Abstract
The incidence of meniscal cyst is low. In case of symptomatic meniscal cysts, MRI is recommended in order to evaluate both the cyst and the adjacent meniscus. Asymptomatic meniscal cyst does not require treatment. The injection of steroids into the cyst should not be recommended, because it is rather an interim treatment and shows a high failure rate.
Symptomatic meniscal cysts require arthroscopy for treatment of the meniscal pathology, but preservation of the meniscus should be the primary aim. Drainage of the cyst, which can be done arthroscopically or by open resection, is obligatory in addition.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
A cyst is defined as a cavum filled with fluid and coated from inside with a monolayer of cells. The meniscal cyst is located close to the meniscus’ periphery and most commonly associated with a horizontal meniscal lesion. Fibroblasts coat the cavum of the meniscal cyst surrounded by a thick layer of fibrous tissue (Fig. 24.1a, b). The Alcian-blue staining shows an increase of hyaluronic acid within the capsule.
Cysts around the knee are localized either intra-articular or extra-articular. Intra-articular cysts can arise from the anterior cruciate ligament [20, 63], posterior cruciate ligament [19, 37], infrapatellar fat pad [2], or transverse meniscal ligament [42]. Intra-articular cysts are rare with an incidence of 1 % [32]. Most of the intra-articular cysts are clinically asymptomatic. Kurdwig et al. reported that 76 out of 85 intra-articular soft tissue masses are asymptomatic and incidentally diagnosed. The prevalence and the size of asymptomatic meniscal cysts were studied in 102 asymptomatic knees [59]. Subjects with a mean age of 42.8 years (18–72 years) received magnetic resonance imaging (MRI) examination. Four medial meniscal cysts were found and showed an average size of 9 mm × 6 mm × 13 mm. The maximal diameter was less than 16 mm. No lateral meniscal cyst was identified in the study. Nineteen synovial cysts were diagnosed in the popliteal space.
Parameniscal cysts are most commonly located at the level of the medial or lateral joint line caused due to the strong association to the meniscus. Extra-articular cyst can also arise from the posterolateral capsule without having contact to the meniscus [24].
2 Etiology and Pathology of Meniscal Cysts
Two main theories about the meniscal cysts formation have been proposed. One theory suggests that synovial cells are displaced into the meniscus and produce mucin resulting in a cyst formation (Fig. 24.2) [56].
The mechanism might be induced due to abnormal stress or trauma on a meniscus [4]. Some studies report about a proportion of up to 50 % of traumatic genesis [27, 36].
A myxoid degenerative process has been identified histologically [6, 34]. The yellow color of the meniscal tissue frequently seen during arthroscopy is caused by the myxoid degeneration [21].
Figure 24.3 shows an arthroscopic view of the intermediate and posterior zone of the medial meniscus with central myxoid degeneration of the tissue.
In some studies, a cyst-lesion relationship of up to 100 % of the cases has been reported [25, 50]. However, there is no correlation between the size of the meniscal lesion and the size of the cyst. Large meniscal lesions may show very small cyst formation, and large cysts might be seen with small or no meniscal lesions [48].
The second theory presumes that the cyst formation occurs due to extrusion of the synovial fluid through the torn meniscal tissue [4, 21, 31, 60]. Cystic degeneration of the meniscus may cause either enlargement of the meniscus’ periphery (i.e., intrameniscal cyst) or extrusion into the parameniscal tissue (i.e., parameniscal cyst) [16]. Signal characteristics of the fluid in MRI within the meniscal cysts had shown comparable intensity to the synovial fluid in over 96 % of the cases [3]. The second theory might be more likely due to the fact that, in 98 % or higher, meniscal cysts are associated with horizontal meniscal lesions [9, 25, 27, 60]. However, it has been reported that the meniscal lesion does not need to reach the articular surface (Grade-III lesion) [3, 6]. This goes in line with the theory by Reagan et al. [48]. He presumes an initial meniscal lesion within the meniscal substance as classified by Stoller [57]. The lesion may progress either to the meniscus’ periphery or to the inner circumference. In case the meniscal lesion progresses to the periphery, cyst formation may occur without presenting a Grade-III meniscal lesion.
Meniscal cysts can be classified as parameniscal, intrameniscal, or a combination of both. One may presume that cyst formation starts within the meniscal tissue as a result of degeneration followed by the expression into the parameniscal tissue. A high percentage of cysts are missing because they are asymptomatic at the early stage especially prior any extrusion. When cysts increase in size and extrude, they may become symptomatic. A critical size of 12 mm of the meniscal lesion has been considered for the formation of parameniscal cysts [62].
The extension of the medial and lateral parameniscal cysts was studied according to MRI [16]. Three layers are distinguished on the medial site of the knee: the crural fascia (layer I), superficial (layer II), and the deep layer of the medial collateral ligament (layer III). Histological studies showed that the medial meniscus is attached to the joint capsule but separated from the medial collateral ligament by loose connective tissue [54]. Thus, the cyst can easily enlarge into the connective tissue before extruded anterior or posterior from the medial collateral ligament. Medial meniscal cysts are predominantly located more at the posterior horn of the meniscus and less superficial [8, 51].
Lateral meniscal cysts are most frequently located in the midportion of the meniscus and show an extrusion either anteriorly (35 %) or posteriorly (66 %) [28].
3 Incidence of Meniscal Cysts
The incidence of meniscal cysts ranges between 1.8 and 20 % [3, 9, 17, 34, 47, 60] (Table 24.1). There are controversial findings regarding the location. Some authors report that meniscal cysts occur predominantly on the medial site and others on the lateral one.
Meniscal cysts are commonly found in young to middle-aged patients [27].
4 Clinical Evaluation and Diagnostic
The most common clinical sign seems to be the joint line tenderness especially under loading and sometimes in association with swelling at the level of the medial or lateral joint line (Fig. 24.4a, lateral; b, c, medial). Often these patients present a history of symptoms for months or years. The main symptom is pain. Effusion, locking, or giving way seems to be less common.
Lateral meniscal cysts are easier to diagnose by physical examination than medial ones because of their relatively anterior and more subcutaneous position. A mass might be palpable solid or fluctuant in consistence. The size of the cyst may change in regard to the degree of knee flexion. Usually, there is a connection between the cyst and the anterior horn of the meniscus. There is a potential risk that large lateral meniscal cysts may cause peroneal nerve palsy [30]. Patients presenting unexplained nerve palsy should receive an MRI of the knee and the proximal tibiofibular joint.
It has been reported that only 16 % of all medial or lateral meniscal cysts are palpable during physical examination [15]. However, parameniscal cysts are better palpable on the lateral site with 20–60 % than on the medial site with 6 % [9, 17].
The accuracy of the joint line fullness and joint line tenderness was studied in meniscal pathologies [13]. Joint line fullness did not correlate well with the presence of meniscal cysts and showed a very low predictive value of 29 % only. The accuracy, sensitivity, and specificity of the joint line fullness in detecting meniscal pathologies were 73 %, 70 %, and 82 %, respectively. The joint line tenderness showed an accuracy, sensitivity, and specificity of 68 %, 87 %, and 30 %, respectively. The finding goes in line with others [41]. The authors report about a mass palpation in 58 out of 636 cases at the level of the joint line having the knee at 45° of flexion. Thirty of these patients presented a cyst formation during arthroscopy only. However, no MRI was evaluated in the study and thus some cysts might be missed. The knee position of 45° of knee flexion is in contrast to what A. Pisani described [46]. He reported that the cysts become less prominent or even disappear at a knee flexion angle of 45° (Pisani’s sign).
Routine radiographs should include an anteroposterior weight-bearing and lateral view. The Rosenberg view is more sensitive than the anteroposterior view in the assessment of joint space narrowing and should be recommended [5]. The radiographies may look normal, but sometimes erosion at the tibial plateau or femoral condyle can be observed, due to increased pressure by the cyst [1, 58] (Fig. 24.5). Wang et al. have showed also that medial or lateral meniscal extrusion is associated with subchondral bone marrow lesions and bone cysts [61].
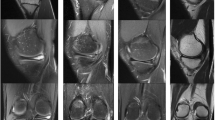
The diagnosis of meniscal cysts is nowadays mainly based on MRI (Fig. 24.6a–f). The appearance of meniscal cysts in MRI showed in 91 % meniscal cysts immediately adjacent to the meniscal lesion. Only 4 % of the cysts seem to be separated from the meniscus [60]. Magnetic resonance imaging (MRI) is the first diagnostic step to search for and assess the meniscal cysts (Fig. 24.6). The MRI is critical to define precisely the meniscal tear. This imaging exam allowed a meticulous exploration of the size, location, extension to the articular surface of the meniscus, and the communication between the cyst and the tear. MRI is very useful to locate the cyst and to search for associated intra-articular damage [63] (especially articular cartilage lesions) and differential diagnosis (cyst of the Hoffa ligaments (Fig. 24.7a) and cyst of the tibiofibular joint and its surgical excision (Fig. 24.7b, c) and preoperative planning).
MRI imaging. (a, b) MRI of the right knee. (a) Coronal plane (T2W-SPIRT), (b) axial plane (PSW-TSE-SP). The images show a large parameniscal cyst of the medial meniscus. (c) MRI T2 showing a medial meniscal cyst and the associated meniscal tear. (d–f) MRI T2 showing a lateral meniscal cyst and the associated meniscal tear
Some patients, such as patients with pacemaker, for instance, show contraindications for MRI examination. In these patients, ultrasound or CT-arthrography might be considered as a useful tool [12]. Ultrasound is an easy to perform and cheap technique, which might be used in diagnosing meniscal cysts (Fig. 24.8).
The sensitivity and specificity of detecting meniscal lesions with ultrasound has been reported of 70–80 % and use to be significantly lower in comparison to MRI [23, 53]. However, the more recently developed high-resolution ultrasonography (HRUS) shows significant higher sensitivity and specificity of 94–97 % and 86–100 %, respectively ([49, 55]).
Despite the fact that CT-arthrography provides a high sensitivity and specificity in detecting meniscal pathologies, it should not be considered for routine diagnostics due to the availability of MRI technology as a noninvasive tool and without any exposure to radiation [35]. The sensitivity and specificity for CT-arthrography of 91.7–100 % and 98.1 %, respectively, have been reported [35].
Differential diagnosis includes meniscal lesion without cyst, loose bodies, exostosis, bursal inflammation, ganglion, tendinitis, and tumor.
5 Treatment of Meniscal Cysts
Meniscal cysts can be treated conservatively or by surgery. Surgery should include both resection or repair of the meniscal lesion and removal or debridement of the meniscal cyst [48].
5.1 Conservative Treatment
Injection of steroids into the cyst [4] or ultrasound-guided percutaneous drainage might be an option for treating meniscal cysts nonsurgically [40]. The steroid injection may stop the inflammatory process and production of fluid and may induce fibrosis of the cyst and closure of the cavum. The injection of steroids lasts often for a short term of several weeks only [40]. Others had reported more promising results [38]. Ultrasound-guided percutaneous drainage of meniscal cysts was evaluated by MRI. Ten out of 18 patients (13 medial and 5 lateral) experienced complete relief of symptoms but 6 of them complained again after an initial pain-free period. Cyst aspiration may be considered in patients presenting contraindication for surgical treatment. Fluid aspiration causes reduction of swelling, but the cyst formation remains intact and a high risk of recurrence can be expected.
5.2 Surgical Treatment
Meniscal cysts formation occurs mainly in conjunction with meniscal lesions. Hulet et al. studied a series of 105 lateral meniscal cysts retrospectively and reported a prevalence of Grade-III meniscal lesions in 99 % of the patients [27]. Reagan [40] suggested that there are several stages to the development of lateral meniscal cysts and that a complete meniscal lesion depends on the stage of progression, in a given patient [48]. Among the different types of meniscal tears, the predominant form is a horizontal component presenting itself as a cleavage [11, 25, 39, 44] (Fig. 24.9a, b).
Glasgow reported 72 tears and described 30 simple horizontal cleavages, 23 oblique-horizontal cleavages, and 4 discoid menisci [25]. Hulet et al. found that a horizontal component (56 % horizontal cleavages and 10 complex lesions) accounted for 64 % of the cases [27]. The majority of these lesions were radial slits (44 %). Horizontal cleavage is the most frequently encountered tear in lateral meniscal cysts. Meniscal cysts are located in the midportion of the lateral meniscus with an extension to the anterior portion in 21 % of the cases. Concerning the medial meniscus, Saidi et al. reported 5 cases [52]. In these five cases, all the meniscal tears had developed from the posterior segment. In a retrospective MRI review, Campbell and Mitchell found a majority of medial meniscal cyst (n = 72) [9]. In this report, the meniscal tear was a horizontal cleavage in 90 % of cases, and the location of the medial meniscal cyst was adjacent to the posterior horn in 74 % of cases (Fig. 24.10a, b).
For that reason, arthroscopy should be performed in order to treat the meniscal pathology followed by resection or debridement of the cyst. There are different options in the management of the meniscal lesion.
Patients scheduled for meniscal surgery should receive MRI prior to surgery in order to diagnose the exact location and size of both the meniscal lesion and the cyst. The intra-articular pathology needs to be addressed in conjunction with the treatment of the cyst.
Horizontal meniscal lesions require partial or subtotal meniscus resection showing the myxoid degeneration (yellow substance) [14] (Fig. 24.11a, b). In addition, horizontal lesions with extension into the meniscal-synovial junction should receive vertical sutures in order to close the lesion (Fig. 24.12a, b). However, no clinical data are available yet, which have proven the novel concept.
Different techniques for arthroscopic surgery have been described [26, 29].
Standard arthroscopy portals should be used initially. Sometimes an inferomedial or inferolateral portal is required in addition for better visualization of either the medial or lateral compartment [18]. A spinal needle introduced percutaneously through the cystic mass may help to identify the sinus tract between cyst and meniscus (Fig. 24.13). A meniscal punch may be entered into the cyst in order to widen the sinus tract. Thus, the fluid of the cyst can be drained into the joint. Additionally, a small-motorized shaver may be introduced into the cyst, assisting in cystic decompression and stimulating inflammation and scarring of the cyst [33].
An arthroscopic technique has been described recently for lateral parameniscal cyst compression using a very superomedial portal at the most proximal part of the suprapatellar pouch, just medial to the quadriceps tendon [26].
Some surgeons recommend suturing the remnants of the sinus tract within the meniscus after partial meniscectomy, although it may not be necessary. Drainage of the cyst into the knee via the natural tract seems to be sufficient [33, 52]. Open resection could be performed when the cyst is too large.
Open resection of the cyst in addition to arthroscopy was compared with solely arthroscopic treatment of parameniscal cysts [52]. No difference in clinical outcome was reported. The isolated treatment of meniscal lesions by partial meniscus resection has shown inferior results. Good and excellent results have been reported in 50 % of the patients in comparison to a combined arthroscopic debridement and open resection procedure with 80 % of excellent results [48].
Special attention is required in multiple lobular cysts. A complete decompression can only be achieved with open surgery (Fig. 24.16).
A clinical and surgical algorithm for treatment of meniscal cysts is proposed when a symptomatic lateral meniscal cyst is suspected clinically (Fig. 24.14).
MRI is the first diagnostic step to search a meniscal tear. If a meniscal cyst is suspected clinically, an MRI is the diagnostic test of choice. The MRI is critical in identifying additional diagnoses and to precisely delineate the lateral meniscal tear (size, location, extension to the articular surface of the meniscus, communication with the cyst) and the cyst.
If the tear was clearly opened into the joint, arthroscopy is first performed to characterize the meniscal tear (Fig. 24.15).
In the case of a smaller tear, cystectomy should be performed (most often with open technique); then the repair suture technique should be tried to preserve the meniscal tissue. In the case of important and complex tears, arthroscopic partial meniscectomy and cyst decompression were indicated.
If the tear was not opened into the joint, an arthroscopy should be performed with diligent search on both menisci surfaces of a meniscal tear, followed by an open cystectomy and meniscal suture laterally to medially.
Depending on the location of the tear, the cyst could be decompressed arthroscopically for the anterior horn. In all cases, meniscal tissue preservation should be attempted to preserve the knee biomechanics. The meniscal tear is usually a primary lesion and results from a degenerative breakdown of the ultrastructure of the meniscal collagen.
6 Results
Good and excellent outcome has been reported in up to 85 % for the medial meniscus in numerous studies [22, 25, 27, 39, 40, 43, 45, 48]. Similar results are also reported for the lateral meniscus, showing clearly that functional outcome is related to the meniscal lesion and not the presence of a cyst [5]. The patients with lateral meniscal cysts treated by arthroscopic resection were clinically followed up after 5 years [27]. The recurrence rate was 10.5 % (11 patients). The author also reported that 77 % of the active patients returned to their previous level of activity and 16 % showed lower performance. Ninety-one out of 104 patients received arthroscopic resection, and 14 patients had open surgery.
Biedert [7] had encouraged this management in a randomized clinical trial of treatment of intra-substance meniscal lesion of the medial meniscus. Forty patients of 31 years of age were included and they all had horizontal Grade-II meniscal lesions.
The same surgeon performed four treatments: conservative treatment (75 % nearly normal or normal at final evaluation), arthroscopic suture repair with access channels (90 % nearly normal or normal at final evaluation), arthroscopic minimal central resection (43 % nearly normal or normal at final evaluation), and suture and arthroscopic partial meniscectomy (100 % nearly normal or normal at final evaluation).
A recurrent rate of cysts formation has been reported ranging between 9.5 and 15.6 % [39, 48]. Early revision arthroscopy is likely when insufficient meniscus resection has been performed. Late revision arthroscopy in contrast is rather caused due to progression in meniscus degeneration. Revision surgery showed no effect on the final outcome. The incidence of osteoarthritis was 9 % at an average of 5 years of follow-up. The amount of meniscus resection seems to correlate directly with the development of osteoarthritis [10]. The 10-year follow-up of 98 patients showed a much higher incidence of osteoarthritis of 38 % [28]. Arthroscopic suture repair is an effective alternative to meniscectomy to prevent the development of osteoarthritis of the knee joint. The number of cases treated in this way, with their follow-up periods, is still insufficient.
7 Conclusion
The incidence of meniscal cyst is low. Meniscal cyst is a particular entity in meniscal pathology. When a symptomatic meniscal cyst is suspected clinically, magnetic resonance imaging (MRI) is the first diagnostic step to explore the meniscal tear. Asymptomatic meniscal cyst should be treated conservatively. Data reported in the literature suggest the following management protocol for patients with a symptomatic meniscal cyst based on careful examination of the surfaces of the menisci during arthroscopy. In all cases, meniscal tissue preservation should be the rule for the future of the knee. As seen in the long-term results following lateral or medial meniscectomy, attempts to preserve the meniscus are clearly justified. The meniscal tear is usually a primary lesion and results from a degenerative breakdown of the ultrastructure of the meniscal collagen with myxoid degeneration. Ultimately, one essential question remains: whether or not a meniscus undergoing myxoid degeneration is likely to function properly or, more likely, to progressively fail because of repetitive shear forces concentrated centrally. Nevertheless, a meniscus that is functioning at some level is still preferable to no meniscus (Fig. 24.16).
References
Al-Khateeb H, Ruiz A (2006) Lateral meniscal cyst producing lesion of the tibial plateau and literature review. Int J Surg. doi:10.1016/j.ijsu.2006.05.004
Amin M, Torreggiani W, Sparkes J (2008) Infrapatellar ganglion that developed from infrapatellar fat and had minimal intraarticular extension. Knee Surg Sports Traumatol Arthrosc 16:179–181
Anderson JJ, Connor GF, Helms CA (2010) New observations on meniscal cysts. Skeletal Radiol 39:1187–1191
Barrie HJ (1979) The pathogenesis and significance of meniscal cysts. J Bone Joint Surg Br 61-B:184–189
Beaufils P, Hardy P, Clavert P, Djian P, Frank A, Hulet C, Potel JF, Verdonk R, et al, SFA (2006) Adult lateral meniscus. Rev chir Orthop Reparatrice Appar Mot 92:2S169–2S194
Bhatti A, Iqbal MJ (2006) Pericruciate intra-articular lateral meniscal cyst without meniscal tear. Knee Surg Sports Traumatol Arthrosc 14:869–871
Biedert RM (2000) Treatment of intrasubstance meniscal lesions: a randomized prospective study of four different methods. Knee Surg Sports Traumatol Arthrosc 8:104–108
Campbell WC, Mitchell JI (1929) Semilunar cartilage cysts. Am J Surg 6:330–336
Campbell SE, Sanders TG, Morrison WB (2001) MR imaging of meniscal cysts: incidence, location, and clinical significance. AJR Am J Roentgenol 177:409–413
Chambat P, Neyret P, et al, SFA (1996) Méniscectomies sous arthroscopie à plus de 10 ans sur un genou stable sans antécédents chirurgicaux. Ann Soc Française Arthrosc 6:93–153
Chassaing V, Parier J, Artigala P (1985) L’arthroscopie opératoire dans le traitement du kyste du ménisque externe. J Med Lyon 66:449–453
Chen H (2015) Diagnosis and treatment of a lateral meniscal cyst with musculoskeletal ultrasound. Case Rep Orthop. 2015:432187 dx. doi.org/10.1155/2015/432187
Couture JF, Al-Juhani W, Forsythe ME, Lenczner E, Marien R, Burman M (2012) Joint line fullness and meniscal pathology. Sports Health 4:47–50
Cowden CH, Barber FA (2014) Meniscal cysts: treatment options and algorithm. J Knee Surg 27:105–111
Crowell MS, Westrick RB, Fogarty BT (2013) Cysts of the lateral meniscus. Int J Sports Phys Ther 8:340–348
De Maeseneer M, Shahabpour M, Vanderdood K, Machiels F, De Ridder F, Osteaux M (2001) MR imaging of meniscal cysts: evaluation of location and extension using a three-layer approach. Eur J Radiol 39:117–124
De Smet AA, Graf BK, del Rio AM (2011) Association of parameniscal cysts with underlying meniscal tears as identified on MRI and arthroscopy. AJR Am J Roentgenol 196:W180–W186
Dougados M, Ayral X, Listrat V, Gueuguen A, Bahuaud J (1994) The SFA system for assessing articular cartilage lesions at arthroscopy of the knee. Arthroscopy 10:69
Durante JA (2009) Ganglion cyst on the posterior cruciate ligament: a case report. JCCA J Can Chiropr Assoc 53:334–338
England E, Wissman RD, Mehta K, Burch M, Kaiser A, Li T (2015) Cysts of the anterior horn lateral meniscus and the ACL: is there a relationship? Skeletal Radiol 44:369–373
Ferrer-Roca O, Vilalta C (1980) Lesions of the meniscus. Part II: Horizontal cleavages and lateral cysts. Clin Orthop Relat Res 146:301–307
Flynn M, Kelly JP (1976) Local excision of cyst of lateral meniscus of knee without recurrence. J Bone Joint Surg Br 58:88–89
Friedl W, Glaser F (1991) Dynamic sonography in the diagnosis of ligament and meniscal injuries of the knee. Arch Orthop Trauma Surg 110:132–138
Fukuda A, Kato K, Sudo A, Uchida A (2010) Ganglion cyst arising from the posterolateral capsule of the knee. J Orthop Sci 15:261–264
Glasgow MMS, Allen PW, Blakeway C (1993) Arthroscopic treatment of cysts of the lateral meniscus. J Bone Joint Surg Br 75:299–302
Haklar U, Ayhan E, Ustundag S, Canbora K (2014) A new arthroscopic technique for lateral parameniscal cyst decompression. Knee 21:126–128
Hulet C, Souquet D, Alexandre P, Locker B, Beguin J, Vielpeau C (2004) Arthroscopic treatment of 105 lateral meniscal cysts with 5-year average follow-up. Arthroscopy 20:831–836
Hulet C, Menetrey J, Vargas R, Javois C, Charrois O, Beaufils P, Hardy P, Wajsfisz A, Servien E, Acquitter Y, Djian P, Chambat P, Seil R, and the French Arthroscopic Society (SFA) (2015) Clinical and radiographic results of 89 arthroscopic lateral meniscectomies in stable knees with a minimum follow up of 20 years. Knee Surg Sports Traumatol Arthrosc 23:225–231
Imamura H, Kimura M, Kamimura T, Momohara S (2014) An arthroscopic check valve release improves knee intrameniscal cyst symptoms in adolescent: a case report. Orthop Traumatol Surg Res 100:239–241
Jowett AJ, Johnston JF, Gaillard F, Anderson SE (2008) Lateral meniscal cyst causing common peroneal palsy. Skeletal Radiol 37:351–355
Kim JR, Kim BG, Kim JW, Lee JH, Kim JH (2013) Traumatic and non-traumatic isolated horizontal meniscal tears of the knee in patients less than 40 years of age. Eur J Orthop Surg Traumatol 23:589–593
Krudwig WK, Schulte K-K, Heinemann C (2004) Intra-articular ganglion cysts of the knee joint: a report of 85 cases and review of the literature. Knee Surg Sports Traumatol Arthrosc 12:123–129
Kumar NS, Jakoi AM, Swanson CE, Tom JA (2014) Is formal decompression necessary for parameniscal cysts associated with meniscal tears? Knee 21:501–503
Lantz B, Singer KM (1990) Meniscal cysts. Clin Sports Med 9:707–725
Lee W, Kim HS, Kim SJ, Kim HH, Chung JW, Kang HS, Hong SH, Choi JY (2004) CT arthrography and virtual arthroscopy in the diagnosis of the anterior cruciate ligament and meniscal abnormalities of the knee joint. Korean J Radiol 5:47–54
Locker B, Hulet C, Vielpeau C (1992) Les lésions méniscales traumatiques. Encycl Med Chir Appareil locomoteur. Fasc 14084:A 10, Exp Sci Fr
Lunhao B, Yu S, Jiashi W (2011) Diagnosis and treatment of ganglion cysts of the cruciate ligaments. Arch Orthop Trauma Surg 131:1053–1057
MacMahon J, Brennan D, Duke D, Forde S, Eustace S (2007) Ultrasound-guided percutaneous drainage of meniscal cysts: preliminary clinical experience. Clin Radiol 62:683–687
Maffuli N, Petricciulo F, Pintore E (1991) Lateral meniscal cyst: arthroscopic management. Med Sci Sports Exerc 23:779–782
Mills CA, Henderson IJ (1993) Cysts of the medial meniscus. Arthroscopic diagnosis and management. J Bone Joint Surg Br 75:293–298
Morgan-Jones R, Watson AS, Cross MJ, Saldanha JD (2001) The meniscal “pseudocyst.” A clinical sign of a torn meniscus. Am J Sports Med 29:543–544
Pandya NK, Huffman GR (2009) Intra-articular ganglion cyst of the knee originating from the transverse meniscal ligament. Curr Orthop Pract 20:470–472
Parisien JS (1990) Arthroscopic treatment of cysts of the menisci. Clin Orthop 257:154–158
Passler JM, Hofer HP, Peicha G, Wildburger R (1993) Arthroscopic treatment of the meniscal cysts. J Bone Joint Surg Br 75:303–304
Pedowitz RA, Feagin JA, Rajagopalan S (1996) A surgical algorithm for treatment of cystic degeneration of the meniscus. Arthroscopy 12:209–216
Pisani AJ (1947) Pathognomonic sign for cyst of the knee cartilage. Arch Surg 54:188–190
Raine GET, Gonet LCL (1972) Cysts of the menisci of the knee. Postgrad Med J 48:49–51
Reagan WD, McConkey JP, Loomer RL, Davidson RG (1989) Cysts of the lateral meniscus: arthroscopy versus arthroscopy plus open cystectomy. Arthroscopy 5:274–281
Rutten MJ, Collins JM, van Kampen A, Jager GJ (1998) Meniscal cysts: detection with high resolution sonography. Am J Roentgenol 171:491–496
Ryu RKN, Ting AJ (1993) Arthroscopic treatment of meniscal cysts. Arthroscopy 9:591–595
Saidi H, Ayach A, Fikry T, Oudeh K, Katabi M (2007) Intraarticular medial meniscal cyst: a report of five cases. J Trauma Sports 24:139–142
Sarimo J, Rainio P, Rantanen J, Orava S (2002) Comparison of two procedures for meniscal cysts. A report of 35 patients with a mean follow-up of 33 months. Am J Sports Med 30:704–707
Seymour R, Lloyd DC (1998) Sonographic appearances of meniscal cysts. J Clin Ultrasound 26:15–20
Śmigielski R, Becker R, Zdanowicz U, Ciszek B (2015) Medial meniscus anatomy-from basic science to treatment. Knee Surg Sports Traumatol Arthrosc 23:8–14
Sorrentino F, Iovane A, Nicosia A, Vaccari A, Candela F, Cimino PG, Midiri M (2007). High-resolution ultrasonography (HRUS) of the meniscal cyst of the knee: our experience. Radiol Med.;112(5):732–9
Steinbach LS, Stevens KJ (2013) Imaging of cysts and bursae about the knee. Radiol Clin North Am 51:433–454
Stoller DW, Martin C, Crues JV 3rd, Kaplan L, Mink JH (1987) Meniscal tears: pathologic correlation with MR imaging. Radiology 163:731–735
Thompson SM, Cross TM, Cross MJ, Wood DG (2015). Medial meniscal cyst as a cause of painful erosion of the tibial plateau. Knee Surg Sports Traumatol Arthrosc. DOI 10.1007/s00167-015-3596-6
Tschirch FT, Schmid R, Pfirmann CW, Romero J, Hodler J, Zanetti M (2003) Prevalence and size of meniscal cysts, ganglionic cysts, synovial cysts of popliteal space, fluid-filled bursae and other fluid collections in asymptomatic knees on MR imaging. Am J Roentgenol 180:1431–1436
Tyson LL, Daughters TC Jr, Ryu RKN, Crues JV III (1995) MRI appearance of meniscal cysts. Skeletal Radiol 24:421–424
Wang Y, Wluka AE, Pelletier JP, Martel-Pelletier J, Abram F, Ding C, Cicuttini FM (2010). Meniscal extrusion predicts increases in subchondral bone marrow lesions and bone cysts and expansion of subchondral bone in osteoarthritic knees. Rheumatology (Oxford). 49(5):997–1004
Wu CC, Hsu YC, Chiu YC, Chang YC, Lee CH, Shen HC, Huang GS (2013) Parameniscal cyst formation in the knee is associated with meniscal tear size: an MRI study. Knee 20:556–561
Zantop T, Rusch A, Hassenpflug J, Petersen W (2003) Intra-articular ganglion cysts of the cruciate ligaments: case report and review of the literature. Arch Orthop Trauma Surg 123:195–198
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 ESSKA
About this chapter
Cite this chapter
Hulet, C., Kopf, S., Rochcongar, G., Roland, B. (2016). Meniscal Cysts. In: Hulet, C., Pereira, H., Peretti, G., Denti, M. (eds) Surgery of the Meniscus. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-662-49188-1_24
Download citation
DOI: https://doi.org/10.1007/978-3-662-49188-1_24
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-662-49186-7
Online ISBN: 978-3-662-49188-1
eBook Packages: MedicineMedicine (R0)