested as an adjuvant to virally mediated NIS gene expression, but it would appear that this may present a promising approach to optimising NIS expression, radioiodide uptake and, ultimately, therapeutic gain.
7 Conclusions
Radiovirotherapy is an innovative approach that aims to deliver a radioisotopic treatment selectively to tumours. Initial attempts to exploit replication-defective viral vectors to deliver NIS have more recently given way to the development and clinical translation of replication-competent oncolytic viruses that can serve this function. This field is rapidly evolving with a number of potential avenues for improving therapeutic efficacy. These include the use of imaging to guide the timing of treatment, the application of non-iodide radioisotopes (rhenium-188, astatine-211), innovations in viral vector design and the combination of NIS radioisotopic therapy with standard anti-cancer treatments. Given this breadth of opportunities, it is to be hoped that effective clinical translation of NIS-mediated radiovirotherapy will soon be achieved.
References
Ajjan RA, Kamaruddin NA, Crisp M, Watson PF, Ludgate M, Weetman AP (1998) Regulation and tissue distribution of the human sodium iodide symporter gene. Clin Endocrinol (Oxf) 49:517–523
Allen C, Opyrchal M, Aderca I, Schroeder MA, Sarkaria JN, Domingo E et al (2013) Oncolytic measles virus strains have significant antitumor activity against glioma stem cells. Gene Ther 20:444–449
Barton KN, Stricker H, Brown SL, Elshaikh M, Aref I, Lu M et al (2008) Phase I study of noninvasive imaging of adenovirus-mediated gene expression in the human prostate. Mol Ther 16:1761–1769
Barton KN, Stricker H, Elshaikh MA, Pegg J, Cheng J, Zhang Y et al (2011) Feasibility of adenovirus-mediated hNIS gene transfer and 131I radioiodine therapy as a definitive treatment for localized prostate cancer. Mol Ther 19:1353–1359
Boelaert K, Smith VE, Stratford AL, Kogai T, Tannahill LA, Watkinson JC et al (2007) PTTG and PBF repress the human sodium iodide symporter. Oncogene 26:4344–4356
Boland A, Ricard M, Opolon P, Bidart JM, Yeh P, Filetti S et al (2000) Adenovirus-mediated transfer of the thyroid sodium/iodide symporter gene into tumors for a targeted radiotherapy. Cancer Res 60:3484–3492
Caraccio N, Giannini R, Cuccato S, Faviana P, Berti P, Galleri D et al (2005) Type I interferons modulate the expression of thyroid peroxidase, sodium/iodide symporter, and thyroglobulin genes in primary human thyrocyte cultures. J Clin Endocrinol Metab 90:1156–1162
Carlson SK, Classic KL, Hadac EM, Bender CE, Kemp BJ, Lowe VJ et al (2006) In vivo quantitation of intratumoral radioisotope uptake using micro-single photon emission computed tomography/computed tomography. Mol Imaging Biol 8:324–332
Carlson SK, Classic KL, Hadac EM, Dingli D, Bender CE, Kemp BJ et al (2009) Quantitative molecular imaging of viral therapy for pancreatic cancer using an engineered measles virus expressing the sodium-iodide symporter reporter gene. AJR Am J Roentgenol 192:279–287
Cengic N, Baker CH, Schütz M, Göke B, Morris JC, Spitzweg C (2005) A novel therapeutic strategy for medullary thyroid cancer based on radioiodine therapy following tissue-specific sodium iodide symporter gene expression. J Clin Endocrinol Metab 90:4457–4464
Chen RF, Li ZH, Pan QH, Zhou JJ, Tang QB, Yu FY et al (2007) In vivo radioiodide imaging and treatment of pancreatic cancer xenografts after MUC1 promoter-driven expression of the human sodium-iodide symporter. Pancreatology 7:505–513
Cho J-Y, Xing S, Liu X, Buckwalter TL, Hwa L, Sferra TJ et al (2000) Expression and activity of human Na1/I2 symporter in human glioma cells by adenovirus-mediated gene delivery. Gene Ther 7:740–749
Coelho SM, Corbo R, Buescu A, Carvalho DP, Vaisman M (2004) Retinoic acid in patients with radioiodine non-responsive thyroid carcinoma. J Endocrinol Invest 27:334–339
Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ et al (2009) Revised American thyroid association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
Dearnaley DP, Sydes MR, Graham JD, Aird EG, Bottomley D, Cowan RA et al (2007) Escalated-dose versus standard-dose conformal radiotherapy in prostate cancer: first results from the MRC RT01 randomised controlled trial. Lancet Oncol 8:475–487
Dingli D, Peng KW, Harvey ME, Greipp PR, O’Connor MK, Cattaneo R et al (2004) Image-guided radiovirotherapy for multiple myeloma using a recombinant measles virus expressing the thyroidal sodium iodide symporter. Blood 103:1641–1646
Dwyer RM, Bergert ER, O’Connor MK, Gendler SJ, Morris JC (2005a) In vivo radioiodide imaging and treatment of breast cancer xenografts after MUC1-driven expression of the sodium iodide symporter. Clin Cancer Res 11:1483–1489
Dwyer RM, Schatz SM, Bergert ER, Myers RM, Harvey ME, Classic KL et al (2005b) A preclinical large animal model of adenovirus-mediated expression of the sodium-iodide symporter for radioiodide imaging and therapy of locally recurrent prostate cancer. Mol Ther 12:835–841
Dwyer RM, Bergert ER, O’Connor MK, Gendler SJ, Morris JC (2006a) Sodium iodide symporter-mediated radioiodide imaging and therapy of ovarian tumor xenografts in mice. Gene Ther 13:60–66
Dwyer RM, Bergert ER, O’Connor MK, Gendler SJ, Morris JC (2006b) Adenovirus-mediated and targeted expression of the sodium-iodide symporter permits in vivo radioiodide imaging and therapy of pancreatic tumors. Hum Gene Ther 17:661–668
Faivre J, Clerc J, Gérolami R, Hervé J, Longuet M, Liu B et al (2004) Long-term radioiodine retention and regression of liver cancer after sodium iodide symporter gene transfer in wistar rats. Cancer Res 64:8045–8051
Gaut AW, Niu G, Krager KJ, Graham MM, Trask DK, Domann FE (2004) Genetically targeted radiotherapy of head and neck squamous cell carcinoma using the sodium-iodide symporter (NIS). Head Neck 26:265–271
Hakkarainen T, Rajecki M, Sarparanta M, Tenhunen M, Airaksinen AJ, Desmond RA et al (2009) Targeted radiotherapy for prostate cancer with an oncolytic adenovirus coding for human sodium iodide symporter. Clin Cancer Res 15:5396–5403
Handkiewicz-Junak D, Roskosz J, Hasse-Lazar K, Szpak-Ulczok S, Puch Z, Kukulska A et al (2009) 13-cis-retinoic acid re-differentiation therapy and recombinant human thyrotropin-aided radioiodine treatment of non-functional metastatic thyroid cancer: a single-center, 53-patient phase 2 study. Thyroid Res 2:8
Harrington KJ, Nutting CM (2002) Interactions between ionizing radiation and drugs in head and neck cancer: how can we maximize the therapeutic index? Curr Opin Investig Drugs 3:807–811
Harrington KJ, Vile RG, Melcher A, Chester J, Pandha HS (2010) Clinical trials with oncolytic reovirus: moving beyond phase I into combinations with standard therapeutics. Cytokine Growth Factor Rev 21:91–98
Hasegawa K, Pham L, O’Connor MK, Federspiel MJ, Russell SJ, Peng KW (2006) Dual therapy of ovarian cancer using measles viruses expressing carcinoembryonic antigen and sodium iodide symporter. Clin Cancer Res 12:1868–1875
Herve J, Cunha AS, Liu B, Valogne Y, Longuet M, Boisgard R et al (2008) Internal radiotherapy of liver cancer with rat hepatocarcinoma-intestine-pancreas gene as a liver tumor-specific promoter. Hum Gene Ther 19:915–926
Hingorani M, White CL, Zaidi S, Merron A, Peerlinck I, Gore ME et al (2008a) Radiation-mediated up-regulation of gene expression from replication-defective adenoviral vectors: implications for sodium iodide symporter gene therapy. Clin Cancer Res 14(15):4915–4924, Epub 2008/08/05
Hingorani M, White CL, Merron A, Peerlinck I, Gore ME, Slade A et al (2008b) Inhibition of repair of radiation-induced DNA damage enhances gene expression from replication-defective adenoviral vectors. Cancer Res 68:9771–9778
Hingorani M, Spitzweg C, Vassaux G, Newbold K, Melcher A, Pandha H et al (2010a) The biology of the sodium iodide symporter and its potential for targeted gene delivery. Curr Cancer Drug Targets 10:242–267
Hingorani M, White CL, Zaidi S, Pandha HS, Melcher AA, Bhide SA et al (2010b) Therapeutic effect of sodium iodide symporter gene therapy combined with external beam radiotherapy and targeted drugs that inhibit DNA repair. Mol Ther 18:1599–1605
Ho AL, Grewal RK, Leboeuf R, Sherman EJ, Pfister DG, Deandreis D et al (2013) Selumetinib-enhanced radioiodine uptake in advanced thyroid cancer. N Engl J Med 368:623–632
Hutzen B, Pierson CR, Russell SJ, Galanis E, Raffel C, Studebaker AW (2012) Treatment of medulloblastoma using an oncolytic measles virus encoding the thyroidal sodium iodide symporter shows enhanced efficacy with radioiodine. BMC Cancer 12:508
Jung H (2002) The sodium/substrate symporter family: structural and functional features. FEBS Lett 529:73–77
Kakinuma H, Bergert ER, Spitzweg C, Cheville JC, Lieber MM, Morris JC (2003) Probasin promoter (ARR(2)PB)-driven, prostate-specific expression of the human sodium iodide symporter (h-NIS) for targeted radioiodine therapy of prostate cancer. Cancer Res 63:7840–7844
Kogai T, Curcio F, Hyman S, Cornford EM, Brent GA, Hershman JM (2000) Induction of follicle formation in long-term cultured normal human thyroid cells treated with thyrotropin stimulates iodide uptake but not sodium/iodide symporter messenger RNA and protein expression. J Endocrinol 167:125–135
Kogai T, Taki K, Brent GA (2006) Enhancement of sodium/iodide symporter expression in thyroid and breast cancer. Endocr Relat Cancer 13:797–826
Li H, Peng KW, Russell SJ (2012) Oncolytic measles virus encoding thyroidal sodium iodide symporter for squamous cell cancer of the head and neck radiovirotherapy. Hum Gene Ther 23:295–301
Liu YY, van der Pluijm G, Karperien M, Stokkel MP, Pereira AM, Morreau J et al (2006) Lithium as adjuvant to radioiodine therapy in differentiated thyroid carcinoma: clinical and in vitro studies. Clin Endocrinol (Oxf) 64:617–624
Mandell RB, Mandell LZ, Link CJ (1999) Radioisotope concentrator gene therapy using the sodium/iodide symporter gene. Cancer Res 59:661–668
Massart C, Corbineau E (2006) Transporteurs d’iodures et fonction thyroïdienne. Immuno-analyse and Biologie Spécialisée 21:138–143
Merron A, Peerlinck I, Martin-Duque P, Burnet J, Quintanilla M, Mather S et al (2007) SPECT/CT imaging of oncolytic adenovirus propagation in tumours in vivo using the Na/I symporter as a reporter gene. Gene Ther 14:1731–1738
Msaouel P, Iankov ID, Allen C, Aderca I, Federspiel MJ, Tindall DJ et al (2009) Noninvasive imaging and radiovirotherapy of prostate cancer using an oncolytic measles virus expressing the sodium iodide symporter. Mol Ther 17:2041–2048
Ottolino-Perry K, Diallo JS, Lichty BD, Bell JC, McCart JA (2010) Intelligent design: combination therapy with oncolytic viruses. Mol Ther 18:251–263
Peerlinck I, Merron A, Baril P, Conchon S, Martin-Duque P, Hindorf C et al (2009) Targeted radionuclide therapy using a Wnt-targeted replicating adenovirus encoding the Na/I symporter. Clin Cancer Res 15:6595–6601
Penheiter AR, Wegman TR, Classic KL, Dingli D, Bender CE, Russell SJ et al (2010) Sodium iodide symporter (NIS)-mediated radiovirotherapy for pancreatic cancer. AJR Am J Roentgenol 195:341–349
Petrich T, Quintanilla-Martinez L, Korkmaz Z, Samson E, Helmeke HJ, Meyer GJ et al (2006) Effective cancer therapy with the alpha-particle emitter [211At]astatine in a mouse model of genetically modified sodium/iodide symporter-expressing tumors. Clin Cancer Res 12:1342–1348
Rajecki M, Kangasmäki A, Laasonen L, Escutenaire S, Hakkarainen T, Haukka J et al (2011) Sodium iodide symporter SPECT imaging of a patient treated with oncolytic adenovirus Ad5/3-Δ24-hNIS. Mol Ther 19:629–631
Reddi HV, Madde P, McDonough SJ, Trujillo MA, Morris JC III, Myers RM et al (2012) Preclinical efficacy of the oncolytic measles virus expressing the sodium iodide symporter in iodine non-avid anaplastic thyroid cancer: a novel therapeutic agent allowing noninvasive imaging and radioiodine therapy. Cancer Gene Ther 19:659–665
Riedel C, Levy O, Carrasco N (2001) Post-transcriptional regulation of the sodium/iodide symporter by thyrotropin. J Biol Chem 276:21458–21463
Riesco-Eizaguirre G, Santisteban P (2006) A perspective view of sodium iodide symporter research and its clinical implications. Eur J Endocrinol 155:495–512
Ross DS (2011) Radioiodine therapy for hyperthyroidism. N Engl J Med 364:542–550
Saez C, Martinez-Brocca MA, Castilla C, Soto A, Navarro E, Tortolero M et al (2006) Prognostic significance of human pituitary tumor-transforming gene immunohistochemical expression in differentiated thyroid cancer. J Clin Endocrinol Metab 91:1404–1409
Schipper ML, Weber A, Béhé M, Göke R, Joba W, Schmidt H, Bert T et al (2003) Radioiodide treatment after sodium iodide symporter gene transfer is a highly effective therapy in neuroendocrine tumor cells. Cancer Res 63:1333–1338
Scholz IV, Cengic N, Baker CH, Harrington KJ, Maletz K, Bergert ER et al (2005) Radioiodine therapy of colon cancer following tissue-specific sodium iodide symporter gene transfer. Gene Ther 12:272–280
Shimura H, Haraguchi K, Myazaki A, Endo T, Onaya T (1997) Iodide uptake and experimental 131I therapy in transplanted undifferentiated thyroid cancer cells expressing the Na+/I- symporter gene. Endocrinology 138:4493–4496
Sieger S, Jiang S, Schönsiegel F, Eskerski H, Kübler W, Altmann A et al (2003) Tumour-specific activation of the sodium/iodide symporter gene under control of the glucose transporter gene 1 promoter (GTI-1.3). Eur J Nucl Med Mol Imaging 30:748–756
Simon D, Körber C, Krausch M, Segering J, Groth P, Görges R et al (2002) Clinical impact of retinoids in redifferentiation therapy of advanced thyroid cancer: final results of a pilot study. Eur J Nucl Med Mol Imaging 29:775–782
Smanik PA, Liu Q, Furminger TL, Ryu K, Xing S, Mazzaferri EL et al (1996) Cloning of the human sodium iodide symporter. Biochem Biophys Res Commun 226:339–345
Spitzweg C, Joba W, Eisenmenger W, Heufelder AE (1998) Analysis of human sodium iodide symporter gene expression in extrathyroidal tissues and cloning of its complementary deoxyribonucleic acids from salivary gland, mammary gland, and gastric mucosa. J Clin Endocrinol Metab 83:1746–1751
Spitzweg C, Zhang S, Bergert ER, Castro MR, McIver B, Heufelder AE et al (1999) Prostate specific antigen (PSA) promoter-driven androgen-inducible expression of sodium iodide symporter in prostate cancer cell lines. Cancer Res 59:2136–2141
Spitzweg C, O’Connor MK, Bergert ER, Tindall DJ, Young CY, Morris JC (2000) Treatment of prostate cancer by radioiodine therapy after tissue-specific expression of the sodium iodide symporter. Cancer Res 15:6526–6530
Spitzweg C, Dutton CM, Castro MR, Bergert ER, Goellner JR, Heufelder AE et al (2001a) Expression of the sodium iodide symporter in human kidney. Kidney Int 59:1013–1023
Spitzweg C, Dietz AB, O’Connor MK, Bergert ER, Tindall DJ, Young CY et al (2001b) In vivo sodium iodide symporter gene therapy of prostate cancer. Gene Ther 8:1524–1531
Spitzweg C, Scholz IV, Bergert ER, Tindall DJ, Young CY, Goke B et al (2003) Retinoic acid-induced stimulation of sodium iodide symporter expression and cytotoxicity of radioiodine in prostate cancer cells. Endocrinology 144:3423–3432
Supiot s, Thillays F, Rio E, Mahe MA, Barbet FJ, Kraeber-Bodere F et al (2007) Le point sur les avancees recentes de la radio-immunotherapie alpha (Alpha-radioimmunotherapy: a review of recent developments). Cancer Radiother 11:252–259
Syndikus I, Morgan RC, Sydes MR, Graham JD, Dearnaley DP (2010) Late gastrointestinal toxicity after dose-escalated conformal radiotherapy for early prostate cancer: results from the UK Medical Research Council RT01 trial (ISRCTN47772397). Int J Radiat Oncol Biol Phys 77:773–783
Taki K, Kogai T, Kanamoto Y, Hershman JM, Brent GA (2002) A thyroid-specific far-upstream enhancer in the human sodium/iodide symporter gene requires Pax-8 binding and cyclic adenosine 3′,5′-monophosphate response element-like sequence binding proteins for full activity and is differentially regulated in normal and thyroid cancer cells. Mol Endocrinol 16:2266–2282
Touchefeu Y, Vassaux G, Harrington KJ (2011) Oncolytic viruses in radiation oncology. Radiother Oncol 99:262–270
Touchefeu Y, Khan AA, Borst G, Zaidi SH, McLaughlin M, Roulstone V et al (2013) Optimising measles virus-guided radiovirotherapy with external beam radiotherapy and specific checkpoint kinase 1 inhibition. Radiother Oncol 108:24–31
Unterholzner S, Willhauck MJ, Cengic N, Schutz M, Goke B, Morris JC et al (2006) Dexamethasone stimulation of retinoic acid-induced sodium iodide symporter expression and cytotoxicity of 131-I in breast cancer cells. J Clin Endocrinol Metab 91:69–78
Vayre L, Sabourin JC, Caillou B, Ducreux M, Schlumberger M, Bidart JM (1999) Immunohistochemical analysis of Na+/I- symporter distribution in human extra-thyroidal tissues. Eur J Endocrinol 141:382–386
Willhauck MJ, Sharif Samani BR, Gildehaus FJ, Wolf I, Senekowitsch-Schmidtke R, Stark HJ et al (2007) Application of 188rhenium as an alternative radionuclide for treatment of prostate cancer after tumor-specific sodium iodide symporter gene expression. J Clin Endocrinol Metab 92:4451–4458
Willhauck MJ, Sharif-Samani B, Senekowitsch-Schmidtke R, Wunderlich N, Goke B, Morris JC et al (2008a) Functional sodium iodide symporter expression in breast cancer xenografts in vivo after systemic treatment with retinoic acid and dexamethasone. Breast Cancer Res Treat 109:263–272
Willhauck MJ, Sharif Samani BR, Klutz K, Cengic N, Wolf I, Mohr L et al (2008b) Alpha-fetoprotein promoter-targeted sodium iodide symporter gene therapy of hepatocellular carcinoma. Gene Ther 15:214–223
Willhauck MJ, Samani BR, Wolf I, Senekowitsch-Schmidtke R, Stark HJ, Meyer GJ et al (2008c) The potential of 211Astatine for NIS-mediated radionuclide therapy in prostate cancer. Eur J Nucl Med Mol Imaging 35:1272–1281
Willhauck MJ, O Kane DJ, Wunderlich N, Goke B, Spitzweg C (2011) Stimulation of retinoic acid-induced functional sodium iodide symporter (NIS) expression and cytotoxicity of 131I by carbamazepine in breast cancer cells. Breast Cancer Res Treat 125:377–386
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag Wien
About this chapter
Cite this chapter
Harrington, K.J. (2014). Radiovirotherapy for the Treatment of Cancer. In: Lukashevich, I., Shirwan, H. (eds) Novel Technologies for Vaccine Development. Springer, Vienna. https://doi.org/10.1007/978-3-7091-1818-4_9
Download citation
DOI: https://doi.org/10.1007/978-3-7091-1818-4_9
Published:
Publisher Name: Springer, Vienna
Print ISBN: 978-3-7091-1817-7
Online ISBN: 978-3-7091-1818-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)